Teeth Whitening Pen
Teeth Whitening Pen
Teeth whitening pens are small brush-on gels that can brighten mild surface stains on natural teeth when used as directed. Most people see subtle changes after several days, with best results in 1–2 weeks. Results aren’t permanent and can fade if you regularly drink coffee, tea, or wine.
What Is A Teeth Whitening Pen?

A teeth whitening pen is a slim, travel-friendly applicator filled with whitening gel. Most formulas use hydrogen peroxide or carbamide peroxide, which are common whitening agents in at-home products. You paint a thin layer of gel directly onto the front surfaces of your teeth, then let it set.
How Teeth Whitening Pens Work
Whitening gels work by breaking down stain compounds so teeth look brighter. Pens tend to deliver a smaller amount of gel and shorter contact time than trays or in-office treatments, so results are usually modest. They’re best for mild yellowing and everyday surface stains from foods and drinks.
Whitening pens only change the color of natural tooth enamel. They won’t lighten crowns, fillings, veneers, or bonding, and they may make color differences more noticeable if you have dental work on front teeth.
How To Use A Teeth Whitening Pen

Exact instructions vary by brand, so follow the label first. These steps cover the usual process and help you get more even results.
- Clean your teeth: Brush and floss (or rinse well) so the gel contacts the tooth surface, not plaque or residue.
- Dry the front teeth: Use a clean tissue or cotton pad to gently dry the teeth you plan to whiten. A drier surface helps the gel stay in place.
- Dispense a small amount: Twist, click, or squeeze the pen until a little gel appears on the brush tip.
- Apply a thin layer: Paint a light, even coat on the front surfaces of the teeth you show when you smile. Avoid the gums and lips.
- Let it set: Keep lips off your teeth while the gel dries. Many pens set in under a minute, but use the timing on your product.
- Avoid food and drinks briefly: Skip eating or drinking for about 30–60 minutes (or as directed) so the gel can do its job.
Most brands suggest using a pen once or twice daily for 1–2 weeks. Using it more often than recommended can increase sensitivity without improving results.
How Long Until You See Results?
Some people notice a small change after a few uses, especially if stains are mostly on the surface. For many users, the most noticeable improvement happens after 1–2 weeks of consistent application. If you don’t see any change after the full recommended course, the discoloration may be deeper and less responsive to pen-style products.
Results depend on things like:
- How dark the stains are and whether they’re surface stains or deeper discoloration
- How often you drink staining beverages like coffee, tea, or red wine
- Whether you smoke or vape nicotine products
- The strength of the whitening agent and how long it stays on the teeth
- How closely you follow the product directions
How Long Do Results Last?
Whitening from a pen is not permanent. Teeth can pick up new stains over time, and the brightness you gain may fade over days or weeks depending on your habits. Many people use pens for occasional touch-ups rather than ongoing daily use.
To help results last longer:
- Limit staining foods and drinks when possible, or rinse with water after having them
- Use a straw for iced coffee, tea, or colored drinks to reduce contact with front teeth
- Wait at least 30 minutes after acidic foods before brushing to protect enamel
- Keep up with daily brushing and flossing, plus regular dental cleanings
Pros And Cons Of Teeth Whitening Pens
Pros:
- Quick, simple application with minimal setup
- Portable and easy to carry for travel or events
- Lower cost than professional whitening
- Useful for touch-ups between cleanings or treatments
Cons:
- Results are usually subtle and temporary compared with trays or in-office whitening
- May trigger tooth sensitivity or mild gum irritation, especially if overused
- Not effective on crowns, veneers, fillings, or severe discoloration
- Uneven results are possible if gel touches gums or is applied inconsistently
Common Mistakes To Avoid
- Skipping brushing first: Gel works best on clean enamel, not on plaque or residue.
- Applying on wet teeth: Saliva can dilute the gel and make it slide around.
- Using too much product: A thick layer doesn’t whiten faster and can irritate gums.
- Letting gel hit the gums: Peroxide can cause temporary whitening or burning of soft tissue.
- Eating or drinking right away: Give the product time to sit so you don’t wash it off immediately.
- Overusing for “faster” results: More frequent use can increase sensitivity and doesn’t always improve whitening.
- Storing it in heat: Heat can affect the gel’s stability; keep it sealed in a cool, dry place.
Safety, Sensitivity, And Who Should Avoid Whitening Pens

When used as directed, whitening pens are generally considered safe for many adults. The most common side effect is temporary tooth sensitivity, which can happen because peroxide passes through enamel and irritates the tooth’s inner layer. Mild gum irritation can also happen if gel touches the soft tissue.
To reduce sensitivity:
- Use the pen less often or stop for a day or two if sensitivity builds
- Apply a thinner layer and avoid the gumline
- Use toothpaste for sensitive teeth and a soft-bristled brush
- Avoid very hot or cold foods for a day if your teeth feel reactive
Talk to a dentist before whitening if you have untreated cavities, gum disease, worn enamel, recent dental work on visible teeth, or persistent sensitivity. Whitening is also typically not recommended for children and should be discussed with a dentist during pregnancy or breastfeeding.
Teeth Whitening Pen FAQ
Are teeth whitening pens safe?
They can be safe for many adults when used exactly as directed and purchased from reputable brands. If you have dental pain, active gum problems, or very sensitive teeth, get advice from a dentist first.
Do teeth whitening pens cause sensitivity?
They can. Sensitivity is usually temporary and often improves when you reduce frequency or pause treatment. If sensitivity is strong or lasts more than a few days after stopping, see a dentist.
Do teeth whitening pens work on all teeth?
They work on natural teeth, mainly for mild surface staining. They do not whiten crowns, veneers, fillings, or bonding, and they may not help with deep gray or brown discoloration.
How often should you use a whitening pen?
Most products recommend once or twice daily for about 1–2 weeks, then occasional touch-ups. Don’t exceed the schedule on the label.
Can children or pregnant women use teeth whitening pens?
They’re usually not recommended for children. If you’re pregnant or breastfeeding, it’s best to check with your dentist before using any whitening product.
When To See A Dentist Instead
Consider a dental check before whitening if you have:
- Tooth pain, visible cavities, or broken fillings
- Bleeding gums, swelling, or signs of gum disease
- Dark gray, blue, or banded discoloration that may be internal
- Crowns or veneers on front teeth and you want an even color match
- Sensitivity that doesn’t settle after reducing or stopping whitening
When Should a Dental Implant Be Placed After Tooth Extraction?
When Should a Dental Implant Be Placed After Tooth Extraction?
A dental implant can be placed on the same day as an extraction, a few weeks later, or after the socket heals—often 4–8 weeks or 12–16 weeks, and sometimes 6+ months when infection, bone loss, or grafting is involved. The safest timing depends on bone, gum thickness, and your medical history.
Why Timing Matters After An Extraction
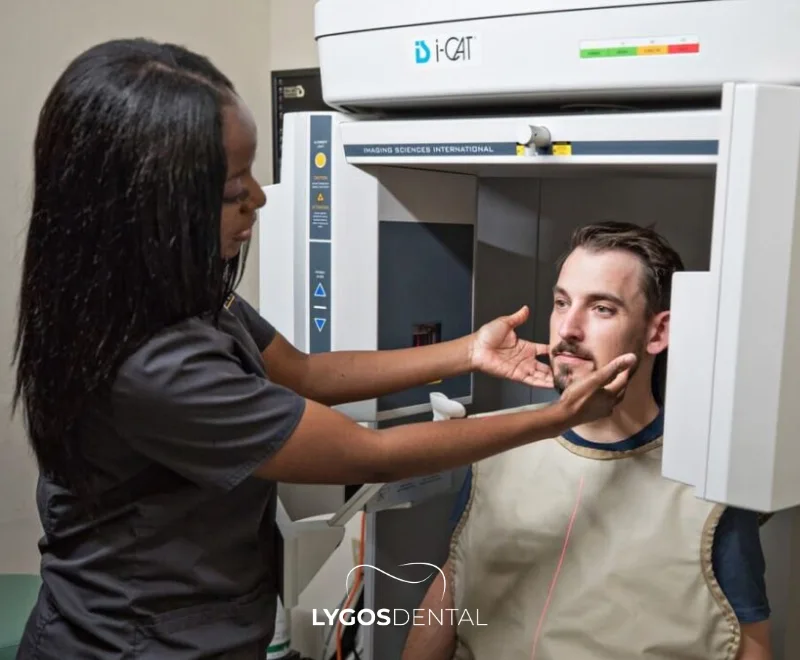
After a tooth is removed, the socket starts to heal and the jawbone naturally remodels. This is normal, but it can reduce the width of the ridge and change the gum contour—especially in the first weeks and months.
Implant timing is planned to balance three goals: placing the implant in the ideal position, achieving strong initial stability in bone, and lowering the risk of complications such as infection or gum recession. Your dentist uses an exam and imaging to decide which window fits your site.
What A Dental Implant Is And How Treatment Works
A dental implant is a small titanium or titanium-alloy post that replaces the root of a missing tooth. Over time, it bonds with the jawbone (osseointegration), creating a stable base for a crown, bridge, or denture.
Most implant treatments follow these steps:
- Assessment and planning (medical history, bite evaluation, and X-rays/3D imaging when needed)
- Tooth extraction and site management (sometimes with socket preservation grafting)
- Implant placement (either right away or after a healing period)
- Healing and integration (typically several weeks to a few months, depending on the case)
- Final restoration (crown or other prosthesis) and long-term maintenance
The best question is usually not only “how long should I wait,” but “which timing option will give the safest, most stable result for my mouth.”
Implant Timing Options After Tooth Extraction

