Best Dental Clinic In Istanbul: How To Choose Safely
Best Dental Clinic in Istanbul
The “best” dental clinic in Istanbul is the one that matches your needs, follows strict infection-control standards, uses proven materials, and provides a clear treatment plan with aftercare. Before you book, check dentist credentials, sterilization processes, imaging and planning, transparency on costs, and how follow-up care is handled once you return home.
Table of Contents
Why Istanbul Is A Popular Choice For Dental Treatment
Istanbul attracts many international patients because clinics often combine modern dentistry with easier scheduling and competitive overall costs. Still, “dental tourism” comes with extra planning: you’re coordinating treatment, travel, and follow-up across borders. That’s why choosing carefully matters more than choosing fast.
A Practical Checklist To Find A Top Dental Clinic In Istanbul

1) Dentist Credentials And Clinical Experience
Start with the basics: Who will actually perform your treatment, and what is their training and focus area? Cosmetic cases, implants, and complex restorations benefit from a clinician who does that work routinely—not occasionally.
Ask to see before/after cases with similar starting conditions to yours. A well-run clinic will explain what’s realistic and what isn’t, instead of promising perfect results.
2) Infection Control And Sterilization Standards
Infection control is non-negotiable. A clinic should be able to explain how instruments are cleaned, packaged, sterilized, and monitored. The CDC outlines clear expectations for instrument processing, including packaging before heat sterilization and using monitoring methods to confirm sterilization effectiveness.
If the clinic avoids questions here, treat it as a red flag. You’re not being “difficult”—you’re being safe.
3) Diagnostics And Treatment Planning (Not Guesswork)
Quality dentistry begins with proper diagnosis. Depending on your case, this can include digital X-rays, photos, scans, and bite assessment. If you’re considering veneers or a smile makeover, ask how they plan aesthetics and function together, and whether you’ll see a preview (mock-up or digital design) before anything irreversible.
A thoughtful plan also includes timelines. Same-week transformations can be possible in selected cases, but rushed dentistry can create long-term problems.
4) Materials And Lab Quality
Ask what brands or material types they use for implants, crowns, and veneers, and why. You don’t need to memorize names—you just want to hear a clear rationale and understand warranty policies.
Also ask who makes your restorations. An experienced dental lab (and good communication between dentist and technician) is a big part of natural-looking, comfortable results.
5) Transparent Pricing And A Written Treatment Plan
A quote should never be a vague number in a chat message. Request a written plan that lists each procedure, the material choices, and what’s included (imaging, temporary restorations, follow-up checks, medications if needed).
The American Dental Association notes that standards, equipment, and regulations can vary by country, which makes clarity and documentation especially important when you seek care abroad.
6) Communication, Consent, And Comfort
If you’re traveling, you’ll likely communicate in English. Make sure the clinic can explain procedures, risks, alternatives, and aftercare clearly—without rushing you.
Comfort matters too. If you have dental anxiety, ask what support they offer (longer appointments, gentle techniques, or sedation options where appropriate). You should feel listened to, not managed.
7) Aftercare Plan For When You Fly Home
This is the step many people overlook. Dental tourism resources commonly emphasize planning for follow-up and understanding what happens if adjustments are needed later.
Ask these follow-up questions:
- • How many post-treatment checks are included while you’re in Istanbul?
- • What’s the plan if something feels “off” two weeks later at home?
- • Can they coordinate with your local dentist if needed?
A reliable clinic will have a clear aftercare pathway, not just a goodbye at the airport.
Questions to Ask Before Booking
• Who will perform my treatment, and what is their experience with cases like mine?
• What sterilization and monitoring steps do you follow?
• What diagnostics will you do before finalizing the plan?
• Which materials/brands are you using, and what warranty applies?
• What’s included in the price, and what could cost extra?
• What aftercare is included, and how do you support patients after travel?
Where Lygos Dental Fits in
Lygos Dental is one of the clinics in Istanbul that works with international patients. The focus is on clear treatment planning, straightforward communication, and structured aftercare for people who travel. Use the checklist above to compare any clinic, and ask for a written plan before you book.
How To Contact Lygos Dental
For appointments or questions about cosmetic dentistry, dental crowns, dental implants, or general dentistry, use the contact form below (website embed).
Frequently Asked Questions (FAQs)
How to choose a dental clinic in Turkey?
Choose a Ministry-licensed, TDA-registered clinic with modern sterilization and documented cases.
How to choose the best dental clinic?
Choose a licensed, TDA-registered clinic with specialists, transparent pricing, warranties, and verified reviews.
What is the most reputable dentist in Turkey?
No single dentist is officially the most reputable; verify TDA registration and credentials.
How to choose a clinic in Turkey?
Choose a clinic offering specialist consultation, written treatment plan, itemized quote, and aftercare.
Is it safe to get dental care in Turkey?
Yes, if the clinic is licensed, TDA-registered, and follows strict sterilization.
How much does a full set of teeth cost in Turkey?
Typically €8,000–€16,000 for full-mouth implant bridges (both jaws), depending on implants/materials.
Tooth Whitening: What We Now Know
Tooth Whitening: What We Now Know
Tooth whitening brightens natural teeth using peroxide-based gels that break down stain molecules inside enamel and dentin. Dentist-led treatments and custom take-home trays usually give the most predictable results. Temporary sensitivity is common, and crowns or fillings won’t change colour, so a dental check helps you choose a safe method and a realistic, natural-looking shade.
How Tooth Whitening Works
Table of Contents
Tooth colour changes for two main reasons: surface stains (for example, coffee, tea, red wine, and smoking) and deeper colour shifts within the tooth. Whitening can improve both, but it only works on natural tooth structure.
Most evidence-based whitening relies on hydrogen peroxide or carbamide peroxide. These agents penetrate enamel and dentin and oxidise stain compounds, which is why they can brighten teeth beyond what most “whitening toothpastes” can achieve.
What The Evidence Says About Today’s Whitening Options
In-Office Whitening
In-office whitening uses higher-concentration gels with careful gum protection and clinical supervision. The main benefit is speed and close control of soft-tissue safety.
The most common trade-off is sensitivity, often peaking in the first 24–48 hours. If you’re prone to sensitivity, dentists can adjust gel strength, limit exposure time, or use a staged plan rather than pushing for a dramatic change in one visit.
Dentist-Supervised Take-Home Trays
Custom trays with dentist-provided gel are slower than in-office whitening, but results can be very even and easier to fine-tune. Many people prefer this option because they can control day-to-day wear time and stop as soon as the shade looks right.
If your goal is a natural improvement rather than an ultra-bright change, trays are often the most flexible approach.
Over-The-Counter Strips And Kits
Whitening strips can work well for mild to moderate staining when used consistently. Results vary more than dentist-supervised options because one-size products don’t account for tooth shape, gum line, existing sensitivity, or restorations.
A practical rule: if a product burns your gums, feels sharp on exposed root areas, or triggers strong sensitivity early, stop using it and get professional advice.
