Laminate Veneers in Turkey | LYGOS DENTAL
Laminate Veneers in Turkey: A Comprehensive Guide to Your Dream Smile
Laminate veneers are thin porcelain or composite shells bonded to the front of teeth to improve color, shape, and symmetry. In Turkey, veneer treatment is popular with international patients because many clinics combine experienced cosmetic dentists, modern labs, and predictable timelines. Most smile makeovers take about 5–7 days, depending on the material and the number of teeth.
What Are Laminate Veneers?

Laminate veneers (often called veneers or “porcelain laminates”) are ultra-thin restorations placed on the visible surface of the teeth. They are designed to improve aesthetics while keeping as much natural tooth structure as possible.
Veneers can correct discoloration that does not respond to whitening, small chips, mild spacing, uneven edges, and minor alignment issues. They are usually made from porcelain (including lithium disilicate options such as E-max) or composite resin.
Why People Choose Turkey For Veneers
Turkey has become a well-known destination for cosmetic dentistry because many clinics offer competitive pricing, shorter waiting times, and treatment plans designed around travel.
The best results come from a combination of clinical planning (bite, gum health, and tooth preparation) and strong laboratory work. When those basics are done well, veneers can look natural rather than “overdone.”
How The Veneer Process Works In Turkey
1) Consultation And Smile Planning
Your dentist will evaluate oral health, discuss goals, and confirm that veneers are appropriate. For international patients, many clinics offer an online pre-assessment using photos and recent X-rays.
2) Tooth Preparation
For conventional laminate veneers, a very small amount of enamel is typically reduced so the veneer sits flush. Many clinics describe preparation in the range of roughly 0.3–0.5 mm, but the exact amount depends on your case and the material selected.
3) Impressions, Scans, And Temporaries
Your teeth are scanned or impressed and sent to a dental laboratory. Temporary veneers may be fitted so you can function normally while the final veneers are produced.
4) Try-In, Shade Check, And Bonding
At the final visit, the dentist checks fit, bite, and shade before bonding. Once approved, the veneers are cemented with adhesive and light-cured for strength.
For many patients, the full process takes around 5–7 days in Turkey. Complex cases, gum treatment, or additional procedures can extend the schedule.
Laminate Veneers Turkey Cost In 2026
Veneer pricing varies by city, clinic standards, the dentist’s experience, and the material used. Packages may also include accommodation, transfers, and follow-up checks, which can change the total value even when per-tooth pricing looks similar.
As a general 2026 guide, composite veneers are often priced around $180–$250 per tooth, standard porcelain veneers around $200–$350 per tooth, and premium options such as E-max laminate veneers commonly around $300–$600 per tooth. Prices can be higher for complex smile design or celebrity clinics.
What can affect your final quote:
- Number of veneers needed (e.g., 6–10 front teeth vs. a larger smile line).
- Material choice (composite, porcelain, E-max/lithium disilicate, zirconia-based options).
- Whether you need extra treatment first (cleaning, fillings, gum shaping, bite correction).
- Lab quality and customization (hand-layered ceramics, mock-ups, digital smile design).
Who Is A Good Candidate?
Laminate veneers can be a strong option when your teeth and gums are healthy and your main concerns are cosmetic. They are commonly used for:
- Severe or patchy staining that whitening cannot fully correct.
- Chipped, cracked, or worn edges.
- Small gaps between teeth.
- Mild shape or size irregularities.
- Smile makeovers that aim for a brighter, more symmetrical look.
If you grind your teeth heavily (bruxism), have active gum disease, or need major orthodontic correction, your dentist may recommend treating those issues first or considering alternative options.
Benefits And Limitations
Benefits
- Natural-looking esthetics when shape, shade, and translucency are planned well.
- Stain resistance for porcelain materials.
- Conservative compared with full crowns because less tooth structure is removed.
- Confidence boost for many patients who feel self-conscious about their smile.
Limitations To Understand
- Veneers are not “reversible” in most cases because some enamel is usually removed.
- They can chip or debond if you bite hard objects, use your teeth as tools, or have an untreated bite problem.
- Overly aggressive preparation or poor planning can lead to sensitivity or an unnatural result.
- You may need replacements in the future; longevity varies by material, bite, and care.
How To Choose A Reputable Clinic In Turkey
Clinic quality varies, so it pays to be selective. Use the checklist below before you book flights:
- Ask for before-and-after cases that look natural and similar to your starting point.
- Confirm the dentist who will do the preparation and bonding (not just the clinic brand).
- Request details on materials (brand/type), lab process, and whether a try-in or mock-up is included.
- Make sure your bite is evaluated, not just the front teeth.
- Clarify what happens if a veneer chips after you return home and what the warranty covers.
- Avoid promises of “instant Hollywood teeth” without a proper exam or x-rays.
Aftercare And Maintenance
Veneers do not require complicated maintenance, but they do need sensible habits. Brush twice daily, floss, and keep up with professional cleanings.
Avoid biting ice, pens, or very hard foods with the front teeth. If you clench or grind at night, ask your dentist about a night guard to protect your veneers and your natural teeth.
FAQs About Laminate Veneers In Turkey
How long do laminate veneers last?
With good oral hygiene and a stable bite, porcelain veneers often last around 10–15 years, and sometimes longer. Composite veneers usually have a shorter lifespan and may need polishing or repairs over time.
Are laminate veneers painful?
Most patients tolerate the procedure well. Local anesthesia is typically used during preparation, and any mild sensitivity after bonding usually settles within days.
Can I combine veneers with other treatments while in Turkey?
Yes. Some patients combine veneers with whitening, gum contouring, or orthodontic aligners. A proper plan matters so treatments happen in the right order.
Do clinics offer payment plans?
Some clinics offer staged payments or card payments for international patients, but terms vary. Confirm what is required as a deposit and what is due before bonding.
Do veneers need special care?
Treat them like natural teeth: brush, floss, and avoid habits that create heavy pressure. Regular dental check-ups help spot bite issues early.
Is the procedure safe for international patients?
It can be safe when clinics follow proper diagnosis, sterilization, and evidence-based planning. Choose providers who share clear medical documentation and aftercare guidance.
Oral and Maxillofacial Surgery | LYGOS DENTAL
Oral And Maxillofacial Surgery: Everything You Need To Know
Oral and maxillofacial surgery is a fascinating and essential branch of healthcare that addresses a wide range of conditions affecting the face, jaw, mouth, and teeth. This surgical specialty combines the precision of dentistry with the expertise of medical surgery, offering solutions for everything from impacted wisdom teeth to complex facial reconstructions.
If you’ve ever wondered about procedures like jaw realignment, treatment for facial trauma, or even dental implants, oral and maxillofacial surgery is at the forefront of these advancements. In this article, we’ll delve into the details of what oral and maxillofacial surgery entails, its risks and benefits, costs, and when you might need to see a specialist.
What Is Oral And Maxillofacial Surgery?
Oral and maxillofacial surgery (often shortened to OMFS) focuses on diagnosing and surgically treating conditions of the face, jaws, mouth, teeth, and surrounding tissues. Many surgeons complete both dental training and advanced surgical training, which is why they may handle problems that are too complex for routine dental care.

Common Conditions And Procedures
Oral and maxillofacial surgeons manage both functional and medically urgent problems, as well as planned corrective care. Common reasons people are referred include:
- Impacted or painful wisdom teeth
- Dental implant placement and related bone grafting
- Corrective jaw surgery (orthognathic surgery) for bite issues, jaw asymmetry, or airway concerns
- Facial trauma, including jaw fractures and soft-tissue injuries
- Temporomandibular joint (TMJ) problems when surgery is appropriate
- Cysts, benign growths, and evaluation/removal of suspicious oral lesions
- Congenital or developmental conditions such as cleft lip/palate (often as part of a multidisciplinary team)
The exact treatment plan depends on your diagnosis, imaging findings, and overall health. For major jaw surgery or trauma care, planning may include 3D imaging, virtual surgical planning, and coordination with orthodontic treatment.
Benefits And Risks
Every procedure has trade-offs. A good consultation should cover why surgery is recommended, what alternatives exist, and what recovery will realistically look like for your situation.