Clinicians commonly describe four timing categories. The time ranges below are typical; your plan may differ based on anatomy, infection, and whether grafting is needed.
| Option | Typical Timing | Common Reasons To Choose It | Trade-Offs |
| Immediate (Type I) | Same visit as extraction | Healthy socket, no acute infection, enough bone for stability | Technique-sensitive; recession risk can be higher in thin tissues |
| Early With Soft-Tissue Healing (Type II) | About 4–8 weeks | Lets gums close over the socket; time to confirm infection has settled | Two procedures; some early bone remodeling occurs |
| Early With Partial Bone Healing (Type III) | About 12–16 weeks | Improves stability after more bone fill; useful after larger lesions | Longer overall timeline; ridge changes may be more advanced |
| Late / Healed Site (Type IV) | About 6+ months | When grafting, significant infection, or a planned delay is needed | More ridge resorption risk; grafting is more likely |
Immediate Implant Placement (Same Day)
Immediate placement means the implant is inserted right after the tooth is removed, during the same appointment. It can work well when the socket walls are intact, the gums are healthy, and there is enough bone to anchor the implant securely.
It may be considered when:
- There is no acute infection at the extraction site
- The facial (front) bone wall and surrounding gum tissue are thick and stable
- Your dentist can achieve strong primary stability in the correct 3D position
Immediate placement can reduce the number of surgeries and shorten total treatment time. Still, it is not the best choice for every site, especially in high-aesthetic areas with thin bone or thin gums.
Early Placement After Soft-Tissue Healing (4–8 Weeks)
In this approach, the extraction site is allowed to close with gum tissue before the implant is placed. That extra soft tissue can make it easier to manage the site and can provide a clearer picture of whether inflammation or infection has resolved.
Early Placement After Partial Bone Healing (12–16 Weeks)
Waiting a few months allows more bone fill to develop inside the socket, which can help with implant stability. This window is often considered when a larger periapical lesion or other local issue makes earlier placement less predictable.
Late Placement In A Fully Healed Site (6+ Months)
Late placement means the implant is placed after the socket has healed and remodeled. This timing is sometimes preferred when significant grafting is planned, when infection needs full resolution, or when treatment has been delayed for personal or medical reasons.
The drawback is that the ridge may shrink during healing, which can increase the need for bone augmentation to rebuild the site.
What Factors Decide The Right Timing?

Your dentist looks at site-related and health-related factors together. These are the most common decision points:
Bone volume and density: Adequate bone is needed to stabilize the implant. If the socket is thin or damaged, grafting may be recommended before or during placement.
Infection and gum disease: Acute infection is a reason to delay placement. Chronic periodontal problems may need treatment first to lower the risk of peri‑implant disease.
Gum thickness and aesthetics: Thin gums and thin facial bone carry a higher risk of gum recession, especially with immediate placement in the front of the mouth.
Need for bone grafting or sinus procedures: If ridge preservation, staged grafting, or a sinus lift is required, the timeline may extend to allow graft healing.
General health and medications: Uncontrolled diabetes, immune suppression, radiotherapy history, and certain bone medications can affect healing and risk. A tailored plan is essential.
Smoking and nicotine use: Nicotine reduces blood flow and is linked with higher implant complication and failure rates. Stopping before and after surgery improves healing.
Is Immediate Or Delayed Placement Better?
Neither option is automatically “better.” Immediate placement can be efficient, but it demands ideal anatomy and careful technique. Early or late placement can be safer when the socket is compromised, infection is present, or grafting is required.
A good plan focuses on predictable stability and healthy gums around the final crown. If your dentist recommends waiting, it is usually to protect the long-term result—not to slow the process down.
Things To Do Before And After Implant Treatment
Before Extraction Or Implant Planning
- Share your full medical history and medication list, including osteoporosis drugs and any history of radiotherapy.
- Ask whether you need a temporary tooth option during healing (flipper, bonded bridge, or temporary crown).
- If you smoke or use nicotine, plan a quit window—healing outcomes are better without nicotine.
- Treat active gum disease and keep plaque levels low before implant surgery.
After Extraction (If You Are Waiting)
- Follow the extraction aftercare instructions closely, especially for cleaning and diet in the first days.
- Keep up gentle brushing and any recommended rinses to help the gums heal.
- Ask whether socket preservation grafting is recommended to limit ridge shrinkage.
- Avoid smoking and vaping during healing, as it can slow tissue repair.
After Implant Surgery
- Stick to softer, cooler foods on day one and avoid chewing on the surgical side.
- Take prescribed medications exactly as directed and finish any antibiotics if they were prescribed.
- Maintain careful oral hygiene around the site, using the brush and interdental aids your dentist recommends.
- Attend follow-up visits so the clinician can monitor healing and the stability of the implant.
What Happens If You Don’t Replace The Tooth?
Leaving an extraction space unfilled can lead to gradual bone shrinkage in that area. Over time, nearby teeth can drift, the bite can change, and chewing efficiency may drop.
Gaps in visible areas can also affect appearance and speech clarity. If you are unsure which replacement option is best, a consultation soon after extraction keeps more choices on the table.
Frequently Asked Questions
Can a dental implant be placed immediately after tooth extraction?
Yes, same-day placement is sometimes possible. It works best when there is no acute infection and your dentist can stabilize the implant in healthy bone. In many cases, a small amount of grafting is also used to support the contour around the implant.
How long should I wait if immediate placement isn’t suitable?
A common next step is early placement after soft-tissue healing (around 4–8 weeks) or after partial bone healing (around 12–16 weeks). If grafting is needed or the site needs more time to settle, treatment may be planned for 6 months or longer.
What if I wait too long after extraction?
The longer the gap, the more the ridge tends to shrink. That can make implant placement more complex and may increase the need for bone grafting to restore the ideal shape for a stable, natural-looking crown.
Does dental implant placement hurt?
The procedure is typically done with local anesthetic, so you should not feel pain during surgery. Soreness and swelling afterward are common for a few days and are usually managed with prescribed or over-the-counter pain relief, depending on your clinician’s advice.
How do I know if I’m a good candidate for an implant?
Your dentist will assess gum health, bite forces, and bone volume using an exam and X-rays or 3D imaging. Good oral hygiene, controlled health conditions, and avoiding nicotine use generally improve candidacy and long-term success.
5 Serious Harms of Smoking on Oral and Dental Health
5 Serious Harms of Smoking on Oral and Dental Health
Smoking dries the mouth, disrupts oral bacteria, and reduces blood flow to the gums. Over time it raises the risk of gum disease, bad breath, tooth staining, slow healing after extractions or implants, tooth loss, and oral cancer. Regular dental checkups and quitting are the most effective ways to cut these risks.
Smoking affects far more than the lungs. In the mouth, tobacco smoke changes saliva, feeds harmful bacteria, and reduces oxygen and nutrients reaching the gums.
These changes make dental problems start earlier and progress faster. Below are the most common and most serious oral and dental harms linked to smoking, plus practical signs to watch for and steps that help.
How Smoking Affects The Mouth
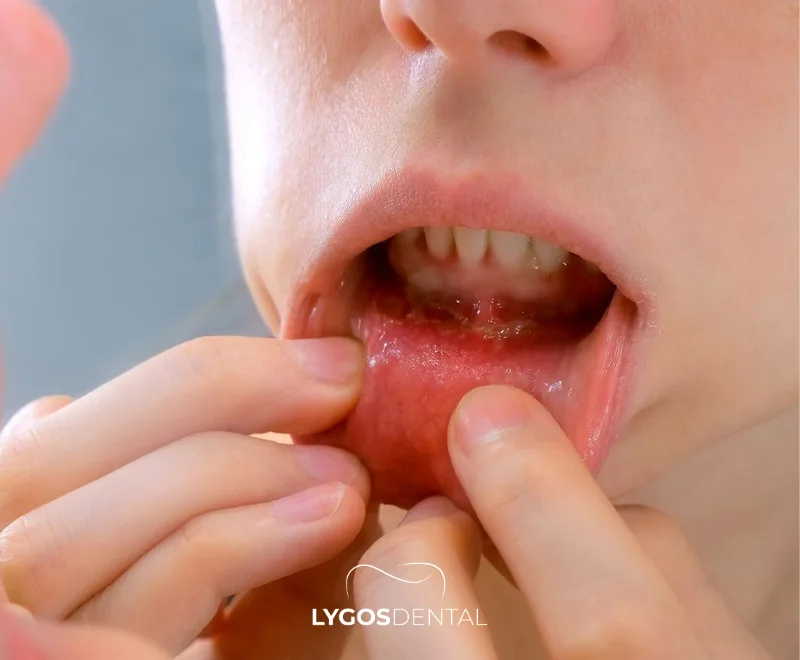
Tobacco smoke contains chemicals that irritate tissues, narrow blood vessels, and interfere with the body’s normal repair process. It also dries the mouth, which makes it easier for plaque and infection to build up.
Common effects in the mouth include:
- Less saliva (dry mouth), which reduces the mouth’s natural cleaning and buffering.
- A shift in the oral microbiome, allowing odor‑causing and disease‑causing bacteria to dominate.
- More plaque and tartar build-up, raising cavity and gum disease risk.
- Reduced blood flow to the gums, which can hide early warning signs and slow healing.
- A higher chance of infections such as thrush, especially if oral hygiene is already poor.
The 5 Most Serious Oral And Dental Harms Of Smoking