Whitening Toothpastes
Most “whitening toothpastes” mainly remove surface stains through gentle abrasives and polishing agents. They can make teeth look cleaner and brighter, but they don’t usually change the underlying shade the way peroxide gels can.
They work best as maintenance after whitening, or for people who want small improvements without bleaching.
LED Or Laser “Power Whitening”
Light-activated whitening is heavily marketed, but the research is mixed. Some studies show little to no added benefit compared with peroxide alone, while others report faster initial change depending on the gel and protocol.
In practice, diagnosis, gum protection, and a sensible treatment plan usually matter more than whether a lamp is used.
What We Now Know About Safety And Side Effects
Sensitivity Is Common And Usually Temporary
Short-term sensitivity (to cold air or cold drinks) is the most common complaint. It typically settles within a few days.
Desensitising toothpaste, spacing sessions, and choosing a lower-strength plan can help. If you already have sensitivity, whitening may still be possible, but it should be planned around the cause—such as enamel wear, gum recession, cracks, or decay.
Gum Irritation Is Often A Fit And Technique Issue
Gel that leaks onto the gums can irritate soft tissue. Custom trays and professional barriers reduce this risk.
If your gums turn white briefly during whitening, that’s often a sign of chemical irritation from gel contact and a reminder that fit and application technique matter.
Whitening Doesn’t “Ruin Enamel” When Done Properly
Peroxide whitening, when used as directed, is generally considered safe and effective for healthy adults. Problems usually come from misuse: over-wearing trays, using high-strength gels too often, or stacking multiple products at the same time.
Be cautious with abrasive “hacks.” Charcoal-based products may remove some surface staining, but research has linked many charcoal formulas to increased enamel roughness/abrasion with limited true whitening benefit.
Not Everyone Is A Good DIY Candidate
A dental exam is especially important if you have:
- Cavities, cracked teeth, or leaking fillings
- Gum disease or inflamed gums
- Significant sensitivity or gum recession
- Multiple crowns, veneers, or bonding in the smile zone (they won’t whiten)
Regulations vary by country, but in many places higher-peroxide whitening gels are restricted to dental professionals, and cosmetic whitening for under-18s is generally not permitted.
Getting A Result That Looks Natural
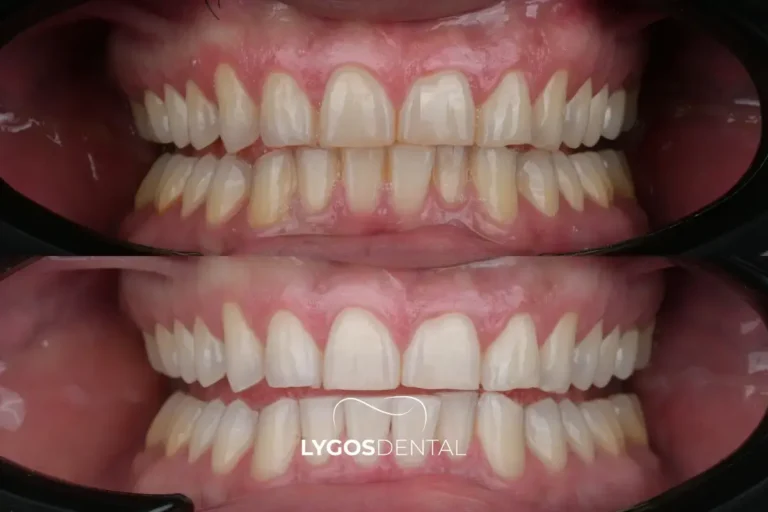
Shade Goals: Brighter Beats “Blinding”
The most believable smiles usually brighten by a few shades rather than a dramatic leap. A dentist can help you choose a target shade that suits your skin tone and avoids the greyish or overly opaque look that can happen when whitening is pushed too far.
Restorations Don’t Whiten: Plan For Colour Matching
Crowns, veneers, bonding, and tooth-coloured fillings do not change colour with whitening. If restorations show when you smile, the usual strategy is to whiten first, then replace or adjust restorations (if needed) to match the new shade.
How Long Does Whitening Last?
Longevity depends on habits and maintenance. Coffee, tea, red wine, smoking, and inconsistent brushing shorten results.
Many people maintain their shade with periodic “top-ups” (often using trays) rather than repeating full-strength whitening frequently.
A Simple Pre-Whitening Checklist
Before you spend money on kits or sessions, make sure you know:
- Whether your staining is mainly surface-level or deeper colour change
- If you have restorations that will need shade matching
- Your sensitivity risk and how to reduce it
- Which method best protects your gums and enamel
A short dental appointment can prevent weeks of trial-and-error and help you get a result that looks natural.
Book A Whitening Consultation
If you’d like personalised advice, a dentist can check for hidden causes of discolouration, assess sensitivity risk, and recommend a whitening plan that fits your teeth and any visible restorations.
Frequently Asked Questions (FAQs)
What to know after teeth whitening?
Avoid staining foods and smoking for 24–48 hours; expect temporary sensitivity.
Is niacinamide good for teeth whitening?
Niacinamide isn’t proven to whiten teeth; use dentist-approved whiteners for predictable results.
What to know before getting your teeth whitened?
Get a dental exam; treat cavities/gum disease; match expectations; plan for sensitivity.
How do you know if teeth whitening is working?
You’ll see teeth lighten a few shades within days; compare photos or shade guide.
What is not allowed after teeth whitening?
Avoid coffee, tea, red wine, tobacco, and dark sauces for 24–48 hours.
How soon to brush teeth after whitening?
Wait about 30 minutes, then brush gently with a soft toothbrush.
What is a Temporary Filling?
What Is A Temporary Filling?
A temporary filling is a short-term material placed to protect a tooth while treatment is still in progress. Dentists use it after procedures like root canal therapy or when a tooth needs time to settle before a permanent filling or crown. It helps block bacteria, reduce sensitivity, and keep the tooth sealed until your next appointment.
Temporary Fillings Explained
A temporary filling is used when a tooth needs protection, but the final restoration cannot be placed yet. It acts like a protective cover, sealing the tooth between visits. This step is planned and common in treatments that require more than one appointment.
When A Temporary Filling Is Needed
Temporary fillings are often placed after a root canal when the inside of the tooth has been treated but the final restoration must wait. They are also used when swelling, infection, or sensitivity needs to calm down first. Placing a permanent filling too soon can increase the risk of ongoing pain or complications.
Dentists may choose a temporary filling when:
- The tooth is still sensitive.
- Pain needs to be monitored between visits.
- A permanent filling or crown is being prepared.
- The tooth needs short-term sealing and protection.
How Long Do Temporary Fillings Last?
Table of Contents
Temporary fillings are not designed to last for months or years. Many stay in place for a few days to a few weeks, depending on the material and the bite forces on that tooth. Because the material is softer than permanent options, it can wear down, crack, or fall out over time.
If a temporary filling comes out, avoid leaving the tooth open. Food and bacteria can irritate the area, especially after root canal treatment. Contact your dentist as soon as you can for advice and a replacement.
