What to Do If a Laminate Veneer Breaks?
What to Do If a Laminate Veneer Breaks?
If a laminate veneer chips or breaks, save the piece if you can, avoid chewing on that tooth, and contact your dentist promptly. Rinse gently with warm salt water and use over-the-counter pain relief if you feel sensitivity. Most breaks can be repaired or replaced, and early care helps protect the underlying tooth.
Laminate veneers can look very natural and, with proper care, often last for years. Still, accidents happen, and a veneer can crack, chip, or come off.
The right next steps depend on how the veneer failed and whether the tooth underneath is exposed. This guide covers what to do immediately, common repair options, and practical ways to prevent another break.
This information is general guidance and does not replace an in-person dental exam. If you have significant pain, swelling, or facial trauma, seek urgent dental or medical care.
What A Laminate Veneer Is

A laminate veneer is a thin porcelain shell bonded to the front surface of a tooth, most often on the front teeth. It can improve color, shape, minor spacing, and small alignment concerns while preserving much of the natural tooth.
Because veneers are thin, they rely on strong bonding and a stable bite. When the bond is stressed or the veneer takes a direct hit, it can chip, crack, or detach.
Common Reasons Veneers Break
- Trauma or impact: Falls, sports injuries, or a direct hit to the mouth can fracture porcelain.
- Teeth grinding or clenching (bruxism): Night-time grinding puts repeated pressure on veneer edges.
- Biting hard foods or objects: Ice, hard candy, bones, and using teeth as tools can chip porcelain.
- Bite changes or uneven contact: A high spot can concentrate force on one part of the veneer.
- Bonding or material issues: Contamination during bonding or weakened porcelain can reduce strength over time.
What To Do Right Away

- Save any fragments: Place the broken piece in a clean container. If it is intact, your dentist may be able to rebond it.
- Protect the tooth: Avoid chewing on that side and choose softer foods until you are evaluated.
- Rinse gently: Warm salt-water rinses can help keep the area clean if the tooth feels rough or irritated.
- Manage sensitivity: Over-the-counter pain relief can help if the tooth is sensitive. Avoid very hot or very cold foods.
- Cover sharp edges if needed: If the veneer edge feels sharp, a small amount of dental wax from a pharmacy can reduce irritation.
- Book a dental visit quickly: Prompt care reduces the chance of further chipping and protects the tooth underneath.
Seek urgent help sooner if you notice severe pain, ongoing bleeding, facial swelling, a loose tooth, or if the break followed a significant impact.
Can A Broken Laminate Veneer Be Fixed?
Often, yes. The best option depends on the size of the break, where it occurred, the condition of the bonding surface, and whether the underlying tooth or filling material was damaged.
Your dentist will usually check your bite, look for cracks, and evaluate the tooth underneath before deciding whether a repair is predictable or a replacement is safer.
Treatment Options For A Broken Laminate Veneer
Composite Bonding For Small Chips
Small chips at the edge can sometimes be smoothed or repaired with tooth-colored composite. This is typically completed in one visit and can be a cost-effective fix, though it may not be as wear-resistant as porcelain.
Rebonding The Veneer
If the veneer came off in one piece and the porcelain is not fractured, rebonding may be possible. Success depends on how clean the veneer and tooth surfaces are and whether enough bonding surface remains.
Replacing The Veneer
For larger fractures, repeated breakage, or poor fit, replacing the veneer is often the most durable option. A new veneer may require an impression or digital scan and a short lab turnaround, with a follow-up appointment for bonding.
Temporary Veneer While You Wait
If your tooth looks uneven or feels sensitive while you wait for a final restoration, a temporary veneer or temporary composite can protect the tooth and maintain appearance.
How To Reduce The Risk Of Another Break
- Avoid hard biting: Skip ice, hard candy, and cracking nuts with your front teeth.
- Wear a night guard if you grind: A custom guard can reduce stress on veneers during sleep.
- Use a sports mouthguard: Protection matters for contact sports and activities with fall risk.
- Keep up with routine checkups: Your dentist can spot bite issues, early cracks, or loose margins.
- Maintain daily oral hygiene: Brush and floss to keep the margins healthy and reduce decay risk around the veneer.
- Do not use your teeth as tools: Opening packages and biting pens are common causes of chips.
Frequently Asked Questions
Is immediate action necessary if a veneer breaks?
Contact a dentist as soon as you can. Early assessment helps prevent further damage and makes repair options more predictable.
Will a broken veneer heal on its own?
No. A veneer cannot repair itself. It needs professional evaluation to decide on smoothing, bonding repair, rebonding, or replacement.
Can the natural tooth be damaged when a veneer breaks?
Sometimes. A veneer may chip without affecting the tooth, but a deeper fracture or a knocked-off veneer can expose enamel or dentin, which may cause sensitivity.
How long does veneer repair take?
Minor smoothing or composite repair is often completed in one visit. If a new veneer is needed, it usually takes more than one appointment because a lab or milling step is involved.
Does a broken veneer cause pain?
Not always. Pain or strong sensitivity is more likely if the tooth underneath is exposed, the bite is high, or the break happened with trauma.
A broken laminate veneer is frustrating, but it is usually manageable with the right timing and treatment choice. Protect the area, avoid chewing on the tooth, and arrange a dental visit promptly so your dentist can restore function and appearance safely.
Braces for Adults
Braces for Adults
Adults can get braces at almost any age as long as teeth and gums are healthy. Treatment usually takes 12–30 months and can be done with metal, ceramic, lingual braces, or clear aligners. An orthodontist will choose the best option based on your bite, crowding, and lifestyle.
Can Adults Get Braces?

Yes. Teeth move because the periodontal ligament and surrounding bone respond to steady, gentle pressure, and that biology still works in adulthood.
What matters most is overall oral health. If your gums and supporting bone are stable, orthodontic treatment can work well in your 20s, 40s, 60s, and beyond.
Adults often seek treatment for crowding, spacing, bite problems, jaw discomfort, or relapse after earlier braces. Bruxism (teeth grinding) can also push some people to get a bite assessment and align their teeth.
Benefits Of Braces In Adulthood
Adult orthodontic treatment can improve both appearance and long‑term dental health.
- A more confident smile: Straighter teeth can make your smile look cleaner and more balanced.
- Easier cleaning: Aligned teeth reduce tight, hard‑to‑reach areas that trap plaque, lowering cavity and gum‑disease risk.
- Better function: Many people notice improved chewing and less uneven wear once the bite is corrected.
- Protection for teeth and gums: Reducing crowding can make hygiene easier and may help slow gum recession linked to difficult-to-clean overlaps.
Is There An Age Limit For Braces?
There is no strict age limit. Adults may see slightly slower tooth movement than teenagers, so treatment can take a bit longer in some cases.
An orthodontist will check gum health, bone levels, and existing restorations before starting. If there is active periodontal disease, it usually needs to be treated first.
Treatment Options For Adult Braces

Modern orthodontics offers discreet choices that fit different budgets, lifestyles, and bite complexities.
Metal Braces
Metal braces are the most common option and tend to be the most cost‑effective. They are durable and work well for mild to complex alignment and bite problems.
Ceramic Braces
Ceramic braces use tooth‑colored brackets that blend in better than metal. They can stain if oral hygiene is poor, but they remain a popular choice for adults who want a less noticeable look.
Lingual Braces
Lingual braces sit behind the teeth, so they are hidden from view. They can take longer to get used to and are usually priced higher due to customization and technique sensitivity.
Clear Aligners
Clear aligners (such as Invisalign and similar systems) are removable and nearly invisible. They suit many mild to moderate cases and can be convenient for work and social life, but they require consistent wear to stay on track.
How Long Does Treatment Take?
Treatment time depends on crowding, bite issues, and the type of appliance. For many adults, treatment falls in the 12–30 month range.
Minor alignment can finish in 6–12 months, while more complex bite corrections may take closer to two years. Keeping appointments and following wear instructions (especially for aligners) makes a big difference.
Cost Of Braces For Adults In Turkey
Fees depend on case complexity, materials, clinic location, and how long treatment lasts. Clinics typically confirm a final plan after an exam and X‑rays.
As of 2026, many clinics in Turkey advertise the following rough ranges for full treatment (these can vary):
- Metal braces: about 25,000–40,000 TL
- Ceramic braces: about 35,000–55,000 TL
- Lingual braces: about 60,000–90,000 TL
- Clear aligners: often 50,000 TL and up (complex cases can exceed 100,000 TL)
Some clinics offer installment plans. If you compare quotes, ask what is included (records, retainers, emergency visits, and refinements for aligners).
Tips For Adults Wearing Braces

