How to Care for Dentures?
How To Care For Dentures
Clean dentures every day by rinsing after meals, brushing with a soft denture brush and non‑abrasive cleanser, and soaking as directed. Handle them over a towel or water-filled sink to prevent breakage. Remove dentures at night unless your dentist advises otherwise, and keep your gums, tongue, and any natural teeth clean too.
Dentures can restore chewing, speech, and smile confidence after tooth loss. They also need routine care because plaque and food debris can build up on the surface just like on natural teeth. A few consistent habits make dentures more comfortable, reduce odour, and help them last longer.
What Dentures Are
Dentures are removable dental appliances that replace missing teeth. Full dentures replace all teeth in the upper or lower jaw, while partial dentures fill gaps and clip to remaining natural teeth. Some dentures are supported by implants, which can improve stability but may require extra attention around attachments.
Who Might Need Dentures
- Adults who have lost teeth due to decay or gum disease.
- People who have lost teeth after trauma.
- Patients born with missing teeth or tooth development issues.
- Anyone whose missing teeth affect function, comfort, or appearance.
Why Denture Care Matters
Poor denture hygiene can lead to bad breath, gum irritation, and infections such as denture-related stomatitis (often linked to yeast). It can also cause staining, unpleasant taste, and faster wear of the denture material. Regular cleaning and correct storage help maintain fit and reduce the risk of sores.
How Often To Clean Dentures
Aim to clean dentures at least morning and night, and rinse after meals to remove loose food. Night-time cleaning is especially useful because plaque and bacteria can build up during the day. If you use denture adhesive, clean off leftover adhesive daily so it doesn’t harden and trap bacteria.
Step-by-step: How To Clean Dentures
Remove them carefully. Take dentures out gently. Clean them over a folded towel or a sink partly filled with water to protect them if they slip.
Rinse first. Rinse under running water to remove food particles. Use cool to lukewarm water—very hot water can warp some materials.
Brush all surfaces. Use a soft denture brush and a non‑abrasive denture cleanser (or mild soap if recommended). Brush the teeth surfaces, the gum-coloured base, and the grooves that sit against your gums.
Rinse thoroughly. Rinse well before putting dentures back in your mouth. Never use denture cleansers while dentures are in the mouth.
Soak when needed. Soak dentures in water or a denture-soaking solution as directed by the product and your dentist. Many dentures need to stay moist to keep their shape.
Products That Are Safe For Dentures
Choose products designed for denture materials, and follow the manufacturer’s instructions for soaking time and use.
- Soft denture brush (or a soft toothbrush used only for dentures).
- Non‑abrasive denture cleanser, cream, paste, or tablets.
- Denture-soaking solution or plain water for overnight storage (as advised).
- Interdental brushes, floss threaders, or water flossers for implant-supported dentures—use the tools your dental team recommends.
Common Mistakes To Avoid
- Using regular toothpaste or abrasive powders (they can scratch dentures and attract more plaque).
- Cleaning with bleach or harsh chemicals (they may weaken materials or discolor the denture).
- Soaking in very hot water (can distort or warp some dentures).
- Scrubbing with hard-bristled brushes (can create surface damage).
- Wearing dentures overnight without guidance (may increase irritation and infection risk).
- Skipping checkups (fit can change over time as gums and bone remodel).
Night-time Routine And Storage
Most people should remove dentures at night to give the gums time to rest, unless their dentist recommends otherwise. After cleaning, store dentures in water or the recommended soaking solution so they don’t dry out. If your dentures have metal parts, ask your dentist which solutions are safe to avoid tarnishing.
Don’t Forget Your Mouth

Even with full dentures, your mouth still needs daily care. Gently brush your gums, tongue, and the roof of your mouth with a soft toothbrush to remove plaque and stimulate circulation. If you have natural teeth, clean them with fluoride toothpaste and floss daily.
When To See A Dentist
Book a dental visit if dentures feel loose, rub, or cause sores, or if you notice persistent bad breath despite cleaning. Also seek advice if you develop red, inflamed tissue under the denture or a burning sensation—these can be signs of infection or an allergy. Regular reviews help ensure fit, comfort, and safe cleaning habits.
Frequently Asked Questions
Is daily denture cleaning really necessary?
Yes. Daily brushing and rinsing reduces plaque, odour, and infection risk. Combine mechanical brushing with soaking as directed for the best results.
Can I use regular toothpaste on my dentures?
Usually no. Many toothpastes are abrasive and can scratch denture surfaces. Use a denture-specific cleanser or a mild soap recommended by your dental professional.
Can I sleep with dentures in?
Many dentists advise removing dentures overnight to reduce irritation and infection risk. Follow your dentist’s guidance if you’ve been told to wear them for a specific reason.
How long do dentures last?
With good care, many dentures last about 5 to 10 years, but they may need relining, adjustments, or replacement as your mouth changes over time.
What Is an Ectopic Tooth?
What Is An Ectopic Tooth? Symptoms, Causes, And Treatment
An ectopic tooth is a tooth that develops or erupts outside its normal path, such as a canine or wisdom tooth that comes in at an unusual angle or in the wrong spot. It may cause crowding, pain, swelling, or damage to nearby teeth, but some cases are found only on X‑rays. Treatment ranges from monitoring to orthodontic guidance or surgical removal.
What Is An Ectopic Tooth?
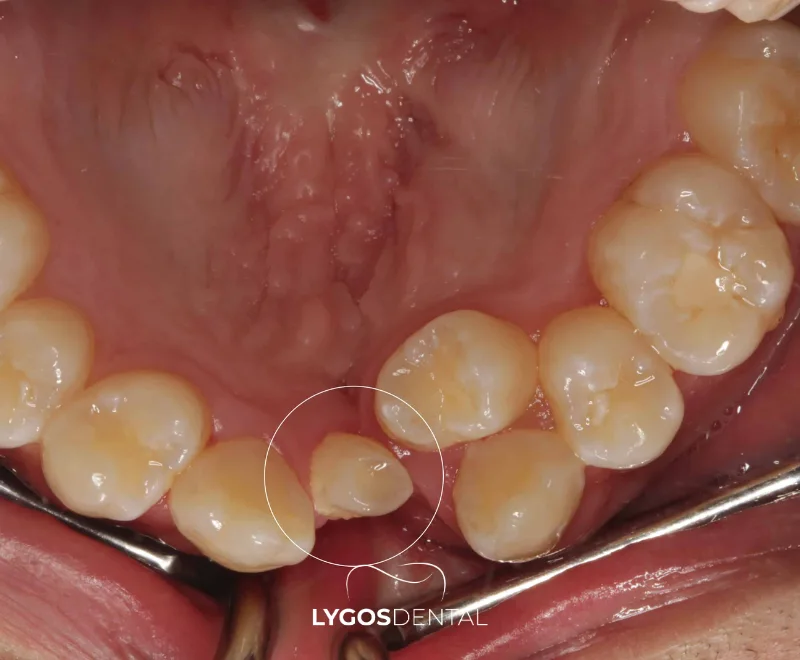
An ectopic tooth is a tooth that erupts in an abnormal position instead of its expected place in the dental arch. It may sit outside the jawbone’s normal eruption pathway, remain trapped in the bone, or emerge in the gum at an unusual angle. Ectopic eruption is most often discussed in relation to maxillary (upper) canines and third molars, but any tooth can be affected.
Why Do Ectopic Teeth Happen?
Ectopic eruption usually has more than one cause. In many people, the issue is local—space, timing, or guidance problems during tooth development—rather than one single trigger.
Common Risk Factors
- Crowding or lack of space in the jaw, especially when the dental arch is narrow.
- Genetics and family history of impacted or ectopic teeth.
- Early loss of baby teeth or delayed shedding, which can alter the eruption path of permanent teeth.
- Abnormal tooth size, shape, or position of the developing tooth bud.
- Trauma or infection affecting the jaw or developing teeth during childhood.
At What Age Are Ectopic Teeth Usually Found?
Many cases are identified in childhood or early adolescence, when permanent teeth are erupting and orthodontic checks are common. A frequent window for detection is roughly ages 7 to 14, particularly for upper canines. Wisdom teeth may be discovered later, often between ages 17 and 25, especially when they become symptomatic or show up on imaging.
