Dental Treatments with CAD/CAM Technology
Dental Treatments With CAD/CAM Technology
CAD/CAM dentistry uses a digital scanner to capture your teeth, then designs and mills restorations such as crowns, veneers, inlays/onlays, and implant crowns with high precision. Many cases can be completed faster than traditional lab workflows, often with a more comfortable impression process and a highly natural look—depending on your bite, materials, and clinical needs.
Dentistry has moved quickly toward digital workflows, and CAD/CAM has become one of the most practical upgrades for both patients and clinics. Instead of taking a putty impression and waiting days for a lab, many restorations can be planned digitally and produced with tighter tolerances.
This guide explains what CAD/CAM technology is, where it is used in modern dentistry, and what to expect in terms of benefits, limitations, and pricing.
Table of Contents
What Is CAD/CAM Technology?
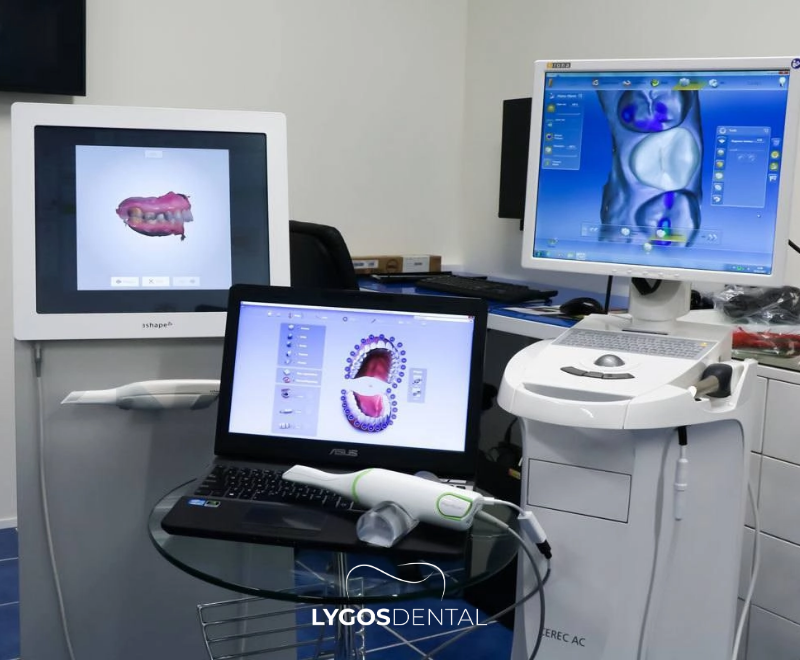
CAD/CAM stands for Computer‑Aided Design (CAD) and Computer‑Aided Manufacturing (CAM). In dentistry, it typically includes three steps:
- Digital scanning of teeth and gums with an intraoral scanner (or a scan of a physical model).
- Designing the restoration on a computer using specialized software.
- Manufacturing the piece by milling or 3D printing, then finishing and bonding or cementing it.
Common CAD/CAM materials include ceramics such as zirconia, lithium disilicate (e.g., E.max), and other high‑strength porcelain options.
Where CAD/CAM Is Used In Dentistry
CAD/CAM can support a wide range of restorative and aesthetic treatments. The most common applications include:
Crowns And Bridges: Single‑tooth crowns and multi‑unit bridges can be designed to match your bite and smile line more precisely.
Veneers (Laminates): Thin ceramic shells for front teeth can be digitally planned for shape, symmetry, and shade.
Inlays And Onlays: Custom restorations for larger cavities or fractured cusps when a standard filling is not ideal.
Implant‑Supported Restorations: Implant crowns, bridges, and full‑arch prostheses can be designed with careful attention to emergence profile and screw/cement access.
Orthodontic Appliances: Clear aligner workflows and some retainers can be planned digitally and produced with high consistency.
Key Advantages For Patients
- Faster turnaround: many cases can be delivered sooner, and some clinics offer same‑day options for selected restorations.
- High precision: digital scanning and manufacturing can reduce distortion and improve the fit of margins and contacts.
- More comfortable impressions: scanners can replace messy impression materials in most cases.
- Natural aesthetics: modern ceramics can closely mimic enamel translucency and color.
- Biocompatible materials: zirconia and other ceramics are widely used and well tolerated for many patients.
Your dentist may still recommend a conventional approach for certain situations, such as complex bite issues, extensive gum treatment needs, or when a lab‑crafted restoration is clinically preferable.
CAD/CAM Vs Traditional Dentistry
Both methods can produce excellent results. The difference is often the workflow and speed rather than the final goal.
| Feature | Traditional Method | CAD/CAM Method |
| Impressions | Putty/paste impressions (can trigger gag reflex) | Digital scan with an intraoral scanner (typically more comfortable) |
| Production Time | Often several days (lab turnaround) | Often faster; sometimes same‑day for selected cases |
| Accuracy | More steps where distortion can occur | Digital workflow can improve consistency and fit |
| Aesthetics | Depends on lab and materials | Digital planning + modern ceramics can improve predictability |
| Appointments | Commonly 2+ visits | Can be fewer visits depending on the case |
Who Is CAD/CAM Suitable For?
CAD/CAM is suitable for many people, but case selection matters. It is commonly recommended for patients who:
- Want a natural-looking, aesthetic restoration for visible teeth.
- Need a precise crown, veneer, inlay/onlay, or implant restoration.
- Prefer a shorter, more streamlined treatment process.
- Have had problems with impressions in the past (gag reflex, discomfort).
A clinical examination, X‑rays, and sometimes a digital bite analysis help your dentist decide whether a CAD/CAM restoration is the best option for your mouth and bite.
CAD/CAM Dental Treatment Prices In 2026

