Cracked Tooth Syndrome | LYGOS DENTAL
Cracked Tooth Syndrome
Cracked tooth syndrome is a small fracture in a tooth that can trigger sharp pain when you bite, especially on release, along with hot/cold sensitivity. Cracks are often hard to spot on X-rays, so diagnosis relies on a careful dental exam. Treatment ranges from bonding or crowns to root canal therapy, depending on depth.
Table of Contents
What Cracked Tooth Syndrome Is
Cracked tooth syndrome refers to a crack in the enamel and/or dentin that causes pain or sensitivity but may not be visible to the naked eye. Because the crack can open slightly under pressure, you may feel a sharp, fleeting pain while chewing and then feel fine once the pressure is released.
People often struggle to identify which tooth is responsible, and the symptoms can come and go. Early assessment matters because a small crack can deepen over time and reach the tooth’s nerve (pulp), making treatment more complex.
Common Causes Of A Cracked Tooth

Cracks can develop from repeated stress on the tooth or from a single traumatic event. Common triggers include:
- Teeth grinding or clenching (bruxism): Night-time clenching can create microcracks that slowly widen.
- Biting hard foods or objects: Ice, hard candy, unpopped popcorn kernels, and nut shells can overload enamel.
- Large fillings or restorations: Teeth with extensive restorations may be weaker and more prone to cracking.
- Trauma or impact: A blow to the face or a sports injury can cause a crack that becomes symptomatic later.
- Sudden temperature changes: Very hot then very cold foods/drinks may stress enamel, especially when a tooth is already weakened.
- Age and normal wear: Cracks are reported more often in adults, as enamel naturally wears and teeth accumulate stress over time.
Symptoms Of Cracked Tooth Syndrome
Symptoms can be intermittent, which is why this condition is sometimes missed at first. The most common signs include:
- Sharp pain when chewing — Often felt when you bite down or as you release pressure.
- Sensitivity to hot or cold — The tooth may twinge with temperature changes.
- Sweet sensitivity — Sugary foods can trigger a quick sting.
- Pain that’s hard to localize — Discomfort may feel like it’s coming from a general area rather than one specific tooth.
- Pressure discomfort — As the crack progresses, the tooth may feel “off” when biting.
How Dentists Diagnose A Cracked Tooth
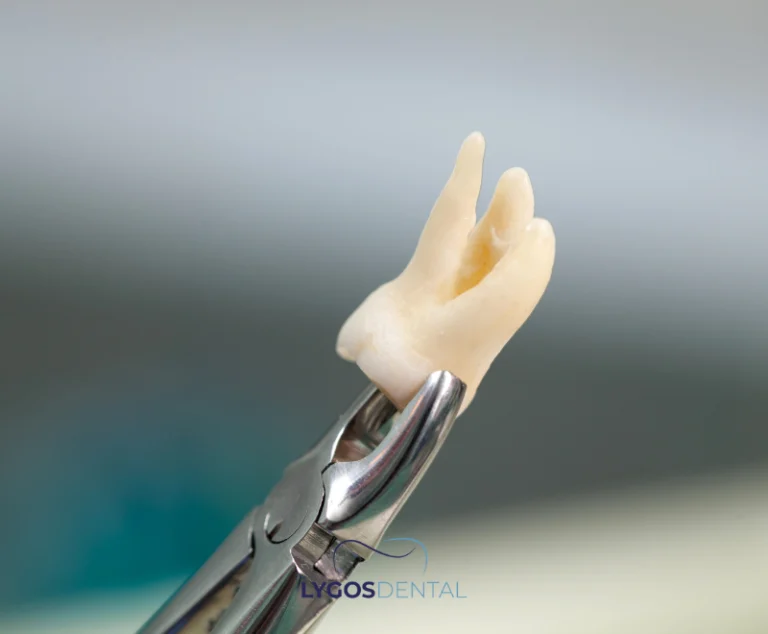
A dental exam is essential because fine cracks may not appear on standard X-rays. Your dentist may use a bite test, special lighting (transillumination), staining, magnification, or periodontal probing to locate the crack and assess its depth.
If symptoms suggest the crack may extend deeper, additional imaging may be recommended to evaluate the tooth and surrounding bone. Diagnosis also includes ruling out other causes of bite pain, such as high fillings, gum inflammation, or tooth decay.
Treatment Options
Treatment depends on where the crack sits, how deep it is, and whether the tooth’s nerve is affected. Your dentist will recommend the least invasive option that protects the tooth and prevents the crack from spreading.
- Bonding or a small filling: For minor surface cracks, bonding can help seal and strengthen the affected area.
- Onlay or crown: When the tooth needs reinforcement, an onlay or crown can hold the tooth together and reduce flexing during chewing.
- Root canal treatment (if the pulp is involved): If the crack reaches the nerve, root canal therapy may be needed, typically followed by a crown to protect the tooth.
- Bite adjustment: In some cases, reshaping a high spot helps reduce pressure on the cracked area.
- Night guard for bruxism: A custom night guard reduces grinding forces and supports long-term protection.
- Extraction (last resort): If the crack extends into the root and the tooth cannot be restored, warning signs may include persistent pain, deep probing, or repeated infection.
Can Cracked Teeth Be Prevented?

You can’t prevent every crack, but these habits can lower your risk:
- Wear a dentist-recommended night guard if you grind or clench your teeth.
- Avoid chewing ice, hard candy, and other hard objects that can overload teeth.
- Don’t use your teeth as tools (opening packages, cracking shells, holding objects).
- Keep up with regular dental checkups so small issues are caught early.
- Support enamel health with a balanced diet that includes calcium and vitamin D.
What Happens If A Cracked Tooth Is Not Treated?
Leaving a crack untreated increases the chance it will spread. Possible outcomes include:
- A larger fracture that shows up suddenly while chewing
- Infection of the pulp and development of an abscess
- A need for more involved treatment, such as root canal therapy and a crown
- Tooth loss if the crack becomes non-restorable
- Jaw discomfort or wear on other teeth if you start chewing on one side
When To See A Dentist
Book an appointment if you notice sharp pain on biting, recurring sensitivity to temperature or sweets, or pain that comes and goes. These symptoms can overlap with other conditions, so an exam is the safest way to identify the cause and protect the tooth.
FAQ
How is cracked tooth syndrome treated?
Crown/onlay to splint; bond minor cracks; root canal if pulp involvement.
How can cracked teeth be repaired naturally?
Cracked teeth can’t be repaired naturally; only temporary protection and prompt dental care help.
Why do cracked teeth hurt so much?
Crack flexing irritates dentin/pulp, causing sharp bite pain and cold sensitivity.
What are the clinical features of cracked tooth syndrome?
Pain on biting/release, cold sensitivity, sometimes sweet sensitivity; vitality tests usually positive.
Is cracked tooth syndrome a dental emergency?
Yes—treat as urgent; early evaluation prevents crack propagation, infection, and tooth loss.
Does cracked tooth syndrome require root canal treatment?
Only if the crack inflames/infects pulp; otherwise crown/onlay or bonding may suffice.
How is cracked tooth syndrome tested?
Bite test, transillumination, probing, and vitality tests; X-rays often miss cracks.
What deficiency causes cracked teeth?
Vitamin D deficiency can weaken mineralization; vitamin A deficiency is also linked to brittleness.
How Does Pacifier Use Affect Dental Development? | LYGOS DENTAL
How Does Pacifier Use Affect Dental Development?
Pacifiers are generally safe in infancy, but frequent, prolonged sucking can change how the teeth and jaws grow. Over time, it may increase the chance of an open bite, crossbite, or protruding front teeth—especially if the habit continues beyond the toddler years. Choosing a well-designed pacifier and weaning early helps reduce the risk.
Quick Take For Parents

Pacifier use doesn’t automatically mean dental problems. The biggest drivers are how often the pacifier is used, how long the habit lasts, and the pacifier’s shape and firmness.
Many bite changes in baby teeth improve after stopping the pacifier early. If you’re unsure, a pediatric dentist can check growth and reassure you during routine visits.
What Happens In The Mouth When A Baby Uses A Pacifier
Babies are born with a strong sucking reflex. When a pacifier is in the mouth for long periods, it applies gentle but consistent pressure to the gums, developing palate, and jaw.
Because these structures are still forming, repeated pressure can influence the width of the palate and how the front teeth erupt. The effect is usually dose‑dependent: longer and more intense use tends to create bigger changes.
Dental Changes Linked To Long-Term Pacifier Use