- Keep cleaning simple and consistent: Brush after meals when you can, and use interdental brushes or a water flosser to reach around brackets.
- Stay on schedule: Regular adjustments and checkups keep treatment moving and help prevent small issues from becoming delays.
- Choose brace‑friendly foods: Avoid very hard or sticky foods that can break brackets or bend wires.
- Protect brackets and teeth: Skip nail biting and using teeth as tools. If you play contact sports, wear a mouthguard.
- Plan for retention: Retainers are part of treatment. Wearing them as advised helps prevent relapse.
Braces For Adults FAQ
Are braces too noticeable for adults?
No. Ceramic brackets and clear aligners are designed to be discreet, and many adults choose them for that reason. Your orthodontist can also suggest low‑profile bracket options if appearance is a priority.
Will braces affect my speech?
You might notice small changes during the first few days, especially with lingual braces or new aligners. Most people adapt quickly as the tongue finds a new normal.
Will braces interfere with work?
Usually not. Aligners can be removed briefly for important events, and bracket systems are common in professional settings. Planning appointments ahead and keeping a small oral‑care kit at work helps.
Will my teeth move again after treatment?
Teeth can drift over time without retention. Wearing your retainer as instructed is the best way to keep your results stable.
Do braces hurt?
Expect pressure or soreness for a few days after fittings and adjustments. Soft foods and over‑the‑counter pain relief can help, but ask your dentist or orthodontist for guidance if discomfort feels severe or persistent.
Do Teeth Get Whiter After Quitting Smoking?
Do Teeth Get Whiter After Quitting Smoking?
Quitting smoking stops new nicotine and tar stains from building up, and many people notice a cleaner, brighter surface after a professional cleaning and a few months of good oral care. Deep brown stains that have soaked into enamel won’t vanish on their own, but whitening treatments can usually lighten them safely.
Why Smoking Makes Teeth Look Yellow

Cigarette smoke contains tar and nicotine that cling to the tooth surface and seep into microscopic pores in enamel. Over time, this creates a yellow or brown film that regular brushing can’t fully remove. The longer you smoke, the deeper and more stubborn the discoloration usually becomes.
Surface Stains vs. Deeper Discoloration
Most smoker stains are “extrinsic,” meaning they sit on the outside of the tooth. These often respond well to professional cleaning and whitening. Some discoloration becomes “intrinsic” when pigments penetrate deeper, and that may need stronger whitening or cosmetic options such as bonding or veneers.
Dry Mouth and Plaque Build-Up
Smoking can reduce saliva and change the oral microbiome, which makes plaque and tartar build up faster. That build-up traps pigments and makes teeth look dull. It can also worsen bad breath, which many people notice improves after quitting.
What Changes After You Quit Smoking
Quitting removes the main source of new staining, so discoloration stops getting worse day by day. As your mouth rehydrates and your gums receive better blood flow, the tissues often look healthier and cleaner. Those changes can make your smile look fresher, even before you do any whitening.
Will Teeth Whiten on Their Own?
Teeth rarely “bleach” naturally after quitting, but they can look lighter as surface stains fade and plaque levels drop. A dental cleaning is often the turning point because it removes tartar and polishes away surface discoloration. If stains have been building up for years, whitening treatments are usually needed for a clear shade change.
How Long Does It Take to Notice a Difference?
There isn’t one timeline that fits everyone. The change depends on how long you smoked, the type of tobacco, how much coffee or tea you drink, and how consistent your oral care is. What most people notice first is less odor and a cleaner feeling mouth, followed by gradual brightening.
- Typical milestones (general guidance):
- First few weeks: fresher breath and less dry mouth can make teeth look less dull.
- 1–3 months: gums may look healthier, and plaque build-up often slows with good home care.
- 3–6 months: surface stains may start to look lighter, especially after a professional cleaning.
- 6–12 months: many ex-smokers see their best “natural” improvement, but deep stains usually remain without whitening.
How to Whiten Teeth Faster After Quitting
If you want noticeable shade improvement, combine strong daily habits with the right professional care. The goal is to remove stain and tartar safely without over-scrubbing enamel.
At-Home Habits That Make a Real Difference
- Brush twice a day with a fluoride toothpaste and a soft-bristled brush.
- Clean between teeth daily with floss or interdental brushes.
- Use a fluoride mouthwash if you’re prone to cavities or dry mouth.
- Rinse with water after coffee, tea, or red wine to reduce new staining.
Over-the-Counter Whitening Options
Whitening toothpastes can help polish away surface stains, but they won’t change the internal tooth shade. Whitening strips or gels can lighten teeth more effectively, but they may trigger sensitivity. If you have gum recession, cavities, or ongoing gum disease, it’s safer to get a dentist’s advice before starting.
Professional Options That Work Best for Smoker Stains
- Scaling and polishing: removes tartar and surface staining, often with an immediate visual improvement.
- In-office or dentist-supervised whitening: faster, more predictable shade change than most at-home products.
- Air polishing: a targeted way to lift stubborn surface stains during hygiene visits.
- Cosmetic dentistry (bonding or veneers): considered when stains are deep or teeth are chipped, worn, or uneven.
Other Oral Health Benefits After Quitting
A brighter smile is a nice bonus, but the bigger win is health. Quitting smoking can lower your risk of gum disease and tooth loss, and it often improves healing after dental treatments. Many people also notice less inflammation, fewer mouth sores, and a more comfortable, hydrated mouth.
When to See a Dentist
Book a dental visit if you’re struggling to improve the look of your teeth or if you have symptoms that point to gum disease. A dentist or hygienist can tell you whether stains are surface-level, check for decay, and recommend the safest whitening route.
Consider making an appointment if you have:
- Dark or patchy stains that don’t change after a cleaning.
- Bleeding gums, persistent swelling, or bad taste in the mouth.
- Tooth sensitivity, loose teeth, or receding gums.
- Old fillings or crowns in the front that no longer match the shade of your teeth.
Frequently Asked Questions
Will yellow stains disappear completely after quitting?
Some surface staining can fade once you stop smoking and keep up with cleanings. Deep brown stains that have penetrated enamel usually need whitening or cosmetic treatment to lighten significantly.
What’s the fastest way to get a whiter smile after quitting?
Start with a professional cleaning. If you still want a brighter shade, ask about dentist-supervised whitening. That combination targets both tartar-related staining and deeper discoloration.
Do whitening products damage enamel?
Used correctly, most reputable whitening products are safe for enamel. Problems tend to happen when products are overused, trays don’t fit, or there’s untreated decay or gum disease. If you’re sensitive or have recession, get personalised advice first.
Can I whiten if I have gum disease or cavities?
It’s better to treat gum disease and cavities before whitening. Whitening gel can irritate inflamed gums, and it won’t fix the underlying problem. Once your mouth is healthy, whitening results are usually better and more comfortable.
Do Carbonated Drinks Harm Teeth?
Do Carbonated Drinks Harm Teeth?
Carbonated drinks can harm teeth because their acids lower mouth pH and soften enamel. Frequent sipping—especially between meals—raises the chance of enamel erosion, sensitivity, and cavities. Sugary sodas add extra risk, but sugar‑free fizzy drinks are still acidic. Limit frequency, rinse with water, and time brushing to protect enamel.
What Counts As A Carbonated Drink?