1. Higher Risk Of Gum Disease
Smoking is strongly linked to periodontal (gum) disease. When blood flow is reduced, the gums receive less oxygen and nutrients, and the immune response is weaker.
Gum disease often starts quietly with mild tenderness or bleeding, then progresses to gum recession and bone loss around the teeth. As the supporting bone breaks down, teeth can become loose and eventually fall out.
2. Persistent Bad Breath And Loss Of Taste
Dry mouth and bacterial build-up are a common recipe for long‑lasting bad breath (halitosis). Even strong mints can only mask the odor when the underlying cause is ongoing smoke exposure.
Smoking also dulls the taste buds and sense of smell. Many people notice food tastes flatter over time, which can affect appetite and meal choices.
3. Tooth Staining And Faster Tartar Build-Up
Nicotine and tar leave stubborn stains on the teeth and along the gumline. Over time, discoloration can become harder to remove, even with professional cleaning.
Smokers also tend to form tartar more quickly. That rough surface makes plaque stick, which increases the cycle of irritation and gum inflammation.
4. Slower Healing And Greater Risk Of Tooth Loss
Because smoking restricts circulation, the mouth heals more slowly after extractions, deep cleanings, implants, or other procedures. This increases the risk of infection, dry socket after extraction, and complications during recovery.
Over the long term, untreated gum disease and ongoing bone loss make tooth loss more likely. Missing teeth can affect chewing, speech, and confidence, and may lead to further shifting of nearby teeth.
5. Increased Risk Of Oral Cancer
Smoking is a major risk factor for cancers of the mouth, tongue, throat, and lips. Cigarette smoke contains thousands of chemicals, including around 70 known carcinogens that can damage DNA in oral cells.
Early detection matters. Regular dental exams help spot suspicious sores or patches before they become harder to treat.
What Can Improve After You Quit Smoking

Stopping smoking gives the mouth a chance to recover. Many people notice fresher breath, better taste, and less dryness as saliva production normalizes.
Gums also respond better to professional treatment when smoking stops. While past damage can’t always be reversed, quitting reduces the chance that gum disease and tissue changes will continue to worsen.
When To Book A Dental Checkup
Arrange a dental visit if you notice any of the following:
- Bleeding, swollen, or tender gums
- Gum recession or teeth that look “longer” than before
- Persistent bad breath or a bad taste that doesn’t go away
- Loose teeth or changes in the way your bite fits together
- Sores, lumps, or white/red patches in the mouth that last more than two weeks
Frequently Asked Questions
Does smoking cause gum disease?
Yes. Smoking increases plaque and tartar, weakens the immune response, and reduces blood flow to the gums, making gum disease more likely and harder to treat.
Does smoking cause bad breath?
Yes. Smoke, dry mouth, and bacterial build-up commonly lead to chronic bad breath.
Is teeth whitening effective for smokers?
Whitening can help, but stains often return if smoking continues. A dental cleaning first, good daily hygiene, and reducing or quitting smoking make results last longer.
Does smoking increase the risk of oral cancer?
Yes. Smoking is a major risk factor for oral cancers, and the risk rises with longer and heavier use. Regular dental exams improve the chance of early detection.
Does oral health improve after quitting smoking?
For many people, yes. Breath and taste often improve, gums heal better after treatment, and the risk of further damage drops compared with continued smoking.
How Does Wearing Braces Affect Social Life?
How Does Wearing Braces Affect Social Life?
Braces can feel socially awkward at first because they change your smile, may slightly affect speech, and require extra care when eating out. Most people adjust within a few days to a few weeks. Over time, straighter teeth often boost confidence and make smiling easier, which can improve social comfort.
Orthodontic treatment can improve bite function, oral health, and the look of your smile. At the same time, it can influence how you feel in social settings—especially early on, when the mouth is still adapting. The good news is that most social changes are temporary, and many people feel more confident as treatment progresses.
What Changes Most In The First Few Weeks

The first days with braces often come with a visible change in your smile, mild soreness, and a learning curve with cleaning. If you are a teen, you may worry about comments at school; if you are an adult, you may feel self-conscious at work or on dates. These feelings usually settle as braces become part of your normal routine.
If visibility is your biggest concern, ask your orthodontist about lower-profile options such as ceramic braces, lingual braces (behind the teeth), or clear aligners when they are appropriate for your case.
Eating Out And Social Events
Meals with friends can feel different at first because certain foods can loosen brackets or bend wires. With a few simple habits, most people keep eating out without feeling restricted.
Foods To Be Careful With
Hard, sticky, or very chewy foods are the most likely to cause problems. When you are out, choose softer options and cut food into smaller pieces so you can chew comfortably.
- Hard items: nuts, ice, hard candy, crusty bread
- Sticky items: caramel, chewing gum, toffee
- Biting hazards: whole apples, corn on the cob, thick sandwiches (cut them first)
Handling Food Stuck In Braces
Food getting caught in braces is common and can feel embarrassing, but it is easy to manage. Carry a travel toothbrush, interdental brush, or floss threaders in your bag. A quick rinse with water after eating also helps until you can brush properly.
Speaking, Smiling, And Photos

