Advantages of Zirconium Dental Crowns
Advantages Of Zirconium Dental Crowns
Zirconium (zirconia) dental crowns are all-ceramic restorations known for a natural, light-reflecting look and strong bite resistance. They are gum-friendly, metal-free, and less likely to cause temperature sensitivity than metal-supported options. For many patients, they provide a durable, aesthetic solution for damaged, stained, or heavily restored teeth.
Table of Contents
What Are Zirconium Dental Crowns?
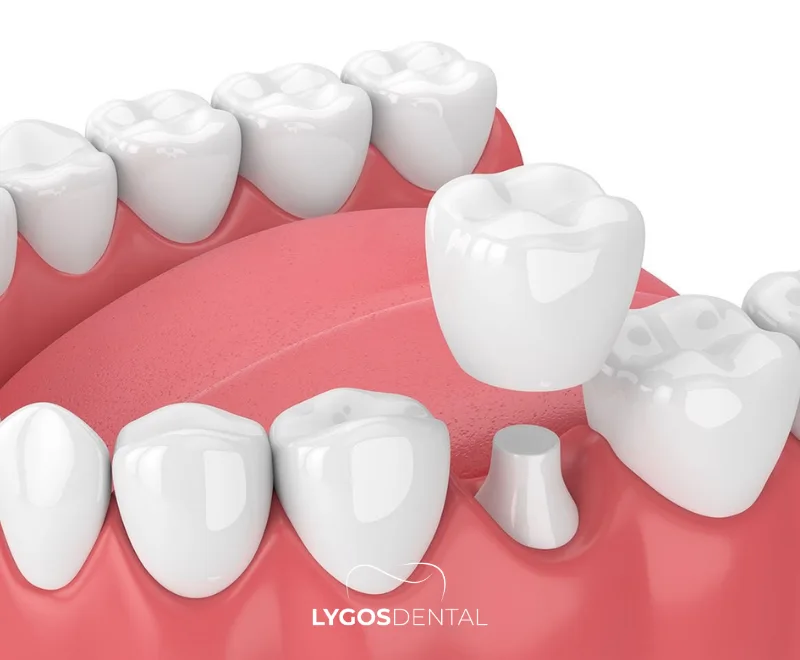
A zirconium dental crown is made from zirconium dioxide (zirconia), a white, high-strength ceramic used widely in modern dentistry. Because it contains no metal, it avoids the dark gum-line shadow sometimes seen with metal-supported crowns. Its semi-translucent structure helps the crown blend with nearby teeth for a more natural finish.
When Are Zirconium Crowns Recommended?
Zirconium crowns are commonly used when a tooth needs both strength and an aesthetic upgrade, such as:
- Severely discolored or darkened teeth that don’t respond well to whitening
- Broken, cracked, or worn teeth that need full coverage
- Cosmetic reshaping when orthodontics isn’t preferred or isn’t suitable
- Replacing old crowns that look unnatural or irritate the gums
Key Advantages Of Zirconium Crowns

Zirconium crowns are suitable for individuals of all ages with high aesthetic concerns. They are especially recommended for people with:
- Aesthetic expectations,
- Crooked or misaligned teeth,
- Tooth discoloration issues,
- Wide gaps between teeth,
- Broken or worn tooth structure,
- Dissatisfaction with previous metal-supported crowns.
Thanks to the advantages of zirconium crowns, they can also be safely used for individuals with sensitive gums.
Zirconium Dental Crown Prices in 2025
As of 2025, the cost of zirconium dental crowns can vary depending on the quality of material used, the number of crowns, the dentist’s experience, and the clinic’s location.
Generally, the price for a single zirconium crown ranges between 3,000 TL and 7,500 TL. Some clinics may also offer package deals for multiple teeth (e.g., 6 or 8 crowns).
Considering the advantages of zirconium crowns, their long lifespan and aesthetic benefits make them a cost-effective investment.
Post-Treatment Care for Zirconium Crowns
Natural-Looking Aesthetics
Zirconia can be layered or shaded to match surrounding teeth closely. Because it is metal-free, it doesn’t create gray reflections at the gum margin. This is especially valuable for visible front teeth and smile makeovers.
High Strength And Long-Term Performance
Zirconium crowns are designed to handle chewing forces well and can be suitable for both front and back teeth. Longevity depends on bite habits, crown design, and oral hygiene, but many patients use them for years without issues. Your dentist will check your bite to reduce the risk of chipping or wear.
Gum Compatibility And Low Allergy Risk
Zirconia is biocompatible, meaning it is generally well tolerated by soft tissues. For patients who are sensitive to metals or have a history of gum irritation, zirconium crowns are often a comfortable option. A precise fit and good plaque control still matter for keeping gums healthy.
Lower Temperature Sensitivity
Compared with metal-supported crowns, zirconium typically transmits temperature less. That can help reduce discomfort with hot or cold foods, particularly for people with sensitive teeth. Sensitivity can still occur if the tooth nerve is inflamed or if the bite needs adjustment.
Stain Resistance And Easy Maintenance
Zirconium crowns are resistant to staining from everyday foods and drinks such as tea and coffee. They don’t discolor the way some older materials can over time. Routine brushing, flossing, and professional cleaning keep the margins healthy and the smile bright.
Zirconium Vs Porcelain Crowns

The right crown depends on aesthetics, bite forces, gum health, and budget. Traditional porcelain crowns are often supported by metal, which can create a dark line near the gums and may affect light reflection. Zirconium crowns are fully ceramic, so they typically offer a more natural look at the gumline.
For front teeth, zirconium is frequently chosen for its light-handling and lifelike appearance. For back teeth, the decision may depend on your bite, grinding habits, and how much tooth structure remains. A dentist can recommend the most suitable material after an examination.
Who Is Suitable For Zirconium Crowns?
Zirconium crowns can be a good fit for many adults who want a durable, natural-looking result, including those with:
- High aesthetic expectations (especially for front teeth)
- Misaligned teeth that need cosmetic correction
- Persistent tooth discoloration
- Gaps that require restorative reshaping
- Broken, chipped, or heavily filled teeth
- Unwanted appearance or gum irritation from older metal-supported crowns
They can also be appropriate for people with sensitive gums, as long as daily cleaning and regular check-ups are maintained.
Zirconium Dental Crown Prices In 2026
Pricing varies by clinic, location, dentist experience, lab quality, and the type of zirconia used (standard, multilayer, or premium options). The final cost can also change if additional treatments are needed, such as root canal therapy, gum treatment, or a build-up under the crown.
In Turkey, clinics may quote a per-tooth zirconium crown price in a broad range—often roughly 7,500 TL to 15,000 TL. Some clinics offer package pricing when multiple crowns are planned. For an accurate quote, a clinical examination and treatment plan are essential.
Aftercare And Maintenance
Good aftercare helps crowns last longer and keeps the gums around them healthy:
- Brush twice daily and clean between teeth with floss or interdental brushes
- Use an alcohol-free mouthwash if recommended by your dentist
- Attend routine check-ups and professional cleanings (commonly twice a year)
- Avoid chewing very hard items such as ice or unpopped kernels
- If you grind your teeth, ask about a night guard to protect the crowns and your natural teeth
Book A Consultation
If you’re considering zirconium crowns, a consultation helps confirm whether they’re the right option for your teeth and bite. Your dentist can explain the expected outcome, number of appointments, and alternative treatments based on your needs.
FAQ
What are the disadvantages of zirconia crowns?
Disadvantages include lower translucency, difficult adjustments, potential opposing-tooth wear, and possible cementation issues.
How long do zirconia crowns last?
Usually 10–15 years; many last 15–20+ with good hygiene and bite.
Why do zirconia crowns fall out?
They fall out from poor fit, cement failure, decay, short tooth prep, or bruxism.
Do teeth decay under crowns?
Yes; decay can occur at crown margins if the seal leaks or hygiene is poor.
What is the best toothpaste for zirconia crowns?
Use a non-abrasive fluoride toothpaste; avoid harsh whitening or charcoal pastes.
Common Oral and Dental Health Mistakes
Common Oral And Dental Health Mistakes
Most dental problems start with everyday habits: rushing your brushing, scrubbing with a hard brush, skipping interdental cleaning, sipping sugary or acidic drinks, and delaying dental check-ups. Gentle brushing for two minutes with fluoride toothpaste, daily flossing, smarter snacking, and regular exams help protect enamel, gums, and breath.
Table of Contents
Tooth Brushing Mistakes
Brushing Too Quickly
Brushing for a few seconds rarely removes plaque along the gumline and between teeth.
Aim for about two minutes, covering every surface: outer, inner, and chewing surfaces, plus the tongue for fresher breath.
Brushing Too Hard Or Using Hard Bristles