Dental professionals most often watch for bite changes rather than cavities from pacifier use itself. The following patterns are the ones most commonly associated with frequent, extended pacifier habits.
Open Bite
An open bite means the upper and lower front teeth don’t meet when the back teeth are together. A pacifier can hold the front teeth apart and keep the tongue forward, which encourages this gap over time.
Posterior Crossbite
A crossbite can happen when the upper jaw becomes relatively narrow, causing the upper back teeth to bite inside the lower teeth. Long-term sucking may contribute by putting outward pressure on the cheeks and inward pressure on the palate.
Increased Overjet And Protruding Front Teeth
Some children develop upper front teeth that tip forward (often called increased overjet). This can affect lip closure and raise the risk of chipping a front tooth during falls or play.
Narrow Palate
In some cases, the palate may not widen as naturally as it should. A narrower palate can be linked to crowding and bite issues later, depending on growth patterns and genetics.
When Does Risk Increase?
In many children, short, occasional pacifier use is unlikely to cause lasting harm. The risk rises when a child uses the pacifier for many hours a day, sleeps with it nightly for years, or keeps it in the mouth most of the day.
Pediatric dental guidance commonly focuses on stopping by around age 3, because bite changes such as open bite are more likely to persist when the habit continues longer. Some guidance also recommends reducing use earlier to limit effects on the developing mouth and ear infections.
How To Use A Pacifier More Safely
Choose A One-Piece, Orthodontic-Shaped Pacifier
If you use a pacifier, choose a one-piece design that is age-appropriate and easy to clean. Many parents prefer orthodontic-shaped pacifiers, which are designed to reduce pressure on the palate compared with round, bulb-shaped tips.
Limit Daytime Use
Try to avoid “all-day” pacifier use. Saving the pacifier for naps, bedtime, or short calming moments reduces the total time pressure is applied to the teeth and jaws.
If your child can be soothed with rocking, a comfort blanket, or a short routine, these can gradually replace the pacifier without a daily battle.
Keep It Clean And Never Sweeten It
Replace worn pacifiers and clean them regularly. Avoid dipping a pacifier in honey, syrup, or any sugary substance—this increases the risk of tooth decay, and honey is unsafe for infants under 12 months due to botulism risk.
If your child uses a pacifier at night once teeth have erupted, keep brushing as the last step before sleep and offer only water afterward.
Pacifier Use Vs. Thumb-Sucking

Both habits can affect dental development when they are frequent and long-lasting. A pacifier is often easier to limit and remove because parents control access, while thumb-sucking can be harder to stop because the “habit tool” is always available.
If your child prefers thumb-sucking, talk to a pediatric dentist early. Gentle habit guidance can help before the behavior becomes deeply routine.
If Your Child Already Has Bite Changes
What Often Improves On Its Own
When pacifier use stops early, many mild bite changes in baby teeth improve naturally as the mouth continues to grow. Improvement is more likely when the habit ends before it becomes a long-term, daily pattern.
When To See A Pediatric Dentist Or Orthodontist
Book a dental check if you notice a persistent gap between the front teeth, one side biting “inside” the other, speech concerns, or if the pacifier habit continues past the toddler years.
A clinician can monitor growth, advise on weaning strategies, and suggest treatment options if a bite problem does not self-correct.
Need Personalized Advice?
If you’re concerned about pacifier use or your child’s bite, a pediatric dental exam can confirm whether development is on track and whether any early changes are likely to resolve after weaning.
Frequently Asked Questions
Is using a pacifier harmful for babies?
Not necessarily. For many babies, pacifiers are a normal soothing tool. Dental concerns are mainly linked to heavy, prolonged use rather than short, occasional use.
Which pacifier model is best for dental health?
Look for an age-appropriate, one-piece pacifier with an orthodontic-shaped nipple and a shield that allows airflow. Replace it when it shows wear.
When should pacifier use be stopped?
Many professionals suggest starting to reduce use in the second year and aiming to stop by around age 3 to lower the chance of longer-lasting bite changes.
If a pacifier caused dental problems, can they be fixed?
Often, yes. Mild changes may improve after stopping early. If a bite issue persists, a pediatric dentist or orthodontist can recommend monitoring or treatment.
Which is more harmful: pacifier use or thumb-sucking?
Either can affect the bite if frequent and long-lasting. Thumb-sucking is often harder to control because it can’t be taken away, so it may persist longer in some children.
Aesthetic Advantages of Zirconium Crowns | LYGOS DENTAL
Aesthetic Advantages of Zirconium Crowns
Zirconia crowns are metal-free ceramic restorations that can deliver a natural-looking smile, especially when matched carefully to your tooth shade and translucency. They help avoid the gray gum-line shadow seen with metal-backed crowns, resist staining, and hold their polish well for years when designed and finished by an experienced dental team.
Table of Contents
What Is A Zirconia Crown?
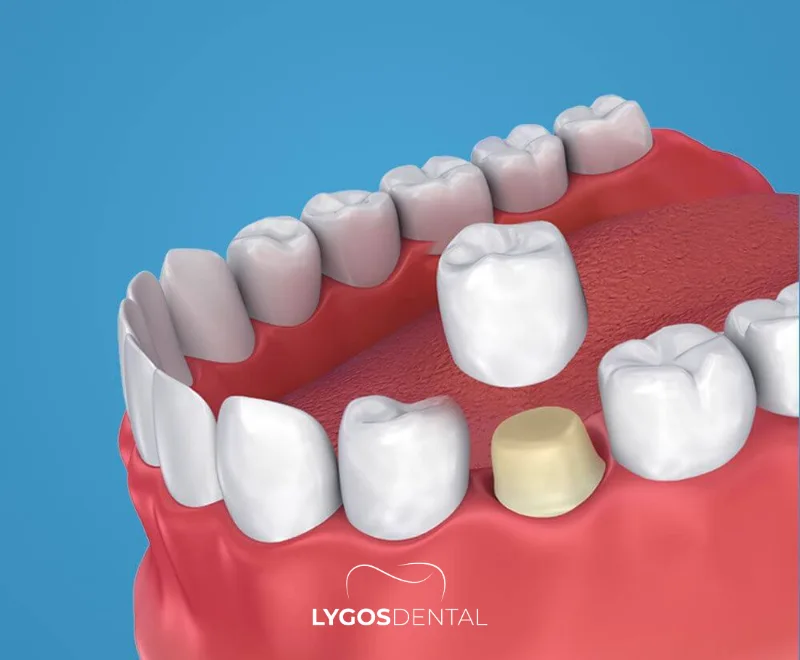
A zirconia crown is a dental crown made from zirconium dioxide (zirconia), a strong ceramic used to restore damaged or heavily filled teeth. Because it contains no metal, it typically blends better at the gum line and is well tolerated by many patients. Dentists use zirconia for both front and back teeth, depending on bite forces and aesthetic goals.
Why Zirconia Can Look So Natural
Aesthetic dentistry is all about how a restoration handles light. Modern zirconia can be manufactured in different translucency levels, which helps the crown mimic the way natural enamel reflects and diffuses light. When the shade, surface texture, and edge profile are finished well, the crown can sit in the smile line without drawing attention.
That said, zirconia is not one single material. Some zirconia types are more opaque and are chosen on purpose to mask dark underlying tooth color, while more translucent zirconia is selected when a softer, enamel-like look is the priority.
Aesthetic Benefits Of Zirconia Crowns
- Enamel-like light behavior: Can be selected in translucency levels to avoid a flat or “chalky” look.
- Custom shade matching: Built to blend with surrounding teeth for a seamless smile.
- Natural-looking gum line: No metal core, so there is typically no dark margin or gray reflection at the gum edge.
- Long-term color stability: Zirconia does not absorb stains the way some materials can, so it tends to keep its shade.
- Durable surface polish: A smooth, well-polished finish can maintain a healthy-looking shine.
- Strong enough for posterior teeth: Useful when you want aesthetics without sacrificing strength in the molars.
Why Zirconia Is Popular In Smile Design