Pricing varies by material, case complexity, number of teeth, and the clinic’s equipment and lab setup. In Turkey, many clinics quote in EUR or USD for international patients, so exchange rates can affect the final cost.
Typical price drivers include:
- Material choice (zirconia, lithium disilicate, multilayer ceramics, etc.).
- Tooth preparation complexity and whether temporary restorations are needed.
- Number of units (single tooth vs multi‑unit bridge).
- Additional treatments (gum shaping, root canal treatment, bite adjustments).
- Clinic location and clinician experience.
Indicative per‑tooth price ranges in Turkey (2026):
| Procedure (Typical Example) | Approximate Range (TRY) |
| Zirconia Crown (per tooth) | ₺6,700 – ₺10,300 |
| Porcelain Veneer (per tooth) | ₺8,700 – ₺15,200 |
| Composite Veneer (per tooth) | ₺7,800 – ₺10,800 |
| E.max / Lithium Disilicate Veneer (per tooth) | ₺13,000 – ₺26,000 |
| Inlay (per tooth) | ₺5,900 – ₺17,800 |
| Onlay (per tooth) | ₺8,900 – ₺23,700 |
| Single Implant Package (implant + abutment + crown) | ₺17,400 – ₺34,700 |
These figures are broad estimates. A written treatment plan after examination is the only reliable way to confirm pricing for your specific case.
FAQ
What is CAD/CAM technology?
Computer-aided design and manufacturing create precise dental restorations from digital scans.
Types of CAD/CAM Systems in Dentistry
Systems include chairside, lab-based, and centralized milling/printing workflows with intraoral scanners.
Advantages and Disadvantages of CAD/CAM in Dentistry
Pros: speed, precision, consistency; cons: high cost, training needs, material and esthetic limits.
Is CAD/CAM technology safe?
Yes; it’s widely used and safe when clinicians follow proper scanning, design, and fabrication protocols.
What treatments can be performed with CAD/CAM?
It can make crowns, bridges, inlays/onlays, veneers, implant abutments, guides, and dentures.
Symptoms of Gum Inflammation (Gingivitis Symptoms)
Symptoms Of Gum Inflammation (Gingivitis Symptoms)
Gum inflammation (gingivitis) is an early stage of gum disease caused mainly by plaque buildup at the gumline. Common signs include red or swollen gums, bleeding when brushing or flossing, persistent bad breath, tenderness, and gum recession. With early dental care and consistent home hygiene, gingivitis is usually reversible.
Oral health plays a major role in overall wellbeing, and gum disease often starts quietly. Gingivitis can look minor at first, but it’s a clear signal that the gumline is under attack from bacteria. Spotting the signs early can help you avoid deeper infections that affect the bone and support around the teeth.
Table of Contents
What Is Gum Inflammation?
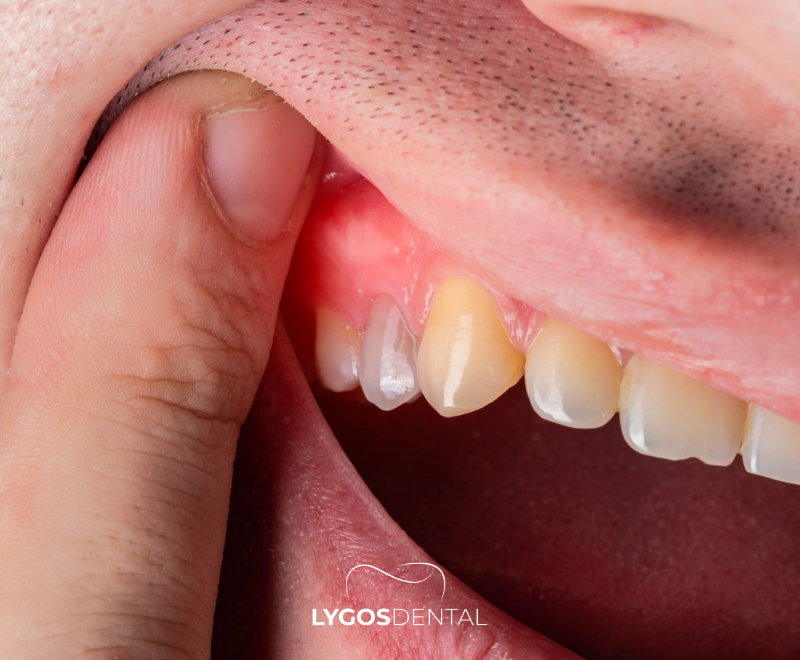
Gum inflammation is the irritation and swelling of the gum tissue. The medical term is gingivitis, and it most often develops when bacterial plaque isn’t removed effectively from the teeth and gumline. Over time, the gums react by becoming red, puffy, and prone to bleeding.
The good news is that gingivitis is typically reversible when addressed early with professional cleaning and improved daily care. When it’s ignored, it can progress to periodontitis, a more serious form of gum disease that may lead to bone loss and loose teeth.
Common Causes And Risk Factors
Plaque buildup is the main trigger, but several factors can raise the risk or make symptoms worse. Some are lifestyle-related, while others are linked to hormonal changes or health conditions. If you’re seeing symptoms repeatedly, it’s worth looking at both your routine and your medical background.
- Inconsistent brushing and flossing, or difficulty cleaning around crowns, bridges, braces, or implants
- Smoking or tobacco use
- Hormonal shifts (for example, pregnancy)
- Dry mouth, which reduces saliva’s natural cleansing effect
- Diabetes and other conditions that can affect immune response
- Certain medications that reduce saliva or irritate gum tissue
Most Common Gingivitis Symptoms
Gingivitis can vary from person to person, but the core signs are fairly consistent. Many people notice bleeding first, especially when brushing or flossing. If you have several of the symptoms below, a dental exam is the safest way to confirm what’s going on.
- Red, swollen, or shiny-looking gums (healthy gums are typically firm and pink)
- Bleeding when brushing, flossing, or biting into firm foods
- Bad breath that doesn’t improve with brushing and tongue cleaning
- Tenderness at the gumline or discomfort when chewing
- Gum recession (teeth may look longer)
- Increased sensitivity to hot, cold, or sweet foods
- A bad taste in the mouth
Does Gum Inflammation Cause Bad Breath?

Yes. When plaque and bacteria accumulate around the gumline, they release compounds that can cause persistent bad breath. If the odor returns quickly after brushing, or if it comes with bleeding or swollen gums, it’s often a sign that the problem is coming from the gums rather than the tongue alone.
Professional cleaning and treating the underlying gum inflammation usually makes a noticeable difference. If bad breath persists after treatment, your dentist may also check for cavities, dry mouth, tonsil stones, or other causes.
Does Gingivitis Cause Pain?
Gingivitis doesn’t always hurt, especially in the early stages. That’s one reason it can be easy to miss. Some people feel mild soreness or a “raw” sensation at the gumline, while others notice sensitivity when eating or drinking.
If you’re experiencing significant pain, throbbing, swelling that spreads, or a pimple-like bump on the gum, it may point to a deeper infection and should be assessed promptly.
What Can Happen If Gingivitis Is Left Untreated?
Untreated gingivitis can move beyond the surface gums and affect the supporting tissues around the teeth. At that point, home care alone usually isn’t enough. Early treatment is simpler, less invasive, and typically more affordable than advanced gum therapy.
- Periodontitis (infection that can damage the bone supporting the teeth)
- Gum recession and pockets around teeth that trap bacteria
- Loose teeth and, in advanced cases, tooth loss
- Gum abscesses or pus drainage
When Should You See A Dentist?
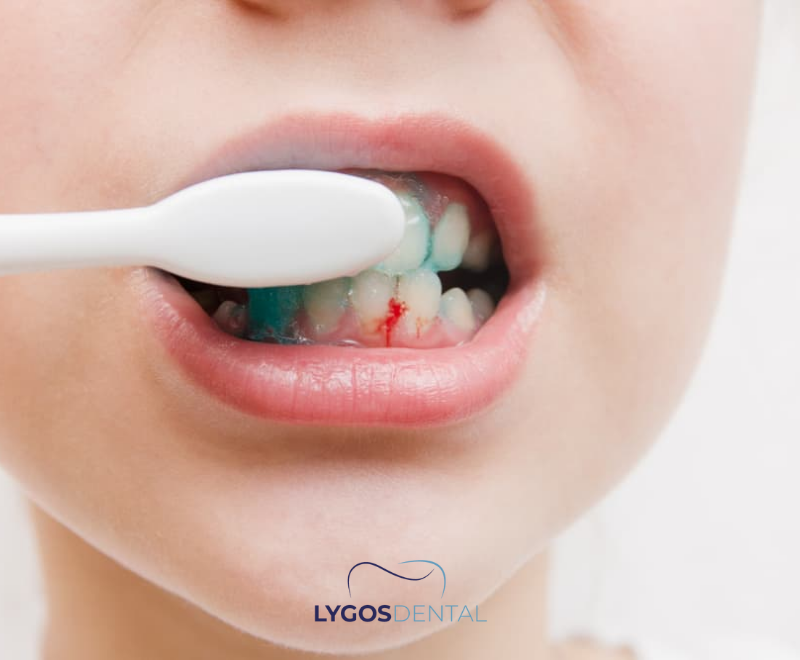
Book a dental checkup if you notice any of the following signs, especially if they last more than a week or keep coming back. A dentist can confirm whether it’s gingivitis, check for periodontitis, and recommend the right cleaning and home-care plan.
- Bleeding gums during brushing or flossing
- Redness, swelling, or tenderness at the gumline
- Bad breath or a bad taste that doesn’t go away
- Gum recession or teeth that look longer
- Sensitivity, discomfort when chewing, or teeth that feel loose
How To Reduce Gum Inflammation At Home
Home care can make a real difference, but it works best when combined with professional cleaning if plaque has hardened into tartar. Aim for gentle, consistent hygiene rather than aggressive brushing, which can irritate gums further.
- Brush twice daily for two minutes with a soft-bristled toothbrush
- Clean between teeth daily with floss or interdental brushes
- Pay special attention to the gumline and the back molars
- Replace your toothbrush head regularly, especially if bristles flare
- If you smoke, consider quitting support—tobacco is strongly linked to gum disease
Need Professional Support?
If you suspect gum inflammation or want a preventive checkup, contact our clinic to schedule an appointment. We can also advise on cosmetic dentistry, dental crowns, dental implants, and general dentistry services based on your needs.
FAQ
What is gum disease?
Gum disease is infection and inflammation of gums and supporting bone around teeth.
What is the most common symptom of gum disease?
Bleeding gums when brushing or flossing is the most common symptom.
How is gum disease treated?
Professional cleaning, improved home care, and sometimes antibiotics or gum surgery.
What happens if it is not treated?
It can cause recession, bone loss, loose teeth, abscesses, and tooth loss.
How long does it take for gum disease to heal?
Gingivitis can improve in 1–2 weeks; periodontitis needs ongoing care.
How Does a Vegan Diet Affect Dental Health?
How Does A Vegan Diet Affect Dental Health?
A well-planned vegan diet can support good dental health, but it may increase enamel wear or gum issues if it’s high in acids and sugars or low in calcium, vitamin D, and B12. With fortified foods, supplements when needed, and consistent oral hygiene, most vegans can maintain healthy teeth and gums.
Vegan eating patterns can be very tooth-friendly when they focus on whole foods, adequate minerals, and good oral routines. Problems usually come from frequent acidic drinks, sticky sugars, and nutrient gaps that affect enamel and gum tissues. The sections below cover the most common risks and the practical steps that help vegans keep their smile healthy.
Table of Contents
Does A Vegan Diet Harm Dental Health?
A vegan diet is not automatically harmful to teeth or gums. Oral health is shaped more by overall diet quality, snacking frequency, fluoride exposure, and daily hygiene than by the absence of animal foods alone.
That said, a poorly planned vegan diet can increase risk in a few predictable ways. Low calcium or vitamin D can affect the strength of teeth and supporting bone, while low vitamin B12 may be linked with mouth ulcers and gum issues. Highly processed vegan snacks and frequent fruit juices can also raise the mouth’s acid and sugar load.
How A Plant-Based Diet Influences Teeth

