In-Office Laser Teeth Whitening Process and Prices
In-Office Laser Teeth Whitening: Process and 2026 Prices
In-office laser teeth whitening is a chairside procedure where a dentist applies a professional whitening gel and activates it with a light/laser system to brighten your natural tooth color. Most people see a noticeable change after one visit, with results depending on staining, enamel thickness, and aftercare habits like avoiding dark foods for 48 hours.
What In-Office Laser Teeth Whitening Is
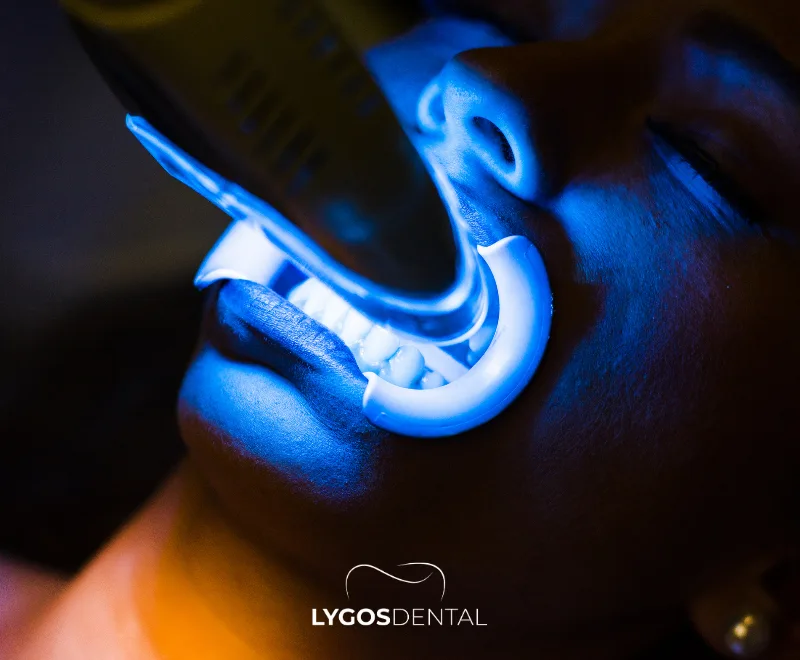
In-office laser teeth whitening is a professional whitening treatment performed in a dental clinic. A high-strength whitening gel is placed on the tooth surfaces and activated with a laser or high-intensity light to speed up the brightening effect.
Because the process is controlled by a dentist, it tends to be faster and more predictable than over-the-counter products. It targets external stains (tea, coffee, smoking) and some deeper discoloration, depending on the cause.
How The Procedure Works
Exact protocols vary by clinic and brand of whitening system, but most appointments follow a similar sequence.
Exam And Shade Selection
Your dentist checks the health of your teeth and gums and identifies issues that should be treated first, such as cavities, gum inflammation, or heavy tartar. A starting shade is recorded so you can compare the change after treatment.
Gum Protection And Gel Application
A protective barrier is placed over the gums to reduce irritation. The whitening gel is then applied only to the visible tooth surfaces.
Light/Laser Activation
The gel is activated with a light or laser system to enhance the whitening reaction. Depending on the system, the gel may be refreshed and reactivated in short cycles during the visit.
Rinse And Final Check
After the last cycle, the gel is removed and the teeth are rinsed. Your dentist checks the final shade and may recommend a desensitizing product if you are prone to sensitivity.
How Many Sessions You Might Need

Many patients complete in-office whitening in one session, usually lasting about 30–60 minutes. If your teeth start out very dark or you want a brighter target shade, your dentist may recommend 2–3 sessions.
Spacing sessions gives the teeth time to rehydrate and helps manage sensitivity. Your dentist can set realistic expectations based on the cause of discoloration and your enamel condition.
Who Is A Good Candidate
In-office whitening is typically suitable for healthy, natural teeth with yellow or brown staining. It may be postponed if you have untreated cavities, active gum disease, or severe enamel wear.
Fillings, crowns, and veneers do not whiten with gel. If you have visible restorations on the front teeth, plan for possible replacement after whitening so the shades match.
Before And Aftercare Tips
24 Hours Before
Have a dental exam first, and consider a professional cleaning if you have tartar buildup. Try to limit smoking and strongly colored drinks like coffee, tea, and red wine the day before your appointment.
First 48 Hours After
For the first two days, choose a “white diet” where possible: water, milk, yogurt, rice, pasta, eggs, and light-colored soups. Avoid staining foods and drinks such as coffee, tea, cola, wine, tomato sauces, and dark spices.
Managing Sensitivity
Mild sensitivity can happen and usually settles within a few days. A toothpaste for sensitive teeth, lukewarm water, and avoiding very cold or acidic foods can help. Contact your dentist if sensitivity is strong or lasts longer than a week.
To keep results longer, brush twice daily, floss regularly, and schedule routine cleanings. Stain habits (smoking, coffee/tea) have the biggest impact on how long your shade lasts.
Advantages And Limitations
Advantages include speed, professional supervision, and controlled gum protection. Many patients see a noticeable change after a single visit.
Limitations include temporary sensitivity and the fact that whitening does not change the color of crowns, veneers, or fillings. Very gray discoloration (such as some tetracycline staining) may need a different cosmetic plan.
2026 Laser Teeth Whitening Prices In Turkey

Prices vary widely by city, clinic facilities, the whitening system used, and whether you are whitening one arch (upper or lower) or both arches. A consultation is the only way to get a precise quote for your teeth.
What Affects Cost
- Number of sessions and whether the fee is per session or a package
- Upper arch only vs. both arches
- Pre-treatment needs (exam, X-rays, tartar cleaning, fillings)
- Dentist experience, clinic location, and the brand of whitening system
Typical Price Ranges
Based on publicly listed 2025–2026 clinic ranges and current fee guides in Turkey, in-office laser/LED-assisted whitening is commonly quoted in the following bands:
| Service (Typical) | Estimated 2026 Range (TRY) |
| Single in-office session (both arches) | 9,000 – 15,000 |
| Single arch (upper or lower) | 8,000 – 13,000 |
| Two-session package | 16,000 – 26,000 |
| Three-session package | 22,000 – 35,000 |
Clinics may price whitening separately from the exam and cleaning, while others bundle these into a package. If you see a much lower quote, confirm whether it covers both arches and whether it includes gum protection and follow-up checks.
Frequently Asked Questions
Is in-office laser teeth whitening safe?
When performed by a licensed dentist with proper gum isolation, in-office whitening is considered a safe cosmetic procedure for most adults. Your dentist will screen for cavities, gum problems, and enamel issues before starting.
Does it hurt?
Most people do not feel pain during the appointment. Some experience temporary sensitivity, especially to cold air or drinks, and it typically improves within a few days.
How long do results last?
Results vary with diet and habits. Many people maintain a brighter shade for several months, and longer with good oral hygiene and reduced staining habits.
What age is it suitable for?
Dentists often prefer to wait until tooth development is complete. Your dentist can advise whether whitening is appropriate for teenagers based on dental maturity and sensitivity risk.
How long does a session take?
A typical appointment takes around 30–60 minutes, depending on the whitening system and the number of gel cycles used.
Will it whiten crowns or veneers?
No. Restorations do not change color with whitening gel. If you have visible restorations, plan shade matching with your dentist after whitening.
Symptoms of Tooth Decay
Symptoms Of Tooth Decay
Tooth decay often starts quietly, then progresses to sensitivity, visible spots, and pain. Early signs include brief twinges with cold or sweet foods and chalky white areas on the enamel. As the cavity deepens, you may notice persistent toothache, bad breath, pain when chewing, or gum swelling. A dentist can confirm decay and recommend the right treatment.
Tooth decay (dental caries) happens when acids produced by mouth bacteria gradually break down tooth enamel. Catching it early usually means simpler treatment and less risk of infection, root canal treatment, or tooth loss.
What Tooth Decay Is
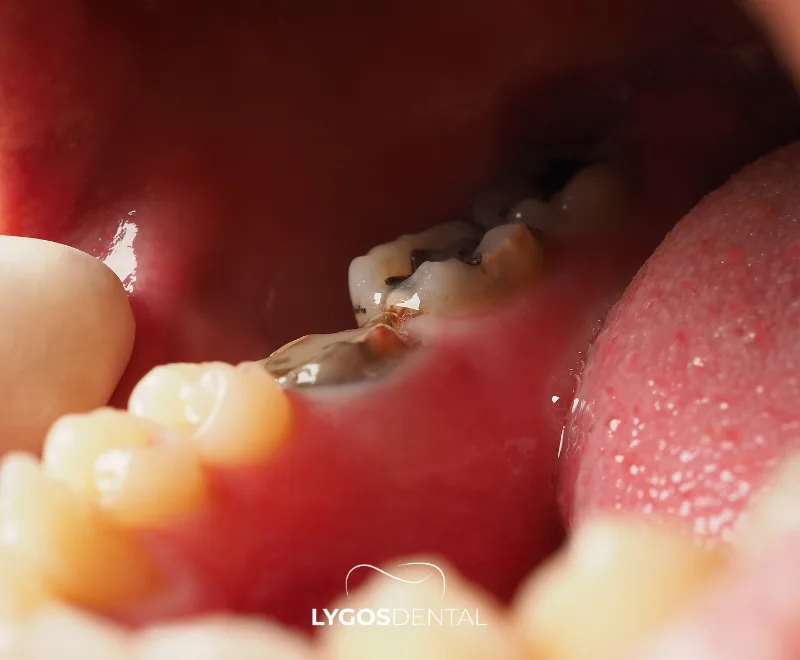
Tooth decay begins when plaque bacteria feed on sugars and starches and produce acid. Over time, repeated acid attacks pull minerals out of the enamel (demineralization). If the surface breaks down, a cavity forms and can spread into dentin and, eventually, the pulp where the nerve sits.
Common Causes Of Tooth Decay
Most cavities develop due to a mix of diet, daily habits, and individual risk factors. The most common triggers include:
- Poor oral hygiene: Infrequent brushing and flossing allow plaque to build up and stay on the tooth surface.
- Sugary or acidic foods and drinks: Frequent soda, sweets, juice, and sticky snacks raise acid levels and weaken enamel.
- Dry mouth: Low saliva reduces the mouth’s ability to neutralize acids and wash away food particles.
- Frequent snacking: Eating or sipping throughout the day gives teeth less time to recover between acid attacks.
- Tooth anatomy and genetics: Deep grooves, crowded teeth, and naturally weaker enamel can increase risk.
Symptoms Of Tooth Decay

