What is Surgical Tooth Extraction
Surgical Tooth Extraction: What It Is, When It’s Needed, And Recovery
Surgical tooth extraction is a minor oral surgery used when a tooth can’t be removed with a standard “simple” extraction—most often because it’s impacted, badly broken, or the roots are difficult to access. The dentist makes a small incision, may remove a little bone, and sometimes divides the tooth into sections before removal, then closes the area with stitches.
What Surgical Tooth Extraction Means
Surgical tooth extraction is used when pulling a tooth straight out isn’t safe or possible. It’s commonly needed for impacted wisdom teeth, teeth that have broken at the gumline, or roots that are curved, deep, or fragile. The procedure is usually done under local anesthesia, and sedation can be an option for anxious patients.
Surgical vs Simple Tooth Extraction
A simple extraction removes a fully visible tooth using elevators and forceps, with no gum incision. A surgical extraction involves accessing the tooth through the gum, and sometimes the surrounding bone, to remove it with minimal trauma.
Surgical cases can take longer and may cause more swelling than a simple extraction. Most people still return to routine activities within a few days, depending on the tooth and the level of surgery.
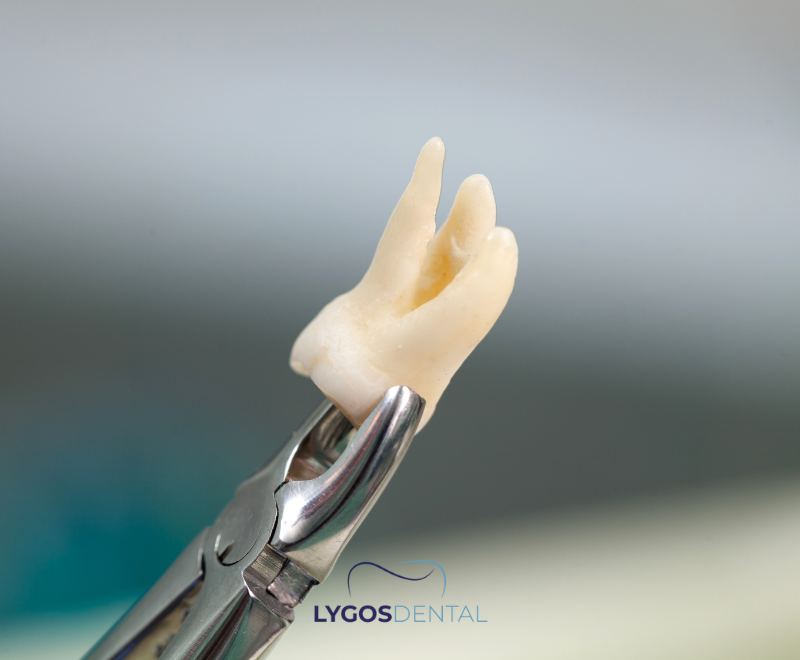
Table of Contents
When Surgical Extraction Is Needed
Dentists usually recommend a surgical approach in situations like these:
- Impacted teeth: The tooth is trapped under gum or bone, which is common with wisdom teeth.
- Severely broken teeth: The crown has fractured and there isn’t enough tooth above the gum to grip safely.
- Root fractures or complex root shape: A cracked root or sharply curved roots can make simple extraction unreliable.
- Advanced decay or infection: The tooth structure is too weak, or the surrounding tissue needs careful management.
- Certain orthodontic plans: Extractions may be needed for space, and a surgical approach is chosen if access is difficult.
- Severe gum or periodontal disease with mobility issues: Inflamed tissue and bone loss can complicate removal and healing.
How The Procedure Works
Exact steps vary by tooth position and imaging findings, but the flow is usually consistent:
- Numbing and comfort planning: Local anesthesia is used. Depending on the case, the clinic may offer sedation.
- Access: A small incision is made in the gum to reach the tooth. If needed, a small amount of bone is removed.
- Removal: The tooth may be lifted out in one piece or divided into sections to protect nearby tissue.
- Cleaning and closure: The socket is cleaned, and stitches may be placed to support healing.
- Aftercare instructions: You’ll be given guidance on pain control, diet, and oral hygiene, plus a follow-up plan if needed.
Recovery Timeline And Aftercare
Most surgical extraction sites heal in stages. Soft tissue often settles within 7–10 days, while deeper healing can take a few weeks, especially after impacted tooth removal.
First 24 Hours
Expect some bleeding, swelling, and soreness. Bite gently on gauze as directed, rest, and use cold packs on the outside of the cheek in short intervals. Avoid spitting, smoking, or using a straw, since suction can dislodge the blood clot.
Days 2–3
Swelling usually peaks and then starts to improve. Keep up with prescribed or recommended pain relief, and stay hydrated. If your dentist recommends it, gentle salt-water rinses can help keep the area clean.
First Week
Stick to soft foods, then slowly return to normal eating as comfort allows. Brush normally but gently around the site, and avoid poking the socket. Heavy exercise can raise bleeding risk, so keep activity light for a few days.
Weeks 2–4
Tenderness and food trapping usually reduce as the gum closes. If you had stitches, they may dissolve on their own or be removed at a follow-up visit, depending on the type used.
Risks And Possible Complications
Surgical extractions are routine, but complications can happen. Your dentist balances these risks against the benefits of removal.
- Dry socket (alveolar osteitis): Clot loss can cause increasing pain a few days after extraction.
- Infection: Persistent swelling, fever, or pus can signal infection and needs assessment.
- Prolonged bleeding: Oozing is common early on, but heavy bleeding should be addressed promptly.
- Nerve irritation: Lower wisdom teeth sit near nerves; temporary numbness is possible in some cases.
- Sinus communication: Upper back teeth can be close to the sinus, which may require specific aftercare.
When To Contact A Dentist Urgently
- Bleeding that doesn’t slow after firm gauze pressure
- Pain that worsens after day 3, especially with a bad taste or odor
- Fever, chills, or rapidly increasing swelling
- Trouble swallowing or breathing
- Numbness that doesn’t improve
Surgical Tooth Extraction Cost In Turkey
Pricing depends on the tooth’s position, whether it’s impacted, the imaging required (such as panoramic X‑ray or CBCT), the anesthesia or sedation choice, and the clinic’s location and expertise. Because the procedure can range from straightforward to highly complex, clinics typically quote after an exam.
As a rough reference, Turkish clinics and price guides for 2026 describe standard extractions starting from around 1,800–2,600 TL, while more complex or impacted (surgically removed) teeth may be several times higher, commonly falling in the mid‑thousands of TL depending on complexity. International patient packages may be priced differently if they include consultations, imaging, medications, and follow-up care.
Frequently Asked Questions
When is surgical tooth extraction necessary?
Surgical extraction is necessary when the tooth is impacted, broken, or not accessible for forceps.
What is the recovery time for a surgical tooth extraction?
Most people resume routine activities in 2–3 days; full bone healing takes weeks.
What to expect after a surgical tooth extraction?
Expect bleeding first hours, swelling 1–2 days, soreness, and gradual improvement over a week.
When can I go back to work after a surgical tooth extraction?
Desk work is often possible in 1–2 days; heavy labor may need 3–5.
Why does my tooth need to be surgically removed?
Your tooth needs surgery because it’s trapped, fractured, or too damaged for simple removal.
Is surgical extraction different from normal extraction?
Yes; surgical extraction uses an incision and sometimes sectioning, unlike simple forceps removal.
Dental Crown Fell Off?
My Dental Crown Fell Off: What Should I Do?
Save the crown, rinse it gently, and book a dental appointment as soon as you can. Keep the exposed tooth clean and avoid chewing on that side. If the crown fits, you may use over-the-counter temporary dental cement for short-term protection. Skip household glues, and seek urgent care for swelling, severe pain, or fever.
First, Check For Urgent Problems
A lost crown is usually fixable, but some symptoms should be treated as urgent. Contact an emergency dentist (or urgent dental service) if you notice any of the following:
- Facial swelling, a pimple-like bump on the gum, or pus
- Severe, worsening toothache that doesn’t settle with typical pain relief
- Fever, feeling unwell, or swollen lymph nodes
- Bleeding that won’t stop, or the crown came off after a significant injury
- Trouble swallowing or breathing (call emergency services)
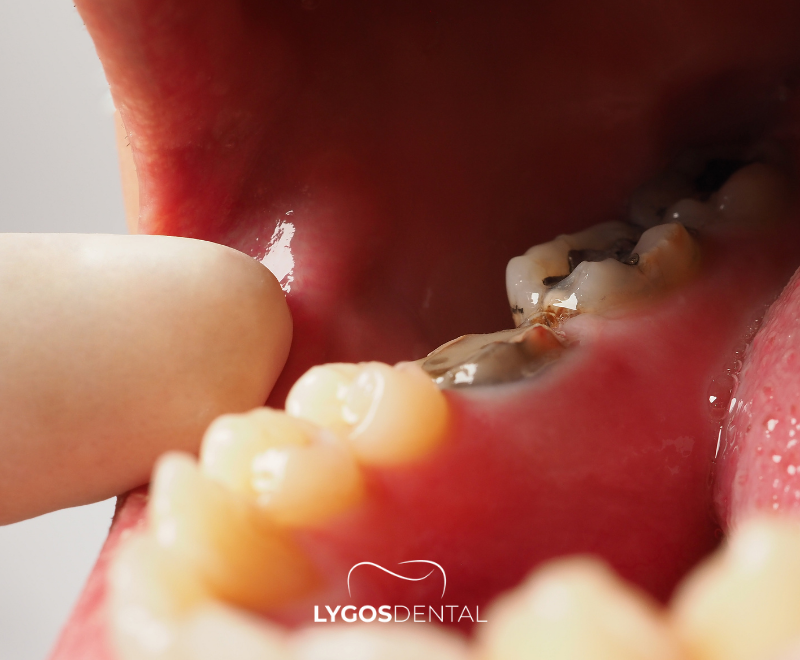
Table of Contents
Step-By-Step: What To Do When A Crown Comes Off
Most of the time, your goal is simple: protect the tooth and keep the crown safe so your dentist can assess it.
- Find the crown and store it safely.
Place it in a small container or tissue so it doesn’t get lost. Try not to swallow it if it came loose while eating.
- Rinse your mouth and the crown.
Use lukewarm water. Avoid scrubbing the crown aggressively—just remove obvious debris.
- Look at the tooth and the crown.
If you see a broken piece of tooth, sharp edges, or the crown is cracked, don’t try to force it back on.
- Protect the area.
If the tooth feels sharp, cover the edge with orthodontic wax (or sugar-free chewing gum as a very short-term option).
- Call your dentist and arrange the soonest appointment.
A crown can sometimes be re-cemented, but the tooth may need treatment first if there’s decay or damage underneath.
Can I Put The Crown Back On At Home?
You can sometimes place a crown back temporarily, but it’s not a permanent repair. The safest at-home option is an over-the-counter temporary dental cement or an emergency dental repair kit from a pharmacy.
How To Do A Temporary Refit Safely
- Wash your hands, then gently dry the tooth and the inside of the crown with clean tissue.
- Apply a small amount of temporary dental cement inside the crown (a thin layer is usually enough).
- Seat the crown carefully in the right direction. Bite down gently to help it settle.
- Wipe away any excess material and avoid eating on that side.
- See a dentist as soon as possible, even if it feels fine.
What To Avoid
- Do not use superglue or household adhesives. They can irritate tissue and make professional re-cementing harder.
- Do not force the crown into place if it doesn’t seat easily.
- Do not ignore the problem for days. Teeth can shift and the exposed tooth can decay quickly.