Smile design focuses on tooth proportions, symmetry, and shade harmony. Zirconia is often chosen because it allows predictable strength and controlled aesthetics, which helps when multiple crowns are planned across the smile. In many cases, layered or multi-layer zirconia options can add depth and character so the result doesn’t look uniform.
Aesthetic Limitations To Consider
Zirconia is an excellent option, but it is not automatically the most aesthetic choice for every case. Your dentist may recommend a different ceramic when the goal is maximum translucency in very thin restorations.
- Potential opacity in some cases: Standard zirconia can look more opaque than high-translucency ceramics (such as lithium disilicate) on front teeth.
- Technique sensitive results: Shade, translucency, and surface texture depend on the lab and the finishing protocol.
- Not ideal for ultra-thin, highly translucent work: When minimal thickness is required, other ceramics may better mimic natural enamel.
- Cost: Zirconia crowns can cost more than basic porcelain-fused-to-metal options because of materials and lab work.
Porcelain Vs Zirconia Crowns: Key Aesthetic Differences

“Porcelain crown” can mean different things, including porcelain-fused-to-metal (PFM) crowns or all-ceramic options. From an aesthetic perspective, the biggest differences are usually at the gum line and in how the crown transmits light.
Light And Translucency
Zirconia: Available in various translucency levels; some types are designed to mask dark teeth, while others aim for a softer, enamel-like appearance.
PFM porcelain: The metal substructure can block light, which may make the crown look flatter or more opaque, especially in bright light.
Gum-Line Appearance
Zirconia: Metal-free, so the margin typically stays bright without a gray shadow at the gum edge.
PFM porcelain: The metal edge may create a dark line over time, especially if the gums recede.
Long-Term Look
Zirconia: Generally maintains its color and gloss well when the surface is properly finished and maintained.
PFM porcelain: Can look good, but chips in porcelain layering or gum-line shadowing may affect aesthetics over the long term.
Call To Action
If you are considering zirconia crowns for aesthetic reasons, ask your dentist to show before-and-after cases and discuss which zirconia type is planned for your teeth. A shade-matching appointment and a quality dental lab are key parts of a natural-looking result.
FAQ
What are the pros and cons of zirconia crowns?
Strong, metal-free, biocompatible; downsides include cost, less translucency, possible opposing-tooth wear.
Do celebrities get veneers or crowns?
Yes; veneers are common for cosmetic changes, while crowns provide full-tooth coverage.
Can zirconia crowns last 20 years?
Yes, with good fit, hygiene, and bite control, zirconia crowns can last 20 years.
Do your teeth need to be filed down for zirconia crowns?
Yes; teeth are reduced to create space, though zirconia often needs less reduction.
What is the healthiest type of crown?
High-noble gold crowns are among the most biocompatible; zirconia is another excellent option.
Why do dentists encourage the use of zirconia?
High strength, fracture resistance, metal-free biocompatibility, and conservative preparation make zirconia attractive.
Why do zirconia crowns fall out?
They debond from poor retention or contaminated bonding surfaces, plus improper cementation or fit.
Natural Ways to Relieve Toothache | LYGOS DENTAL
Natural Ways to Relieve Toothache
A toothache can feel urgent, but many cases can be soothed at home while you arrange dental care. Saltwater rinses, cold compresses, and clove oil may ease discomfort by lowering bacteria, swelling, or nerve irritation. If pain lasts more than 48–72 hours, or you have swelling, fever, or trouble swallowing, see a dentist promptly.
Toothache is a common problem that can disrupt eating, sleep, and concentration. Natural approaches can help manage symptoms, especially when medication is not an option or you want extra comfort. These steps are meant for short-term relief and do not replace an exam when the cause is unclear or the pain is severe.
Table of Contents
What Causes Toothache?
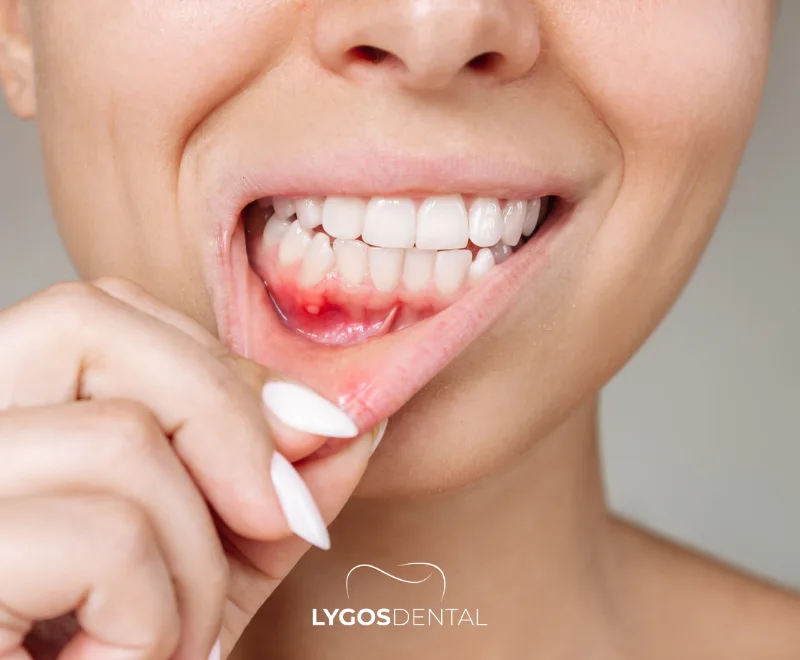
Tooth pain usually points to an issue in the tooth, gum, or surrounding tissues. Relief methods work best when they match the cause, so it helps to think about what triggered the pain. Common causes include:
- Tooth decay: sugar, frequent snacking, and poor brushing can weaken enamel and lead to cavities.
- Gum disease: gingivitis or periodontitis can cause soreness, bleeding, and sensitivity.
- Cracked or broken teeth: biting hard foods, grinding, or trauma can expose sensitive layers.
- Sinus-related pressure: upper tooth pain can occur with sinus congestion or infection.
- Tooth sensitivity: sharp pain with hot, cold, or sweet foods may signal enamel wear or gum recession.
If you recently had dental work, sensitivity can also be temporary. Ongoing or worsening pain usually needs a dental assessment.
How To Manage Toothache At Home
Home care focuses on calming inflammation and keeping the area clean. Use these steps for temporary relief while you monitor symptoms or schedule a visit.
1) Rinse With Warm Salt Water
Mix about 1/2 teaspoon of salt in a glass of warm water, then swish for 30 seconds and spit. This can help reduce bacteria and soothe irritated gums. Repeat a few times per day, especially after meals.
2) Use A Cold Compress
Apply a cold compress to the outside of the cheek near the painful area for 15–20 minutes, then take a break. Cold can reduce swelling and dull pain signals. Wrap ice or a gel pack in a cloth to protect the skin.
3) Keep Your Head Elevated
When lying flat, blood pressure in the head can increase throbbing pain. Try resting with an extra pillow or sleeping slightly upright. This is often helpful at night.
4) Sip Soothing Herbal Tea
Warm herbal teas such as peppermint or chamomile may feel calming and can be used as a gentle mouth rinse once cooled. Avoid very hot liquids if you have sensitivity. Stop if any tea irritates your mouth or stomach.
Natural Remedies For Toothache

Some natural options have a long history of use and may offer short-term comfort. Use care with anything applied directly to the gums, and discontinue if you notice burning, rash, or worsening pain.
Clove Oil (Eugenol)
Clove oil contains eugenol, which can numb and calm irritated tissues. Dilute 1–2 drops in a small amount of carrier oil (such as olive oil), then dab it on the sore tooth with a cotton swab. Do not swallow clove oil, and avoid using it on young children without professional advice.
Garlic Paste
Garlic has antibacterial compounds that may help when decay or gum irritation is involved. Crush a small piece of garlic and mix it with a pinch of salt to form a paste, then apply briefly to the affected tooth. Rinse afterward, and stop if it causes burning.
Fresh Ginger
Ginger may help reduce inflammation and can be used as fresh slices, chewed gently on the opposite side, or as tea. Avoid if ginger upsets your stomach or if you are advised to limit it for medical reasons. Rinse with water afterward to keep the area clean.
Aloe Vera Gel
Food-grade aloe vera gel may soothe inflamed gums. Apply a small amount to the gumline near the painful tooth, then rinse after a short time. Do not use aloe meant for cosmetic products unless it is labeled safe for oral use.
Baking Soda Rinse
Baking soda can help neutralize acids and reduce bacteria in the mouth. Stir 1/2 teaspoon of baking soda into a glass of warm water and rinse, then spit. Use sparingly if your mouth feels dry or irritated.
What Quickly Relieves Toothache?
Fast relief usually comes from reducing swelling and numbing the area. Try one or two approaches at a time so you can tell what helps.
- Cold compress + saltwater rinse: a solid first step for swelling and gum irritation.
- Diluted clove oil on the tooth: can numb pain quickly for some people.
- A gentle rinse after eating: helps remove trapped food that can trigger sharp pain.
Avoid placing aspirin directly on the tooth or gums, as it can burn oral tissues. If you need medication, follow label directions or ask a pharmacist or dentist.
Preventive Measures For Toothache