Symptoms depend on how deep the decay is. Some cavities cause no pain at first, especially between teeth, so regular dental check-ups still matter. These are the most typical signs people notice:
- Tooth sensitivity: A quick, sharp feeling with cold, hot, or sweet foods.
- Toothache: A dull ache or throbbing pain, sometimes worse at night.
- Visible changes: White, brown, or black spots; rough areas; or a visible pit or hole.
- Pain when chewing: Discomfort when biting, especially on hard or sugary foods.
- Bad breath or bad taste: Plaque bacteria and food trapped in a cavity can cause persistent odor or taste.
- Gum tenderness or swelling: Irritation near the tooth, sometimes linked to a deeper infection.
What A Tooth Decay Toothache Can Feel Like
Early decay often causes brief sensitivity that stops once the trigger is gone. When decay reaches dentin, pain can become more frequent and more intense. If the pulp is involved, pain may be constant, throbbing, or sharp, and it can radiate to the jaw or ear. Severe pain with swelling or fever can signal an abscess and needs urgent dental care.
How Dentists Diagnose Tooth Decay
A dentist usually checks for soft spots, discoloration, and areas that catch or feel rough. Bitewing X-rays are commonly used to find decay between teeth and assess depth. Some clinics also use light-based tools to spot early enamel mineral loss.
Treatment Options For Tooth Decay
Treatment depends on the stage of decay and whether the nerve is affected. A dentist will recommend the most conservative option that restores strength and stops the bacteria.
- Fluoride treatment: In very early decay (before a hole forms), fluoride varnish, gel, or prescription toothpaste can help remineralize enamel.
- Dental filling: Once a cavity forms, the decayed area is removed and the tooth is restored with a filling material.
- Crown: If a large portion of the tooth is weakened, a crown may be used to protect it from cracking.
- Root canal treatment: If decay reaches the pulp, infected tissue is removed and the tooth is sealed and restored.
- Extraction and replacement: Severely damaged teeth may need removal; common replacements include implants, bridges, or dentures.
When To See A Dentist
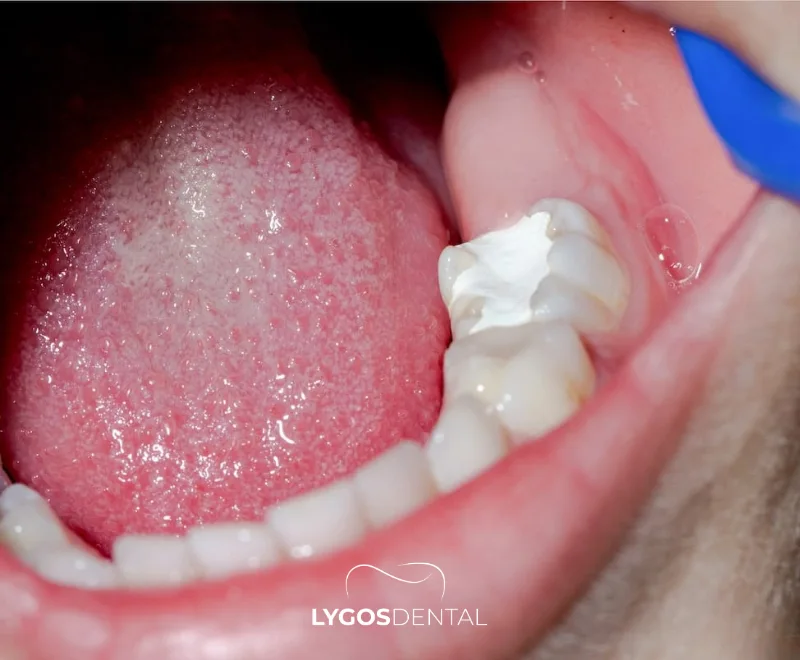
Book a dental visit if you have sensitivity that keeps returning, a toothache, pain on chewing, or any visible pits or dark spots. Seek urgent care if you have facial swelling, pus, fever, or trouble swallowing, as these can point to a spreading infection.
How To Prevent Tooth Decay
Good prevention focuses on plaque control, fluoride exposure, and reducing how often teeth are exposed to sugar and acid.
- Brush twice daily with fluoride toothpaste and clean along the gumline.
- Floss (or use interdental brushes) once a day to clean between teeth.
- Limit sugary snacks and drinks, especially between meals.
- Drink water after eating and consider fluoridated water where available.
- Keep up with regular dental check-ups and professional cleanings based on your dentist’s advice.
Book An Appointment
If you’d like a professional assessment or treatment options such as fillings, crowns, implants, or cosmetic dentistry, contact your dental clinic to arrange an appointment.
Symptoms Of Tooth Decay FAQ
Can a decayed tooth heal on its own?
A formed cavity cannot “heal” back to normal. In the earliest stage—before a hole develops—enamel can sometimes be strengthened through remineralization with fluoride and improved home care.
How long do symptoms of tooth decay last?
Sensitivity may come and go at first. If decay continues, symptoms often become more frequent and can progress to persistent pain until the tooth is treated.
How can I relieve tooth decay pain at home?
Short-term relief may come from over-the-counter pain medicine (follow the label), avoiding very hot, cold, or sweet triggers, and rinsing with warm salt water. These steps do not treat the cause, so a dental visit is still needed.
What are the most common symptoms of a decayed tooth?
Typical signs include sensitivity to hot or cold, toothache, pain when chewing, visible white/brown/black spots or a pit, bad breath, and gum tenderness near the tooth.
Emax or Zirconium on Implants
Emax Or Zirconium On Implants
For implant crowns, zirconium (zirconia) is usually chosen when strength and long-term durability come first, especially for back teeth or heavy biting. Emax can be an excellent option in the front when you want the most natural translucency and the bite load is controlled. The best choice depends on tooth position, bite force, and design.
Dental implants can replace missing teeth with a result that looks and functions like a natural tooth. The implant itself is only part of the outcome—the crown material plays a major role in appearance, comfort, and longevity. Two of the most common all-ceramic options are Emax and zirconium. Below is a practical comparison to help you understand where each material tends to perform best.
What’s The Difference Between Emax And Zirconium?
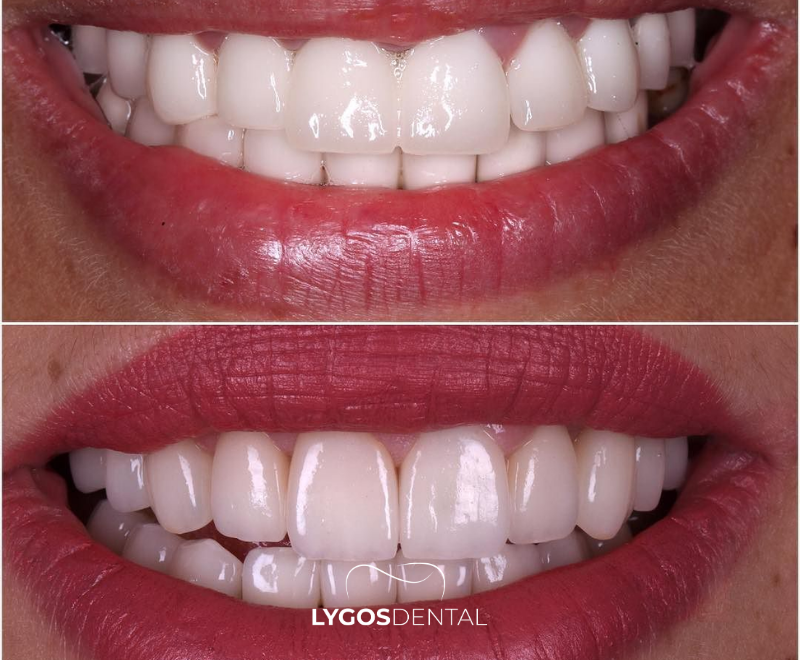
Both options are metal-free, tooth-colored ceramics, but they behave differently under light and pressure. You’ll also see different terms used in clinics: “zirconium” crowns typically refer to zirconia (zirconium dioxide).
Emax (Lithium Disilicate)
Emax is a lithium disilicate glass-ceramic known for its translucency. It lets light pass through in a way that closely mimics enamel, which is why it is often selected for visible front teeth. With careful planning, it can also be used on implants when bite forces are moderate.
Zirconium (Zirconia)
Zirconia is a very strong ceramic with high fracture resistance. That strength makes it a common choice for implant crowns, particularly in the back of the mouth where chewing forces are highest. Modern monolithic zirconia has also improved in shade and surface texture compared with earlier generations.
Advantages Of Emax And Zirconium Crowns
Each material has clear strengths. Your dentist may recommend one over the other based on the location of the implant, bite forces, and how visible the tooth is when you smile.
Emax Crown Advantages
- High translucency for a natural, enamel-like appearance
- Strong aesthetic performance in the front teeth
- Good soft-tissue (gum) response when contours are designed correctly
- Smooth surface that can be comfortable for the opposing teeth
- Color stability with proper hygiene and regular checks
Zirconium Crown Advantages
- Very high strength, suitable for molars and heavy chewing
- Metal-free and generally well tolerated by soft tissues
- Low risk of discoloration over time
- Long service life when the bite is properly adjusted
- Often preferred for full-contour (monolithic) implant crowns
Which Looks More Natural On Implants?
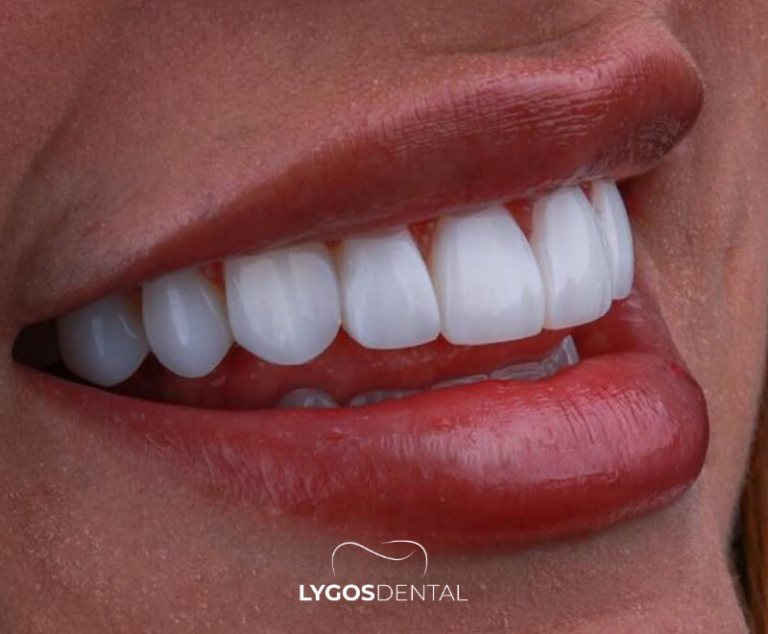
If your priority is the most lifelike appearance—especially for a single front tooth—Emax often has the edge. Its light transmission can blend more seamlessly with adjacent natural teeth, particularly in bright environments or under flash photography.
Zirconia can still look excellent, especially with newer translucent grades and good staining and glazing. The main difference is that zirconia typically remains a bit more opaque than Emax, which may matter when the tooth is very visible or the gum line is thin.
Which Is More Durable For Chewing Forces?
For strength under pressure, zirconia is usually the safer bet. Implant crowns can be exposed to high forces, and zirconia’s fracture resistance makes it a reliable option for premolars and molars.
Emax is durable for many cases, but it is more sensitive to heavy load or parafunctional habits such as grinding (bruxism). When a patient clenches or grinds, dentists often lean toward zirconia and may also recommend a night guard to protect both the crown and the implant components.
Emax Or Zirconium: How Dentists Decide
There isn’t a one-size-fits-all answer, but a few clinical patterns show up again and again:
- Front implant crown with high aesthetic demand: Emax may be considered, especially when bite forces are controlled.
- Back implant crown, bridges, or high bite force: zirconia is commonly preferred for strength and stability.
- Grinding or clenching: zirconia is often recommended, plus bite adjustment and protective night guard if needed.
- Thin gum tissue or high smile line: Emax or highly translucent zirconia may be selected depending on shade matching and the abutment design.
Your dentist will also consider crown design (screw-retained vs cement-retained), available space, and the condition of the opposing teeth. A careful bite check is essential with either material, because implants don’t have the same shock absorption as natural teeth.
Emax And Zirconium Prices In Turkey

