What Are Braces? Types, Benefits, Treatment Time, And Costs
What Are Braces? Orthodontic Treatment And Costs
Braces are orthodontic appliances that use brackets and wires to gradually move teeth into healthier alignment and improve the bite. They’re used for crowding, spacing, and jaw or bite problems in both teens and adults. Treatment time depends on complexity and cooperation, while total cost varies by brace type, clinic, and the length of care.
When people ask, “What are braces?”, they’re usually thinking about straighter teeth. Orthodontic treatment can also improve chewing comfort, support gum health, and make daily cleaning easier.
Below you’ll find a clear explanation of how braces work, who they suit, how long they typically take, what to watch out for during treatment, and the main factors that shape the overall cost.
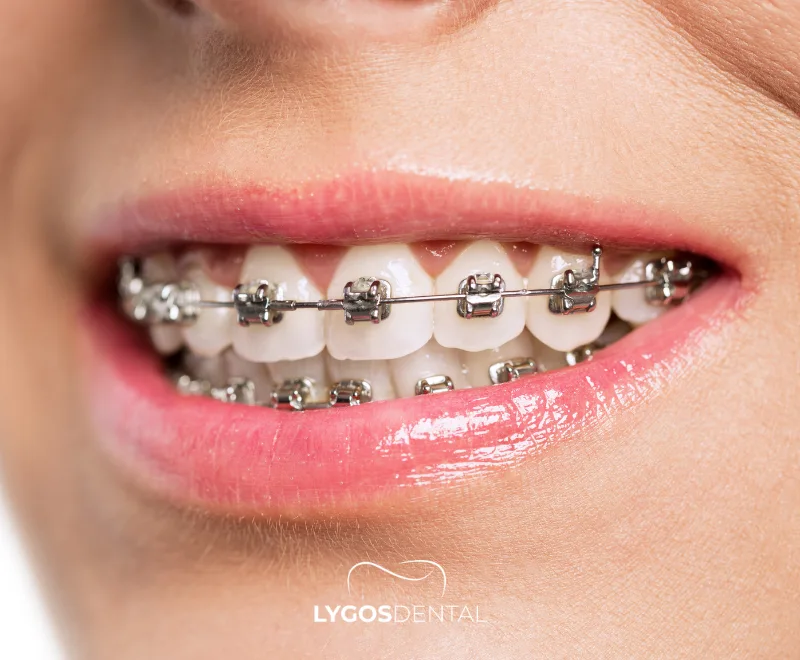
What Are Braces?
Braces are orthodontic tools used to correct crooked teeth, spacing, bite problems, and certain jaw-related alignment issues. They work through a simple mechanical system: small brackets are attached to the teeth and connected with a wire. As the wire is adjusted over time, it applies gentle, steady pressure that guides teeth into their planned positions.
What Are Braces Used For?
Braces are often chosen for cosmetic reasons, but they also support long-term oral health. They can help with:
- Straightening crowded or crooked teeth
- Closing gaps between teeth
- Correcting bite issues and some jaw misalignments
- Improving chewing efficiency and comfort
- Reducing the risk of plaque build-up in hard-to-clean areas
When teeth fit together properly, brushing and flossing tend to be more effective, and routine dental cleanings are usually easier.
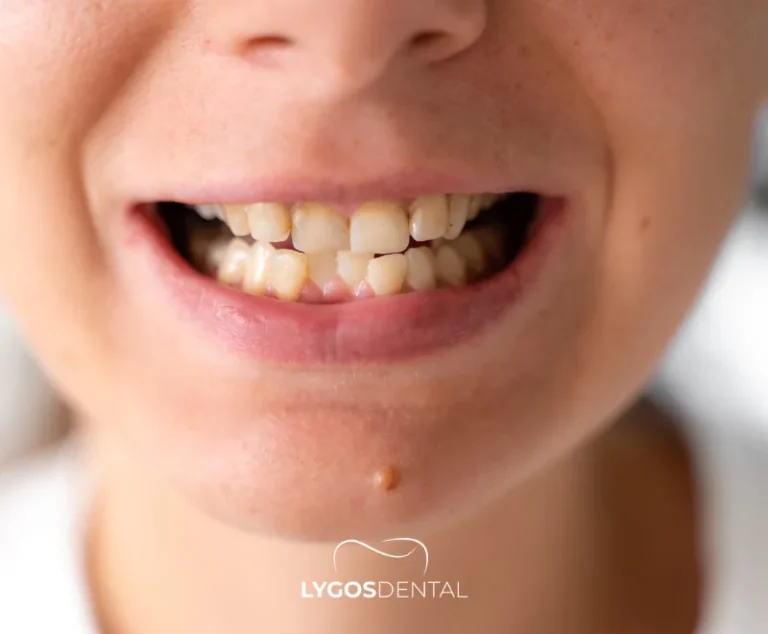
Who Are Braces Suitable For?
Braces are commonly used in childhood and the teen years, but adults can also benefit from orthodontic treatment. A dental exam and orthodontic assessment determine whether braces (or another option) is the right fit.
Braces are often recommended when:
- There is noticeable crowding
- Upper and lower teeth do not align well (malocclusion)
- There are visible gaps between teeth
- Front teeth protrude or tilt inward
- Jaw structure creates aesthetic or functional concerns
For people dealing with these issues, braces can be a practical way to improve comfort, function, and confidence.
How Long Does Braces Treatment Take?
Treatment length varies from person to person. It depends on how far the teeth need to move and how the bite responds to adjustments.
Common factors that affect timing include:
- The level of crowding or spacing
- How easily the teeth move
- The severity of bite problems
- Keeping appointments and following care instructions
Your orthodontist can give a more accurate timeline after an exam and a treatment plan.

What Should You Pay Attention To After Getting Braces?
Good daily habits make braces more comfortable and help treatment stay on track:
Oral Hygiene: Brush after meals when possible and clean around brackets carefully. Flossing aids or interdental brushes can help.
Food Choices: Avoid very hard or sticky foods that can loosen brackets or bend wires.
Regular Check-Ups: Adjustments work best when appointments are kept consistently.
Short-Term Discomfort: Mild pressure after fitting or tightening is common and usually settles within a few days.
Sports Protection: Use a mouthguard for contact sports to protect teeth and appliances.
Get Information Now!
Contact us to learn more about Cosmetic Dentistry, Dental Crown, Dental Implant, and General Dentistry, and to book an appointment.
How Much Do Braces Cost?
Braces pricing depends on the treatment method, case complexity, and follow-up care. Clinics may also price differently based on the orthodontist’s experience and the materials used.
Typical price ranges by type include:
- Metal Braces: 15,000 TL – 25,000 TL
- Ceramic Braces: 20,000 TL – 35,000 TL
- Lingual Braces: 30,000 TL – 50,000 TL
- Clear Aligners: 25,000 TL – 60,000 TL
For the most accurate estimate, ask for a personalized plan and a written quote after an in-person evaluation.
What Are Braces? Frequently Asked Questions (FAQ)
What are braces and when should they be applied?
Braces are orthodontic appliances used to align teeth and address bite or jaw alignment problems. Many patients start between ages 9 and 14, but adults can also be treated after an orthodontic assessment.
Do braces hurt?
You may feel mild pressure or soreness when braces are first fitted and after adjustments. This is usually temporary and eases within a few days.
How long does braces treatment last?
Treatment often lasts 1.5 to 3 years, depending on the complexity of the case and how closely care instructions are followed. Mild cases can be shorter.
Are braces covered by health insurance (SGK)?
Coverage rules can vary. In some cases, patients under 18 may receive partial coverage when treatment is medically necessary and approved through a state hospital evaluation.
Can you eat normally with braces?
Yes. Avoid hard, sticky, or very crunchy foods that can damage brackets or wires, and cut tougher foods into smaller pieces.
Dental Care For Kids
Why Dental Care Matters For Children
Baby teeth help children chew comfortably, speak clearly, and guide adult teeth into the right position. Cavities in primary teeth can cause pain, infections, and missed school days, and may also affect eating and sleep. Early routines make brushing and dental visits feel normal, so kids are less likely to resist care later.
When To Start Brushing And How Much Toothpaste To Use
Oral care starts at birth. Before teeth erupt, gently wipe your baby’s gums once a day with a clean, damp cloth.
When the first tooth appears (often around 6 months), brush twice daily with a soft, age-appropriate toothbrush. Use a tiny smear of fluoride toothpaste—about the size of a grain of rice—until age 3.
From ages 3 to 6, increase to a pea-sized amount of fluoride toothpaste. Supervise brushing and help your child spit out toothpaste; young kids don’t have the coordination to brush well on their own.