Scrubbing aggressively or using a hard-bristled brush can wear enamel and irritate gums.
Use a soft-bristled brush and gentle pressure. If your bristles splay out quickly, you’re likely brushing too hard.
Not Replacing Your Toothbrush Regularly
A worn brush cleans less effectively and can harbor bacteria.
Replace your toothbrush or electric brush head every 3–4 months, or sooner if the bristles are frayed or after illness.
Brushing Right After Acidic Foods Or Drinks
Acidic items like citrus, soda, sports drinks, wine, and sour candies can temporarily soften enamel.
Brushing immediately afterwards may increase enamel wear. Rinse with water first and wait about 30–60 minutes before brushing.
Brushing Before Or After Breakfast
Brushing before breakfast removes overnight plaque and leaves a protective fluoride layer on the teeth.
If you prefer brushing after breakfast, wait about 30 minutes after eating (especially after coffee, juice, or fruit) so enamel isn’t softened by acids.
Ignoring Your Gumline
Plaque tends to collect where teeth meet gums, which can trigger bleeding and inflammation.
Angle your brush slightly toward the gumline and make small, gentle strokes rather than wide scrubbing motions.
Skipping Your Tongue
The tongue can hold bacteria that contribute to bad breath and coating.
Brush your tongue gently or use a tongue scraper once a day.
Flossing And Interdental Cleaning Mistakes
Not Flossing At All
A toothbrush can’t clean between teeth where plaque often hides.
Clean between teeth daily using floss, interdental brushes, or water flossers—choose what you can do consistently.
Flossing Too Hard
Snapping floss down can cut gums and make flossing unpleasant.
Guide floss gently between teeth, curve it into a “C” shape around each tooth, and slide it up and down.
Only Flossing When Food Gets Stuck
Interdental cleaning isn’t just for removing food—it removes plaque that contributes to cavities and gum disease.
Make it a daily habit, even if you don’t feel anything stuck.
Mouthwash Mistakes
Using Mouthwash As A Substitute For Brushing
Mouthwash can support oral hygiene, but it doesn’t remove plaque like brushing and flossing.
Use it as an add-on, not a replacement—especially if you’re prone to gum inflammation or cavities.
Rinsing Right After Brushing With Fluoride Toothpaste
Rinsing immediately after brushing can wash away fluoride, reducing its protective benefit.
Spit out toothpaste after brushing and avoid rinsing for a while so fluoride can stay on the teeth longer.
Overusing Strong Antiseptic Mouthwashes
Frequent use of strong antiseptic rinses can cause dryness or irritation for some people.
Follow the label directions. If your dentist recommends one, it’s often for short-term use.
Diet And Lifestyle Mistakes
Frequent Snacking And Sipping Sugary Drinks
Each snack or sugary drink can start an “acid attack” that weakens enamel.
Try to limit grazing. Drink water between meals and keep sugary or acidic drinks to mealtimes when possible.
Too Many Acidic Foods And Drinks
Acidic choices can soften enamel, especially when consumed often.
Use a straw for acidic drinks, rinse with water after, and avoid brushing right away.
Not Drinking Enough Water
Saliva helps neutralize acids and wash away food particles.
Staying hydrated supports saliva flow and can help reduce dry mouth and bad breath.
Smoking Or Vaping
Tobacco and nicotine products can increase staining, dry mouth, gum disease risk, and slower healing.
Quitting or cutting back can improve gum health and reduce oral health complications over time.
Skipping Dental Visits And Early Warning Signs
Waiting Until Pain Starts
Many dental problems don’t hurt until they’re advanced.
Regular check-ups help catch decay and gum disease early, when treatment is simpler and less costly.
Ignoring Bleeding Gums
Bleeding during brushing or flossing is often a sign of gum inflammation.
If it persists for more than a week or two despite improved cleaning, book a dental visit to assess gum health.
Not Addressing Tooth Sensitivity
Sensitivity can come from enamel wear, exposed roots, cavities, or grinding.
Don’t self-diagnose—use a sensitivity toothpaste and schedule an exam if it continues.
Tooth Whitening And DIY Treatments Mistakes
Overusing Whitening Products
Overuse can increase sensitivity and irritate gums.
Follow the recommended schedule and take breaks if you notice discomfort.
Trying Harsh DIY “Hacks”
Abrasive or acidic DIY methods can damage enamel.
If you want whiter teeth, ask your dentist about safer options and realistic results.
Grinding, Clenching, And Jaw Habits
Ignoring Night Grinding
Grinding can flatten teeth, cause cracks, and lead to jaw soreness or headaches.
If you wake with jaw pain or notice tooth wear, ask about a night guard or other treatment.
Chewing Ice Or Hard Objects
Chewing hard items can chip enamel and crack fillings.
Choose softer snacks and avoid using your teeth as tools.
FAQ
Dental problems and solutions
Common problems: cavities, gum disease, sensitivity; solutions: hygiene, fluoride, dentist treatment.
How often should I brush my teeth?
Twice daily for two minutes, and after sugary meals if possible.
Oral and dental problems
Include cavities, gingivitis, periodontitis, bad breath, erosion, ulcers, and tooth loss.
What are the 5 oral health diseases?
Dental caries, gingivitis, periodontitis, oral cancer, and oral candidiasis are five.
Definition of oral hygiene
Oral hygiene is daily practices that keep teeth and gums clean and healthy.
How to Prevent Gum Recession in Smokers
How To Prevent Gum Recession In Smokers
Gum recession in smokers often develops quietly because smoking reduces blood flow and can hide bleeding. Prevention focuses on gentle brushing, daily interdental cleaning, professional cleanings, and early gum checks. Quitting tobacco is the biggest step: it improves healing and lowers ongoing risk, even if already-receded gums do not grow back.
Table of Contents
Why Smoking Raises The Risk Of Gum Recession
Smoking affects the gums in a few connected ways. Nicotine constricts blood vessels, so less oxygen and fewer nutrients reach gum tissue. That slows repair and makes the gums more vulnerable to ongoing irritation.
Tobacco also changes the mouth’s bacterial balance and weakens immune response. As a result, plaque hardens into tartar more easily, infections become harder to control, and gum disease is more likely to progress.
Many smokers also bleed less during brushing because of reduced circulation. That can mask inflammation and delay diagnosis, which is one reason recession may be noticed late.
Common Causes Of Gum Recession In Smokers