Braces change the way the lips and tongue move around the teeth, so it is normal to notice small differences at first. Most people adapt quickly, and friends typically notice far less than you do.
Temporary Pronunciation Changes
Some sounds (like ‘s’ or ‘t’) can feel different in the first week or two, especially if you have bite ramps or new elastics. Reading aloud for a few minutes a day can speed up the adjustment. If speech feels unchanged after several weeks, your orthodontist can check for a specific cause.
Feeling Confident In Your Smile
It is common to smile less in the beginning, particularly in close-up photos. As teeth start to align, many people feel more comfortable smiling and laughing again. If you feel tense in photos, practice relaxed smiles in the mirror so you know what feels natural.
Confidence And Self-Image Over Time
Confidence tends to dip at the start of treatment and rise as progress becomes visible. Seeing straighter teeth, a better bite, or reduced crowding can shift your focus from the braces to the results. For many people, that change makes social situations easier, not harder.
Communication And Other People’s Reactions
Most people are used to seeing braces and will not think twice about them. If someone makes an awkward comment, a calm response can shut it down without turning it into a big moment. Simple lines like “Yep—getting them straightened” or “Finally fixing my bite” usually move the conversation on.
Common Social Challenges And How To Manage Them

A few practical tools can prevent the situations people worry about most. These tips are especially helpful for school, work meetings, travel, and special events.
Sore spots: Use orthodontic wax on irritating brackets and rinse with warm salt water if your orthodontist says it is suitable.
Dry lips or irritation: Keep lip balm handy and drink water regularly, especially in heated or air-conditioned spaces.
Broken bracket or poking wire: Contact your orthodontist promptly; short-term fixes like wax can help until you are seen.
Worry about close-up conversations: Angle your body slightly, keep eye contact, and speak at a relaxed pace—people focus on your face, not your braces.
Feeling self-conscious: Remind yourself that treatment is temporary and the results are long-term.
Social Benefits Many People Notice
Braces are not only about appearance. They can support better oral hygiene habits, make cleaning easier as alignment improves, and reduce the discomfort that can come from a poor bite. As your smile changes, it often becomes easier to speak, laugh, and show your teeth without overthinking it.
When To Speak With Your Orthodontist
If pain, mouth sores, or speech changes feel intense or do not improve, it is worth checking in with your orthodontist. Small adjustments—like smoothing a wire, changing elastic wear, or adding wax in the right spots—can make a big difference. Getting advice early helps you stay comfortable and social throughout treatment.
Frequently Asked Questions
Does wearing braces negatively affect my social life?
Some people feel more self-conscious at first, and eating or speaking can take a little practice. As you adjust, social life usually returns to normal, and many people feel more confident as their teeth straighten.
Is it harder to speak with braces?
It can be for a short period, especially in the first week or two. Reading aloud and speaking slowly at first often helps, and most people return to their usual speech quickly.
Do braces lower self-confidence?
They can at the beginning if you are focused on the change in your smile. Confidence often improves as you see progress and feel good about investing in your long-term oral health.
Do people get socially excluded for having braces?
Braces are common, and most people are supportive or neutral. If someone teases you, keeping your response simple and confident usually ends the interaction.
Is smiling with braces something to be embarrassed about?
No. A natural smile is still a natural smile. If you feel unsure at first, give yourself time—many people end up smiling more as treatment moves forward.
Bruxism in Children (Teeth Grinding)
Bruxism in Children (Teeth Grinding)
Bruxism in children is involuntary teeth clenching or grinding, most often during sleep. It can wear down teeth, strain jaw muscles, and disturb rest. Many cases are mild and temporary, but ongoing grinding, morning jaw pain, headaches, or visible tooth wear should be assessed by a dentist to check for bite or sleep-related issues.
What Is Bruxism In Children?

Bruxism is the involuntary clenching or grinding of teeth. In children, it most commonly happens during sleep, so it may go unnoticed until a parent hears grinding or a dentist spots wear. Bruxism can affect baby teeth and permanent teeth. If it persists, it may cause muscle fatigue, tooth sensitivity, or disrupted sleep.
Signs And Symptoms Of Teeth Grinding
Children do not always report symptoms, so parents often notice changes first. Look for one or more of the following signs:
- Grinding or clicking sounds during sleep
- Jaw pain, tightness, or fatigue in the morning
- Flattened, worn, chipped, or cracked teeth
- Tooth sensitivity to cold, heat, or brushing
- Headaches, ear pain, or facial soreness
- Restless sleep, frequent waking, or daytime tiredness
- Trouble concentrating at school
If symptoms are frequent or worsening, schedule a dental visit so the cause and any tooth damage can be checked early.
Common Causes Of Bruxism In Children
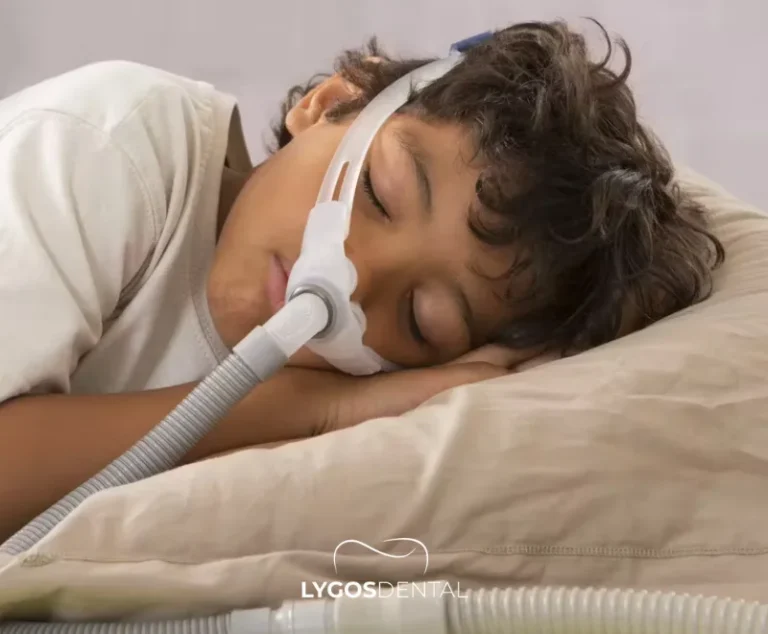
Bruxism rarely has a single cause. It is usually linked to a mix of emotional, dental, and sleep-related factors.
Stress And Emotional Triggers
Big changes can show up in a child’s sleep. School pressure, exams, family stress, anxiety, or a new routine may increase nighttime clenching. Some children also grind when they are excited or overstimulated.
Dental And Bite Changes
Teeth grinding can appear during normal growth, especially while baby teeth are falling out and permanent teeth are erupting. An uneven bite, jaw misalignment, or irritation from a loose tooth may also contribute.
Sleep Problems
Bruxism can be associated with disturbed sleep, snoring, or sleep-disordered breathing. If your child snores loudly, pauses breathing, or wakes unrefreshed, mention this to your dentist or pediatrician.
Medical, Neurological, And Developmental Factors
Some children grind more often when they have attention, sensory, or developmental differences. Certain medications and medical conditions may also play a role, so a full history helps guide next steps.
Possible Problems If Bruxism Is Left Untreated
Mild, occasional grinding may not cause harm. Persistent bruxism, though, can lead to:
- Enamel wear and increased tooth sensitivity
- Chipped teeth, cracks, or broken fillings
- Jaw joint (TMJ) pain, clicking, or limited opening
- Head, neck, or shoulder discomfort
- Poor sleep quality and daytime fatigue
How Bruxism Is Diagnosed
Diagnosis usually starts with a dental exam. Your dentist may look for tooth wear, cracks, gum recession, or jaw tenderness. They may also ask about sleep habits, stress, snoring, and daytime symptoms. If sleep-disordered breathing is suspected, your child may be referred to a pediatrician or sleep specialist.
Treatment Options For Bruxism In Children