Potential Benefits
- Better chewing, speech, and jaw function
- Relief from pain or recurrent infections caused by impacted teeth or disease
- Improved facial balance after corrective jaw procedures
- Restoration after injury, helping return normal appearance and function
- A single specialist who can manage both dental and surgical aspects of care
Possible Risks
- Swelling, bruising, and temporary discomfort
- Bleeding, especially within the first 24–48 hours
- Infection (usually uncommon when post-op instructions are followed)
- Nerve irritation or injury, which can cause temporary or, rarely, persistent numbness
- Complications related to anesthesia or sedation, which are uncommon but possible
Your surgeon will explain how these risks apply to your specific procedure, and what steps are used to reduce them (sterile technique, careful planning, medication guidance, and follow-up care).
Typical Cost And Insurance Considerations
Costs vary widely by country, clinic setting, complexity, imaging needs, and whether anesthesia or a hospital stay is required. Many insurance plans cover procedures that are medically necessary, such as trauma repair, infection management, tumor removal, and jaw surgery performed to correct function or breathing. Cosmetic-only procedures are less likely to be covered.
As a general guide, wisdom tooth removal and surgical extractions can range from a few hundred dollars to several thousand depending on complexity, location, and anesthesia fees. Dental implant treatment is usually quoted as a package that may include the implant, abutment, and crown. If you are comparing quotes, ask what is included, what imaging is needed, and whether bone grafting may be required.
Before booking surgery, request a written estimate and ask your insurer what documentation they need (diagnosis codes, pre-authorization, and proof of medical necessity where relevant).
How To Find The Right Oral And Maxillofacial Surgeon
Start with referrals from your general dentist, orthodontist, or primary care clinician. When narrowing your options, focus on experience with your specific procedure and the quality of the consultation.
- Credentials and training that match your needs (hospital privileges can be a helpful sign for complex cases)
- Clear explanation of the diagnosis, options, and expected recovery
- A detailed plan for anesthesia/sedation and post-op pain control
- Transparent pricing and a written treatment estimate
- Comfort with the team and communication style—especially if you need multi-stage care
In the United States, some surgeons also hold certification through the American Board of Oral and Maxillofacial Surgery (ABOMS).
When To Call A Doctor
Seek urgent care if you have any of the following:
- Facial trauma with suspected fracture, uncontrolled bleeding, or changes in your bite
- Rapidly increasing swelling, fever, or spreading redness
- Severe pain that does not improve with prescribed medication
- Trouble breathing, swallowing, or opening your mouth
For non-urgent concerns—like wisdom tooth pain, recurring jaw clicking with discomfort, or a mouth sore that does not heal—book an evaluation. Early assessment often leads to simpler treatment.
FAQs
How long is recovery?
Recovery depends on the procedure. Simple extractions may improve within a few days, while jaw surgery and trauma repair can take weeks. Your surgeon will give a timeline based on your plan.
Will it hurt?
You should not feel pain during the procedure due to anesthesia or sedation. Afterward, soreness is expected, but it is usually manageable with the plan your surgeon provides.
How do I prepare?
Follow your pre-op instructions closely. They may include fasting, arranging transport home, reviewing medications, and planning soft foods and time off work or school.
Are oral and maxillofacial surgeons dentists?
Many are dentists with advanced surgical training, and some also have medical degrees. Training pathways vary by country.
Is it covered by insurance?
Coverage depends on your plan and the reason for treatment. Medically necessary procedures are more commonly covered than cosmetic-only care.
Tooth Abscess Causes – Dental Abscess – LYGOS DENTAL
Everything You Need to Know About a Tooth Abscess
A tooth abscess is a pocket of pus caused by a bacterial infection in or around a tooth. It can trigger severe toothache, swelling, and a bad taste in the mouth. Treatment usually requires a dentist to drain the infection and fix the cause (often a root canal or extraction). Seek urgent care right away if you have fever, facial swelling, or trouble swallowing or breathing.
A dental abscess is not something to “wait out.” Without proper treatment, the infection can spread to the jaw, face, or deeper tissues. Below you’ll find the main types of abscesses, common symptoms, the usual causes, and what dentists do to treat them. You’ll also learn what a wisdom tooth infection looks like and what to consider during pregnancy.
What A Tooth Abscess Is
A dental abscess is an infection that collects as pus either at the tip of a tooth’s root or within the gum and supporting tissues. It usually starts when bacteria reach the dental pulp (the soft inner tissue that contains nerves and blood vessels) or when gum disease creates a deep pocket around the tooth. The pressure from the infection is what often causes the intense, throbbing pain.
Types Of Tooth Abscess
- Periapical abscess: forms at the tip (apex) of the tooth’s root, usually after decay reaches the pulp.
- Periodontal abscess: develops in the gum near the root, often linked to gum disease or food trapped in a deep pocket.
- Gingival abscess: occurs in the gum tissue only, often related to a foreign object (such as a popcorn hull) lodged in the gum.
Symptoms You Should Not Ignore
Symptoms can vary, but most people notice pain and swelling. Sometimes the abscess drains and the pain eases, but the infection can still be present.
- Severe, throbbing toothache or gum pain
- Sensitivity to hot or cold
- Swollen, red, or tender gums
- Facial or jaw swelling on the affected side
- Bad breath or a foul taste (especially if pus drains)
- Pain when chewing, or difficulty opening the mouth (trismus)
When It Becomes An Emergency
Seek urgent dental or medical care the same day if you have fever, rapidly worsening swelling, or trouble swallowing, speaking, or breathing. These signs can mean the infection is spreading and needs immediate attention.
Common Causes
A tooth abscess usually happens when bacteria have a path into the tooth or gum tissues. The most common reasons include untreated tooth decay, advanced gum disease, and cracks or trauma that expose deeper layers of the tooth. Poor oral hygiene raises risk, but abscesses can also occur in people who brush well if there is decay under a filling or a deep gum pocket.
- Untreated cavities that progress into the pulp
- Gum disease (periodontitis) and deep gum pockets
- Cracked, chipped, or traumatized teeth
- Dental work complications (for example, leakage under a crown or filling)
Wisdom Tooth Infection (Pericoronitis)
A partially erupted wisdom tooth can trap food and bacteria under a gum flap. This is called pericoronitis and it can progress into a deeper infection or abscess if it spreads. Recurring infections are one reason dentists may recommend removing the wisdom tooth.
- Pain and swelling around the back molars
- Bad taste or bad breath
- Jaw stiffness and discomfort when chewing
- Swollen lymph nodes or fever in more severe cases
How Dentists Treat A Tooth Abscess
The goal is to drain the infection, relieve pain, and remove the source so it does not come back. Antibiotics may be used in certain situations, but they usually do not solve the problem on their own when the source remains in place.
1) Drainage
A dentist may make a small opening to drain pus and reduce pressure. This can provide fast relief, but the underlying cause still needs definitive treatment.
2) Root Canal Therapy
If the tooth can be saved, a root canal removes the infected pulp, disinfects the inside of the tooth, and seals it. A crown is often recommended afterward to protect the tooth from fracture.
3) Extraction (Infected Tooth Removal)
If the tooth is too damaged to restore, extraction may be the safest option. After removal, the socket is cleaned and you’ll receive aftercare instructions to lower the risk of complications. Your dentist can discuss replacement options such as an implant, bridge, or partial denture when healing is complete.
4) Antibiotics
Antibiotics may be prescribed when there are signs the infection is spreading, when you have fever, or when urgent dental treatment is not immediately available. Always take them exactly as directed and follow up for definitive dental care, because medication alone may not eliminate the source of infection.
Dental Abscess And Pregnancy
Dental infections should still be treated during pregnancy. Let your dentist and prenatal care team know you’re pregnant, especially if you’re in the first trimester or close to delivery. Many routine dental procedures are considered safe, and treating infection is often safer than delaying care.
Medication And Treatment Notes
- Local anesthetics and urgent treatments like drainage can be used when needed, with appropriate precautions.
- Acetaminophen is commonly used for pain in pregnancy; avoid taking any medication without your clinician’s advice.
- Certain antibiotics are commonly used in pregnancy for dental infections (for example, penicillins such as amoxicillin, and some cephalosporins). Your clinician will choose what’s appropriate for you.
