How Can Fear of The Dentist be Overcome?
How Can Fear Of The Dentist Be Overcome?
Fear of the dentist can be reduced by understanding what triggers your anxiety, choosing a dentist who explains each step, and using practical calming techniques before and during appointments. Modern pain-control methods, gradual exposure, and therapy such as CBT can help. For severe phobia, sedation may be an option after clinical assessment.
Table of Contents
Why Dental Fear Happens
Dental fear ranges from mild nervousness to dental phobia, where people avoid care even when they are in pain. It often builds after one bad experience, but it can also develop without a clear trigger.
Common triggers include:
- Past painful or distressing treatment experiences.
- Expectation of pain based on old beliefs, social media, or stories from friends and family.
- Feeling a loss of control while lying back in the chair.
- Embarrassment or shame about oral health, especially after delayed checkups.
- Sensitivity to sounds, smells, or the sight of dental instruments.
Signs And Symptoms Of Dental Phobia
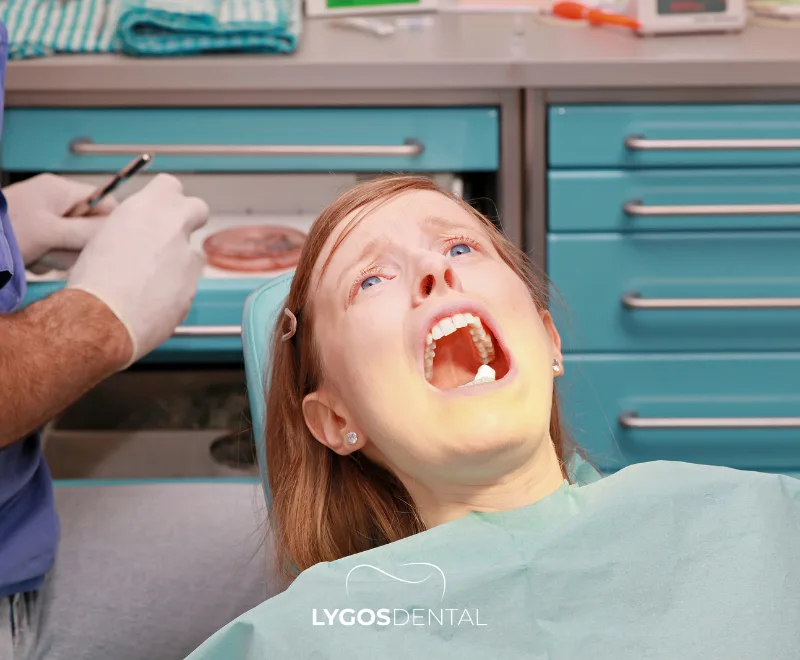
Dental anxiety can show up in the body, in thoughts, and in behavior. When it starts affecting sleep, daily life, or keeps you from seeking care, it is worth addressing directly.
- Nausea, sweating, trembling, or a racing heartbeat before an appointment.
- Panic-like feelings in the waiting room or when sitting in the chair.
- Repeatedly canceling or postponing visits.
- Avoiding the dentist even as tooth or gum problems get worse.
- Difficulty sleeping because you are anticipating treatment.
How Dental Anxiety Starts In Children
Many adult fears begin early. A child’s first dental visits, and the way adults talk about dentistry, can shape long-term attitudes toward care.
In children, fear often develops from:
- Parental anxiety or negative comments about dentists.
- A painful first experience or a rushed appointment.
- Arriving without preparation, so the child does not know what to expect.
- Using the dentist as a threat (for example, “If you misbehave, you’ll go to the dentist”).
Supportive language, short introductory visits, and a calm parent in the room can prevent fear from taking hold. If a child is very anxious, ask the dental team about child-friendly approaches and pacing.
Practical Ways To Reduce Dental Anxiety

What you do before the appointment often matters as much as what happens in the chair.
Before your visit
- Choose a dentist who is comfortable treating anxious patients and is willing to answer questions.
- Book an early-day appointment so you spend less time anticipating it.
- Ask for a step-by-step explanation and agree on a stop signal (such as raising your hand).
- Avoid caffeine on the day of the visit if it increases your jitters.
- Practice slow breathing for a few minutes before you arrive.
During treatment
- Use paced breathing: inhale through the nose, exhale slowly through the mouth.
- Bring headphones or listen to calming audio if the clinic allows it.
- Ask for short breaks so you do not feel trapped.
- Tell the dentist where you feel sensitive; numbing can be adjusted.
Evidence-based psychological approaches
For persistent or severe anxiety, psychological strategies can make a lasting difference, especially when paired with a supportive dental team.
- Cognitive Behavioral Therapy (CBT): helps reframe catastrophic thoughts and builds coping skills.
- Graded exposure: gradual steps such as a clinic visit, a short exam, then a simple procedure.
- Relaxation training: breathwork, progressive muscle relaxation, or brief mindfulness exercises.
- Desensitization: getting used to triggers like the sound of instruments in a controlled way.
Modern Options That Make Treatment More Comfortable
Dentistry has changed a lot. Many clinics now use techniques that reduce discomfort and shorten treatment time, which can be reassuring if you have had older, painful experiences.
Examples you can ask about include:
- Laser dentistry for selected procedures, which may reduce noise and vibration compared with traditional drilling.
- Needle-free anesthetic systems offered by some clinics for certain cases (availability varies).
- Digital impressions with 3D scanners instead of traditional impression trays.
Sedation And General Anesthesia

When fear is intense, sedation can help you get essential care while staying calmer. Your dentist will review your medical history and explain benefits and risks before recommending any option.
Common approaches
- Sedation: you remain responsive but deeply relaxed, and you may remember little of the procedure.
- General anesthesia: you are fully asleep; it is typically reserved for specific situations and requires an appropriately equipped setting and qualified professionals.
If you are considering sedation or general anesthesia, discuss the plan in detail, including monitoring, recovery time, and whether you will need someone to take you home.
When To Get Extra Support
If you avoid dental care for years, have panic attacks, or feel unable to sit through even an exam, consider asking for help beyond self-management. A dentist experienced with anxious patients, a therapist, or both can work together so you can receive care without feeling overwhelmed.
Frequently Asked Questions
How do I get over my fear of the dentist?
Use gradual exposure, discuss fears, choose a gentle dentist, and practice relaxation techniques.
How do you treat dental fear?
Treat with education, behavioral therapy, desensitization, supportive communication, and sedation when appropriate.
What phobia is the fear of dentists?
Dental phobia is called odontophobia.
Is it common to be scared of the dentist?
Yes, dental anxiety is common, affecting many children and adults.
What can I take to calm my nerves before a dentist?
Ask your dentist about nitrous oxide or a prescribed anxiolytic; avoid alcohol.
Things You Need to Know Before Getting Braces
Things You Need To Know Before Getting Braces
Braces straighten teeth and improve how your bite works, which can make cleaning easier and reduce uneven wear over time. Before starting, you’ll need an orthodontic exam to confirm the problem, choose the right appliance (metal, ceramic, lingual, or clear aligners), and treat any cavities or gum issues. Good hygiene and regular checkups are key to a smooth result.
A straight smile isn’t only about appearance. When teeth and jaws don’t line up well, you may be more prone to plaque buildup, gum irritation, or uneven tooth wear. Orthodontic treatment can address both cosmetic and functional concerns, but it works best when you know what to expect from day one.
Who Can Get Braces