Treatment depends on the cause, the child’s age, and whether there is tooth damage or pain. In many children, monitoring and simple habit changes are enough.
Monitoring And Reassurance
When grinding is mild and there is no pain or tooth damage, dentists often recommend watchful waiting with regular check-ups. As the bite changes during growth, bruxism may reduce on its own.
Night Guard Or Splint
A custom night guard can protect teeth by reducing direct tooth-to-tooth contact. Not every child is a candidate, especially if they are still in active tooth eruption, so the fit and timing should be decided by a dentist.
Managing Stress
If stress is a clear trigger, support at home can make a difference. For ongoing anxiety, a child psychologist or counselor may help with age-appropriate coping strategies such as play-based techniques or structured routines.
Sleep Hygiene And Routine
A consistent bedtime, screen-free wind-down time, and a calm sleeping environment can reduce nighttime arousals. Avoid stimulating drinks and heavy meals close to bedtime when possible.
Treating Underlying Conditions
If bruxism is linked to snoring, nasal congestion, reflux, or another medical issue, treating that problem may reduce grinding. Orthodontic treatment may be considered when bite or jaw alignment contributes to symptoms.
What Parents Can Do At Home
Parents can help by watching patterns and reducing triggers. Practical steps include:
- Talk with your child about worries or changes that may be affecting sleep
- Use a relaxing bedtime routine such as a warm bath, reading, or gentle music
- Keep the bedroom quiet, dark, and comfortably cool
- Encourage daytime physical activity to help release tension
- Book regular dental check-ups to monitor tooth wear
- Note when grinding happens and any related symptoms to share with your dentist
When To See A Dentist Or Doctor
Book an appointment if you notice any of the following:
- Grinding most nights for several weeks
- Morning jaw pain, headaches, or facial soreness
- Visible tooth wear, chips, or sensitivity
- Snoring, breathing pauses, or restless sleep
- Daytime tiredness or concentration problems
Prompt assessment can prevent damage and helps identify whether dental, stress-related, or sleep issues are driving the problem.
Bruxism In Children FAQ
When Does Bruxism In Children Become Dangerous?
Bruxism needs evaluation when it causes tooth wear, pain, headaches, jaw joint symptoms, or poor sleep. If your child’s quality of life is affected or you can see damage to the teeth, schedule a dental visit.
Does Bruxism In Children Resolve On Its Own?
Yes, many children outgrow bruxism as their teeth and bite change. Even so, it should be monitored so tooth wear and jaw discomfort are caught early.
At What Age Does Teeth Grinding Begin In Children?
Teeth grinding often starts between ages 3 and 6, when the mouth and jaw are changing quickly. Stress and sleep disruption can trigger it at any age.
Is Teeth Grinding A Permanent Habit?
It can continue if the trigger is not addressed. With the right support—such as stress management, sleep routines, and dental care—most children can reduce symptoms.
Can Teeth Grinding In Children Cause Sleep Disorders?
Bruxism can be linked with micro-awakenings and muscle activity that disturb sleep. Children may feel tired during the day or have attention difficulties if sleep quality drops.
The Effect of Sugary Foods on Tooth Enamel
The Effect of Sugary Foods on Tooth Enamel
Sugary foods feed plaque bacteria, which quickly make acids that soften tooth enamel. Each sugary snack triggers an acid attack for about 20 minutes, and repeated snacking keeps enamel under stress. Over time this can lead to thinning, sensitivity, and cavities. Limiting frequency and using fluoride helps protect enamel.
Oral health affects comfort, diet, and confidence. Sugar isn’t the only reason teeth decay, but frequent sweet snacks and drinks give mouth bacteria steady fuel. When that happens, enamel spends more time under acid attack, making cavities and sensitivity more likely.
What Tooth Enamel Does
Tooth enamel is the outer protective layer of each tooth and the hardest tissue in the human body. It shields the softer dentin underneath from daily wear, temperature changes, and acids in the mouth. Enamel is strong, but it isn’t living tissue, so it can’t grow back once it is lost.
How Sugar Leads To Enamel Erosion And Cavities
Sugar itself doesn’t “burn” teeth. The problem starts when sugars and refined starches sit in plaque, allowing bacteria to produce acids. Those acids pull minerals out of enamel (demineralization), leaving it softer and easier to wear down.
Why Frequency Matters More Than Amount
Each time you eat or drink something sugary, acid levels rise for roughly 20 minutes. If you sip or snack all day, enamel has little time to recover between attacks. Keeping sweets to mealtimes and cutting down on “little bites” often makes a bigger difference than perfect willpower.
Sticky Sweets And Sugary Drinks Are Tough On Enamel
Sticky foods like caramels, gummies, and dried fruit can cling to teeth and feed plaque for longer. Sugary drinks, including soda, energy drinks, and sweetened coffee, are risky because people tend to sip them slowly. A straw, drinking in one sitting, and following with water can reduce contact time.
Signs Your Enamel May Be Wearing Down

Enamel wear can happen gradually, so the early signs are easy to miss. If you notice any of the changes below, a dentist can check whether enamel loss, decay, or grinding is involved.
- Sensitivity to cold, hot, or sweet foods.
- Teeth that look more yellow as the dentin shows through.
- Rough edges, small chips, or a glassy/shiny look on the tooth surface.
- More frequent cavities, especially near the gumline.
- Translucent or “see-through” tips on front teeth.
Practical Ways To Protect Enamel If You Eat Sweets
You don’t need a perfect diet to protect enamel. The goal is to lower how often teeth are exposed to sugar and acid, and to strengthen enamel with fluoride and good daily habits.
- Brush twice a day with fluoride toothpaste and a soft-bristled brush.
- Spit after brushing instead of rinsing so fluoride stays on the teeth longer.
- Floss once a day to remove plaque between teeth where a brush can’t reach.
- Keep sugary foods and drinks to mealtimes and avoid frequent grazing.
- Choose water or milk between meals; rinse with water after sweets when you can.
- See a dentist regularly for early detection and personalized prevention.
Oral Care After Sugary Snacks
Right after you’ve had something sweet, your enamel is more vulnerable. A few simple steps help neutralize acids and clear sugars before you brush.
Wait Before Brushing
If the snack or drink was acidic (for example, soda, citrus, or sour candy), avoid brushing straight away. Waiting at least 30 minutes gives saliva time to buffer acids and lets enamel reharden. If you can’t wait that long, rinse with water first and brush gently.
Quick Steps That Help
- Rinse with water to wash away sugars and dilute acids.
- Chew sugar-free gum (ideally with xylitol) for 10–20 minutes to boost saliva.
- Use a fluoride mouthwash at a different time from brushing if your dentist recommends it.
- Clean your tongue gently; plenty of bacteria live there.
Lower-Sugar Swaps That Are Kinder To Teeth

No sweetener is completely “tooth-proof,” but some choices are less likely to feed acid-producing bacteria. Texture matters too: sticky foods tend to linger on teeth.
- Stevia or other non-sugar sweeteners in drinks instead of added sugar.
- Xylitol-sweetened gum or mints, which don’t fuel the same bacteria and may help lower cavity risk.
- Whole fruit instead of candy or dried fruit; the water and fiber reduce how long sugars stick around.
- Plain yogurt, cheese, or nuts as snacks when you want something satisfying without a sugar hit.
- If you choose honey or dates, treat them like any other sugar and keep them to mealtimes.
Sugary foods can damage tooth enamel over time, mainly when they’re eaten or sipped frequently. The good news is that small changes—fewer sugary “moments” in the day, smart timing around brushing, and consistent fluoride use—can make a real difference. If you’re dealing with sensitivity, visible wear, or frequent cavities, ask your dentist about tailored prevention and enamel-strengthening options.
Frequently Asked Questions
How do sugary foods damage tooth enamel?
Sugary foods feed plaque bacteria, which produce acids. Those acids pull minerals from enamel and make it softer, increasing the risk of erosion and cavities. Frequent snacking keeps the cycle going.
How quickly can sugar start affecting my teeth?
Acid levels can rise within minutes of eating or drinking sugar and stay elevated for around 20 minutes. Every new snack or sip restarts the process, which is why frequency matters so much.
Is fruit sugar (fructose) also harmful to teeth?
All sugars can be used by plaque bacteria. Whole fruit is usually less of a problem than sweets because it contains water and fiber and is typically eaten faster. Dried fruit and fruit juices are more likely to stick to teeth or be sipped slowly.
Can tooth enamel grow back once it’s damaged?
Lost enamel doesn’t regrow, but early weakening can sometimes be stabilized through remineralization. Fluoride toothpaste, saliva, and dentist-recommended treatments can help strengthen remaining enamel and slow further loss.
Is It Possible to Treat Baby Teeth?
Is It Possible to Treat Baby Teeth?
Yes. Cavities and damage in baby teeth can be treated with fillings, small crowns, and pulp therapy (pulpotomy or pulpectomy) when the nerve is affected. Treating baby teeth prevents pain and infection, supports chewing and speech, and helps permanent teeth erupt in the right position.
Baby teeth may be temporary, but they do a full-time job: they help children chew comfortably, speak clearly, and hold space for the adult teeth developing underneath. When a baby tooth has a cavity or injury, treating it early usually means simpler care and less discomfort for your child.
Table of Contents
Why Treating Baby Teeth Matters