Preventing A Future Abscess
Most abscesses start with decay or gum disease, so prevention focuses on catching problems early. Brush twice daily with fluoride toothpaste, clean between teeth every day, and keep up with routine dental visits. If you notice a cracked tooth, persistent sensitivity, or bleeding gums, book a dental exam before it turns into an emergency.
Frequently Asked Questions
Can a tooth abscess heal on its own?
Usually not. Symptoms may temporarily improve if the abscess drains, but the infection source often remains and can flare again or spread. A dentist should evaluate and treat it.
Is a tooth abscess contagious?
The abscess itself is not “catching” in the way a cold is. The bacteria involved are common in the mouth, but the infection develops when they get into vulnerable tissue through decay, gum pockets, or cracks.
How fast should I get treatment?
As soon as possible. Same-day care is recommended if you have swelling, fever, or significant pain, and emergency care is needed for trouble swallowing or breathing.
Are antibiotics enough?
They can help control infection in certain cases, but many abscesses also require dental treatment such as drainage, a root canal, or extraction to remove the source.
Gum Recession | LYGOS DENTAL
Gum Recession: Causes, Symptoms, Treatment, and Prevention
Gum recession happens when the gum line pulls away from the teeth, exposing more tooth surface or the root. It can cause sensitivity, make teeth look longer, and raise the risk of decay and gum infection. Early care—gentle brushing, daily flossing, and timely dental treatment—can slow progression and protect long-term tooth support.
What Is Gum Recession?
Gum recession is the gradual loss of gum tissue around a tooth, which exposes more of the tooth and sometimes the root. It may affect one tooth or several and often develops slowly, so it can be easy to miss at first. Catching it early matters because exposed roots are more vulnerable to sensitivity and decay.
Common Causes Of Receding Gums
- Aggressive brushing: Brushing with too much pressure or using a hard-bristled toothbrush can wear tissues down and contribute to recession.
- Gum disease (periodontal disease): Bacterial infection and inflammation can damage gum tissue and the bone that supports teeth.
- Genetics: Some people are more prone to thin or fragile gum tissue, even with good oral hygiene.
- Plaque and tartar buildup: Plaque that isn’t removed hardens into tartar, which irritates gums and can accelerate recession.
- Hormonal changes: Hormonal shifts can make gums more sensitive and easier to inflame, which may worsen recession in susceptible patients.
- Misaligned teeth or bite problems: Uneven biting forces can overload certain teeth and their supporting tissues.
Signs And Symptoms
- Tooth sensitivity to cold, hot, or sweet foods and drinks
- Teeth that look longer than before
- Notches near the gum line or a visible root surface
- Tender, swollen, or bleeding gums (especially with gum disease)
- Bad breath or a bad taste that doesn’t improve with brushing
Risk Factors
- Age: Recession becomes more common over time, especially if earlier inflammation or brushing habits have taken a toll.
- Tobacco use: Smoking and smokeless tobacco can irritate gums and worsen periodontal disease.
- Diabetes: Higher infection risk and inflammation can make gum problems harder to control.
- Teeth grinding or clenching: Excess force can strain teeth and the supporting tissues.
- Inconsistent oral hygiene: Irregular brushing/flossing allows plaque to build up and inflame gum tissues.
Why Gum Recession Matters
As gums recede, exposed roots can become sensitive and more likely to develop root cavities. Recession can also create areas that trap plaque, increasing the risk of gum inflammation and infection. If the underlying bone support is affected by gum disease, teeth may loosen over time.

Swollen Gums: What It Can Mean
Swollen gums often signal irritation or early gum disease. It can happen alongside recession, but swelling can also occur without visible recession. If swelling lasts more than a few days, comes with bleeding, or you notice a persistent bad taste, a dental exam is recommended.
Treatment Options For Swollen Gums
- Professional cleaning: Removing plaque and tartar helps reduce inflammation and makes home care more effective.
- Deep cleaning (scaling and root planing): A targeted cleaning below the gum line used when gum pockets and infection are present.
- Antibiotics (when needed): Sometimes prescribed to control bacterial infection, often alongside professional cleaning.
- Saltwater rinses: A warm saltwater rinse can soothe irritated tissues and reduce bacteria temporarily.
Can Invisalign Affect Gum Recession?
Clear aligners can be a safe way to straighten teeth, but gum recession can still occur if gums are already thin, if oral hygiene slips during treatment, or if biting forces concentrate on certain teeth. Regular checkups and excellent cleaning around aligners reduce risk, and your dentist or orthodontist can adjust the plan if gum irritation appears.
Managing Gum Recession
- Routine dental visits: Regular examinations help spot recession early and identify gum disease or bite issues.
- Gentle brushing technique: Use a soft-bristled toothbrush and light pressure. Angle the bristles toward the gum line rather than scrubbing.
- Daily interdental cleaning: Floss or use interdental brushes to remove plaque where brushes miss.
- Fluoride support: Fluoride toothpaste or in-office fluoride can reduce sensitivity and help protect exposed roots from decay.
Home Care That Supports Gum Health
Home care can improve comfort and reduce inflammation, but it won’t replace professional treatment when gum disease or significant recession is present. If you try home remedies, treat them as supportive care and stop if irritation worsens.
- Green tea: May support gum health thanks to naturally occurring antioxidants.
- Aloe vera (oral gel): Some people find it soothing for irritated gums when used as directed.
- Oil pulling: Swishing with coconut or sesame oil may reduce oral bacteria for some people, but it should not replace brushing and flossing.
Professional Treatment For Gum Recession
The right treatment depends on the cause, how much tissue has receded, and whether gum disease is present. A dentist will usually check pocket depth, inflammation, bite forces, and the thickness of your gum tissue before recommending a plan.
- Scaling and root planing: Deep cleaning to remove tartar and bacteria below the gum line and help tissues reattach.
- Gum graft surgery: Adds tissue to cover exposed roots and protect vulnerable areas when recession is significant.
- Regenerative procedures: Used in selected cases to encourage regrowth of lost bone and supporting tissues.
How To Help Prevent Gum Recession
- Brush twice a day with a soft-bristled toothbrush and light pressure
- Clean between teeth daily (floss or interdental brushes)
- Treat gum bleeding as a sign to check in with a dentist, not something to ignore
- Wear a night guard if you grind or clench, if recommended
- Avoid tobacco and keep diabetes well managed with your medical team
- Ask your dentist about bite issues or tooth alignment that may be stressing certain areas
What’s New In Gum Recession Care
Dentistry continues to refine less invasive ways to manage gum disease and protect exposed roots. Laser-assisted periodontal therapy is used in some practices to reduce bacteria and inflammation, and ongoing research looks at biologic materials that may support tissue healing. Your dentist can explain which options are appropriate for your case and what evidence supports them.
Frequently Asked Questions
What is gum recession?
Gum recession is when gum tissue pulls away from the teeth, exposing more tooth surface or the root.
What causes gum recession?
Common causes include gum disease, aggressive brushing, plaque and tartar buildup, genetics, tobacco use, and bite or alignment problems.
How do I know if I have gum recession?
Sensitivity, teeth that look longer, notches near the gum line, and gum inflammation are common clues. A dental exam can confirm the extent and the cause.
Can Invisalign lead to gum recession?
It can contribute in susceptible patients if hygiene is poor or tissues are already thin, but many people complete aligner treatment without recession when gums are healthy and monitored.
Are there home treatments for gum recession?
Home care can reduce inflammation and sensitivity, but it won’t rebuild lost gum tissue. Professional evaluation is important to rule out gum disease and prevent further damage.
What is the best treatment for swollen gums?
Professional cleaning and improved daily hygiene are the foundation. If infection or deep pockets are present, your dentist may recommend scaling and root planing and, in some cases, medication.
When To See A Dentist
Book an appointment if you notice new sensitivity, gum bleeding, a change in the gum line, or teeth that look longer. Prompt treatment can protect the roots, reduce inflammation, and prevent further loss of supporting bone.