Braces can be an option for children, teens, and adults. What matters most is your dental development, jaw alignment, and overall oral health. An orthodontist will check your teeth, gums, and bite, then recommend a plan that matches your needs and lifestyle.
Braces are commonly recommended for:
- Children (often when most adult teeth have erupted, commonly around ages 9–14)
- Teenagers
- Adults of any age
- People with healthy teeth and a stable jaw structure
- Patients whose gums are free from active disease
When Braces Are Recommended
Orthodontic treatment is used to correct bite problems and alignment issues. Some people start for cosmetic reasons, but many cases also have a functional goal—helping the teeth meet properly and reducing strain on certain teeth or jaw areas.
Common reasons an orthodontist may recommend braces include:
- Crowded, rotated, or misaligned teeth
- Gaps between teeth (diastema)
- Bite problems such as open bite, deep bite, crossbite, or underbite
- Protruding or recessed front teeth
- Wear patterns linked to an uneven bite
- Changes related to habits such as thumb-sucking or long-term mouth breathing
Types Of Braces
There are several orthodontic options today. The best choice depends on how complex your case is, how visible you want the appliance to be, and whether you can follow daily wear instructions for removable systems.
Metal Braces
The classic option. Metal brackets are durable, effective for a wide range of cases, and often the most budget-friendly choice.
Ceramic (Clear) Braces
Tooth-colored brackets that are less noticeable than metal. They can be a good fit for adults who want a subtler look, though they may require a bit more care to avoid staining.
Lingual Braces
Placed on the back of the teeth, so they’re hidden from view. They can be helpful for people who want an invisible option, but they may take longer to get used to and can be harder to clean.
Clear Aligners (For Example, Invisalign®)
Removable trays that gradually move teeth. They’re discreet and can be easier for brushing and flossing, but they only work well when you wear them as directed and attend regular follow-ups. They’re typically best for mild to moderate corrections.
How Long Braces Treatment Takes
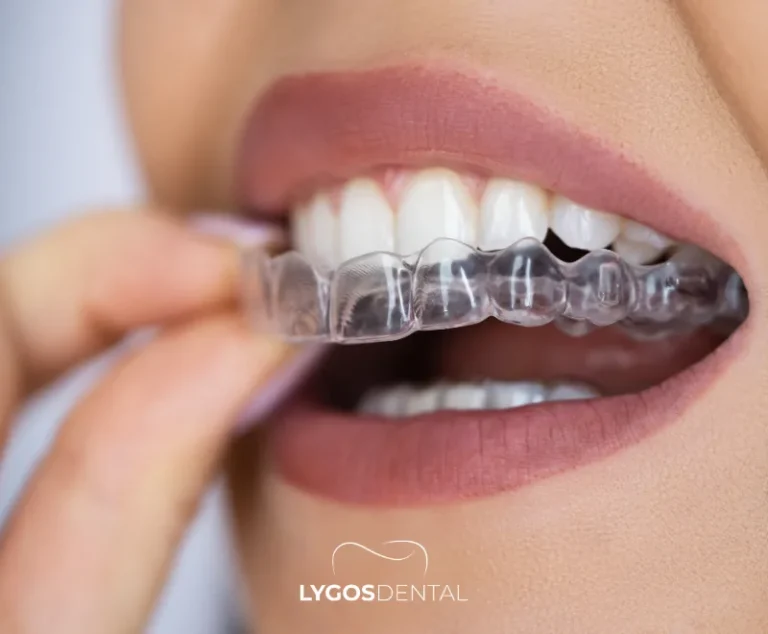
Treatment time varies from person to person. Your orthodontist will estimate a timeline after reviewing your bite, the amount of movement needed, and your overall dental health.
Typical ranges are:
- Mild cases: about 6–12 months
- Moderate cases: about 12–18 months
- More complex cases: 24 months or longer
What can affect the timeline:
- Age and how your teeth respond to movement
- Severity of crowding or bite problems
- Keeping appointments for adjustments or new aligners
- Daily habits, including oral hygiene and following wear instructions
Checklist Before Your Braces Go On
Starting with a healthy mouth makes treatment easier and lowers the risk of complications. Your dentist or orthodontist may coordinate a few steps before placement.
- Professional cleaning to remove plaque and tartar
- Treating cavities before brackets or aligners begin
- Addressing gum inflammation or periodontal issues
- Planning for diet changes (hard, sticky, and crunchy foods can damage brackets and wires)
- Setting expectations: mild soreness is common in the first days, and progress takes time
Caring For Braces After Placement

Daily care plays a major role in how your teeth look when the braces come off. Good hygiene helps prevent white spot lesions, cavities, and gum irritation during treatment.
- Brush carefully after meals and before bed; take extra time around brackets and the gumline
- Use interdental brushes, floss threaders, or a water flosser to clean between teeth
- Avoid foods that can bend wires or break brackets (ice, hard nuts, sticky candy, chewing gum)
- Attend scheduled adjustment visits so your orthodontist can keep teeth moving safely
- If you play contact sports, wear a mouthguard designed for braces
If you feel sore after an adjustment, soft foods and orthodontic wax can help. Over-the-counter pain relief may be an option if it’s safe for you—follow label directions and your clinician’s advice.
Frequently Asked Questions
Does getting braces hurt?
You won’t feel pain while they’re being placed. It’s normal to feel pressure or soreness for a few days afterward and after adjustments. Most people adapt within a week.
Should cavities be treated before getting braces?
Yes. Cavities and active gum problems should be treated first. Braces make some areas harder to clean, so starting with healthy teeth lowers the risk of decay during treatment.
What affects the cost of braces?
Price depends on the type of appliance, how long treatment lasts, case complexity, and where you receive care. Clear aligners and lingual braces tend to cost more than standard metal braces in many clinics.
Will braces affect my speech?
Traditional braces usually cause minimal speech changes. You may notice a short adjustment period with lingual braces or clear aligners, but most people adapt quickly with practice.
How Does Diet Affect Dental Health?
How Does Diet Affect Dental Health?
Diet affects dental health by changing how often your teeth face acid attacks and whether your body gets the minerals and vitamins needed to maintain enamel and healthy gums. Sugary and acidic foods feed bacteria and lower mouth pH, raising cavity risk—especially with frequent snacking. Calcium, phosphorus, vitamin D, and vitamin C support stronger teeth and gum tissue.
Oral health is closely tied to everyday eating and drinking habits. The foods you choose, the drinks you sip, and how often you snack all influence enamel strength, saliva flow, and the bacteria that cause tooth decay. Small changes at the table can make a noticeable difference at the dentist.
What Is The Relationship Between Diet And Dental Health?