How To Build Good Dental Habits
Kids learn routines faster when brushing feels predictable and positive. Aim for two minutes, twice a day, and keep the tone calm even if it takes time to cooperate.
- Lead by example: brush and floss where your child can see you.
- Use a timer or a two-minute song to pace brushing.
- Create a simple reward system, like a sticker chart for consistent brushing.
- Make it a family routine by brushing together morning and night.
If your child fights brushing, start small and build up. Even 30 seconds twice a day is a useful first step while you work toward the full two minutes.
Choosing Toothbrushes And Toothpaste For Kids
The best products are the ones your child will actually use. Look for a comfortable handle, a small brush head, and soft bristles.
Toothbrushes
- Soft bristles to protect gums and enamel.
- Small head size to reach back teeth easily.
- Fun design or favorite character to boost interest.
- Optional: a child-sized electric toothbrush can help some kids brush more thoroughly.
Toothpaste
- Fluoride helps prevent cavities; choose an age-appropriate formula.
- A mild, kid-friendly flavor can reduce resistance.
- Check for reputable dental association acceptance or clear fluoride labeling.

When To See A Dentist For The First Time
Plan the first dental visit by your child’s first birthday or within six months of the first tooth erupting. This early appointment is usually quick and focuses on prevention, not procedures.
Your dentist will check growth and bite development, look for early signs of decay, and review feeding, brushing, and fluoride needs. Regular checkups are typically recommended every six months, unless your dentist suggests a different schedule based on risk.
Common Dental Problems And How To Prevent Them
Even with good routines, some children are more prone to dental issues due to diet, enamel strength, crowding, or dry mouth. Spotting problems early keeps treatment simpler and reduces discomfort.
Tooth Decay (Cavities)
Cavities form when bacteria feed on sugars and produce acids that weaken enamel.
Prevention Tips:
- Limit frequent sugary snacks and drinks (especially juice and sweetened milk).
- Brush twice daily with fluoride toothpaste and help with nighttime brushing.
- Keep regular dental checkups and ask about fluoride varnish or sealants when age-appropriate.
Early Tooth Loss
Losing baby teeth too early can affect spacing and how adult teeth come in.
Prevention Tips:
- Use a mouthguard for contact sports.
- Avoid falling asleep with a bottle or sippy cup of milk or juice.
- Treat cavities early to prevent infections that can lead to tooth loss.
Gum Irritation (Gingivitis)
Red, swollen, or bleeding gums can be a sign that plaque is building up along the gumline.
Prevention Tips:
- Brush gently at the gumline and replace worn toothbrushes.
- Start flossing once two teeth touch.
- Schedule professional cleanings if gums keep bleeding after brushing improves.
Thumb Sucking And Pacifier Use
Non-nutritive sucking is common in infants, but long-term habits can affect bite alignment.
Prevention Tips:
- Try to phase out pacifiers and thumb sucking by around age 3.
- Use positive reinforcement and offer other soothing routines (blanket, bedtime story).
- If the habit continues or teeth shift, ask a pediatric dentist for help.
Dental Care For Kids Frequently Asked Questions
When should my child start brushing?
Start oral care at birth by wiping gums daily. Begin brushing as soon as the first tooth erupts, usually around 6 months.
When should the first dentist appointment be?
Book the first visit by age 1, or within six months after the first tooth comes in. Early visits help prevent cavities and build comfort with the dental office.
Which toothpaste should children use?
Use fluoride toothpaste as soon as teeth erupt: a rice-grain smear until age 3, then a pea-sized amount from ages 3 to 6. Your dentist can recommend the right fluoride level if your child is at higher cavity risk.
My child hates brushing. What can I do?
Keep it routine and low-pressure. Use a timer or song, let your child choose a toothbrush, and brush together. If sensitivity or pain is the issue, schedule a dental checkup to rule out cavities or gum irritation.
Things To Consider Before And After Tooth Extraction
Things To Consider Before And After Tooth Extraction
Tooth extraction recovery depends on protecting the blood clot, keeping the area clean, and following your dentist’s instructions. Plan ahead by sharing your medical history and medications. After the procedure, bite on gauze, avoid rinsing and smoking, choose soft foods, and use cold compresses. Call your dentist if bleeding won’t stop or pain worsens after a few days.
Oral health plays a big role in daily comfort, nutrition, and confidence. When a tooth is too damaged or infected to save, your dentist may recommend an extraction to protect the rest of your mouth.
Most extractions heal without issues when you prepare properly and follow simple aftercare steps. The guidance below covers what patients typically need to know before treatment and during the first week of healing.
What Is Tooth Extraction?
A tooth extraction is the removal of a tooth by a dentist or oral surgeon. Depending on the tooth’s position and condition, extractions are usually done in one of two ways:
-
- Simple extraction: Used when the tooth is visible and can be removed with instruments after local anaesthetic.
- Surgical extraction: Used for teeth that are broken at the gumline, impacted (such as some wisdom teeth), or difficult to access. This may involve a small incision and stitches.
Common reasons include severe decay, advanced gum disease, infection, fractures, crowding for orthodontic treatment, or impacted teeth.
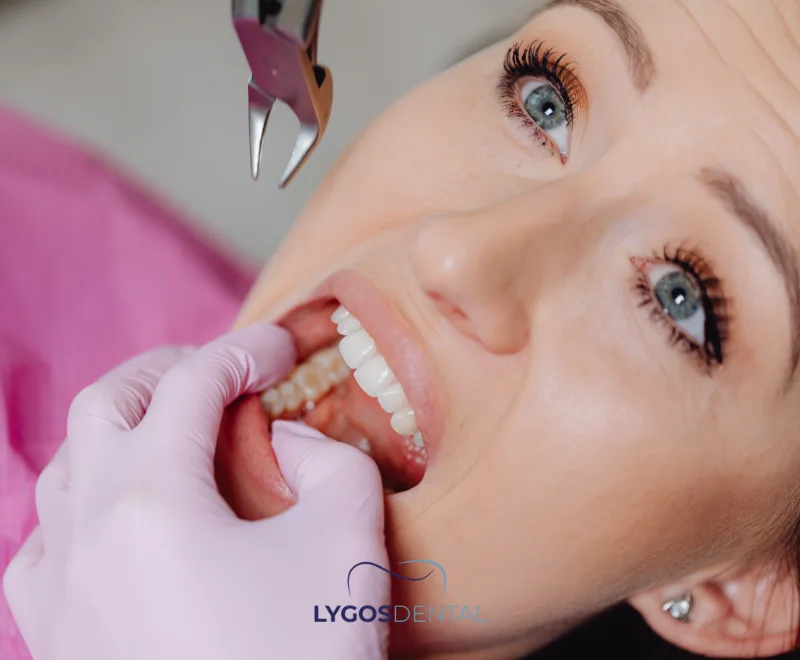
What To Consider Before Tooth Extraction
A short checklist before your appointment can reduce surprises and make recovery easier.
- Share your full medical history, including allergies and any heart, bleeding, immune, or bone conditions.
- List all medicines and supplements you take. This is especially important for blood thinners, aspirin, anti‑inflammatories, and bisphosphonates.
- Ask about sedation or general anaesthesia. If sedation is planned, you may be told not to eat or drink for a set period and to arrange a ride home.
- Avoid smoking and alcohol for at least 24 hours beforehand, unless your clinician gives different instructions.
- Plan a lighter schedule for the rest of the day so you can rest after the procedure.
What To Do In The First 24 Hours After Extraction
The first day is mainly about stopping bleeding, protecting the clot, and keeping swelling under control.
- Bite on gauze for 30–60 minutes (or as advised). If bleeding continues, replace with fresh gauze and keep steady pressure.
- Avoid rinsing, spitting, or vigorous mouth movements. These can dislodge the clot and slow healing.
- Rest and keep your head slightly elevated when lying down.
- Use a cold compress on the outside of your cheek for 10–15 minutes at a time during the first day.
- Take pain relief only as prescribed or recommended by your dentist.
- Avoid heavy exercise and lifting on day one, as it can restart bleeding.
What To Eat And Drink After Tooth Extraction
First Few Hours
- Wait until the numbness wears off before eating so you don’t bite your lip or cheek (often 2–3 hours, but it varies).
- Start with cool or room‑temperature liquids and soft foods.
Days 1–2
- Choose soft foods such as yogurt, soups cooled to lukewarm, eggs, mashed potatoes, smoothies eaten with a spoon, and well‑cooked pasta.
- Drink plenty of water, but avoid using a straw.