Acid Exposure And Enamel Erosion
Many plant-based staples are acidic or become acidic in the mouth, especially when eaten often. Citrus fruits, vinegar-based foods, wine, kombucha, and fruit juices can soften enamel over time. Starchy foods that linger on the teeth may also feed acid-producing bacteria, increasing cavity risk.
Saliva-Friendly Whole Foods
Whole, fibrous foods can work in your favor. Crunchy vegetables, nuts, and seeds stimulate saliva, which helps neutralize acids and wash away food particles. Water-rich foods and steady hydration support saliva flow, an important defense against both decay and bad breath.
Key Nutrients Vegans Should Watch For Oral Health
Calcium And Vitamin D
Calcium helps maintain strong teeth and jawbone, while vitamin D supports calcium absorption. Without dairy, vegans usually rely on a mix of naturally calcium-rich foods and fortified products.
Practical vegan sources include:
- Calcium-set tofu, fortified plant milks and yogurts
- Tahini (sesame), chia seeds, almonds
- Kale, broccoli, bok choy, and other leafy greens
- Vitamin D from sensible sun exposure, fortified foods, or supplements when needed
Vitamin B12 And Gum Health
Vitamin B12 is essential for healthy blood cells and nerve function, and it supports immune response in the mouth. Because B12 is limited in unfortified plant foods, deficiency is more common in strict vegans who do not use fortified foods or supplements.
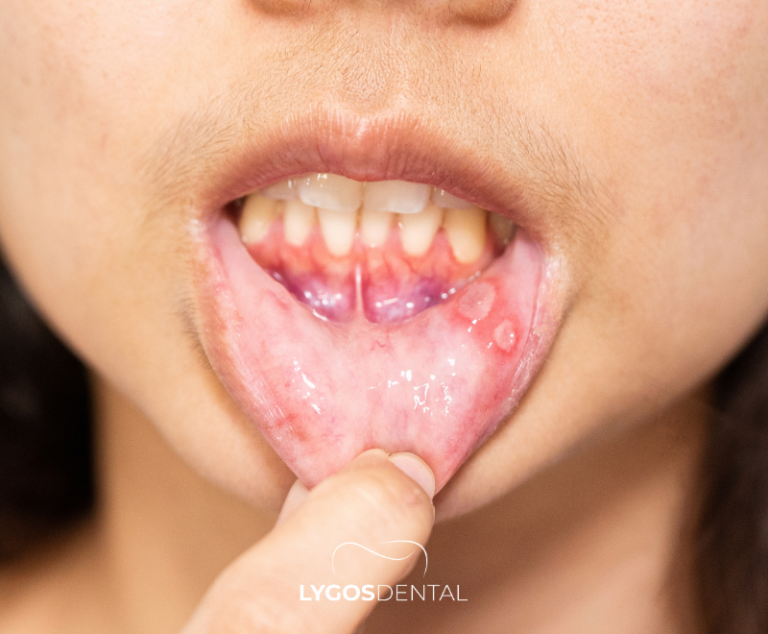
Low B12 has been associated with oral symptoms such as:
- Mouth ulcers or sore spots
- A burning or tingling sensation on the tongue
- Gum tenderness or easier bleeding
A reliable B12 supplement or regular intake of B12-fortified foods is the most consistent way to prevent deficiency.
Omega-3s And Inflammation
Omega-3 fats play a role in inflammation control, which matters for gum health. Plant foods mainly provide ALA from flax, chia, walnuts, and hemp, while DHA and EPA are available from algae-based supplements.
Iron And Zinc
Iron and zinc support immune function and tissue repair. If either is consistently low, some people notice more frequent mouth sores or slower healing after dental work.
Plant-based sources to prioritize:
- Lentils, beans, chickpeas, and pumpkin seeds
- Whole grains and oats
- Cashews and tahini
- Vitamin C–rich foods with meals to improve iron absorption
Daily Habits That Protect Vegan Smiles