Pricing varies by city, clinic experience, laboratory quality, and whether the crown is part of a larger implant plan. Clinics commonly quote ranges like the following in 2026:
| Crown Type | Typical Range (TRY) |
| Emax crown | 4,000 – 7,000 TL |
| Zirconium (zirconia) crown | 3,000 – 5,500 TL |
Ask whether the quote includes the abutment, try-in appointments, and any warranty or follow-up checks. A lower price can sometimes reflect a different lab process, a less customized shade match, or fewer follow-up visits.
Frequently Asked Questions
Can Emax Be Used On Implants?
Yes. Emax can be used for implant crowns, most commonly in the aesthetic zone. The case needs proper planning so the crown isn’t exposed to excessive bite forces, and the shade and contours must be matched carefully to the surrounding teeth and gums.
Does Zirconium Look As Natural As Emax?
In many cases, zirconia can look very natural, especially with modern translucent materials and good finishing. Emax still tends to provide a slightly more enamel-like translucency, which can matter most for a single front tooth or very high cosmetic expectations.
Which Crown Is More Durable?
Zirconia is generally more durable under heavy chewing forces and is often selected for molars, implant bridges, and patients who clench or grind. Emax is strong enough for many situations, but it is typically chosen when the visual result is the main priority and forces are moderate.
Single Tooth Implant Crown Prices
Single Tooth Implant Crown Prices
Single tooth implant crown prices in Turkey depend on the implant brand, crown material, clinic location, and whether you need extra procedures like bone grafting. In 2025, typical total costs for one implant with a crown ranged from 9,000 TL to 24,000 TL. Your final quote is confirmed after an exam and imaging.
A single implant crown replaces a missing tooth with an artificial root (the implant) and a fixed crown. It restores chewing, supports jawbone health, and avoids trimming adjacent teeth for a bridge. Because pricing varies widely between cases and clinics, it helps to understand what drives the total cost.
What Is A Single Tooth Implant?
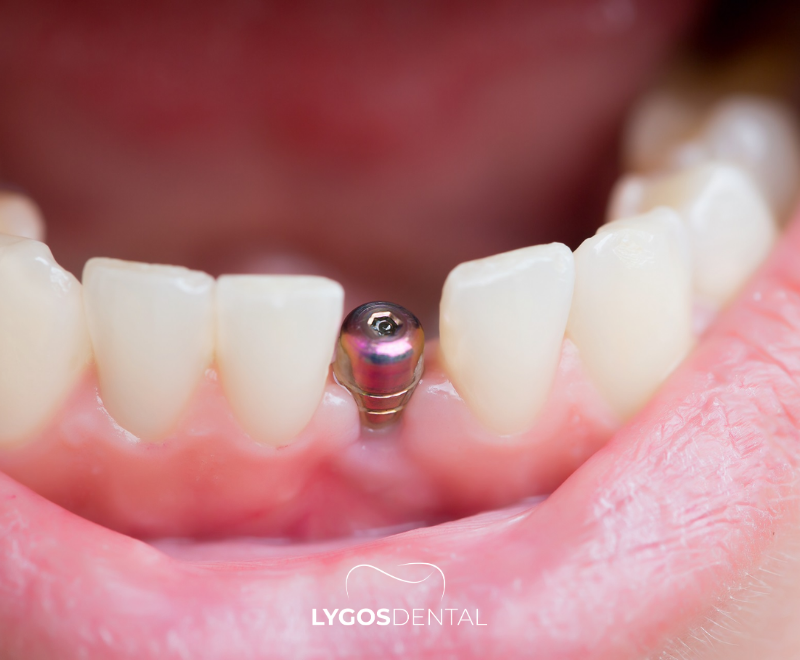
A single tooth implant is a small titanium (or titanium-alloy) post placed into the jawbone to act as an artificial root. After healing and bone integration, a crown is attached to restore the look and function of the missing tooth. When planned correctly, it is a long-term, fixed solution that feels and functions close to a natural tooth.
What’s Included In The Total Price?
Clinics may quote prices as an all-in package or as separate items. A complete single-tooth restoration often includes the implant, the connecting part (abutment), and the crown, plus clinical and lab work. Always confirm exactly what is included so you can compare offers fairly.
- Implant fixture (the root placed in bone)
- Abutment (the connector between implant and crown)
- Crown (porcelain or zirconia, depending on your choice)
- Surgical and prosthetic appointments
- Laboratory fees (if billed separately)
Factors Affecting Single Tooth Implant Crown Prices
Single tooth implant crown prices are influenced by both clinical needs and material choices. Two people missing the same tooth can receive different quotes because bone quality, aesthetics, and bite forces vary. The key cost drivers are below.
Implant Brand And Country Of Manufacture
Implant systems differ in design, research background, and manufacturing standards. Domestic implants are usually priced lower, while well-known imported systems from countries such as Germany, Switzerland, or the USA tend to cost more.
Crown Material
Porcelain crowns are often the more budget-friendly option. Zirconia crowns typically offer stronger aesthetics and durability, which can increase the overall price—especially for front teeth where appearance matters most.
Dentist Experience And Clinic Location
Fees can be higher in major cities such as Istanbul and Ankara due to operating costs and demand. A clinician’s experience, planning approach, and the lab they work with can also affect pricing and the quality of the final fit.
Additional Procedures
Some cases require preparatory treatments before the implant is placed. Bone grafting, sinus lift procedures, and gum shaping can add to the total, but they may be necessary for stability and long-term success.
Price Ranges For Single Tooth Implants In Turkey (2025–2026)
The ranges below reflect typical 2025 pricing shared by clinics and may shift in 2026 due to inflation, exchange rates, and differences in what is included. Use them as a starting point, not as a fixed tariff.
- Domestic implant + porcelain crown: 9,000 TL – 13,000 TL
- Imported implant + porcelain crown: 13,000 TL – 18,000 TL
- Imported implant + zirconia crown: 17,000 TL – 24,000 TL
Does SGK Cover Single Tooth Implant Treatment?
SGK coverage for dental implants is limited and usually depends on medical necessity and where the treatment is provided. In many routine, private-clinic cases, implants are not covered. In specific situations—such as trauma-related tooth loss or congenital absence—partial support may be possible with documentation and an approved medical board report in a public setting.
Additional Costs To Consider
Ask for a written plan that lists any extra fees beyond the implant and crown. These items can change the final total and are useful for comparing clinics.
- X-rays and 3D tomography: Imaging may be needed for safe planning and precise placement.
- Bone grafting (bone powder): If bone volume is insufficient, grafting may add roughly 2,000 TL – 5,000 TL.
- Temporary crown or healing cap: Sometimes used to protect the area or manage appearance during healing.
- Medications and follow-up visits: Some clinics include check-ups; others bill them separately.
What To Know Before Getting A Single Tooth Implant
Treatment Timeline
Bone integration commonly takes around 2–4 months, then the crown is fitted. Depending on your bone condition and whether extra procedures are needed, the full process often completes within 3–6 months.
Who Is A Good Candidate?
General health, smoking habits, gum condition, and bone density all influence suitability and success. A clinical exam and imaging are essential to confirm whether an implant is the best option for you.
Aftercare And Maintenance
Implants need daily brushing and cleaning between teeth, just like natural teeth. Regular check-ups help catch early gum inflammation and protect the investment long term.
Warranty And Documentation
Some clinics provide written warranties for implant components or workmanship. Ask what is covered, for how long, and what maintenance visits are required to keep the warranty valid.
Single Tooth Implant Crown Prices: FAQ
How long does a single tooth implant take to complete?
It typically takes 2–4 months for the implant to integrate with the jawbone. After that, the crown is placed. If your bone is adequate and no additional procedures are needed, many cases finish within 3–6 months.
What are the 2025–2026 prices for a single tooth implant in Turkey?
Typical 2025 ranges for an implant with a crown were 9,000 TL to 24,000 TL, depending on implant brand and crown material. Prices can shift in 2026 and vary by clinic, city, and what is included in the package.
Is a single tooth implant painful?
Implant placement is done under local anesthesia, so you shouldn’t feel pain during the procedure. Mild swelling or tenderness afterward is common and is usually controlled with prescribed medication.
Does SGK cover dental implants?
SGK coverage is limited. Routine implants in private clinics are often not covered, while medically necessary cases in public settings may be supported with proper documentation and approvals.
What should I watch out for after the procedure?
Follow your dentist’s instructions, keep the area clean, and avoid smoking during healing. Stick to softer foods at first and attend follow-up visits so the implant can be monitored as it integrates.
Post-Dental Implant Care
Post-Dental Implant Care
Post-dental implant care is about protecting the surgical site while the implant bonds with your jawbone. For the first 24 hours, control bleeding with gentle gauze pressure, use cold compresses, and avoid rinsing, spitting, straws, and smoking. Over the following weeks, keep the area clean, choose soft foods, take prescribed medication, and attend follow-ups.
What Is a Dental Implant?
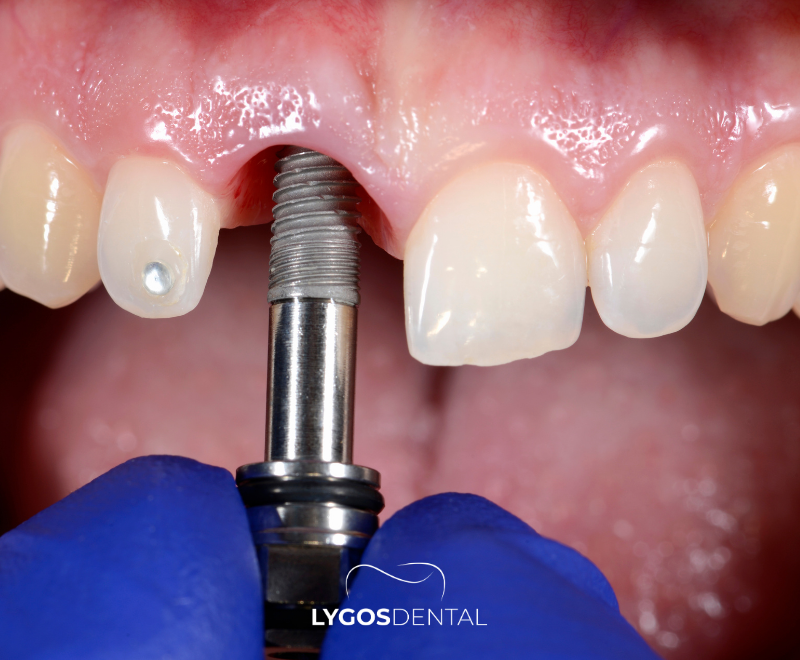
A dental implant is a titanium post placed in the jawbone to replace a missing tooth root. After it heals and becomes stable, a crown (or another restoration) is attached on top to restore chewing function and appearance.
Implants can be a long-lasting solution, but the result depends heavily on how well the area heals in the weeks and months after surgery.
The First 24–72 Hours After Surgery
Swelling, mild bleeding, and soreness are common early on. The goal in this phase is simple: protect the blood clot, keep the area calm, and follow your clinic’s instructions.
Control Bleeding
Light bleeding or oozing can happen during the first day. Bite down gently on gauze as instructed and replace it if needed. If bleeding becomes heavy or won’t settle, contact your dentist or surgeon.
Reduce Swelling
Swelling often peaks within the first couple of days. Cold packs on the outside of the face can help during the early period, especially on day one. Keep sessions short and give your skin breaks.
Manage Pain Safely
Take pain relief exactly as advised. If you were prescribed antibiotics or an antiseptic rinse, use them on schedule. If pain worsens rather than improves after a few days, get checked.
Rest and Activity
Take it easy for the first couple of days. Avoid strenuous exercise, heavy lifting, and anything that raises your heart rate too much, since this can increase bleeding and swelling.
Avoid These Common Mistakes
For the first 24 hours, many clinics advise avoiding anything that can disturb healing, such as vigorous rinsing, spitting, drinking through a straw, and smoking. Skip very hot drinks and alcohol during early recovery, especially if you’re taking medication.
Dental Implant Healing Process
After placement, the implant needs time to fuse with the jawbone (osseointegration). A typical healing window is around 3 to 6 months, though timing can vary based on bone quality, implant location, and personal health factors.
During this period, your dentist may schedule follow-ups to monitor healing and plan the next step (such as fitting the crown). Keep those appointments even if you feel fine.
Eating and Drinking After a Dental Implant