Why Dental Crowns Come Loose
Crowns can last many years, but they can still come off. Common causes include:
- Cement breaking down over time
- Tooth decay at the crown margin
- A crack or fracture in the tooth underneath
- Biting something hard, sticky foods, or clenching and grinding
- A crown that no longer fits as the tooth or gum line changes
What Your Dentist Will Do
Your dentist will check both the crown and the tooth to decide whether the same crown can be reused. If everything is intact, they may clean the crown, remove old cement, and re-cement it.
If there is decay, a crack, or not enough healthy tooth structure to hold the crown, you may need treatment first. That could mean a new filling/core build-up, root canal treatment, or a replacement crown.
How To Protect The Tooth Until Your Appointment
An uncovered tooth can feel sensitive to cold, heat, and sweet foods. These tips help you stay comfortable and reduce risk until you’re seen:
- Chew on the other side and avoid hard or sticky foods.
- Brush gently around the area and keep flossing, but slide floss out rather than snapping it up.
- If the tooth is sensitive, use toothpaste for sensitive teeth. You can dab a small amount directly onto the tooth and leave it for a few minutes.
- Use pain relief only as directed on the label, and avoid placing aspirin directly on the gum or tooth.
How To Prevent A Crown From Falling Off Again
Once your dentist has fixed the cause, a few habits can help your crown stay put longer:
- Avoid crunching ice and hard sweets, and be careful with sticky candies.
- If you grind your teeth, ask about a night guard.
- Keep up with routine checkups so early decay around the crown can be caught.
- Maintain daily brushing and interdental cleaning to reduce plaque at the crown edges.
FAQ
Is it common for dental crowns to fall off?
Yes, crowns sometimes fall off, especially if cement fails or tooth decays.
How long can you go without a crown that fell out?
A few days at most; see a dentist promptly and protect the tooth.
Can you put a crown back in after it falls out?
Yes, if the crown is intact, a dentist can usually recement it.
Can I still eat if my crown falls out?
Yes, eat soft foods and avoid chewing on that side.
What will a dentist do if a crown falls off?
A dentist will assess damage, clean surfaces, and recement or replace the crown.
What is the average lifespan of a dental crown?
About 10–15 years on average, though some last longer with good care.
What is Preventive Dentistry?
Preventive Dentistry
Preventive dentistry focuses on stopping dental problems before they start. It combines regular exams, professional cleanings, fluoride and sealants when needed, plus daily brushing, flossing, and smart diet habits. The goal is to reduce cavities and gum disease, catch issues early, and protect overall health while keeping treatment simpler and less costly.
What Preventive Dentistry Means
Preventive dentistry focuses on keeping teeth and gums healthy by reducing the chance of problems such as cavities, gum disease, and enamel wear. It blends professional care with daily routines at home. The aim is simple: protect your mouth now and avoid complex treatment later.
Table of Contents
Why Preventive Care Matters
Many dental issues start quietly, then become painful or expensive once they progress. Regular prevention helps spot early warning signs and deal with them while treatment is still straightforward. Oral health also connects with overall wellbeing, and research has found links between gum inflammation and systemic conditions, so keeping gums healthy is part of looking after the whole body.
Common Preventive Dentistry Services
A dentist tailors preventive care to your age, risk level, and medical history. These are the most common services:
- Dental exams and risk checks (including gum screening) to catch problems early
- X-rays when clinically needed to see areas that are hard to check by eye
- Professional cleaning (scale and polish) to remove plaque and tartar that brushing cannot reach
- Fluoride treatments to strengthen enamel and lower cavity risk
- Fissure sealants for deep grooves on back teeth, commonly used for children and teens
- Personalised advice on brushing, flossing, diet, dry mouth, and sensitivity
For many people, a check-up every six months works well, though some may need visits more or less often depending on their risk and the dentist’s advice.