Why Dentists Use Temporary Fillings
A temporary filling helps protect a tooth without rushing the final treatment. Every tooth responds differently, and your dentist may want to confirm that symptoms improve before placing a long-lasting restoration. This approach can reduce the chance of future sensitivity or the need for repeat treatment.
A temporary filling can help by:
- Keeping food out of the tooth.
- Blocking bacteria from entering the treated area.
- Reducing sensitivity to cold, heat, or pressure.
- Giving your dentist time to plan the next step.
Temporary Vs Permanent Fillings
The difference is not only how long they last. Temporary fillings are softer and easier for a dentist to remove at the next visit. Permanent fillings are stronger, built for daily chewing, and intended to last for years when the tooth is stable.
Temporary fillings are typically:
- Softer and more flexible.
- Easier to remove.
- Not intended for heavy chewing.
- Used for short-term protection.
Permanent fillings are typically:
- Stronger and more wear-resistant.
- Designed for everyday chewing.
- Made to last for years with proper care.
- Placed once the tooth is stable and symptoms are resolved.
Is A Temporary Filling Painful?
Getting a temporary filling is usually comfortable. If the tooth was treated just before the filling, it is often already numb. You may feel pressure during placement, followed by mild sensitivity afterward.
Mild sensitivity often settles on its own. Sharp pain, increasing discomfort, or swelling is not typical and should be checked by a dentist.
Can You Eat Normally With A Temporary Filling?

You can eat, but it helps to be careful because temporary materials are not as strong as permanent restorations. Hard, crunchy, or sticky foods can chip the filling or pull it out. If possible, chew on the opposite side until your next appointment.
Helpful tips include:
- Wait a few hours before eating if your dentist recommends it.
- Avoid sticky foods like toffee or chewing gum.
- Skip very hard foods such as ice, nuts, or hard candy.
- Chew gently and avoid biting directly on the filled tooth.
How To Care For A Temporary Filling
Daily care is similar to your normal routine, but gentle technique matters. Brush carefully around the tooth and avoid aggressive scrubbing at the edges of the filling. When flossing, slide the floss out to the side instead of snapping it upward, which can dislodge the material.
Most importantly, keep your follow-up appointment. Temporary fillings are a planned step, not the final solution, and delaying treatment can lead to cracking or reinfection.
When To Call Your Dentist
Reach out to your dental office if the filling falls out, the tooth feels sharp, or you notice worsening pain. It is also worth calling if you have swelling, fever, or a bad taste that does not go away. These signs can suggest irritation or infection that needs timely care.
Appointment And Service Information
If you have questions about a temporary filling or need to schedule a follow-up visit, contact your dental clinic for guidance. Many practices can also advise on cosmetic dentistry, crowns, implants, and general dentistry options based on your needs.
Frequently Asked Questions
How long does a temporary filling last?
A temporary filling usually lasts a few days to several weeks, sometimes longer.
Why would a dentist do a temporary filling?
A dentist uses a temporary filling to protect a tooth between treatment visits.
What is the difference between temporary and permanent filling?
Temporary fillings are short-term and weaker; permanent fillings are durable, long-term restorations.
Can I eat normally with a temp filling?
Yes, but avoid sticky, hard, or very hot foods that can dislodge it.
What are the disadvantages of temporary fillings?
They can wear, leak, break, or fall out, causing sensitivity or decay risk.
Can you brush your teeth normally with a temporary filling?
Yes, brush gently and floss carefully, keeping pressure off the temporary filling.
Why Do Teeth Become Transparent and How to Fix It?
Why Do Teeth Become Transparent And How To Fix It
Transparent (translucent) teeth usually mean the enamel has thinned, most often from acid exposure, teeth grinding, aggressive brushing, or reflux. Because enamel doesn’t grow back, the goal is to stop further wear and restore strength and appearance with options like fluoride support, bonding, veneers, or crowns—based on how much enamel has been lost.
What It Means When Teeth Look Transparent
Healthy teeth look slightly off-white and solid. When the edges of a tooth start to look clear or glassy—especially on the front teeth—it usually points to enamel thinning.
Enamel is the hard outer layer that protects the tooth. Under it is dentin, which is naturally darker and more yellow. As enamel wears down, more dentin shows through, making the tooth look translucent at the tips
Common Causes Of Transparent Teeth

Table of Contents
Tooth transparency rarely has a single cause. It usually builds up over time from repeated exposure to acid, pressure, or abrasion.
Acidic Foods And Drinks
Soda, energy drinks, citrus juices, sports drinks, and frequent snacking on acidic foods can soften enamel. Once enamel is softened, normal chewing and brushing can wear it down faster.
Teeth Grinding Or Clenching
Night-time grinding (bruxism) or daytime clenching puts constant pressure on teeth. The edges and biting surfaces often thin first, which is why transparency commonly appears at the tips.
Brushing Too Hard Or Using A Hard Brush
Scrubbing aggressively or using a hard-bristled toothbrush can gradually abrade enamel and irritate gums. A soft brush and gentle technique clean just as well with less damage.
Acid Reflux Or Frequent Heartburn
Stomach acid is extremely erosive. If reflux reaches the mouth—especially at night—it can slowly dissolve enamel without you noticing until sensitivity or translucency appears.
Whitening Overuse
Overusing whitening products can increase sensitivity and may make thin enamel look more translucent. Whitening doesn’t replace lost enamel, so it’s best used under dental guidance when enamel is already compromised.
Natural Aging And Wear
Enamel naturally becomes thinner with age. Everyday chewing, past dental work, and long-term habits can speed up normal wear.
Is Tooth Transparency A Problem?
Sometimes it’s mainly a cosmetic concern, but it can also be a warning sign. Thinner enamel means less protection against temperature changes, acids, and physical stress.
With ongoing wear, teeth can become more sensitive, chip more easily, or develop rough edges. If you notice fast changes, sensitivity, cracks, or uneven tooth length, a dental exam is worth booking sooner rather than later.
How To Fix Transparent Teeth
The right solution depends on how much enamel is left and whether the tooth has weakened.
Support And Protect Remaining Enamel
In early stages, a dentist may recommend fluoride varnish, prescription fluoride toothpaste, or remineralizing products to help strengthen the surface and slow further erosion. These options can’t rebuild lost enamel thickness, but they can improve resistance to acid and sensitivity.
Dental Bonding
For mild transparency, tooth-colored composite bonding can restore a solid-looking edge and add a protective layer. Bonding is conservative and typically completed in a single visit, though it can stain or chip over time and may need touch-ups.
Porcelain Veneers
If front teeth look see-through and the appearance bothers you, veneers can cover the front surface and create a more natural, even shade. Veneers are durable, but they usually require removing a small amount of enamel.
Crowns Or Onlays
When the tooth structure is weakened or there are cracks, a crown or onlay may be the safest way to protect the tooth long term. These restorations reinforce the tooth and reduce the risk of fracture.