Carbonated drinks are beverages with dissolved carbon dioxide, which creates bubbles and forms a mild acid (carbonic acid). Many brands add other acids—such as citric or phosphoric acid—for flavor and shelf life. Those extra acids are a big reason some fizzy drinks are tougher on enamel than others.
- Regular and diet sodas (cola, lemon‑lime, orange, root beer, etc.)
- Energy drinks and many sports drinks that are fizzy
- Flavored sparkling waters and “seltzers” (especially citrus flavors)
- Carbonated iced teas and ready‑to‑drink fizzy beverages
Note: Some non‑carbonated drinks—like citrus juices, kombucha, and vinegar‑based beverages—can also be acidic enough to contribute to enamel erosion. The “fizz” isn’t the only factor; acidity and how often you sip matter most.
How Carbonated Drinks Affect Teeth
Tooth enamel is strong, but it can soften when your mouth becomes acidic. After you drink something acidic, the pH in your mouth drops and minerals in enamel start to dissolve (demineralization). Saliva can repair early damage by neutralizing acid and returning minerals to the enamel (remineralization), but it needs time—especially if you sip acidic drinks over a long period.
Over time, frequent acid exposure can wear down enamel, leading to dental erosion. Erosion is different from cavities, but the two often show up together because a rough, weakened surface makes it easier for plaque to cling to teeth.
Sugar Makes The Risk Higher
Sugary carbonated drinks bring a second problem: tooth decay. Mouth bacteria feed on sugars and release acids that attack enamel. So with many sodas and energy drinks, you’re dealing with both the drink’s own acidity and the acid produced by bacteria afterward.
Signs Of Enamel Erosion To Watch For

Enamel erosion can be subtle at first. Common warning signs include:
- Sensitivity to cold, hot, or sweet foods
- Teeth that look more yellow as the underlying dentin shows through
- A dull, rough, or “chalky” appearance on the surface
- Small chips, thinning edges, or changes in tooth shape
- More frequent cavities or fillings that fail sooner than expected
If you notice these changes, a dental visit is worth it. Early erosion can often be stabilized with fluoride, habit changes, and targeted advice before it becomes a bigger restorative issue.
How To Protect Teeth If You Drink Carbonated Beverages
1) Reduce Contact Time
The longer an acidic drink sits on your teeth, the more opportunity it has to soften enamel. Try to have fizzy drinks with meals rather than sipping between meals, and avoid swishing them around your mouth.
- Use a straw (position it toward the back of the mouth).
- Finish the drink in one sitting instead of grazing on it for hours.
2) Rinse And Neutralize
After a carbonated drink, plain water helps wash acids away and supports saliva’s natural buffering effect. Sugar‑free gum can also boost saliva, which helps enamel recover.
- Drink a few sips of water right after.
- If you can’t brush, chew sugar‑free gum for 10–20 minutes.
3) Time Brushing Properly
Brushing immediately after acidic drinks can scrub softened enamel. Most dental guidance recommends waiting at least 30 minutes—and sometimes up to an hour—before brushing, depending on the acidity and your individual risk.
- If you want to freshen up sooner, rinse with water first.
- Brush with a soft‑bristled brush and fluoride toothpaste once the waiting period has passed.
4) Strengthen Enamel Day To Day
Enamel can’t grow back, but it can become more resistant to acid. A consistent routine makes a noticeable difference over time.
- Use fluoride toothpaste twice daily; your dentist may suggest a higher‑fluoride option if you’re at higher risk.
- Floss or use interdental brushes daily to reduce plaque that holds acid against teeth.
- Limit acidic snacks and drinks to set times rather than constant grazing.
Healthier Alternatives To Fizzy Drinks

If you want to cut risk without feeling deprived, these options are generally kinder to enamel:
- Still water (fluoridated tap water is a strong everyday choice)
- Milk or plain yogurt drinks (calcium and phosphate support enamel)
- Unsweetened tea or herbal tea
- Plain sparkling water without added acids or sugar (check labels for citric acid and “flavorings”)
Do Carbonated Drinks Affect Children’s Teeth More?
Children and teens can be more vulnerable because habits form early and frequent sipping is common. Baby teeth and newly erupted adult teeth can also be less resistant to acid until they fully mature. If a child regularly drinks soda, sports drinks, or energy drinks, a dentist can suggest practical swaps and fluoride strategies suited to their age.
Frequently Asked Questions
Do carbonated drinks really harm teeth?
Yes. Their acids can soften enamel and contribute to dental erosion. If the drink also contains sugar, the cavity risk goes up because bacteria produce even more acid.
Is one carbonated drink a day harmful?
It can be over time, especially if it’s sipped slowly or taken between meals. Having it with food, using a straw, and rinsing with water afterward can lower the impact.
Should I brush my teeth right after a carbonated drink?
No. Wait at least 30 minutes (and up to an hour after very acidic drinks) so enamel can reharden. Rinse with water in the meantime.
Do sugar‑free carbonated drinks harm teeth?
They can. Even without sugar, many are acidic enough to soften enamel. They may be better for cavities than sugary sodas, but they still carry an erosion risk if consumed often.
What’s the safest fizzy option for teeth?
Plain sparkling water is usually the gentlest choice. Flavored sparkling waters can be more acidic, so treat them more like a soft drink and keep them occasional.
What is a Tetracycline Tooth Stain?
What is a Tetracycline Tooth Stain?
A tetracycline tooth stain is a type of intrinsic tooth discoloration that forms when tetracycline-class antibiotics are taken while teeth are developing (during pregnancy or early childhood). The drug binds to mineralizing tooth tissue, leaving yellow, gray, brown, or blue bands that brushing can’t remove. Cosmetic dentistry can usually improve the appearance.
Tooth color changes can come from foods, smoking, trauma, aging, or certain medications. Tetracycline staining is different because it forms inside the tooth rather than sitting on the surface. That’s why a typical cleaning or whitening toothpaste won’t make it disappear.
What Are Tetracyclines?

Tetracyclines are a family of broad-spectrum antibiotics used to treat a range of bacterial infections. Common examples include tetracycline, doxycycline, and minocycline. They’re prescribed for conditions such as acne, respiratory infections, some skin infections, and certain tick-borne illnesses.
Why Tetracycline Can Stain Teeth
These antibiotics have a strong attraction to calcium. When teeth are forming, tetracyclines can become incorporated into the developing enamel and dentin. Over time, the trapped compounds can darken, especially with light exposure, creating a stain that’s built into the tooth structure.
What Tetracycline Stains Look Like
Tetracycline-related discoloration often appears as yellow, brown, gray, or blue tones. Some people notice horizontal bands across the teeth, while others see a more even, generalized change in shade. The exact color and pattern depend on the type of antibiotic, the dose, and the stage of tooth development at the time of exposure.
Who Is Most Likely To Be Affected?