Dental Implant Front Tooth | LYGOS DENTAL
Dental Implant For A Front Tooth
A front tooth dental implant replaces a missing incisor with a titanium or zirconia post placed in the jawbone and a custom crown on top. It looks and functions like a natural tooth, helps protect the bone under the gum, and avoids trimming healthy neighboring teeth. Treatment usually takes a few months from placement to final crown.
Table of Contents
What A Front Tooth Dental Implant Is
A dental implant for a front tooth uses three parts: an implant post, an abutment, and a crown. The post is placed in the jawbone, where it bonds during healing. Once the area is stable, a custom crown is fitted to match the color and shape of your surrounding teeth.
Why Front Teeth Need Careful Planning
Front teeth sit in a highly visible area, so the gum line, tooth shape, and color matching matter as much as strength. The bone at the front of the mouth can be thin, especially after a tooth has been missing for a while. Your dentist may recommend grafting or soft-tissue work to support a natural-looking result.
Key Benefits
- Natural look and feel: A well-made crown can mirror the translucency and contours of a real incisor.
- Bone preservation: The implant post helps reduce bone shrinkage that can happen after tooth loss.
- Strong, stable bite: Implants do not slip like removable options can.
- Protects neighboring teeth: Unlike a bridge, an implant usually does not require reshaping adjacent teeth.
- Long-term solution: The implant fixture is designed to last for many years, while the crown may need replacement from normal wear.
Front Lower Teeth Replacement
Implants can also replace lower front teeth. Those teeth guide the bite, support speech, and help keep the remaining teeth aligned. Replacing a missing lower incisor can reduce shifting and make cleaning easier compared with leaving a gap.
Which Implant Type Is Best For Front Teeth?
The best option depends on your bone volume, gum thickness, smile line, and medical history. Your clinician will also consider how quickly you need the tooth replaced and whether an extraction is involved.
Common Options
- Titanium implants: The most widely used option, valued for strength and long-term clinical track record.
- Zirconia implants: Metal-free and tooth-colored, sometimes chosen for aesthetics or metal sensitivities.
- Immediate implant placement: In select cases, an implant can be placed at the same visit as extraction, but only when the site is suitable.
- Mini implants: Occasionally used in narrow spaces, but they are not appropriate for every front tooth case and require careful evaluation.
How Natural Can A Front Tooth Implant Look?
A front tooth implant can look very natural when the crown, gum contour, and implant position are planned together. Dentists often use digital scans, photos, and shade guides to match the surrounding teeth. All-ceramic crowns (porcelain or zirconia-based) can reflect light in a way that closely resembles enamel.
Treatment Steps And Timeline
Most patients go through several stages, even when the process is streamlined. Your exact timeline depends on healing, bone quality, and whether grafting is needed.
- Consultation and imaging (often 3D scan) to plan implant position and crown shape.
- Extraction (if needed) and site preparation; grafting may be recommended to support the gum and bone.
- Implant placement surgery, followed by a healing phase while the post bonds to bone.
- Abutment and crown phase: impressions or scans are taken and the final crown is fitted and adjusted.
Cost Of A Front Tooth Implant
Pricing varies widely by country, clinic location, and case complexity. A single-tooth implant is usually priced as a bundle that includes the implant post, abutment, and crown.
Typical Cost Range (United States)
Many clinics quote around $3,000–$6,000 for one front tooth implant including the implant, abutment, and crown. The total can be higher if you need bone grafting, gum grafting, or temporary tooth solutions during healing.
What Influences Price
- Need for bone grafting or soft-tissue grafting
- Type of crown material and lab fees
- Implant brand and surgical complexity
- Specialist involvement (periodontist/oral surgeon vs general dentist)
- Imaging, sedation, and follow-up appointments
Dental Tourism In Turkey
Turkey is a popular destination for implant treatment because prices can be lower than in many Western countries. Depending on the clinic and materials used, a single implant package is commonly advertised in the few-hundred-dollar range, sometimes bundled with transfers and accommodation.
What To Check Before Booking
- Who performs the surgery and their credentials in implant dentistry
- The implant system and crown materials being used (ask for brand names and warranty terms)
- Whether the quote includes imaging, grafting (if required), and a temporary tooth for the front area
- The lab turnaround time and how many visits you will need
- Aftercare plan once you return home, including who will handle adjustments or complications
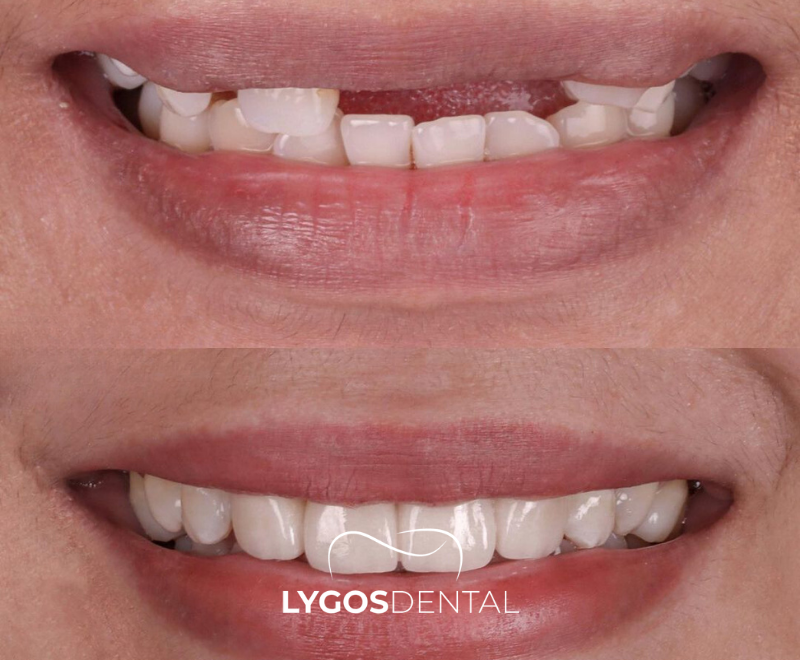
Before And After: What Usually Changes
Before treatment, a missing front tooth can affect confidence, pronunciation, and biting into foods. Over time, bone and gum tissue can shrink in the area, which may change the way the smile line looks.
After healing and the final crown, patients typically notice a fuller smile and easier speech. The goal is a crown that blends with neighboring teeth and a gum line that looks balanced from the front.
Aftercare And Long-Term Maintenance
Implants are not immune to gum disease, so daily cleaning matters. Brush twice a day, clean between teeth, and keep regular dental check-ups so the implant and surrounding gum stay healthy.
- Use interdental brushes or floss designed for implants to clean along the gum line.
- Consider a night guard if you grind your teeth.
- Avoid smoking during healing and long-term if possible, as it increases the risk of implant complications.
- Report bleeding, swelling, or a loose feeling early rather than waiting.
FAQ
Can dental implants be done on front teeth?
Yes, front teeth can be replaced with dental implants when bone and gums allow.
How much does the average front tooth implant cost?
Typically $3,000–$6,000 total per tooth, including crown and abutment.
What is the cheapest way to replace a front tooth?
A removable partial denture (“flipper”) is usually the lowest-cost front-tooth replacement.
How painful is a front tooth implant?
Usually mild-to-moderate soreness for several days; local anesthesia prevents procedure pain.
How long will a front tooth implant last?
Often 15–25+ years with good hygiene, bite control, and regular dental care.
Dental Tourism in Turkey | LYGOS DENTAL
Dental Tourism in Turkey
Dental tourism in Turkey means traveling to Turkey for dental care—often implants, veneers, crowns, or whitening—at prices that can be lower than in the UK, EU, or North America. Many clinics offer modern technology and English-speaking teams. The key is choosing a properly licensed clinic, confirming what’s included in your quote, and planning follow-up care at home.
Why Turkey Attracts Dental Patients
Turkey has become a well-known destination for patients who want high-quality dentistry with clearer pricing and shorter waiting times. Major cities such as Istanbul, Antalya, and Izmir host clinics that focus on international patients, with treatment plans built around travel schedules. For many visitors, the appeal is the mix of modern clinics, experienced dentists, and the chance to combine care with a city break.
That said, results depend heavily on the provider you choose. Dentistry isn’t a commodity, and the cheapest quote is rarely the best value. If you’re considering treatment abroad, it pays to understand common procedures, typical costs, timelines, and the practical checks that reduce risk.