- Plaque and tartar buildup along the gumline (often worse with dry mouth).
- Gum disease (gingivitis and periodontitis) that progresses faster and responds less predictably to treatment.
- Aggressive brushing or a hard-bristled toothbrush, which can wear down the gum margin.
- Grinding or clenching, which can increase stress on the supporting tissues.
- Poorly fitting dental work or bite issues that trap plaque or irritate the gums.
Early Signs You Shouldn’t Ignore
Recession is usually gradual. If you smoke, it’s worth checking your gums regularly in good light.
- Tooth sensitivity to cold, hot, or sweet foods.
- Teeth looking “longer” or roots becoming visible.
- Notches near the gumline or a change in the way the gums hug the tooth.
- Food getting stuck more often between teeth.
- Persistent bad breath or a bad taste that returns quickly after brushing.
- Bleeding, swelling, or tenderness—even if it’s mild or occasional.
A Daily Routine That Protects Your Gums
Brush Gently, Twice A Day
Use a soft-bristled toothbrush and small circular motions at the gumline. Aim for two minutes. Hard scrubbing can make recession worse, especially if the gums are already inflamed.
Clean Between Teeth Every Day
Floss, interdental brushes, or a water flosser can remove plaque where brushes miss. Choose the option you can do consistently; technique matters more than the tool.
Use Mouthwash With A Purpose
An antiseptic mouthwash can reduce bacterial load, while fluoride rinses support enamel. If you have dry mouth, look for alcohol-free options and ask your dentist what fits your situation.
Don’t Skip Tongue Cleaning
A tongue scraper or brushing the tongue can reduce odor-causing bacteria and help overall oral hygiene.
Professional Care That Makes The Biggest Difference

Home care is essential, but it can’t remove tartar once it hardens. Regular professional cleanings help keep gum inflammation under control.
If you smoke, many dentists recommend cleanings and gum checks at least every 6 months, and sometimes more often depending on your gum measurements and tartar buildup.
If early gum disease is found, treatment may include deep cleaning (scaling and root planing), targeted antibacterial care, and a review of your brushing technique.
Quitting Smoking: What Improves And What Doesn’t
Stopping tobacco use is the strongest long-term move for gum health. Circulation and immune response improve over time, which supports healing and makes periodontal treatment more effective.
Quitting does not “regrow” gums that have already receded, but it can slow or stop further damage. If recession has created significant sensitivity or exposed roots, your dentist can discuss options such as bonding, grafting, or desensitizing treatments.
Nutrition That Supports Gum Tissue

Diet won’t replace dental treatment, but it can support gum repair and immune function—especially if smoking has left the tissues irritated.
- Vitamin C: supports collagen formation in gum tissue.
- Vitamin D and calcium: support bone and tooth structure.
- Zinc: supports healing and immune function.
- Magnesium and vitamin K: support mineral balance and normal tissue repair.
If you’re considering supplements, discuss them with a clinician—especially if you take blood thinners, have kidney disease, or are pregnant.
When To See A Dentist Soon
Book an appointment sooner rather than later if you notice sensitivity, visible root surfaces, loose teeth, pus, persistent swelling, or bad breath that doesn’t improve with better cleaning. Early treatment is usually simpler and more predictable.
FAQ
Do receding gums grow back?
No; receding gums don’t regrow naturally, but grafting can restore gum tissue.
What is the best toothpaste for receding gums?
Use low-abrasive fluoride toothpaste; stannous fluoride may reduce gingival inflammation and sensitivity.
Do gums heal after quitting smoking?
Yes; blood flow improves, inflammation decreases, but recession won’t reverse.
If gums recede, will teeth fall out?
Not inevitably; risk rises if periodontal disease progresses and bone loss occurs.
How can smokers strengthen their gums?
Quit smoking, brush twice daily, floss, get cleanings, and treat gum disease promptly.
Changes in Dental Structure by Age
Changes In Dental Structure By Age
Teeth change throughout life—from the eruption of baby teeth to enamel wear, gum recession, and a higher risk of tooth loss later on. Knowing what’s typical at each age helps you spot problems early, plan checkups, and adjust daily care. With consistent hygiene, smart nutrition, and timely dental visits, most age-related issues can be prevented or managed.
Dental health isn’t static. As the jaw grows, teeth erupt, and tissues respond to diet, hormones, and daily use, the structure and function of the mouth shifts in predictable ways.
Understanding these changes makes it easier to protect your smile at every stage—whether you’re caring for a teething baby, supporting a teenager with braces, or managing sensitivity and gum health later in life.
Table of Contents
Tooth Development In Infancy (0–3 Years)

What Typically Changes
- Primary (baby) teeth usually begin erupting around 6 months, often starting with the lower front teeth.
- By about age 3, most children have 20 primary teeth, which support chewing, speech, and jaw development.
- Teething may cause drooling and irritability. If a child has a significant fever or seems unwell, it’s best to consult a pediatrician.
Care Tips That Matter
- Clean gums with a soft, damp cloth; once teeth appear, use a small, soft toothbrush.
- Avoid putting babies to bed with bottles containing milk or sugary drinks to reduce early cavities.
- Schedule the first dental visit by age 1, or within six months of the first tooth erupting.
Tooth Transition And Permanent Teeth Formation In Children (4–12 Years)
What Typically Changes
- Around age 6, baby teeth begin to loosen and fall out as permanent teeth erupt.
- The first permanent molars (often called “6‑year molars”) typically appear behind baby teeth and do not replace any tooth.
- Jaw growth continues, which influences spacing, crowding, and bite alignment.
Care Tips That Matter
- Help children brush twice daily and clean between teeth as contact points tighten.
- Watch for early signs of crowding or an uneven bite; many orthodontic concerns are easier to address when caught early.
- Keep checkups regular to detect cavities quickly, especially as new permanent molars come in.
Dental Health During Adolescence (13–18 Years)

What Typically Changes
- Hormonal changes can make gums more reactive, increasing the likelihood of bleeding or inflammation when plaque builds up.
- Most permanent teeth are in place, so orthodontic treatment is often timed for this period.
- Diet choices and busy schedules can raise cavity risk, especially with frequent sugary or acidic snacks and drinks.
Care Tips That Matter
- Focus on thorough brushing along the gumline and around orthodontic appliances if present.
- Encourage consistent routines—morning and night brushing is non‑negotiable during these years.
- Limit frequent sipping of acidic beverages; rinse with water after snacks when brushing isn’t possible.
Changes In Dental Structure In Adulthood (19–40 Years)
What Typically Changes
- Daily chewing and lifestyle factors can gradually wear enamel, especially with acidic diets or reflux.
- Stress-related clenching or grinding may cause flattening of tooth surfaces, chips, or jaw discomfort.
- Wisdom teeth may erupt or create crowding and inflammation in some adults.
Care Tips That Matter
- Book routine cleanings and exams to catch early decay, gum inflammation, and bite issues.
- If you grind your teeth, ask about a night guard to protect enamel and reduce strain on the jaw.
- Use protective gear for contact sports and address sensitivity early rather than avoiding one side when chewing.
Dental Problems And Precautions In Middle Age (41–60 Years)