- Skip hot, spicy, crunchy, and very acidic foods if they irritate the area.
Days 3–7
- Gradually return to normal foods as comfort allows, chewing on the opposite side.
- Avoid nuts, seeds, chips, and sticky foods until the socket is no longer tender.
How To Reduce Pain And Swelling
Mild pain and swelling are common, especially during the first 48–72 hours. These steps usually help:
- Cold compresses on day one; warm compresses may feel better after the first 24 hours for some people.
- Follow the dosing instructions for any pain medicine. Do not mix medications unless your dentist or pharmacist says it’s safe.
- After the first 24 hours, gently rinse with warm salt water several times a day, especially after meals (unless your dentist advises otherwise).
- Brush and floss as normal, but keep the toothbrush away from the socket and stitches.

What Not To Do After Tooth Extraction
- Do not smoke or use tobacco. Aim for at least 72 hours, and longer if possible.
- Do not drink through a straw or create suction in the mouth.
- Do not touch the socket with fingers, tongue, or objects.
- Avoid alcohol and alcohol‑based mouthwash during the early healing period.
- Avoid vigorous rinsing, heavy physical activity, and hot foods or drinks in the first 24 hours.
When To Call Your Dentist
Contact your dentist or oral surgeon promptly if you notice any of the following:
- Bleeding that does not slow down after applying pressure with gauze for a few hours.
- Severe pain that gets worse after day 2–3 (this can be a sign of dry socket).
- Increasing swelling, fever, foul taste, or pus‑like discharge.
- Rash, difficulty breathing, or other signs of an allergic reaction to medication.
- Numbness that doesn’t improve after the anaesthetic should have worn off.
Before And After Tooth Extraction: Frequently Asked Questions
Is tooth extraction painful?
During the procedure, local anaesthetic prevents pain. After the numbness wears off, soreness is normal for a few days and is usually managed with recommended pain relief.
When can I eat after a tooth extraction?
Eat only after the numbness has worn off. Start with soft foods and avoid hot foods on day one. Your dentist may give you specific timing based on the extraction and any stitches.
Can I smoke after a tooth extraction?
It’s best to avoid smoking because it increases the risk of dry socket and delays healing. Try to stop for at least 72 hours, and longer if you can.
How should I clean my mouth after extraction?
Avoid rinsing for the first 24 hours. After that, rinse gently with warm salt water and brush carefully around the area without disturbing the socket or stitches.
How long does healing take?
Initial healing often takes about 1–2 weeks, but the exact timeline depends on the tooth, the extraction type, and your overall health. Follow‑up appointments help confirm that healing is on track.
What Is Good For Gum Pain?
What Is Good For Gum Pain?
Gum pain is often caused by irritation, trapped food, or early gum disease. For quick relief, rinse with warm salt water, use a cold compress for swelling, and keep brushing gently with a soft toothbrush. If your gums are swollen, bleeding, or the pain lasts more than a few days, a dentist should check the cause.
Gums are sensitive tissue, so even small problems can feel bigger than they look. The goal is to calm inflammation, keep the area clean, and spot the warning signs of infection. The steps below are safe for most people, but they do not replace a dental exam when symptoms persist.
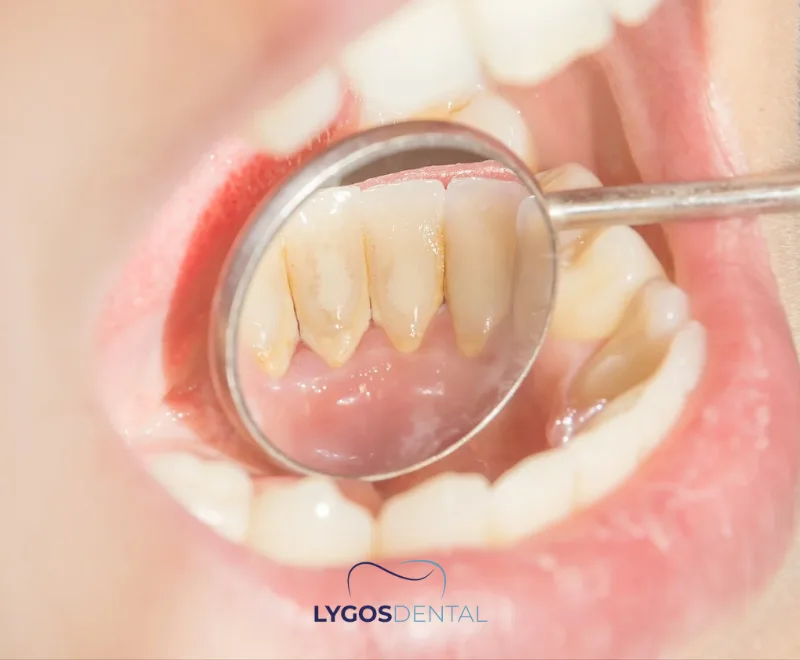
Common Causes Of Gum Pain
Gum pain has a short list of usual suspects. Pinpointing the cause matters because home care can soothe irritation, but it cannot treat a deep infection or advanced gum disease.
- Plaque buildup and gingivitis (early gum disease), which can cause red, puffy, bleeding gums.
- Tartar (calculus) along the gumline, which irritates the tissue and is hard to remove at home.
- Food stuck between teeth or under the gum edge, especially around crowns, bridges, or tight contacts.
- Abrasive brushing, a hard toothbrush, or brushing too aggressively.
- Mouth ulcers (canker sores) or minor injuries from sharp foods.
- Teething or wisdom tooth eruption (pericoronitis) causing sore tissue around a partly erupted tooth.
- Hormonal changes (pregnancy, puberty, menopause) that can make gums more reactive.
- Dry mouth, smoking, or poorly fitting dental appliances that rub the gums.
Symptoms That Often Come With Gum Pain
Gum pain rarely shows up alone. These symptoms help you judge whether you’re dealing with mild irritation or something that needs a dental visit.
- Redness, swelling, or tenderness along the gumline
- Bleeding when brushing or flossing
- Bad breath or a persistent bad taste
- Receding gums or teeth that look “longer” than before
- Soreness when chewing, or sensitivity to hot/cold
- A pimple-like bump on the gum (possible drainage from an abscess)
- Loose or shifting teeth (a late warning sign)

Fast Home Remedies That Usually Help
If the pain is mild and you do not have fever or facial swelling, home care can reduce irritation while you arrange a dental checkup if needed.
1) Warm Salt Water Rinse
Mix about ½ teaspoon of salt into a glass (around 8 oz / 240 ml) of warm water. Swish gently for 20–30 seconds, then spit it out. Do this 2–4 times a day, especially after meals.
2) Gentle Cleaning Around The Sore Area
Brush with a soft toothbrush and light pressure. Floss carefully to remove trapped food, but stop if you feel sharp pain. If flossing is difficult, an interdental brush or water flosser can be gentler.
3) Cold Compress For Swelling
Apply a cold pack to the cheek near the sore area for 10–15 minutes, then take a break. Cold helps reduce swelling and can dull pain, especially after minor trauma.
4) Avoid Irritants While It Heals
- Very hot, very cold, spicy, or acidic foods (citrus, vinegar-based dressings)
- Crunchy foods that can cut gums (chips, crusty bread)
- Smoking or vaping, which slows healing and can worsen inflammation
- Alcohol-based mouthwashes if they sting
Over-the-counter Pain Relief Options
Pain relievers can take the edge off, but they do not fix the underlying cause. Use the lowest effective dose and follow the label directions.
Common OTC Choices
- Ibuprofen can help when inflammation is the main issue. Avoid it if you have a history of stomach ulcers/bleeding, kidney disease, certain heart conditions, or if a clinician has told you not to take NSAIDs.
- Acetaminophen (paracetamol) can help with pain if NSAIDs are not suitable. Stay within the maximum daily dose on the label, and be cautious if you have liver disease or drink alcohol heavily.
- Topical oral gels can numb the area for short periods. Use sparingly and follow age restrictions on the product.
What To Avoid When Treating Gum Pain
A few popular “hacks” can make gums worse. Skip these.
- Placing aspirin directly on the gums or tooth. It can burn soft tissue.
- Undiluted hydrogen peroxide or essential oils inside the mouth. These can irritate or injure tissue.
- Over-brushing to “scrub away” the problem. This often increases soreness and recession.
- Ignoring a draining bump, swelling, or fever. These can be signs of infection.
When To See A Dentist
Book a dental visit if gum pain keeps coming back or if you notice bleeding or swelling. Get urgent care if you suspect infection.