What Dental Tourism In Turkey Means
In simple terms, dental tourism is when you travel to another country for dental treatment that is expensive or slow to access at home. In Turkey, international patients most often come for cosmetic dentistry, implant dentistry, and full-arch restorations.
Many clinics offer remote consultations before you travel. You can usually share dental X‑rays, photos, and a short medical history to receive a preliminary plan, then confirm details after an in-person exam and 3D imaging once you arrive.
Most Popular Dental Treatments
Dental Implants
Implants are a common reason people fly to Turkey, especially for missing teeth, unstable bridges, or loose dentures. Typical quotes vary based on implant brand, imaging, bone grafting needs, and whether the crown and abutment are included. Patient platforms and clinic price guides commonly list single-implant packages in the range of roughly $470–$700, with wider variation depending on what’s included.
Veneers And Smile Makeovers
Veneers are used to change tooth shape, colour, and alignment for a more uniform smile. Prices depend on material (composite vs porcelain), lab quality, and whether you need gum contouring or bite adjustments. Recent Turkey-focused price guides commonly put veneers around $150–$250 for composite and $250–$450 for porcelain, with premium materials (such as E‑max) often higher.
Teeth Whitening
In-office whitening is popular because it can be completed in a single visit. Pricing depends on the system used (LED, laser, Zoom-style treatments) and whether scaling is required first. Typical Turkish clinic ranges are often quoted around $200–$400 per session, while clinics in the US commonly list several hundred dollars to around $1,000 for in-office whitening.
Orthodontics
For orthodontics, Turkey offers both fixed braces and clear aligners. Because aligner treatment requires multiple check-ins, many visitors choose a local orthodontist for long-term monitoring or plan shared-care between countries.
Full-Arch And Full-Mouth Restorations
Patients who need extensive work sometimes choose full-arch solutions such as All-on-4 style treatment. Costs vary widely by material and complexity, but patient platforms frequently list All-on-4 packages in Turkey roughly between $2,100 and $6,000 per arch, compared with higher typical ranges reported in the US.
Typical 2026 Price Ranges
Real prices vary by city, clinic, and what’s included (consultations, CBCT scans, abutments, crowns, temporary teeth, sedation, and follow-ups). Use ranges as a planning guide, then ask for a written, itemised quote.
Single dental implant (often quoted as implant + abutment + crown): $470–$700+ in Turkey (packages vary)
Porcelain veneer (per tooth): $250–$450
Composite veneer (per tooth): $150–$250
In-office teeth whitening: $200–$400
All-on-4 style full-arch implants (per arch): $2,100–$6,000
If you’re comparing against the UK, private implant quotes are commonly reported in the £1,800–£4,500 range per tooth, and implants are only available through the NHS in limited clinical circumstances. That gap is one of the main reasons some patients look abroad.
Dental Holidays In Istanbul
Istanbul is the most common entry point for dental visitors because it has a large choice of clinics, direct flights, and plenty to do between appointments. Most treatment plans involve at least two visits to the clinic, with free time in between for light sightseeing.
If you’re having surgery (implants, grafting, extractions), keep plans low-key. Gentle walking is fine for many people, but crowded tours, long day trips, and heavy exercise can make swelling and discomfort worse.
What Results To Expect
Most reputable clinics can show real case examples, explain material choices, and set realistic expectations about shade, shape, and bite changes. Ask for examples that match your starting point, not just the ‘perfect smile’ cases.
If you’re choosing veneers or crowns, the planning stage matters as much as the final fitting. A careful smile design, temporary teeth (when needed), and a bite check reduce the chance of sensitivity, chipping, or an unnatural look.
How To Choose A Reputable Clinic
- Verify the dentist’s registration and the clinic’s licensing details, and ask who will perform each step (not just who you speak to online).
- Ask what brand of implant system and materials will be used, and whether the lab work is in-house or outsourced.
- Request an itemised quote that lists what is included and what could add cost (CBCT, extractions, bone grafting, sinus lifts, sedation).
- Review aftercare: medications, emergency contact, and how follow-up adjustments are handled once you return home.
- Be cautious with aggressive ‘same-day full mouth’ marketing. Some cases need staged treatment for best long-term stability.
Planning Your Trip And Treatment Timeline
For cosmetic procedures like whitening or a small number of veneers, a short trip may be enough. Implants usually require staged visits because the implant needs time to integrate with bone before the final crown is fitted.
Good clinics will explain what can be completed on the first visit, what needs healing time, and whether you should plan a second trip. If your schedule is tight, ask about temporary options that look good while you’re waiting for final restorations.
FAQs
Is dental treatment in Turkey safe?
Many clinics deliver excellent care, but safety depends on the provider. Choose a licensed clinic, confirm hygiene standards, and make sure your plan includes proper diagnostics (especially CBCT imaging for implants) and clear aftercare.
Do dentists in Turkey speak English?
In clinics that work with international patients, English-speaking staff are common, and translation support may be available. Ask who will translate during clinical appointments so nothing is lost in communication.
Can I travel around after treatment?
After non-invasive treatments you can usually explore as normal. After surgery, keep travel light for a few days and avoid long trips that would make it hard to return to the clinic if you need a check-up.
Will my dentist at home provide follow-up care?
Some dentists will help with routine checks, but they may not take responsibility for work done elsewhere. It’s smart to plan where you’ll go if you need adjustments, repairs, or ongoing maintenance.
Is Turkish dental work internationally recognised?
Quality is clinic-dependent. Focus on the dentist’s training, materials used, documentation (treatment notes, implant passport, warranties), and whether the clinic can provide clear medical records for your dentist at home.
Book A Consultation
If you’re considering treatment in Turkey, start with a remote consultation. Share recent X‑rays if you have them, explain your goals, and ask for a written plan that lists materials, timeline, and total costs. A clear, itemised quote makes it easier to compare clinics on quality—not just price.
Mini Dental Implant Treatment | LYGOS DENTAL
Mini Dental Implants
Mini dental implants are slim, one-piece titanium posts that can replace missing teeth or secure dentures with less surgery than standard implants. They’re often used when space is tight or bone volume is limited. Treatment can be faster and more affordable, but they’re not ideal for every bite pattern or every area of the mouth.
Table of Contents
What Mini Dental Implants Are
Mini dental implants (MDIs) are narrower than conventional implants and are commonly made as a single, integrated unit (implant and abutment together). Most are roughly 1.8–3.3 mm in diameter, which helps them fit into thinner ridges or narrower gaps.
Because they’re smaller, MDIs may be placed with a smaller incision or even a flapless technique in appropriate cases. Your dentist still needs adequate bone quality and careful planning to avoid nerves, sinuses, and adjacent roots.
How MDIs Differ From Traditional Implants
Traditional implants are wider and often use a two-piece design (implant body plus a separate abutment). MDIs are typically narrower and commonly one-piece, which can simplify placement and reduce components.
The trade-off is strength. Smaller diameter implants can be more vulnerable to overload, especially in patients who clench, grind, or place heavy biting forces on the restoration.
Benefits
- Less invasive placement in many cases, which can mean less swelling and a quicker return to normal routines.
- May reduce the need for bone grafting when bone width is limited (case-dependent).
- Useful in narrow spaces where full-size implants may not fit.
- Commonly used to stabilize removable dentures for improved comfort and chewing confidence.
- Often lower overall cost per implant compared with standard implants.
Limitations And Risks
- Not suitable for every tooth position. They’re often used for small-to-medium biting loads rather than high-load molar zones.
- Higher risk of mechanical complications if the bite is heavy or if the implant is overloaded.
- Like all implants, they can fail due to infection (peri-implant disease), poor oral hygiene, smoking, or uncontrolled medical conditions.
- May not be the best choice when significant bone height is missing or when the site needs major reconstruction.
How The Procedure Works
Most treatment plans start with an exam, X-rays, and often a 3D scan to assess bone and map safe implant positions. If you’re replacing a single tooth, the goal is to position the implant so the crown sits in a clean, easy-to-clean spot.
On the day of placement, the dentist prepares a small pilot site and threads the implant into the jawbone. Depending on stability and the type of restoration, a crown, bridge, or denture attachment may be fitted the same day or after healing.