What Typically Changes
- Gum recession becomes more common, exposing root surfaces that are more vulnerable to decay and sensitivity.
- Long-term plaque buildup can progress to periodontal disease, which is a leading contributor to tooth loss.
- Certain medications and hormonal changes may contribute to dry mouth, increasing cavity risk.
Care Tips That Matter
- Prioritize professional periodontal checks; gum issues are easier to stabilize when treated early.
- Choose low‑abrasive toothpaste and a soft brush if enamel feels thinner or sensitivity increases.
- If teeth are missing, discuss replacement options such as bridges or implants to support chewing and prevent shifting.
Tooth Loss And Denture Use In Older Age (60+ Years)
What Typically Changes
- The risk of root decay rises as gums recede and dry mouth becomes more common.
- Tooth loss can affect nutrition, speech, and confidence, especially when chewing becomes less efficient.
- Dentures, bridges, and implants may be needed to restore function and comfort.
Care Tips That Matter
- Clean dentures daily and remove them as advised to reduce irritation and infection risk.
- Maintain dental visits even with dentures—oral cancer screenings and gum checks still matter.
- Support oral health with balanced nutrition and hydration, especially if dry mouth is an issue.
How Often To See A Dentist
Most people benefit from regular exams and professional cleanings. Your dentist may recommend more frequent visits if you have gum disease, dry mouth, a history of cavities, or ongoing orthodontic treatment.
Book An Appointment
If you’d like tailored advice on cosmetic dentistry, dental crowns, implants, or general dentistry, contact our clinic to schedule an appointment.
FAQ
Does tooth structure change with age?
Yes; enamel wears, teeth darken, and dentin thickens as you age.
Which vitamins help teeth grow?
No vitamins make adult teeth grow; vitamin D and A support developing teeth.
At what age do teeth start to decay?
Decay can start as soon as teeth erupt, even in early childhood.
Do your teeth become more crooked as you age?
Yes; teeth often shift and crowd gradually with age, especially without retainers.
Oral Lesions in Autoimmune Diseases
Oral Lesions in Autoimmune Diseases
Autoimmune diseases can trigger mouth ulcers, soreness, and persistent dryness when immune activity inflames the oral tissues or damages salivary glands. The most common causes include Behçet’s disease, lupus, Sjögren’s syndrome, and pemphigus vulgaris. Management usually combines treating the underlying condition with local pain control and careful oral care.
Autoimmune diseases are long-term conditions in which the immune system mistakenly targets the body’s own tissues. When the mouth is involved, symptoms can feel disproportionally disruptive—pain can make eating, speaking, and toothbrushing difficult.
Oral lesions are not always caused by autoimmune disease, but recurring or unexplained problems in the mouth can be an early clue. A dentist or physician may use these signs, together with other symptoms, to guide testing and diagnosis.
Table of Contents
What Is An Autoimmune Disease?
In a healthy immune system, immune cells identify and eliminate harmful threats such as bacteria and viruses. In autoimmune disease, that defense system misidentifies normal cells as “foreign” and creates inflammation that can damage organs and tissues.
Many autoimmune conditions can affect oral health directly (through inflammation of the oral mucosa) or indirectly (through dry mouth, medication effects, or systemic flare-ups).
Common Oral Symptoms
Oral symptoms may involve the oral mucosa, lips, tongue, gums, and salivary glands. People often report one or more of the following:
- Painful, recurring mouth ulcers (aphthae)
- Dry mouth (xerostomia) and thick or foamy saliva
- Gum inflammation, bleeding, or swelling
- Burning or soreness of the tongue
- Changes in taste
- Cracked, dry lips or corners of the mouth
Because these symptoms overlap with common issues such as stress, vitamin deficiencies, infections, and trauma, patterns matter. Ulcers that recur frequently, last longer than expected, or appear with other systemic symptoms deserve a clinical assessment.
Autoimmune Conditions Often Linked To Oral Lesions
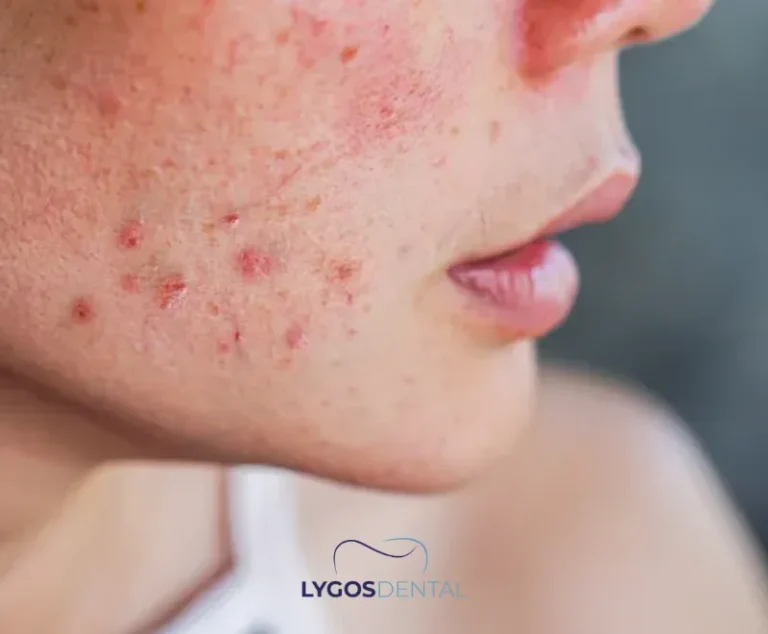
Behçet’s Disease
Behçet’s disease is a multisystem inflammatory condition in which recurrent oral ulcers are a hallmark feature. The ulcers are typically painful, may be multiple at once, and often return in cycles.
Lesions can occur anywhere in the mouth, including the lips, cheeks, tongue, and palate. When oral ulcers are deep and persistent—especially alongside genital ulcers, eye symptoms, or skin lesions—Behçet’s disease becomes an important consideration.
Systemic Lupus Erythematosus (Lupus)
Lupus is a systemic autoimmune disease that can involve skin, joints, kidneys, blood, and the nervous system. Oral ulcers are common and may occur during periods of higher disease activity.
Classic lupus mouth ulcers often appear on the palate and can be red or white. They are sometimes painless, which means they may go unnoticed unless the mouth is examined carefully.
Sjögren’s Syndrome
Sjögren’s syndrome affects the salivary and tear glands, leading to dry mouth and dry eyes. Reduced saliva changes the mouth’s natural protection against acids and microbes.
Dry mouth increases the risk of cavities, gum disease, oral yeast infections, and traumatic irritation from speaking, chewing, or dentures. Some people also notice tongue fissures, burning sensations, and difficulty swallowing dry foods.
Pemphigus Vulgaris
Pemphigus vulgaris is an autoimmune blistering disease. In many patients, the first signs appear inside the mouth as fragile blisters that rupture quickly.
The result is widespread, painful erosions that can make eating and oral hygiene challenging. Prompt diagnosis and specialist treatment are important because symptoms can progress beyond the mouth.
How Lupus, Behçet’s, And Sjögren’s Affect The Mouth