Make A Routine Appointment If You Have:
- Pain that lasts more than 3–5 days
- Gums that bleed often when brushing or eating
- Swollen, tender gums or persistent bad breath
- Receding gums or sensitivity that is getting worse
Seek Urgent Dental Or Medical Care If You Have:
- Fever, facial swelling, or swelling that spreads
- Trouble swallowing, breathing, or opening your mouth
- Severe pain that is not improving with OTC medication
- Pus, a bad taste, or a gum boil near a tooth
- Loose teeth or a sudden change in your bite
How To Prevent Gum Pain From Coming Back
Most gum pain is preventable. A steady routine works better than occasional “deep cleans.”
- Brush twice daily with a soft brush and fluoride toothpaste, focusing gently along the gumline.
- Clean between teeth daily with floss, interdental brushes, or a water flosser.
- Schedule regular dental checkups and professional cleanings, especially if you build tartar quickly.
- If you smoke, consider quitting. It’s one of the biggest risk factors for gum disease and slow healing.
- Stay hydrated and manage dry mouth (ask your dentist about saliva substitutes if needed).
Frequently Asked Questions
How Long Does Gum Pain Last?
Minor irritation can settle within 24–72 hours once the area is cleaned and you avoid triggers. If pain lasts beyond a few days, keeps returning, or comes with bleeding and swelling, a dental exam is the safest next step.
Does Salt Water Really Help Gum Pain?
Yes. A warm salt water rinse can soothe inflamed tissue and help keep the area clean. It works best as a short-term comfort measure alongside gentle brushing and flossing.
Can Gum Pain Be Serious?
It can be. Persistent pain may come from gum disease, an abscess, or a problem with a tooth or filling. Fever, facial swelling, pus, or loose teeth are red flags that need prompt care.
What Foods Should I Avoid While My Gums Hurt?
Avoid spicy, acidic, very hot, and very cold foods, plus crunchy snacks that can scratch gums. Soft, lukewarm foods are usually easier until the soreness calms down.
Can Stress Cause Gum Pain?
Stress does not directly inflame gums, but it can affect sleep, immune response, and habits like clenching or skipping oral care. If gum symptoms show up during a stressful period, focus on a simple routine and book a checkup if bleeding or swelling continues.
Is It Safe To Use OTC Painkillers For Gum Pain?
For many people, yes, when used exactly as directed on the label. If you’re pregnant, on blood thinners, have stomach, kidney, or liver disease, or you’re treating a child, check with a clinician or pharmacist first.
Myths About Teething
Myths About Teething
Teething is a normal stage that can bring drooling, tender gums, and a strong urge to chew. Many widely shared “facts” are myths—like blaming every fever or diarrhea on new teeth. Knowing what’s typical, what isn’t, and how to soothe sore gums safely helps you care for your baby with confidence.
Teething is part of normal development, but it’s also a stage surrounded by half-truths. Some myths can lead parents to miss signs of illness, while others encourage remedies that aren’t safe for babies.
Below are the most common teething myths, what the evidence and pediatric guidance supports, and practical ways to keep your baby comfortable.
Signs Of Teething
Babies can show different teething signs, and symptoms may come and go as each tooth moves through the gums.
Common signs include:
- Irritability or fussiness
- More drooling than usual (sometimes with a mild rash on the chin or cheeks)
- Swollen or tender gums where the tooth is coming through
- Chewing or gnawing on fingers, toys, or other safe objects
- Changes in sleep or appetite for a short period
Myth check: teething can make babies uncomfortable, but it shouldn’t be used to explain away significant symptoms such as a high fever, persistent vomiting, or severe diarrhea.

Table of Contents
When Does The First Tooth Erupt?
Many babies get their first tooth around 6 months, but a normal range is broad. Some start closer to 4 months, while others don’t see a first tooth until later in the first year.
The first tooth is often one of the lower front teeth. After that, teeth typically come in a pattern, but the exact order and timing can vary from baby to baby.
Should Baby Teeth Be Cleaned?
Yes. Baby teeth need care from the start, even though they’re temporary.
Once a tooth appears, gently clean it twice a day. A soft, age-appropriate brush and a smear of fluoride toothpaste (about the size of a grain of rice) is commonly recommended—your pediatrician or dentist can confirm what’s right for your baby.
Early habits help prevent cavities, protect gum health, and support healthy spacing for adult teeth later on.
Does Teething Hurt?
Teething discomfort is real, but it isn’t the same for every baby. Some barely notice new teeth, while others have sore, swollen gums for a few days at a time.
A myth worth dropping: teething doesn’t automatically mean constant crying. If your baby seems unusually distressed or unwell, it’s smart to look for other causes.

Safe, Natural Remedies For Teething
Simple, low-risk comfort measures usually work best. Try one option at a time so you can see what helps.
- Offer a chilled (not frozen) teething ring. Cold can reduce gum swelling and soothe soreness.
- Let your baby chew on a clean, cool washcloth. Supervise closely and remove it if it starts to fray.
- Gently rub your baby’s gums with a clean finger for a minute or two.
- Keep drool under control with soft wipes and a protective barrier cream on irritated skin (avoid fragranced products).
Avoid risky “quick fixes” such as teething jewelry (choking/strangulation risk) or numbing gels and liquids unless a clinician specifically recommends them for your child.
Common Mouth Problems During Teething
Most teething-related mouth issues are temporary. These tips can help:
- Gum tenderness or minor bleeding: Use gentle pressure with a clean finger or gauze. If bleeding is heavy or keeps returning, call your child’s clinician.
- Drool rash: Pat the skin dry and apply a thin layer of barrier cream. Keep bibs clean and dry.
- Reduced appetite: Offer softer foods and smaller, more frequent feeds. Watch for dehydration signs such as fewer wet diapers.
- Mouth sores: Occasional irritation can happen from chewing. If sores are widespread, persistent, or your baby refuses feeds, seek medical advice.
When To Call A Doctor
Teething shouldn’t mask illness. Contact your pediatrician (or urgent care) if your baby has:
- A temperature of 38°C (100.4°F) or higher
- Diarrhea, vomiting, or signs of dehydration
- Trouble breathing, a widespread rash, or extreme sleepiness
- Crying that is intense, persistent, and not eased by comfort measures
- Any symptom that worries you or feels out of character
Myths About Teething: Frequently Asked Questions
Is there a link between early teething and IQ?
No, early teething isn’t linked to higher or lower IQ in evidence.
What are the worst months of teething?
Molars often cause worst symptoms, typically around 12–19 months and 23–33 months.
What vitamins help with teething?
No vitamins reliably help teething; avoid supplements unless prescribed for deficiency.
Does breastfeeding help with teething?
Breastfeeding can soothe teething discomfort, but it doesn’t change tooth-eruption timing.
What time of day is teething the worst?
Nighttime is often worst, when distractions drop and discomfort feels more noticeable.
Upper Dental Implants Cost
Upper Dental Implants Cost
Upper dental implant pricing varies widely based on the implant brand, the dentist’s experience, clinic location, and whether you need extras like a sinus lift or bone graft. In many markets, a single upper implant can range from a few hundred to several thousand dollars. Your final quote depends on your exam, scans, and the type of restoration placed on top.
Missing upper teeth can affect your smile, speech, and bite strength. Dental implants are a long-term option designed to look and function like natural teeth.
Costs differ from patient to patient because treatment plans are rarely identical. The sections below break down what an upper implant is, what drives pricing, and the common extra fees people overlook.
What Is An Upper Dental Implant?
An upper dental implant is a small post (most commonly titanium or zirconia) placed into the upper jaw to replace a missing tooth root. After the implant bonds with the bone, a connector piece (abutment) and a crown are attached to restore the visible tooth.
Because the upper jaw can be softer and sits close to the sinuses, some patients need additional procedures to create enough stable bone. This is one of the biggest reasons upper implant quotes can vary.