- Limit frequent sipping on fruit juice, soda, kombucha, and other acidic drinks.
- After acidic foods or drinks, rinse with water and wait about 30 minutes before brushing.
- Brush twice daily with a fluoride toothpaste and clean between teeth every day (floss or interdental brushes).
- Choose snacks that are less sticky and less sugary; pair fruit with nuts or meals rather than grazing all day.
- Chew sugar-free gum after meals if you’re prone to dry mouth (it can boost saliva).
- Schedule routine dental check-ups and professional cleanings (often every six months, or as advised).
Are Vegan Toothpastes Effective?
Vegan toothpaste can be just as effective as conventional options when it contains proven anti-cavity ingredients. Many vegan formulas include fluoride, which strengthens enamel and reduces decay risk. Some are fluoride-free, so check the label and follow your dentist’s guidance if you’re choosing an alternative active ingredient.
When To See A Dentist
Book a dental visit sooner than your next routine check-up if you notice persistent bleeding gums, new sensitivity, mouth ulcers that do not heal, a burning tongue sensation, or ongoing dry mouth. These symptoms can have several causes, including nutrient deficiencies, irritation, or gum disease, and are worth evaluating early.
Book An Appointment
Contact us to learn more about cosmetic dentistry, dental crowns, dental implants, and general dentistry. We can help you choose an oral care plan that fits your diet and your goals.
FAQ
Vegan nutrition and dental health
Vegan diets can support dental health with adequate calcium, vitamin D, B12, and hygiene.
Does vegetarian nutrition cause tooth decay?
No; decay is caused by sugars, acids, and plaque, not vegetarianism.
Dental problems in vegetarians
Vegetarians may have erosion or cavities if diets are acidic or sugary.
Are vegetarians’ teeth healthier?
Not automatically; oral health depends on hygiene, fluoride, and sugar frequency.
Why Does Tartar Form?
Why Does Tartar Form?
Tartar (also called dental calculus) forms when plaque is left on teeth long enough to harden. Minerals in saliva “set” the sticky film into a rough deposit—often near the gumline and between teeth. Good brushing, daily flossing, and regular professional cleanings stop plaque before it turns into tartar and irritates gums.
Table of Contents
What Tartar Is
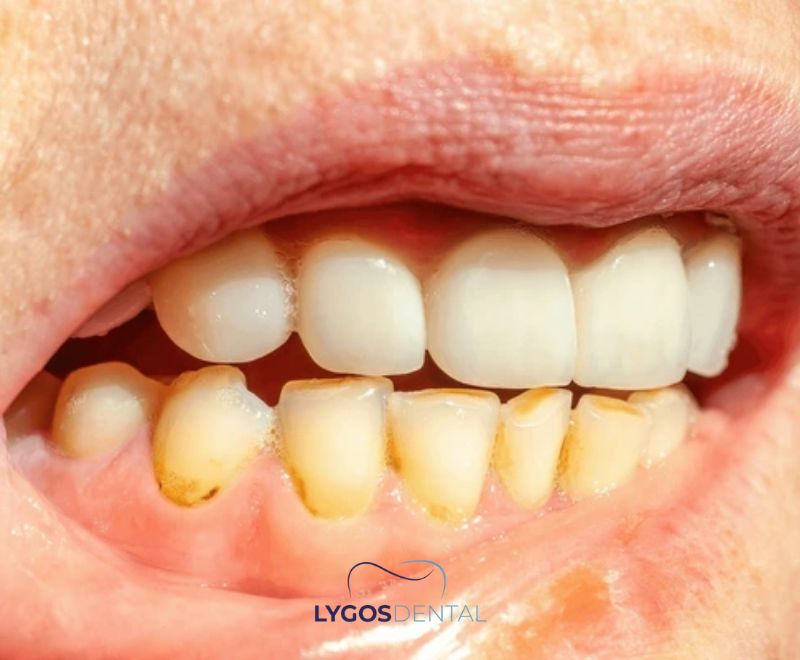
Plaque is a soft, sticky layer of bacteria and food particles that forms on teeth every day. When plaque isn’t removed thoroughly, it can mineralise and become tartar. Unlike plaque, tartar bonds to the tooth surface and creates a rough area where new plaque sticks more easily.
Tartar tends to build up most around the gumline, behind the lower front teeth, and on the outer surfaces of upper back teeth. Over time it can contribute to gum inflammation, persistent bad breath, and a higher risk of cavities.
Why Tartar Forms
Plaque Left On Teeth
The most common reason is missed plaque during daily cleaning. If brushing is rushed or irregular, plaque remains along the gumline and between teeth. As it hardens, it becomes tartar that can’t be removed with a toothbrush.
Saliva Minerals And Dry Mouth
Saliva naturally contains minerals such as calcium and phosphate. People with higher mineral content in their saliva may develop tartar more quickly. Dry mouth (from dehydration, some medications, or mouth breathing) reduces saliva’s cleansing effect and can speed up buildup.
Smoking And Tobacco Use
Smoking and other tobacco use can increase plaque and stain deposits. It also irritates gum tissue and can mask early gum disease by reducing visible bleeding. That combination often leads to heavier tartar accumulation over time.
Diet High In Sugar And Starch
Sugary and starchy foods feed plaque-forming bacteria, especially when snacking is frequent. Sticky foods and sweet drinks can linger on tooth surfaces and between teeth. The longer plaque sits, the more likely it is to harden into tartar.
Skipping Interdental Cleaning
A toothbrush can’t fully reach the tight spaces between teeth. When floss or interdental brushes aren’t used, plaque builds up in these areas and near the gumline. This is why many people notice tartar first between teeth and behind the lower front teeth.
Signs You May Have Tartar
Tartar can look different depending on where it sits and how long it has been there. Common signs include:
- Yellow, tan, or brown deposits on teeth (often near the gums)
- A rough feeling on the tooth surface that doesn’t brush away
- Bad breath that keeps coming back
- Bleeding or tender gums when brushing or flossing
- Red, swollen gums or gum recession
- Increased tooth sensitivity or more frequent cavities
Habits That Speed Up Tartar Buildup

Small routine choices can make a big difference. These habits commonly increase plaque retention and tartar formation:
- Brushing less than twice a day, or brushing for too short a time
- Skipping floss or interdental brushes
- Not cleaning the gumline gently but thoroughly
- Frequent late-night snacking without brushing afterwards
- Regular smoking or vaping with nicotine products
- High intake of sugary drinks, sweet snacks, or refined carbohydrates
How Dentists Remove Tartar
Once plaque becomes tartar, home care can’t lift it off. A dentist or dental hygienist removes it using professional instruments, often with ultrasonic scaling. Teeth are then polished to smooth the surface and make plaque less likely to stick.
If tartar extends below the gumline or there are signs of gum disease, you may need a deeper cleaning (sometimes called periodontal scaling and root planing). Your dentist will recommend the right approach based on your gum health.
Many people do well with a professional cleaning every 6–12 months. If you build tartar quickly or have gum disease risk factors, your dentist may advise more frequent visits.
How To Prevent Tartar From Coming Back
Prevention comes down to stopping plaque before it hardens. A simple routine works best when it’s consistent:
- Brush twice daily for two minutes with a fluoride toothpaste, paying special attention to the gumline.
- Floss once a day or use interdental brushes if you have wider spaces, bridges, or braces.
- Consider an electric toothbrush if you struggle with technique or plaque control.
- Rinse with water after meals and stay well hydrated to support healthy saliva flow.
- Limit frequent sugary snacks and drinks; keep sweet foods to mealtimes when possible.
- Schedule regular dental check-ups and cleanings so tartar is removed early.
When To See A Dentist
Book an appointment if you notice bleeding gums, persistent bad breath, gum swelling, tooth looseness, or pain when chewing. These can be signs of gingivitis or more advanced gum disease, which needs professional care. Early treatment is usually simpler and helps protect the bone supporting your teeth.
FAQ
How can you prevent tartar buildup?
Brush with fluoride twice daily, clean between teeth daily, and get regular professional cleanings.
What is the main cause of tartar?
Tartar forms when plaque isn’t removed and mineralizes from saliva.
Is it okay to scrape tartar off your teeth?
No; DIY scraping can damage enamel and gums and worsen infection risk.
What happens if tartar is not cleaned?
It can cause gum disease, bad breath, recession, bone loss, and tooth loss.
Will teeth fall out if tartar is cleaned?
No; cleaning doesn’t loosen healthy teeth, but it can reveal existing periodontal looseness.
Splint Prices for Teeth Grinding (Bruxism)
Splint Prices For Teeth Grinding (Bruxism) In Turkey
Splints (night guards) are custom dental appliances that protect teeth and jaw joints from grinding. In Turkey, prices usually depend on the splint type, materials, and lab work. Most patients pay within typical clinic ranges for soft, hard, or hybrid designs, with extra fees possible for consultation, scans, and follow‑up adjustments.
Splints (night guards) are custom dental appliances that protect teeth and jaw joints from grinding. In Turkey, prices usually depend on the splint type, materials, and lab work. Most patients pay within typical clinic ranges for soft, hard, or hybrid designs, with extra fees possible for consultation, scans, and follow‑up adjustments.
Table of Contents
What Is Teeth Grinding (Bruxism)?

Bruxism is involuntary clenching or grinding of the teeth. It most often happens during sleep, but some people also clench during the day when stressed or concentrating. Over time, untreated bruxism can wear down enamel, strain jaw muscles, and irritate the temporomandibular joint (TMJ).
Common Symptoms
Bruxism can be subtle, especially if it happens at night. Signs dentists commonly see include:
- Jaw or facial muscle pain, especially in the morning
- Headaches (often around the temples)
- Flattened, chipped, or worn tooth surfaces
- Tooth sensitivity or cracked enamel
- Ear pain without an ear infection
- Grinding noises noticed by a partner
If these symptoms sound familiar, a dental exam can confirm wear patterns and rule out other causes. Your dentist may also ask about sleep quality, stress, and any jaw clicking or locking.
What Is A Splint And How Does It Help?
A splint (often called a night guard) is a clear appliance fitted to your teeth. It creates a protective barrier so your teeth do not grind directly against each other. It can also help reduce muscle overload and protect the TMJ by stabilizing the bite during sleep.
A properly fitted splint can help with:
- Reducing tooth wear and preventing fractures
- Lowering jaw muscle fatigue and morning tightness
- Protecting dental work such as crowns or veneers
- Supporting TMJ comfort in patients who clench
Types Of Splints Used For Bruxism