Leaving decay untreated can lead to pain, swelling, and infection. Infections in a baby tooth can also affect the nearby gums and, in some cases, the developing permanent tooth.
Early tooth loss may cause neighboring teeth to drift into the empty space. That can make it harder for the permanent tooth to erupt in the right place and may increase the chance of crowding later on.
When Baby Teeth Erupt And Fall Out
Most children get their first baby tooth around 6 months of age, and the full set of 20 baby teeth usually comes in by about age 3.
Baby teeth typically start to loosen around age 6. The transition to adult teeth often continues until around ages 12–13, depending on the child.
Common Signs Of Cavities Or Infection

Cavities can be easy to miss early on, especially on the back teeth and between teeth that touch. Call a dentist if you notice any of the following:
- White, brown, or black spots on a tooth
- Sensitivity to cold, hot, or sweet foods
- Toothache, crying while eating, or avoiding chewing on one side
- Bad breath that doesn’t improve with brushing
- Swollen, red, or bleeding gums near a tooth
- A pimple-like bump on the gum (possible sign of infection)
- A chipped or broken tooth after a fall
How Dentists Treat Baby Teeth
The right treatment depends on your child’s age, the size of the cavity, and whether the tooth’s nerve (pulp) is involved. A dentist may use an exam and, when needed, X‑rays to confirm what’s happening under the surface.
Preventive Care: Fluoride And Sealants
If a cavity is just starting, dentists may focus on prevention to stop it from getting worse. This can include professional fluoride, guidance on brushing, and sealing deep grooves on back teeth if they are at higher risk for decay.
In some cases, a dentist may recommend silver diamine fluoride (SDF) to help slow or stop early decay, especially when traditional treatment needs to be delayed.
Fillings For Early Cavities
When decay is limited to the outer layers of the tooth, a filling is often enough. The dentist removes the decayed area and restores the tooth with a child‑safe material, commonly tooth‑colored composite.
Local anesthetic may be used to keep your child comfortable. After the filling, the tooth can usually function normally the same day.
Crowns For Larger Cavities Or Broken Teeth
If a baby tooth has a large cavity or a weak, broken structure, a crown may protect it better than a filling. Stainless steel crowns are commonly used on back baby teeth because they are durable and cover the whole tooth.
Crowns help children chew without pain and reduce the risk of the tooth breaking again.
Pulpotomy And Pulpectomy (Baby ‘Root Canal’)
If decay reaches the nerve, the dentist may recommend pulp therapy rather than removing the tooth. A pulpotomy treats an inflamed nerve in the crown of the tooth, while a pulpectomy removes infected tissue from the crown and roots.
In primary teeth, the canals are filled with a resorbable material designed for baby teeth. The goal is to keep the tooth in place until it is ready to fall out naturally.
When Extraction Or Space Maintainers Are Needed
Sometimes a baby tooth can’t be saved—for example, if the infection is severe or the tooth is badly broken. In those situations, removing the tooth may be the safest option.
If a tooth is lost early, the dentist may recommend a space maintainer to help keep room for the permanent tooth and reduce the risk of future crowding.
When To Take Your Child To The Dentist
The American Academy of Pediatric Dentistry recommends the first dental visit by age 1 or within 6 months of the first tooth appearing. Early visits help establish a routine and catch small issues before they turn into painful problems.
Book an appointment sooner than a routine checkup if your child has tooth pain, swelling, a fever with dental symptoms, or a tooth injury after a fall.
How To Help Prevent Cavities At Home
Prevention is usually easier than treatment. These habits make a real difference:
- Brush twice a day with a soft toothbrush. For young children, an adult should do or supervise brushing.
- Use fluoride toothpaste in the right amount: a smear (about a grain of rice) for children under 3, and a pea‑sized amount for ages 3–6.
- Floss once a day when two teeth touch and food gets stuck between them.
- Limit frequent sugary snacks and drinks. Sipping juice, sweetened milk, or soda over long periods is especially hard on teeth.
- Avoid putting a child to bed with a bottle or sippy cup containing anything other than water.
- Keep regular dental checkups so small cavities are found early.
Frequently Asked Questions
Can rotting baby teeth be fixed?
Yes—dentists remove decay with fillings, crowns, or extraction, then prevent recurrence.
What is the 3-3-3 rule for teeth?
Brush 3 times daily for 3 minutes and replace your toothbrush every 3 months.
Is it worth fixing cavities in baby teeth?
Yes—treating cavities prevents pain, infection, early tooth loss, and chewing/speech problems.
What age is late for baby teeth?
After about age 13, keeping baby teeth is considered late and needs evaluation.
Do baby teeth rot over time?
No—baby teeth decay when plaque and sugars persist; time alone doesn’t cause rot.
Dentinogenesis Imperfecta
Dentinogenesis Imperfecta
Dentinogenesis imperfecta is an inherited dentin defect that can make teeth look blue‑gray or yellow‑brown and wear down faster than normal. Because the dentin layer is weak, enamel may chip and teeth can fracture. A dentist can confirm the diagnosis with an exam and X‑rays, then plan protective restorations to preserve chewing and appearance.
Table of Contents
What Is Dentinogenesis Imperfecta?
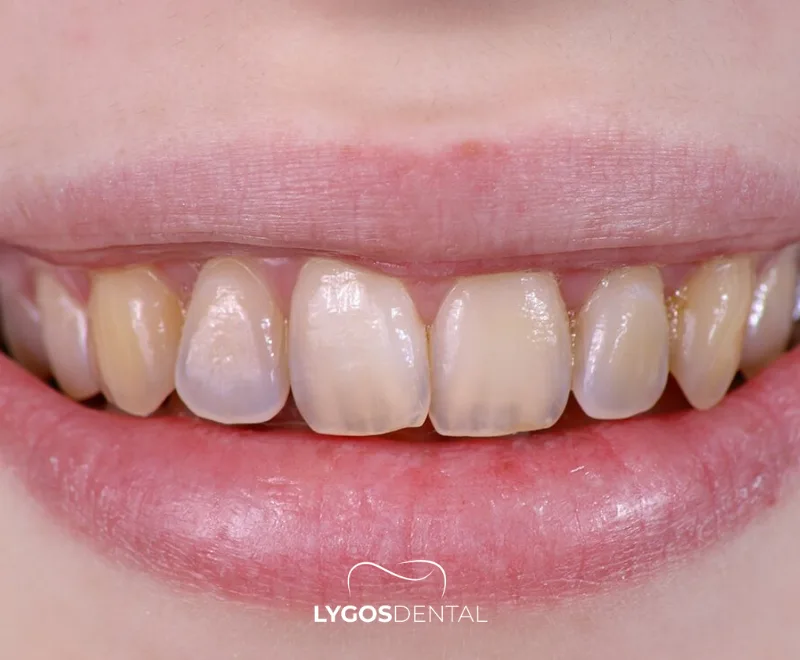
Dentinogenesis imperfecta is a genetic condition where the dentin (the layer under the enamel) forms abnormally. As a result, teeth may look darker, appear more translucent or “opalescent,” and wear down or fracture more easily than expected.
It can affect primary teeth, permanent teeth, or both. Because dentin supports enamel, even a thin chip in the enamel can expose weaker dentin and accelerate breakdown.
Signs And Symptoms
Symptoms can vary by age and severity. Many people notice changes in color or rapid wear early on, often in the front teeth.
- Tooth discoloration (yellow‑brown, amber, or blue‑gray tones)
- A dull or opalescent appearance with reduced natural shine
- Enamel chipping or peeling away from the underlying dentin
- Fast tooth wear (attrition) and a higher risk of fractures
- Teeth that look rounded or “bulbous,” with short or narrow roots on X‑rays
- Sensitivity to hot or cold if dentin becomes exposed
- In some cases, increased risk of cavities due to weakened tooth structure
Children and teens may feel self‑conscious about the appearance of their teeth. Supportive, early care often helps protect both confidence and function.
Causes And Genetics
Dentinogenesis imperfecta is most often inherited in an autosomal dominant pattern, so a parent with the condition may pass it on to a child. In many non‑syndromic cases, the cause is a pathogenic variant in the DSPP gene, which plays a key role in dentin formation.
Some people have dentinogenesis imperfecta as part of osteogenesis imperfecta (a connective‑tissue disorder). In those cases, the dental findings can be linked to collagen gene variants (such as COL1A1 or COL1A2) that also affect bone strength.
Types Of Dentinogenesis Imperfecta