Daily Habits That Help Prevent Cavities
Home care is where prevention really happens. Small routines done consistently make the biggest difference.
- Brush twice a day with fluoride toothpaste and spend at least two minutes each time
- Clean between teeth daily using floss or interdental brushes
- Keep sugary snacks and acidic drinks to occasional treats, especially between meals
- Drink water regularly, particularly after meals, to help wash away food acids
- Choose tooth-friendly foods (cheese, yoghurt, nuts, fibrous vegetables) more often
- Avoid tobacco and limit alcohol, since both raise the risk of gum disease and oral problems
Preventive Dentistry For Adults
Adult preventive care often focuses on gum health, existing restorations, and lifestyle factors. Many adults also deal with dry mouth from medications, which increases cavity risk. If you have crowns, bridges, implants, or dentures, cleaning routines and regular reviews help protect the investment and prevent inflammation around these areas.

Preventive Dentistry For Children
Starting early builds habits that last. Children benefit from age-appropriate brushing instruction, diet guidance, fluoride where indicated, and sealants on the back teeth once they erupt. Parents play a key role by supervising brushing until a child has the dexterity to do it well on their own.
Who Benefits Most From Extra Preventive Support
Preventive dentistry suits everyone, yet some people may need closer follow-up or more frequent cleanings:
- Children and teenagers, especially during orthodontic treatment
- Pregnant women, since hormonal changes can increase gum sensitivity
- People with diabetes or conditions that affect immunity
- Smokers and people with a history of gum disease
- Anyone with implants, dentures, or complex dental work
- People with persistent dry mouth or a high cavity rate
Frequently Asked Questions
What is preventive dentistry?
Preventive dentistry is care that prevents disease, including cleanings, exams, fluoride, sealants.
What is preventative dental?
Preventative dental means preventive dental care—services that stop cavities and gum disease.
What is the difference between general dental and preventative dental?
General dental covers all routine care; preventative dental focuses specifically on preventing disease.
What are the three levels of prevention in dentistry?
Primary prevents disease onset; secondary detects early; tertiary limits damage and restores function.
Are preventative fillings worth it?
Often no: sealants or remineralization are preferred unless decay already requires a filling.
What is the difference between preventive and restorative dentistry?
Preventive dentistry avoids disease; restorative dentistry repairs existing damage with fillings, crowns, or implants.
How To Fix Crooked Teeth
How To Fix Crooked Teeth
Crooked teeth are usually corrected with orthodontic treatment such as braces or clear aligners. An orthodontist checks crowding, bite, and jaw position, then creates a plan that gently moves teeth into alignment. Afterward, wearing a retainer as directed helps keep the result stable, along with good oral hygiene and regular check-ups.
Crooked teeth can affect confidence, but they can also make daily cleaning harder and put extra stress on the bite. The right fix depends on the cause, the amount of crowding or spacing, and whether the bite or jaw needs correction.
What Causes Crooked Teeth?
Teeth can become misaligned for several reasons, including genetics, crowding as adult teeth erupt, and jaw growth patterns. Childhood habits such as thumb sucking or prolonged pacifier use may push teeth out of position. Early or late loss of baby teeth, missing teeth, and mouth breathing related to airway issues can also contribute.

Table of Contents
Do Crooked Teeth Lead To Health Problems?
Yes. Misaligned teeth are not only a cosmetic concern; they can also affect oral health and comfort.
- Harder-to-clean areas that can trap plaque and tartar
- Higher risk of cavities and gum disease
- Uneven wear or difficulty chewing properly
- Jaw discomfort or joint strain in some cases
- Speech issues for certain bite patterns
Addressing alignment early can reduce these risks and make long-term maintenance easier.
Orthodontic Treatments For Straightening Crooked Teeth
Orthodontic treatment moves teeth gradually into a healthier position. Your orthodontist may recommend one of the following options based on your bite, aesthetics, and lifestyle:
- Metal Braces: A strong, reliable option that works well for mild to complex cases.
- Ceramic Braces: Similar to metal braces, but less noticeable because the brackets blend with tooth color.
- Lingual Braces: Braces placed behind the teeth, hidden from view, with suitability depending on bite and anatomy.
- Functional Appliances: Devices often used in growing patients to guide jaw development and improve alignment.
An orthodontic exam and X-rays help confirm which approach fits your needs.

Treating Crooked Teeth With Clear Aligners
Clear aligners are a popular, comfortable alternative for many people because they are nearly invisible and removable. They can work well for mild to moderate crowding or spacing, as long as they are worn for the recommended hours each day. Some complex bite problems may still require braces or a combined approach, so suitability should be confirmed by an orthodontist.
What To Consider After Straightening Crooked Teeth?
Retention is what protects your result. Teeth naturally try to shift over time, especially in the first months after treatment. Following your provider’s retainer plan and keeping up with hygiene and check-ups makes relapse much less likely.
Key points to keep in mind:
- Use a retainer: Wear it for the duration and schedule recommended by your orthodontist.
- Keep up oral hygiene: Brush and floss consistently, and use any cleaning tools suggested for retainers or attachments.
- Be mindful with food: If you have fixed retainers or braces, avoid very hard or sticky foods that can damage appliances.
- Attend regular check-ups: Routine visits help spot early shifting, gum issues, or wear.
- Limit smoking and alcohol: These habits can worsen gum health and staining, and can complicate maintenance.
Healthy gums and stable retention are the foundation of long-lasting straight teeth.