How To Prevent Teeth From Becoming Transparent
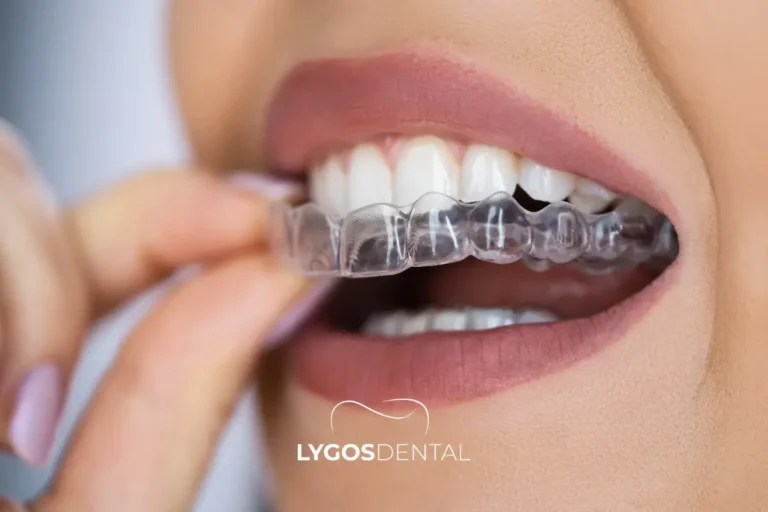
Small changes can slow enamel wear and help teeth keep their natural opacity.
Use A Soft-Bristled Toothbrush
Brush gently with a fluoride toothpaste for two minutes, twice a day. If you’re unsure about technique, ask your dentist or hygienist to show you a low-abrasion method.
Wait After Acidic Foods
After acidic drinks or meals, rinse with water and wait about 30 minutes before brushing. Brushing right away can scrub softened enamel.
Reduce Acid Exposure
Limit sipping acidic drinks over long periods. Use a straw when possible, and choose water between meals to give saliva time to neutralize acid.
Treat Grinding And Clenching
If you wake up with jaw tension or notice flattened edges, ask about a night guard. Reducing grinding can prevent further thinning.
Manage Reflux
If you have frequent heartburn, speak with a medical professional. Managing reflux protects both your teeth and overall health.,
Book An Appointment
If you’re concerned about translucent teeth or sensitivity, a dentist can check for enamel erosion, grinding, or reflux-related wear and recommend the least invasive fix. Cosmetic options like bonding or veneers can often restore a natural, solid look once the underlying cause is under control.
Frequently Asked Questions
Can transparent teeth be fixed?
Yes; early cases may remineralize, otherwise bonding, veneers, or crowns restore appearance.
Is there a way to reduce transparency in teeth?
Yes; use fluoride, limit acids, treat grinding, and consider cosmetic bonding.
Is it bad if my teeth are becoming transparent?
Yes; it often signals enamel loss and higher sensitivity or decay risk.
What deficiency causes transparent teeth?
Usually none; acid enamel erosion causes transparency, sometimes childhood vitamin D/calcium deficiency.
What vitamins help with translucent teeth?
Vitamin D with adequate calcium supports remineralization; no vitamin rebuilds lost enamel.
Can vitamin D reverse yellow teeth?
No; vitamin D won’t reverse yellowing—professional cleaning or whitening treats discoloration.
Dental Implants for Diabetics
Dental Implants for Diabetics: What You Need to Know
Most people with well-controlled diabetes can get dental implants safely. The key is stable blood sugar before and after surgery, healthy gums, and careful aftercare. Many clinics look for an HbA1c around 7% (53 mmol/mol) or lower, with final decisions tailored to your overall health and infection risk.
Why Diabetes Changes Implant Planning
Diabetes can affect how quickly the body heals and how well it fights infection. When blood glucose runs high, soft tissue repair may slow down and inflammation can stay active longer.
Dental implants depend on predictable healing of the gum tissue and the jawbone. If healing is delayed, the implant may take longer to integrate with bone, and the risk of early infection increases.
Can You Get Dental Implants If You Have Diabetes?

Table of Contents
In many cases, yes. Diabetes alone does not disqualify you from implant treatment, especially when your blood sugar is stable and your mouth is healthy.
Your dentist will usually review your recent medical history, medications, gum health, bone quality, and day‑to‑day glucose control. Coordination with your physician may also be recommended for patients with complex medical histories.
HbA1c And Blood Sugar Targets Before Surgery
HbA1c reflects your average blood sugar over roughly the last 2–3 months. Because it is linked to healing and infection risk, many clinics use HbA1c as a practical benchmark before implant surgery.
A common target is around 7% (53 mmol/mol) or lower. Some patients with results slightly above this may still be eligible, but higher HbA1c values often mean it is safer to improve control first.
If your HbA1c is elevated, your dentist may delay surgery and work with you on a plan that can include periodontal treatment, hygiene support, and medical follow‑up. That delay is about reducing risk, not denying treatment.
Who Is And Isn’t A Good Candidate

Implant candidacy depends on overall health, gum stability, and your ability to follow aftercare. These factors matter for everyone, but they carry extra weight in diabetes.
Implants may not be recommended, or may need to be postponed, if you:
- Have uncontrolled or highly variable blood sugar
- Have active, untreated gum disease
- Smoke heavily and are not willing to stop during healing
- Have severe bone loss without a predictable grafting option
- Have medical conditions or medications that significantly impair healing (your dentist will review this with you)
If any of these apply, it does not always mean “no.” It often means “not yet,” with a focus on stabilizing the risk factors first.
What The Process Looks Like For Diabetic Patients
Planning is usually more detailed, with an emphasis on preventing infection and supporting healing. Your clinician may recommend a periodontal assessment, professional cleaning, and imaging before confirming the surgical plan.
Some practices use short-term antiseptic rinses and, in selected cases, preventive antibiotics. You will also be given a clear plan for pain control, nutrition, and home care that will not disrupt glucose management.
Healing And Aftercare
Healing time varies, but the goal is the same: stable gums, low inflammation, and strong bone integration. Many people with controlled diabetes heal on a similar timeline to non‑diabetic patients, while others need a little longer.
After surgery, focus on these basics:
- Keep blood sugar as stable as possible and follow your medical plan
- Brush gently but thoroughly, and clean around the implant exactly as instructed
- Attend follow‑up visits so your dentist can track healing early
- Avoid smoking, and keep alcohol intake modest during the healing phase
- Call the clinic if you notice increasing swelling, pus, persistent bleeding, fever, or a “loose” sensation
Long‑Term Risks And How To Reduce Them

The main long‑term concern is peri‑implant inflammation (mucositis or peri‑implantitis). Diabetes is associated with a higher risk of these complications, especially when glucose control is poor.
The best protection is routine maintenance: daily home cleaning, regular professional cleanings, and early treatment if bleeding or deep pockets develop. If you have a history of gum disease, your maintenance schedule may be more frequent.
Frequently Asked Questions
Should people with diabetes get dental implants?