Clinicians commonly describe dentinogenesis imperfecta using three types. The types help explain whether the condition is linked to osteogenesis imperfecta and what is seen on dental X‑rays.
Type I (Associated With Osteogenesis Imperfecta)
Type I occurs alongside osteogenesis imperfecta. Teeth can be discolored and prone to wear, and patients may also have signs such as frequent fractures or blue‑tinted sclerae. Dental management typically requires coordination between dental and medical teams.
Type II (Non‑Syndromic)
Type II is the most common form and affects the teeth without osteogenesis imperfecta. Both primary and permanent teeth may show discoloration, enamel chipping, and accelerated wear. X‑rays often show bulbous crowns, cervical constriction, and reduced or obliterated pulp spaces.
Type III (Brandywine Type)
Type III is rare and was first described in the Brandywine population in the United States. Teeth can have severe wear and breakage early in life. Radiographs may show unusually large pulp chambers and thin dentin, sometimes described as a “shell tooth” appearance.
How It Is Diagnosed
Diagnosis is usually made by a dentist based on a clinical exam and dental imaging. Family history is helpful, since similar tooth changes across generations can point to an inherited dentin disorder.
- Clinical examination for discoloration, enamel loss, rapid wear, and fractures
- Dental X‑rays to evaluate crown shape, root form, dentin thickness, and pulp chamber size
- Review of medical history for signs of osteogenesis imperfecta or other connective‑tissue disorders
- Genetic testing in selected cases, especially when the diagnosis is unclear or there is a suspected syndrome
Treatment Options
There is no way to change the genetic cause, but treatment can protect teeth and improve function and appearance. The plan depends on age, severity, and how much tooth structure has already been lost.
Prevention And Protection
- Regular dental checkups with a focus on early wear and fracture prevention
- Fluoride and tailored home care to reduce decay risk
- Protective coatings or sealants when appropriate
- Night guards for people who grind their teeth
Restorative Care
- Tooth‑colored fillings or bonding for small chips and defects
- Full‑coverage crowns (including ceramic or zirconia options) to protect teeth with significant wear
- In children, full‑coverage restorations may be used to preserve primary teeth and maintain bite height
Orthodontics
Braces or aligners can be used when needed, but planning should account for fragile enamel and dentin. Your orthodontist may coordinate with a restorative dentist to protect teeth throughout treatment.
Prosthetics And Implants
When tooth loss is extensive, fixed or removable prosthetics can restore chewing and appearance. Dental implants may be an option for adults once jaw growth is complete and overall oral health is stable.
Follow‑Up And Support
Long‑term maintenance matters because teeth can continue to wear over time. Many patients benefit from scheduled monitoring, preventive cleanings, and timely repair of chips before they become larger fractures.
Frequently Asked Questions
What is the difference between Type 1 and Type 2 dentinogenesis imperfecta?
Type 1 occurs with osteogenesis imperfecta; Type 2 occurs without systemic bone disease.
How rare is dentinogenesis imperfecta?
About 1 in 6,000–8,000 people have dentinogenesis imperfecta.
How to differentiate between amelogenesis imperfecta and dentinogenesis imperfecta?
Amelogenesis imperfecta affects enamel; dentinogenesis imperfecta affects dentin with opalescent, fragile teeth.
What is a tulip shaped tooth seen in?
Dentinogenesis imperfecta causes tulip-shaped crowns from cervical constriction at the cementoenamel junction.
Which cultures don’t brush their teeth?
No culture universally skips oral hygiene; many clean teeth using chewing sticks or rinses.
How To Find A Pediatric Dentist Near Me?
How To Find A Pediatric Dentist Near Me?
To find a pediatric dentist near you, start with your insurance directory and the American Academy of Pediatric Dentistry’s dentist finder, then compare reviews and office hours. Call to confirm child-friendly services, comfort options, and emergency coverage. Choose a dentist who explains care clearly and makes your child feel safe.
Finding the right dentist for your child is about more than convenience. The goal is to choose someone trained to care for growing mouths, communicate in kid-friendly language, and help your child feel calm during visits.
The steps below will help you narrow your options quickly and book with confidence, whether you are scheduling a first checkup or looking for a new dental home after a move.
Table of Contents
Why A Pediatric Dentist Matters

Pediatric dentists complete extra training focused on children’s oral development, behavior guidance, and preventive care. That specialization can be useful for everything from teething questions to cavity risk, sports mouthguards, and habits like thumb-sucking.
A good fit can also shape how your child feels about dental care long term. When visits feel predictable and supportive, kids are more likely to keep up with checkups as they grow.
When To Start Looking
Most professional guidelines recommend a first dental visit by age one, or within six months of the first tooth coming in. Early appointments are usually short and focus on prevention, feeding and brushing tips, and spotting problems early.
If your child has tooth pain, swelling, white or brown spots, or has had an injury to the mouth, book sooner rather than waiting for a routine slot.
What To Check Before You Book
Credentials And Training
Look for a dentist who completed a pediatric dentistry residency. Many practices also highlight board certification through the American Board of Pediatric Dentistry, which can be a helpful signal of advanced training and ongoing standards.
Experience With Kids
Pay attention to how the team talks about children who are shy, neurodivergent, or anxious. The right office will describe clear behavior guidance approaches and explain how they keep appointments comfortable and unhurried.
Office Atmosphere And Scheduling
A welcoming waiting area helps, but the real tell is how staff interact with families. Ask about appointment times, wait times, and whether the dentist offers early-morning or after-school visits.
Location matters too. A nearby office reduces stress on busy days and can be critical if your child ever needs same-day care.
Communication And Parent Involvement
Choose a dentist who explains findings in plain language and gives practical home-care guidance. You should leave appointments knowing what to watch for, how to brush and floss for your child’s age, and when to return.
Insurance, Pricing, And Policies
Confirm that the office accepts your plan and is taking new patients. If you are paying out of pocket, request typical fees for an exam, cleaning, X-rays, and common fillings, plus any payment plans.
Also ask about cancellation policies, who you can contact after hours, and how emergencies are handled.
Reviews And Recommendations
Online reviews can highlight patterns such as gentle chairside manner or long wait times. Balance those with recommendations from your pediatrician, local parent groups, and friends whose children have similar needs.
Ways To Find Pediatric Dentists Near You

Use Trusted Directories
Start with your dental insurance provider directory to identify in-network offices. If you want to confirm specialty training, you can also search professional directories such as the American Academy of Pediatric Dentistry’s “Find a Pediatric Dentist” tool or the American Board of Pediatric Dentistry roster.
Ask Your Pediatrician Or School Community
Pediatricians and school nurses often know which offices are responsive with kids. Local parent groups can be helpful for practical details, like which dentists are patient with toddlers or work well with children who have sensory sensitivities.
Shortlist And Call
Create a shortlist of three to five offices and call each one. A two-minute conversation with the front desk can reveal a lot about availability, policies, and how the team treats families.
If possible, stop by the office before your child’s appointment. You will get a quick sense of cleanliness, pacing, and whether the environment feels calm.
Questions To Ask On The Phone
- Are you accepting new pediatric patients, and how soon is the next routine appointment?
- What ages do you see, and do you treat teens as well?
- Do you offer same-day visits for tooth pain or injuries?
- How do you help anxious children feel comfortable?
- What comfort options do you offer (for example, nitrous oxide), and when are they used?
- Which insurance plans are in-network, and what are the expected out-of-pocket costs?
- Who can I contact after hours if my child has an urgent issue?
How Often Should Your Child Visit The Dentist?