Recovery And Aftercare
Recovery is usually mild, but you should expect some tenderness for a few days. Follow the clinic’s instructions on pain control, diet, and cleaning around the implant.
Long-term success comes down to daily plaque control and regular professional maintenance. If you grind your teeth, a night guard may be recommended to protect both the implant and the restoration.
How Long Mini Dental Implants Last
Lifespan varies widely. Many clinics quote ranges such as 6–15 years, but outcomes depend on bite forces, placement, the type of restoration, and maintenance habits. Some MDIs perform well for longer, while others may need replacement earlier if they’re overloaded or if gum disease develops.
Ask your dentist what success looks like in your specific case and what the backup plan is if an implant fails. That conversation is especially important if you’re considering MDIs for back teeth or for full-arch work.
Mini Dental Implants Cost
Pricing depends on country, clinic fees, and the complexity of your restoration. A commonly cited range is about $500–$1,500 per mini implant, while standard implants can cost several thousand dollars per implant before the crown or denture work.
Your total cost can also include scans, extractions, temporary teeth, denture conversion, and follow-up visits. If you’re comparing quotes, make sure you’re comparing the same scope of work.
Who May Be A Good Candidate
MDIs can be a good fit for patients who need denture stabilization, have limited bone width, or have narrow spaces between teeth. They’re also considered when patients want a shorter, less invasive route than graft-heavy treatment.
They may not be suitable if you have active gum disease, uncontrolled diabetes, heavy smoking habits, severe grinding, or complex bite problems. A clinician needs to evaluate these factors before recommending any implant type.
Questions To Ask At A Consultation
- Am I a candidate for MDIs, standard implants, or both—and why?
- Will you use a 3D scan, and how will you protect nearby nerves or sinuses?
- Can the restoration be loaded immediately, or do you recommend a healing phase?
- What maintenance visits do you recommend, and what costs should I expect over time?
- If an implant fails, what are the next-step options?
FAQs
Are mini dental implants any good?
Yes, for suitable candidates, they effectively stabilize dentures and some single-tooth replacements.
How much does a mini dental implant cost?
Typically US$500–$2,000 per mini implant, plus abutment/restoration and imaging fees.
How long does a mini dental implant last?
Often 5–10+ years, longer with good bone, hygiene, and low biting forces.
What is the failure rate of mini dental implants?
Reported failure is roughly 5–15% over several years, depending on case selection.
How painful are mini dental implants?
Usually mild-to-moderate soreness for 1–3 days, controlled with OTC pain relievers.
Can mini implants be done in one day?
Yes, many are placed and loaded the same day for denture stabilization.
What are the risks of mini implants?
Risks include infection, loosening, fracture, bone loss, gum recession, and rare nerve injury.
Tooth Reshaping | LYGOS DENTAL
Tooth Reshaping: The Complete Guide To A Beautiful Smile
Tooth reshaping (also called dental contouring or enameloplasty) is a conservative cosmetic treatment that gently smooths or shortens tooth edges by removing tiny amounts of enamel. It’s best for small chips, uneven edges, or slight overlaps. Results are immediate and permanent, but it must be done carefully to avoid sensitivity or weakening the tooth.
What Is Tooth Reshaping?
Tooth reshaping is a minimally invasive cosmetic dental procedure that changes a tooth’s shape, length, or surface by removing a very small amount of enamel. Dentists use it to refine minor issues such as uneven edges, tiny chips, pointy corners, or slight overlaps. Because enamel has no nerves, many patients feel little to no discomfort during treatment.
Tooth reshaping works best when your teeth and gums are healthy and the changes needed are subtle. If you have larger chips, deep cracks, significant crowding, or bite problems, your dentist may recommend alternatives such as bonding, veneers, or orthodontics.
How Tooth Reshaping Works
Most appointments are completed in one visit. Your dentist will aim for small, conservative adjustments so your teeth still look natural and stay strong.
Step-By-Step
- Consultation and assessment: Your dentist checks your enamel thickness, tooth shape, and bite. X-rays may be taken to confirm there’s enough enamel for safe contouring.
- Planning the changes: The dentist identifies the areas to smooth or shorten and discusses the expected result. Some clinics use photos or a quick mock-up to guide the plan.
- Shaping the enamel: Using fine diamond burs, discs, or polishing tools (and sometimes a laser), the dentist removes tiny amounts of enamel gradually. The goal is a smooth, symmetrical outline—not a dramatic reduction.
- Smoothing and polishing: The tooth surface is refined and polished so it feels natural and is easier to clean.
- Final checks and protection: Your bite is checked to make sure no area is taking extra pressure. A fluoride application may be used to support enamel after contouring.
Benefits Of Tooth Reshaping
- Fast results, often in a single appointment.
- Conservative treatment that preserves most of the natural tooth.
- Typically painless, with little or no downtime.
- Can improve symmetry and make small chips and edges less noticeable.
- A smoother surface may help reduce plaque retention in hard-to-clean spots.
Risks And Limitations
Tooth reshaping is generally safe when performed by an experienced dental professional, but it isn’t risk-free. The main consideration is that enamel does not grow back, so the change is permanent.
- Tooth sensitivity (usually temporary) if enamel is thinned near sensitive areas.
- Higher risk of wear, chips, or cavities if too much enamel is removed.
- Limited correction—reshaping cannot fix major crowding, gaps, or discoloration.
- Uneven bite forces if contouring changes how your teeth meet, which is why bite checks are essential.
How Much Does Tooth Reshaping Cost?
Pricing depends on the number of teeth treated, the complexity of the shaping, your location, and the clinician’s experience. Many clinics charge per tooth, and costs are often lower than veneer or orthodontic treatment for small cosmetic changes.
A common estimate is about $50–$400 per tooth. Your dentist should provide a written quote after examining your teeth.
What Can Affect The Price?
- Dentist’s experience and technology: Advanced cosmetic planning, magnification, or digital imaging may raise fees but can improve precision.
- Location and clinic overhead: Urban areas and specialist practices often price higher.
- Number of teeth and degree of adjustment: Minor smoothing of one edge costs less than contouring multiple teeth and balancing a bite.
Before And After: What Changes To Expect
Results tend to be subtle but noticeable. Before treatment, you may see small chips, uneven edges, or a tooth that looks slightly longer than its neighbor. After reshaping, the edges typically look smoother and more even, and the overall smile line can appear more balanced.
If you want a more dramatic change in shape or color, ask your dentist to show options such as bonding or veneers, often combined with contouring for a more refined result.
Who Is A Good Candidate?
Tooth reshaping is usually a good fit if you have healthy teeth with enough enamel and you want minor cosmetic refinement. It’s commonly used for:
- Small chips or worn edges.
- Slightly uneven tooth length or shape.
- Minor overlaps or pointy corners.
- Tiny rough spots that catch floss.
If you have thin enamel, active decay, gum disease, or significant bite issues, reshaping may not be recommended until those problems are addressed.
Aftercare Tips
- Brush twice daily with fluoride toothpaste and floss consistently.
- Avoid biting hard objects (ice, pens, packaging) to reduce the chance of chipping.
- If you clench or grind, ask about a night guard to protect the reshaped edges.
- Keep regular checkups so your dentist can monitor wear and polish if needed.
FAQs About Tooth Reshaping
Is tooth reshaping painful?
It’s usually not painful because the dentist works on enamel, which doesn’t contain nerves. Some people feel mild vibration or brief sensitivity.
How long does tooth reshaping last?
The change is permanent. Your teeth can still wear over time, so protecting them from grinding and maintaining good hygiene matters.
Can tooth reshaping fix crooked teeth?
It can mask very slight irregularities, but it cannot correct significant crowding or alignment problems. Orthodontic treatment is better for true straightening.
Can reshaping be combined with bonding?
Yes. Bonding can add tooth-colored material where needed, while reshaping refines edges for a smoother, more natural finish.
Will my teeth be sensitive afterward?
Some people notice short-term sensitivity to cold. It usually settles quickly, but persistent sensitivity should be assessed by your dentist.