Yes, with well-controlled diabetes and coordinated care, dental implants are usually appropriate.
Who should not do dental implants?
People with poorly controlled diabetes should avoid implants until diabetes is controlled.
Can diabetics get permanent dentures?
Yes, controlled diabetics can get fixed implant-supported dentures after medical and dental assessment.
What to know before getting dental implants?
Know your HbA1c, gum health, bone volume, medications, and smoking status beforehand.
Can a diabetic do dental implants?
Yes, if HbA1c is controlled; otherwise infection and failure risks increase.
What is the success rate of dental implants in diabetic patients?
About 96–97% at 1 year and 87–96% at 5 years controlled diabetes.
Itchy Gums: Causes and Treatment
Itchy Gums: Causes and Treatment
Itchy gums are usually a sign of irritation or early inflammation along the gumline—most often from plaque buildup. They can also be triggered by dry mouth, sensitivity to oral care products, allergies, or something rubbing the gums. If itching comes with bleeding, swelling, bad breath, or loose teeth, a dental check is the safest next step.
Gums can itch in a way that feels “tickly,” irritated, or slightly sore. Some people notice it after brushing, others on waking, and sometimes it’s limited to one tooth.
The goal is to identify what’s driving the irritation so you can calm the tissue and prevent it from progressing into a bigger gum problem.
What Itchy Gums Usually Mean
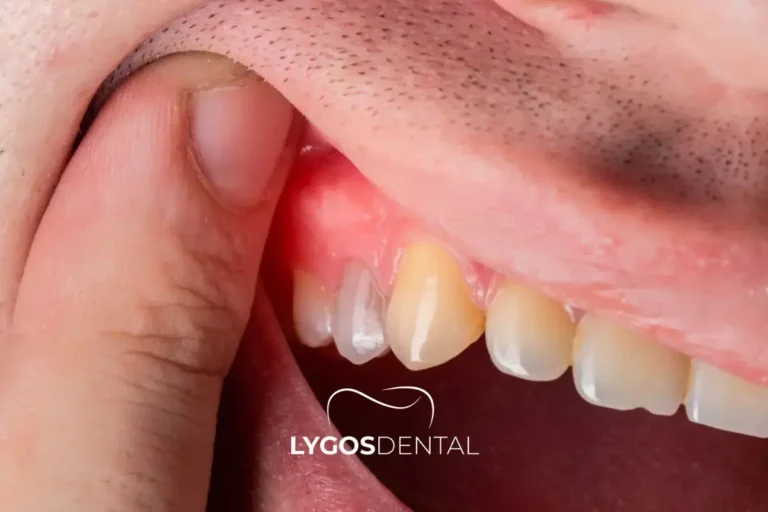
Table of Contents
Most of the time, itching is your body’s way of flagging irritation at the gum edge. That irritation may be caused by inflammation (often from plaque), a contact reaction to a product, dryness, or mechanical rubbing. The right fix depends on the trigger, so it helps to look for patterns—when it starts, where it happens, and what makes it better or worse.
Most Common Cause: Plaque And Early Gingivitis

If you had to pick one main culprit, it’s plaque along the gumline. Plaque is a soft, sticky film that forms every day. When it sits near the gums, the tissue can become inflamed and may feel itchy, tender, or “tickly.” The early stage of gum inflammation is called gingivitis.
Signs It’s Likely Gingivitis
- Gums that bleed when you brush or clean between teeth
- Redness, puffiness, or a shiny gum edge
- Bad breath or a lingering “off” taste
Gingivitis is often reversible with consistent daily cleaning and a professional scale and polish if tartar has built up.
Other Causes Of Itchy Gums
Sensitivity To Toothpaste Or Mouthwash
If itching started soon after switching toothpaste, mouthwash, whitening products, or even flavored floss, a sensitivity is possible. Strong flavors and certain additives can irritate the soft tissue in some people. A useful clue is timing: symptoms appear shortly after use and improve when you stop.
Dry Mouth, Especially At Night
A dry mouth can leave gum tissue feeling raw and more vulnerable. Saliva helps neutralize acids and control bacteria, so when there’s less of it, the mouth can feel uncomfortable and gum inflammation can flare more easily. Mouth breathing, some medications, dehydration, and snoring can all contribute.
Allergies And Seasonal Triggers
Some people notice oral itching during allergy seasons. Post-nasal drip, sinus congestion, and general inflammation can make the mouth feel sensitive. If itching coincides with other allergy symptoms and settles when those do, allergies may be part of the picture.
Hormonal Changes
Hormonal shifts can make gums more reactive, so they may bleed or feel irritated more easily. This is sometimes seen during puberty, pregnancy, and menopause. Good daily cleaning and regular dental checks are especially helpful during these times.
Something Rubbing The Gumline
Retainers, aligners, dentures, or a rough edge on a filling or crown can rub the gumline and keep it inflamed. If the itch is in one spot—especially if it feels sore—mechanical irritation is worth checking.
Brushing Or Flossing Technique
If you’ve recently started cleaning between teeth again, or you’re brushing hard, the gums can feel irritated at first. Aim for gentle technique and consistency. Cleaning between teeth is one of the most effective ways to calm gum inflammation over time.
When It May Be More Than Early Inflammation
If gum disease progresses, symptoms often move beyond itching to bleeding, recession, and sometimes tooth looseness. Persistent itching shouldn’t be ignored, especially if it’s accompanied by other changes.
Safe At-Home Relief
If itching is mild and you’re not seeing obvious swelling, severe pain, or ulcers, these steps are a sensible place to start.
- Clean the gumline gently—but thoroughly.Brush twice daily with a soft-bristled brush, focusing on the gum edge rather than scrubbing. Consistency matters more than pressure.
- Clean between teeth once a day.Use floss or an interdental brush/pick that fits comfortably. If you’re new to it, a little tenderness can happen at first, but it should improve with gentle daily care.
- Pause new products for a week.If you recently changed toothpaste or mouthwash, switch back to a plain, mild option. If the itch fades, you’ve found a likely trigger.Use a soothing rinse.
- Warm saltwater can feel calming for irritated gums. Keep it gentle—overusing strong antiseptic mouthwashes can sometimes make dryness and irritation worse.
- Check for a ‘hot spot’.
Run your tongue along the area. If something feels sharp, tight, or scratchy, don’t file or cut anything yourself. If it’s an aligner or retainer, contact your dental team for advice.
Treatments Your Dentist May Recommend
Dental treatment focuses on removing the cause of irritation and supporting your daily routine so symptoms don’t keep returning.
Professional Cleaning
If plaque and tartar are driving the irritation, a professional clean removes what home care can’t. For many people, this is the turning point for persistent itchy or bleeding gums.
Gum Health Assessment And Tailored Care
Your dentist may measure gum pockets, check for inflammation, and suggest the right interdental tools for your spacing and gum health. Early support can help prevent progression.
Adjusting Appliances Or Restorations
If a retainer or aligner is pinching, or a restoration edge is irritating the gum, a small adjustment can make a big difference.