Dentists recommend different designs depending on the severity of grinding, your bite, and jaw symptoms. The three most common options are soft, hard, and hybrid splints.
Soft Splints
Soft splints are flexible and often used for mild to moderate clenching or grinding. They can feel more comfortable at first, but they may wear out faster in heavy grinders.
Hard Splints
Hard splints are made from more rigid materials and are usually recommended for moderate to severe bruxism. They are durable and typically provide more stable bite guidance, which can be helpful for TMJ protection.
Hybrid Splints
Hybrid designs combine a softer inner surface with a harder outer shell. They aim to balance comfort with durability, especially for patients with sensitive jaws or strong bite forces.
Splint Prices In Turkey (2026)
Clinics set fees based on materials, lab work, and the appointment plan. The ranges below reflect common private-clinic pricing and can vary by city, dentist expertise, and technology used.
| Splint Type | Typical Price Range (TL) |
| Soft splint | 1,500 – 2,500 |
| Hard splint | 2,500 – 4,000 |
| Hybrid splint | 3,000 – 4,500 |
These ranges may or may not include the exam, impressions or digital scan, fitting, and follow‑up adjustments. If you have private insurance, ask whether dental splints are covered and what documentation is required.
What Affects The Total Cost?
A price quote can differ from one clinic to another even for the same splint type. The biggest factors usually include:
- Dentist experience and clinic location (major cities and central locations often cost more)
- Splint material and design (hard and hybrid options tend to be higher priced)
- Laboratory workflow (precision impressions, CAD/CAM production, and quality control)
- Number of visits and adjustments included in the package
- Extra services when clinically needed (e.g., TMJ assessment, physiotherapy referral)
How To Choose The Right Splint

The best splint is the one that fits accurately and matches your diagnosis. Over‑the‑counter guards may look cheaper, but they can fit poorly and may worsen bite or jaw symptoms. A dentist‑made splint is designed from your bite records and can be adjusted if it feels too tight or changes your bite.
When comparing clinics, ask:
- Is the price for a custom, lab‑made splint or a chairside/standard guard?
- Does the quote include follow‑up adjustments?
- What is the expected lifespan for my grinding intensity?
- What should I do if the splint feels uncomfortable or changes my bite?
How Long Does A Splint Last?
Lifespan depends on how strongly you grind, the splint material, and daily care. Many patients replace a splint every 1 to 3 years. Regular checkups help catch cracks, thinning areas, and bite changes early.
FAQ
What is a splint for teeth grinding (bruxism)?
A bruxism splint is a custom nightguard that protects teeth and relaxes jaw muscles.
How much does a splint for bruxism cost?
$200–$800 for a custom dentist-made splint; store-bought guards cost less.
Are dental splints expensive?
Yes; custom splints can feel expensive, but they’re cheaper than repairing tooth damage.
How long is a splint used?
Months to years, worn nightly, depending on ongoing grinding and symptoms.
Does wearing a splint cause pain?
Usually not; mild pressure or soreness may occur initially, then settles quickly.
The Harms of Using a Hard Toothbrush
The Harms Of Using A Hard Toothbrush
Hard toothbrushes can look like they clean better, but stiff bristles combined with heavy pressure often do more harm than good. They can wear down enamel at the gumline, irritate and injure gum tissue, and increase tooth sensitivity over time. For most people, a soft-bristled brush used gently is the safer everyday option.
Oral hygiene supports overall health, but the tools you choose matter as much as how often you brush. Hard-bristled toothbrushes are designed for specific situations, yet many people use them daily because they feel “stronger.” When a hard brush is paired with forceful brushing or an abrasive toothpaste, it can slowly damage teeth and gums.
Table of Contents
What Is A Hard Toothbrush And When Is It Used?

A hard toothbrush has dense, stiff bristles that do not flex easily. Dentists may recommend one for targeted, short-term tasks, such as cleaning certain prosthetic surfaces, orthodontic appliances, or areas where plaque control is difficult. It is not a default choice for routine daily brushing for most natural teeth and gums.
The common belief that “harder cleans better” is misleading. Plaque removal depends more on technique, time, and reaching the gumline gently than on bristle stiffness.
Can A Hard Toothbrush Damage Tooth Enamel?
Yes, it can contribute to tooth surface wear, especially near the gumline where enamel is thinner and root surfaces may be exposed. With repeated heavy pressure, stiff bristles can increase abrasion and lead to non-cavity wear (sometimes seen as notches at the neck of the tooth). Because enamel does not grow back, this kind of wear is cumulative.
As enamel thins, teeth may look more yellow, feel sensitive to cold or heat, and become more prone to chipping at weakened areas. If the wear reaches dentin, sensitivity often increases and restorative treatment may be needed.
Can Hard Bristles Cause Gum Recession?

Gum tissue is delicate, and repeated scrubbing with stiff bristles can cause irritation, small abrasions, and gradual recession. Recession exposes the tooth root, which is softer than enamel and more vulnerable to wear and sensitivity. It can also make teeth look longer and create spaces that trap plaque.
Gum recession has many causes, including genetics, inflammation from gum disease, and poor brushing technique. A hard toothbrush can speed up the process when brushing is aggressive.
Other Problems Linked To Hard Toothbrush Use
- Mouth irritation: repeated trauma to the cheeks, tongue, or palate can trigger soreness or ulcers.
- Gum bleeding from abrasions: bleeding is not “normal” if it is caused by mechanical injury.
- Worsening sensitivity: exposed root surfaces react strongly to cold, sweets, and acidic foods.
- Cosmetic changes: wear at the gumline can alter tooth shape and create uneven edges over time.
If you notice rough gumline notches, persistent sensitivity, or bleeding right after brushing, your brush and technique should be reassessed. These signs are often easier to address early than after significant tissue loss.
Long-Term Damage From Using A Hard Toothbrush

Short-term discomfort can be easy to ignore, but long-term brushing trauma may lead to chronic sensitivity and progressive gum recession. As roots become exposed, they are more likely to wear down and develop decay. In advanced cases, restoring function and aesthetics can require fillings, gum grafting, or other periodontal treatment.
How To Choose A Toothbrush And Brush Safely
For most adults and children, dentists commonly advise a soft-bristled toothbrush for daily use. Medium bristles may be suitable for some people with good technique, but hard bristles increase the risk of abrasion when pressure is high.
Toothbrush Checklist
- Bristles: soft (or extra-soft if you have sensitivity or recession).
- Head size: small to medium so it can reach behind molars comfortably.
- Bristle tips: end-rounded filaments are gentler on gums.
- Handle: comfortable grip so you are less likely to “scrub.”
- Replacement: replace the brush every 3–4 months, or sooner if bristles fray.
Brushing Technique Tips
- Use light pressure. If the bristles bend dramatically, you are pressing too hard.
- Angle the brush about 45 degrees toward the gumline and use small, controlled motions.
- Brush for two minutes and avoid sawing back and forth across the gumline.
- If you use an electric brush, let it do the work—don’t add extra pressure.
Who Should Use A Hard Toothbrush?
A hard toothbrush may be appropriate only when a dentist recommends it for a specific reason, and typically for limited use. If you have gum recession, enamel wear, sensitivity, or a history of abrasion, a hard brush is rarely the best choice. When in doubt, ask your dentist or hygienist to demonstrate the right brush and technique for your mouth.
Book An Appointment
If you have sensitivity, gum recession, or signs of brushing abrasion, a dental exam can identify the cause and the best next step. Contact us to learn more about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry, or to schedule an appointment.
FAQ
Is it better to brush hard or soft?
Soft brushing is better; use gentle pressure to clean without damaging gums.
Is brushing your teeth too hard harmful?
Yes, brushing too hard can wear enamel and irritate gums, causing recession.
Which toothbrush is the healthiest to use?
A soft-bristled, small-head toothbrush (manual or electric) is healthiest for most people.
Which toothbrush do dentists recommend most?
Dentists most often recommend soft-bristled brushes; oscillating-rotating electric models can be very effective.
Is brushing hard harmful to gum recession?
Yes, hard brushing worsens gum recession by traumatizing gum tissue and abrading roots.
How to Choose a Dental Clinic?
How To Choose A Dental Clinic
Choose a dental clinic by checking the dentist’s credentials, the clinic’s sterilization standards, and the range of treatments offered. Confirm pricing is transparent, modern diagnostic tools are available, and the location is practical for follow‑up visits. A short visit or consultation helps you assess cleanliness, communication, and whether the team can handle your needs in one place.
Oral health affects comfort, confidence, and long‑term wellbeing—so picking the right clinic matters. While cleanliness and location are part of the decision, they’re rarely enough on their own.
Use the checks below to compare clinics in a practical, patient-first way and avoid surprises once treatment starts.
Check The Dental Team And Specialties
Dentistry includes several sub‑specialties, and the right expertise can change both the outcome and the experience. Look for a clinic that can provide the services you may need—such as orthodontics, periodontics (gum care), pediatric dentistry, endodontics (root canals), oral surgery, and cosmetic dentistry—without constantly referring you elsewhere.
When a clinic has multiple dentists with clear focus areas, complex cases can be planned together. That team approach often means faster diagnosis, smoother treatment planning, and better continuity of care.
Look For Clear Sterilization And Infection‑Control Standards