These conditions can look similar at first glance, but their patterns help differentiate them in clinic.
In lupus, ulcers often involve the palate and may be painless. In Behçet’s disease, ulcers tend to be deeper, more painful, and strongly recurrent.
In Sjögren’s syndrome, dryness drives many of the problems—irritation, fissures, higher cavity risk, and recurrent infections—rather than a single “ulcer type”.
Treatment Options
Treatment is tailored to the underlying diagnosis, the severity of symptoms, and how often lesions recur. The main goals are to reduce pain, speed healing, and prevent complications such as infection or tooth decay.
Systemic Treatment (Prescribed By A Specialist)
When oral lesions reflect active autoimmune disease, systemic therapy may be needed to control inflammation. Depending on the condition, clinicians may use corticosteroids, immunosuppressive medicines, or targeted biologic therapies.
Local Treatment And Supportive Care
Local care focuses on comfort and protecting the oral tissues. Options may include topical corticosteroid gels, antiseptic mouth rinses, and short-term anesthetic products.
For Sjögren’s-related dryness, saliva substitutes, moisturizing sprays, and strategies to stimulate saliva can help reduce irritation and lower cavity risk.
Self-Care And Prevention
Simple changes often reduce flare-ups and make lesions less painful. Many patients do better when they avoid spicy or acidic foods during active sores and keep up with gentle, consistent oral hygiene.
If you smoke, stopping can improve healing and reduce irritation. Stress management can also help, as stress is a common trigger for recurrent mouth ulcers in general.
Are Oral Lesions Permanent?
In many autoimmune conditions, oral lesions come and go in flares rather than remaining permanently. Behçet’s disease is well known for recurrent oral ulcers, while lupus mouth ulcers often correlate with disease activity.
In Sjögren’s syndrome, the dryness can be long term, which means the downstream risks—cavities, gum disease, and chronic irritation—may persist without ongoing prevention and dental follow-up.
When To Seek Medical Or Dental Care
Seek evaluation if mouth ulcers recur frequently, last longer than two weeks, or are accompanied by fever, weight loss, rashes, joint pain, eye symptoms, or genital ulcers.
Urgent care is appropriate if you cannot drink enough fluids, pain is severe, or there are signs of infection such as spreading redness, pus, or a high fever.
FAQ
Which autoimmune disease causes mouth lesions?
Behçet’s, lupus, pemphigus, and oral lichen planus can cause mouth lesions.
Which autoimmune disease causes extreme fatigue?
Lupus, rheumatoid arthritis, Sjögren’s, and autoimmune thyroid disease often cause extreme fatigue.
What is the best diet to reverse an autoimmune disease?
No diet reliably reverses autoimmune disease; Mediterranean-style diets can reduce inflammation and symptoms.
How can I get rid of autoimmune mouth sores?
See your clinician; treat the disease, use topical steroids, and avoid triggering foods.
Which autoimmune disease is the most difficult to diagnose?
None is universally hardest; lupus and vasculitis are often difficult due to variability.
Does Tartar Cleaning Damage Tooth Enamel?
Does Tartar Cleaning Damage Tooth Enamel?
Professional tartar cleaning (also called scaling) does not damage tooth enamel when it’s performed by a trained dental professional. The instruments are designed to lift hardened deposits from the tooth surface and along the gumline. Temporary sensitivity can happen after cleaning, but it’s usually caused by exposed dentin or irritated gums—not enamel loss.
Table of Contents
What Tartar Is
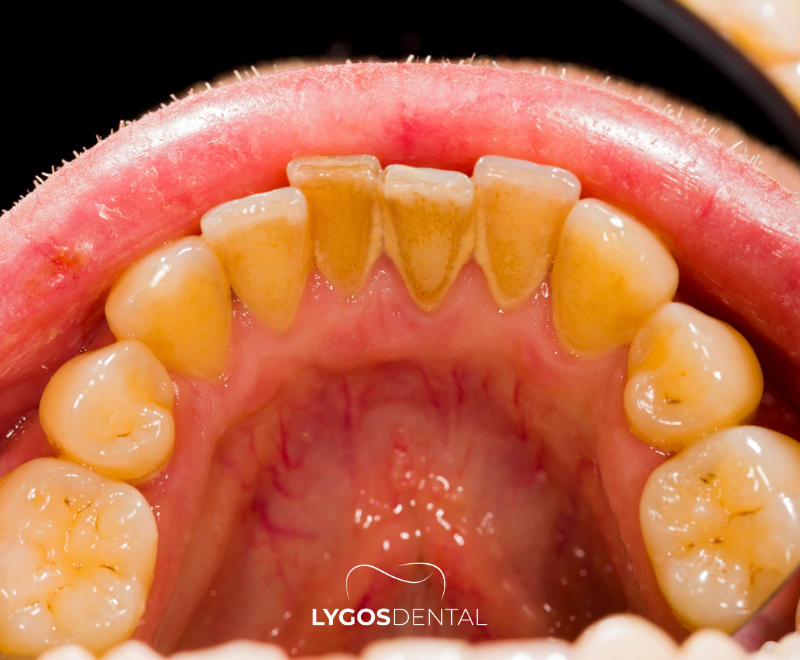
Tartar (calculus) is plaque that has hardened after minerals in saliva bind to it. Unlike soft plaque, tartar cannot be removed fully with brushing alone once it has formed.
It tends to build up near the gumline, between teeth, and behind the lower front teeth—areas that are harder to clean consistently.
Why Dentists Remove Tartar
Tartar traps bacteria against the teeth and gums. Over time, that increases the risk of gum inflammation and can contribute to periodontal (gum) disease.
Removing tartar helps reduce:
- Gum inflammation (gingivitis)
- Bleeding gums and gum recession
- Persistent bad breath
- Progression toward periodontitis and tooth loss
- Visible staining and rough tooth surfaces
Does Tartar Cleaning Harm Enamel?
No—routine tartar removal does not “strip” enamel when it is done properly. Dental professionals use hand scalers and/or ultrasonic scalers to break up and lift calculus from the tooth surface.
These tools are used with controlled pressure and angles, targeting deposits rather than shaving tooth structure. After cleaning, teeth can feel smoother because the hard buildup is gone, not because enamel has been removed.
If you already have enamel wear, exposed roots, or gum recession, you may notice more sensitivity during or after the visit. That sensitivity is related to exposed dentin or root surfaces (roots don’t have enamel), not new enamel damage from the cleaning.
Is Tooth Sensitivity Normal After Tartar Cleaning?

Mild sensitivity is common for a short time after scaling. It typically feels like a quick “zing” with cold air, cold drinks, or brushing.
Why Sensitivity Can Happen
Common reasons include:
- Tartar previously covering sensitive areas near the gumline
- Temporary gum irritation after instruments are used around inflamed tissue
- Existing gum recession exposing dentin or root surfaces
How Long It Lasts And When To Call Your Dentist
Most people feel better within a few days. If discomfort is severe, lasts longer than a week, or is accompanied by swelling, persistent bleeding, or pain when biting, contact your dentist to rule out cavities, cracked teeth, or gum infection.
How Often Should You Get Tartar Cleaning?