When To Book A Dental Appointment
Book an appointment if you notice any of the following:
- Bleeding when brushing, flossing, or eating crunchy foods
- Swollen, sore, or receding gums
- Persistent bad breath or a bad taste that doesn’t settle
- Loose teeth, changing gaps, pus, or a gum abscess
If itching is persistent, keeps returning, or is limited to one area that feels tender, it’s worth getting it checked. Early treatment is usually simpler and more comfortable.
Prevention Tips For Healthier Gums
- Brush twice daily with a soft brush and fluoride toothpaste
- Clean between teeth daily with floss or interdental brushes
- Replace your brush head regularly and avoid hard brushing
- Stay hydrated and address dry mouth if it’s a regular issue
- Keep up with routine dental check-ups and professional cleaning
Frequently Asked Questions (FAQs)
How do I stop my gums from itching?
Rinse with warm saltwater, brush gently, floss, avoid irritants; see a dentist.
What is a home remedy for itchy gums?
Warm saltwater rinses and cold compresses can soothe; avoid spicy or acidic foods.
What does it mean if your gums are itchy?
Itchy gums often indicate gingivitis, allergy, irritation, or healing; persistent symptoms need dental evaluation.
How to get rid of a itchy gum?
Treat the cause: improve oral hygiene, rinse with saltwater, avoid irritants; see a dentist.
Is gum itching a symptom of diabetes?
Gum itching isn’t specific, but diabetes increases gum disease risk; get checked if concerned.
What disease starts with itching?
Itching can be an early sign of eczema, allergy, liver disease, or kidney disease.
What Helps Toothache Under a Filling? At Home and Naturally
What Helps Toothache Under a Filling? At-Home and Natural Relief
A toothache under a filling is often caused by a high bite, short-term sensitivity, or irritation near the nerve. At home, rinse with warm saltwater, use a cold compress, and consider over-the-counter pain relief if it’s safe for you. Avoid chewing on that side and watch for swelling, fever, or pain that lasts longer than two days.
Pain under a filling can feel surprising, especially if the procedure seemed straightforward. Sometimes it settles on its own as the tooth calms down. Other times, it’s a sign the bite needs adjustment or the tooth needs further treatment.
Below are practical steps you can take at home, sensible “natural” options, and clear signs that you shouldn’t wait.
Why A Tooth Can Hurt Under A Filling
Most pain under a filling falls into a few common patterns. The timing and what triggers the pain can offer clues.
A High Filling Or Bite Imbalance
If the filling sits slightly too high, that tooth can take extra pressure when you bite down. This often feels like sharp pain when chewing. A dentist can usually fix it quickly with a simple bite adjustment.
Normal Post-Filling Sensitivity
It’s common to feel sensitivity to cold, sweet foods, or pressure for a short period after a filling. This usually improves as the tooth settles. If sensitivity is mild and trending better, home care may be enough while you monitor it.
Pulp Irritation Or Pulpitis
A deep cavity or drilling close to the nerve can irritate the pulp inside the tooth. This may cause lingering sensitivity or throbbing pain. Sometimes it improves, but worsening or persistent pain can mean the nerve needs treatment.
Leakage, New Decay, Or A Crack
If a filling loses its seal, if decay returns at the edges, or if the tooth develops a crack, bacteria can reach sensitive areas. Pain that keeps coming back, changes in intensity, or becomes hard to ignore is worth a dental check.
What Helps At Home Right Now

Table of Contents
These steps are low-risk and can help you stay comfortable until you can be evaluated. They won’t fix the underlying cause, but they can reduce irritation and pain.
Warm Saltwater Rinse
Rinse gently with warm saltwater, especially after eating. It can help keep the area clean and soothe irritated gum tissue.
Cold Compress On The Cheek
If the area feels sore or slightly swollen, apply a cold compress to the outside of the cheek for short intervals. Avoid putting heat on facial swelling.
Over-The-Counter Pain Relief (If Safe For You)
Nonprescription pain relievers such as ibuprofen or acetaminophen are commonly used for dental pain until you can see a dentist. Follow the label directions and avoid them if you’ve been advised not to take them.
Avoid Triggers For 24–48 Hours
- Chew on the other side.
- Skip very hot or very cold foods and drinks.
- Avoid hard, crunchy bites that put pressure on the filling.
- Limit sugary or acidic snacks if they spike sensitivity.
Keep The Area Clean (Gently)
Brush softly and floss carefully. If food is stuck near the edge of the filling, removing it can reduce pressure and gum irritation.
Natural Remedies: What’s Reasonable

Some home remedies may offer short-term comfort. Use them cautiously, and treat them as temporary support—not a substitute for dental care.
Clove Oil (Short-Term Only, Use Carefully)
Clove oil contains eugenol, which can numb the area for a short time. If you use it, dilute it and apply sparingly. Undiluted clove oil can irritate or burn oral tissues.
Peppermint Tea Bag Compress (Mild, Optional)
A cooled peppermint tea bag held against the sore area can feel soothing for some people. It won’t treat the cause, but it may help you feel more comfortable.
What To Avoid
- Heat on facial swelling (it may worsen inflammation).
- Placing aspirin directly on the gums (it can burn tissue).
- Relying on “natural antibiotics” instead of getting dental care when pain persists.
When To See A Dentist Urgently
Home care is only a bridge. Seek dental advice quickly if any of the following applies:
- Pain lasts longer than two days, is getting worse, or disrupts sleep.
- Swelling, fever, or feeling generally unwell.
- Severe throbbing, a bad taste, or pus.
- Swelling that affects breathing or swallowing (seek urgent medical care).
What A Dentist Can Do For Pain Under A Filling
Treatment depends on the cause. Common options include:
- Bite adjustment if the filling is high.
- Polishing, repairing, or replacing the filling if the seal is compromised.
- Treating recurrent decay at the filling margins.
- Root canal treatment if the nerve is irreversibly inflamed or infected.
Antibiotics are not the first-line solution for most dental pain. They’re generally considered when there are signs of spreading infection or systemic symptoms, alongside the right dental treatment.
Get Information Now
Contact us to learn more about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry. You can also book an appointment or request service information using the form below.
Frequently Asked Questions
How to soothe toothache from filling?
Take ibuprofen/paracetamol if safe, rinse salt water, avoid hot/cold and chewing; see dentist if persistent.
What is the strongest natural pain reliever for toothache?
Clove oil (eugenol) numbs tooth pain best; use diluted, briefly, and avoid swallowing.
How to treat a tooth that needs a filling at home?
You can’t treat a cavity at home; keep clean, fluoride toothpaste, avoid sugar, book dentist.
What is the 3 3 3 rule for toothaches?
It’s informal: soothe/rinse every 3 hours for 3 minutes; see dentist in 3 days.
How long does it take for a dental filling to stop hurting?
Minor sensitivity usually settles within a few days and resolves in 1–2 weeks.