Teeth are living structures supported by minerals and nutrients from your diet. Enamel relies on a steady supply of calcium and phosphorus, while vitamin D helps your body absorb and use these minerals effectively. Gum tissue benefits from vitamin C and protein, which support collagen and healing.
Food timing matters as much as food choice. Each time you eat or drink something with fermentable carbs (like sugar or refined starch), bacteria can produce acids that soften enamel. When you graze throughout the day, your mouth gets less recovery time, so enamel stays under stress longer.
How Do Sugary Foods Harm Teeth?
Mouth bacteria thrive on sugar. As they break it down, they release acids that pull minerals out of enamel. Over time, repeated acid exposure can lead to white spots, sensitivity, and cavities.
Some options are tougher on teeth because they combine sugar with acidity or stickiness. Sodas, sports/energy drinks, sweetened iced teas, and packaged fruit juices can bathe teeth in acid. Sticky sweets, dried fruit, and chewy candies cling to enamel and keep fueling bacteria.
Why Snacking Frequency Matters

It’s not only the amount of sugar—it’s the number of times teeth are exposed. Frequent snacking keeps mouth pH low for longer periods. Saliva needs time to neutralize acids and start remineralizing enamel.
If you snack, keep it structured. Aim for tooth-friendlier options and avoid slowly sipping sweet drinks over hours. Water between meals helps rinse away food particles and supports a healthier pH balance.
Foods And Drinks That Support Dental Health
A tooth-supportive diet focuses on minerals, vitamins, and foods that stimulate saliva.
- Dairy or fortified alternatives (milk, yogurt, cheese): calcium and phosphorus to support enamel.
- Leafy greens (spinach, kale): minerals plus antioxidants.
- Eggs and oily fish (salmon, sardines): vitamin D and protein.
- Nuts, beans, and lean meats: phosphorus, protein, zinc, and iron to support oral tissues.
- Crunchy produce (apples, carrots, celery): fiber that helps mechanically clean teeth and boosts saliva.
- Water: rinses the mouth and helps dilute acids.
Can Poor Nutrition Lead To Dental Problems?
Yes. Diets low in key nutrients can weaken enamel and reduce the mouth’s ability to repair itself. Low vitamin D or calcium intake may affect mineral support for teeth, while low vitamin C can make gums more prone to bleeding and slower to heal.
When protein intake is consistently low, immune defenses can suffer, which may increase the risk of oral infections. Iron and zinc deficiencies may also be linked with mouth sores or altered taste in some people.
Children, older adults, and people with restricted diets benefit from extra attention to nutrient intake and regular dental checkups.
Which Foods Should Be Limited For Gum Health?
Gum health depends on stable blood flow, low inflammation, and good daily plaque control. Certain foods and drinks can make that harder by increasing acid exposure or promoting plaque buildup.
Try to limit:
- Acidic drinks such as soda, cola, energy drinks, and frequent citrus juices.
- Refined carbohydrates (white bread, chips, crackers, cookies) that break down into sugars quickly.
- Sticky sweets and frequent grazing on sugary snacks.
- Very salty processed foods that can contribute to dry mouth in some people.
Severe gum disease has been associated with chronic conditions like diabetes and cardiovascular disease, so protecting gum health is part of looking after overall wellbeing.
What Should You Eat For Healthy Teeth?

Brushing and flossing are essential, but diet helps set the baseline for how resilient your teeth and gums are. A practical approach is to build meals around nutrient-dense foods and keep sugary exposure predictable and limited.
A tooth-friendly plate often includes:
- Calcium-rich foods (milk, yogurt, cheese, calcium-fortified alternatives).
- Vitamin D sources (egg yolks, salmon, sardines, fortified foods) to support calcium use.
- Vitamin C sources (citrus, kiwi, berries, bell peppers) to support gum tissue.
- Fiber-rich fruits and vegetables to boost saliva and reduce food residue.
- Water as the default drink.
If you want something sweet, having it with a meal is usually better than nibbling over a long period. Afterward, rinse with water. If brushing isn’t possible right away, sugar-free gum (especially xylitol-sweetened) can stimulate saliva.
Simple Daily Habits That Protect Your Mouth
- Keep sweet drinks occasional, and avoid sipping them slowly over time.
- Choose snacks that don’t cling to teeth (cheese, nuts, plain yogurt, fresh fruit).
- Wait 30 minutes after acidic foods or drinks before brushing to avoid brushing softened enamel.
- If you have dry mouth, speak with a dentist or doctor—medications and dehydration can play a role.
How Does Diet Affect Dental Health? Frequently Asked Questions
Does Diet Really Affect Tooth Decay?
Yes. Tooth decay is driven by repeated acid exposure created when bacteria metabolize sugars and refined carbs. Higher frequency of sugary or acidic foods and drinks increases risk, especially when oral hygiene and fluoride exposure are limited.
Which Vitamins And Minerals Are Most Important For Dental Health?
Calcium and phosphorus help maintain enamel, and vitamin D supports how your body uses those minerals. Vitamin C supports gum tissue and healing. Vitamin A and several B vitamins also play roles in oral tissue health and immune function.
Are “Sugar-Free” Snacks Always Safe For Teeth?
Not always. Some sugar-free products still contain fermentable starches that can turn into acids in the mouth. Look for snacks that are low in added sugars and don’t stick to teeth. If chewing gum, xylitol-sweetened options are generally considered tooth-friendlier.
How Much Water Should I Drink For Better Oral Health?
Hydration needs vary by body size, activity, and climate. Many public health guidelines suggest roughly 6–8 cups of fluids a day for most adults, and a useful rule of thumb is aiming for pale yellow urine. From an oral health perspective, choosing water often—and using it to rinse after meals—helps reduce acid and food residue.
How Do Dairy Products Help Teeth?
Milk, yogurt, and cheese provide calcium and phosphorus, which help maintain enamel mineral balance. Cheese can also stimulate saliva, supporting a healthier mouth pH after eating.
Is Fluoride Toothpaste Harmful?
Is Fluoride Toothpaste Harmful?
Fluoride toothpaste is considered safe for most people when used as directed. It strengthens enamel, helps reverse early decay, and lowers cavity risk. Problems usually come from frequent swallowing or long-term excessive fluoride exposure, which can cause mild dental fluorosis in young children. Use the right amount for age and spit after brushing.
Oral health is closely linked to overall health, and fluoride toothpaste is one of the most widely used tools for preventing tooth decay. Still, you may have seen concerns online about fluoride’s safety. The real question isn’t whether fluoride exists in toothpaste, but whether it’s used in the right way and dose.
What Is Fluoride?