Exposure During Pregnancy
Tetracyclines can cross the placenta. If taken during the later stages of pregnancy—when a baby’s primary teeth and the early parts of permanent teeth are mineralizing—staining can occur. For this reason, tetracyclines are usually avoided during pregnancy unless a clinician determines the benefits clearly outweigh the risks.
Children Under About 8 Years Old
The highest risk is in young children because many permanent teeth are still developing. When tetracycline-class antibiotics are used during this window, the discoloration can affect both baby teeth and the adult teeth that erupt later. In practice, clinicians usually choose other antibiotics for routine infections in this age group.
Long-Term Use In Teens And Adults
Most adults won’t develop classic tetracycline banding because their teeth have already formed. That said, minocycline—especially with long-term use—has been linked to staining in erupted teeth and gum tissue in some patients. If you notice new discoloration while taking a tetracycline for acne or another condition, ask your prescriber and dentist about alternatives.
Are Tetracycline Stains Permanent?
In many cases, yes. Because the discoloration sits inside the tooth, brushing, polishing, and most over-the-counter products won’t remove it. The good news is that modern cosmetic dentistry can often lighten or fully mask the stain, depending on its depth and color.
Treatment Options That Can Improve The Appearance
A dentist will usually start by checking for cavities, enamel defects, and gum health, then match treatment to the stain’s severity. Mild yellow or light brown staining may respond to conservative options, while gray or blue tones often need coverage-based solutions. Sometimes, combining treatments gives the most natural result.
Professional Whitening
In-office bleaching and dentist-supervised at-home trays can help with mild to moderate staining. Results tend to be better for yellow-brown discoloration than for deep gray-blue tones. Whitening may take longer than usual, and sensitivity management is part of the plan.
Composite Bonding
Composite bonding uses tooth-colored resin to cover discoloration and refine tooth shape. It can be a good option for smaller areas or as a budget-friendly cosmetic fix. Bonding is less durable than porcelain and may need maintenance over time.
Porcelain Veneers
Veneers are thin porcelain shells bonded to the front surfaces of teeth. They can reliably mask moderate to severe tetracycline staining, especially when banding is visible on the front teeth. A careful shade plan is essential so the veneers look bright without appearing opaque.
Full-Coverage Crowns
When discoloration is severe or the tooth also needs structural repair, a crown may be the best choice. Materials such as zirconia or porcelain-fused options can block dark internal color while restoring strength. Crowns require more tooth reduction than veneers, so dentists reserve them for the right clinical situations.
How To Prevent Tetracycline Tooth Staining

Prevention is mainly about timing and medication choice:
- Avoid tetracycline-class antibiotics in pregnancy and early childhood unless a clinician specifically recommends them.
- For children under 8, ask whether a non-tetracycline antibiotic is appropriate for the infection being treated.
- If a tetracycline is prescribed for a serious illness, follow the prescriber’s guidance and don’t stop medication without medical advice.
- Tell your dentist about any past tetracycline use so discoloration can be assessed early.
When To See A Dentist
Book an appointment if you see banding, gray-blue discoloration, or uneven tooth color that doesn’t improve with routine cleaning. A dentist can confirm whether the stain is internal, rule out other causes, and explain realistic outcomes for each treatment option. Photos and shade tracking are often helpful when planning whitening, veneers, or crowns.
Frequently Asked Questions
What is a tetracycline tooth stain?
It’s an internal (intrinsic) discoloration that forms when tetracycline-class antibiotics are taken while teeth are developing. The stain becomes part of the tooth structure, which is why brushing cannot remove it.
Do tetracycline stains fade on their own?
They typically don’t. Some teeth may look darker over time, especially with light exposure and natural aging. Cosmetic treatment is usually needed to noticeably change the appearance.
Can whitening remove tetracycline stains?
Whitening can help in mild cases, but deep gray or blue discoloration often responds poorly. Many people get the best results with whitening plus veneers or bonding, depending on the tooth and the shade.
Do all tetracycline antibiotics cause staining?
The risk is highest when tetracycline antibiotics are used during tooth development. Certain drugs in this family, such as minocycline, have also been linked to staining in erupted teeth with long-term use.
What colors can tetracycline staining be?
Shades range from yellow and brown to gray or blue. The pattern may be uniform or appear as horizontal bands across the teeth.
What is Fluoride Treatment?
What is Fluoride Treatment?
Fluoride treatment is a brief, in-office application of concentrated fluoride—usually varnish or gel—that strengthens enamel, helps repair early mineral loss, and reduces the chance of cavities. It’s commonly recommended for children and for adults who get cavities often, wear braces, or have dry mouth. Your dentist will suggest the right schedule for your risk level.
How Fluoride Protects Teeth
Fluoride is a naturally occurring mineral that supports enamel, the hard outer layer of the tooth.
When fluoride sits on the tooth surface, it helps replace minerals lost during acid attacks and makes enamel more resistant to future damage. It can also slow the activity of cavity-causing bacteria.
You get small amounts of fluoride from toothpaste, drinking water in many areas, and some foods. Professional fluoride treatments deliver a higher concentration directly where it’s needed.
Who Benefits From Fluoride Treatment
Dentists often recommend topical fluoride for people with a higher-than-average risk of tooth decay. Common examples include:
- Children as baby teeth and new permanent teeth erupt
- Adults with a history of frequent cavities
- People wearing braces or other orthodontic appliances
- Anyone with dry mouth (from medications, medical conditions, or mouth breathing)
- People with gum recession, which exposes cavity-prone root surfaces
- Patients who struggle with daily brushing and flossing
- High-sugar diets or frequent snacking and sipping sweet drinks
A quick exam helps your dentist decide whether you need fluoride varnish, gel, foam, or a prescription-strength home option.
How Fluoride Treatment Is Done
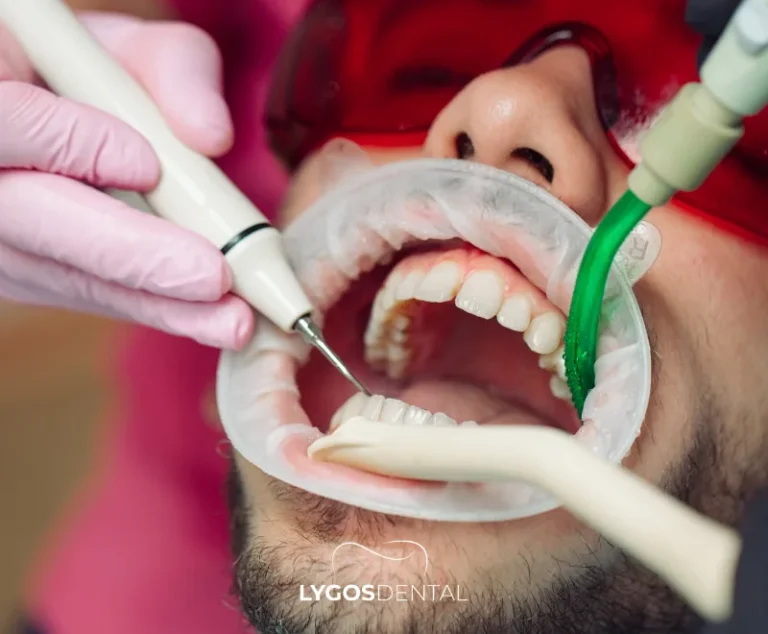
In-office fluoride treatment is simple, fast, and typically painless. A standard visit looks like this:
- Cleaning and drying: The teeth are cleaned and dried so the fluoride can contact enamel evenly.
- Application: Fluoride varnish, gel, or foam is placed on the teeth with a small brush or in a tray.
- Set time: Depending on the product, the fluoride stays on the teeth for a short period while it adheres.
- Aftercare: You’ll get instructions on when to eat, drink, and brush afterward.
Most appointments take around 5–10 minutes. The goal is prevention—strengthening teeth before small problems turn into cavities.
How Often Should You Get Fluoride Treatment?
Many children and adults do well with fluoride treatment about twice a year, often at routine checkups.
If your cavity risk is higher, your dentist may recommend applications every 3–6 months. The right frequency depends on your cavity history, diet, home care, and factors like braces or dry mouth.
Aftercare Tips
After fluoride varnish or gel, follow your dentist’s instructions. Common guidance includes:
- Avoid eating or drinking for about 30 minutes.
- For a few hours, choose soft foods and skip very hot, sticky, or hard foods.
- Avoid acidic drinks for the rest of the day if you’re prone to sensitivity.
- Keep brushing twice daily with fluoride toothpaste. If you were told to delay brushing, resume as directed.
If you’re unsure what applies to the product used in your visit, call the clinic and ask for the specific aftercare steps.
Benefits Of Fluoride Treatment
- Lowers the risk of new cavities by strengthening enamel
- Helps stop early enamel demineralization before it becomes a hole
- Supports cavity prevention around brackets and wires during orthodontic treatment
- Can reduce sensitivity by reinforcing weak enamel and exposed root surfaces
- Helps protect teeth over time, supporting long-term oral health
Safety And Possible Side Effects