Preventing toothache starts with controlling plaque and protecting enamel. Small habits make the biggest difference over time.
- Brush twice daily with fluoride toothpaste and replace your toothbrush regularly.
- Floss or use interdental cleaners to remove plaque between teeth.
- Limit sugary snacks and acidic drinks; rinse with water afterward when you can’t brush.
- Choose a balanced diet with calcium, vitamin D, and plenty of fibrous fruits and vegetables.
- Book routine dental checkups to catch cavities and gum issues early.
When Should You See A Dentist?
Home remedies can take the edge off, but they cannot fix cavities, deep cracks, or infections. Arrange a dental visit as soon as you can if pain is persistent or keeps returning.
Seek urgent care if you have:
- Pain that lasts longer than 48–72 hours or is severe
- Facial or jaw swelling
- Fever, chills, or feeling unwell
- Pus, a bad taste, or persistent bleeding from the gums
- Difficulty opening your mouth, swallowing, or breathing
These signs can indicate an infection that needs prompt treatment.
Get Information And Book An Appointment
If you’d like professional advice or treatment options, contact us to ask about cosmetic dentistry, dental crowns, dental implants, and general dentistry services. We can help you choose the right next step based on your symptoms and goals.
FAQ
What quickly stops toothache?
Ibuprofen, or ibuprofen plus acetaminophen, usually stops toothache fastest temporarily until you see a dentist.
What is the 3-3-3 rule for toothache?
Online “3-3-3” varies; common version: 600mg ibuprofen, three times daily, ≤3 days, then dentist.
What is the most powerful natural painkiller for toothache?
Clove oil eugenol is the most potent common natural topical numbing agent for toothache.
What relieves nerve pain in the tooth?
Ibuprofen plus acetaminophen relieves nerve-driven tooth pain; definitive relief needs dental treatment.
How can a tooth infection be treated without root canal therapy?
Extraction or incision-and-drainage treats infection without root canal; antibiotics are adjunct when indicated.
What relieves a tooth infection?
Drainage or tooth removal relieves infection; antibiotics help only with spreading or systemic illness.
Why are toothaches so severe at night?
Lying down increases head pressure, saliva drops, and fewer distractions make pain feel worse.
Which finger should you press for toothache?
Press the web between thumb and index finger (LI4); avoid if pregnant.
What to Do If a Dental Filling Falls Out | LYGOS DENTAL
What to Do If a Dental Filling Falls Out
If a filling falls out, rinse your mouth, gently clean the tooth, and avoid chewing on that side. Cover the area with an over‑the‑counter temporary filling or dental wax, then call a dentist as soon as you can—ideally within 24–48 hours. Seek urgent care if swelling, fever, or severe pain starts.
Table of Contents
Why Dental Fillings Fall Out

A filling can fail for several reasons, and the cause helps your dentist choose the right repair. Sometimes the filling material simply reaches the end of its lifespan, but new decay or a crack in the tooth can also be the trigger.
- Normal wear and aging: Fillings aren’t permanent. Composite fillings often last around 5–10 years, while amalgam fillings can last 10–15 years or longer, depending on the tooth and bite.
- Biting forces: Chewing hard foods or grinding/clenching (bruxism) can loosen or fracture a filling.
- New decay around the filling: Bacteria can creep in at the edges over time and weaken the bond.
- Tooth damage: A chip or crack in the tooth can cause the filling to break free.
Moisture or bonding issues: Less-than-ideal bonding conditions can shorten the life of a filling.
What To Do Right Away
Most lost fillings aren’t life-threatening, but the exposed tooth is more likely to become sensitive or fracture. Try to protect the tooth and arrange dental care as soon as you can.
- Rinse and clean gently. Rinse with warm water and brush softly to remove food debris. Avoid aggressive scrubbing over the exposed area.
- Save the filling if you can. If the piece came out intact, place it in a clean container and bring it to your appointment.
- Avoid chewing on that side. Stick to softer foods and skip hard, crunchy, or sticky snacks that could crack the tooth.
- Manage sensitivity. If hot, cold, or sweet foods sting, avoid triggers. Over-the-counter pain relief may help if it’s safe for you.
- Book a dental visit. Aim to be seen promptly, especially if the tooth is painful or the hole is large.
Temporary At-Home Protection Until You See a Dentist

Home fixes are meant to protect the tooth for a short time. They don’t replace a proper filling, and they won’t stop decay if it’s present.
Over-The-Counter Temporary Filling Material
Pharmacies often sell temporary filling kits or dental cement. Follow the package directions closely and keep the area as dry as possible while placing the material.
Dental Wax For Sharp Edges
If the tooth feels sharp and is rubbing your tongue or cheek, dental wax can make it more comfortable until you’re treated.
Saltwater Rinses
A warm saltwater rinse can soothe irritated gums and help keep the area clean. Swish gently and spit—don’t swallow the rinse.
What Not To Use
Avoid household glues (including superglue), as they aren’t made for oral tissues and can be harmful. Also avoid packing aspirin or powders into the hole, which may irritate the gums.
When It’s Urgent
Call a dentist urgently—or seek emergency care—if you notice any of the following signs. These can point to infection or a deeper tooth problem.
- Facial or jaw swelling
- Fever, pus, or a bad taste that won’t go away
- Severe, worsening, or throbbing pain
- Trouble swallowing or breathing
- Bleeding that won’t stop
- A cracked tooth or pieces of tooth breaking away
What Your Dentist May Do
The best option depends on how much tooth structure is left and whether there’s new decay. Your dentist will check the tooth, clean the area, and recommend a repair that will hold up to your bite.
- Replace the filling: The tooth is cleaned and a new filling is bonded in place.
- Repair or rebuild the tooth: If the tooth is chipped or the cavity is large, your dentist may build it up before placing a new filling.
- Crown (cap): A crown may be recommended when a large portion of the tooth is weakened or cracked.
- Root canal treatment: If the nerve is inflamed or infected, treatment may be needed before the tooth can be restored.
- Extraction: This is uncommon, but it can be the safest choice when the tooth can’t be saved.
How To Help Prevent A Filling From Falling Out Again
Good daily habits and regular checkups make fillings last longer. If you’ve lost a filling once, ask your dentist whether bite adjustment or a night guard would help.
- Keep up with checkups and cleanings so early decay is caught before it undermines a filling.
- Brush twice daily and floss once daily to reduce plaque around the edges of fillings.
- Limit hard and sticky foods that can pull at restorations.
- Treat grinding and clenching with a dentist-recommended night guard if needed.
- Cut back on smoking and frequent acidic drinks, which can affect oral health and contribute to wear.
Book An Appointment
If you’ve lost a filling and need an exam, schedule a visit as soon as possible. A dentist can protect the tooth and reduce the chance of further damage.
Cosmetic Dentistry • Dental Crowns • Dental Implants • General Dentistry
FAQ
How long can you manage when a filling falls out?
One to two days; same day if pain, swelling, or fever.
How many times can a tooth be filled?
No fixed limit; fillings can be replaced until too little tooth remains.
What is the average lifespan of a dental filling?
About 5–15 years, depending on material, size, and chewing forces.
What does an old filling look like when it falls out?
A hard piece, silver or tooth-colored, often worn, cracked, or stained.
Can a tooth become infected when a filling falls out?
Yes, bacteria can enter the exposed cavity and infect the pulp.
What factors shorten the lifespan of a filling?
Decay, poor hygiene, large fillings, bruxism, hard biting, and acidic/sugary diets shorten lifespan.
The Effect of a Gluten-Free Diet on Gum Health | LYGOS DENTAL
The Effect of a Gluten-Free Diet on Gum Health
A gluten-free diet can support gum health for people with celiac disease or gluten sensitivity by lowering systemic inflammation and improving nutrient absorption. It won’t replace brushing, flossing, or dental cleanings, and poorly planned gluten-free eating can cause deficiencies that irritate gums. Focus on whole foods and balanced minerals.
Gluten-free eating is essential for people with celiac disease and often helpful for those with non-celiac gluten sensitivity. It has also become common among people trying to reduce bloating, discomfort, or inflammation.
Diet changes can show up in the mouth quickly, since gum tissues react to inflammation, dry mouth, and nutrient gaps. Below is how a gluten-free diet may influence gum health—and where it can fall short.
Table of Contents
What Is a Gluten-Free Diet?