Because dental care involves close contact and instruments used in the mouth, infection control should be visible and consistent. A trustworthy clinic will be open about how instruments are cleaned, packaged, and sterilized between patients.
Pay attention to practical signals: single‑use items where appropriate, sealed sterilization pouches, staff wearing gloves and masks, and a tidy clinical area. Clean restrooms, an organized waiting area, and a well‑maintained reception space usually reflect the same standards in treatment rooms.
Review The Treatment Range And Referral Process
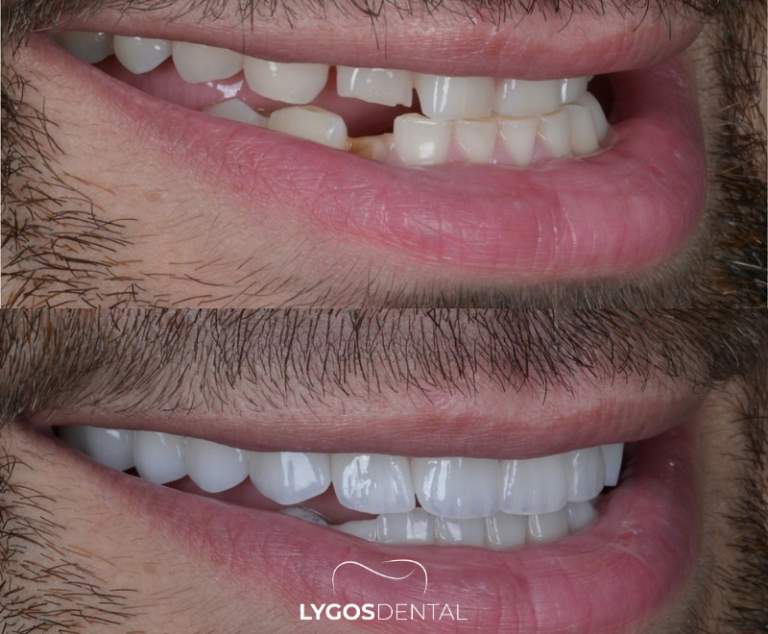
A good way to gauge a clinic’s scope is to review the treatments it provides and how it handles referrals. Some clinics focus on routine care, while others also offer implants, orthodontics, pediatric care, laser dentistry, and smile-design services.
If you expect longer-term treatment (for example, orthodontics or implant planning), ask whether everything can be done in-house. When referrals are needed, the clinic should explain why, share options, and coordinate your records so you’re not starting from scratch elsewhere.
Consider Location, Accessibility, And Follow‑Up Visits
Many dental treatments require more than one appointment. A clinic that is easy to reach can make follow‑ups far less stressful—especially when you have a tight schedule or you’re dealing with discomfort.
Check public transport access, parking options, and how quickly you could get there in an urgent situation. Also consider appointment availability, evening or weekend hours, and how the clinic handles unexpected problems after a procedure.
Compare Pricing With Transparency, Not Just The Lowest Fee
Price matters, but the lowest quote isn’t always the best value. Fees can reflect the dentist’s experience, materials used, the lab work involved, and the technology required for accurate planning.
Look for clear, written estimates before treatment begins and ask what is included. A reputable clinic explains potential add‑on costs, warranty terms (where relevant), and payment options such as insurance coverage or installments.
Ask About Technology, Imaging, And Materials
Modern equipment can improve comfort and accuracy. Digital X‑rays, panoramic imaging, 3D scans, and digital impressions can speed up diagnostics and reduce guesswork in treatment planning.
Technology alone isn’t the goal—the goal is safer, more predictable care. Ask how imaging is used in your case, whether the clinic follows up-to-date protocols, and what brands or material standards are used for restorations like crowns or implants.
Questions To Ask Before You Book
- Which dentist will be responsible for my treatment, and what is their experience with cases like mine?
- How do you sterilize instruments, and do you use single‑use items where appropriate?
- What diagnostic imaging will you use, and will I receive a copy of my records if needed?
- Can you provide a written treatment plan with an itemized estimate?
- Who should I contact if I have pain or complications after hours?
- Do you offer alternatives if a treatment option isn’t suitable for me?
Make An Appointment Or Request Information
If you’re considering cosmetic dentistry, dental crowns, dental implants, or general dentistry, reach out to the clinic to ask about suitability, timelines, and fees. A short consultation is often the quickest way to confirm whether the team and facilities match your expectations.
How To Choose A Dental Clinic: Frequently Asked Questions
What is the most important factor when choosing a dental clinic?
Start with the dentist’s qualifications and experience in the treatment you need. Strong infection control, clear communication, and reliable diagnostics should support that expertise.
How can you assess the hygiene of a dental clinic?
Visit the clinic if you can. Look for clean, organized treatment areas, properly packaged instruments, and staff using protective equipment. A clinic should be comfortable explaining its sterilization process.
Why is a dental clinic’s technological infrastructure important?
Technology can make diagnosis more accurate and treatment more comfortable. Digital imaging and modern impression systems can improve planning for procedures such as orthodontics, crowns, and implants.
Are high-quality dental clinics always expensive?
Not always. High fees don’t guarantee quality, and very low fees can lead to compromises or extra costs later. What matters is transparent pricing that matches the materials, skill, and scope of care provided.
Can a single clinic handle all types of dental treatments?
Many clinics can manage routine care and advanced treatments under one roof, especially when they have multiple specialists. If something must be referred out, you should expect clear explanations and good coordination.
Confidence Issues After Tooth Loss
Confidence Issues After Tooth Loss
Tooth loss can make people feel self‑conscious about smiling, speaking, and being seen, which may lead to avoidance and social anxiety. Confidence often improves when the cause is addressed—through a dental plan that restores function and appearance, plus emotional support if needed. With the right steps, most people return to normal social and professional life.
Psychological Impact Of Tooth Loss
Missing teeth can change how you see yourself. People often report embarrassment, shame, or a sense of loss because their smile no longer matches their identity. If front teeth are involved, everyday moments—laughing, talking, even ordering coffee—can start to feel stressful.
For some, tooth loss also brings worries about aging or health, especially when it happens earlier than expected. Those thoughts can spiral into low mood, withdrawal, or reluctance to meet new people. If these feelings persist or interfere with daily life, professional support can help.
Signs Your Confidence Is Taking A Hit

Confidence changes look different for everyone, but these patterns are common after losing teeth:
- Avoiding smiling, laughing, or speaking in public
- Covering your mouth with your hand, phone, or other objects
- Keeping conversations short or staying quiet in groups
- Skipping photos, video calls, or social events
- Feeling unhappy with your appearance when you look in the mirror
- Avoiding situations that involve scrutiny, such as interviews, presentations, or dating
If you recognize several of these signs, it may help to name the problem clearly: you are reacting to a real change in comfort, function, and appearance. That means there are practical solutions.
How Missing Teeth Can Trigger Social Anxiety
Tooth loss is not only cosmetic. It can affect speech clarity, chewing, and breath, which may increase self‑monitoring during conversations. Many people become preoccupied with the idea that others are staring or judging, even when that isn’t happening.
This type of anxiety can show up at work, in close relationships, and in new social settings. Over time, avoidance can shrink your social circle and reinforce the fear. Addressing both the dental cause and the emotional response tends to work best.
Practical Ways To Cope And Rebuild Confidence