How Much Does Crooked Teeth Treatment Cost?
Treatment cost varies with the severity of misalignment, how long treatment is expected to take, and the method used. In many clinics, metal braces tend to be the lower-cost option, while clear aligners and less visible brace types may cost more.
Location, the orthodontist’s experience, and whether you need additional procedures can also affect pricing. For an accurate estimate, book a consultation so the provider can assess your bite and outline a full treatment plan.
FAQ: How To Fix Crooked Teeth?
When is it too late to fix crooked teeth?
Never, if your gums and bone are healthy enough for orthodontic treatment.
How can I fix my crooked teeth naturally?
You can’t reliably fix crooked teeth naturally; braces or aligners are needed to move teeth.
Can you fix crooked teeth?
Yes, orthodontics like braces or clear aligners can straighten most crooked teeth.
Is it worth fixing crooked teeth?
Yes, straightening can improve bite, cleaning, wear, and confidence for many people.
Is crooked teeth a turnoff?
Sometimes, but many people focus more on health, hygiene, and confidence.
What is Gum Cancer?
What Is Gum Cancer?
Gum cancer (also called gingival cancer) is a form of oral cavity cancer that develops in the tissues around the teeth. Most cases are squamous cell carcinoma, which starts in the thin, flat cells lining the mouth. Because early symptoms can resemble common gum problems, persistent changes should be checked by a dental professional.
Common Signs And Symptoms
Signs vary from person to person, but these are the symptoms clinicians most often associate with cancers of the mouth and gums:
- A sore or ulcer on the gum that doesn’t heal.
- A lump, thickened area, or uneven swelling along the gumline.
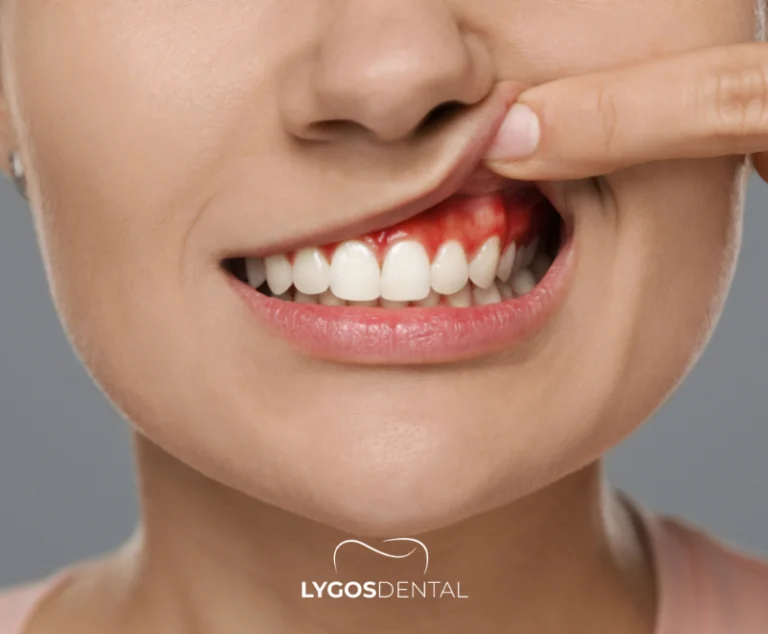
- Unusual bleeding from the gums that isn’t explained by brushing technique or gum disease.
- Red or white patches on the gums or nearby mouth lining.
- Loose teeth, a change in how dentures fit, or a tooth-extraction site that doesn’t heal as expected.
- Pain, tingling, or numbness in the gums, jaw, or lip.
If you have a mouth sore or gum change that lasts longer than two weeks, book a dental appointment. Most causes are not cancer, but it’s worth ruling out anything serious.
Table of Contents
Risk Factors
No single factor causes gum cancer, yet certain exposures and health conditions raise risk. The strongest, well‑established risks for oral cancers include tobacco and heavy alcohol use.
- Smoking cigarettes, cigars, pipes, or using smokeless tobacco.
- Frequent or heavy alcohol consumption (especially when combined with tobacco).
- Age (oral cancers are more common in older adults).
- A history of head and neck cancer.
- Weakened immune system.
- Poor diet low in fruits and vegetables.
- Chronic irritation and untreated gum disease may complicate oral health; they should be addressed even though they are not considered primary drivers in the way tobacco and alcohol are.

How Gum Cancer Is Diagnosed
Diagnosis starts with a dental or medical exam of the mouth, gums, tongue, and neck. If a suspicious area is found, a biopsy is done to confirm whether cancer cells are present. Imaging tests such as CT, MRI, or PET scans may be used to understand the size of the tumor and whether it has spread.
Treatment Options
Treatment depends on the tumor’s size, location, and stage, along with your overall health. A head and neck cancer team often includes an oral surgeon, ENT surgeon, oncologist, and radiation specialist.
- Surgery to remove the tumor, sometimes with removal of nearby lymph nodes.
- Radiation therapy, either after surgery or as a main treatment in selected cases.
- Chemotherapy given with radiation (chemoradiation) for higher‑risk or more advanced disease.
- Targeted therapy or immunotherapy may be considered for certain advanced or recurrent cancers, based on specialist evaluation.
Ask your care team how treatment may affect chewing, speech, and appearance, and whether dental work is needed before radiation.