Fluoride is a naturally occurring mineral found in water, soil, and some foods. In dentistry, it’s valued because it helps the outer layer of the tooth (enamel) resist acid attacks from plaque bacteria and sugar.
Does Fluoride Toothpaste Work?
Yes. Research consistently shows that brushing with fluoride toothpaste reduces cavities. Fluoride supports remineralization (repair of early enamel damage) and makes enamel more resistant to future demineralization.
Over-the-counter toothpastes commonly contain about 1,000–1,500 ppm fluoride, a range considered effective for cavity prevention.
Benefits Of Fluoride Toothpaste

Strengthens tooth enamel
Fluoride integrates with enamel and helps it withstand acids produced after eating or drinking sugary foods.
Helps prevent cavities
By slowing demineralization and supporting repair, fluoride lowers the chance that early weak spots develop into cavities.
Supports remineralization
Early enamel changes can often be stabilized when fluoride is available regularly through brushing.
May reduce sensitivity in some formulas
Certain fluoride toothpastes are designed to help protect exposed areas, which can reduce sensitivity for some people.
What Are The Risks Of Too Much Fluoride?
Like many helpful ingredients, fluoride can cause problems when intake is excessive. With toothpaste, the main risk is repeated swallowing by young children or very frequent use of high‑fluoride products without professional guidance.
Dental fluorosis
During tooth development (typically in early childhood), swallowing too much fluoride over time can lead to dental fluorosis. Mild fluorosis often appears as faint white streaks or spots and is mainly cosmetic.
Stomach upset from swallowing toothpaste
Swallowing large amounts of toothpaste at once may cause nausea, vomiting, or stomach pain. This is one reason adult supervision matters for young children.
High‑fluoride toothpaste without dental advice
Prescription-strength toothpastes may contain much higher fluoride levels (for example, 5,000 ppm) and are intended for people at higher cavity risk. These should be used only when recommended by a dentist.
Is Fluoride Toothpaste Safe For Children?

In general, yes—when the amount matches the child’s age and brushing is supervised. Many dental and public health bodies advise using fluoride toothpaste from the eruption of the first tooth, while focusing on minimizing swallowing.
Recommended amount by age
- Under age 3: use a smear the size of a grain of rice.
• Ages 3–6: use no more than a pea-sized amount.
• Under age 2: ask your dentist or doctor for guidance, especially if your child is likely to swallow toothpaste.
Practical tips for parents
Help your child brush, keep toothpaste out of reach between uses, and encourage spitting rather than rinsing and swallowing. If your child repeatedly swallows toothpaste, speak with a pediatric dentist about the best approach for your situation.
How To Use Fluoride Toothpaste Safely
- Use the right amount. More foam doesn’t mean better cleaning.
- Brush twice daily for about two minutes and spit out afterward.
- Supervise young children to prevent swallowing.
- Check the label for fluoride concentration. For everyday cavity protection, many products are in the 1,000–1,500 ppm range.
- Ask your dentist before using high‑fluoride products or if you have a history of frequent cavities.
Bottom Line
Fluoride toothpaste is not harmful for most people when used correctly. It remains one of the simplest, best-supported ways to protect enamel and reduce cavities. The key is dosage—especially for young children—and using higher-strength products only under professional guidance.
Frequently Asked Questions
What is fluoride toothpaste?
Fluoride toothpaste contains fluoride compounds that help strengthen enamel and reduce the risk of tooth decay when used regularly.
Is fluoride toothpaste harmful?
Not when used as directed. The main concerns involve swallowing toothpaste frequently (especially in young children) or using high‑fluoride products without dental advice.
Can children use fluoride toothpaste?
Yes, with age-appropriate amounts and adult supervision. Use a rice-grain smear under age 3 and a pea-sized amount from ages 3–6.
What happens if too much fluoride is ingested?
Over time, excess swallowed fluoride in early childhood can cause dental fluorosis. Swallowing a large amount at once can also cause stomach upset.
Does Nighttime Teeth Grinding Break Teeth?
Does Nighttime Teeth Grinding Break Teeth?
Yes—nighttime teeth grinding (sleep bruxism) can damage teeth over time. Repeated clenching and grinding may wear down enamel, create small cracks, and break dental work like fillings or crowns. In more severe cases, teeth can chip or fracture. Early signs and a dentist‑made night guard can help prevent permanent damage.
What Nighttime Teeth Grinding Is

Nighttime teeth grinding is a form of bruxism that happens during sleep. Many people aren’t aware they do it until a partner hears grinding sounds or a dentist notices wear.
Sleep bruxism can range from occasional clenching to frequent grinding episodes. When it happens regularly, the jaw muscles and teeth absorb forces that are higher and longer-lasting than normal chewing.
Can Sleep Bruxism Crack Or Break Teeth?
It can. Repeated pressure can flatten biting surfaces, expose dentin, and make teeth more sensitive. Over time, that stress may lead to enamel cracks, chips, or fractures—especially if a tooth already has a large filling or a weak cusp.
Bruxism can also damage dental work. Fillings may loosen or crack, crowns can chip, and veneers may fail. If you’ve invested in restorative work, protecting it is a big reason to address grinding early.
Signs You Might Be Grinding At Night
Sleep bruxism often shows up through symptoms rather than obvious awareness. Common signs include:
- Jaw or facial muscle soreness when you wake up
- Morning headaches, especially around the temples
- Tooth sensitivity (hot, cold, or sweet)
- Flattened, chipped, or worn-looking teeth
- Pain or pressure near the ears
- A partner hearing grinding or clicking sounds during sleep
Common Causes And Risk Factors

Bruxism doesn’t have a single cause. For many people, several factors stack together.
Stress and anxiety
High stress can increase clenching, both during the day and at night. People often notice flare-ups during busy periods or after major life changes.
Sleep disruption
Sleep problems such as snoring or obstructive sleep apnea may be linked with sleep bruxism. If you also wake up tired, gasp, or snore loudly, it’s worth mentioning to a clinician.
Bite and dental factors
A misaligned bite, missing teeth, or poorly fitting restorations can contribute to jaw strain in some cases. Your dentist can assess whether your bite needs adjustment.
Medications and health conditions
Certain medications and neurological conditions have been associated with bruxism. If grinding started after a medication change, discuss it with the prescribing clinician rather than stopping it on your own.
What To Do If You Suspect Bruxism

Start with a dental exam. Dentists look for wear patterns, cracks, gum recession, and changes in the jaw muscles.
Treatment is usually aimed at protecting teeth and reducing triggers. A plan may include:
- A custom night guard (occlusal splint) to separate the teeth and reduce damage
- Repairing cracked teeth or worn restorations before they worsen
- Jaw relaxation exercises or physical therapy when muscle pain is present
- Stress management strategies if tension is a major trigger
- Evaluation for sleep apnea when symptoms point in that direction
Prevention And Self‑Care Tips
You can’t always stop sleep bruxism on willpower alone, but you can reduce the load on your teeth and jaw.
- Avoid chewing gum and limit very hard or chewy foods if your jaw feels tired.
- Cut back on caffeine and alcohol in the evening if you notice they worsen clenching.
- Build a wind-down routine: warm shower, light stretching, or slow breathing.
- Use heat on sore jaw muscles for 10–15 minutes before bed.
- If you wake with jaw tension, try gentle jaw opening and side-to-side movements—no force.
Frequently Asked Questions
Can nighttime teeth grinding cause gum problems?
It can contribute. Grinding may accelerate gum recession in some people, especially if there’s existing inflammation or aggressive brushing. A dentist can tell whether recession is linked to bruxism, brushing habits, or gum disease.
Does nighttime teeth grinding happen in children?
Yes. It can be seen in children and often improves as they grow. If a child has tooth wear, jaw pain, or disturbed sleep, a pediatric dentist can guide next steps.
Should a night guard be worn every night?
If your dentist prescribed one for sleep bruxism, consistent use offers the best protection. Your dentist can also check the fit over time and replace it if it wears down.
Can bruxism cause headaches?
Yes. Many people with sleep bruxism report morning headaches or tightness in the temples due to overworked jaw muscles.
Can bruxism be cured?
Some cases settle when triggers change, while others need long-term management. Even when grinding continues, protecting teeth and addressing contributing factors usually reduces damage and symptoms.
How to Get Rid of Bad Breath?
How To Get Rid Of Bad Breath
Bad breath is most often caused by bacteria on teeth, gums, and the tongue. Brush and floss daily, clean your tongue, stay hydrated, and treat dry mouth. If odor persists for more than a couple of weeks or comes with bleeding gums, reflux, or sinus symptoms, book a dental or medical check-up to find the root cause.
What Causes Bad Breath