Professional fluoride treatment is considered safe when applied by a dental professional in appropriate amounts.
Side effects are uncommon, but they can happen:
- Mild stomach upset if fluoride is swallowed (more likely in young children)
- Rare allergy or sensitivity to ingredients in some varnishes (tell your dentist about known allergies, including rosins/colophony)
- Dental fluorosis (white marks on developing teeth) from repeated excessive fluoride intake during early childhood—typically linked to swallowing toothpaste or supplements, not a single in-office application
Parents can reduce fluorosis risk by supervising brushing, using a smear or pea-sized amount of toothpaste as recommended for a child’s age, and helping children spit instead of swallowing.
Fluoride Treatment Cost In 2026
Fluoride treatment prices vary widely by location, clinic, and the product used. Some public health programs offer fluoride varnish to children at low or no cost, while private clinics set their own fees.
Cost is usually influenced by:
- How often you receive treatment (one-time vs. a scheduled prevention plan)
- The type of fluoride used (varnish, gel, foam, or prescription-strength options)
- Your overall oral health and cavity risk
- Whether the visit is combined with a routine cleaning and exam
- Insurance coverage or local public programs
For an accurate quote, ask your dental office after an exam. In many cases, prevention costs less than restoring cavities later.
Fluoride Treatment FAQs
What is fluoride treatment and who is it suitable for?
Fluoride treatment is a professional topical application of fluoride (often varnish or gel) that strengthens enamel and helps prevent cavities. It’s commonly used for children, but it can also help adults with frequent cavities, dry mouth, gum recession, or braces.
Does fluoride treatment hurt?
No. The application is quick and usually comfortable. You may notice a temporary coating on the teeth, especially with varnish, but there’s no drilling or numbing involved.
How long does fluoride treatment take?
Most in-office applications take about 5–10 minutes, not counting your cleaning and exam.
Is fluoride treatment harmful?
When applied by a dental professional in the correct dose, fluoride treatment is considered safe. Problems like fluorosis are typically related to long-term excessive fluoride intake in early childhood, especially from swallowing toothpaste or supplements.
What should I avoid after fluoride treatment?
Most people are advised to avoid eating or drinking for about 30 minutes. Your dentist may also suggest soft foods for a few hours and avoiding very hot, sticky, or hard foods until the varnish has set.
If you’re unsure whether fluoride treatment is right for you or your child, ask your dentist for a caries-risk assessment and a prevention plan tailored to your needs.
Laser Gum Treatment
Laser Gum Treatment
Laser gum treatment uses dental lasers to clean periodontal pockets by reducing bacteria and removing inflamed tissue. It’s used for gum disease and for cosmetic reshaping, often with less bleeding and a shorter recovery than traditional surgery. The right approach depends on your diagnosis, pocket depth, and the laser system your dentist uses.
What Laser Gum Treatment Is
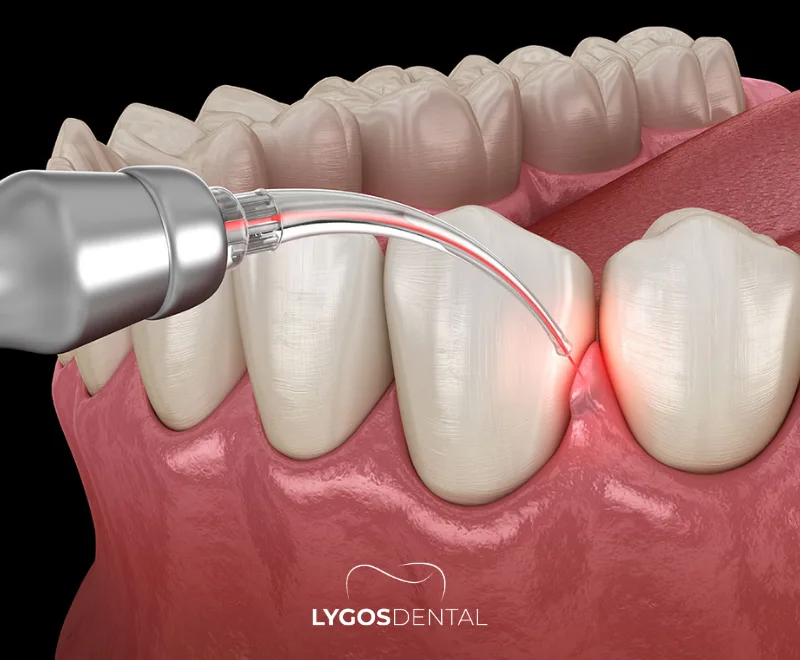
Laser gum treatment is a modern approach used to manage gum disease (periodontal disease) and certain cosmetic gum concerns. The dentist uses a dental laser to reduce bacteria and remove diseased or inflamed tissue with a high level of precision. In many cases, it’s performed as an adjunct to deep cleaning rather than as a full replacement for conventional periodontal surgery.
Different laser types are used in dentistry, and the technique matters as much as the device. Your clinician will choose a protocol based on pocket depth, the condition of the bone and gum, and whether you also need scaling and root planing (deep cleaning).
When Dentists Recommend Laser Gum Treatment
Laser-assisted periodontal therapy may be considered in several situations. Your dentist will confirm the diagnosis and decide whether laser support is appropriate for your case.
- Gingivitis: to help reduce inflammation and bacterial load alongside professional cleaning.
- Periodontitis: to access deeper pockets and support decontamination when there is attachment loss.
- Peri-implant infection: to manage inflammation around implants as part of a broader maintenance plan.
- Gum reshaping and ‘gummy smile’ correction: to contour excess tissue and improve symmetry.
- Minor soft-tissue lesions: in some cases, lasers can be used to support comfort during treatment of small oral sores (your dentist will advise).
How The Procedure Works
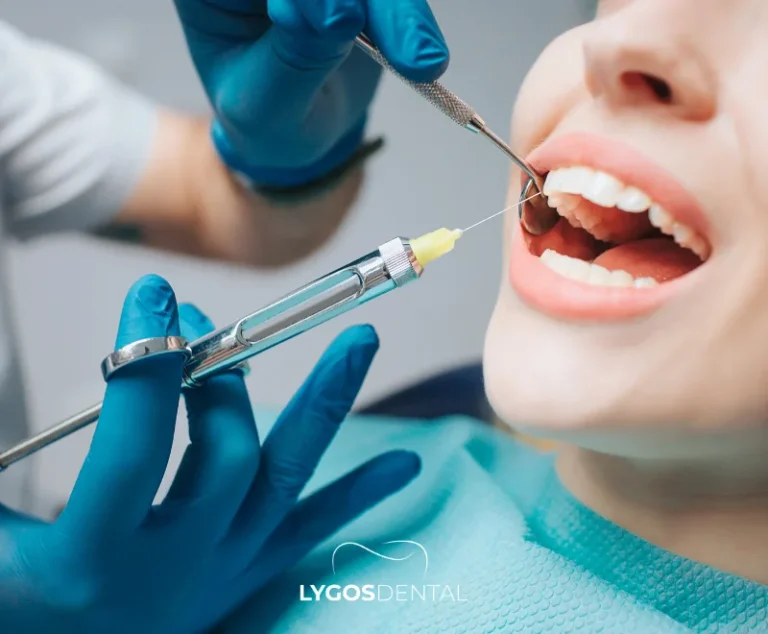
Examination And Planning
The appointment starts with a full periodontal assessment. This may include pocket measurements, X-rays, and a review of your medical history and medications. Your dentist will explain what the laser will be used for and whether deep cleaning will be done in the same visit.
Numbing And Comfort
Local anesthesia is commonly used, especially for deeper pockets. Some people feel only mild discomfort, but comfort varies from patient to patient. Your dentist can adjust numbing, suction, and cooling to keep the session manageable.
Laser Cleaning And Tissue Management
The laser is directed into the periodontal pocket to target bacteria and diseased tissue while preserving healthy gum as much as possible. Depending on the protocol, the dentist may also use ultrasonic and hand instruments to remove hardened deposits from the root surface. At the end of the session, the area is rinsed and checked for bleeding control.
Follow-Up And Maintenance
Many patients need a review visit to reassess pocket depth and gum healing. Your dentist may schedule additional sessions, particularly if multiple areas require treatment. Long-term success depends on home care and ongoing professional maintenance visits.
Benefits And Realistic Expectations
Laser-assisted therapy is valued for being less invasive in many cases. That can mean a calmer experience in the chair and a smoother early recovery.
- Less bleeding and swelling for many patients.
- No stitches for many soft-tissue applications.
- Precise work in tight areas, which can help preserve healthy gum.
- Often a quicker return to normal routines compared with surgical flap procedures.
Laser treatment is not automatically the best option for every stage of gum disease. Advanced bone loss, complex pocket anatomy, or other clinical findings may still require surgical periodontal treatment. A periodontal specialist (periodontist) can advise when laser support is appropriate.
Possible Risks And Limitations
When performed by trained clinicians with proper safety measures, dental lasers are widely used. Still, there are limits and potential downsides to know about.
- Not every case responds the same way, and some patients still need surgery or grafting.
- Temporary sensitivity or soreness can occur, especially after deep cleaning.
- Overheating and tissue irritation are possible if protocols are not followed, which is why experience matters.
- Costs may be higher than conventional cleaning, depending on the number of sessions.
Tell your dentist if you are pregnant, have diabetes, take blood thinners, or have any condition that affects healing. These factors don’t always prevent treatment, but they can change how the plan is managed.
Recovery And Aftercare