Food choices can either protect the site or irritate it. Aim for soft, nourishing meals and avoid chewing directly on the surgical side until your dentist says it’s safe.
First 24–48 Hours
Stick with liquids and very soft foods. Many post-op instructions recommend a soft or liquid diet at first, then a gradual return as comfort improves.
Good options:
- Yogurt, smoothies (no straw), soups that are not hot
- Mashed potatoes, scrambled eggs, oatmeal
- Soft fish, well-cooked pasta
The First Week
Choose soft foods and avoid anything hard, crunchy, sticky, or spicy. Some guidance suggests keeping meals soft for at least a week while tissues settle.
Drink plenty of water. Avoid alcohol early on, especially with pain medication.
How To Clean Around a New Implant
Cleanliness matters, but early on you need a gentle approach. Your dentist may give instructions that differ based on stitches, bone grafts, or how the implant is positioned.
Brushing and Cleaning
Continue brushing the rest of your teeth carefully. For the implant area itself, some hospitals advise not brushing directly over the surgical site for about a week, using an antiseptic (chlorhexidine) mouthwash instead if recommended.
Use a soft toothbrush and avoid aggressive scrubbing near stitches. Once your dentist gives the green light, clean around the implant daily using gentle brushing and interdental cleaning.
Rinsing
Many post-op instructions recommend avoiding rinsing for the first 24 hours, then starting gentle rinses after that. This may be warm salt water or a recommended mouthwash, depending on your dentist’s plan.
Smoking and Alcohol