Halitosis usually starts in the mouth, but it can also be linked to the nose, throat, or digestive system. Common triggers include:
- Poor oral hygiene: Plaque, trapped food particles, and an unclean tongue allow odor-producing bacteria to build up.
- Dry mouth (xerostomia): Low saliva makes it easier for bacteria and sulfur compounds to linger.
- Gum disease and cavities: Inflamed gums, tartar, and untreated decay can create a persistent odor.
- Tonsil stones, sinusitis, or postnasal drip: Mucus and debris can feed bacteria and cause a strong smell.
- Smoking and alcohol: Both dry the mouth and leave odor-causing residues.
- Diet and fasting: Garlic/onions, low-carb diets, and long gaps between meals can change breath chemistry.
- Reflux: Stomach acid or regurgitation can contribute to unpleasant breath in some people.
Fast Ways To Improve Breath Today
If you need a same-day reset, these steps help most people:
- Brush for two minutes, then floss (or use interdental brushes) to remove trapped debris.
- Clean your tongue from back to front with a tongue scraper or the bristles of your toothbrush.
- Drink water and rinse your mouth; repeat if you’ve had coffee, alcohol, or a dry-mouth spell.
- Chew sugar-free gum (xylitol is a good option) to stimulate saliva.
- Use an alcohol-free, antibacterial mouthwash as a short-term boost.
Daily Oral Care Routine That Prevents Bad Breath
Consistency matters more than any single product. Aim for:
- Brush twice daily: Focus on the gumline and the back molars; brush before bed without rushing.
- Floss once daily: Odor often comes from between teeth where a toothbrush can’t reach.
- Clean your tongue daily: Most odor-causing compounds come from the tongue’s surface.
- Hydrate and manage dry mouth: Sip water, limit alcohol, and ask your dentist about dry-mouth sprays or lozenges if needed.
- See a dentist regularly: Professional cleanings and early treatment of gum disease make a noticeable difference.
Home Remedies That Are Worth Trying

Home remedies can help as add-ons, but they won’t replace brushing, flossing, and dental care.
- Saltwater rinse: A gentle rinse can freshen the mouth and soothe irritated gums.
- Baking soda rinse: May neutralize acids and reduce odor; avoid overuse if it irritates your mouth.
- Parsley or mint: Useful for short-term freshness, especially after meals.
- Green tea: Supports oral hygiene and can reduce sulfur-like odors for some people.
- Plain yogurt or other probiotic foods: May help if digestive imbalance is contributing to odor.
Foods That Help And Foods That Make It Worse
Breath changes with what you eat and how often you eat.
Breath-Friendly Foods
- Crunchy fruits and vegetables (apples, carrots, cucumbers) to stimulate saliva and reduce plaque.
- Plain yogurt and fermented foods for probiotics.
- Water, especially between meals and after coffee.
Common Triggers
- Garlic, onions, and heavily spiced meals (odor can persist for hours).
- Sugary snacks and frequent sipping of sweet drinks (feeds bacteria).
- Alcohol and tobacco (drying effect and residue).
- Very low-carb diets or prolonged fasting (can lead to ketone-related breath).
When Bad Breath Signals A Health Issue

If you’re doing the basics well and the odor doesn’t improve, it’s worth looking beyond brushing. Possible contributors include ongoing sinus infection/postnasal drip, untreated gum disease, reflux, or poorly controlled diabetes. Serious causes are uncommon, but persistent halitosis should be checked rather than ignored.
When To See A Dentist Or Doctor
Book an appointment if you notice any of the following:
- Bad breath that lasts more than 2–3 weeks despite good oral care.
- Bleeding gums, gum swelling, loose teeth, or tooth pain.
- A coated tongue that returns quickly, or a persistent bad taste.
- Frequent heartburn, sour taste, or regurgitation.
- Ongoing congestion, facial pressure, or postnasal drip.
- Unexplained weight loss, fever, or other systemic symptoms.
Frequently Asked Questions
Is morning breath normal?
Yes. Saliva drops during sleep, so odor often increases overnight. Brushing, flossing, and tongue cleaning in the morning usually resolves it.
What’s the best natural option?
A tongue scraper plus hydration is often the most effective “natural” approach. Herbs like parsley can help short term, but they don’t remove the underlying bacterial film.
Does mouthwash cure bad breath?
Mouthwash can reduce odor temporarily, but it won’t fix cavities, gum disease, or dry mouth. Choose alcohol-free formulas if dryness is a problem.
Can stomach problems cause bad breath?
Sometimes. Reflux can contribute to odor, but most cases start in the mouth. If you have frequent heartburn or regurgitation, speak to a clinician.
How to Close Gaps Between Teeth (Diastema)?
How To Get Rid Of Bad Breath
Bad breath is most often caused by bacteria on teeth, gums, and the tongue. Brush and floss daily, clean your tongue, stay hydrated, and treat dry mouth. If odor persists for more than a couple of weeks or comes with bleeding gums, reflux, or sinus symptoms, book a dental or medical check-up to find the root cause.
What Causes Bad Breath