Most people return to normal activities quickly after laser-assisted gum treatment. Mild tenderness or sensitivity is common for a short period, particularly if deep cleaning was performed.
- Choose soft foods for the first 24 hours and avoid very hot or very cold drinks if you feel sensitive.
- Brush gently and follow the cleaning instructions you were given (a soft toothbrush is often recommended).
- Use any prescribed mouth rinse as directed and complete any medications if they were provided.
- Avoid smoking and alcohol during early healing, as both can slow tissue recovery.
Contact your dentist if you notice worsening pain, swelling, pus, fever, or bleeding that doesn’t settle. These symptoms are uncommon, but they deserve a prompt check.
Laser Gum Treatment Costs In Turkey
Pricing varies because clinics may charge per tooth, per quadrant, or as a package that includes deep cleaning and follow-up sessions. The laser type, the severity of disease, the city, and whether a periodontist is involved can all change the total cost.
In 2026, private clinics in Turkey commonly quote periodontal care in the low thousands of TL for limited areas, with higher totals for full-mouth, multi-session treatment or combined cosmetic procedures. The only reliable quote is the one you receive after a clinical examination and a written treatment plan.
If you have private or supplementary health insurance, ask your provider what is covered. Coverage varies, and many plans treat periodontal and cosmetic procedures differently.
Laser Gum Treatment FAQ
Does laser gum treatment hurt?
Most patients are comfortable with local anesthesia. You may feel pressure or mild sensitivity during and after the visit, especially if deep cleaning is performed. Discomfort is usually short-lived and can often be managed with your dentist’s advice.
How long does a session take?
It depends on how many areas are treated. A focused session may take around 20–60 minutes, while full-mouth treatment is usually planned over multiple visits.
Is laser gum treatment permanent?
Results can be long-lasting when gum disease risk factors are controlled. Daily brushing and interdental cleaning, quitting smoking, and regular maintenance visits are the biggest predictors of stability over time.
Who may need extra evaluation before treatment?
People with uncontrolled diabetes, immune conditions, bleeding disorders, or complex medical histories often need additional planning. Let your dentist know about all medications and any recent medical changes so the safest approach can be chosen.
What Happens If an Impacted Tooth Is Not Removed?
What Happens If an Impacted Tooth Is Not Removed?
When it comes to oral and dental health, one of the most common issues people face is impacted teeth. The question “What happens if an impacted tooth is not removed?” is frequently asked for this reason. This condition, often associated with wisdom teeth, can lead to serious complications in oral health if not treated in time. In this article, we’ll cover everything from what an impacted tooth is, why it occurs, its symptoms, and most importantly, what happens if an impacted tooth is not removed.
What Is an Impacted Tooth?
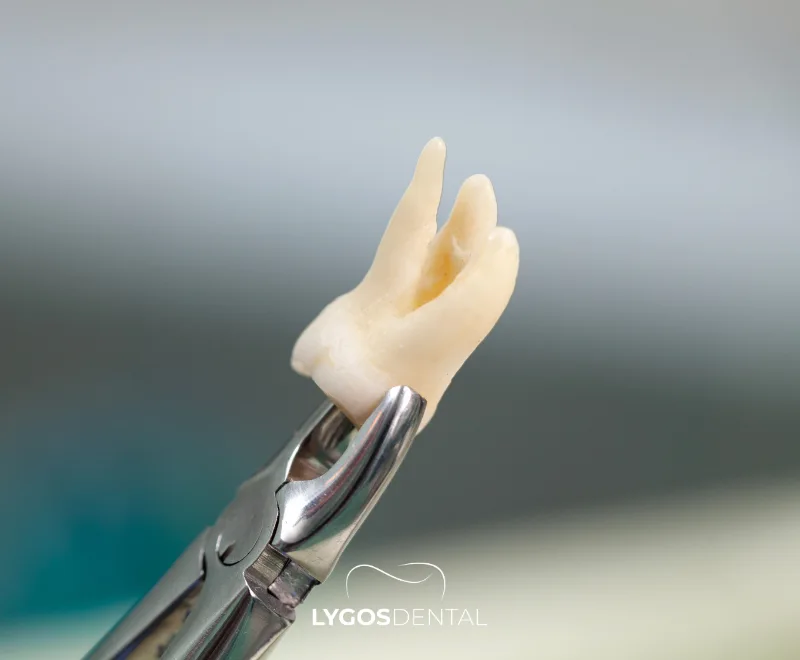
An impacted tooth is one that fails to erupt fully or partially into the mouth and remains embedded in the jawbone or gum tissue. This condition most commonly affects third molars, also known as wisdom teeth, but can also occur with canines and other molars. What happens if an impacted tooth is not removed? The answer often relates to the complications these teeth can cause over time.
While impacted teeth may sometimes show no symptoms, they often lead to pain, infection, and misalignment of adjacent teeth. Depending on their position and the individual’s jaw structure, the degree of impaction can vary. This is why the question “What happens if an impacted tooth is not removed?” becomes crucial, especially when symptoms appear.
Why Do Impacted Teeth Develop?
Several factors can lead to impacted teeth:
Narrow jaw structure: Lack of space in the jaw prevents the tooth from erupting.
Improper angling of the tooth: A tooth growing at an angle may not be able to emerge.
Genetics: A family history of impacted teeth increases the likelihood.
Delayed eruption: Wisdom teeth, in particular, tend to erupt late and may get trapped.
Retained baby teeth: These can block the eruption of permanent teeth.
Among these, jaw structure is a significant reason, and it’s closely related to the question: What happens if an impacted tooth is not removed?
What Are the Symptoms of an Impacted Tooth?
While not every impacted tooth causes symptoms, many are associated with:
Localized pain in the mouth
Swelling and redness of the gums
Difficulty opening the mouth
Bad breath
Headaches or earaches
Swollen lymph nodes
If these symptoms are present, consulting a dentist is essential, as they may indicate that the answer to “What happens if an impacted tooth is not removed?” could involve serious complications.
What Happens If an Impacted Tooth Is Not Removed?
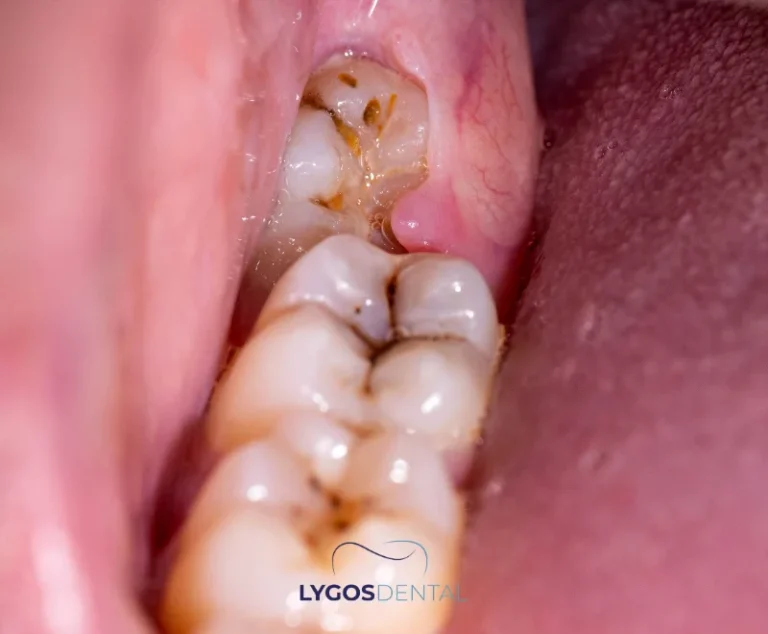
If left untreated, an impacted tooth can lead to several problems beyond the immediate area, affecting overall oral health. Here are some detailed answers to the question “What happens if an impacted tooth is not removed?”:
- Chronic Infections: Impacted teeth can trap bacteria and food particles, leading to infections such as pericoronitis. One of the primary answers to “What happens if an impacted tooth is not removed?” is recurring or chronic infections in the surrounding gum tissue.
- Cyst or Abscess Formation: Fluid-filled cysts or pus-filled abscesses may develop around the impacted tooth. These not only cause pain but can damage jawbone and neighboring teeth. So, what happens if an impacted tooth is not removed? Cystic growth and potential bone destruction are serious possibilities.
- Damage to Adjacent :Teeth An impacted tooth may exert pressure on the neighboring teeth, leading to damage, misalignment, or decay. This is one of the most direct answers to “What happens if an impacted tooth is not removed?”
- Orthodontic Problems: The pressure from an impacted tooth can misalign your bite or shift front teeth, especially if you’ve had braces in the past. What happens if an impacted tooth is not removed?—you may need orthodontic treatment again.
- Pain and Discomfort: Persistent pain is common and can affect your ability to sleep, eat, or speak comfortably. The discomfort caused is another clear outcome in the discussion of “What happens if an impacted tooth is not removed?”
Impacted Teeth That Harm the Jaw and Other Teeth