For many children, a checkup and cleaning every six months is a common schedule. Your dentist may suggest more frequent visits if your child is at higher risk for cavities, has orthodontic concerns, or needs closer monitoring.
Consistency helps kids get used to the routine, which often lowers anxiety over time.
Planning For Dental Emergencies
Before an emergency happens, save the office number and confirm their urgent-care process. Ask what to do after hours, how quickly they can usually see a child with pain, and whether they refer to an emergency clinic on weekends or holidays.
If your child has a knocked-out or badly chipped tooth, facial swelling, bleeding that will not stop, or trouble breathing, seek urgent medical care right away.
Frequently Asked Questions
How to choose the right pediatric dentist for your child?
Choose a board-certified pediatric dentist with child-friendly office, good reviews, and emergency access.
What is the rule of 7 in pediatric dentistry?
It’s a milestone guide: dental checks at ages 1, 7, 14, and 21.
When should your child see a pediatric dentist?
Schedule the first visit by age 1, or within six months of first tooth.
What is the 2 2 2 rule in dentistry?
Brush twice daily for two minutes and see a dentist twice yearly.
Do kids get teeth at 4 or 5?
Most kids have all baby teeth by 3; permanent teeth erupt around 6.
First Aid For Children’s Dental Emergencies
First Aid for Children’s Dental Emergencies
If your child has a dental injury, stay calm, check for serious bleeding or head injury, and call a dentist right away. For a broken tooth, rinse gently and save any pieces. For a knocked-out permanent tooth, hold it by the crown, keep it moist in milk or saline, and get urgent care—ideally within 60 minutes.
Table of Contents
Kids are active, and bumps to the mouth happen—playground falls, sports collisions, and sudden tooth pain are common. Knowing what to do in the first minutes can reduce pain, lower infection risk, and improve the chance of saving a tooth.
This guide covers the most common dental emergencies in children, what you can do at home, and when you should seek urgent dental or medical care.
Common Dental Emergencies In Children
- Chipped, cracked, or broken teeth (from falls, sports, or biting something hard).
- Knocked-out teeth (avulsion).
- Toothache or swelling (often linked to cavities or infection).
- Baby-tooth injuries (loose, displaced, or knocked out).
- Cuts to the lips, tongue, cheeks, or gums.

First Steps For Any Dental Injury
- Keep your child calm and seated. If there’s dizziness, vomiting, confusion, or loss of consciousness, treat it as a possible head injury and seek emergency medical help.
- Check breathing and look for objects that could be swallowed or inhaled (broken tooth pieces, blood clots).
- Control bleeding with gentle, steady pressure using clean gauze or a cloth.
- Use a cold compress on the outside of the cheek for 10 minutes on/10 minutes off to reduce swelling and discomfort.
- Call your child’s dentist as soon as you can—most offices can guide you and arrange urgent care.
Broken Or Cracked Tooth
What To Do Right Away
- Rinse the mouth gently with warm water or saline. Avoid vigorous swishing if the area is bleeding.
- Find and save any broken pieces. Keep them in a clean container; your dentist may be able to reattach a fragment.
- If there’s bleeding, apply gentle pressure with gauze for 10 minutes.
- If a sharp edge is cutting the cheek or tongue, cover it with dental wax (if you have it) or a piece of sugar-free chewing gum until you reach a dentist.
- Offer age-appropriate pain relief if needed (follow the label directions).
When It’s Urgent
Seek same-day dental care if the tooth is sensitive to air or temperature, the crack looks deep, the tooth is loose, or you can see a pink/red area (possible nerve exposure). Go to urgent medical care or the ER if bleeding won’t stop, your child has trouble breathing, or there are signs of a head or jaw injury.
Knocked-Out Tooth (Avulsion)
If It’s A Permanent Tooth
Time matters. A knocked-out permanent tooth has the best chance of survival when it’s replanted quickly or kept moist and seen by a dentist as soon as possible (ideally within 60 minutes).
- Pick up the tooth by the crown (the white chewing surface), not the root.
- If it’s dirty, rinse briefly with running water or saline for a few seconds. Do not scrub or use soap.
- If your child is cooperative and you feel confident, gently try to place the tooth back into the socket and have the child bite on gauze to hold it in place.
- If you cannot reinsert it, keep the tooth moist in cold milk, saline, or the child’s saliva (for older children who can safely hold it in the cheek). Avoid storing it in plain water.
- See a dentist immediately.
If It’s A Baby Tooth
Do not put a baby tooth back into the socket. Reimplanting can damage the developing permanent tooth underneath. Control bleeding with gauze, use a cold compress, and arrange prompt dental assessment.
Toothache In Children
Toothache is often a sign of decay, a loose filling, or infection. Home care can reduce discomfort, but it doesn’t replace an exam—especially if pain lasts more than a day or swelling appears.
- Rinse with warm water. If your child is old enough to spit safely, a warm salt-water rinse can help soothe irritated gums.
- Use dental floss to remove food stuck between teeth.
- Use a cold compress on the outside of the cheek if there’s swelling or the pain followed an injury.
- Use age-appropriate pain relief as directed on the label. Do not place aspirin or other painkillers directly on the gums.
Call a dentist urgently if your child has facial swelling, fever, pus, a bad taste in the mouth, pain that wakes them from sleep, or trouble opening the mouth. If there is swelling under the jaw, difficulty swallowing, or breathing problems, seek emergency medical care.
Cuts To Lips, Tongue, Or Cheeks
- Rinse gently with cool water to clear blood and debris.
- Apply steady pressure with clean gauze for 10–15 minutes.
- Use a cold compress to reduce swelling.
- Seek urgent care if the cut is large, deep, gaping, caused by an animal/human bite, or bleeding won’t stop.
When To See A Dentist Or Emergency Care Immediately
- A knocked-out permanent tooth.
- A tooth that is loose, pushed out of position, or very sensitive after trauma.
- Deep cracks, visible nerve exposure, or severe pain.
- Swelling of the face or gums, fever, or signs of infection.
- Bleeding that does not stop after 10–15 minutes of firm pressure.
- Jaw pain, trouble opening the mouth, or any signs of head injury.
Dental first aid is about protecting the area and buying time until a professional can treat the cause. If you’re unsure, call a dentist—getting advice early is usually the safest choice.
Frequently Asked Questions
What is the 3 3 3 rule for toothache?
No single accepted definition; it often means 600 mg ibuprofen three times daily, three days.
What to do if a child has a dental emergency?
Call dentist immediately; manage pain/bleeding, save the tooth in milk, seek ER for breathing.
What is the 7 4 rule for tooth eruption?
First tooth erupts near 7 months, then about 4 new teeth every 4 months.
What is the first aid for a dental emergency?
Rinse, apply pressure to bleeding, cold compress, preserve tooth in milk, seek urgent care.
How to treat toothache in children?
Use cold compress, saltwater rinse, children’s acetaminophen/ibuprofen as directed, and see dentist.