Smoking is strongly linked with slower healing and higher complication risk. If you smoke, the best move for healing is to stop completely, or at least avoid smoking throughout the critical early healing window.
Alcohol can interfere with healing and is often discouraged in the early days, especially if you’re taking post-op medication.
Possible Complications and When To Call Your Dentist
Some discomfort is normal. These signs deserve a call:
- Bleeding that doesn’t slow down
- Swelling that gets worse after a few days
- Fever, pus, or a bad taste that suggests infection
- Severe or increasing pain
- Implant feels loose
- Ongoing numbness or tingling
When in doubt, check in. Early treatment prevents small issues from becoming bigger ones.
Post-Dental Implant Care FAQ
How Long Does Post-Dental Implant Care Last?
Daily care starts immediately and continues for life, like caring for natural teeth. The main surgical healing and bone bonding phase often takes about 3 to 6 months.
When Can I Return To Normal Eating Habits?
Most people start with soft foods and progress gradually. Many providers suggest staying on softer foods for at least the first week and avoiding chewing directly on the implant site until advised.
How Long Does Pain Last After Implant Surgery?
Soreness usually improves over several days. If pain is severe, worsening, or not improving, contact your dentist for an assessment.
Can I Smoke After Dental Implant Surgery?
It’s best not to. Smoking can slow healing and raise the risk of complications and implant failure.
How Should Dental Implants Be Cleaned Long Term?
Brush twice daily, clean between teeth, and attend regular professional check-ups. Your dentist may recommend specific tools (interdental brushes, implant-safe floss) based on the type of restoration.
Hollywood Smile and Social Media
Hollywood Smile And Social Media
A Hollywood Smile is a customized smile design that improves tooth color, shape, and symmetry—often through whitening, veneers, gum contouring, or aligners. On social media, a balanced smile reads clearly on camera, can reduce reliance on filters, and helps profiles look polished. Results depend on planning and oral health.
Social media puts faces front and center. High-resolution photos, short-form video, and close-up selfies make small details—especially teeth and gums—more noticeable than ever.
That’s why “Hollywood Smile” treatments have become a common topic for people who want a brighter, more balanced smile for both everyday confidence and on-camera presence. The key is getting a result that looks natural, functions well, and fits your facial features.
What Is A Hollywood Smile?

A Hollywood Smile is a personalized smile makeover designed by a dentist. Instead of a single procedure, it’s a plan that can combine cosmetic and restorative treatments to improve color, alignment, proportions, and gum symmetry while protecting bite function.
Treatments That May Be Included
Your dentist selects options based on tooth structure, gum health, bite, and your goals. Common components include:
- Professional teeth whitening (bleaching) — Brightens natural enamel. Touch-ups are sometimes needed over time, especially if you drink coffee, tea, or smoke.
- Laminate veneers or zirconia restorations — Changes shape and color for a more even look. The best choice depends on enamel thickness, bite forces, and how many teeth are treated.
- Gum contouring (pink aesthetics) — Reshapes gum levels to improve symmetry or reduce a “gummy” smile when clinically appropriate.
- Orthodontics (braces or clear aligners) — Moves teeth into a better position so restorations can be minimal and more conservative.
- Implants or restorative work when needed — Replaces missing teeth or rebuilds damaged teeth so the smile looks complete and functions comfortably.
- Composite bonding (in some cases) — A more conservative option for small chips or gaps, often used when veneers are not necessary.
Why The Hollywood Smile Stands Out On Social Media
Cameras exaggerate contrast. Bright teeth framed by healthy gums create a clear focal point in thumbnails, Reels, and TikTok clips, even with fast scrolling.
A well-planned smile design can also make facial expressions look more relaxed, because you’re less likely to hide your teeth or force a tight smile for the camera.
That said, a “white” smile isn’t always a better smile. Natural shade, surface texture, and symmetry usually read more believable than an overly uniform look.
Why Influencers And Public-Facing Professionals Choose It

For creators and professionals who appear on camera daily, small visual improvements can add up. A consistent, healthy-looking smile can help profiles feel polished across photos, live streams, and brand content.
People often pursue a Hollywood Smile to look more refreshed on camera, cut down on heavy filters, and feel more confident speaking or laughing in videos.
Smile Design For Photos And Video: What Dentists Look At
A natural-looking result comes from planning, not just whitening. During a consultation, dentists commonly assess:
- Facial midline and tooth proportions (width-to-length balance)
- Lip line and how much tooth shows when talking and smiling
- Gum symmetry and the contour of the gumline
- Bite function and grinding habits (bruxism) that affect durability
- Shade selection that suits skin tone and avoids a “flat” appearance on camera
Many clinics use digital smile design tools to preview shape and shade before any irreversible steps. This is useful for setting expectations and avoiding a result that looks too artificial in real life.
How A Hollywood Smile Can Affect Content And Engagement
After treatment, many people feel more comfortable smiling widely, which can change how they present themselves on camera. That confidence shift is often what followers notice first.
Transformations also perform well as “before and after” content, but it’s smart to share responsibly. Clear lighting, consistent angles, and honest context help viewers understand what changed and why.
What To Know Before You Start Treatment