Symptoms Of Ectopic Teeth

Symptoms depend on where the tooth is located and whether it is erupting into the mouth or remains impacted. Some people have no symptoms and only learn about the problem during a routine dental exam or X‑ray.
Possible Signs
- A tooth erupting in an unexpected spot or at an unusual angle.
- Crowding, shifting, or gaps as neighboring teeth are pushed out of position.
- Gum swelling, tenderness, or recurrent inflammation around the area.
- Jaw pressure, facial discomfort, or pain that comes and goes.
- Chewing difficulty or bite changes if the tooth interferes with normal contact.
Problems Ectopic Teeth Can Cause
Left unmanaged, ectopic teeth can create both cosmetic and functional issues. The main concern is damage to surrounding structures, including adjacent tooth roots and supporting bone.
Potential Complications
- Increased crowding and bite problems that may worsen over time.
- Root resorption of neighboring teeth in some impacted canine cases.
- Cysts associated with impacted teeth (such as dentigerous cysts) in a small number of patients.
- Repeated gum infection or inflammation if the tooth partially erupts and traps bacteria.
- Jaw or sinus-related symptoms in rare cases where a tooth is displaced into an unusual anatomical space.
How Dentists Diagnose An Ectopic Tooth
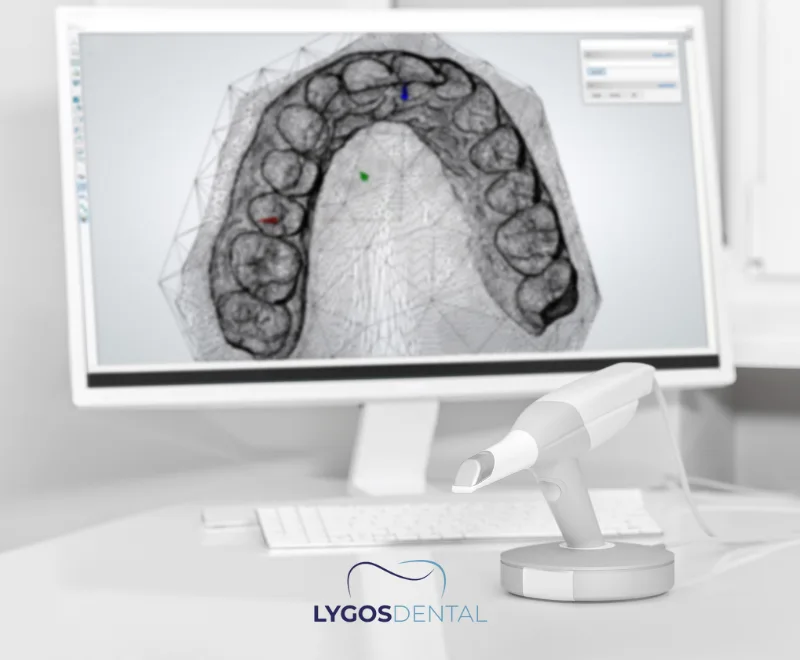
Diagnosis starts with a clinical exam, but imaging is often needed to confirm the tooth’s exact position. Dentists commonly use panoramic X‑rays, and may recommend CBCT (3D imaging) when surgical planning or complex anatomy is involved.
Treatment Options
Treatment depends on the tooth involved, its position, your age, and whether there is a risk of harm to nearby teeth. Many plans aim to prevent complications first, then restore function and alignment.
Orthodontic Guidance
If there is enough space and the tooth can be guided into place, orthodontic treatment may help move it into the correct position. This approach is often considered for ectopic upper canines, especially when detected early.
Surgical Exposure Or Removal
When the tooth is too far from its normal path, or when it poses a risk to nearby teeth, a dentist or oral surgeon may recommend surgery. Options include surgical exposure (sometimes combined with braces) or extraction for teeth that cannot be repositioned safely.
Monitoring
If the ectopic tooth is fully impacted, symptom-free, and not threatening nearby structures, careful monitoring can be appropriate. This usually involves periodic imaging and review to watch for changes such as cyst formation or pressure effects.
Frequently Asked Questions
How do you know if you have an ectopic tooth?
Some people notice a tooth coming in out of place, swelling, or crowding. Others have no symptoms, and the tooth is found on routine X‑rays or orthodontic scans.
Can an ectopic tooth fix itself?
Occasionally a mildly misdirected tooth improves as space is created, but many cases do not self-correct. Early dental assessment is the safest way to avoid complications.
Do ectopic teeth always need to be removed?
No. If the tooth can be guided into position or if it is stable and not causing harm, removal may not be necessary. Your dentist will base the plan on imaging and risk.
What specialist treats ectopic teeth?
General dentists can diagnose ectopic eruption, but orthodontists and oral surgeons often manage treatment, especially for impacted canines or wisdom teeth.
What Is Sinus Lifting?
What Is Sinus Lifting? Why Is It Done?
Sinus lifting (a sinus lift) is a bone‑grafting procedure used before dental implants in the back of the upper jaw. The surgeon raises the sinus membrane and places graft material to create enough bone height for a stable implant. It’s recommended when bone has thinned after tooth loss or when the sinus is too close to the implant site.
What Is Sinus Lifting?
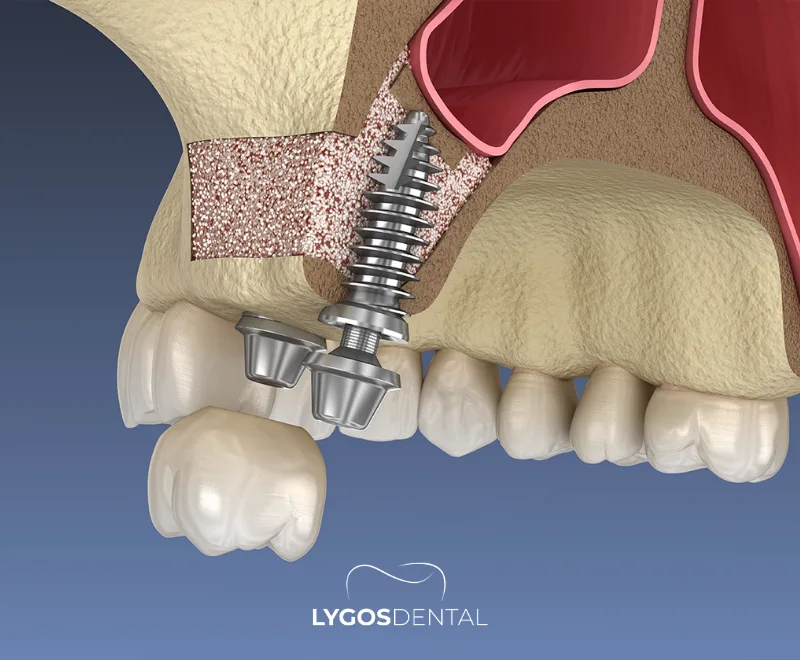
Sinus lifting is a surgical technique that increases bone volume in the posterior (back) part of the upper jaw so dental implants can be placed safely. The maxillary sinus is an air‑filled space above the upper molars and premolars. After tooth loss, the jawbone in this area can shrink and the sinus can expand downward, leaving too little bone for an implant.
During a sinus lift, the surgeon creates space by elevating the sinus membrane (also called the Schneiderian membrane) and filling the area with bone graft material. Over time, new bone forms around the graft, creating the height and density needed for long‑term implant stability.
Why Is Sinus Lifting Done?
A sinus lift is recommended when there is not enough native bone to anchor an implant in the upper back jaw. Common reasons include long‑standing tooth loss, bone resorption, and natural anatomy where the sinus sits close to the gum line.
The goal is to improve implant support and reduce the risk of implant failure. Your clinician typically confirms the need for sinus lifting with a clinical exam and 3D imaging (often a CBCT scan) to measure bone height and sinus position.
How Is Sinus Lifting Performed?
Sinus lifting is usually performed under local anesthesia, and sedation may be offered for comfort. The exact steps vary by technique, but the procedure generally includes careful access to the sinus, gentle elevation of the membrane, placement of graft material, and closure with sutures.
In some cases, an implant can be placed in the same appointment if there is enough existing bone to secure initial stability. When bone is very thin, the graft is placed first and the implant is inserted after healing.
Open vs Closed Sinus Lifting: What’s The Difference?