Impacted teeth don’t just stay quietly in place—they can damage surrounding tissues and structures. In this regard, “What happens if an impacted tooth is not removed?” becomes a question about bone loss in the jaw or the risk of neighboring tooth loss.
Structural deformities in the jaw or temporomandibular joint (TMJ) pain can result from untreated impacted teeth. Therefore, what happens if an impacted tooth is not removed? The risks go beyond dental health and extend into broader health concerns.
When Should an Impacted Tooth Be Removed?
Not every impacted tooth requires extraction. However, removal becomes necessary when:
There is an active infection or abscess
The impacted tooth is damaging adjacent teeth
Orthodontic treatment is planned
Oral hygiene is compromised
If left unaddressed, each of these conditions clearly answers the question: What happens if an impacted tooth is not removed? It leads to long-term damage and unnecessary complications.
What Happens If an Impacted Tooth Is Not Removed? Frequently Asked Questions (FAQ)
Is it necessary to remove all impacted teeth?
Not always. But if an impacted tooth causes pain, infection, or damage to other teeth, it must be removed. Again, what happens if an impacted tooth is not removed? It can worsen over time.
How long does pain from an impacted tooth last?
Pain may be temporary or persistent. Chronic pain is a sign that what happens if an impacted tooth is not removed? includes ongoing discomfort and inflammation.
Can an impacted tooth erupt on its own?
Rarely. Most impacted teeth remain stuck and require professional intervention. Otherwise, what happens if an impacted tooth is not removed? It may cause hidden problems.
Is surgery to remove an impacted tooth difficult?
Not usually. It’s a common procedure done under local anesthesia. Avoiding it, however, leads to the problems associated with what happens if an impacted tooth is not removed?
Can tooth loss occur due to an impacted tooth?
Yes. Pressure from an impacted tooth can damage or even cause loss of adjacent teeth. So, what happens if an impacted tooth is not removed? Potential tooth loss is one of the risks.
What is Baby Bottle Tooth Decay
What is Baby Bottle Tooth Decay? How to Take Care of Baby Teeth?
aby bottle tooth decay, also called early childhood caries, happens when an infant’s teeth are repeatedly exposed to sugary liquids—most often from sipping or falling asleep with a bottle. Sugars feed bacteria that make acid, which weakens enamel and causes cavities. Good feeding habits, daily cleaning, and early dental visits can prevent most cases.
What Is Baby Bottle Tooth Decay?
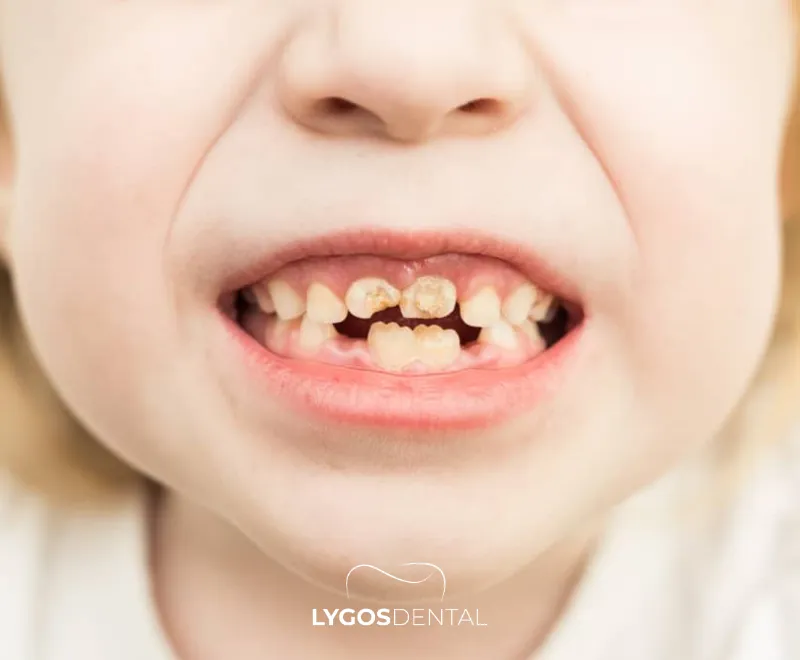
Baby bottle tooth decay is a type of early tooth decay that affects infants and toddlers. It develops when teeth are exposed to sugars for long periods—especially when a child sips sweet drinks throughout the day or falls asleep while feeding.
You may also hear it called early childhood caries (ECC). It often starts on the upper front teeth, but it can spread to other teeth if the habits that caused it continue.
Why Baby Bottle Tooth Decay Happens
Cavities form when bacteria in dental plaque use sugars from drinks and foods to produce acid. That acid attacks enamel repeatedly, and young teeth can break down quickly.
Common triggers include:
- Falling asleep with a bottle or frequently sipping from it, especially when it contains milk, formula, juice, sweetened tea, or other sugary liquids.
- Frequent snacking or drinks with added sugar between meals.
- Not cleaning gums and teeth once the first tooth erupts.
- Sweetened pacifiers (for example, dipped in honey or jam).
Which Teeth Are Usually Affected?
Baby bottle tooth decay often begins on the upper front teeth because they can be bathed in liquid during feeding. Lower front teeth are sometimes less affected because the tongue and saliva offer more natural protection.
Early Signs And Symptoms To Watch For
Early detection makes treatment easier. Look for:
- Chalky white spots near the gumline (an early sign of enamel weakening).
- Yellow, brown, or black discoloration.
- Rough areas, pits, or visible holes in the tooth.
- Sensitivity or discomfort during feeding.
- Bad breath or irritated gums.
How To Prevent Baby Bottle Tooth Decay