A Hollywood Smile is a long-term decision. Before moving forward, consider the points below:
- Start with oral health — Cavities, gum disease, and old restorations may need treatment first for predictable results.
- Ask for a conservative plan — In many cases, aligners, bonding, or limited veneers can achieve the goal with less tooth reduction.
- Choose a natural shade — Very bright shades can look opaque in daylight and harsh under studio lighting.
- Understand longevity and maintenance — Veneers and zirconia restorations can last many years, but they still require checkups, good hygiene, and sensible habits.
- Protect your investment — If you grind your teeth, a night guard can reduce the risk of chipping or wear.
- Discuss cost and timeline clearly — Pricing and appointment count vary based on the number of teeth and the treatments involved.
For most people, the best outcome is a smile that looks healthy and believable in everyday life. When that foundation is right, it also tends to photograph well—without relying on heavy edits.
Frequently Asked Questions
How long does a Hollywood Smile take?
It depends on what’s included. Whitening can be done quickly, while aligners, gum work, or veneers often require multiple visits over several weeks. Your dentist can confirm a timeline after an exam and planning.
Is the Hollywood Smile permanent?
Results are long-lasting, but not “forever.” Whitening may need occasional touch-ups. Veneers and zirconia restorations can commonly last 10–15 years or longer with good care, depending on bite forces and habits.
Is the Hollywood Smile painful?
Most steps are done with local anesthesia when needed. Some people feel temporary sensitivity after whitening or tooth preparation, which usually settles with time and proper aftercare.
Will dental aesthetics alone make me look better on social media?
A balanced smile helps, but camera angle, lighting, facial expression, and overall styling also matter. Think of smile design as one part of a wider on-camera presentation.
Can everyone get a Hollywood Smile?
Many people are candidates, but gum disease, untreated cavities, or severe bite issues may need to be addressed first. A dental exam is essential to confirm what’s safe and realistic.
7 Factors That Damage Your Gum Health
7 Factors That Damage Your Gum Health
Gum problems usually start when plaque and inflammation build up. Smoking, tartar, pregnancy hormones, chronic stress and teeth grinding, certain medications, vitamin and mineral deficiencies, and poorly controlled diabetes can all weaken gum tissue. Addressing these triggers early helps prevent gingivitis, recession, and tooth loss.
Healthy gums hold teeth in place and act as a barrier against bacteria. When gums stay inflamed, the risk of bleeding, bad breath, and sensitivity rises. Early gum disease (gingivitis) can often be reversed with consistent care, while advanced disease (periodontitis) may lead to bone loss and tooth mobility.
Most gum problems come down to inflammation plus a trigger that keeps irritation going. Some triggers are lifestyle-related, while others are linked to hormones, nutrition, or medical conditions. Below are seven common factors that can undermine gum health, along with practical ways to reduce the impact.
1. Smoking And Tobacco Use

Tobacco use reduces blood flow in the mouth and makes it harder for gum tissue to heal. It also changes the balance of bacteria and can mask early warning signs, such as bleeding.
People who smoke often see faster progression of gum disease and a weaker response to treatment. Quitting is one of the most effective steps you can take for long-term gum stability.
What helps:
- Ask your dentist about support options, including quit plans and nicotine alternatives.
- Schedule regular cleanings so inflammation is spotted early.
2. Plaque And Tartar Buildup
Plaque is a sticky film of bacteria that forms on teeth every day. If it is not removed, it can harden into tartar (calculus), especially near the gumline.
Tartar is rough and holds more bacteria against the gums, which keeps inflammation active. Once tartar forms, it usually needs professional removal to prevent gum pockets from deepening.
What helps:
- Brush twice daily and clean between teeth once a day with floss or interdental brushes.
- Consider an electric toothbrush if plaque tends to build up quickly.
3. Pregnancy-Related Hormonal Changes
During pregnancy, hormonal shifts can make gums more reactive to plaque and easier to irritate. Swelling, tenderness, and bleeding with brushing are common signs of pregnancy gingivitis.
Good daily cleaning and routine dental visits can keep symptoms under control. If nausea makes brushing difficult, rinsing with water after vomiting and brushing later can help protect gums and enamel.
What helps:
- Tell your dentist you are pregnant so care can be tailored appropriately.
- Choose bland-flavored toothpaste if strong flavors trigger nausea.
4. Stress And Teeth Grinding (Bruxism)

High stress can weaken immune defenses and make it easier for gum inflammation to linger. Stress can also contribute to clenching or grinding, which puts extra force on teeth and supporting tissues.
Over time, bruxism may aggravate gum recession and lead to jaw discomfort or cracked teeth. Managing stress and protecting teeth at night can reduce the load on gums.
What helps:
- Ask your dentist if a night guard is suitable for you.
- Try short, realistic stress reducers such as daily walks, breathing exercises, or a consistent sleep routine.
5. Medications That Affect Gums
Some medications can change the way gums respond, either by causing dry mouth or by triggering gum overgrowth. Dry mouth lowers saliva’s protective effect and can raise the risk of plaque buildup.
Examples include certain blood pressure medications, anticonvulsants, and immune-suppressing drugs. Never stop a prescribed medicine on your own—work with your dentist and prescribing clinician if gum changes appear.
What helps:
- Sip water regularly and consider sugar-free gum to stimulate saliva, if appropriate for you.
- Bring an up-to-date medication list to dental appointments.
6. Vitamin And Mineral Deficiencies
Gum tissue relies on nutrients to maintain its structure and resist infection. Low intake of vitamin C, vitamin D, calcium, and certain B vitamins can make gums more prone to bleeding and irritation.
A balanced diet with fruit, vegetables, protein, and calcium-rich foods supports both gums and bone. If you suspect a deficiency, discuss testing and supplements with a healthcare professional.
What helps:
- Aim for whole foods first; supplements can help when diet alone is not enough.
- If you follow a restricted diet, mention it during dental and medical visits.
7. Diabetes And Blood Sugar Control
Diabetes can increase the risk of gum infection by affecting circulation and the body’s response to bacteria. Gums may heal more slowly, and inflammation can become harder to control.
There is also a two-way relationship: severe gum disease may make blood sugar harder to manage. Consistent oral hygiene, regular cleanings, and working toward stable glucose levels all support healthier gums.
What helps:
- Tell your dentist if you have diabetes and share your latest control status if you track it.
- Keep dental appointments on schedule, even when symptoms feel mild.
Practical Ways To Protect Gum Health
Daily habits make the biggest difference because plaque forms continuously. A few small changes can lower inflammation and keep gums firm.
- Brush gently along the gumline for two minutes, twice a day.
- Clean between teeth daily; this is where gum inflammation often starts.
- Limit frequent sugary snacks and acidic drinks that feed bacteria.
- Replace your toothbrush (or brush head) regularly and after illnesses.
- Book routine dental check-ups and cleanings based on your dentist’s advice.
When To See A Dentist
Contact a dentist if you notice any of the following signs, especially if they persist for more than a week or two:
- Bleeding when brushing or flossing
- Red, swollen, or tender gums
- Persistent bad breath or a bad taste
- Gums pulling away from teeth
- Loose teeth or changes in the way your bite feels
- Pain when chewing
This information is for general education and does not replace a personalized diagnosis or treatment plan.
Frequently Asked Questions
What Are The Early Signs Of Gum Disease?
Common early signs include bleeding with brushing or flossing, redness, swelling, and tenderness. Bad breath and mild gum recession can also appear. Early evaluation helps prevent progression into deeper gum pockets.
What Daily Oral Hygiene Habits Protect Gum Health?
Brush twice a day with gentle pressure and clean between teeth once daily with floss or interdental brushes. A fluoride toothpaste is usually recommended, and a dentist may suggest a specific mouthwash based on your needs. Regular professional cleanings support home care by removing tartar.
What Should You Do If Gum Problems Increase During Pregnancy?
Book a dental check-up and keep up daily brushing and interdental cleaning. Tell your dental team that you are pregnant so they can plan care appropriately. If bleeding or swelling worsens, do not ignore it—early treatment is typically simpler.
How Does Diabetes Affect Gum Disease?
High blood sugar can make it easier for infections to take hold and can slow healing. This raises the risk of inflammation, gum pockets, and bone loss around teeth. Strong oral hygiene plus good blood sugar control offers the best protection.
Zirconium Crown or Metal-Supported Crown?
Zirconium Crown or Metal-Supported Crown?
Zirconia crowns (often called “zirconium” crowns) are metal‑free ceramic crowns valued for a natural, light‑reflecting look and good gum tolerance. Metal‑supported crowns (porcelain‑fused‑to‑metal) use a metal core for proven strength, but may look more opaque and can show a gray line if gums recede. The best choice depends on tooth location and bite forces.
What Is A Zirconia (Zirconium) Crown?
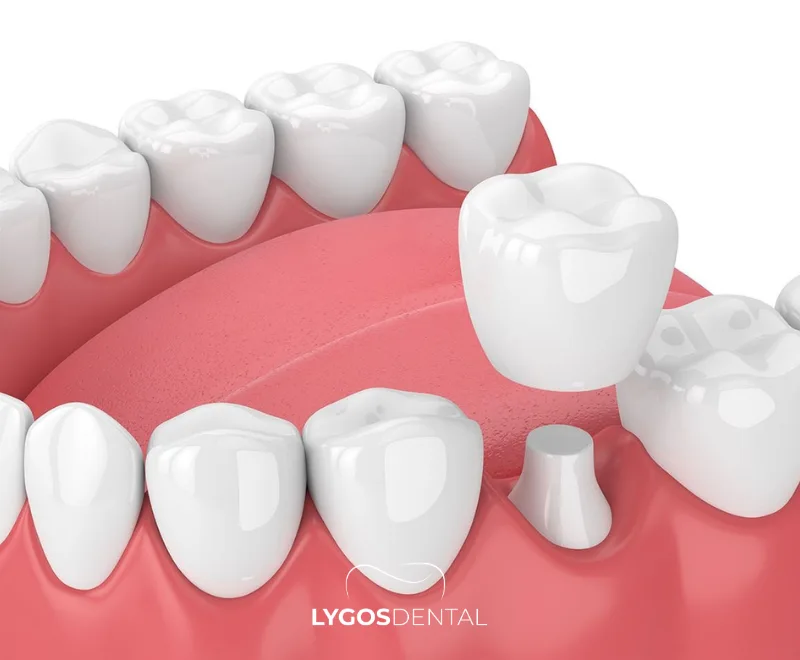
A zirconia crown is an all‑ceramic crown made from zirconium dioxide, a high‑strength dental ceramic. Many clinics call it a “zirconium crown,” but the crown itself is zirconia. Because it contains no metal, it can look closer to a natural tooth, especially near the gumline.
Zirconia crowns are commonly produced with digital scanning and CAD/CAM milling for a precise fit. They can be made as monolithic zirconia (one solid piece) for strength, or layered with porcelain for extra translucency in visible areas. Your dentist will choose the design based on where the tooth sits and how you bite.
What Is A Metal-Supported Crown (PFM)?
A metal‑supported crown is usually a porcelain‑fused‑to‑metal (PFM) crown. It has a metal substructure for strength with a porcelain outer layer for tooth‑colored appearance. PFM crowns have a long clinical track record and are still used widely, especially where durability matters.
Because the core is metal, the crown can appear less translucent than natural enamel. If the gums recede over time, a thin dark line at the edge of the crown may become visible. This is mainly an aesthetic issue, but it can be a deciding factor for front teeth.
Zirconia Vs Metal-Supported Crowns: Key Differences
| Factor | Zirconia (“Zirconium”) Crown | Metal-Supported Crown (PFM) |
| Appearance | Naturally tooth‑colored and can reflect light; no metal margin at the gumline. | Tooth‑colored porcelain on top, but can look more opaque; metal edge may show if gums recede. |
| Strength Under Bite Force | Very strong and fracture‑resistant; monolithic designs are often chosen for molars and heavy bites. | Strong metal framework; porcelain veneer can chip in some cases. |
| Gumline Look Over Time | No gray line from metal; usually a cleaner gumline appearance. | Higher chance of a gray/dark line if gum tissue thins or recedes. |
| Allergy / Sensitivity | No metal; very low risk of material sensitivity. | Depends on the alloy; sensitivities can occur in a small number of patients (often nickel‑related). |
| Tooth Reduction | Often needs slightly less space than PFM, depending on the case and crown design. | May require more room for both metal and porcelain layers. |
| Best Fit For | Patients prioritizing aesthetics, gum harmony, or metal‑free dentistry; also common for molars when strength is needed. | Patients who want a proven option for back teeth or when a metal framework is preferred. |
Which Crown Is Best For Different Situations?