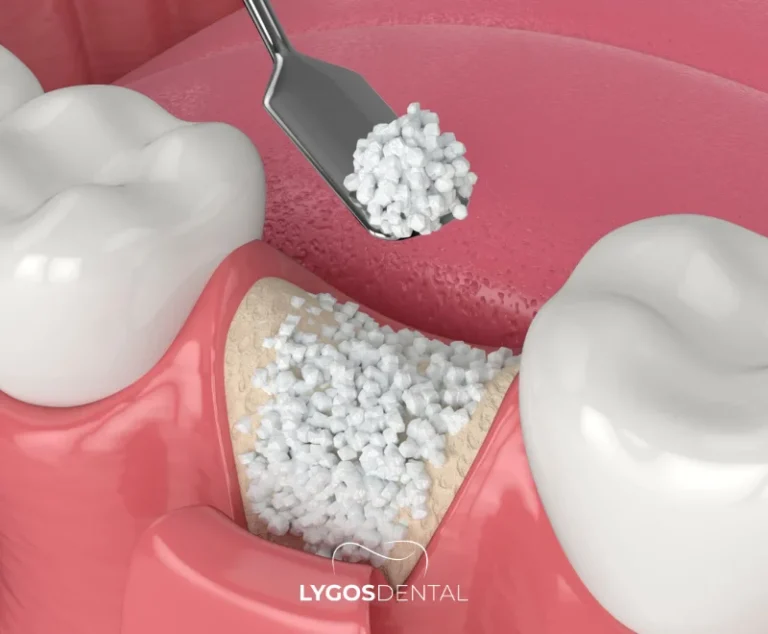
Open sinus lift (lateral window technique)
This approach is used when bone height is significantly reduced and more graft volume is needed. The surgeon creates a small window in the side of the upper jaw to access the sinus membrane directly. Implant placement is often delayed until the graft has matured.
Closed sinus lift (crestal approach)
This method is suitable when bone loss is mild to moderate and only a small lift is required. The membrane is elevated through the implant site as the implant socket is prepared. It is less invasive and implants are frequently placed in the same session, depending on bone quality.
What To Consider Before And After Surgery
Before the procedure
Share your full medical history, medications, and any allergies with your oral surgeon or implant dentist. Smoking can slow healing and increase complication risk, so stopping before surgery is strongly advised. If you have sinus symptoms or an active infection, treatment may need to be postponed until it resolves.
After the procedure
Avoid blowing your nose, forceful sneezing (sneeze with your mouth open), and heavy lifting for the period your surgeon recommends. Take prescribed antibiotics or pain relief exactly as directed, and keep the surgical area clean using the oral hygiene routine provided.
Stick to soft foods and avoid very hot or hard items in the first days. Contact your clinic promptly if you develop increasing swelling, fever, persistent bleeding, or a bad taste or discharge that worsens.
Recovery Time And Healing
Initial soft‑tissue healing typically takes about 7–10 days, which is when sutures are often removed if non‑resorbable stitches were used. Some swelling, mild pain, and bruising are common in the first few days and usually respond well to prescribed medication.
Bone maturation takes longer. Most patients need roughly 4–6 months for the graft to integrate before implant placement (or before the implant is fully loaded), though timelines vary based on graft type, technique, and individual healing.
Possible Risks And How They’re Managed

Sinus lifting is a well‑established procedure, but it remains delicate because the sinus membrane is thin. The most common intra‑operative issue is a membrane tear; when it occurs, surgeons can often repair it and continue or reschedule implant placement depending on severity.
Other potential risks include infection, sinus congestion, graft movement, or sinusitis. Choosing an experienced clinician, following aftercare instructions, and attending follow‑up visits helps keep risks low.
Frequently Asked Questions
Who needs sinus lifting?
It is most often recommended for people who want implants in the upper molar or premolar region but do not have enough bone height. This can happen after tooth loss, periodontal bone loss, or due to naturally large sinuses.
Is sinus lifting painful?
The procedure is performed with anesthesia, so you should not feel pain during surgery. Soreness afterward is common and is usually controlled with prescribed pain relief and cold compresses in the first 24–48 hours.
When can implants be placed after a sinus lift?
If there is adequate bone for initial implant stability, implants may be placed at the same time as the lift. When bone height is very limited, many clinicians wait about 4–6 months for graft integration before placing the implant.
How long does the procedure take?
Many sinus lift procedures take around 30–60 minutes, depending on whether the approach is open or closed and how much grafting is required. Your clinic can give a more accurate estimate after imaging and examination.
What should I avoid after surgery?
Avoid actions that increase sinus pressure, such as nose blowing, using straws, or strenuous exercise until your clinician says it is safe. Smoking should be avoided during healing because it can compromise blood flow and slow bone formation.
Orthodontics During Adolescence
Orthodontics During Adolescence
Orthodontic treatment during adolescence is often faster and more predictable because the jaws are still growing and most permanent teeth have erupted. Treatments like braces or clear aligners can improve bite function, support easier cleaning, and boost confidence. Many teens begin between ages 10 and 14, while an early orthodontic evaluation is commonly recommended around age 7.
Why orthodontic treatment matters in adolescence

Adolescence is a high-growth period for the jaws and face. When orthodontic problems are addressed at this stage, tooth movement can be more efficient and the results are easier to stabilize.
Orthodontic care is not only about aesthetics. Correcting alignment and bite issues can also support clearer speech, more comfortable chewing, and better long-term gum and tooth health.
Common reasons teens need orthodontics
- Crowded or overlapping teeth that are hard to clean, raising the risk of cavities and gum inflammation.
- Narrow, misaligned, or asymmetrical jaws that can affect chewing, speech, and facial balance.
- Overbite, underbite, crossbite, or open bite that can increase uneven tooth wear over time.
- Mouth-breathing and some oral habits that may influence dental and facial development.
- Self-consciousness about prominent or crooked teeth, which can impact social confidence.
Most common orthodontic options for adolescents

Metal braces
Metal braces remain one of the most effective options for a wide range of bite and alignment problems. Brackets and wires apply gentle, controlled forces that move teeth into healthier positions over time.
Ceramic braces
Ceramic braces work like metal braces, but use tooth-colored brackets that are less noticeable. They can be a good choice for teens who want a subtler look while still needing the control braces provide.
Lingual braces
Lingual braces sit behind the teeth, so they are not visible from the front. They may suit select cases, though they often require a specialist with specific training and can take some time to get used to.
Clear aligners (Invisalign Teen and similar systems)
Clear aligners use a series of custom trays to gradually guide teeth into position. They are removable, which can make eating and brushing easier, and many teens like the low-visibility design.
Success depends heavily on daily wear time. Some teen systems include wear indicators that help the orthodontic team and parents track whether the aligners are being used as prescribed.
Best age to start orthodontic treatment
For many adolescents, comprehensive orthodontic treatment begins between ages 10 and 14, when most permanent teeth are present and jaw growth is still active. That said, timing is not identical for every child.
Many orthodontic associations advise an initial orthodontic evaluation around age 7. This does not mean treatment must start immediately, but it helps identify developing concerns early and plan the best window for intervention.
How long treatment usually takes
Treatment length depends on the complexity of the bite and alignment, the type of appliance used, and how consistently the teen follows instructions. Many plans fall in the 12–30 month range, though shorter or longer timelines are possible.
What can affect the timeline
- Severity of crowding or bite discrepancies.
- Growth pattern and jaw development.
- Oral hygiene and the health of gums and teeth.
- Consistency with elastics, aligner wear time, and other instructions.
- Keeping regular follow-up appointments.
Keeping teeth stable after treatment

Retention is a critical part of orthodontic care. Teeth naturally try to drift back toward their old positions, especially in the first year after active treatment.
Retention options
- Removable retainers: Often worn full-time at first, then at night as advised.
- Bonded retainers: A thin wire attached behind the teeth to help maintain alignment.
- Periodic check-ups: Short follow-ups help detect shifting early and adjust retention if needed.
Good brushing and flossing habits should continue after treatment. If teeth grinding (bruxism) is an issue, a dentist or orthodontist may suggest a night guard to protect teeth and retainers.
Frequently asked questions
Is orthodontic treatment painful?