A gluten-free diet essentially means completely eliminating gluten — a protein found in wheat, barley, rye, and their derivatives — from one’s meals. Gluten gives dough its elasticity and structure, particularly in baked goods like bread. However, some individuals experience negative reactions to gluten in their digestive system.
Celiac disease, for example, is an autoimmune condition in which consuming gluten triggers the immune system to damage the small intestine. For this reason, individuals with celiac disease, gluten intolerance, or sensitivity adopt a gluten-free diet. In recent years, however, many people have chosen this diet to feel healthier or to reduce inflammation in their bodies.
At this point, the effect of a gluten-free diet on gum health becomes significant because inflammation in the digestive system can manifest in other parts of the body — especially in the mouth.
Possible Effects of Gluten on Oral and Dental Health
Gluten can affect not only the digestive system but also the immune system and the mucous membranes in the mouth. Individuals with celiac disease, for instance, may experience mouth ulcers, canker sores, or weakened tooth enamel. In some cases, systemic inflammation linked to gluten exposure may contribute to gum inflammation.
Some studies have shown that people with gluten intolerance are more likely to experience gum recession, bleeding, and dry mouth. The primary reason is that gluten can disrupt the balance of gut flora, leading to immune system irregularities. When the immune system is weakened, the gums become more vulnerable to bacterial infection.
Thus, the effect of a gluten-free diet on gum health is not only due to the absence of gluten itself but also due to the reduction of overall inflammation in the body. In other words, a gluten-free diet can indirectly support gum health.
How Does a Gluten-Free Diet Affect Gum Health?

The impact of a gluten-free diet on gum health can be explained through several mechanisms.
• Anti-inflammatory benefits: A gluten-free diet often has anti-inflammatory effects. When systemic inflammation decreases, the risk of gingivitis (gum inflammation) and periodontitis (advanced gum disease) may also decline.
• Nutrient-rich foods: Gluten-free diets usually emphasize fresh vegetables, fruits, and healthy fats while avoiding processed foods. These foods are rich in antioxidants, which support gum tissue regeneration. Vitamins C and K, as well as omega-3 fatty acids, are particularly beneficial for gum health.
• Improved gut and immune health: When a gluten-free diet improves gut health, it helps stabilize the immune system. A balanced immune system can better defend the gums against bacterial infections. Therefore, the effect of a gluten-free diet on gum health is closely tied to overall body health and balance.
Things to Watch for When Protecting Gum Health on a Gluten-Free Diet
If not followed correctly, a gluten-free diet can lead to nutritional deficiencies. Essential nutrients such as B vitamins, iron, calcium, and zinc — all important for gum health — might be insufficient. For this reason, maintaining a balanced diet is crucial to ensure that the effect of a gluten-free diet on gum health remains positive.
Here are some key points to keep in mind:
- • Choose alternatives to whole grains: Gluten-free grains like buckwheat, quinoa, amaranth, and teff are rich in minerals that nourish the gums.
- • Get enough vitamins and minerals: Vitamin C (found in oranges, kiwis, broccoli), vitamin D (from fish, eggs), calcium (from almonds, leafy greens), and zinc (from pumpkin seeds, chickpeas) all support gum health.
- • Reduce sugar intake: Many gluten-free products contain added sugar for flavor, which can trigger gum inflammation.
- • Stay hydrated: Drinking plenty of water prevents dry mouth and helps keep gum tissues moist and healthy.
By following these guidelines, the positive effect of a gluten-free diet on gum health can be maximized.
Recommended Oral Care Routine for Those on a Gluten-Free Diet

Oral hygiene is just as important as nutrition for those who follow a gluten-free lifestyle, as dietary changes can alter the oral microbiome. To fully experience the benefits of a gluten-free diet on gum health, the following oral care habits are recommended:
- • Brush twice daily: Use a fluoride-containing but gluten-free toothpaste.
- • Use dental floss: It helps prevent plaque buildup and gum recession.
- • Rinse with mouthwash: Choose alcohol-free, antibacterial mouth rinses.
- • Visit the dentist regularly: Early detection and treatment of gum inflammation are essential.
- • Be cautious with food residues: Some gluten-free snacks can be sticky and get trapped between teeth, so clean your mouth after every meal.
These simple but effective routines can make the gum health benefits of a gluten-free diet more lasting.
Is a Gluten-Free Diet Truly Beneficial for Gum Health?
Answer: Yes — but it depends on individual circumstances.
For people with celiac disease or gluten sensitivity, a gluten-free diet can make a noticeable difference in gum comfort and inflammation. When a trigger for chronic immune activation is removed, gums may bleed less and feel less tender. Improved intestinal absorption can also help the body use nutrients that support the gums.
Adopting a gluten-free diet as a trend—without planning—can create problems. Nutrient gaps may weaken gum tissue and slow healing. If you’re going gluten-free for health reasons, it helps to check in with a dietitian and keep routine dental visits on schedule.
Overall, research suggests that a gluten-free diet may reduce inflammation and support gum tissue health—especially for people who react negatively to gluten. Results vary from person to person. A nutrient-rich gluten-free diet, paired with consistent oral hygiene and regular checkups, offers the most reliable support for healthy gums.
A healthy smile is not only the result of proper brushing — it also begins with proper nutrition.
Book A Consultation
Contact us to book an appointment and ask about cosmetic dentistry, crowns, implants, or general dental care. If you’re following a gluten-free diet, we can also help you tailor an oral-care routine that fits your needs.
FAQ
Can gluten affect your gums?
Yes, in celiac/gluten sensitivity it can worsen oral inflammation via immune reactions and deficiencies.
What foods help repair gums?
Vitamin C–rich fruits, leafy greens, omega-3 fish, and adequate protein support gum healing.
What happens to my body if I stop consuming gluten?
If you’re not gluten-sensitive, stopping gluten may not help and can reduce nutrients.
Do dentists use products containing gluten?
Rarely; most dental materials are gluten-free, but some flavorings/pastes may contain gluten.
What foods worsen gum disease?
Sugary drinks, refined carbs, sticky sweets, and frequent snacking worsen plaque and gum inflammation.
Why do so many doctors oppose a gluten-free diet?
Because unnecessary gluten avoidance can cause deficiencies and complicate accurate celiac disease testing.
Is it healthier to stop consuming gluten?
Only for celiac disease or gluten sensitivity; otherwise whole-grain gluten foods are healthy.
The Cheapest Country for Dental Treatment | LYGOS DENTAL
The Cheapest Country For Dental Treatment
Turkey is often the cheapest country for dental treatment when you compare modern clinic standards with typical prices for implants, crowns, and cosmetic work. Hungary, Poland, Thailand, Mexico, and India can also offer strong value. The best option depends on your treatment plan, travel costs, and how carefully you verify the clinic, materials, and aftercare.
Dental care can be expensive in many countries, especially for implants, crowns, and cosmetic dentistry. That’s why dental tourism has grown—patients travel abroad to reduce costs while still choosing reputable clinics and experienced dentists. This guide explains where prices are typically lowest and what to check before you book.
Table of Contents
Which Country Is The Cheapest For Dental Treatment?
There isn’t one perfect answer for everyone. The cheapest destination depends on the procedure, the clinic, and what’s included in the quote (consultations, scans, implant brand, temporary teeth, lab work, and follow-up visits). That said, several countries consistently rank among the most affordable:
- Turkey (often the best overall balance of price and clinic infrastructure)
- Hungary (a long-standing option for patients traveling from Europe)
- Poland (competitive pricing within the EU)
- Thailand (strong private healthcare sector and tourist-friendly services)
- Mexico (popular for patients traveling from the United States)
- India (very low prices, especially for extensive treatment plans)
When patients compare like-for-like treatment plans, Turkey is commonly the most cost-effective choice in Europe and nearby regions.
Why People Choose Dental Treatment Abroad