Can Gum Cancer Be Prevented?
You can’t prevent every case, but you can lower risk and improve early detection.
- Stop using tobacco in any form.
- Limit alcohol and avoid combining heavy drinking with tobacco.
- Keep up with daily brushing and interdental cleaning to reduce gum inflammation and infections.
- Eat a balanced diet rich in fruits and vegetables.
- See a dentist regularly for check-ups and oral cancer screening, especially if you have risk factors.
Recovery And Follow-Up Care
After treatment, follow-up visits help monitor healing and check for recurrence. Your dentist and oncology team may recommend more frequent cleanings, saliva management, nutrition support, and exercises for jaw function. Report new sores, swelling, bleeding, or unexplained pain promptly rather than waiting for the next appointment.
Frequently Asked Questions
What are the first signs of gum cancer?
Nonhealing sore, persistent red/white patch, lump, bleeding, pain, loose teeth, numbness.
Is cancer of the gum curable?
Yes, early gum cancers are often curable with surgery, sometimes radiotherapy/chemotherapy.
What did gum cancer look like?
It may appear as an ulcer, red/white patch, swelling, or wartlike growth.
How to prevent gum cancer?
Avoid tobacco, limit alcohol, keep good oral hygiene, get regular dental checkups.
What are the 7 warning signs of mouth cancer?
Nonhealing ulcer, red/white patch, lump, persistent mouth pain, difficulty swallowing, numbness, persistent hoarseness.
What is the 3 finger test for mouth cancer?
Use three fingers to palpate mouth and neck for lumps, hardness, asymmetry.
How to Perform Tartar Cleaning?
What is tartar?
Tartar, also called dental calculus, forms when plaque mineralizes and hardens on the tooth surface. It can build up above the gumline and below it, where it may contribute to gum inflammation. Because tartar has a rough surface, it attracts more plaque and can make teeth look yellow or brown.
Why tartar forms
Tartar usually develops when plaque isn’t removed regularly and has time to harden. Some people also form tartar faster due to saliva composition, diet, or habits. Reducing risk comes down to consistent daily care and routine professional cleanings.
Common risk factors include:
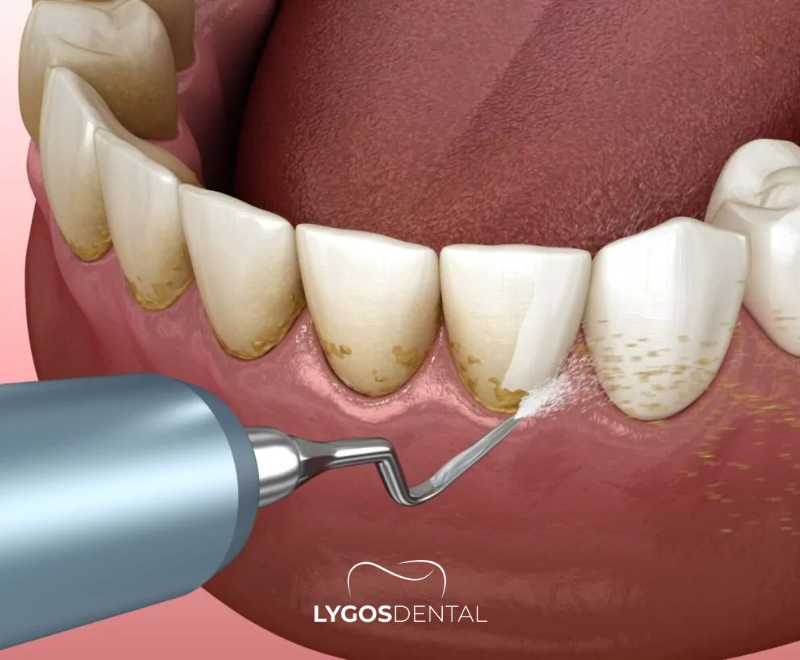
Table of Contents
Can you remove tartar at home?
Once plaque turns into tartar, it becomes tightly attached to the tooth and can’t be removed effectively with a toothbrush or floss. Trying to scrape it off at home can damage enamel or irritate the gums. If you notice hard deposits or bleeding gums, the safest option is a professional dental cleaning.
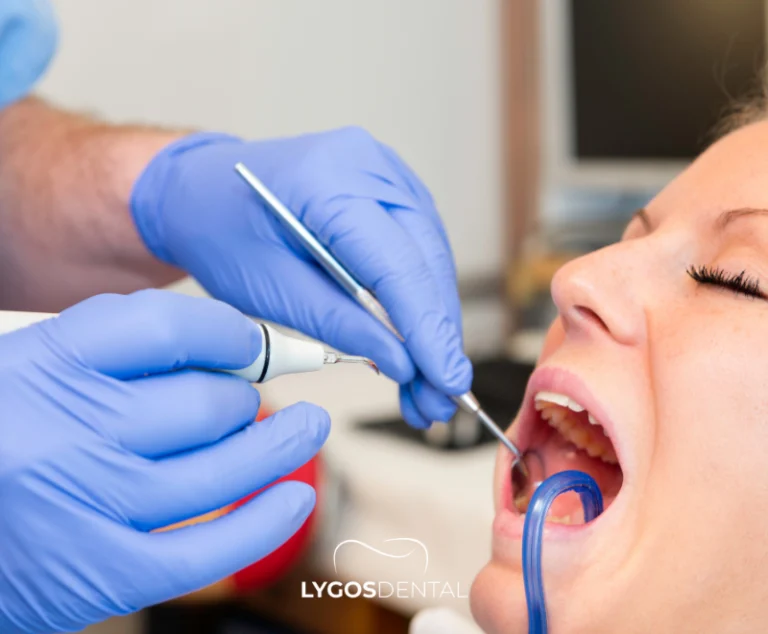
How professional tartar cleaning is performed
Professional tartar cleaning (scaling) is designed to remove calculus from tooth surfaces and, when needed, from below the gumline. The exact approach depends on how much tartar you have and whether there are signs of gum disease.
Typical steps include:
- Examination: The dentist or hygienist checks for tartar, gum inflammation, and areas that may need deeper cleaning.
- Ultrasonic scaling: An ultrasonic scaler uses vibrations and water to break up and flush away tartar.
- Hand scaling: Manual instruments remove remaining deposits and refine hard-to-reach areas.
- Polishing: Teeth are polished to smooth the surface and help reduce new plaque retention.
- Fluoride (optional): Fluoride may be applied to strengthen enamel and reduce sensitivity.
Aftercare tips
Some sensitivity is normal for a short time after scaling, especially if there was heavy tartar or gum inflammation. A few simple habits can help you stay comfortable and protect your gums while they settle.
- Avoid very hot or very cold foods for a few hours if you feel sensitive.
- Skip hard, very acidic, or very spicy foods for the first day if your gums are tender.
- Use a soft-bristled toothbrush and brush gently along the gumline.
- If recommended by your dentist, use a desensitizing toothpaste or mouthwash.
- Avoid smoking and tobacco products, which can slow gum healing.
How to prevent tartar buildup
Prevention is mainly about stopping plaque before it hardens. A consistent routine makes the biggest difference, especially cleaning between teeth where tartar often starts.
- Brush twice a day for two minutes using fluoride toothpaste.
- Clean between teeth daily (floss, interdental brushes, or water flosser).
- Rinse with an antiseptic or fluoride mouthwash if it suits your needs.
- Limit frequent snacking on sugary foods and reduce acidic drinks.
- Drink water throughout the day, especially after meals.
- Book routine dental check-ups and cleanings as advised.