It’s normal to feel pressure or mild soreness after braces are placed or adjusted, or when switching to a new aligner tray. The discomfort usually settles within a few days. Soft foods, good hygiene, and orthodontist-approved pain relief can help if needed.
Do all permanent teeth need to be in before starting treatment?
Not always. Some orthodontic plans begin earlier, especially when jaw growth guidance is helpful. Many comprehensive teen treatments start once most permanent teeth have erupted, but your orthodontist will decide based on development and the specific problem.
Can a teenager straighten teeth without braces?
In many mild to moderate cases, clear aligners are an option. For more complex crowding or bite correction, braces may offer better control. A consultation is the best way to match the method to the case.
Will braces affect school, sports, or music?
Most teens adapt quickly. Mouthguards can protect braces during contact sports, and orthodontic wax can reduce irritation. If a teen plays a wind instrument, there may be a short adjustment period while the lips and cheeks get used to the brackets.
Do braces cause tooth decay?
Braces do not cause decay on their own, but they can trap food and plaque if cleaning is inconsistent. Careful brushing, interdental cleaning, and regular dental visits reduce the risk.
What happens if treatment is delayed until adulthood?
Orthodontic treatment can work at any age, but teen treatment may be faster because growth can be used to guide development. Adults may need longer treatment times, and certain jaw issues may be harder to correct without more complex options.
What is Pericoronitis?
What is Pericoronitis? Symptoms & Treatments
Pericoronitis is a painful infection of the gum around a partially erupted wisdom tooth. When a small gum flap traps food and bacteria, the area can swell and become tender, causing bad taste, trouble chewing, and limited mouth opening. Dentists treat it with cleaning, medication, and—when it keeps returning—gum flap removal or wisdom tooth extraction.
What pericoronitis is
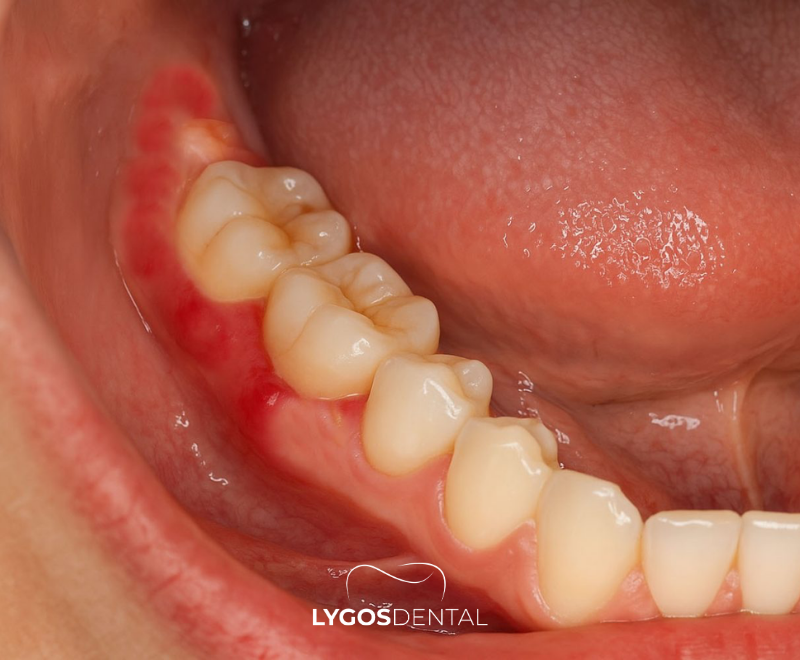
Pericoronitis is inflammation and infection of the gum tissue surrounding a wisdom tooth that has only partially erupted. The partially covered area (often called an operculum) can form a pocket where plaque, food debris, and bacteria collect. That trapped buildup irritates the gum and can trigger an infection that spreads into nearby soft tissue if not treated.
Common causes and risk factors
Most cases occur around lower wisdom teeth because they frequently erupt at an angle or remain partly impacted. The risk is higher when the area is hard to clean, when opposing teeth bite into the gum flap, or when general oral hygiene is disrupted. Stress, illness, and smoking can also make it easier for an infection to take hold.
- Partially erupted or impacted wisdom teeth (especially lower third molars)
- Food trapping under the gum flap and poor access for brushing/flossing
- Irritation from the upper wisdom tooth biting on the gum tissue
- Crowding around the back molars and plaque buildup
- Smoking or reduced immune resilience during illness
Symptoms of pericoronitis
Symptoms can range from mild soreness to significant pain and facial swelling. They often worsen when chewing and may flare up repeatedly over weeks or months.
- Throbbing pain at the back of the jaw (often on one side)
- Red, swollen, or tender gum tissue around the wisdom tooth
- Bad breath or a bad taste (sometimes with pus or discharge)
- Difficulty chewing or pain when biting down
- Limited mouth opening (jaw stiffness)
- Swollen lymph nodes under the jaw or in the neck
When to see a dentist urgently
Pericoronitis can become serious if the infection spreads. Seek urgent dental or emergency care if you notice any of the following warning signs.
- Fever, chills, or feeling generally unwell
- Rapidly increasing facial swelling
- Trouble swallowing, breathing, or opening the mouth
- Swelling extending into the neck or under the tongue
- Severe pain that does not improve with over-the-counter medication
How pericoronitis is diagnosed
A dentist usually diagnoses pericoronitis with an oral exam and a discussion of your symptoms. They check for swelling, trapped debris, and tenderness around the tooth. Dental X-rays are often used to see the tooth’s position and whether there is an impaction or surrounding bone involvement.
Treatment options
In-office cleaning and drainage
For many people, the first step is gently cleaning the pocket around the tooth and flushing it with an antiseptic solution. If there is pus, the dentist may help it drain, which can quickly reduce pressure and pain.
Medication
Pain relief is typically managed with anti-inflammatory medication when appropriate. Antibiotics may be prescribed when there are signs of spreading infection, fever, or significant swelling. Medication works best alongside professional cleaning because bacteria can remain trapped under the gum flap.
Gum flap removal (operculectomy)
If the tooth is expected to erupt into a healthy position, removing the gum flap can eliminate the pocket where bacteria collect. This can reduce the chance of recurrence, though it may not be suitable if the tooth is poorly positioned.
Wisdom tooth extraction
If pericoronitis keeps returning, or if the wisdom tooth is impacted or difficult to clean long term, extraction is often the most definitive solution. Your dentist or oral surgeon will confirm the best option based on your X-rays, symptoms, and overall oral health.
Home care for short-term relief
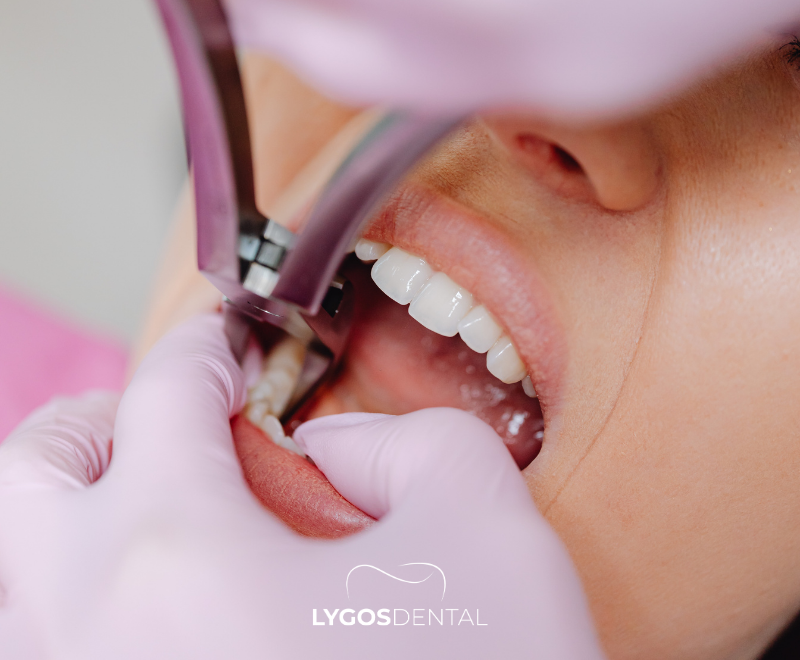
Home measures can reduce discomfort while you arrange dental care, but they do not remove the underlying cause. Avoid applying aspirin directly to the gum, and do not rely on home remedies if symptoms are worsening.