Patients usually travel for a mix of financial and practical reasons:
- Lower total treatment cost compared with prices in Western Europe, the UK, and the U.S.
- Shorter waiting times for consultations and procedures at many private clinics.
- Access to modern dentistry (digital scans, 3D planning, and newer implant systems) at a lower price point.
- The ability to combine treatment with travel—useful when multiple visits are required.
Why Turkey Is So Popular For Dental Treatment
Lower Prices, Often 50%–70% Less Than The UK Or U.S.
Turkey’s prices are usually lower because of operating costs (rent, staffing, laboratory fees) and the exchange rate, not because modern dentistry is unavailable. As a rough example, a single implant that can cost several thousand pounds in the UK may be quoted in the hundreds to low thousands in Turkey, depending on brand and complexity.
Experienced Dentists And International Patient Services
Many clinics that focus on international patients provide English-speaking coordinators, clear treatment plans, and bundled services. Look for transparent pricing, a named dentist, and clinical documentation (x-rays/CT scans and a written plan).
Modern Clinics, Technology, And Convenience
Major cities such as Istanbul, Antalya, and Izmir host clinics equipped with digital dentistry workflows, in-house imaging, and sterilization systems aligned with common European practice. For many travelers, short flight times and frequent routes make planning easier.
Typical Dental Treatment Prices By Country (2026)
Prices vary by clinic, city, implant/crown brand, and what’s included (implant fixture vs. implant + abutment + crown). Use these ranges as a starting point and request a fully itemized quote.
| Country | Implant (per tooth) | Zirconium Crown | Root Canal Treatment | Teeth Whitening |
| Turkey | €500 – €900 | €150 – €250 | €100 – €250 | €150 – €300 |
| Hungary | €800 – €1,500 | €200 – €350 | €150 – €300 | €200 – €350 |
| Poland | €900 – €1,600 | €220 – €400 | €180 – €350 | €200 – €350 |
| Thailand | €900 – €1,700 | €250 – €450 | €200 – €400 | €250 – €450 |
| Mexico | €700 – €1,300 | €200 – €350 | €150 – €300 | €200 – €350 |
| UK | €1,600 – €4,000 (approx.) | €600 – €900 (approx.) | €400 – €900 (approx.) | €450 – €850 (approx.) |
Tip: If your quote seems unusually low, confirm the implant brand, warranty terms, lab quality, and whether the crown, abutment, scans, and medications are included.
What To Consider When Choosing Affordable Dental Care

Low prices are only a win if the treatment is planned well and supported with proper aftercare. Use this checklist before you book:
- Clinic licensing and standards: ask for the clinic’s registration details and sterilization protocol.
- Dentist credentials: confirm who will perform the procedure and review their training and case experience.
- Materials and brands: request the exact implant system and crown material in writing.
- Imaging and planning: ensure you’ll receive x-rays/CT scans and a documented treatment plan.
- Guarantee and aftercare: understand what is covered, for how long, and how issues are handled once you return home.
- Realistic scheduling: implants often require healing time, so avoid “one-trip” promises unless your case truly suits immediate loading.
Best Countries For Dental Tourism
If you want both value and a smooth patient experience, these destinations are the most common starting points:
- Turkey: frequently the best value for implants, crowns, and full smile makeovers.
- Hungary: strong option for EU travelers and multi-visit treatment plans.
- Poland: competitive EU pricing with easy travel from Western Europe.
- Thailand: popular in Asia with many private clinics used to international patients.
- Mexico: convenient for U.S. travelers, especially for border cities and major hubs.
Your “cheapest” option is the one that matches your clinical needs, includes the right materials, and still makes sense after travel and accommodation.
Request Information
If you’re comparing options, share your recent x-ray (or panoramic image), a list of your priorities, and your travel timeline. A reputable clinic should respond with an itemized plan and clear answers about materials, warranties, and follow-up care.
You can contact us to ask about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry, and to request an appointment or a quote.
FAQ
Which is the cheapest country to get your teeth treated?
Turkey is among the cheapest for complex dental work, especially package pricing.
Which is the best country to get my teeth treated?
Hungary is a top dental-tourism choice for EU-standard care and specialist implant clinics.
Why is dental treatment so cheap in Mexico?
Lower wages, overhead, and stronger competition make dental care in Mexico cheaper.
Is it cheaper to get dental implants abroad?
Yes, dental implants abroad are often 50–70% cheaper than UK/US prices.
In which country are the best dental implants made?
Switzerland and Sweden lead premium implant manufacturing, including Straumann and Nobel Biocare.
Which country offers cheap crowns?
Turkey offers low-cost dental crowns, often via all-inclusive packages.
Use of Stem Cells in Dental Treatments | LYGOS DENTAL
Use of Stem Cells in Dental Treatments
Stem cells are being studied in dentistry for their potential to support tissue repair—especially in the dental pulp, gums (periodontium), and jawbone. Some approaches have reached early clinical use in carefully selected cases, while others—such as growing a brand‑new tooth—remain experimental and largely limited to animal research.
Table of Contents
What Stem Cells Are and Why They Matter in Dentistry
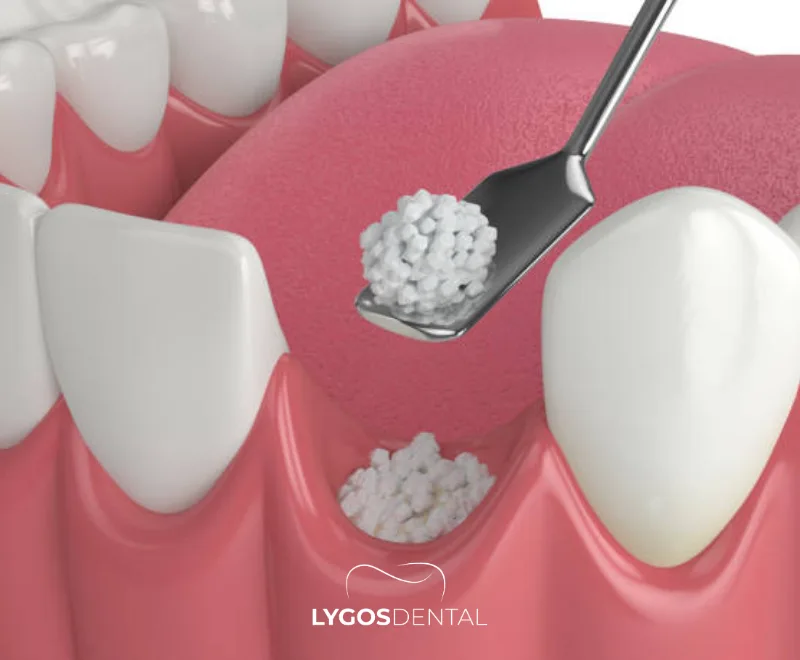
Stem cells are cells that can self‑renew and, under the right conditions, develop into more specialized cell types. In regenerative dentistry, researchers focus mainly on mesenchymal stem cells (MSCs), including dental‑origin stem cells found in tissues such as dental pulp, periodontal ligament, and exfoliated (baby) teeth.
The goal is not to “fill” or “replace” tissue in the classic sense, but to encourage the body to rebuild damaged structures—often with the help of biomaterials (scaffolds) and signaling molecules that guide the healing process.
Where Stem Cell‑Based Approaches Are Being Explored Today
Pulp and Root Canal‑Related Regeneration
When the dental pulp is severely inflamed or infected, conventional root canal treatment removes the diseased tissue and seals the canal. Regenerative endodontics aims to restore living tissue inside the tooth so it can regain some biological function.
Dental pulp stem cells (DPSCs) and stem cells from exfoliated deciduous teeth (often called SHED) have been widely studied for this purpose. The strongest evidence today sits in early clinical research and controlled clinical trials, but protocols are still being refined and are not yet routine in everyday practice.
Gum, Periodontal Ligament, and Bone Regeneration
Periodontitis can destroy the periodontal ligament and the bone supporting the teeth. Conventional periodontal therapy can control infection and slow progression, yet complete regeneration of lost structures is difficult.
Stem cell‑based tissue engineering is being investigated for periodontal bony defects and advanced periodontal disease. Recent reviews and clinical research report promising improvements in certain outcomes, but results vary by defect type, cell source, delivery method, and patient factors.
Scaffolds, Biomaterials, and Growth‑Factor Support
Stem cells rarely work alone. Many regenerative protocols combine cells with biocompatible scaffolds that help the cells attach and organize, plus biological signals that nudge them toward forming the right tissue.
In clinical dentistry, blood‑derived concentrates such as PRP (platelet‑rich plasma) and PRF (platelet‑rich fibrin) are sometimes used as adjuncts because they release growth factors over time. These are not the same as stem cell transplantation, but they can support wound healing and regeneration in selected indications.
Can a New Tooth Be Grown from Stem Cells?
Whole‑tooth regeneration is one of the most exciting ideas in regenerative dentistry—and also one of the least mature clinically. Researchers have created tooth‑germ or tooth‑bud‑like structures in the laboratory and achieved tooth‑like formation in animal models.
At the moment, these advances do not translate to routine “grow me a new tooth” treatment for humans. Challenges include reliably forming enamel, controlling shape and eruption, achieving stable nerve and blood supply, and proving long‑term safety. For patients today, implants, bridges, and prosthetics remain the standard options for missing teeth.
Benefits and Limitations Patients Should Know
Potential benefits
- Biologically driven repair: aims to rebuild tissue rather than simply replace it.
- Better integration: regenerated tissue may behave more like natural gum, bone, or pulp compared with synthetic substitutes.
- Inflammation control: MSCs are being studied for their immunomodulatory effects, which may support healing in some contexts.
Limitations and risks
- Not standardized everywhere: many protocols are still evolving, and availability varies by country and clinic.
- Cost and complexity: cell isolation, expansion, and quality control can be expensive and resource‑intensive.
- Time to see results: true tissue regeneration can take weeks to months, and outcomes are not guaranteed.
- Evidence varies by indication: some applications have stronger human data than others; “tooth regrowth” remains experimental.
Stem Cell–Related Dental Treatments in Turkey