Types of Dental Implants | LYGOS DENTAL
Tooth Reshaping: The Complete Guide To A Beautiful Smile
Tooth reshaping (also called dental contouring or enameloplasty) is a conservative cosmetic treatment that gently smooths or shortens tooth edges by removing tiny amounts of enamel. It’s best for small chips, uneven edges, or slight overlaps. Results are immediate and permanent, but it must be done carefully to avoid sensitivity or weakening the tooth.
What Is Tooth Reshaping?
Tooth reshaping is a minimally invasive cosmetic dental procedure that changes a tooth’s shape, length, or surface by removing a very small amount of enamel. Dentists use it to refine minor issues such as uneven edges, tiny chips, pointy corners, or slight overlaps. Because enamel has no nerves, many patients feel little to no discomfort during treatment.
Tooth reshaping works best when your teeth and gums are healthy and the changes needed are subtle. If you have larger chips, deep cracks, significant crowding, or bite problems, your dentist may recommend alternatives such as bonding, veneers, or orthodontics.
How Tooth Reshaping Works
Most appointments are completed in one visit. Your dentist will aim for small, conservative adjustments so your teeth still look natural and stay strong.
Step-By-Step
- Consultation and assessment: Your dentist checks your enamel thickness, tooth shape, and bite. X-rays may be taken to confirm there’s enough enamel for safe contouring.
- Planning the changes: The dentist identifies the areas to smooth or shorten and discusses the expected result. Some clinics use photos or a quick mock-up to guide the plan.
- Shaping the enamel: Using fine diamond burs, discs, or polishing tools (and sometimes a laser), the dentist removes tiny amounts of enamel gradually. The goal is a smooth, symmetrical outline—not a dramatic reduction.
- Smoothing and polishing: The tooth surface is refined and polished so it feels natural and is easier to clean.
Final checks and protection: Your bite is checked to make sure no area is taking extra pressure. A fluoride application may be used to support enamel after contouring.
Benefits Of Tooth Reshaping
- Fast results, often in a single appointment.
- Conservative treatment that preserves most of the natural tooth.
- Typically painless, with little or no downtime.
- Can improve symmetry and make small chips and edges less noticeable.
- A smoother surface may help reduce plaque retention in hard-to-clean spots.
Risks And Limitations
Tooth reshaping is generally safe when performed by an experienced dental professional, but it isn’t risk-free. The main consideration is that enamel does not grow back, so the change is permanent.
- Tooth sensitivity (usually temporary) if enamel is thinned near sensitive areas.
- Higher risk of wear, chips, or cavities if too much enamel is removed.
- Limited correction—reshaping cannot fix major crowding, gaps, or discoloration.
- Uneven bite forces if contouring changes how your teeth meet, which is why bite checks are essential.
How Much Does Tooth Reshaping Cost?
Pricing depends on the number of teeth treated, the complexity of the shaping, your location, and the clinician’s experience. Many clinics charge per tooth, and costs are often lower than veneer or orthodontic treatment for small cosmetic changes.
A common estimate is about $50–$400 per tooth. Your dentist should provide a written quote after examining your teeth.
What Can Affect The Price?
- Dentist’s experience and technology: Advanced cosmetic planning, magnification, or digital imaging may raise fees but can improve precision.
- Location and clinic overhead: Urban areas and specialist practices often price higher.
Number of teeth and degree of adjustment: Minor smoothing of one edge costs less than contouring multiple teeth and balancing a bite.
Before And After: What Changes To Expect
Results tend to be subtle but noticeable. Before treatment, you may see small chips, uneven edges, or a tooth that looks slightly longer than its neighbor. After reshaping, the edges typically look smoother and more even, and the overall smile line can appear more balanced.
If you want a more dramatic change in shape or color, ask your dentist to show options such as bonding or veneers, often combined with contouring for a more refined result.
Who Is A Good Candidate?
Tooth reshaping is usually a good fit if you have healthy teeth with enough enamel and you want minor cosmetic refinement. It’s commonly used for:
- Small chips or worn edges.
- Slightly uneven tooth length or shape.
- Minor overlaps or pointy corners.
- Tiny rough spots that catch floss.
If you have thin enamel, active decay, gum disease, or significant bite issues, reshaping may not be recommended until those problems are addressed.
Aftercare Tips
- Brush twice daily with fluoride toothpaste and floss consistently.
- Avoid biting hard objects (ice, pens, packaging) to reduce the chance of chipping.
- If you clench or grind, ask about a night guard to protect the reshaped edges.
- Keep regular checkups so your dentist can monitor wear and polish if needed.
FAQs About Tooth Reshaping
Is tooth reshaping painful?
It’s usually not painful because the dentist works on enamel, which doesn’t contain nerves. Some people feel mild vibration or brief sensitivity.
How long does tooth reshaping last?
The change is permanent. Your teeth can still wear over time, so protecting them from grinding and maintaining good hygiene matters.
Can tooth reshaping fix crooked teeth?
It can mask very slight irregularities, but it cannot correct significant crowding or alignment problems. Orthodontic treatment is better for true straightening.
Can reshaping be combined with bonding?
Yes. Bonding can add tooth-colored material where needed, while reshaping refines edges for a smoother, more natural finish.
Will my teeth be sensitive afterward?
Some people notice short-term sensitivity to cold. It usually settles quickly, but persistent sensitivity should be assessed by your dentist.
What is Tooth Extraction? | LYGOS DENTAL
Tooth Extraction: A Comprehensive Guide to Understanding the Procedure, Benefits, and Costs
A tooth extraction is the removal of a tooth from its socket to stop pain, control infection, or protect your overall oral health. Dentists use local anaesthetic for most cases, and oral surgeons handle more complex extractions such as impacted wisdom teeth. With proper aftercare, most people heal in about 1–2 weeks.
What Is Tooth Extraction?
Tooth extraction is a dental procedure where a tooth is removed from the gum and jawbone socket. It’s commonly recommended when a tooth can’t be saved with treatments such as a filling, root canal, or crown, or when keeping the tooth may harm nearby teeth and gums. Extractions are usually done in an outpatient setting.
Your dentist will numb the area with local anaesthetic, and may recommend sedation if you feel anxious or if the procedure is expected to be lengthy. After the tooth is removed, the goal is to protect a stable blood clot in the socket, because it’s essential for normal healing.
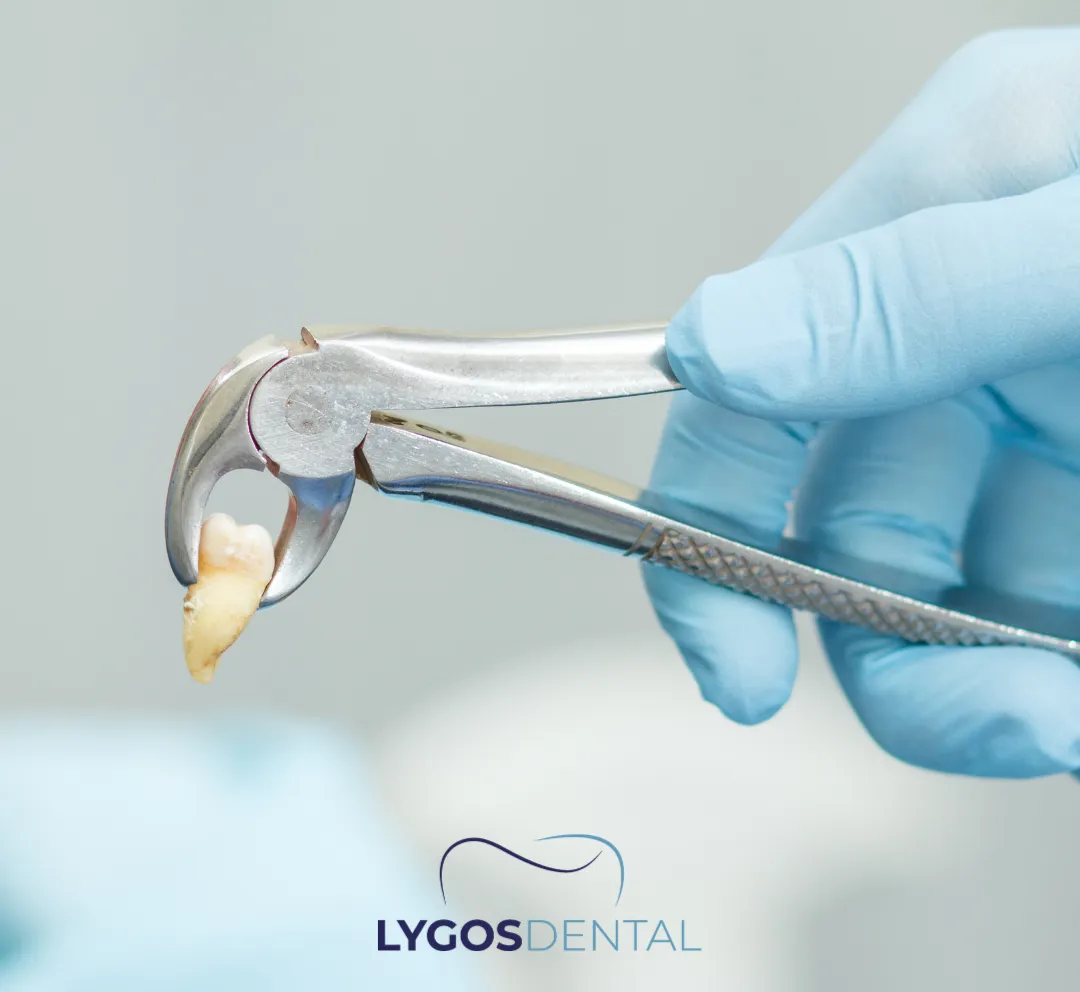
Types Of Tooth Extraction
Dentists generally perform two main types of extraction:
- Simple extraction: Used when the tooth is fully visible above the gum line. The dentist loosens the tooth and removes it with specialised instruments.