- Rinse gently with warm salt water a few times per day
- Brush carefully around the area and use an interdental brush if you can do so comfortably
- Use cold compresses on the cheek for swelling
- Choose softer foods and avoid chewing on the painful side
- Use over-the-counter pain relief only as directed and only if it is safe for you
How long pericoronitis takes to heal
With appropriate treatment, pain and swelling often start to improve within a few days. Mild cases may settle in 3–5 days once the area is cleaned and irritation is reduced. More significant infections may take 7–10 days, and recovery after a minor procedure or extraction can take up to around two weeks.
How to prevent recurrence
Pericoronitis is more likely to come back when the wisdom tooth remains partly covered by gum tissue. Good daily cleaning helps, but it may not be enough if the tooth is impacted or the gum flap is repeatedly irritated.
- Keep the back molar area clean with gentle brushing and flossing or an interdental brush
- Attend regular dental check-ups, especially during wisdom tooth eruption years
- Address recurring food trapping early—don’t wait for severe pain
- Discuss long-term options (operculectomy or extraction) if you have repeated flare-ups
Frequently asked questions
Can pericoronitis go away on its own?
Symptoms can temporarily ease if trapped debris is removed and irritation decreases. Even when pain settles, the pocket under the gum flap can remain, so flare-ups are common without dental assessment and long-term management.
Can it be treated without removing the tooth?
Sometimes, yes. Cleaning, medication, and gum flap removal may be enough when the tooth is erupting into a good position. If the tooth is impacted or infections keep returning, extraction is often the most reliable way to prevent repeat episodes.
Is pericoronitis contagious?
The infection itself is not considered contagious in the way a cold or flu is. However, the bacteria that cause gum infections are common in the mouth, so prevention focuses on reducing bacterial buildup and improving access for cleaning.
Interdental Brush or Dental Floss?
Interdental Brush or Dental Floss?
If your teeth are tightly spaced, dental floss is usually the better fit. If you have larger gaps, gum recession, braces, bridges, or implants, an interdental brush often cleans more effectively. Many people get the best results by using floss for tight contacts and a brush for wider spaces, once a day.
rushing is essential, yet a toothbrush cannot fully clean the narrow spaces between teeth and along the gumline. That’s where interdental cleaning comes in. The right tool depends on the shape of your teeth, the size of the spaces, and any dental work you have.
Interdental Brushes: What They Are And Who They Suit

An interdental brush is a small bristled brush designed to slide between teeth and sweep plaque from the sides of the teeth and the gum margin. They come in different diameters, so sizing matters. A brush should pass through with light resistance and without forcing.
Interdental brushes tend to work best when there is enough room for the bristles to contact the tooth surface on both sides.
They are often recommended for:
• Visible gaps between teeth
• Gum recession that creates open embrasures
• Bridges and implants (where plaque builds around margins)
• Braces and orthodontic appliances
• People who struggle with floss technique
Common benefits include more complete plaque removal in open spaces, gentle gum stimulation, and easier access around dental work.
Dental Floss: What It Is And When It Works Best
Dental floss is a thin filament—usually nylon or PTFE—made to clean tight contacts where a brush cannot fit. Used correctly, floss disrupts plaque and removes trapped debris from between teeth.
Floss is a strong choice when the teeth touch closely and the space is too narrow for any brush size.
Floss is especially useful for:
• Tight contacts between natural teeth
• Areas prone to cavities between teeth
• People who prefer a compact, travel-friendly option
Technique matters. Snapping floss into the gum can cause soreness or bleeding, while a gentle curve around the tooth cleans more effectively.
Key Differences At A Glance
| Factor | Interdental Brush | Dental Floss |
| Best for space size | Open spaces and gum recession | Tight contacts |
| Dental work | Excellent for implants, bridges, braces | Works, but can be tricky around appliances |
| Ease of use | Usually easier once sized correctly | Requires practice and good technique |
| Gum comfort | Can massage gums when used gently | Can irritate gums if snapped or forced |
| Portability | Less compact; tips can bend | Very compact and easy to carry |
How To Choose Based On Your Situation
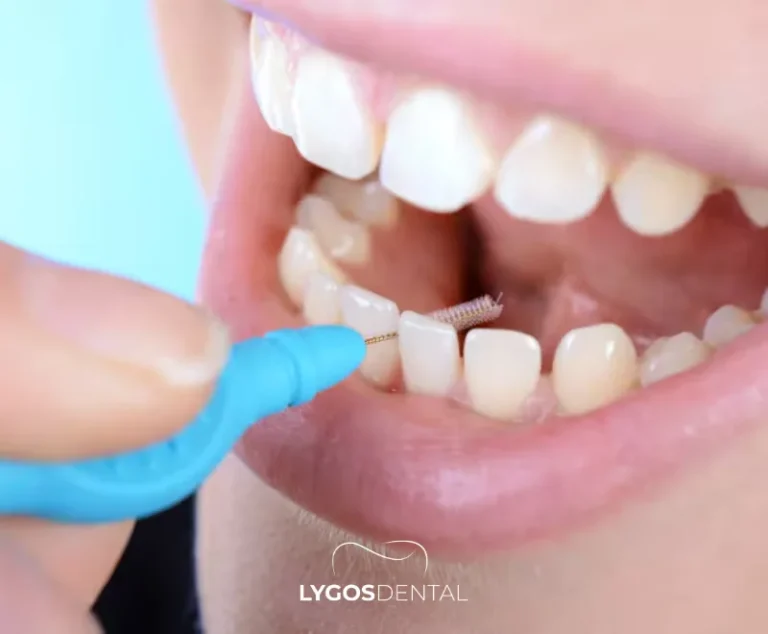
The simplest rule is fit. If a tool cannot enter the space comfortably, it is not the right option for that area.
Use dental floss when you have:
• Tight spaces with teeth in contact
• No visible gaps and healthy gum contours
Choose an interdental brush when you have:
• Spaces where floss feels loose or doesn’t wipe the tooth sides well
• Gum recession or black triangles between teeth
• Implants, bridges, or braces that trap plaque
It can be normal to use both. Many mouths have a mix of tight and open areas, so a combination routine is often the most practical.
Orthodontic Treatment: Braces And Aligners
With braces, plaque and food debris collect around brackets and wires, so interdental cleaning becomes more demanding. Interdental brushes can reach around hardware quickly, especially angled designs. Floss can still be used, but it may require floss threaders or specialized orthodontic floss.
If you wear clear aligners, flossing is usually straightforward because there are no brackets, but an interdental brush can still help in any areas with small gaps or gum recession.
Dentist Tips For Better Interdental Cleaning
For safer, more effective results:
• Clean between teeth once a day, preferably before bed.
• Avoid forcing any tool. If it doesn’t fit, switch size or use floss for that contact.
• For interdental brushes, ask a dentist or hygienist to size you; the right diameter makes the biggest difference.
• Rinse the brush after use and let it dry. Replace it when bristles splay or the wire bends.
• If your gums bleed for more than a week despite gentle technique, book a dental check-up.
Frequently Asked Questions
Which Is More Effective: Interdental Brush Or Dental Floss?
Effectiveness depends on the space. Interdental brushes usually remove more plaque in open gaps, while floss is better for tight contacts where brushes cannot enter. If you are unsure, a dentist can recommend sizes and show technique.
Can I Use An Interdental Brush Instead Of Floss?
Yes, for spaces where the brush fits with light resistance. For very tight contacts, floss remains the safer and more effective option. A mixed routine is common.
How Often Should I Clean Between My Teeth?
Once a day is a practical baseline for most people. Consistency matters more than doing it multiple times a day.
Can Dental Floss Harm My Gums?
It can if you force it or snap it down. Use a gentle sawing motion to pass the contact, then curve the floss into a “C” shape against one tooth and move it up and down.
How Often Should An Interdental Brush Be Replaced?
Many brushes last about 1–2 weeks with daily use, depending on the brand and how tight the spaces are. Replace sooner if the bristles spread out or the wire bends, since cleaning performance drops.
Why Do Gums Swell?
Why Do Gums Swell?
Gum swelling is usually a sign of inflammation caused by plaque buildup, infection, irritation, hormonal changes, or certain medicines. It may show up as puffy, red, tender gums that bleed when brushing or flossing. Early care and a dental check-up help prevent gum disease and protect the teeth and supporting bone.