There isn’t one perfect schedule for everyone. Many patients do well with a check-up and cleaning about every six months, but the ideal interval depends on your risk factors and oral health history.
Your dentist may recommend more frequent cleanings if you:
- Smoke or use tobacco
- Have a history of gum disease
- Have diabetes or other conditions that affect gum health
- Wear orthodontic appliances or have many restorations that trap plaque
- Build tartar quickly due to saliva composition or genetics
Aftercare Tips To Protect Teeth And Gums
To keep results longer and reduce sensitivity:
- Brush twice daily with a soft-bristled toothbrush and fluoride toothpaste.
- Clean between teeth daily with floss or interdental brushes.
- For 24–48 hours, avoid very cold, very hot, or acidic foods if you feel sensitive.
- If your dentist recommends it, use a desensitizing toothpaste for a week or two.
- Keep regular dental visits so tartar doesn’t have time to harden again.
FAQ
Does tartar removal damage tooth enamel?
No; professional tartar removal doesn’t damage enamel when performed correctly.
Can I restore my tooth enamel?
No; enamel can’t regrow, but fluoride can remineralize early enamel weakening.
Why do dentists recommend deep cleaning?
Because it removes buildup below gums, reduces pockets, and treats periodontal disease.
How can tartar be removed without damaging tooth enamel?
By professional scaling with proper instruments and technique, avoiding DIY scraping.
What happens if tartar is not removed?
Tartar causes gum disease, bad breath, recession, and bone loss, increasing tooth-loss risk.
Dental Health Problems After Menopause
Dental Health Problems After Menopause
After menopause, lower estrogen can reduce saliva, make gums more sensitive, and contribute to bone loss in the jaw. Many women notice dry mouth, gum bleeding, burning sensations, or more cavities. With consistent home care, targeted products for dryness, and routine dental checkups, these changes are often manageable and preventable.
Table of Contents
Why Menopause Affects Oral Health
Estrogen helps maintain healthy oral tissues and supports normal bone turnover. When estrogen levels fall during menopause, the mouth may feel drier and soft tissues can become thinner or more reactive. At the same time, age-related changes and reduced bone density can affect the jaw, which supports the teeth.
Common Dental And Oral Problems

Gum Disease (Gingivitis And Periodontitis)
Hormonal shifts can make gums more prone to inflammation and tenderness. You might notice swelling, bleeding during brushing, bad breath, or gum recession. Untreated periodontitis can damage the bone around teeth and raise the risk of tooth loss.
Dry Mouth (Xerostomia)
A drop in saliva flow is common and can change how the mouth feels day to day. Saliva protects teeth by washing away food debris and buffering acids. When saliva is low, cavities, plaque buildup, and oral infections become more likely.
Burning Mouth Syndrome
Some women develop a persistent burning, tingling, or scalded feeling on the tongue, lips, or palate. Symptoms can fluctuate and may come with altered taste or a dry sensation. Because triggers vary, it’s worth discussing symptoms with a dentist or physician to rule out other causes.
Tooth Decay
Dry mouth and changes in oral bacteria can increase the chance of cavities. Existing fillings may also start to leak over time, which can hide decay around edges. Regular exams and fluoride support are especially helpful during this stage.
Loose Teeth And Tooth Loss
Bone density changes after menopause can affect the jawbone as well as the spine and hips. If periodontal disease is present, bone loss can progress faster and weaken tooth support. Early gum treatment and bone health monitoring help reduce long-term risk.
Dry Mouth And Menopause
Dry mouth can affect speaking, swallowing, sleep quality, and comfort while eating. It may also lead to mouth sores, cracked lips, bad breath, or a higher rate of cavities. If dryness is persistent, it’s important to treat it as a medical and dental issue rather than a minor annoyance.
Practical steps that often help:
- Sip water regularly and keep water nearby at night.
- Chew sugar-free gum or use xylitol lozenges to stimulate saliva (if appropriate for you).
- Limit alcohol and caffeine if they worsen dryness.
- Use saliva substitutes, moisturizing gels, or dry-mouth rinses.
- Ask your dentist about high-fluoride toothpaste or in-office fluoride treatments.
If you also take medications that can reduce saliva, your dentist can suggest a tailored plan. Seek prompt care if you develop frequent cavities, oral thrush, or painful cracking at the corners of the mouth.
Osteoporosis, Jawbone Changes, And Tooth Stability

Postmenopausal osteoporosis can reduce overall bone strength, and the jawbone is not exempt. Lower jawbone density may contribute to loose teeth and can influence planning for implants or dentures. Coordination between your dentist and physician is useful when bone density is changing or treatment is underway.
Supportive habits for bone and oral health:
- Follow your clinician’s guidance on calcium and vitamin D intake.
- Do regular weight-bearing and strength-based exercise if medically appropriate.
- Keep periodontal disease under control with professional cleanings.
- Ask whether a bone density test is right for you, especially if you have risk factors.
Gum Care During And After Menopause
Gums may feel more sensitive, and brushing that once felt fine can suddenly cause bleeding. Bleeding is a sign of inflammation, not something to ignore. A consistent routine usually improves symptoms within a few weeks, but persistent bleeding should be checked.
A gum-friendly daily routine:
- Brush twice daily with a soft-bristled brush and gentle technique.
- Clean between teeth daily with floss or interdental brushes.
- Use an alcohol-free mouthwash if your mouth is dry.
- Replace your toothbrush every 3 months, or sooner if bristles fray.
Professional cleanings and periodontal assessments remain important every six months, or more often if advised. If you smoke or have diabetes, ask your dental team for extra prevention strategies.
How Menopause-Related Medications Can Affect Teeth

Hormone Therapy
Hormone therapy can improve some menopause symptoms, and its oral effects vary from person to person. If you notice new dry mouth or gum sensitivity after starting or changing therapy, note the timing and share it with your clinician. Avoid stopping any prescribed medication without medical advice.
Antidepressants And Anti-Anxiety Medications
Several common medications can reduce saliva flow and worsen dry mouth. If you rely on these medicines, preventive dental care becomes even more important. Your dentist may recommend fluoride support and more frequent checkups.
Osteoporosis Medications (Including Bisphosphonates)
Antiresorptive medicines used for osteoporosis are important for fracture prevention. In rare cases, they are associated with a jaw complication called medication-related osteonecrosis of the jaw, especially after invasive dental procedures. Always tell your dentist if you take these medicines, and ask your prescriber and dentist for guidance before extractions or implant surgery.
When To See A Dentist
Book a dental visit if you notice ongoing gum bleeding, persistent mouth dryness, or a burning sensation that lasts more than two weeks. Tooth pain, loose teeth, swelling, or sores that don’t heal should be assessed promptly. Early treatment is usually simpler and helps prevent bigger problems.
FAQ
Why do dental and gum problems increase after menopause?
Hormonal estrogen decline reduces saliva and bone support, increasing inflammation and dryness.
Does menopause increase the risk of gum disease?
Yes; menopause-related estrogen loss increases periodontal inflammation and bone loss risk.
Is tooth sensitivity normal during menopause?
Yes; dryness and gum recession can make teeth temporarily more sensitive.
How often should dental checkups be performed after menopause?
Every 6 months, or every 3–4 months if gum disease risk is high.
Is Whitening Teeth with Vinegar Harmful?
Is Whitening Teeth With Vinegar Harmful?
Yes, whitening teeth with vinegar can be harmful because vinegar is acidic and can soften and erode enamel. Even if teeth look slightly brighter at first, repeated exposure may increase sensitivity, irritate gums, and make teeth more prone to staining and cavities. Safer whitening methods exist, including dentist-approved products and professional treatments.
Table of Contents
Why People Try Vinegar For Teeth Whitening