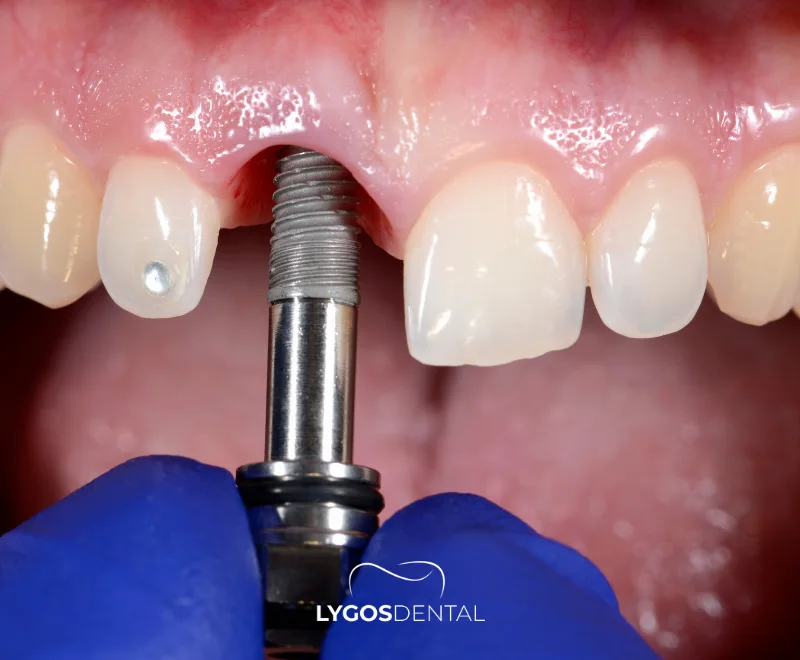
Table of Contents
Factors That Affect Upper Dental Implant Cost
Pricing is usually influenced by a mix of clinical needs and product choices. The most common cost drivers include:
Clinical And Product Factors
- Material quality: Titanium and zirconia implants can sit in different price brackets, and premium surface treatments may add cost.
- Implant brand: Internationally known brands often cost more than regional alternatives.
- Dentist’s expertise: Fees can be higher for experienced implant surgeons, especially for complex cases.
- Clinic location: Prices often increase in major cities and higher-cost healthcare markets.
- Additional treatment needs: Bone grafting, sinus lift surgery, or extractions can raise the total treatment cost.
Ask for a written estimate that separates the surgical implant, abutment, crown, imaging, and any add-on procedures. Itemized quotes make it easier to compare clinics fairly.
Upper Dental Implant Cost By Country
The ranges below are broad averages and can shift based on the clinic, included services, and case complexity. When comparing countries, confirm whether the quote includes the crown and abutment, not just the implant fixture.
Typical Price Ranges
- United States: often around $3,000–$6,000 per implant, depending on the provider and what’s included.
- United Kingdom: commonly about £2,500–£5,000 per implant.
- Turkey: frequently around $600–$1,500 per implant; prices can vary by city, brand choice, and what’s bundled into the package.
- Europe (e.g., Germany, France, Spain): often about €2,000–€4,000 per implant.
If you’re considering treatment abroad, budget for travel, extra days for follow-ups, and the possibility of returning for review visits.
Does Insurance Cover Upper Dental Implants?
Coverage depends on your policy and the reason for tooth replacement. Many standard dental plans limit implant coverage or exclude it, while some private plans may reimburse part of the procedure.
Even when implants are not fully covered, plans may help with related items such as extractions, imaging, or the crown. Contact your insurer and ask what is covered, what documentation is required, and whether pre-authorization is needed.

Hidden Costs To Budget For
Implant quotes can look very different depending on what is included. Common add-ons to ask about are:
- X-rays and CT scans: Diagnostic imaging and planning fees.
- Temporary tooth replacement: A temporary prosthesis while healing.
- Surgical add-ons: Bone grafting or sinus lift procedures when needed.
- Medication and follow-up care: Prescriptions, post-op checkups, and hygiene visits.
Speak With A Dentist
For an accurate estimate, you’ll need a clinical exam and imaging. If you’d like to discuss cosmetic dentistry, crowns, implants, or general dentistry, you can contact us to book an appointment or request pricing information.
Things To Know Before Getting An Upper Dental Implant
A smoother experience usually comes down to planning and realistic expectations. Keep these points in mind:
- Choose a qualified provider: Experience matters, especially for upper jaw cases where sinus-related procedures may be required.
- Understand the timeline: Healing and integration can take months, and extra procedures can extend the schedule.
- Commit to long-term care: Daily brushing and flossing, plus routine checkups, help protect both the implant and surrounding gums.
- Plan your total budget: Factor in imaging, temporary restorations, and possible surgical add-ons so there are fewer surprises.
Upper dental implant costs vary because treatment is tailored to your anatomy and goals. A detailed consultation and an itemized plan are the best way to match expectations with budget.
Upper Dental Implants Cost FAQs
How much does an upper tooth implant cost?
About $3,000–$6,000 per upper tooth implant in the U.S.
How many implants are needed for full upper?
4–6 implants are used for most full upper fixed arches.
How much is a upper dental implant?
About $3,000–$6,000 per upper dental implant in the U.S.
Can dental implants be done on upper teeth?
Yes, dental implants can be placed on upper teeth.
Are upper dental implants safe?
Yes, upper dental implants are safe when properly planned and placed.
How To Fix Bad Breath Permanently
How To Fix Bad Breath Permanently
Bad breath usually comes from bacteria in the mouth, a coated tongue, dry mouth, diet, or gum disease. For lasting results, brush twice daily with fluoride toothpaste, clean your tongue, clean between teeth every day, drink water regularly, and get routine dental checkups. If odor continues after improving habits, ask a dentist or doctor to look for an underlying cause.

Table of Contents
Why Bad Breath Happens
Most persistent bad breath is linked to oral bacteria. These bacteria break down food particles and proteins, releasing odor-causing compounds. The good news is that the cause is often identifiable—and fixable—once you know where to look.
- Poor oral hygiene: Plaque and trapped food feed bacteria, especially between teeth and along the gumline.
- A coated tongue: The tongue’s surface can hold bacteria and debris, creating a strong odor even when teeth look clean.
- Dry mouth (xerostomia): Saliva helps wash away bacteria. Dehydration, mouth breathing, and some medicines can reduce saliva.
- Diet: Garlic, onions, sugary snacks, and high-protein or very low-carb eating patterns can affect breath.
- Smoking and tobacco: Tobacco dries the mouth, irritates gums, and leaves a lingering smell.
- Gum disease or tooth decay: Infection and deep gum pockets can produce ongoing odor.
- Medical causes: Sinus issues, reflux, and uncontrolled diabetes are examples that may need medical care.
How To Tell If You Have Bad Breath
It’s hard to judge your own breath because you quickly get used to smells. These quick checks can help you confirm whether halitosis is an issue.
- Ask someone you trust: A straightforward check is often the most accurate.
- Wrist test: Lick the back of your wrist, let it dry, then smell it.
- Look at your tongue: A thick white or yellow coating can be a clue that bacteria are building up.
- Smell your floss: After cleaning between your teeth, sniff the floss to see if odor is coming from trapped debris.
- Notice dryness: If breath worsens after long periods without water (or after waking), dry mouth may be involved.

Daily Routine That Keeps Breath Fresh
Consistency matters more than special products. Build a routine that reduces bacteria, boosts saliva, and addresses the spots a toothbrush can miss.
Morning
- Brush for two minutes: Use fluoride toothpaste and angle the brush toward the gumline.
- Clean your tongue: Use a tongue scraper or a soft brush to remove coating from back to front.
- Rinse if needed: An alcohol-free mouthwash can help short-term, but it doesn’t replace brushing and flossing.
After Meals
- Drink water: A few sips help wash away food and keep saliva flowing.
- Chew sugar-free gum: It can stimulate saliva when brushing isn’t possible.
- Be careful with “quick fixes”: Mints mask odor, but they don’t remove the source.
Night
- Clean between teeth daily: Floss or use interdental brushes to remove plaque where odor often starts.
- Brush again before bed: Nighttime dryness makes bacteria more active, so bedtime cleaning is key.
- Keep dental appliances clean: If you wear retainers, aligners, or dentures, clean them as directed and let them dry overnight.
Two extra habits help long-term: replace your toothbrush every 3–4 months (or sooner if bristles flare), and keep up with routine dental cleanings.

Foods That Help With Fresh Breath
Food can’t replace oral hygiene, but certain choices support saliva and reduce odor-causing bacteria.
- Crunchy fruits and vegetables: Apples, carrots, and celery increase saliva and help remove debris.
- Plain yogurt: Some evidence suggests it can lower odor compounds for some people.
- Green tea: Contains compounds that may reduce odor-causing bacteria.
- Fresh herbs: Parsley and mint can freshen breath, especially after meals.
- Water: The simplest way to reduce dry mouth-related odor.
Foods And Habits That Make Breath Worse
If you’re working on long-term improvement, watch for common triggers and patterns—especially on days when breath seems worse than usual.
- Onions and garlic: Their sulfur compounds can linger for hours.
- Sugary snacks and drinks: Sugar feeds bacteria and can increase plaque buildup.