What Gum Swelling Means
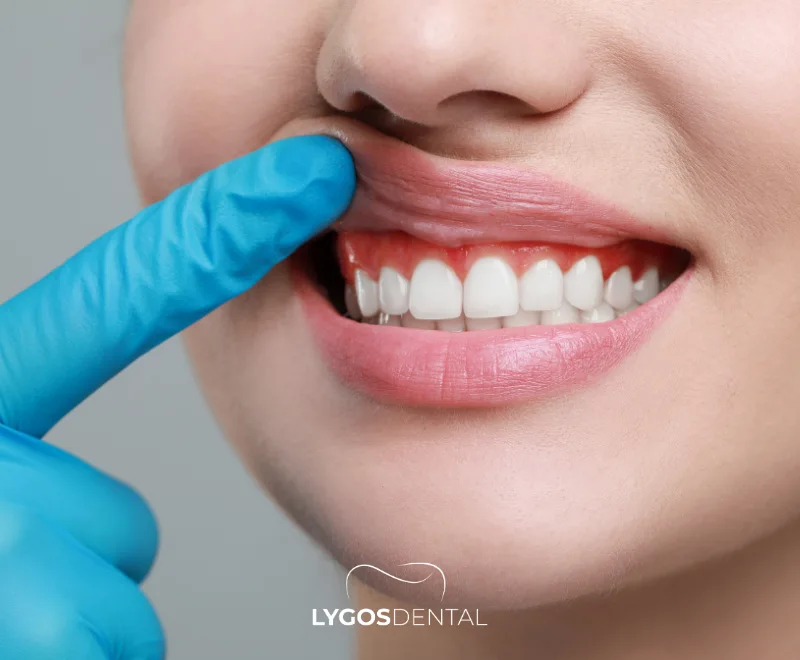
Swollen gums (also called gingival swelling) happen when gum tissue becomes inflamed and puffy. The gums may look darker red than usual, feel sore, and bleed easily. Swelling can be mild and limited to one spot, or it can affect the gums around many teeth.
Gum Swelling Vs. Gum Recession
Gum swelling and gum recession can look similar at a glance, but they are different problems. Swelling is an increase in gum size due to inflammation. Recession is when the gum margin moves upward and exposes more of the tooth or root, often making teeth look longer. Some people can have both at the same time, especially with gum disease.
Common Symptoms
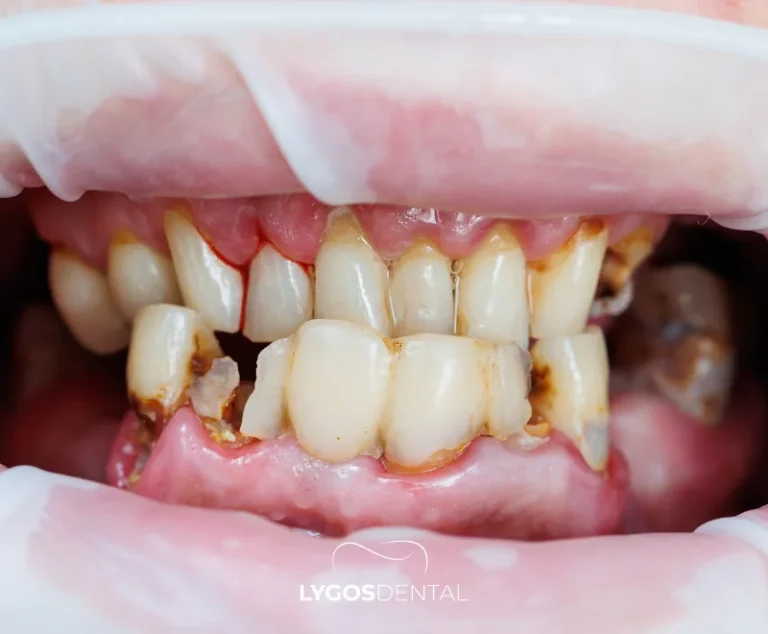
Swollen gums do not always hurt at first. Over time, you may notice changes such as:
- Puffy, red, or shiny-looking gums
- Bleeding during brushing or flossing
- Tenderness or pain, especially when chewing
- Bad breath or a bad taste
- Gum soreness around a specific tooth
- Tooth sensitivity if the gums are also receding
Why Do Gums Swell? The Most Likely Causes
Plaque Buildup And Gingivitis
The most common cause is plaque along the gumline. When plaque is not removed daily, it irritates the gums and triggers inflammation (gingivitis). Gingivitis is usually reversible with improved cleaning and professional dental care.
Periodontitis And Deeper Gum Infection
When gum inflammation is not treated, it can progress to periodontitis. This deeper infection can cause persistent swelling, gum pockets, bone loss, and loose teeth. Periodontitis requires professional treatment such as deep cleaning, and sometimes additional procedures.
Food Trapping And Local Irritation
Swelling limited to one area may be caused by food stuck between teeth, a sharp piece of tooth, or an irritating dental edge. Flossing gently and rinsing with water can help, but ongoing swelling should be checked to rule out infection or decay.
Hormonal Changes
Hormonal shifts during pregnancy, puberty, and menopause can make gums more reactive to plaque. This can lead to swelling and bleeding even when plaque levels are not very high. Good daily cleaning and regular dental visits matter more during these times.
Smoking And Tobacco Use
Tobacco increases the risk of gum disease and slows healing. It may also mask bleeding, so gum problems can progress quietly. Quitting tobacco is one of the most effective steps for long-term gum health.
Brushing Too Hard Or Using The Wrong Tools
Aggressive brushing, hard-bristled toothbrushes, or poor technique can irritate gum tissue. Switching to a soft brush and using gentle, angled strokes along the gumline reduces trauma and helps the gums calm down.
Dental Appliances And Poorly Fitting Restorations
Ill-fitting crowns, fillings, aligners, retainers, or dentures can rub the gums and trap plaque. If swelling started after dental work or a new appliance, have your dentist check the fit and margins.
Medications And Dry Mouth
Some medicines can contribute to gum swelling, or reduce saliva and increase plaque buildup. If swelling began after starting a new medication, do not stop it on your own. Ask your dentist or physician whether an alternative or additional oral care steps may help.
Nutritional Gaps And General Health Factors
Low intake of key nutrients, especially vitamin C, can make gums more prone to bleeding and swelling. Stress, uncontrolled diabetes, and a weakened immune system can also worsen gum inflammation. If gum swelling is frequent, a health check may be part of the solution.
When Gum Swelling Is An Emergency

Seek urgent dental or medical care if you have swelling with fever, facial swelling, pus, severe pain, trouble swallowing, or difficulty breathing. These signs can indicate a spreading infection that needs prompt treatment.
What You Can Do At Home
Home care can ease mild swelling, but it should not replace a dental diagnosis. Helpful steps include:
- Brush twice daily with a soft-bristled toothbrush and gentle pressure
- Clean between teeth daily using floss or interdental brushes
- Rinse with warm salt water for short-term comfort
- Avoid tobacco and limit sugary snacks and drinks
- Use a dentist-recommended mouthwash if advised for inflammation
How Dentists Treat Swollen Gums
Treatment depends on the cause and how advanced the inflammation is. Common options include:
- Professional cleaning to remove plaque and tartar
- Deep cleaning (scaling and root planing) for gum pockets
- Targeted treatment for cavities or broken fillings that irritate the gums
- Antimicrobial rinses or antibiotics when infection is present
- Adjusting or replacing restorations and appliances that trap plaque
- Ongoing periodontal maintenance for people with periodontitis
How To Prevent Gum Swelling
Most gum swelling is preventable with consistent habits. Focus on daily plaque removal, gentle technique, and regular dental check-ups. A balanced diet, adequate hydration, and tobacco avoidance also support gum tissue and healing.
Frequently Asked Questions
Can swollen gums go away on their own?
Mild swelling from temporary irritation may improve with better cleaning, but swelling that lasts more than a few days often needs a dental exam. If gum disease or infection is present, it usually worsens without treatment.
Do swollen gums always mean gum disease?
Not always. Swelling can also come from local irritation, hormonal changes, medications, or a dental appliance. A dentist can identify the cause and check for gum pockets or bone changes.
Why do my gums swell around one tooth?