Halitosis usually starts in the mouth, but it can also be linked to the nose, throat, or digestive system. Common triggers include:
- Poor oral hygiene: Plaque, trapped food particles, and an unclean tongue allow odor-producing bacteria to build up.
- Dry mouth (xerostomia): Low saliva makes it easier for bacteria and sulfur compounds to linger.
- Gum disease and cavities: Inflamed gums, tartar, and untreated decay can create a persistent odor.
- Tonsil stones, sinusitis, or postnasal drip: Mucus and debris can feed bacteria and cause a strong smell.
- Smoking and alcohol: Both dry the mouth and leave odor-causing residues.
- Diet and fasting: Garlic/onions, low-carb diets, and long gaps between meals can change breath chemistry.
- Reflux: Stomach acid or regurgitation can contribute to unpleasant breath in some people.
Fast Ways To Improve Breath Today
If you need a same-day reset, these steps help most people:
- Brush for two minutes, then floss (or use interdental brushes) to remove trapped debris.
- Clean your tongue from back to front with a tongue scraper or the bristles of your toothbrush.
- Drink water and rinse your mouth; repeat if you’ve had coffee, alcohol, or a dry-mouth spell.
- Chew sugar-free gum (xylitol is a good option) to stimulate saliva.
- Use an alcohol-free, antibacterial mouthwash as a short-term boost.
Daily Oral Care Routine That Prevents Bad Breath
Consistency matters more than any single product. Aim for:
- Brush twice daily: Focus on the gumline and the back molars; brush before bed without rushing.
- Floss once daily: Odor often comes from between teeth where a toothbrush can’t reach.
- Clean your tongue daily: Most odor-causing compounds come from the tongue’s surface.
- Hydrate and manage dry mouth: Sip water, limit alcohol, and ask your dentist about dry-mouth sprays or lozenges if needed.
- See a dentist regularly: Professional cleanings and early treatment of gum disease make a noticeable difference.
Home Remedies That Are Worth Trying
Home remedies can help as add-ons, but they won’t replace brushing, flossing, and dental care.
- Saltwater rinse: A gentle rinse can freshen the mouth and soothe irritated gums.
- Baking soda rinse: May neutralize acids and reduce odor; avoid overuse if it irritates your mouth.
- Parsley or mint: Useful for short-term freshness, especially after meals.
- Green tea: Supports oral hygiene and can reduce sulfur-like odors for some people.
- Plain yogurt or other probiotic foods: May help if digestive imbalance is contributing to odor.
Foods That Help And Foods That Make It Worse
Breath changes with what you eat and how often you eat.
Breath-Friendly Foods
- Crunchy fruits and vegetables (apples, carrots, cucumbers) to stimulate saliva and reduce plaque.
- Plain yogurt and fermented foods for probiotics.
- Water, especially between meals and after coffee.
Common Triggers
- Garlic, onions, and heavily spiced meals (odor can persist for hours).
- Sugary snacks and frequent sipping of sweet drinks (feeds bacteria).
- Alcohol and tobacco (drying effect and residue).
- Very low-carb diets or prolonged fasting (can lead to ketone-related breath).
When Bad Breath Signals A Health Issue

If you’re doing the basics well and the odor doesn’t improve, it’s worth looking beyond brushing. Possible contributors include ongoing sinus infection/postnasal drip, untreated gum disease, reflux, or poorly controlled diabetes. Serious causes are uncommon, but persistent halitosis should be checked rather than ignored.
When To See A Dentist Or Doctor
Book an appointment if you notice any of the following:
- Bad breath that lasts more than 2–3 weeks despite good oral care.
- Bleeding gums, gum swelling, loose teeth, or tooth pain.
- A coated tongue that returns quickly, or a persistent bad taste.
- Frequent heartburn, sour taste, or regurgitation.
- Ongoing congestion, facial pressure, or postnasal drip.
- Unexplained weight loss, fever, or other systemic symptoms.
Frequently Asked Questions
Is morning breath normal?
Yes. Saliva drops during sleep, so odor often increases overnight. Brushing, flossing, and tongue cleaning in the morning usually resolves it.
What’s the best natural option?
A tongue scraper plus hydration is often the most effective “natural” approach. Herbs like parsley can help short term, but they don’t remove the underlying bacterial film.
Does mouthwash cure bad breath?
Mouthwash can reduce odor temporarily, but it won’t fix cavities, gum disease, or dry mouth. Choose alcohol-free formulas if dryness is a problem.
Can stomach problems cause bad breath?
Sometimes. Reflux can contribute to odor, but most cases start in the mouth. If you have frequent heartburn or regurgitation, speak to a clinician.
How Does Using a Tongue Cleaner Affect Dental Health?
How Does Using A Tongue Cleaner Affect Dental Health?
Using a tongue cleaner removes the bacteria and debris that sit on the tongue’s surface, especially toward the back. This can noticeably improve bad breath, support a healthier balance of oral bacteria, and reduce the load that contributes to plaque and gum irritation. It takes seconds and works best as a daily habit.
Brushing and flossing do most of the heavy lifting, but the tongue also holds a large share of oral bacteria. When that layer builds up, it can feed bad breath and spread microbes back onto teeth and gums. Tongue cleaning is a simple add-on that can sharpen your routine without adding much time.
What Is A Tongue Cleaner?

A tongue cleaner (often called a tongue scraper) is an oral care tool designed to lift and remove the coating on the tongue. That coating is a mix of bacteria, dead cells, food particles, and saliva proteins. Most cleaners are plastic, stainless steel, or silicone, and the head is curved to match the tongue’s shape.
Many toothbrushes can reach the tongue, but they are not built for scraping. A dedicated cleaner usually removes the coating more efficiently with fewer passes, which can feel gentler for many people.
How To Use A Tongue Cleaner
Technique matters more than force. Aim for a few light, controlled strokes rather than pressing hard.
- Rinse the cleaner with water before you start.
- Stick out your tongue and place the cleaner toward the back (stop if you gag—start a little further forward and work back over time).
- Glide the cleaner forward to the tip of your tongue.
- Rinse the tool under running water after each stroke.
- Repeat 2–5 times, until the surface looks clearer.
- Rinse your mouth with water. Use mouthwash afterward if it’s part of your routine.
- Wash the cleaner and let it dry fully before storing.
How Tongue Cleaning Supports Oral And Dental Health
Helps reduce bad breath
The back of the tongue often harbors anaerobic bacteria that release volatile sulfur compounds. These compounds are a major driver of morning breath and persistent halitosis. Regular tongue cleaning reduces the bacterial layer where those odors start.
May reduce plaque transfer
Bacteria don’t stay in one place. A coated tongue can re-seed microbes onto teeth, which may contribute to plaque buildup over time. Tongue cleaning helps lower that reservoir and supports a cleaner baseline between brushing sessions.
Supports gum comfort
Lowering overall bacterial load can help reduce irritation triggers in the mouth. Tongue cleaning is not a treatment for gum disease, but it can complement brushing, flossing, and professional cleanings.
Can improve taste
A heavy tongue coating can dull taste buds. When the surface is cleaner, many people notice flavors more clearly, especially after waking up.
Choosing The Most Effective Tongue Cleaner