1) Adjust Bedtime And Bottle Habits
Try not to let your child fall asleep while sucking on a bottle. If your child needs a drink for comfort, water is the safest option for teeth.
Many pediatric guidelines encourage beginning the move from bottle to a cup around the first birthday, which can reduce the time teeth are exposed to liquids.
2) Keep Sugary Drinks Off The Teeth
Avoid offering juice or other sweetened drinks in a bottle. Milk, breast milk, and formula are best kept to feeding times, while plain water works well between meals when appropriate.
3) Start Cleaning Early And Keep It Simple
A routine that matches your baby’s age helps prevent plaque from building up. Aim for short, consistent sessions rather than long battles.
Birth to first tooth:
- Wipe the gums with a clean, damp cloth or gauze after feedings and before bed.
When the first tooth erupts:
- Brush gently twice a day with a soft, infant-sized toothbrush.
- Use a smear (grain-of-rice sized) amount of fluoride toothpaste. Keep helping with brushing and use only a tiny amount until your child can reliably spit.
Ages 3 to 6:
- Use a pea-sized amount of fluoride toothpaste and continue to help with brushing.
4) Schedule Dental Checkups Early
Book the first dental visit when the first tooth appears or by age one. Early visits help you catch early changes, review feeding habits, and get personalized guidance.
When To Call A Dentist

Contact a dentist if you see white spots, dark staining, cracks, or holes in the teeth, or if your child seems uncomfortable when eating. Early childhood cavities can progress quickly, and early care can help avoid pain and more complex treatment.
Frequently Asked Questions
Can baby bottle tooth decay be reversed?
Early white-spot lesions can sometimes be stabilized with better hygiene and professional guidance. Once a cavity forms, it usually needs dental treatment.
Does it only affect the front teeth?
It often starts on the upper front teeth, but it can spread to other teeth if sugary exposure continues and cleaning is inconsistent.
Is nighttime feeding always the problem?
Nighttime feeding can increase risk because saliva flow drops during sleep. The bigger issue is frequent, prolonged contact between teeth and sugars—especially when a child falls asleep while feeding.
What if my child refuses toothbrushing?
Keep sessions short and calm, brush at the same times each day, and use a small, soft brush. Let your child hold a second brush as a distraction, and focus on consistency rather than perfection.
How Long Should a Retainer Be Worn?
How Long Should a Retainer Be Worn?
Most orthodontists suggest wearing a retainer full-time (about 20–22 hours a day) for the first 6–12 months after braces. After that, many patients switch to nights only. Because teeth can keep drifting over time, nightly wear for several years—or longer—is common, based on your orthodontist’s plan.
What Is a Retainer?

What Is A Retainer?
A retainer is a custom-made dental appliance that helps keep teeth in the position achieved after orthodontic treatment. Depending on your case, you may have a removable clear retainer (often called an Essix retainer), a wire-and-acrylic Hawley retainer, or a fixed (bonded) retainer attached behind the teeth.
Retention is the part of treatment that protects your result. Even perfectly straight teeth can shift if the supporting tissues haven’t fully adapted.
Why Teeth Can Shift After Braces
After braces or aligners, the gums, periodontal ligaments, and surrounding bone need time to settle around the new tooth positions. During this remodeling phase, teeth are more likely to drift, especially in the first year.
Bite changes, late jaw growth, crowding tendencies, and habits such as clenching or grinding can also contribute to gradual movement over time. That’s why many orthodontists recommend long-term nighttime wear, even after the initial adjustment period.
Typical Retainer Wearing Timeline

Your orthodontist’s instructions always come first, but these timelines reflect common retention plans for removable retainers.
First 6–12 Months: Full-Time Wear
Many patients are advised to wear a removable retainer for 20–22 hours per day, taking it out only for meals and brushing. This is usually the most critical phase for preventing early relapse.
After About 1 Year: Nighttime Only
Once the teeth are more stable, wear is often reduced to nights only. If your retainer feels tight after a break, that can be a sign your teeth have started to move—resume wear and contact your orthodontist for guidance.
Two Years And Beyond: Long-Term Maintenance
Many people benefit from nightly wear for several years. In some cases—especially when there’s a higher risk of crowding or bite changes—nighttime wear may be recommended indefinitely.
Fixed Vs Removable Retainers
Fixed (Bonded) Retainers
A fixed retainer is a thin wire bonded to the back of the front teeth. Because it stays in place, it doesn’t rely on daily compliance, but it does require careful flossing and regular checks to ensure it hasn’t loosened.
Removable Retainers
Removable retainers are taken out for eating and cleaning. They’re easy to keep clean when used correctly, but skipping wear can lead to shifting that may make the retainer stop fitting properly.
Practical Tips For Wearing A Removable Retainer
- Remove your retainer before eating, and avoid chewing gum while wearing it.
- Keep it away from heat (hot water, hot drinks, dishwashers, and car dashboards), which can warp clear plastic.
- Store it in a ventilated case whenever it’s not in your mouth—never wrap it in a napkin.
- Rinse after removing it and brush your teeth before putting it back in, when possible.
- Keep it out of reach of pets; retainers are a common chew target.
- Bring your retainer to checkups so your dentist or orthodontist can confirm fit and condition.
How To Clean A Retainer

Daily Cleaning
- Rinse with lukewarm water when you take it out.
- Gently brush with a soft toothbrush and mild soap.
- Avoid toothpaste on clear retainers, since many formulas are abrasive and can leave micro-scratches.
Weekly Deep Clean
- Soak in a retainer-cleaning tablet solution, following the product directions.
- If your orthodontist approves, a short soak in diluted white vinegar can help with mineral buildup—rinse thoroughly afterward.
- Never use boiling water or harsh household cleaners.
Nighttime Wear: Why It Still Matters
Nighttime retention helps protect against subtle movement that can happen from clenching, grinding, or normal day-to-day forces. Many people don’t notice their teeth shifting until the change is visible or their retainer feels snug.
If you’ve been told to wear your retainer at night, treat it like maintenance—similar to wearing a mouthguard. It’s a small habit that can help preserve years of orthodontic work.
What Happens If You Stop Wearing Your Retainer?
Teeth can begin to drift back toward their old positions, sometimes within weeks. If your retainer no longer fits, don’t force it—contact your orthodontist, since you may need an adjustment or a replacement to avoid damaging the appliance or your teeth.
Frequently Asked Questions
How long do I need to wear a retainer after braces?
Many orthodontists recommend full-time wear for the first 6–12 months, then nighttime wear. Your schedule may be shorter or longer depending on how your teeth respond and your bite stability.
Do I have to wear a retainer for life?
Some patients are advised to wear a retainer at night long-term because teeth can shift with age. If your orthodontist recommends ongoing nighttime wear, it’s usually to prevent gradual crowding or relapse.
What if I forget to wear my retainer for a few days?
Put it back in as soon as you remember. If it feels tight or painful, wear it for shorter periods and call your orthodontist for advice—especially if the fit has changed.
What’s the difference between fixed and removable retainers?
Fixed retainers are bonded behind the teeth and stay in place, while removable retainers are taken out for meals and cleaning. Both can work well when maintained properly.