Surgical extraction: Used when the tooth is broken at the gum line, has curved roots, or is trapped under the gum (impacted). The clinician may make a small incision and, in some cases, remove a little bone or section the tooth to remove it safely.
When Is Tooth Extraction Recommended?
- Severe tooth decay or infection: If decay reaches the pulp and the tooth can’t be predictably restored, removing it may be the safest way to stop pain and prevent the infection from spreading.
- Advanced gum disease: Periodontal disease can weaken the bone and tissues that support teeth. When a tooth becomes very loose, extraction may prevent ongoing infection and discomfort.
- Overcrowding for orthodontic treatment: In some cases, removing one or more teeth creates space so the remaining teeth can align properly.
- Impacted wisdom teeth: Wisdom teeth often lack space to erupt. When they cause pain, recurrent gum infections, decay, or pressure on neighbouring teeth, removal is often advised.
- Teeth fractured beyond repair: Trauma can crack a tooth below the gum line or into the root. If a crown can’t stabilise it, extraction may be recommended.
- Preventive reasons: Occasionally, a tooth is removed to reduce the risk of future problems—for example, a problematic wisdom tooth that’s likely to cause recurring infection.
What Happens During The Procedure?
Most extractions follow a similar flow: an exam (often with an X‑ray), numbing the area, gently loosening the tooth, and removing it. If the extraction is surgical, your clinician may make a small opening in the gum and remove the tooth in one piece or in sections.
Before you leave, you’ll receive aftercare instructions tailored to your case. If sedation or general anaesthetic is used, you’ll need someone to accompany you home and you may be advised to rest for the remainder of the day.
Risks And Possible Complications
Tooth extraction is considered a safe procedure, but any surgical treatment comes with risks. Your dentist or surgeon will review your medical history and explain what applies to your situation.
- Dry socket: The blood clot dislodges or doesn’t form properly, causing significant pain and delayed healing. This is more common after lower wisdom tooth removal.
- Infection: Bacteria can enter the site, especially if aftercare instructions aren’t followed or if you have an existing infection.
- Nerve irritation or injury (rare): Lower molar and wisdom tooth extractions carry a small risk of temporary numbness in the lip, chin, or tongue.
Sinus complications: Upper back teeth can be close to the sinus. In rare cases, an opening can occur and may need additional care.
Benefits Of Tooth Extraction
- Relief from pain: Removing a badly decayed, infected, or cracked tooth can quickly reduce persistent pain.
- Prevention of infection spread: Extraction can help prevent infection from progressing to the jawbone or nearby teeth.
- Improved oral function: Once the problem tooth is removed and the area heals, chewing comfort often improves—especially when the tooth is replaced appropriately.
- Supports orthodontic outcomes: In selected cases, extractions create space to align teeth more effectively.
Wisdom Tooth Extraction
Wisdom teeth (third molars) typically erupt between ages 17 and 25. Because many people have limited jaw space, these teeth may come through at an angle, only partially erupt, or remain trapped under the gums.
When Is Wisdom Tooth Extraction Necessary?
Removal is commonly recommended when wisdom teeth are impacted, repeatedly inflame the gums, develop decay that’s hard to treat, or contribute to crowding or damage to neighbouring teeth. Your dentist may also suggest removal if imaging shows a high risk of future problems.
Tooth Extraction Near Me: How To Choose A Provider
If you’re comparing clinics, look for a licensed dentist or oral surgeon with clear experience in the type of extraction you need (simple, surgical, or impacted wisdom teeth). Patient reviews can be useful, but prioritise clinical credentials, transparent explanations, and a practice that explains anaesthetic options and aftercare clearly.
A short consultation can help you understand the treatment plan, expected recovery, and total cost. If you have dental insurance, ask the clinic to check your coverage and provide an itemised estimate before scheduling the procedure.
Tooth Extraction Cost
Pricing varies by location, the clinician’s experience, whether imaging or sedation is needed, and how complex the extraction is. Insurance may cover part of the cost when the extraction is medically necessary.
Typical cost ranges (may vary widely):
- Simple extraction: Often falls in the range of about $70–$250 per tooth.
- Surgical extraction: Commonly ranges around $200–$600 per tooth, depending on difficulty and setting.

Wisdom Tooth Extraction Cost
Wisdom tooth removal can cost more than routine extractions because the teeth are often impacted and may require sectioning, bone removal, and/or deeper sedation. Total costs are also influenced by how many teeth are removed in one visit and the type of anaesthesia used.
Typical cost ranges (may vary widely):
- Erupted (non‑impacted) wisdom tooth: Often similar to a simple extraction, commonly around $75–$250 per tooth.
- Impacted wisdom tooth (surgical): Frequently in the $300–$1,000+ per tooth range, depending on depth and complexity.
- All four wisdom teeth: Can range from the low thousands upward, especially if multiple impacted teeth and IV sedation are involved.
Care After Tooth Extraction
Good aftercare protects the blood clot and lowers the risk of dry socket and infection. Follow your clinician’s instructions, since recommendations can vary based on the tooth removed and your medical history.
- Control bleeding: Bite on gauze for 30–45 minutes. Replace as directed, and avoid spitting forcefully for the first day.
- Reduce swelling: Use an ice pack on the outside of the cheek in short intervals during the first 24 hours.
- Manage discomfort: Take any prescribed medication as directed. Over‑the‑counter pain relief may be appropriate if your dentist confirms it.
- Protect the clot: Avoid smoking, vaping, alcohol, drinking through a straw, or vigorous rinsing for at least 48 hours (or longer if advised).
- Eat and drink carefully: Choose soft foods, avoid very hot drinks, and chew away from the extraction site for the first few days.
- Keep the mouth clean: Brush gently, avoiding the socket. If you’re told to rinse, do it gently—often starting the day after the procedure.

When To Call Your Dentist
Contact your dental provider promptly if you have heavy bleeding that doesn’t slow, fever, worsening swelling after the first 2–3 days, a bad taste or pus, or severe pain that starts a few days after the extraction (which can be a sign of dry socket).
Frequently Asked Questions
How long does healing take?
Most people feel significantly better within a few days. Soft tissue often heals in about 1–2 weeks, while the underlying bone can take longer.
Will I need a replacement tooth?
If a molar or visible tooth is removed, ask about replacement options such as an implant, bridge, or partial denture to prevent shifting and restore chewing function.
Can I go back to work the same day?
Many people return to normal activities the next day after a simple extraction. Surgical cases, especially wisdom teeth with sedation, often need more recovery time.