Front Teeth And Visible Areas
Zirconia is often chosen for front teeth because it avoids a metal edge and can look more natural at the gumline. If you have a thin gumline or a high smile line, this difference can be noticeable. For very high translucency needs, your dentist may consider a layered zirconia option.
Molars And Heavy Chewing Force
Both materials can work well on molars. Monolithic zirconia is frequently selected when maximum strength is needed, such as in patients who clench or grind. PFM can also be a solid choice, particularly when the bite is complex and a metal substructure offers predictable support.
Gum Recession Risk Or Dark Gumline Concerns
If you are prone to gum recession or you have had a dark crown margin in the past, zirconia may be the safer aesthetic bet. Metal‑supported crowns can look excellent at first, but recession can reveal the metal edge. Your dentist can also design margins to reduce visibility, yet the risk cannot be fully removed.
Metal Allergy Or Sensitivity History
If you have reacted to jewelry metals or have been told you have a nickel sensitivity, tell your dentist before choosing a crown. Zirconia is metal‑free and is often selected for patients who want to avoid metal alloys. When PFM is still preferred, your dentist can discuss high‑noble or nickel‑free alloy options.
Opposing Tooth Wear
Any crown material can contribute to wear if the bite is uneven or the surface is rough. With zirconia, careful polishing after bite adjustments helps reduce wear against the opposing tooth. Ask your dentist how the crown will be finished and checked after cementation.
Cost And Value Considerations

Fees vary by clinic, lab, and the complexity of the case, so it is rarely helpful to compare prices without an exam. Zirconia crowns can cost more because of material and lab processes, especially when advanced shading or layering is used. PFM crowns are often positioned as a cost‑effective option with a long history of use.
Value is not only about price. A crown that fits well, supports the bite, and is easy to keep clean can save you time and discomfort later. When you compare options, ask what is included in the fee, such as temporary crowns, follow‑up checks, and warranty policies.
Questions To Ask Your Dentist Before Choosing
- Which crown material fits my tooth position and bite pattern best?
- Do I show signs of clenching or grinding that should influence the material choice?
- How will you manage the gumline margin to keep it natural‑looking over time?
- Will the crown be monolithic zirconia, layered zirconia, or PFM, and why?
- What steps will you take to polish and adjust the crown so it is gentle on the opposing teeth?
- What is the expected lifespan for my situation, and what maintenance will help it last?
Frequently Asked Questions
Which Looks More Natural?
Zirconia crowns generally look more natural at the gumline because there is no metal underneath. That said, an experienced dentist and dental lab can make a PFM crown look very good, especially on back teeth. Shade matching and gum position are often more important than the material alone.
Do Metal-Supported Crowns Cause A Dark Line At The Gum?
They can. If the gumline recedes or thins, the metal margin may become visible as a gray or dark line. This is less common with zirconia because it has no metal substructure.
Which Is Stronger For Molars?
Both can be strong choices for molars. Monolithic zirconia offers high fracture resistance, while PFM benefits from a metal framework with decades of clinical use. Your dentist will consider your bite, tooth structure, and habits like grinding.
Is Zirconia A Good Option If I Have A Metal Allergy?
Zirconia is metal‑free, so it is commonly used when patients want to avoid metal alloys. True allergies to crown materials are uncommon, but sensitivities to certain dental metals can occur. If you have a known allergy, share it before treatment so the alloy choice can be adjusted.
Will A Zirconia Crown Wear Down The Opposing Tooth?
Polished zirconia is generally considered wear‑friendly, especially when the bite is balanced. Rough or heavily glazed surfaces can increase wear, which is why finishing and polishing matter. Follow‑up visits help your dentist fine‑tune the bite if needed.
How Long Do Crowns Last?
Crown lifespan depends on fit, bite forces, oral hygiene, and habits such as grinding. Many crowns last for years with good care, but no material is “lifetime.” Regular checkups help catch small issues before they become failures.
Prevent Sensitivity After Teeth Whitening
Prevent Sensitivity After Teeth Whitening: 5 Practical Ways
To reduce sensitivity after teeth whitening, start with a desensitizing toothpaste, avoid very hot, cold, and acidic foods for 24–48 hours, brush gently, and use fluoride to support enamel. If discomfort gets stronger, wakes you at night, or lasts longer than a week, pause whitening and speak with a dentist.
Whitening can brighten your smile quickly, but it can also leave teeth feeling “zingy” for a short time. That sensitivity is usually temporary, and most people can keep it mild with a few simple aftercare steps.
The key is to protect enamel while your teeth settle, and to avoid triggers that make nerves react. The tips below work for both in-office whitening and at-home kits, with one rule: follow your dentist’s or product’s instructions first.
Why Teeth Whitening Can Trigger Sensitivity
Most whitening products use peroxide-based ingredients that move through enamel and into the underlying tooth structure. During and shortly after whitening, the tooth can be more reactive to temperature and certain foods, which is why cold water or hot coffee may suddenly feel sharp.
Sensitivity tends to be more noticeable if you already have thin enamel, gum recession, worn fillings, or a history of sensitive teeth. Stronger gels and longer wear times can also increase the chance of discomfort.
5 Practical Ways To Reduce Sensitivity After Whitening
1. Use A Desensitizing Toothpaste Before And After Whitening