How to Choose the Right Dentist for Root Canal Treatment
How to Choose the Right Dentist for Root Canal Treatment
Choosing the right dentist for a root canal comes down to clinical experience, modern imaging and cleaning tools, and clear communication about your options. Ask how many similar cases they treat, whether they use digital X‑rays and precise canal measurement, and when they refer to an endodontist. A calm, comfort-focused approach matters as much as technique.
For many people, the idea of a root canal feels stressful long before they sit in the dental chair. Much of that fear comes from old stories and outdated experiences.
Today, root canal treatment is usually controlled and far more comfortable than expected. The biggest factor that shapes the outcome is the dentist you choose.
At Lygos Dental, patients often ask how to tell whether they’re in the right hands. The answer isn’t just about titles—it’s about experience, planning, and how clearly the dentist guides you through the process.
What A Root Canal Actually Involves
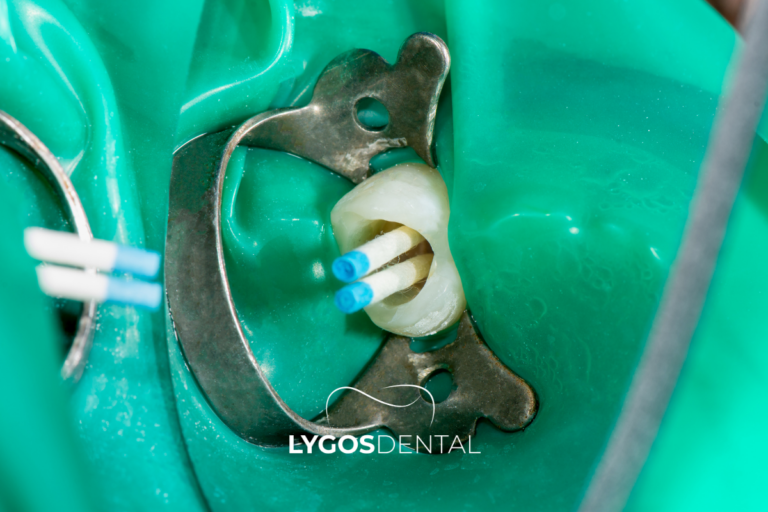
Table of Contents
A root canal is recommended when the inner part of a tooth becomes infected or inflamed. This space contains nerves and blood vessels, which is why pain can become intense if the problem is left untreated.
During treatment, the dentist removes the infected tissue, cleans the canals inside the tooth, and seals them to prevent bacteria from returning. When the canals are fully cleaned and sealed, the infection-related pain typically settles and the natural tooth can be preserved.
Precision matters. Missing even a small area can raise the risk of lingering symptoms or reinfection.
Why The Dentist’s Experience Matters
Root canals aren’t one-size-fits-all. Some teeth have one straight canal, while others have multiple canals that curve, branch, or narrow.
A dentist with strong root canal experience is more likely to locate every canal, manage unexpected anatomy, and reduce the chance of reinfection. Experience often matters more than speed or price.
General Dentist Or Endodontist: How To Decide
Many general dentists perform root canal treatment regularly and achieve excellent results—especially for straightforward cases. In more complex situations, an endodontist (a root canal specialist) may be the safer choice.
A referral is commonly recommended when the tooth is a molar with multiple canals, the roots are unusually curved, a previous root canal has failed, or there’s a significant infection at the root tip.
This isn’t about passing responsibility. It’s about choosing the level of expertise that best protects the tooth.
Technology And Tools That Improve Results
Modern root canal treatment relies on accurate diagnosis and controlled cleaning. A well-equipped clinic should use clear imaging and precise measurement so the canals can be treated to the correct depth.
Helpful tools may include digital X‑rays, electronic measuring devices for canal length, and modern irrigation/cleaning systems. Better tools don’t replace skill, but they support consistency and can make the appointment more comfortable.
Communication That Builds Trust
A good dentist doesn’t rush the explanation. Before treatment, you should understand why the root canal is needed, how many visits are expected, what you’ll feel during and after the appointment, and what restoration (often a filling or crown) is planned afterward.
If you feel pressured or leave the consultation confused, pause and ask questions. Comfort starts with clarity.
Pain Management And Patient Comfort
One of the biggest fears around root canals is pain. With modern anesthesia, most patients are comfortable during treatment.
What matters is how carefully numbness is achieved and how closely the dentist checks in during the procedure. You shouldn’t be expected to “tolerate” pain—tell your dentist right away if you feel anything sharp or uncomfortable.
Questions To Ask Before You Book
- How many root canal cases like mine do you treat in a typical month?
- Will you take updated X‑rays, and do you use precise canal length measurement?
- Do you handle molars and complex canals in-house, or refer to an endodontist?
- What should I expect after treatment, and will I need a crown?
- What is your plan if symptoms persist or the tooth needs retreatment?
Book An Appointment
If you’d like to discuss root canal treatment, contact our team to review your symptoms, imaging, and treatment options. We can also advise whether your case is best treated by a general dentist or an endodontist.
Frequently Asked Questions
What type of dentist is best for a root canal?
An endodontist is best for root canal treatment.
What is the 2 2 2 rule in dentistry?
Brush twice daily for two minutes, and see your dentist twice yearly.
What is the 80/20 rule in dentistry?
It’s the Pareto principle: 80% results come from 20% causes or patients.
What is the 3-3-3 rule for toothache?
It’s an informal pain mnemonic: ibuprofen three times daily for three days, if safe.
Should you let a regular dentist do a root canal?
Yes, if experienced; complex cases are better handled by an endodontist.
What is the normal cost of a root canal?
Varies by country; typically $700–$1,700 per tooth without insurance, plus crown.
Best Dental Clinics in Turkey
Best Dental Clinics in Turkey
Turkey has become a leading destination for veneers, implants, and full smile makeovers thanks to experienced dentists, modern private clinics, and fast treatment timelines. The best results come from choosing a clinic that plans carefully, uses reputable materials, and communicates clearly before and during treatment—rather than focusing on the lowest price.
Why Turkey Became Popular For Dental Treatment
Turkey attracts dental patients from the UK, Europe, the US, and the Middle East for one main reason: value. Treatment often costs less than in many Western countries, while many private clinics operate with modern equipment and strong clinical standards.
High patient volume also plays a role. Dentists who perform cosmetic and restorative work every day build practical skill quickly, which can show in consistency and finishing details.
Time matters, too. In many countries, consultations and procedures can involve long waits. In Turkey, clinics that work with international patients typically move faster, which helps people fit care into a planned trip.
Not Every Clinic Is The Same
Turkey has a wide range of clinics, and quality can vary. A reputable clinic looks beyond teeth alone and evaluates bite, gums, and how the smile fits the face.
Good clinics avoid rushing. They explain options, set realistic expectations, and recommend what makes sense clinically—not what increases the bill.
Clear communication is a strong signal. If answers are vague, promises sound too perfect, or the plan changes without explanation, treat it as a warning sign.