- Coffee and alcohol: Both can dry the mouth, which makes odor worse.
- Smoking or vaping: Leaves odor behind and increases gum disease risk.
- Skipping meals: A dry mouth and “empty stomach” breath can build up when you don’t eat or drink regularly.
When To See A Dentist Or Doctor
If you’ve improved your routine for a couple of weeks and breath still doesn’t improve, get checked. A dentist can rule out gum disease, cavities, dry mouth, and appliance-related issues. If your mouth is healthy, you may be referred to a medical provider for other causes.
- Bleeding gums, gum swelling, or loose teeth: These can point to gum disease and need dental treatment.
- Ongoing dry mouth: A dentist or doctor can review medicines and suggest saliva-supporting options.
- Sinus symptoms or chronic post-nasal drip: Respiratory infections and sinus problems can affect breath.
- Frequent heartburn: Reflux can contribute to persistent odor.
- A fruity, sweet breath smell with other symptoms: This can be linked to poorly controlled diabetes and needs urgent medical advice.
Book An Appointment
If you suspect gum disease, tooth decay, or dry mouth, a dental exam is the fastest way to find the cause and build a plan that works. Contact your dental clinic to schedule a checkup or cleaning, especially if your breath problem has lasted more than a few weeks.
How To Fix Bad Breath Permanently: Frequently Asked Questions
Is it possible to completely get rid of bad breath?
Yes, if underlying cause is diagnosed and treated and oral hygiene maintained.
How do I clean my gut for bad breath?
You can’t “clean” your gut; treat reflux, constipation, and diet issues medically.
Why does my breath stink even after brushing?
Because tongue coating, gum disease, dry mouth, decay, sinus issues, or reflux persist.
What drink kills bad breath?
Water reduces odors by washing debris; unsweetened green tea may temporarily neutralize odors.
What drink kills mouth bacteria?
No drink safely kills mouth bacteria; antiseptic mouthwash reduces them, but don’t swallow.
How to detox your body from bad breath?
Detox isn’t needed; eliminate bad breath by treating causes like dental disease or reflux.
Why does my breath stink so badly?
Severe halitosis often signals gum disease, infection, dry mouth, or medical illness—seek evaluation.
Dental Cleaning Cost Without Insurance
Dental Cleaning Cost Without Insurance
Without insurance, a routine dental cleaning often costs about $75–$200. A deep cleaning (scaling and root planing) may cost $150–$350 per quadrant, or $600–$1,400 for the full mouth. Pricing changes by location and whether your visit includes an exam, X-rays, or fluoride. Dental schools, community clinics, and discount plans can help lower the bill.
What Is Dental Cleaning?
A professional dental cleaning is a preventive visit where a dental hygienist or dentist removes plaque, tartar (calculus), and surface stains. Cleanings help lower your risk of cavities, gum disease, and bad breath, and they give your provider a chance to spot problems early.
A typical cleaning appointment may include:
-
- Scaling and polishing to remove plaque and tartar.
- A brief exam to check for cavities, gum inflammation, and other concerns.
- Fluoride treatment (optional) to strengthen enamel.

Table of Contents
How Much Does A Teeth Cleaning Cost Without Insurance?
Out-of-pocket pricing depends on the type of cleaning and what’s bundled into the visit. Many offices quote one price for a basic cleaning and a different price if you need deeper periodontal care.
Typical price ranges without insurance:
- Standard cleaning (prophylaxis): $75–$200 per visit
- Deep cleaning (scaling and root planing): $150–$350 per quadrant (often $600–$1,400 for the full mouth)
- Periodontal maintenance (follow-up cleanings for gum disease): $120–$250 per visit
Keep in mind that a first-time visit can cost more if it includes an exam, X-rays, or other diagnostics.
Factors Affecting The Cost Of Dental Cleaning
- Where you live: Dental fees are usually higher in large cities and higher-cost regions than in smaller towns.
- Type of cleaning you need: A routine cleaning is typically the least expensive. If you have gum disease or heavy tartar buildup, a deeper cleaning may be recommended.
- What’s included in the appointment: Some prices include an exam and polishing, while others add separate charges for X-rays, fluoride, or periodontal measurements.
- Provider experience and clinic overhead: Costs can rise at practices with more specialized staff, newer technology, or higher operating expenses.
- Office discounts and payment options: Cash-pay discounts, new-patient specials, membership plans, or payment plans can reduce the total you pay.

Affordable Alternatives For Dental Cleaning Without Insurance
If you’re uninsured, you still have several realistic ways to bring the cost down:
- Dental schools: Supervised students often provide cleanings at reduced rates. Appointments can take longer, but costs are usually lower.
- Community health clinics: Many clinics offer sliding-scale fees based on income, and some run limited free-care days.
- Dental discount plans: You pay an annual fee for access to discounted rates at participating dentists. This isn’t insurance, but it can help with predictable pricing.
- In-office membership plans: Some practices offer a monthly or annual plan that includes cleanings and exams, plus discounts on other services.
- Ask about cash-pay pricing: If you can pay at the visit, many offices can offer a lower rate or bundle services.
- Nonprofits and local programs: Charities, public health programs, and mobile dental events sometimes provide low-cost cleanings in the community.
How Often Should You Get A Dental Cleaning?
Cleaning frequency depends on your risk for cavities and gum disease. Many people do well with a cleaning about every six months, while others benefit from more frequent visits.
Common schedules include:
- About every 6 months for people with generally healthy gums and good home care
- Every 3–4 months if you have gum disease, frequent tartar buildup, or other risk factors (such as smoking or certain medical conditions)
- A personalized interval recommended by your dentist based on your exam
Staying on schedule can prevent bigger problems and help avoid higher costs later.
Get Information Now
Want a clearer estimate for your situation? Contact us to ask about appointment availability and pricing for cosmetic dentistry, dental crowns, dental implants, and general dentistry services.
The Importance Of Regular Dental Cleanings For Oral Health
Routine cleanings support your oral health in ways that daily brushing can’t fully replace:
- Helps prevent cavities and gum disease: Professional scaling removes hardened tartar that can’t be brushed away at home.
- Catches issues early: Regular visits can flag early gum inflammation, decay, worn fillings, or other concerns before they become expensive problems.
- Improves breath and appearance: Polishing removes surface stains and can leave teeth feeling smoother and cleaner.
- Supports overall health: Oral infections and inflammation can affect the rest of the body, so keeping your mouth healthy matters.
- Saves money over time: Preventive care is usually far cheaper than treating advanced decay or periodontal disease.
Dental Cleaning Cost Without Insurance Frequently Asked Questions
How much is it to clean teeth at the dentist?
Typically $75–$200 per cleaning; costs vary by location and insurance.
Is dental teeth cleaning worth it?
Yes, it reduces gum disease, cavities, bad breath, and tooth loss risk.
How painful is dental deep cleaning?
Usually mild to moderate discomfort; local anesthetic minimizes pain during scaling and planing.
What happens if you skip dental cleanings?
Skipping cleanings increases tartar buildup, gum disease, cavities, and costly future treatment.
Why are dentists not cleaning teeth?
Dentists often delegate routine cleanings to hygienists while they diagnose and treat problems.
Cosmetic Dentistry Treatments That Can Improve Your Smile
Can Cosmetic Dentistry Improve My Smile?
Yes—cosmetic dentistry can improve your smile by changing tooth color, shape, spacing, and alignment. Treatments like professional whitening, veneers, bonding, crowns, implants, orthodontics, and gum contouring can create a brighter, more balanced look. The best option depends on your oral health, bite, and goals, so an exam is the starting point.
A bright, healthy-looking smile can make day-to-day conversations feel easier. Still, many people live with stains, chips, gaps, uneven edges, or teeth that don’t sit quite where they should.
Cosmetic dentistry focuses on improving how your teeth and gums look while keeping function in mind. With the right plan, small changes can look natural—and bigger changes can be done in stages.
What Is Cosmetic Dentistry?
Cosmetic dentistry covers dental treatments that enhance the appearance of your teeth, gums, and overall smile. It often overlaps with restorative dentistry because many aesthetic improvements also support comfort and chewing.
Depending on your needs, a cosmetic plan may involve whitening, veneers, bonding, crowns, implants, orthodontics, and gum reshaping.
Table of Contents
Cosmetic Dentistry And Smile Design
Smile design is a planning approach that aims for a balanced result that fits your facial features. During a consultation, a dentist reviews tooth shape, alignment, gum display, and how your smile frames your face.
Key elements dentists typically consider:
- Tooth proportions: Teeth can be reshaped or lengthened to better match facial features.