Tartar cleaning costs in Turkey
Costs vary by city, clinic, and whether the cleaning is routine or involves deeper periodontal care. As a reference point, the Turkish Dental Association guide tariff lists detartraj (tartar cleaning) at 3,000 TL excluding VAT (3,300 TL including VAT) for a single jaw. Your final fee may be higher if additional procedures are needed.
FAQ
How is tartar cleaning done?
Dental tartar cleaning is done by a dentist using ultrasonic scaling and hand instruments.
How do you remove hardened tartar?
Hardened tartar is removed with professional scaling and, if needed, root planing.
Can I scrape tartar off my teeth myself?
No; scraping tartar yourself can damage enamel and gums and may miss deposits.
Does vinegar dissolve tartar?
No; vinegar cannot reliably dissolve tartar and may erode tooth enamel.
Will teeth fall out if tartar is removed?
Usually no; removing tartar reduces disease, but loose teeth reflect prior damage.
When is it too late to remove tartar?
Rarely; remove tartar anytime, but advanced periodontal disease needs urgent specialist treatment.
What is a Root Cavity?
What Is A Root Cavity?
A root cavity is decay on the root surface of a tooth, typically close to where the gum meets the tooth. When gums recede, the root becomes exposed to bacteria and acids from plaque. Unlike the crown of the tooth, the root is not protected by enamel, so it is more vulnerable to breakdown.
What Are The Symptoms Of A Root Cavity?
Root cavities can cause little or no pain at first. Common signs include:
-
- Sensitivity to cold, hot, or sweet foods and drinks
- A rough or soft spot near the gumline
- A brown, yellow, or darker area on the root surface
- Tender, inflamed gums around the tooth
- Pain when chewing or spontaneous pain in later stages
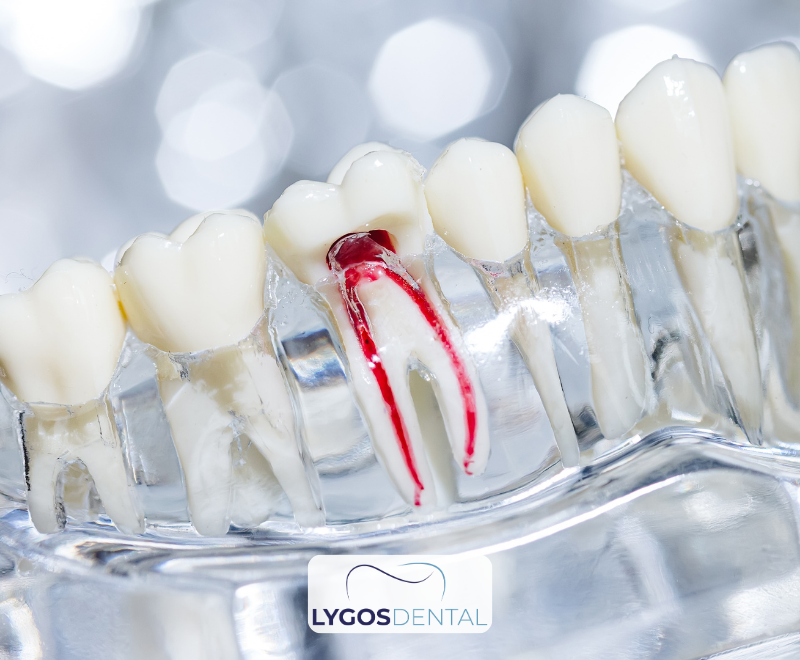
Table of Contents
What Causes Root Cavities?
Root decay usually happens when three things come together: exposed roots, plaque bacteria, and time. These factors can increase risk:
Gum Recession
Receding gums expose the root surface. Periodontal (gum) disease, aggressive brushing, and natural changes with age can all contribute to recession.
Plaque Buildup And Inadequate Oral Hygiene
Plaque collects easily along the gumline and between teeth. If it isn’t removed regularly, acids and bacterial byproducts can soften cementum and dentin and start a cavity.
Dry Mouth (Low Saliva Flow)
Saliva helps neutralize acids and wash away food particles. Medications, certain medical conditions, and dehydration can reduce saliva and make root decay more likely.
Diet And Frequent Snacking
Frequent sugary or starchy snacks keep plaque bacteria active for longer. Sipping sweetened drinks over time can have a similar effect.
Teeth Grinding Or Clenching
Grinding can wear tooth surfaces and irritate the gumline. That wear can make plaque retention easier and may worsen recession in some people.

How Dentists Diagnose Root Cavities
Dentists look for softened areas, discoloration, and plaque retention near the gumline. They may use dental X-rays to check how deep the decay goes and to rule out problems between teeth or under existing restorations.
Treatment Options For Root Cavities
Treatment depends on how early the decay is found and whether the tooth’s nerve is involved. Your dentist may recommend one or more of the following:
Professional Cleaning And Plaque Control
Removing plaque and tartar reduces bacterial load and can help stabilize very early lesions when combined with fluoride and good home care.
Fluoride Treatments
High-fluoride toothpaste or in-office fluoride varnish can help remineralize and harden early root lesions.
Silver Diamine Fluoride (SDF)
SDF can arrest decay in many cases and is quick to apply. It permanently darkens the treated decayed area, so it’s often used where appearance is less of a concern.
Fillings (Restorations)
If the surface is cavitated or the area can’t be kept clean, a filling is placed to protect the root. Dentists often choose materials that bond well in this area and release fluoride.
Root Canal Treatment
If decay reaches the pulp (nerve), a root canal removes infected tissue and allows the tooth to be restored.
Extraction And Replacement
If the tooth can’t be saved, removal may be recommended. Replacement options include an implant, bridge, or partial denture.

How To Prevent Root Cavities
Prevention focuses on controlling plaque at the gumline, protecting exposed roots, and supporting healthy saliva flow:
- Brush twice daily with fluoride toothpaste; use a soft-bristled brush and gentle pressure at the gumline.
- Clean between teeth daily with floss or interdental brushes.
- Ask your dentist whether a higher-fluoride toothpaste or fluoride varnish is appropriate for you.
- Limit frequent snacking and sipping sweetened drinks; keep water as your default beverage.
- Manage dry mouth: sip water, discuss medication-related dryness with your clinician, and consider sugar-free xylitol gum if appropriate.
- Keep regular dental visits so early root decay can be caught before it becomes a filling or root canal.
What Happens If A Root Cavity Is Left Untreated?
Untreated root decay can deepen and spread toward the tooth’s nerve. That can lead to persistent pain, infection, abscess formation, and tooth loss. Oral infections can also strain general health, particularly for people with certain medical conditions, so prompt treatment is the safest approach.
FAQ: Root Cavities
Can a cavity in the root be fixed?
Yes, root cavities can be filled or crowned; severe decay may need extraction.
What does a root cavity feel like?
Feels like sensitivity to cold, sweets, brushing, and sometimes a dull ache.
How bad does a cavity have to be to get a root canal?
A root canal is needed when decay reaches the pulp or causes infection.
Are root cavities more painful?
Yes, they can be more painful because root dentin is less protected.
What are the first signs of needing a root canal?
Early signs include lingering cold sensitivity, spontaneous pain, pain on biting, or swelling.
What happens if a root cavity goes untreated?
Untreated root decay can progress to abscess, severe pain, tooth loss, and systemic infection.
Matthew Lewis Dental Aesthetic
Matthew Lewis Dental Aesthetic
Matthew Lewis’ smile appears to have shifted from mild crowding and uneven colour to a straighter, brighter look. He has said he got braces after finishing the Harry Potter films, and his current symmetry suggests professional whitening and possibly veneers. Only Matthew Lewis or his dentist could confirm the exact treatments.
Matthew Lewis, best known as Neville Longbottom in the Harry Potter films, has been photographed with a noticeably more polished smile over the years. As his career moved into more adult roles, interest in his dental aesthetic grew—especially among fans curious about braces, whitening, and veneers.
Below is a clear breakdown of what’s publicly known, what dental professionals typically infer from photos, and what similar cosmetic treatments usually cost—particularly in Turkey, a popular destination for dental tourism.