Common Dental Treatments People Travel For
International patients most often travel for treatments that can be completed over a short visit, such as:
- Veneers
- Dental implants
- Zirconium or porcelain crowns
- Full smile makeovers
- Teeth whitening
Your exact timeline depends on diagnosis, healing needs, and how complex the case is. A solid clinic will outline the steps before you book travel.
How Lygos Dental Approaches Treatment
Table of Contents
At Lygos Dental, treatment planning is built around the individual patient rather than a one-size-fits-all package. The focus is on natural-looking outcomes that suit facial features and bite, not overly bright or artificial results.
Before any procedure starts, the team checks measurements and details that affect long-term comfort. Material choice is handled carefully, and unnecessary work is avoided when it does not support the goal.
Patients are kept informed throughout the process. When you understand what is happening at each step, it is easier to feel confident—especially when you are traveling for care.
Book An Appointment
To learn more about cosmetic dentistry, crowns, implants, or general dentistry at Lygos Dental, contact the clinic to request an evaluation and treatment plan.
Frequently Asked Questions (FAQs)
Where is the best place to get your teeth done in Turkey?
Istanbul is top for complex dental work; Antalya and Izmir are strong alternatives.
How to choose a dental clinic in Turkey?
Choose Ministry-authorized clinics, TDB-registered dentists, written treatment plans, and documented outcomes.
Is getting your teeth done in Turkey a good idea?
Yes—when you verify licensing, specialist training, quality materials, and aftercare arrangements.
What is the average price to get your teeth done in Turkey?
Average full set of 20 veneers in Turkey costs about $3,500–$6,000.
Who is the number one dentist in Turkey?
No official “number one” dentist; pick a specialist with audited results and aftercare policy.
Where do celebs go in Turkey for teeth?
Celebrities often use private, high-end Istanbul clinics; specific clinics aren’t reliably disclosed.
Hacks: Forgot Your Toothpaste, Now What?
Forgot Your Toothpaste? Now What?
If you forgot your toothpaste, brush with a clean toothbrush and water instead of skipping brushing. Brushing removes plaque and food debris even without paste. If you need a short-term backup, use salt water or a tiny amount of baking soda once or twice. Avoid acidic or abrasive DIY options that can damage enamel.
It happens to almost everyone: you’re packing, rushing out the door, or finishing your morning routine when you realize you have no toothpaste. The good news is that one missed tube won’t undo your oral health. What matters is keeping the cleaning step in your routine.
At Lygos Dental, we hear this question often, especially from travelers and busy families. Here’s what to do right away, plus a few safe stopgaps until you’re back to your usual fluoride toothpaste.
First Rule: Don’t Skip Brushing
If toothpaste is missing, doing nothing is the worst choice. A toothbrush and water can still remove plaque, food particles, and bacteria from the tooth surface and along the gumline.
Toothpaste supports the process, but the brushing motion does most of the mechanical cleaning. So if you’re choosing between brushing without toothpaste and not brushing at all, brushing wins every time.
Safe Temporary Alternatives To Toothpaste

Table of Contents
These options can help for a day or two when toothpaste isn’t available. They are not meant to replace a normal fluoride routine.
1) Water And A Toothbrush
This is the safest fallback. Brush gently for two minutes, focusing on the gumline and the back teeth where plaque builds up. Rinse well after brushing.
2) Salt Water Rinse (Or Light Brushing)
Mix a small pinch of salt into warm water. Swish for 30–60 seconds, then spit. You can also dip your brush into the solution and brush gently if that feels more effective.
Salt can make your mouth feel fresher and may offer mild antibacterial support. Keep it as a short-term option rather than a daily habit.
3) Baking Soda (Emergency Use Only)
Baking soda can help neutralize odors and lift some surface staining. Use a very small amount and brush lightly. Scrubbing hard can wear enamel and irritate gums.
If you have sensitive teeth, gum recession, or known enamel wear, skip baking soda and stick to water brushing instead.

If You Can’t Brush Right Away
When you’re in transit or stuck without a toothbrush, rinsing is still better than nothing. Swish with water a few times to loosen food particles, especially after sugary or sticky snacks.
If you have it, alcohol-free mouthwash can reduce bacteria and freshen breath. It won’t replace brushing, but it can help until you’re able to clean properly.
What Not To Use On Your Teeth
Some popular “natural” hacks can damage enamel or irritate gums, especially if repeated. Avoid the following:
- Lemon juice or other citrus (acid softens enamel).
- Vinegar (highly acidic and harsh on enamel).
- Charcoal powders (often too abrasive and can scratch enamel).
- Salt scrubs or gritty mixtures (abrasive on enamel and gums).
- Hydrogen peroxide used frequently or undiluted (can irritate soft tissues).
Emergency solutions should be gentle, temporary, and low-risk. If something stings, burns, or feels gritty, don’t use it.
The 2-2-2 Rule, In Plain English
The “2-2-2 rule” is a simple reminder for everyday care:
- Brush twice a day.
- Brush for two minutes each time.
- Visit the dentist twice a year.
Forgetting toothpaste once doesn’t break the routine. Consistency over time matters far more than a single imperfect day.
How To Make A Very Basic Emergency Paste
If you want something paste-like, mix a tiny amount of baking soda with a few drops of water until it forms a thin paste. Use it gently and rinse thoroughly.
Skip oils, acids, and “DIY whitening” additives. This mix is only for one or two uses, then switch back to fluoride toothpaste as soon as you can.
Why Toothpaste Still Matters
Toothpaste typically contains fluoride or similar protective ingredients that strengthen enamel and help prevent cavities. Most emergency alternatives do not provide that long-term protection.
That’s why these substitutes are best viewed as short-term bridges. Once you have access to toothpaste again, return to your normal brushing and flossing routine.

A Simple Habit That Prevents This Next Time
If you travel often or tend to forget essentials, keep a travel-size toothpaste in your bag, car, or desk. A spare toothbrush or disposable toothbrush can help too.
Small systems beat willpower. When oral care is easy to do, you’re more likely to stay consistent.
When To Call A Dentist
If you notice persistent tooth pain, bleeding gums that don’t improve, swelling, or a bad taste that doesn’t go away, it’s worth getting checked. These symptoms can point to issues that brushing alone won’t solve.
If you’d like personalized guidance, the team at Lygos Dental can help you plan a routine that fits your needs and sensitivities.
Frequently Asked Questions (FAQs)
What can I use if I forgot my toothpaste?
Use water, a soft brush, or baking soda; floss and rinse afterward.
What to do if you forget your toothbrush and toothpaste?
Rinse vigorously, floss, and wipe teeth with a clean cloth until you can brush.
What to do if you forget your toothbrush and toothpaste?
Rinse vigorously, floss, and wipe teeth with a clean cloth until you can brush.
What is the 3 3 3 rule for brushing teeth?
It means brush three times daily, for three minutes, within three minutes after meals.
Can I just brush my teeth without toothpaste?
Yes, brushing with water still removes plaque, but fluoride toothpaste protects better.
How to make emergency toothpaste?
Mix baking soda with a few drops of water; optionally add a pinch of salt.