- Tooth alignment: Crooked or rotated teeth may be improved with orthodontics, bonding, or veneers, depending on the case.
- Smile line: Many plans aim for a gentle curve that follows the lower lip.
- Gum aesthetics: Gum reshaping can help if the gum line looks uneven or too prominent.
When these details work together, the result usually looks more natural than fixing one issue in isolation.
Cosmetic Dentistry Treatment Options
Cosmetic dentistry offers different options for different concerns. A dentist will usually recommend the least invasive treatment that can reliably meet your goal.
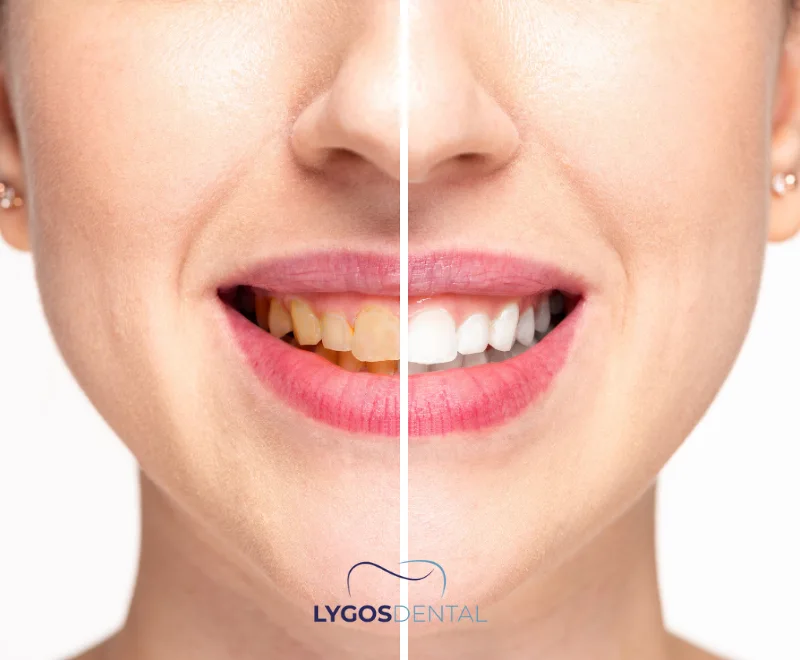
Teeth Whitening
Professional whitening can lift stains caused by coffee, tea, tobacco, and natural aging. In-office whitening is faster, while take-home trays may be more gradual.
Veneers
Veneers are thin shells (often porcelain) that cover the front of the teeth. They can improve shape, color, small gaps, and minor misalignment.
Dental Bonding
Bonding uses a tooth-colored resin to repair chips, close small gaps, and smooth uneven edges. It’s often a cost-effective option for small changes.
Crowns And Bridges
Crowns cover a damaged or heavily filled tooth to restore strength and appearance. Bridges replace missing teeth by anchoring an artificial tooth to neighboring teeth or implants.
Dental Implants
Implants replace missing teeth with a titanium post and a crown. They look and function like natural teeth and help preserve jawbone support.
Orthodontics
Braces or clear aligners can straighten teeth, close gaps, and improve the bite. Orthodontics can also make later cosmetic work (like veneers) more conservative.
Gum Contouring
Gum contouring reshapes the gum line for a more even frame around the teeth. It’s often used for an uneven gum line or a “gummy” smile.
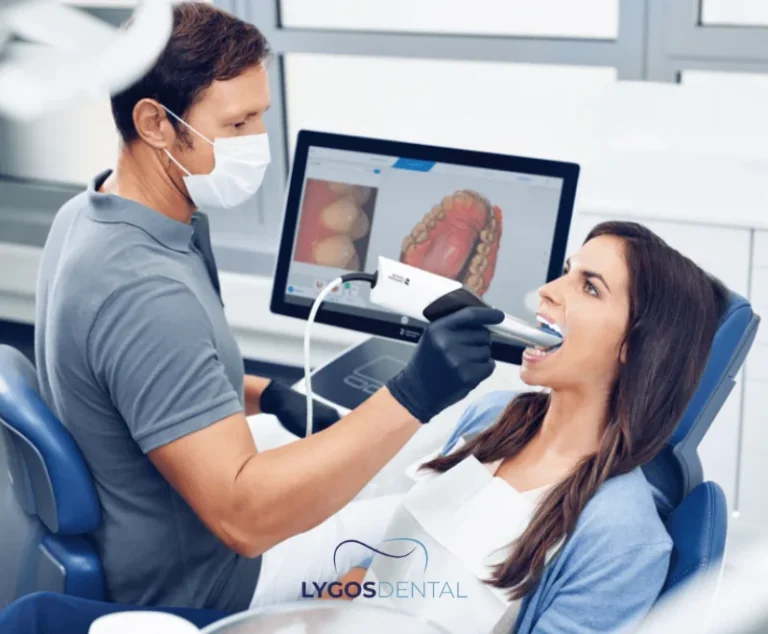
The Cosmetic Dentistry Process
Most cosmetic improvements start with a consultation. Your dentist will check your teeth and gums, listen to what you want to change, and explain realistic outcomes.
A typical process looks like this:
- Consultation and evaluation: Exam, photos, and sometimes X-rays or 3D imaging to understand tooth and jaw structure.
- Treatment plan: A personalized plan that may combine treatments (for example, orthodontics first, then whitening or veneers).
- Treatment: Some options are completed in one visit (whitening, bonding), while others take multiple visits (veneers, implants, orthodontics).
- Aftercare and maintenance: Guidance on cleaning, stain prevention, and follow-ups to protect your results.
If you have active decay, gum disease, or bite problems, those are usually addressed first so the final result lasts.
Cosmetic Dentistry Costs
Costs vary by country, materials, case complexity, and how many teeth are treated. Insurance may cover parts of treatment when there’s a functional or restorative need, but purely cosmetic work is often self-pay.
Approximate self-pay ranges (often quoted in the U.S.) include:
- Teeth whitening: $300–$1,500
- Veneers: $500–$2,500 per tooth
- Bonding: $100–$400 per tooth
- Crowns: $800–$3,000 per crown
- Dental implants: $1,500–$4,000+ per implant (often higher when the crown and imaging are included)
- Orthodontics: $3,000–$8,000 for braces or clear aligners
Many clinics offer staged treatment plans and financing options. If budget is a concern, ask your dentist which changes will make the biggest visible difference first.
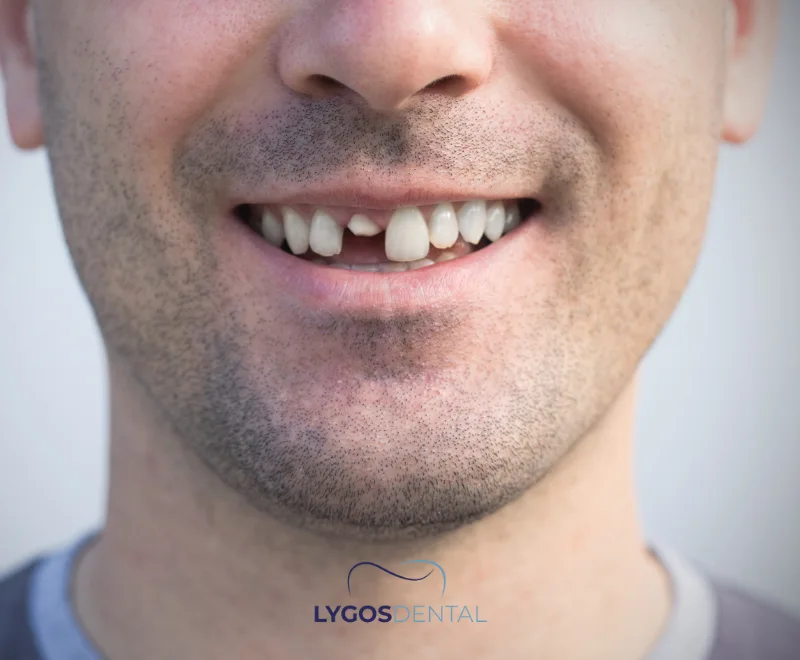
Who Is Cosmetic Dentistry Suitable For?
Cosmetic dentistry is often a good fit for people who are in overall good oral health and want to improve how their smile looks. Common reasons to consider cosmetic treatment include:
- Discolored or stained teeth
- Chipped, cracked, or worn edges
- Small gaps or uneven tooth shapes
- Crooked or crowded teeth
- Uneven gum line or a gummy smile
- Missing teeth
If you have untreated cavities, advanced gum disease, or severe bite issues, those usually need treatment first. A cosmetic dentist can tell you what’s realistic and what will help the result last.