A common reason is food trapping, a cavity, a cracked tooth, or a gum pocket in that area. If swelling is localized, painful, or recurring, it should be evaluated.
Does mouthwash help swollen gums?
It can help reduce bacteria and soothe gums, but it does not remove tartar or fix underlying issues. Use mouthwash as a support step, not a replacement for brushing, flossing, and professional care.
How Do Gum Diseases Affect Heart Health?
How Do Gum Diseases Affect Heart Health?
Gum disease (especially periodontitis) is associated with a higher risk of cardiovascular problems. The likely link is shared inflammation: infected gums can raise inflammatory markers and allow oral bacteria into the bloodstream, which may affect blood vessels. Research shows an association, but it has not proven that gum disease directly causes heart disease.
The Short Answer: What The Research Shows
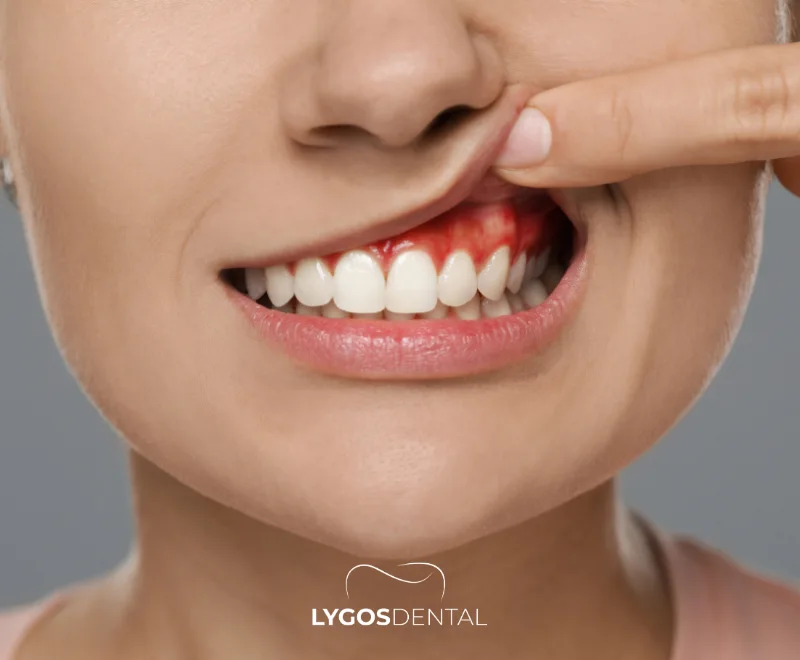
Large studies and expert reviews consistently find an association between periodontitis and atherosclerotic cardiovascular disease (ASCVD), such as coronary artery disease and stroke. That said, association is not the same as causation. Gum disease and heart disease share major risk factors—smoking, diabetes, aging, and socioeconomic factors—so researchers cannot yet say gum disease alone causes heart events.
What Counts As Gum Disease?
Gum disease is an infection and inflammation of the tissues that hold your teeth in place. It typically progresses in stages:
- Gingivitis: Mild inflammation with redness, swelling, and bleeding. It’s often reversible with consistent plaque control and professional cleaning.
- Periodontitis: Deeper infection that damages the gum attachment and supporting bone. Untreated, it can lead to loose teeth and tooth loss.
How Gum Disease May Affect The Heart
Researchers focus on a few biologically plausible pathways. These pathways help explain the association, even though they don’t prove direct cause-and-effect.
1) Systemic inflammation
Periodontitis is a chronic inflammatory condition. Chronic inflammation is also central to atherosclerosis, the process that drives plaque build-up in arteries. When gum inflammation persists, inflammatory signals can spill over into the bloodstream and add to the body’s overall inflammatory burden.
2) Bacteria entering the bloodstream
Everyday actions like brushing or chewing can allow bacteria from infected gums to enter the bloodstream, especially when gums bleed. Oral bacteria and their by-products can then interact with blood vessel walls, potentially contributing to endothelial dysfunction (a key early step in vascular disease).
3) Immune and clotting effects
Chronic infection can keep the immune system activated. Some studies suggest links between periodontitis and changes in platelet function and clotting tendencies, which matters because clots are involved in heart attacks and many strokes.
Does Gum Disease Cause Heart Attacks?
Current evidence supports a relationship, not a guarantee. People with periodontitis tend to have higher rates of heart attack and stroke in observational research, but this does not prove gum disease is the direct trigger. Treating gum disease improves oral health and may lower inflammation, yet clinical trials have not consistently shown a reduction in heart attacks or strokes from dental treatment alone.
Who Should Take This Link Most Seriously?
Everyone benefits from healthy gums, but these groups should be especially proactive:
- People with diabetes, prediabetes, or metabolic syndrome.
- Smokers and former smokers.
- Adults over 40, especially with a history of gum problems.
- Anyone with known heart or vascular disease, high blood pressure, or high cholesterol.
- People with limited access to regular dental care.
Warning Signs You Shouldn’t Ignore
Gum disease can be painless until it becomes advanced. Common signs include:
- Bleeding when brushing or flossing.
- Red, swollen, or tender gums.
- Persistent bad breath or a bad taste.
- Gum recession or teeth that look “longer.”
- Loose teeth or changes in bite.
How To Protect Your Gums And Support Heart Health
Oral care should be part of your broader cardiovascular risk plan. Practical steps:
Daily habits
- Brush twice daily with fluoride toothpaste and a soft-bristled brush.
- Clean between teeth daily (floss or interdental brushes).
- If you have bridges, implants, or orthodontic appliances, use the tools your dentist recommends.
Professional care
- Schedule routine dental checkups and cleanings based on your dentist’s advice.
- If you have gum pockets or a history of periodontitis, ask about periodontal monitoring and maintenance visits.
Lifestyle and medical factors
- Stop smoking—this is one of the biggest shared risk factors for gum and heart disease.
- Keep diabetes and blood pressure well controlled; poor control worsens gum inflammation.
- Aim for a balanced diet with limited added sugars; frequent sugar exposure feeds plaque bacteria.
A Note About Endocarditis Risk
A small subset of people are at increased risk of infective endocarditis (an infection of the heart lining or valves). For these patients, dentists may recommend specific precautions. If you have a prosthetic heart valve, certain congenital heart conditions, or a history of endocarditis, tell your dentist and cardiologist so they can align on the right plan.
Frequently Asked Questions
Do bleeding gums mean I have heart disease?
No. Bleeding gums most often point to gingivitis or periodontitis. It’s a sign to book a dental visit, and it’s also a reminder to review shared risk factors like smoking and diabetes.
Can better oral hygiene lower heart risk?
Good oral hygiene helps reduce gum inflammation and infection. While it’s not a substitute for managing blood pressure, cholesterol, or diabetes, it’s a sensible part of an overall prevention plan.
If I have heart disease, should I see a dentist more often?
Many people with heart disease benefit from consistent preventive care, especially if they have gum problems. Your dentist can recommend a schedule based on your periodontal status and medications.
Nutritional Recommendations During the Teething Period
Nutritional Recommendations During The Teething Period
During teething, many babies eat less because sore gums make chewing uncomfortable. Offer soft, nutrient-dense foods, add cool options like yogurt or chilled purées for comfort, and keep milk feeds consistent. Avoid choking hazards and sugary snacks. If your baby has a fever (38°C/100.4°F or higher) or persistent diarrhea, contact a pediatrician.
Why Nutrition Matters During Teething

Teething can bring drooling, gum tenderness, and extra fussiness. Appetite often dips, which can worry parents. The goal is to keep your baby comfortable while still meeting daily needs for energy, protein, iron, and calcium.
When Does Teething Usually Start?
Many babies begin teething between 4 and 7 months, but earlier or later can still be normal. The first teeth are often the lower front teeth, followed by the upper front teeth. New teeth may continue to appear until around 2½ to 3 years.
Common Signs Of Teething
You may notice one or more of the following:
- More drooling than usual
- Red, tender gums where a tooth is coming through
- Chewing on hands or toys
- Irritability or disrupted sleep
- Temporary changes in feeding patterns
Some symptoms that parents often attribute to teething—such as high fever or significant diarrhea—usually point to another cause. If you are unsure, it’s safer to check with your child’s clinician.