Interest in a brighter smile has made “natural” whitening hacks popular, and vinegar is one of the most shared. Most people use apple cider vinegar, but white vinegar is also mentioned in online recipes.
The idea is simple: acid can loosen some surface stains and plaque, so a quick rinse may make teeth look cleaner. Some people apply vinegar with cotton, dilute it in water as a mouth rinse, or mix it with baking soda and brush.
How Vinegar Affects Tooth Enamel
Vinegar has a low pH, which means it is acidic. When teeth are exposed to acids, enamel can temporarily soften. If acid exposure is frequent or prolonged, enamel can wear away over time.
Enamel does not grow back. Once it thins, the underlying dentin becomes more exposed, which can make teeth look more yellow, feel more sensitive, and become easier to damage.
Does Vinegar Actually Whiten Teeth?
Vinegar may reduce some extrinsic (surface) staining, especially from foods and drinks. Any visible change is usually minor and short-lived.
The trade-off matters. A method that “whitens” by weakening enamel can backfire, because thinner enamel can reveal yellow dentin and increase new staining. A safe whitening approach should improve colour without sacrificing tooth structure.
Main Risks Of Whitening Teeth With Vinegar

Enamel erosion: Acid can gradually wear down enamel, leading to permanent changes in tooth strength and appearance.
Tooth sensitivity: As enamel thins, teeth may react more strongly to cold, hot, sweet, or acidic foods and drinks.
Gum irritation: Vinegar can sting and inflame gum tissue, especially if gums are already sensitive or there are small cuts.
Higher cavity risk: Weaker enamel offers less protection against decay. If brushing becomes painful due to sensitivity, plaque can build up faster.
Uneven results: Stain removal can be patchy, and erosion can create a dull or translucent look at the edges of teeth.
Common Mistakes That Make The Damage Worse
Using vinegar daily or for long rinses. Even “diluted” vinegar is still acidic, and repeated exposure increases risk.
Brushing immediately after using vinegar. Acid can soften enamel, and brushing straight away may increase wear. If you’ve had something acidic, rinse with water and wait before brushing.
Combining vinegar with baking soda. The mix can feel “cleaning,” but it can increase abrasion and is not a controlled whitening system.
Copying social media recipes. Whitening is not one-size-fits-all; existing sensitivity, restorations, and gum health change what is safe.
Safer Alternatives To Vinegar For A Whiter Smile

Dentist-Approved At-Home Options
Over-the-counter whitening products can help when used as directed. Look for products designed for teeth (not DIY acids), and follow label instructions closely.
Whitening toothpastes can polish surface stains and may be a good starting point if you want mild improvement without bleaching.
Professional Whitening
If you want a noticeable colour change, professional whitening is the safest route. Dentists can check for cavities, gum inflammation, and enamel wear before whitening, then choose a method that fits your teeth.
In-office whitening and dentist-supervised take-home trays use controlled peroxide-based gels. This approach is more predictable and easier to adjust if sensitivity occurs.
Habits That Help Teeth Look Brighter Naturally
A lot of “yellowing” comes from surface staining. Daily brushing with fluoride toothpaste, flossing, and regular cleanings often make teeth look noticeably fresher.
If tea, coffee, red wine, or smoking is part of your routine, reducing frequency and rinsing with water afterward can help slow staining.
When To Talk To A Dentist First
If you have sensitivity, visible enamel wear, gum recession, or frequent cavities, skip DIY whitening. The same goes for people with crowns, veneers, or bonding on front teeth, because these restorations will not whiten in the same way as natural enamel.
A dentist can identify whether the colour change is surface staining, enamel thinning, or an internal issue. That diagnosis determines the safest way to improve your smile.
FAQ
Can I whiten my teeth with vinegar?
No; vinegar is acidic and can erode enamel, increasing sensitivity and decay risk.
What is the healthiest way to whiten your teeth?
Dentist-supervised peroxide whitening with custom trays is healthiest and least damaging.
Can white vinegar damage your teeth?
Yes; white vinegar can erode enamel, worsen sensitivity, and irritate gums.
What is the best natural teeth whitener?
None truly whitens naturally; best is professional cleaning plus fluoride brushing to prevent stains.
What happens if I brush my teeth with apple cider vinegar?
It can strip enamel, cause burning, increase sensitivity, and raise cavity risk.
When Do Permanent Teeth Erupt in Children?
When Do Permanent Teeth Erupt In Children?
Most children start getting permanent (adult) teeth at about age 6, often with the first molars and the lower front teeth. Eruption continues through the early teen years, with most permanent teeth in place by 12–13. Third molars (wisdom teeth) may appear later, typically between 17–25.
Table of Contents
Typical Timeline For Losing Baby Teeth
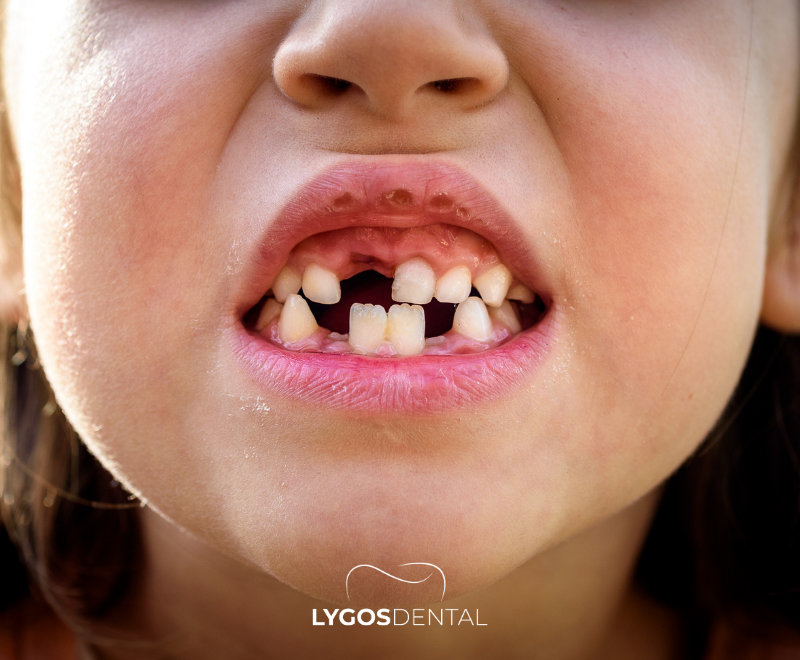
Baby teeth help with chewing, speech, and jaw growth, and they hold space for the adult teeth that follow. Most children start losing baby teeth around age 6, though it can happen a little earlier or later. This period is called the mixed dentition stage because baby teeth and permanent teeth are both present.
When Permanent Teeth Start Coming In
Permanent teeth usually begin erupting between ages 5 and 7, with age 6 as the most common starting point. The first teeth you may notice are the first permanent molars (often called the “6-year molars”) and the lower central incisors. Timing varies by child and can be influenced by genetics, overall growth, and oral health.
Order Of Permanent Tooth Eruption