Cosmetic dentistry can be as simple as whitening or as comprehensive as a full smile makeover. The best results come from a plan that balances appearance with long-term tooth and gum health.
Can Cosmetic Dentistry Improve My Smile? Frequently Asked Questions
Is cosmetic dentistry worth it?
Yes, if it improves function or confidence and fits your budget and expectations.
What are the disadvantages of cosmetic dentistry?
Disadvantages include cost, tooth sensitivity, irreversible enamel removal, maintenance needs, and occasional complications.
How long do cosmetic dental treatments last?
Whitening lasts months–2 years; veneers 10–15 years; bonding 3–10 years.
How painful is cosmetic dentistry?
Mild for most; numbing is used, but some sensitivity or soreness can occur.
Is cosmetic dentistry permanent?
No; some changes are irreversible, but restorations wear and may need replacement.
What is Anodontia
Anodontia: Causes, Symptoms, Diagnosis, And Treatment
Anodontia is a rare condition where a person is born without some or all teeth because tooth development never occurs. It is usually linked to genetics and may appear alone or with syndromes like ectodermal dysplasia. Dentists confirm it with an exam and dental X-rays, then plan treatment such as dentures, implants, or orthodontics.
Missing teeth can affect appearance, speech, and how well you chew. While many cases are caused by injury or decay, some people are born without certain teeth—or, more rarely, without any teeth at all.
When patients ask, “What is anodontia?”, the simplest answer is that it’s a congenital tooth-development disorder. With early diagnosis and a tailored plan, most functional and aesthetic concerns can be managed effectively.
What Is Anodontia?
Anodontia is the congenital absence of teeth due to disrupted tooth development during early growth. It can involve primary teeth, permanent teeth, or both. The condition ranges from missing a small number of teeth to the complete absence of all teeth.
Types Of Anodontia
Clinicians often group congenital tooth absence by how many teeth are missing. These categories help dentists plan timing, prosthetics, and long-term follow-up.
Complete Anodontia
- No teeth develop in the upper and lower jaws. This is extremely rare and often associated with genetic syndromes.
Partial Anodontia (Hypodontia)
- One or more teeth fail to develop. This is the most common pattern of congenital tooth absence.
Oligodontia
- Six or more teeth are missing (excluding wisdom teeth in many clinical definitions). It may occur on its own or with other congenital findings.
Symptoms Of Anodontia
Symptoms vary by severity and the age at which missing teeth become noticeable. Common signs include:
- Delayed eruption of baby teeth or permanent teeth.
- Visible gaps where teeth are expected to appear.
- Chewing difficulty and changes in diet choices.
- Speech differences, especially with missing front teeth.
- Changes in jaw growth or facial profile in more severe cases.
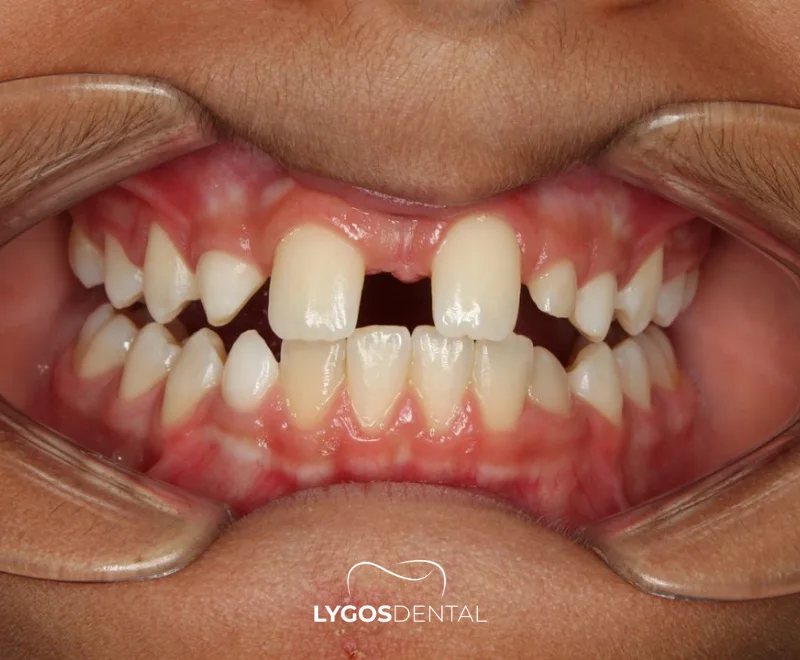
Table of Contents
Causes And Risk Factors
Anodontia is most often genetic. It can run in families or occur as part of a broader syndrome that affects ectodermal structures (such as hair, skin, sweat glands, and nails).
Potential contributors include:
- Genetic variants linked to tooth development (for example, EDA, WNT10A, PAX9, and MSX1).
- Syndromes such as ectodermal dysplasia.
- Less commonly, exposures during pregnancy that disrupt fetal development (for example, certain medications, radiation, or severe infections).
How Is Anodontia Diagnosed?
Diagnosis usually begins when tooth eruption is delayed or when teeth appear to be missing. A dentist confirms whether teeth are absent or simply unerupted using clinical and imaging findings.
- Dental examination to assess gums, spacing, bite, and jaw growth.
- Radiographic imaging (often a panoramic X-ray; sometimes CT/CBCT when detailed planning is needed).
- Genetic evaluation when a syndrome is suspected or there is a strong family history.

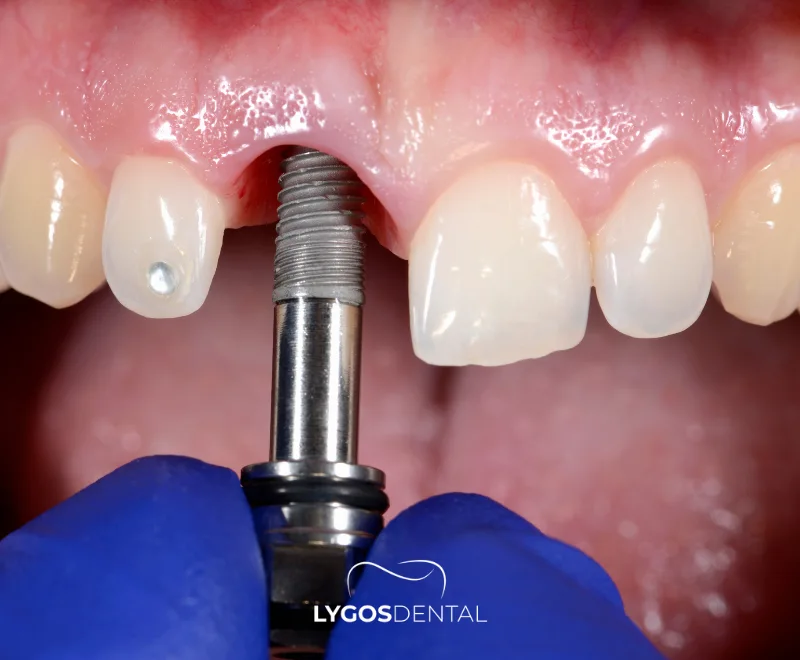
Treatment Methods For Anodontia
Treatment is individualized and depends on age, the number of missing teeth, jaw development, and overall oral health. Care is often coordinated between pediatric dentistry, orthodontics, prosthodontics, and sometimes medical genetics.
- Prosthetic treatment: removable partial dentures, complete dentures, or overdentures to restore function and appearance.
- Implant treatment: dental implants may be an option once jaw growth is appropriate and bone volume is sufficient.
- Orthodontic treatment: space management, bite correction, and support for prosthetic planning.
- Follow-up and adjustments: relines, remakes, or repairs may be needed over time—especially in growing patients.
- Genetic counseling: helpful for families when an inherited pattern is likely.
Anodontia FAQ
When is it too late to reverse gum disease?
It’s too late once periodontitis causes irreversible attachment or bone loss.
What is the best home remedy for gum disease?
Brushing twice daily and cleaning between teeth is the best home care for gum disease.
Can you repair receding gums?
Yes—receding gums can be repaired with periodontal treatment and gum graft surgery.
What toothpaste is good for receding gums?
A stannous-fluoride toothpaste helps reduce gingivitis and protect exposed roots.
Can I live a long life with gum disease?
Yes—with treatment and maintenance, gum disease can be controlled long-term.
How long do you have gum disease before teeth fall out?
Untreated periodontitis can lead to tooth loss over years to decades.