Choose a toothpaste made for sensitive teeth and use it for several days before whitening, then keep using it afterward. Many formulas rely on ingredients such as potassium nitrate, which helps calm the nerve response over time.
For an extra boost, you can smear a thin layer on the sensitive areas for a minute before rinsing (unless the label says otherwise). If you’re whitening with trays, ask your dentist whether a desensitizing gel is a good fit for you.
2. Avoid Extreme Temperatures And Acidic Foods For 24–48 Hours
Right after whitening, stick to lukewarm foods and drinks and keep acidic items to a minimum. Citrus, soda, vinegar-based dressings, and very spicy foods can irritate teeth that are already on edge.
This is also the window when teeth can re-stain more easily. If you can, choose lighter-colored options (water, milk, plain yogurt, rice, eggs, chicken, bananas) until the next day or two.
3. Brush Gently With A Soft-Bristled Toothbrush
A firm brush and heavy pressure can make sensitivity worse, especially if the gumline is exposed. Use a soft-bristled toothbrush and small circular motions, letting the bristles do the work.
If you floss, do it gently and avoid snapping the floss into the gums. A fluoride toothpaste is a good everyday choice because it supports enamel strength.
4. Add Fluoride Support (Rinse Or Gel)
Fluoride helps strengthen enamel and can reduce sensitivity for some people. An alcohol-free fluoride mouthwash is often easier to tolerate right after whitening than a strong, minty rinse.
If you’re prone to sensitivity, your dentist may suggest a fluoride or desensitizing gel to use in trays for a short period. This is a common option when you want whitening results without the sting.
5. Take A Break And See A Dentist If Sensitivity Is Intense

Mild sensitivity that fades within a couple of days is common. Pain that keeps getting worse, feels one-sided, or lingers long after a cold drink can signal a problem such as decay, a crack, or gum recession.
Stop whitening and book a dental check if you have strong pain, swelling, or symptoms that last longer than a week. A dentist can apply professional-strength fluoride, protective coatings, or adjust your whitening plan to something gentler.
Frequently Asked Questions
How Long Does Sensitivity Last After Teeth Whitening?
Most people notice sensitivity for a few hours to a few days. If it isn’t improving after several days, or it’s severe from the start, stop whitening and contact a dentist for advice.
Can I Eat Right After Teeth Whitening?
You can eat once you feel comfortable, but avoid very hot, cold, and acidic foods right away. For the first 24–48 hours, many dentists also recommend skipping strongly pigmented foods and drinks (coffee, red wine, berries) to protect the new shade.
How Long Does Desensitizing Toothpaste Take To Work?
Some people feel improvement within a few days, but best results usually come from consistent use for at least two weeks. If you’re whitening again later, start the toothpaste a few days before you begin.
Does Everyone Experience Sensitivity After Whitening?
No. Sensitivity varies from person to person and depends on enamel thickness, gum recession, existing restorations, and the strength and wear time of the whitening product. If you’ve had sensitivity in the past, a dentist-supervised approach can help you choose a gentler method.
Gum Health Before Laminate Veneers
Gum Health Before Getting Laminate Veneers
Before getting laminate veneers, your gums should be free of inflammation, bleeding, and active infection. Healthy gum tissue supports a natural gumline, helps veneers seat correctly, and reduces the risk of recession exposing veneer margins. A dentist will check your gums first and treat any problems before moving forward.
What Are Laminate Veneers?
Laminate veneers are thin shells—most commonly porcelain—bonded to the front surfaces of teeth to improve appearance. They are used to mask discoloration, close small gaps, and reshape teeth that look chipped, worn, or uneven.
Because veneers sit right at the gumline, they need a stable, healthy foundation. If the gums are inflamed or actively infected, the final fit and the long-term look of the veneers can suffer.
Why Gum Health Matters Before Veneers
Healthy gums frame the teeth and create a clean, even gumline—one of the details that makes veneers look natural. When gum tissue is swollen, tender, or bleeding, it becomes harder to take accurate impressions and place veneers precisely.
Good gum health before laminate veneers also supports durability. Reducing inflammation and plaque around the margins lowers the risk of recession, sensitivity, and decay near the veneer edges.
How Dentists Check Gum Health Before Veneer Placement
A gum evaluation is part of the planning stage for laminate veneers. Your dentist will look for signs that the gum tissue is stable enough for cosmetic work.
Typical checks include:
- Redness, swelling, tenderness, or visible inflammation
- Bleeding when brushing or during an exam
- Gum recession that could expose veneer margins
- Plaque and tartar (calculus) buildup around the gumline
- Periodontal pocket depths and, when needed, X-rays to assess bone support
If any concerns show up, treatment comes first. Once the gums are healthy and settled, the dentist can finalize shade selection, impressions, and the veneer design.
How Gum Disease Can Affect Laminate Veneer Results
Gum disease can range from gingivitis (early inflammation) to periodontitis (a deeper infection that can affect the supporting tissues). Placing veneers on unhealthy gums increases the chance of uneven margins, ongoing bleeding, and irritation.
Recession is a common aesthetic concern. If the gumline pulls back after veneers are placed, the edges may become visible, creating dark lines or gaps that distract from the smile.
Is Tartar Cleaning Necessary Before Laminate Veneers?
In most cases, yes. Professional cleaning removes tartar that can irritate gums and trigger bleeding. Cleaning also gives your dentist a clearer view of the gumline so veneer margins can be planned more accurately.
Some patients need a simple scale and polish, while others may need deeper cleaning if there is significant buildup. Your dentist will usually allow time for the gums to calm down before moving to final impressions.
Treatments That May Be Needed Before Veneers
The right preparation depends on your gum condition and overall oral health. Your dentist may recommend one or more of the following before starting veneer work:
- Treatment for gum infection: Managing inflammation and infection so the gumline is stable.
- Tartar removal and periodontal cleaning: Reducing calculus and plaque around the teeth and under the gums when needed.
- Gum recession management: Assessing whether coverage procedures or other options are appropriate for exposed areas.
- Gingivectomy or gingivoplasty: Reshaping gum contours for a more balanced smile when indicated.
- Orthodontic adjustments: Correcting alignment issues that could affect veneer thickness, bite, or symmetry.
These steps help create healthier tissue around the teeth and a cleaner surface for bonding, which supports both appearance and longevity.
What To Consider Before Getting Laminate Veneers

Laminate veneers can be a long-term cosmetic solution, but results depend on planning and maintenance. A few habits and decisions make the process smoother:
- Choose an experienced dentist: Look for a clinician who regularly performs cosmetic veneer cases and explains options clearly.
- Keep oral hygiene consistent: Brush twice daily, clean between teeth, and follow any gum-care instructions from your dentist.
- Attend routine checkups: Regular visits help monitor gum stability before, during, and after treatment.
- Limit smoking and heavy alcohol use: These habits can irritate gums and affect healing and long-term oral health.
If you notice bleeding, swelling, or persistent bad breath, address it before scheduling veneer placement. Healthy gums are not just an aesthetic detail—they support overall oral health.
Gum Health Before Getting Laminate Veneers FAQ
Why is gum health so important before getting laminate veneers?
It affects both the look and the lifespan of the veneers. Inflamed or bleeding gums can make placement less precise and increase the risk of recession showing veneer margins.
Can I get veneers if I have gum disease?
Yes, but treatment should come first. Veneers are typically planned only after gum disease is controlled and the gum tissue is stable.
Is tartar cleaning a must before laminate veneers?
For most people, yes. Removing tartar reduces gum irritation and helps your dentist plan the veneer margins on a cleaner, healthier gumline.
Can I get veneers if I have gum recession?
It depends on the cause and severity. Your dentist will assess whether the recession is stable and how it might affect veneer edges and overall aesthetics before recommending a plan.