Table of Contents
Who Is Matthew Lewis?
Matthew Lewis is a British actor from Leeds, England. He rose to global fame as Neville Longbottom in the Harry Potter franchise and has since worked across film, television, and theatre. His overall “glow-up” has often been discussed alongside changes to his hairstyle, physique, and smile.
Did Matthew Lewis Get His Teeth Done?
He has confirmed having braces after the final Harry Potter film wrapped, which fits the timing of his smile looking straighter in later appearances. Beyond orthodontics, any other cosmetic work is unconfirmed. That said, the brighter shade and more even edges seen in recent photos are consistent with professional whitening and, in some cases, veneers—though camera lighting and retouching can also exaggerate changes.

What Treatments May Explain The Smile Change?
Based on typical cosmetic dentistry pathways, a celebrity-style smile makeover often involves a combination of the following:
- Orthodontic treatment: Braces or clear aligners to correct crowding, spacing, or bite issues.
- Professional whitening: In-clinic bleaching to lift shade safely and evenly.
- Veneers: Thin shells bonded to the front of teeth to improve shape, alignment appearance, and colour.
- Edge bonding or cosmetic contouring: Subtle reshaping with composite resin or enamel recontouring for cleaner symmetry.
- Gum contouring (in select cases): Minor reshaping of gum margins to balance tooth-to-gum proportions.

Which Materials Are Commonly Used In Cosmetic Dentistry?
When veneers or bonding are involved, material choice affects both the final look and long-term maintenance. Common options include:
- Porcelain veneers: Known for stain resistance and lifelike translucency. Often chosen when patients want a long-lasting, highly polished finish.
- Composite resin veneers/bonding: Usually cheaper and faster to place, but more prone to staining and wear over time.
- Whitening gels: Professional systems typically use peroxide-based formulas applied under controlled conditions to reduce sensitivity risks.
- Dental bonding cements: Strong resin cements are used to bond veneers securely and protect margins when placed correctly.
Matthew Lewis Teeth Before And After
From early red-carpet photos to more recent appearances, the shift is easiest to describe in practical terms:
- Before: Slight misalignment and a more natural, varied tooth shape. Colour appears a little darker, which is normal without whitening.
- After: Straighter alignment and a brighter overall shade. The front teeth look more uniform at the edges, which can come from whitening, careful orthodontics, and sometimes veneers or bonding.
Cost Of Dental Veneers In Turkey
Prices vary widely by city, clinic reputation, dentist experience, material (composite vs porcelain vs E-max), and how many teeth are treated. The ranges below are typical estimates—not quotes—and travel, scans, temporary restorations, and aftercare can add to the total.
Typical Price Ranges (Per Tooth)
- UK: Often around £400–£1,500 per tooth for porcelain veneers, depending on the clinic and case complexity.
- US: Commonly about $900–$2,500 per tooth for porcelain veneers, varying by region and provider.
- Turkey: Frequently around $200–$600 per tooth, with premium materials such as E-max typically at the higher end.
Why People Choose Turkey
Turkey attracts international patients because many clinics offer modern digital workflows, short treatment timelines, and package-style pricing. That said, quality is not uniform, so the provider you choose matters more than the country.
A Quick Safety Checklist Before You Book
- Ask whether you need veneers or crowns (they are not the same).
- Request a conservative plan first: orthodontics, whitening, and bonding may achieve the goal with less enamel removal.
- Confirm the dentist’s registration, experience with cosmetic cases, and who will perform the preparation (not a technician).
- Insist on a proper exam (x-rays and gum health assessment). Veneers placed on unhealthy teeth rarely end well.
- Get the material type in writing (porcelain, E-max, composite) and ask about warranties and aftercare.
FAQ About Matthew Lewis Dental Aesthetic
Did Matthew Lewis get his teeth fixed?
Yes, he straightened them with braces after the final Harry Potter film.
Why did Matthew Lewis’s teeth look so different?
He wore false teeth as Neville, then later straightened his own teeth with braces.
Which actors have fake teeth?
Mike Myers, Robin Williams, Jonah Hill, and Channing Tatum wore fake teeth for roles.
Does Matthew Lewis have veneers on her teeth?
No confirmed report says he has veneers; he publicly described braces after Potter.
When did Matthew Lewis’s teeth change?
After Deathly Hallows filming ended in 2010, he got braces and changed.
Victoria Beckham Dental Aesthetic
Who Is Victoria Beckham?
Victoria Beckham (born Victoria Adams) became known as “Posh Spice” with the Spice Girls in the 1990s. After the band’s success, she moved into fashion and built a global brand as a designer and businesswoman.
Because she’s photographed constantly, even subtle changes in her appearance get noticed. Her smile is no exception, which is why searches around “Victoria Beckham teeth” and “dental aesthetics” remain popular.

Table of Contents
Has Victoria Beckham Had Cosmetic Dental Work?
Victoria Beckham hasn’t publicly shared a detailed list of any dental procedures, and only she and her dental team could confirm the specifics. What people often discuss online is based on comparing older and newer photos of her smile.
From a cosmetic dentistry standpoint, the kind of change people notice—brighter colour, smoother edges, and a more uniform shape—can often be achieved with professional whitening, minor orthodontics, veneers, or a combination of these treatments.

Treatments That Can Create A Similar Smile
A “celebrity smile” is rarely one single procedure. Dentists usually work in steps so the final result looks natural, suits the face, and protects the teeth.
Professional Teeth Whitening
In-clinic whitening can lift surface stains and brighten tooth shade in a controlled way. For longer-lasting results, many dentists combine an in-office session with custom take-home trays.
Whitening won’t change tooth shape or alignment, so it’s often used as a first step before any bonding or veneer work.
Orthodontic Refinement
Clear aligners or short-term braces can correct small gaps, rotations, and uneven tooth positions. Aligning teeth first may reduce how much enamel needs to be removed if veneers are later considered.
Dental Veneers
Veneers are thin shells bonded to the front surface of teeth to refine colour, shape, and symmetry. They’re typically planned with a smile design process so the length, width, and shade look balanced on the face.
Veneers aren’t a one-size-fits-all solution. Bite, gum health, enamel thickness, and habits like grinding all affect whether they’re a good option and how long they last.