The “best” option is the one you will use consistently and comfortably. Material and design affect feel, durability, and ease of cleaning.
Stainless steel
Durable, easy to wash thoroughly, and typically provides firm scraping in one or two passes. Choose rounded edges and a shape that fits your tongue width.
Plastic
Lightweight and inexpensive. Replace it if the edge warps, roughens, or develops cracks where bacteria can hide.
Silicone or soft-tipped designs
A good fit for sensitive tongues or people who are new to scraping. They may require a few extra passes compared with firmer scrapers.
Brush-style tongue cleaners
These combine bristles with a scraping edge or textured pad. They can be comfortable, but models without a scraper often leave more coating behind.
Common Mistakes To Avoid
- Using too much pressure, which can cause soreness or tiny cuts.
- Only cleaning the front of the tongue. The back often needs the most attention.
- Skipping tool hygiene. Rinse well and let it dry to limit bacterial growth.
- Sharing a cleaner. Treat it like a toothbrush—one person only.
- Overdoing it. Once a day is enough for most people.
Where Tongue Cleaning Fits In A Daily Routine
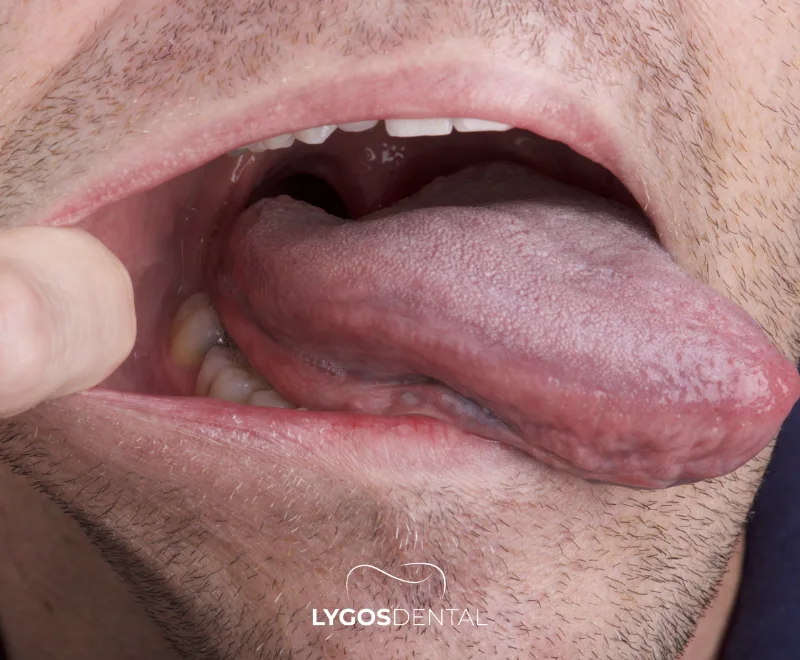
Most people prefer using a tongue cleaner in the morning, when overnight bacteria and dryness make the coating more noticeable. You can do it before brushing or after brushing—either is fine as long as you are consistent. If you have persistent bad breath, a second gentle clean later in the day can help.
When To Speak With A Dentist
If bad breath persists despite brushing, flossing, and tongue cleaning, it may be linked to gum disease, dry mouth, tonsil stones, sinus issues, or digestive causes. Also ask for advice if you have a painful tongue, sores that do not heal, or a coating that does not improve with routine care.
Frequently Asked Questions
Is it really necessary to use a tongue cleaner?
It’s not mandatory, but it can make a noticeable difference for breath and overall oral cleanliness. The tongue holds a large amount of bacteria, and a quick daily clean can reduce that buildup.
How often should I use a tongue cleaner?
Once a day is enough for most people. If you are managing stubborn bad breath, you can use it twice daily as long as you stay gentle.
Is brushing the tongue with a toothbrush enough?
It can help, but toothbrush bristles often smear the coating instead of lifting it. A tongue cleaner is shaped to scrape the surface efficiently.
Can tongue cleaning replace brushing or flossing?
No. Tongue cleaning supports your routine, but brushing and flossing are still the core habits for preventing cavities and gum disease.
Smile Design Prices
How Does Using A Tongue Cleaner Affect Dental Health?
Using a tongue cleaner removes the bacteria and debris that sit on the tongue’s surface, especially toward the back. This can noticeably improve bad breath, support a healthier balance of oral bacteria, and reduce the load that contributes to plaque and gum irritation. It takes seconds and works best as a daily habit.
Brushing and flossing do most of the heavy lifting, but the tongue also holds a large share of oral bacteria. When that layer builds up, it can feed bad breath and spread microbes back onto teeth and gums. Tongue cleaning is a simple add-on that can sharpen your routine without adding much time.
What Is A Tongue Cleaner?

A tongue cleaner (often called a tongue scraper) is an oral care tool designed to lift and remove the coating on the tongue. That coating is a mix of bacteria, dead cells, food particles, and saliva proteins. Most cleaners are plastic, stainless steel, or silicone, and the head is curved to match the tongue’s shape.
Many toothbrushes can reach the tongue, but they are not built for scraping. A dedicated cleaner usually removes the coating more efficiently with fewer passes, which can feel gentler for many people.
How To Use A Tongue Cleaner
Technique matters more than force. Aim for a few light, controlled strokes rather than pressing hard.
- Rinse the cleaner with water before you start.
- Stick out your tongue and place the cleaner toward the back (stop if you gag—start a little further forward and work back over time).
- Glide the cleaner forward to the tip of your tongue.
- Rinse the tool under running water after each stroke.
- Repeat 2–5 times, until the surface looks clearer.
- Rinse your mouth with water. Use mouthwash afterward if it’s part of your routine.
- Wash the cleaner and let it dry fully before storing.
How Tongue Cleaning Supports Oral And Dental Health
Helps reduce bad breath
The back of the tongue often harbors anaerobic bacteria that release volatile sulfur compounds. These compounds are a major driver of morning breath and persistent halitosis. Regular tongue cleaning reduces the bacterial layer where those odors start.
May reduce plaque transfer
Bacteria don’t stay in one place. A coated tongue can re-seed microbes onto teeth, which may contribute to plaque buildup over time. Tongue cleaning helps lower that reservoir and supports a cleaner baseline between brushing sessions.
Supports gum comfort
Lowering overall bacterial load can help reduce irritation triggers in the mouth. Tongue cleaning is not a treatment for gum disease, but it can complement brushing, flossing, and professional cleanings.
Can improve taste
A heavy tongue coating can dull taste buds. When the surface is cleaner, many people notice flavors more clearly, especially after waking up.
Choosing The Most Effective Tongue Cleaner
The “best” option is the one you will use consistently and comfortably. Material and design affect feel, durability, and ease of cleaning.
Stainless steel
Durable, easy to wash thoroughly, and typically provides firm scraping in one or two passes. Choose rounded edges and a shape that fits your tongue width.
Plastic
Lightweight and inexpensive. Replace it if the edge warps, roughens, or develops cracks where bacteria can hide.
Silicone or soft-tipped designs
A good fit for sensitive tongues or people who are new to scraping. They may require a few extra passes compared with firmer scrapers.
Brush-style tongue cleaners
These combine bristles with a scraping edge or textured pad. They can be comfortable, but models without a scraper often leave more coating behind.
Common Mistakes To Avoid