Reframe The Situation
Try to treat tooth loss as a health issue with options, not a personal failure. Reframing reduces shame and makes it easier to take action. A plan, even a simple one, often brings immediate relief.
Get Dental Advice Early
A dentist can explain what caused the tooth loss and what can be done next. Early advice helps prevent shifting teeth, bite changes, and further complications. It also replaces uncertainty with clear choices and timelines.
Support Your Mental Health
If your self‑esteem has dropped sharply, speaking with a therapist can help you challenge harsh self‑talk and reduce avoidance behaviors. Simple strategies—breathing techniques, exposure steps, and confidence scripts for conversations—can make social situations feel manageable again.
Stay Social While You Heal
It’s tempting to disappear until everything is “fixed,” but isolation usually makes anxiety worse. Choose low‑pressure meetups with trusted people first, then build up from there. Small wins matter.
Build Confidence Habits
Posture, eye contact, and steady speech can signal confidence even when you feel unsure. Some people also find it helpful to focus on fitness, hobbies, or skills that reinforce a positive self‑image. The goal is to keep your sense of identity bigger than your smile.
Treatment Options That Can Restore Function And Appearance
Modern dentistry offers several ways to replace missing teeth. The right option depends on the number of missing teeth, gum health, jawbone support, budget, and personal preferences.
Dental Implants
Implants replace the tooth root and are designed to feel stable during eating and speaking. They can be used for single teeth, multiple teeth, or full‑arch restorations, depending on your case. Your dentist will check bone levels and overall health to confirm suitability.
Bridges
A bridge fills the gap by anchoring to neighboring teeth or implants. It can be a strong choice when adjacent teeth already need crowns, or when implants aren’t suitable. Good hygiene is important to protect the supporting teeth and gums.
Dentures
Removable dentures can replace several teeth or a full arch and are often a cost‑effective solution. Fit and comfort vary, and adjustments may be needed as your mouth changes. Some people choose implant‑supported dentures for extra stability.
Zirconia Crowns And Aesthetic Restorations
For visible areas, zirconia and other modern materials can create natural‑looking results. These restorations may be part of a broader plan that includes implants or bridges. A shade match and bite check are key to a comfortable, lifelike outcome.
Oral Health Habits That Help Prevent Future Tooth Loss

Preventing further problems protects both your health and your confidence. These habits make a measurable difference:
- Brush twice a day with fluoride toothpaste and use an interdental brush or floss daily
- Attend routine dental checkups and cleanings (your dentist will advise the best schedule for you)
- Treat gum bleeding early; it can be an early sign of gum disease
- Limit frequent sugary or acidic snacks and drinks
- Avoid tobacco and moderate alcohol use
- Use a mouthguard for contact sports and ask about a night guard if you grind your teeth
When To Seek Professional Support
Consider extra support if you avoid work, dating, or social situations because of your teeth, or if you notice ongoing low mood, sleep changes, or persistent worry. A dentist can handle the functional side, while a mental health professional can help with social anxiety and self‑image. Many people benefit from addressing both at the same time.
Frequently Asked Questions
Does tooth loss really affect confidence?
Yes. Changes in appearance, speech, and chewing can make people feel exposed or judged. That can lead to avoiding smiles, photos, and conversations, which reinforces low confidence.
How can I cope with confidence loss after losing teeth?
Start with a dental assessment so you understand your options. Then focus on small, consistent steps: stay socially connected, practice calm breathing in stressful moments, and consider counseling if anxiety or shame is taking over.
Will my confidence return after dental treatment?
For most people, confidence improves once function and appearance are restored. Feeling comfortable speaking and smiling again often reduces self‑consciousness quickly, especially when paired with supportive habits.
How do missing teeth affect social and professional life?
People may hold back in meetings, avoid interviews, or feel hesitant when meeting someone new. Restoring your bite and addressing anxiety early helps prevent those patterns from becoming long‑term.
How to Clean Tongue Coating?
How to Clean Tongue Coating?
Tongue coating is a layer of bacteria, dead cells, and debris trapped between the tongue’s tiny bumps. To clean it, brush or gently scrape from the back of your tongue toward the tip once a day, then rinse well. Stay hydrated and address dry mouth or smoking. If it lasts more than a few weeks or hurts, get checked.
What Tongue Coating Is
Tongue coating (sometimes called a “white tongue” or “coated tongue”) is a visible layer that can look white, yellow, or light brown. It forms when bacteria, dead cells, and food particles build up on the tongue’s surface, especially toward the back. It’s common and often improves with routine oral hygiene.
Why Tongue Coating Forms

The tongue has papillae—small bumps that can trap debris. When saliva flow is low or cleaning is inconsistent, that debris sticks around and thickens into a coating. Lifestyle factors and certain health issues can also play a role.
- Not cleaning the tongue regularly as part of oral hygiene
- Dry mouth (dehydration, mouth breathing, some medications, or reduced saliva)
- Smoking or tobacco use
- Alcohol use, which can worsen dryness
- Irritation from very hot foods or a recent illness
- Oral thrush (a yeast infection) and other infections in some cases
- Digestive symptoms such as reflux may be associated for some people
Common Symptoms
- A white, yellow, or brown film on the tongue
- Bad breath (halitosis)
- A fuzzy or rough tongue texture
- A lingering unpleasant taste or reduced taste
- Dry mouth, especially on waking
Why It Matters
A mild coating is usually harmless, but it can contribute to bad breath and make your mouth feel less fresh. A persistent, painful, or worsening coating can sometimes point to an underlying issue such as dry mouth, infection, or irritation that needs targeted treatment.
Natural Ways To Remove Tongue Coating

1) Use A Tongue Scraper Or Soft Brush
Mechanical cleaning is the most direct method. A tongue scraper is designed to lift buildup efficiently, but a soft toothbrush works well for many people too.
- Brush your teeth first, then stick out your tongue.
- Place the scraper (or brush) gently toward the back of the tongue, without forcing it.
- Pull forward toward the tip with light pressure. Repeat 3–5 passes.
- Rinse the scraper/brush between passes, then rinse your mouth with water.
- Clean the tool with soap and water and let it dry.
2) Rinse With Salt Water
A warm salt-water rinse can help reduce bacteria and loosen debris. Mix about ½ teaspoon of salt in a cup of warm water, swish for 20–30 seconds, then spit. Use once daily if it feels helpful.
3) Baking Soda A Few Times Per Week
Baking soda can help neutralize acids and reduce odor-causing compounds. You can choose a toothpaste that contains baking soda, or make a thin paste with water and gently brush the tongue 2–3 times per week. If your tongue feels irritated, stop and switch back to water only.
4) Support A Healthier Oral Environment
- Drink enough water through the day to support saliva production.
- If you wake up with a coated tongue, try managing dry mouth (humidifier at night, nasal breathing, sugar-free gum).
- Consider yogurt with live cultures if you tolerate dairy, as part of a balanced diet.
- Cut back on smoking or tobacco, which commonly worsens tongue coating.
Tips For Safe Tongue Cleaning