Children don’t all follow the exact same schedule, but the sequence is fairly consistent. Below are typical age ranges for eruption (upper and lower jaws can differ):
- First permanent molars (6-year molars): 6–7 years
- Lower central incisors: 6–7 years
- Upper central incisors: 7–8 years
- Lateral incisors: 7–9 years
- First premolars (bicuspids): 9–12 years
- Canines (cuspids): 9–12 years
- Second premolars: 10–12 years
- Second molars: 11–13 years
- Third molars (wisdom teeth): 17–25 years (varies widely)
If the order looks different in your child, it doesn’t automatically mean there’s a problem. Dentists focus on patterns such as crowding, teeth that are “stuck,” or large delays between teeth on the right and left sides.
What Are 6-Year Molars And Why Do They Matter?
The 6-year molars are the first permanent molars to erupt, and they do not replace any baby tooth. They come in behind the baby molars, so it’s easy to mistake them for “new baby teeth.” Because they arrive early and have deep grooves, they’re at higher risk for cavities if brushing is inconsistent.
Ask your dentist whether fissure sealants are appropriate once these molars are fully erupted. Sealants can help protect the biting surfaces from decay, especially in children who are prone to cavities.
What If Permanent Teeth Erupt Early Or Late?
A few months’ difference is usually normal. It’s worth booking a dental check if your child is 7–8 and hasn’t started losing any baby teeth, or if a permanent tooth is visible but can’t come through the gum properly.
Common reasons for delayed eruption include:
- Limited space or crowding in the jaw
- Baby tooth roots not resorbing on time
- Extra (supernumerary) teeth blocking eruption
- Teeth developing in an unusual position
- Less commonly, medical or hormonal factors affecting growth
Your dentist may recommend an exam and X-rays to confirm that the adult teeth are present and to check their position. In some cases, removing a retained baby tooth can help the permanent tooth erupt normally.
How To Protect Newly Erupted Permanent Teeth
Newly erupted teeth can be harder for children to clean, especially the back molars. Strong daily habits during the mixed dentition years make a long-term difference.
- Brush twice a day with fluoride toothpaste (a parent should supervise until the child can brush effectively).
- Floss daily once teeth touch, especially around molars.
- Limit frequent sugary snacks and drinks between meals.
- Keep up routine dental visits so eruption, spacing, and bite development can be monitored.
- Consider fluoride varnish and fissure sealants if recommended by your dentist.
FAQ
When do permanent teeth usually start coming in?
Around age 6, first molars and lower incisors usually erupt.
Are there teeth that come in at age 7?
Yes; permanent lateral incisors commonly erupt around age 7–8.
Which vitamins help teeth grow?
No vitamins grow adult teeth; vitamin D and A support tooth development.
Differences Between Implants and Dental Bridges
Differences Between Implants And Dental Bridges
Dental implants replace a missing tooth with a titanium post placed in the jawbone and a crown on top, while a dental bridge fills the gap by anchoring a false tooth to the neighboring teeth. Implants usually last longer and help preserve bone, but they take more time and cost more upfront than bridges.
Table of Contents
What Are Dental Implants And Dental Bridges?
A dental implant is a screw-shaped post made from titanium or another biocompatible material that is placed into the jawbone to act like a tooth root. After healing, a crown (often porcelain or zirconia) is attached to restore the look and function of a natural tooth.
A dental bridge is a fixed prosthesis that replaces one or more missing teeth by using the teeth next to the gap for support. Those neighboring teeth are shaped to hold crowns, and the replacement tooth (pontic) is connected between them.
How Each Treatment Is Done
Implant Treatment Steps
Implant treatment involves a minor surgical procedure to place the implant into the jawbone. The implant then needs time to bond with the bone (osseointegration), which commonly takes several months. Once the site is stable, the dentist fits the final crown onto the implant.
Dental Bridge Treatment Steps
For a dental bridge, the dentist prepares the teeth on either side of the missing tooth and takes impressions or digital scans. A dental lab fabricates the bridge, and the dentist bonds it in place at a follow-up visit. Because there is no implant surgery, treatment is typically completed faster.
Key Differences At A Glance

- Support: Implants are anchored in the jawbone; bridges rely on the neighboring teeth.
- Impact on nearby teeth: Implants usually do not require altering adjacent teeth; bridges typically require shaping them.
- Bone support: Implants can help slow jawbone shrinkage in the missing-tooth area; bridges do not replace the root, so bone changes may continue.
- Longevity: Implants often last longer with good oral hygiene; bridges commonly need replacement over time.
- Treatment time: Implants take longer because healing is required; bridges are usually finished within a shorter period.
Advantages And Disadvantages
Advantages Of Implants
- Help preserve jawbone in the missing-tooth area.
- Do not typically require reducing neighboring teeth.
- Strong, stable chewing function.
- Natural-looking results when properly planned.
Possible Downsides Of Implants
- Require a surgical procedure and healing time.
- Not ideal for everyone (for example, limited bone volume or certain medical risks).
- Higher upfront cost compared with many bridge options.
Advantages Of Dental Bridges
- No implant surgery is needed.
- Faster path to a fixed tooth replacement in many cases.
- Often lower upfront cost.
Possible Downsides Of Dental Bridges
- Neighboring teeth usually need to be shaped, which can affect otherwise healthy tooth structure.
- Do not replace the tooth root, so bone changes may continue under the missing-tooth area.
- May need replacement after years of wear, decay, or gum changes.
Treatment Time And Recovery
With implants, the overall timeline depends on healing and bone integration, so treatment may take several months from start to final crown. Mild swelling or discomfort can occur after placement, and following aftercare instructions helps reduce complications.
With bridges, most patients return to normal routines quickly because there is no surgical site to heal. Some temporary sensitivity can happen after tooth preparation, especially if the prepared teeth were already sensitive.
Costs And Long-Term Value

Implants are usually more expensive upfront because they involve surgical placement, components, and a longer clinical process. Bridges can be more economical at the start, particularly when multiple adjacent teeth are being replaced.
Over the long term, value depends on maintenance, gum health, bite forces, and whether the restoration needs to be replaced. A dentist can explain expected lifespan and maintenance costs for your specific case.
Which Option May Be Right For You?
Implants may be preferred when you want to avoid involving the neighboring teeth and you have enough bone support for predictable placement. Bridges may be considered when you need a quicker fixed option, when implant surgery is not suitable, or when adjacent teeth already need crowns.
The best choice depends on medical history, smoking habits, bone quality, gum health, and your budget. A clinical exam and imaging are essential before deciding.
Care Tips To Protect Your Restoration
Brush twice daily with a soft toothbrush and use interdental cleaning (floss, floss threaders, or interdental brushes) as advised by your dentist. Professional cleanings and routine check-ups help detect early issues such as gum inflammation, bite changes, or decay around bridge margins.
If you grind your teeth, ask about a night guard. Avoid using your teeth as tools and be cautious with very hard foods, especially during the first weeks after treatment.
FAQ
Is a dental implant better than a bridge?
Often yes; implants spare adjacent teeth and bone, but bridges can be suitable.
Which is more expensive, a bridge or an implant?
Usually an implant costs more upfront than a bridge.
Do the teeth under a bridge decay?
Yes; abutment teeth can decay at the margins if hygiene is poor.
What is the 2-2-2 rule in dentistry?
Brush twice daily for two minutes, and visit a dentist twice yearly.
What can I do instead of a bridge?
Consider an implant, removable partial denture, resin-bonded bridge, or orthodontic space closure.