- Using too much pressure, which can cause soreness or tiny cuts.
- Only cleaning the front of the tongue. The back often needs the most attention.
- Skipping tool hygiene. Rinse well and let it dry to limit bacterial growth.
- Sharing a cleaner. Treat it like a toothbrush—one person only.
- Overdoing it. Once a day is enough for most people.
Where Tongue Cleaning Fits In A Daily Routine
Most people prefer using a tongue cleaner in the morning, when overnight bacteria and dryness make the coating more noticeable. You can do it before brushing or after brushing—either is fine as long as you are consistent. If you have persistent bad breath, a second gentle clean later in the day can help.
When To Speak With A Dentist
If bad breath persists despite brushing, flossing, and tongue cleaning, it may be linked to gum disease, dry mouth, tonsil stones, sinus issues, or digestive causes. Also ask for advice if you have a painful tongue, sores that do not heal, or a coating that does not improve with routine care.
Frequently Asked Questions
Is it really necessary to use a tongue cleaner?
It’s not mandatory, but it can make a noticeable difference for breath and overall oral cleanliness. The tongue holds a large amount of bacteria, and a quick daily clean can reduce that buildup.
How often should I use a tongue cleaner?
Once a day is enough for most people. If you are managing stubborn bad breath, you can use it twice daily as long as you stay gentle.
Is brushing the tongue with a toothbrush enough?
It can help, but toothbrush bristles often smear the coating instead of lifting it. A tongue cleaner is shaped to scrape the surface efficiently.
Can tongue cleaning replace brushing or flossing?
No. Tongue cleaning supports your routine, but brushing and flossing are still the core habits for preventing cavities and gum disease.
What is Apical Resection?
What Is Apical Resection?
Apical resection (apicoectomy) is a minor dental surgery that removes infected tissue and a small portion of the root tip when a tooth still has inflammation after root canal treatment. By sealing the end of the root and clearing the infection, the procedure can preserve the natural tooth and protect nearby bone and gums.
Meta Title: Apical Resection (Apicoectomy): What It Is, When It’s Needed, and Recovery
Meta Description: Learn what apical resection (apicoectomy) is, why it’s done after a failed root canal, how the surgery works, key benefits and risks, and what to expect during recovery and follow-up care.
What is apical resection?
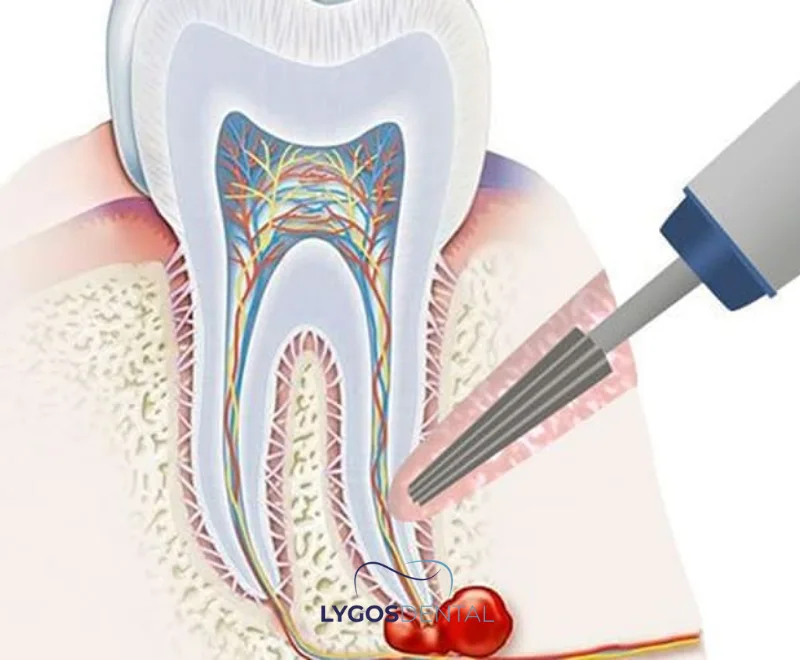
Apical resection is a surgical endodontic procedure used to treat infection at the tip of a tooth root. It’s most often recommended when root canal treatment has already been completed, but the root-end area still shows persistent inflammation, pain, or a recurring abscess. The aim is straightforward: remove the infected tissue and seal the root tip so bacteria can’t keep leaking into the surrounding bone.
Dentists may also call this procedure an apicoectomy. With modern imaging and magnification, it can be carried out with high precision, which improves comfort and predictability for many patients.
When is apical resection recommended?
Your dentist or oral and maxillofacial surgeon may suggest apical resection when non-surgical options aren’t likely to solve the problem. This usually happens after a root canal that cannot be retreated effectively, or when the root anatomy and existing restorations make retreatment risky.
Common reasons include
- A persistent infection or cyst at the root tip after root canal treatment
- Blocked canals (for example, from a post, calcification, or complex anatomy) that prevent adequate retreatment
- A fracture or small defect near the root end that needs direct access
- A root filling that cannot be cleaned or replaced without damaging a crown or bridge
- A desire to keep the natural tooth when extraction is the main alternative
How the procedure is performed
Apical resection is typically done under local anesthesia. After numbing the area, the clinician makes a small incision in the gum and creates a window in the bone to reach the root tip. Inflamed tissue is removed, and a small portion of the root end is trimmed.
The end of the root is then cleaned and sealed with a biocompatible filling material to reduce the chance of reinfection. Finally, the gum is stitched back in place. Most appointments take about 30–60 minutes, depending on which tooth is treated and how complex the root structure is.
Benefits of apical resection
The main advantage is tooth preservation. Keeping your natural tooth can support chewing function, bite stability, and appearance—especially in the front of the mouth. For many patients, apical resection provides a practical “second chance” for a tooth that would otherwise be removed.
Key benefits
- Avoids extraction in suitable cases
- Stops infection from spreading into surrounding bone and tissues
- Can relieve ongoing pain, swelling, or recurrent gum boils
- Often faster and less invasive than replacing the tooth with an implant or bridge
- Helps maintain natural aesthetics and normal bite forces
Risks and possible complications
Like any surgical procedure, apical resection has potential risks. Most are uncommon and manageable, especially when the case is well planned and postoperative instructions are followed.
Possible complications
- Temporary pain, swelling, bruising, or mild bleeding in the first few days
- Infection or delayed healing
- Numbness or tingling (rare), depending on the tooth and nearby nerves
- Sinus involvement when upper back teeth are treated (uncommon)
- Failure to resolve the infection, which may still lead to extraction
Recovery and aftercare
Most patients return to normal routines within a day or two, but the surgical site needs time to heal. Discomfort is usually mild to moderate and can be managed with the medications your clinician recommends. Stitches are commonly removed about 7–10 days after the procedure, unless dissolvable sutures are used.
Practical tips for a smoother recovery
- Use an ice pack for the first 24 hours (10–15 minutes on, then off) to help limit swelling
- Choose soft foods and avoid chewing on the treated side for a few days
- Brush and floss normally, but be gentle around the incision
- Avoid smoking and alcohol while healing, as they can slow recovery
- Take prescribed antibiotics or pain relievers exactly as directed
Contact your dental office if you have heavy bleeding, worsening swelling after the first couple of days, fever, or pain that isn’t improving.
Apical resection vs. extraction

Apical resection is usually considered when the tooth can still be saved and has enough healthy structure to function long term. If the tooth is cracked below the gum line, has severe bone loss, or cannot be restored properly, extraction may be the safer choice. Your clinician will weigh prognosis, costs, timeline, and your overall oral health before recommending the best option.
Frequently asked questions
Is apical resection painful?
The surgery itself is performed under local anesthesia, so you shouldn’t feel pain during the procedure. Soreness afterward is common and typically improves over a few days with appropriate pain relief.
How long does apical resection take?
Most procedures take 30–60 minutes, though complex roots or difficult access can extend the appointment.
How long does healing take?
Initial gum healing usually happens within 7–10 days. Bone healing around the root tip takes longer and is monitored at follow-up visits, often with X-rays.
Can any tooth have apical resection?
Not always. Accessibility, root shape, proximity to nerves or the sinus, and the tooth’s overall restorability all affect suitability. A clinical exam and imaging are needed to confirm whether it’s a good option.
What’s the success rate?
Many cases do well when the tooth is properly selected and the root end can be sealed effectively. Your dentist can give a realistic prognosis based on the tooth involved, existing restoration, and the size of the lesion.