- Be gentle. Scraping too hard can irritate the tongue and make the problem worse.
- Clean once per day for most people. More isn’t always better.
- Avoid sharp-edged tools or aggressive brushing, especially if you have sores or a sensitive gag reflex.
- Rinse your mouth afterward to wash away loosened debris.
- Keep up the basics: brush twice daily, floss, and replace toothbrush heads regularly.
When To See A Dentist Or Doctor
Book a checkup if the coating doesn’t improve with good hygiene, if it lasts longer than a few weeks, or if you have pain. Seek prompt care for symptoms such as sores that don’t heal, bleeding, fever, trouble swallowing, or swelling that affects breathing.
Frequently Asked Questions
Why Is Tongue Coating More Noticeable In The Morning?
Saliva flow drops while you sleep, and the mouth can dry out. With less saliva to wash away bacteria and debris, a coating may be more visible when you wake up.
Is Tongue Coating Only Caused By Poor Oral Hygiene?
No. Oral hygiene is a common factor, but dry mouth, smoking, recent illness, irritation, and infections like oral thrush can also contribute. That’s why persistent or painful changes are worth checking.
What Happens If You Don’t Clean Tongue Coating?
Many cases stay mild, but the buildup can worsen bad breath and taste changes. If an underlying issue is driving it, ignoring it may delay the right treatment.
What Products Work Best?
A tongue scraper or a soft toothbrush is usually enough. If you use mouthwash, choose alcohol-free options if you’re prone to dryness. For suspected infections, a clinician may recommend specific treatment.
Chronic Periodontitis
Chronic Periodontitis
Chronic periodontitis is a long-term gum infection caused mainly by plaque and tartar buildup. It can quietly inflame the gums, deepen pockets around teeth, and gradually weaken the bone that holds teeth in place. With early diagnosis, professional cleaning, and consistent home care, progression can be slowed or stopped and tooth loss can often be prevented.
Gum disease often starts with mild symptoms, so it can be easy to ignore. Chronic periodontitis is one of the most common forms and may progress for months or years before pain appears. Untreated disease can lead to loose teeth, tooth loss, and ongoing inflammation that affects overall health.
What Is Chronic Periodontitis?
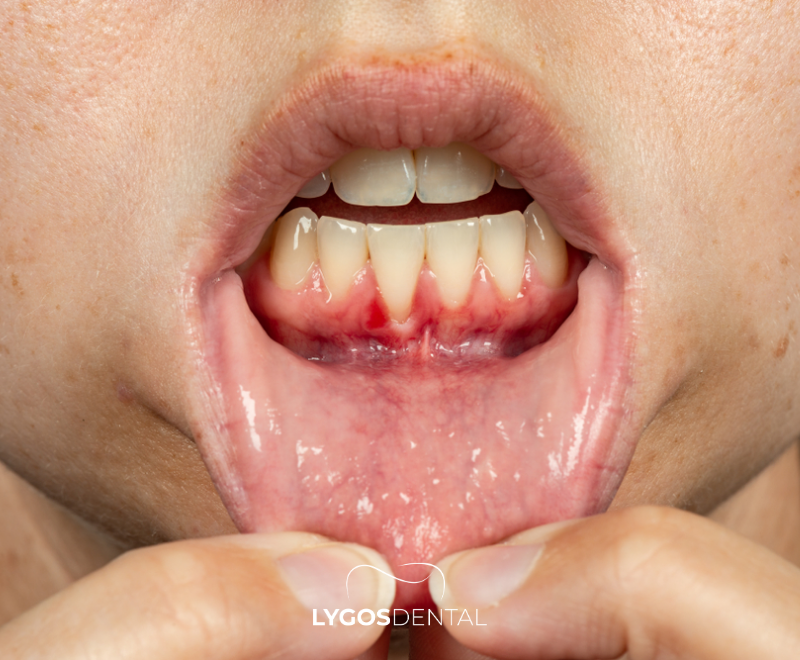
Chronic periodontitis is a slow-progressing inflammation and infection of the tissues that support the teeth. Bacteria in dental plaque trigger irritation of the gums, and over time the infection can reach the periodontal ligament and jawbone. As the supporting structures break down, gums may recede and teeth can become mobile.
Chronic Vs Acute Periodontitis
Both chronic and acute periodontitis affect the gums and the tissues around teeth, but they behave differently. Chronic disease tends to develop gradually with subtle symptoms, while acute episodes usually appear suddenly and can be painful.
| Feature | Chronic Periodontitis | Acute Periodontitis |
| Onset | Slow, often unnoticed at first | Sudden |
| Symptoms | Often mild at the beginning; may include bleeding, recession, bad breath | More intense pain, swelling; may include fever in severe cases |
| Progression | Develops over months or years | Can worsen quickly |
| Prevalence | More common | Less common |
| Treatment urgency | Planned treatment plus long-term maintenance | Needs prompt care to control symptoms and infection |
Acute flare-ups can sometimes occur on top of chronic disease. If pain or swelling appears suddenly, a dental visit should not be delayed.
What Causes Chronic Periodontitis?
The primary trigger is bacterial plaque that stays on the teeth and along the gumline. When plaque hardens into tartar, it becomes harder to remove without professional cleaning and provides a surface where bacteria thrive.
- Plaque and tartar: Inadequate brushing and interdental cleaning allow deposits to build up and irritate the gums.
- Smoking and tobacco use: Tobacco reduces blood flow to gum tissue and makes healing slower.
- Genetic susceptibility: A family history can increase risk, even with reasonable hygiene.
- Systemic conditions: Diabetes and other conditions that affect immunity can make gum infections more likely and harder to control.
- Hormonal changes: Pregnancy, puberty, and menopause can make gums more reactive to plaque.
Who Is at Risk?

Chronic periodontitis can affect anyone, but certain factors make it more likely or more severe. If you recognise one or more of the risks below, regular dental checks are especially important.
- Irregular brushing and flossing or difficulty cleaning around crowded teeth, bridges, or implants
- Smoking or vaping nicotine products
- Uncontrolled diabetes or other conditions that affect immune response
- Family history of gum disease
- Skipping routine dental cleanings and checkups
- High stress and poor sleep, which can affect immunity and habits
- Diet low in key nutrients (including vitamin C and protein)
Symptoms of Chronic Periodontitis
Symptoms can be mild in the early stages. Many people first notice bleeding while brushing or persistent bad breath rather than pain.
- Red, tender, or swollen gums
- Bleeding when brushing, flossing, or eating
- Gum recession or teeth looking “longer”
- Persistent bad breath or a bad taste
- Loose, shifting, or spreading teeth
- Sensitivity or discomfort when chewing
- Pus, abscesses, or a change in how the teeth fit together
How Dentists Diagnose It

Diagnosis is based on a clinical exam and measurements around each tooth. Dentists often use a small probe to measure pocket depths and check for bleeding, along with X‑rays to look for bone loss. The results help determine severity and guide a treatment plan.
Treatment Options
Treatment aims to control infection, reduce inflammation, and stabilise the supporting tissues. The right approach depends on how advanced the disease is and how well you can keep the area clean at home.
Non-Surgical Treatment
Most cases begin with professional deep cleaning, often called scaling and root planing. This removes plaque and tartar above and below the gumline and smooths root surfaces to make reattachment easier. Your dentist may recommend antiseptic rinses or local medications depending on pocket depth and inflammation.
Antibiotics
Antibiotics may be used in selected cases to reduce bacterial load, either as a local gel placed into pockets or as tablets. They are usually an add-on to thorough cleaning rather than a replacement for it.
Surgical Treatment
When pockets are deep or bone loss is significant, surgery may be recommended. Procedures can include flap surgery to clean deep areas, and regenerative options such as bone grafting or guided tissue regeneration to support healing where appropriate.
Laser Treatment
Some practices use laser-assisted therapy as part of periodontal treatment. The goal is to reduce bacteria and inflamed tissue with a minimally invasive approach. Suitability depends on the case and the equipment available.
Maintenance and Follow-Up
Long-term success depends on maintenance. After active treatment, your dentist or periodontist will usually recommend periodontal maintenance visits at a tailored interval, along with a home-care routine to prevent relapse.
Aftercare and Prevention
Chronic periodontitis is typically managed rather than “cured” overnight, so consistency matters. These habits help protect the gums and reduce the chance of recurrence.
- Brush twice daily: Use a soft brush and focus on the gumline.
- Clean between teeth daily: Floss, interdental brushes, or water flossers can help, depending on spacing and restorations.
- Stop smoking: Quitting improves blood flow and healing response.
- Manage medical conditions: Good diabetes control is strongly linked to better gum outcomes.
- Keep up with maintenance visits: Professional monitoring catches relapse early.
Frequently Asked Questions
Can chronic periodontitis be completely cured?
It is a long-term condition, so the focus is usually on stopping progression and keeping the disease stable. With early care, professional treatment, and ongoing maintenance, many people keep their teeth and gums healthy for years.
How long does treatment take?
Mild cases may improve after a small number of visits, while moderate to advanced disease may need several appointments and ongoing follow-up. If surgery is needed, healing and reassessment can extend the timeline.
Can periodontitis cause tooth loss?
Yes. As bone support decreases, teeth can loosen and may eventually need to be removed. Early treatment significantly reduces this risk.
Is chronic periodontitis contagious?
The disease itself is not “caught” like a cold, but the bacteria involved can be shared through saliva. Good oral hygiene for everyone in the household and avoiding sharing toothbrushes are sensible precautions.
If you notice bleeding gums, swelling, or persistent bad breath, book a dental evaluation. Early care is usually simpler and more cost-effective, and it helps protect the teeth and bone support over the long term.