Which Materials Are Used For Veneers?
Material choice affects the look, durability, and maintenance of a smile makeover. A dentist will usually recommend a material based on your bite, the shade you want, and how conservative the preparation can be.
Porcelain Or Ceramic Veneers
Porcelain (including popular ceramics like lithium disilicate/E.max) is chosen for its natural translucency and stain resistance. It’s often used when patients want a bright but realistic finish that holds its colour well.
Composite Resin Veneers
Composite veneers can be built directly on the teeth, often in fewer appointments. They can be a good option for smaller cosmetic changes, although they may stain or wear faster than porcelain depending on diet and habits.
Zirconia Restorations And Crowns
Zirconia is a strong material more commonly used for crowns, bridges, or cases where extra strength is needed. Since crowns cover the whole tooth, they usually require more reduction than veneers—so it’s worth asking whether a crown is truly necessary for a cosmetic goal.
Victoria Beckham Teeth Before And After
When people compare photos from the early Spice Girls era to more recent years, her teeth appear brighter, more even in length, and more uniform in shape. That combination is often associated with whitening plus cosmetic restorations such as veneers or bonding.
Photos can be influenced by lighting, angles, and retouching, so it’s best to treat online “before and after” claims as educated guesses rather than confirmed medical details.
Cost Of Dental Veneers In Turkey
Many patients look to Turkey for cosmetic dentistry because treatment packages can be more affordable than in the UK or the US. Prices vary widely by city, clinic standards, dentist experience, lab quality, and how much preparatory work is needed.
| Veneer Type | Typical Price Range (Per Tooth) |
| Composite Veneer | $150–$250 |
| Standard Porcelain/Ceramic Veneer | $250–$450 |
| E.max/Lithium Disilicate Veneer | $300–$600 |
| Zirconia (Often Used As Crowns/Restorations) | $250–$500 |
In the UK, porcelain veneers commonly fall in the mid-hundreds to over a thousand pounds per tooth, while US pricing often ranges from the high hundreds into the low thousands of dollars. Use any online price as a guide only—your final cost depends on your bite, gum health, and treatment plan.
What’s Often Included In Veneer Treatment
- Consultation and clinical examination
- X-rays or 3D imaging if needed
- Digital smile design and a trial mock-up (in many clinics)
- Temporary veneers during the lab phase (for porcelain)
- Final fitting, bite checks, and polishing
Questions To Ask Before You Book
- Will you be getting veneers or crowns—and why?
- How much tooth preparation is expected in my case?
- Who designs and makes the veneers (in-house lab or partner lab)?
- Can I see real before-and-after cases with similar starting teeth?
- What aftercare, follow-up, and warranty options are available?
How To Get A Similar Look Safely
If you like the polished, bright look associated with celebrity smiles, focus on planning rather than rushing to treatment. A good clinic will prioritise function and long-term oral health, not just colour and symmetry.
- Ask for a smile design preview and a temporary mock-up before anything permanent is done.
- Choose a natural shade that suits your skin tone and age; “ultra-white” isn’t always flattering.
- Discuss night guards if you clench or grind—this protects veneers and bonding.
- Keep regular hygiene visits and avoid using teeth as tools (opening packaging, biting pens).
FAQ: Victoria Beckham Dental Aesthetics
Has Victoria Beckham had her teeth done?
No public confirmation exists that Victoria Beckham has had dental work.
Why does Victoria Beckham rarely smile?
She says posing on her less-flattering side makes her avoid smiling in photos.
When did Beckham get his teeth fixed?
David Beckham hasn’t confirmed a date; his straighter, whiter smile appeared in early 2000s.
Does Victoria Beckham have dental veneers?
Victoria Beckham hasn’t confirmed veneers; experts only speculate based on photos.
What happened to Victoria Beckham’s teeth?
Her teeth look progressively straighter and whiter, suggesting cosmetic dentistry, but unconfirmed.
Steve Harvey Dental Aesthetic
Who Is Steve Harvey?
Steve Harvey is an American comedian, television host, producer, and author. He’s widely known for hosting shows such as Family Feud and for his long-running presence in mainstream entertainment.
Did Steve Harvey Get His Teeth Done?
Fans often ask whether Harvey’s smile is natural or the result of cosmetic dentistry. He hasn’t shared detailed public information about any procedures, so no one outside his dental team can say for certain. Still, the uniform shape and bright shade seen in many recent appearances are characteristics commonly associated with professional smile design.

Table of Contents
Possible Treatments Behind Steve Harvey’s Smile
A camera-ready smile is usually the result of more than one step. If Harvey did choose cosmetic treatment, these are among the most common options dentists use to create a similar look:
- Dental veneers: Thin shells bonded to the front of teeth to improve color, shape, and symmetry. They’re often used to mask chips, minor spacing, or uneven edges.
- Dental crowns: Full-coverage restorations used when a tooth needs more strength or when major shape changes are required. Crowns can also help create a consistent, even smile line.
- Professional whitening: In-office whitening or supervised take-home whitening can brighten natural teeth and help match surrounding restorations.
- Gum contouring: A reshaping of gum tissue that can balance the tooth-to-gum ratio when the gumline looks uneven.
Materials Commonly Used in Cosmetic Dentistry
The material choice affects how natural a result looks and how it wears over time. For high-visibility smiles, dentists typically work with these materials:
- Porcelain: Popular for veneers and many crowns because it can mimic natural enamel translucency and resists staining.
- Composite resin: A more budget-friendly option that can be bonded and shaped directly. It can look very natural, though it may stain or wear faster than porcelain.
- Ceramic (including zirconia-based options): Used for crowns and some veneer styles when durability is a priority. Modern ceramics can look very lifelike when designed and layered well.

Steve Harvey Teeth Before and After
Across long-running TV careers, public photos can show subtle changes in tooth color, edge shape, and alignment. In older images, many people notice more natural variation in shade and small irregularities—totally normal features. In newer appearances, Harvey’s smile often looks brighter and more uniform, which is consistent with cosmetic dentistry and professional maintenance.
Cost of Dental Veneers in Turkey
Turkey is a popular destination for cosmetic dentistry because many clinics combine modern techniques with comparatively lower fees. Pricing depends on the city, the dentist’s experience, the lab used, and the veneer material.
As a general guide, clinics often quote veneer prices per tooth in ranges like these:
- Composite veneers: often quoted around $150–$250 per tooth
- Standard porcelain veneers: often quoted around $250–$450 per tooth
- Premium porcelain options (for example, E‑max laminate veneers): often quoted around $300–$600 per tooth
Total cost usually depends on how many teeth are treated (many “smile line” cases involve 8–10 upper teeth), whether any prep work is needed (fillings, gum treatment, bite adjustments), and what’s included in the package (consultation, digital scans, temporary veneers, aftercare visits, transfers).
For the safest and most natural-looking result, choose a clinic that explains the plan clearly, shows real case photos, and prioritizes conservative tooth preparation when possible. A consultation with a dentist is the right starting point for a personalised quote.

FAQ – Steve Harvey Dental Aesthetic
Are Steve Harvey’s teeth veneers?
Some outlets say veneers; Steve Harvey hasn’t publicly verified this.
Does Steve Harvey have veneer teeth?
Some outlets say veneers; Steve Harvey hasn’t publicly verified this.
Did Steve Harvey have his teeth whitened?
Steve Harvey hasn’t publicly confirmed teeth whitening; veneers can also look very white.
Does Steve Harvey have dentures or veneers?
No public confirmation of dentures; coverage more often points to veneers.
Has Steve Harvey had any dental work done?
Some cosmetic sources suggest dental work; Steve Harvey hasn’t disclosed specific procedures.