Turkey is a well‑known destination for dental care and health tourism. Regenerative dentistry services may include research‑driven stem cell applications in academic settings, as well as more established adjuncts such as PRP/PRF to support soft‑tissue and bone healing.
As with any cell‑ or tissue‑based intervention, regulatory oversight and clinic credentials matter. Patients should ask whether a procedure is part of an approved clinical protocol, what evidence supports the indication, and how the clinic ensures quality and safety (including laboratory standards when cells are processed).
Get More Information
If you’re considering regenerative options—alongside implants, crowns, or periodontal treatment—book a consultation to review your diagnosis, available therapies, and realistic outcomes based on current evidence.
You can contact us to learn more about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry, and to arrange an appointment.
FAQ
Application of stem cells in dentistry
Experimental uses include pulp regeneration, periodontal repair, bone regeneration, and tissue-engineered grafts.
Stem cell dental implants cost
No standard cost; stem-cell dental implants aren’t commercially available outside research trials.
Types of dental stem cells
DPSC, SHED, PDLSC, SCAP, DFSC, gingival MSCs, and alveolar bone MSCs.
Where can i get stem cell dental implants
Only in regulated clinical trials at research dental hospitals; routine clinics don’t offer them.
Stem cell tooth regeneration
Not routine; stem cells may regenerate pulp/periodontium, but whole-tooth regrowth remains experimental.
How Does Tooth Loss Affect Speech? | LYGOS DENTAL
How Does Tooth Loss Affect Speech?
Tooth loss can affect speech by changing how air flows through the mouth and where the tongue and lips make contact. Gaps—especially in the front teeth—often make sounds like s, z, f, v, and th harder to pronounce, leading to lisping or whistling. Replacing missing teeth and adjusting bite support usually improves clarity.
Table of Contents
Why Teeth Matter For Clear Speech

Teeth are part of the “articulation system” that shapes sound. They help control airflow and give the tongue and lips stable surfaces to press against when forming consonants.
When a tooth is missing, the mouth often compensates by changing tongue position or letting extra air escape. That can distort certain sounds, reduce crispness, or make speech feel less effortless—especially at normal conversation speed.
Which Sounds Are Most Affected
S And Z Sounds
Sibilant sounds like “s” and “z” rely on a narrow channel of air directed toward the front teeth. Missing front teeth can widen that channel, causing lisping, whistling, or a softer, less defined sound.
F And V Sounds
For “f” and “v,” the upper front teeth lightly touch the lower lip. If those teeth are missing or significantly shifted, it can be harder to create the correct friction, which may lead to substitutions (for example, a sound closer to “p” or “b”).
T, D, N, And Th Sounds
Sounds such as “t,” “d,” “n,” and “th” depend on precise tongue placement near the teeth and the ridge behind them. Gaps can change the tongue’s target and timing, so words may sound slightly slurred or less clear until you adapt.
What Changes When Teeth Are Missing
The impact isn’t only about the visible gap. Tooth loss can affect speech through several practical changes:
- Air leaks through spaces that used to be sealed by teeth.
- The tongue may sit differently at rest and during speech.
- The bite can shift over time, altering jaw position and muscle balance.
- Chewing efficiency drops, which can affect how you prepare to speak during conversation.
How Location And Number Of Missing Teeth Change The Impact