Best Foods During Teething

Choose foods that are soft, easy to swallow, and rich in nutrients. If your baby is on solids, these options are commonly well tolerated:
- Vegetable and fruit purées (smooth texture, easy to eat)
- Plain yogurt (cool and gentle on gums)
- Mashed banana (soft, filling, and easy to digest)
- Well-cooked vegetables like zucchini, carrot, or potato (mashed or finely chopped)
- Soft cheese or cottage cheese (calcium and protein, if dairy is tolerated)
Soothing, Cool Options For Sore Gums
Cool temperatures can reduce gum discomfort. Use chilled—not rock-hard frozen—foods, and always supervise during feeding.
- Cold yogurt or chilled purée served with a spoon
- Chilled fruit purée (pear or banana are often gentle choices)
- A clean, chilled teething ring or cold washcloth to chew (not tied around the neck)
- Breast milk or formula feeds as usual; slightly cool milk may feel soothing for some babies
Foods To Avoid During Teething
During teething, avoid foods that increase choking risk, irritate sensitive gums, or add unnecessary sugar.
- Hard pieces of food (raw apple slices, raw carrot sticks, popcorn, nuts)
- Sticky foods that cling to teeth (gummy sweets)
- Sugary snacks and sweetened drinks that raise cavity risk
- Honey before 12 months (risk of infant botulism)
- Highly acidic foods if they cause obvious mouth irritation (for example, citrus)
Hydration During Teething
Drooling can be heavy during teething, so hydration matters. Breast milk or formula should remain the main source of fluids. After 6 months, small sips of water can be offered with meals, based on your pediatrician’s guidance.
Skip sugary juices and sweetened compotes. If you offer fruit, whole fruit or unsweetened purée is usually the better choice.
Practical Feeding Tips For Parents

- Offer smaller, more frequent meals if appetite is low.
- Prioritize texture: smooth, mashed, or finely chopped foods are often better tolerated.
- Serve foods lukewarm or cool if warm foods seem to irritate gums.
- Stay with your baby during meals to reduce choking risk.
- Keep oral hygiene gentle: wipe gums and emerging teeth with a soft, clean cloth.
When To Call A Pediatrician
Seek medical advice if your baby has a temperature of 38°C (100.4°F) or higher, shows signs of dehydration, has ongoing diarrhea or vomiting, refuses most feeds, or seems unusually sleepy or difficult to settle. These signs should not be assumed to be “just teething.”
Nutritional Recommendations During the Teething Period Frequently Asked Questions (FAQ)
Is it normal for babies to eat less while teething?
Yes. Gum tenderness can make chewing uncomfortable. Offer soft foods, keep milk feeds consistent, and try smaller meals more often. Appetite usually returns once discomfort eases.
Which fruits are best for teething babies?
Gentle, softer fruits like banana and pear often work well. Serve them mashed or as a smooth purée. If you try apple, cook and mash it rather than offering hard slices.
How many meals should a teething baby have?
There’s no single number that fits every baby. If intake drops, aim for smaller, frequent meals and focus on nutrient-dense choices rather than pushing large portions.
Why does hydration matter so much during teething?
Babies can drool a lot, and some drink less when they are uncomfortable. Breast milk or formula remains most important, and after 6 months you can offer small sips of water with meals.
Is fever part of teething?
Teething can coincide with a slight temperature change, but a true fever—38°C (100.4°F) or higher—should be treated as a sign of illness until a clinician says otherwise.
Is Whitening Teeth with Baking Soda Safe?
Is Whitening Teeth with Baking Soda Safe?
Used occasionally and gently, baking soda can help remove surface stains from coffee, tea, or smoking. It does not bleach teeth or change their natural shade, and it isn’t a substitute for fluoride toothpaste. Avoid mixing it with acidic ingredients like lemon or vinegar, and stop if you notice sensitivity or gum irritation.
Baking soda (sodium bicarbonate) is a common home remedy for a brighter smile because it can polish away some external staining. That said, “natural” doesn’t always mean risk-free. The safest approach depends on how you use it, how often you use it, and your enamel and gum health.
What Baking Soda Does On Teeth

Baking soda is mildly abrasive and alkaline. When you brush with it, it can help loosen plaque and lift superficial stains that sit on the enamel surface. Because it is alkaline, it can also help neutralize acids in the mouth that contribute to enamel demineralization.
Does Baking Soda Actually Whiten Teeth?
It can make teeth look whiter by removing surface discoloration, not by bleaching the tooth. Stains caused by coffee, tea, red wine, and tobacco are the most likely to improve. If your teeth look darker because of genetics, aging, medications, or trauma, baking soda won’t meaningfully change the underlying shade.
Is It Safe For Enamel And Gums?
Evidence reviews note that baking soda has an intrinsically low abrasive nature compared with many other common toothpaste abrasives, and baking-soda dentifrices are considered low in abrasivity. The bigger safety issues usually come from brushing too hard, brushing too long, using it too frequently, or pairing it with acidic DIY mixes that can soften enamel first.
Plain baking soda also does not contain fluoride, which is a key ingredient for cavity prevention. If you replace your regular toothpaste with baking soda long-term, you may miss out on the daily fluoride exposure that helps strengthen enamel.
Potential Downsides To Watch For
- Tooth sensitivity, especially if you already have thinning enamel or exposed roots.
- Gum irritation if the paste is gritty or you scrub along the gumline.
- Uneven results if you focus on certain teeth or brush aggressively in one area.
- Higher cavity risk if baking soda replaces a fluoride toothpaste.
How To Use Baking Soda Safely

For most adults, occasional use is the safest way to treat baking soda as a stain-removal booster rather than a daily toothpaste replacement. A common rule of thumb from dental clinicians is once a week or less, especially if you have sensitivity.
A Gentle At-Home Method
- Wet your toothbrush and sprinkle a small pinch of baking soda onto the bristles, or mix a small amount with water to form a thin paste.
- Brush lightly for about one minute, focusing on stained areas and avoiding heavy pressure at the gumline.
- Rinse well, then brush with a fluoride toothpaste afterward (or use your fluoride toothpaste at the next brushing).
- Stop if you feel sharp sensitivity or notice gum soreness.
Skip recipes that combine baking soda with lemon juice, vinegar, or other acidic ingredients. Acids can soften enamel, and brushing right after that can increase wear.
Who Should Avoid Baking Soda Whitening?

Avoid or get dental advice first if you have moderate to severe tooth sensitivity, gum recession, enamel erosion, untreated cavities, or lots of exposed root surfaces. It’s also not a good idea for children because enamel is still developing and they benefit most from consistent fluoride use.
Safer Alternatives For Noticeable Whitening
If you want predictable whitening, a product designed for teeth usually gives better results with clearer safety directions. Consider these options, starting with the least intensive.
Baking Soda Toothpaste With Fluoride
A fluoride toothpaste that contains baking soda can help with daily plaque removal and surface stain control while still supporting cavity prevention. This is typically a better long-term choice than brushing with plain baking soda.
Peroxide-Based Whitening Strips Or Gels
Over-the-counter whitening strips and gels use peroxide to chemically break down stains, so they can lighten beyond surface discoloration. Follow the instructions closely and take breaks if sensitivity starts.
Dentist-Supervised Whitening
If you have crowns, veneers, bonding, or uneven tooth color, dentist-supervised whitening is often the safest route. A dentist can also check for cavities or cracks first and recommend a plan that fits your enamel and gum health.
Be Careful With Activated Charcoal
Activated charcoal products are popular online, but evidence for meaningful whitening is limited and abrasivity varies widely by product. Some charcoal powders and toothpastes are fluoride-free, which can be a drawback for cavity prevention.
Frequently Asked Questions
Is baking soda whitening permanent?
No. It mainly removes surface stains, so results tend to fade if the staining habits (coffee, tea, tobacco) continue.
Can I use baking soda every day?
Daily use is not ideal for most people, especially if you brush hard or have sensitivity. A fluoride toothpaste is a better daily baseline.
Does baking soda work on yellow teeth?
It can help if the yellow appearance is from surface staining. If the color comes from dentin showing through thinner enamel, baking soda won’t change that.
What should I do if my teeth feel sensitive afterward?
Stop the baking soda routine and switch to a fluoride toothpaste for sensitive teeth. If sensitivity persists for more than a few days, book a dental checkup.