Missing front teeth tend to cause the most noticeable speech changes because they are directly involved in forming many consonants. A single missing tooth may create a subtle whistle, while multiple gaps can make clarity noticeably worse.
Missing back teeth usually affects chewing more than pronunciation at first. Over time, though, back-tooth loss can reduce bite support, encourage shifting, and change jaw posture—which may indirectly influence speech and comfort.
Tooth Loss And Confidence In Social Settings
Speech changes can feel frustrating, even when they’re mild. Some people speak more slowly, avoid certain words, or hold back in social situations because they’re self-conscious about pronunciation or appearance.
If you notice yourself avoiding conversations, meetings, or phone calls, it’s worth addressing the dental cause early. Restoring a stable bite and tooth surfaces often helps both clarity and confidence.
How To Improve Speech After Tooth Loss
Many speech issues improve once missing teeth are replaced and the mouth has time to adapt. The right option depends on how many teeth are missing, where they are, and your overall oral health.
Dental Implants
Implants replace the tooth root and crown, providing a stable, fixed surface for speech and chewing. They can be especially helpful for front-tooth gaps where airflow control and lip contact matter most.
Dental Bridges
Bridges can restore missing teeth by anchoring to nearby teeth. When the fit is precise, bridges often improve pronunciation quickly because they recreate the surfaces the tongue and lips need.
Dentures And Partial Dentures
Dentures can improve speech, but fit is everything. If a denture shifts when you talk, it may cause clicking, slipping, or a muffled sound—issues that often improve with adjustments, relines, or design changes.
When Speech Therapy Helps
If you have an established lisp, long-standing tooth loss, or you’re struggling to adapt after dental work, a speech-language pathologist can teach practical placement and airflow strategies. Dental treatment and speech therapy can work well together.
Can Tooth Loss Be Prevented
Not every case is preventable, but risk drops significantly with consistent home care and routine check-ups. Tooth decay, gum disease, trauma, and habits such as grinding are common contributors.
Brush twice daily with fluoride toothpaste, clean between teeth every day, and keep regular dental visits. If you play contact sports or grind your teeth at night, a mouthguard or night guard can also help protect your teeth.
FAQ
Can tooth loss affect speech?
Yes, tooth loss can cause lisping and difficulty pronouncing s, f, v, th.
Can dental problems cause speech problems?
Yes, pain, swelling, malocclusion, or ill-fitting dentures can impair clear speech.
Does tooth loss affect your voice?
Yes, missing teeth can alter articulation and airflow, subtly changing perceived voice.
Which teeth affect speech the most?
Front incisors and canines, plus upper front teeth, affect s, f, v, th sounds.
Can missing teeth cause speech problems?
Yes, missing teeth disrupt tongue placement and airflow, causing distortion of certain consonants.
Permanent Tooth Before Baby Tooth Falls Out | LYGOS DENTAL
Permanent Tooth Before Baby Tooth Falls Out
A permanent tooth can sometimes erupt behind a baby tooth before the baby tooth loosens. This “double row” (often called “shark teeth”) is usually caused by a baby tooth that hasn’t shed on time. Many cases self-correct as the baby tooth falls out, but a dentist should check for crowding, hygiene problems, or a bite issue.
Table of Contents
What This Situation Is Called
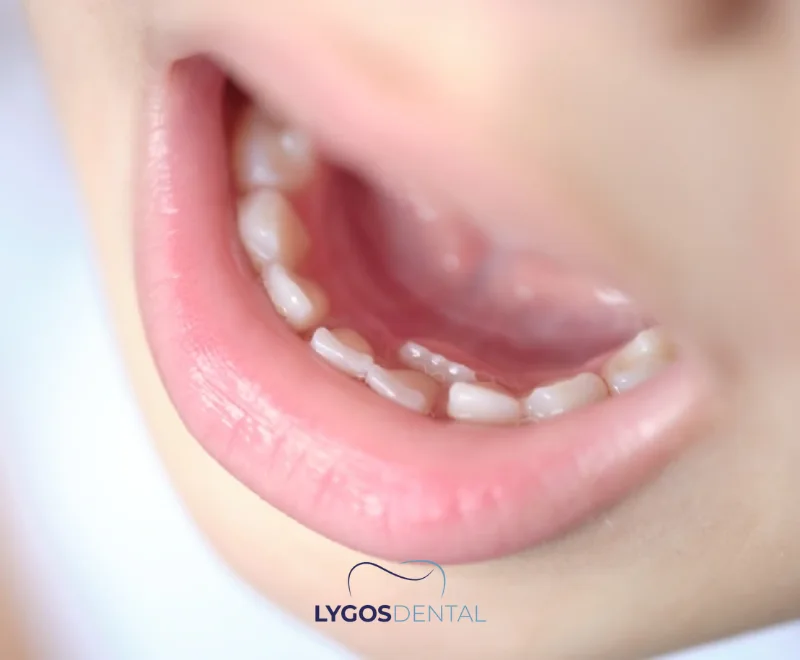
When a permanent tooth appears while the baby tooth is still in place, you may see two rows of teeth. Dentists often describe this as a retained baby tooth with an erupting permanent tooth; many parents know it as “double row teeth” or “shark teeth.” It is common around the lower front teeth, but it can happen anywhere in the mouth.
Normal Tooth Eruption Timeline in Children
Most children get their first baby teeth around 6 months of age, and the full set of 20 baby teeth is usually in place by about 2–3 years old. Permanent teeth commonly begin to come in around age 6 and continue to replace baby teeth through the early teen years. Because every child develops at a slightly different pace, the exact timing can vary.
Why a Permanent Tooth Can Come in Before the Baby Tooth Falls Out
In many cases, the permanent tooth is on schedule, but the baby tooth is not loosening as expected. Here are the most common reasons dentists see:
Genetics and Timing Differences
Eruption patterns often run in families. Some children naturally shed baby teeth later, even when the permanent tooth is ready to erupt.
A Baby Tooth That Is Not Loosening
If the root of the baby tooth does not dissolve on time, the tooth may stay firm in place. The permanent tooth then takes the path of least resistance and can come in behind or in front of it.
Decay, Trauma, or Infection in the Baby Tooth
Cavities or past injury can change how a baby tooth behaves as the permanent tooth approaches. A damaged baby tooth may become unstable, or swelling may alter the eruption path.
Limited Space in the Jaw
If there is not enough room, the permanent tooth may erupt out of line. Crowding is one reason the new tooth may appear behind the baby tooth instead of pushing it out normally.
Signs Parents Often Notice

A second tooth peeking through behind the baby tooth is the classic sign. You may also notice crowding, a tooth that looks rotated, or a baby tooth that does not wiggle even though a new tooth is visible. Mild tenderness can occur during eruption, but significant pain, swelling, or fever should be checked promptly.
What Can Happen If It Is Ignored
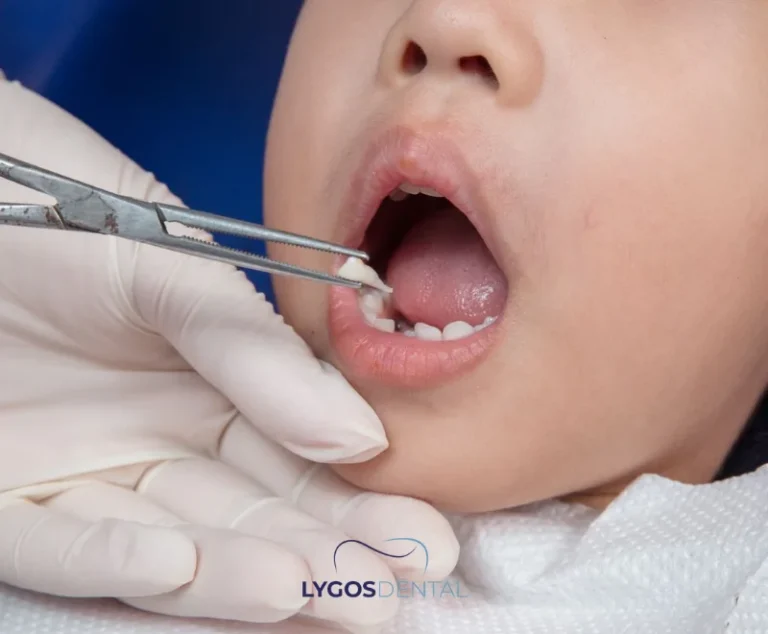
Some children will self-correct once the baby tooth finally falls out, especially if there is good space in the arch. If the baby tooth stays put, the permanent tooth can drift into the wrong position and make future alignment more difficult. Two rows of teeth can also trap food, raising the risk of cavities and gum irritation.
What a Dentist May Recommend
Treatment depends on the child’s age, how loose the baby tooth is, and whether the permanent tooth has room to move into place. A dentist may take an X‑ray to confirm the position of the teeth and the root of the baby tooth.
Watchful Waiting
If the baby tooth is already loose and there is space, the dentist may simply monitor it. Once the baby tooth comes out, the tongue and normal chewing forces often help guide the permanent tooth forward over time.
Removing the Baby Tooth
If the baby tooth is not loosening and it is blocking the permanent tooth, extraction may be recommended. This can reduce the chance of long‑term crowding and helps the permanent tooth move into a healthier position.
Orthodontic Guidance
If crowding is significant or the bite is affected, the dentist may refer your child for orthodontic evaluation. Early interceptive treatment can sometimes create space and reduce the need for more complex treatment later.
What You Can Do at Home
Keep brushing twice a day and pay extra attention to the area where the new tooth is erupting, since food can collect easily. If your child can floss, flossing between crowded teeth helps prevent cavities. Avoid wiggling a firm baby tooth aggressively; let a dentist decide when it is ready to come out.
When to Book a Dental Visit
Schedule an appointment if a permanent tooth is visible and the baby tooth is not loose, or if the tooth looks far out of line. Also seek care if there is swelling, persistent pain, bad taste, or bleeding gums. Early assessment is the best way to prevent crowding and protect the new permanent tooth.
FAQ
Is it normal for permanent teeth to come in before baby teeth fall out?
Yes, it’s common; permanent teeth may erupt before baby teeth shed (“shark teeth”).
What happens if an adult tooth comes in in front of a baby tooth?
It can cause double-row teeth and crowding; a dentist may remove the baby tooth.
What is the 7-4 rule for tooth eruption?
It means first teeth around 7 months, then about four new teeth every 4 months.
What should be done if permanent teeth come in behind baby teeth?
Encourage wiggling if loose; otherwise see a dentist for possible baby-tooth extraction.
How long can a baby tooth remain in place?
Up to age 12 is common; beyond that, evaluate for impaction or missing permanent tooth.
What causes permanent teeth to come in early?
Early eruption can be familial or linked to early baby-tooth loss, trauma, or endocrine disorders.
