Golden Ratio in Smile Design
Golden Ratio In Smile Design
In smile design, the golden ratio (about 1.618) is used as a visual guide for balancing the widths of the front teeth and how they sit within the lips and face. Dentists measure visible tooth proportions, gum symmetry, and smile line dynamics, then adjust shapes and spacing to create a natural, harmonious look that still fits the individual.
Smile design is a personalised plan that improves how the teeth, gums, and lips work together when you talk and smile. It combines aesthetics with function—so the result looks good, feels comfortable, and supports long-term oral health. The golden ratio is sometimes used during planning to check whether proportions look balanced to the eye.
What Is Smile Design?

Smile design is the process of planning an ideal smile in harmony with a person’s facial features, lip movement, and oral health. It often starts with photographs, short videos, and dental scans so the dentist can analyse tooth display, gum levels, and bite function.
Depending on the case, treatment may include whitening, porcelain veneers, zirconia crowns, orthodontic alignment, or gum contouring. The goal is proportional harmony: the front teeth should look like they belong to the face, not like a “one-size-fits-all” template.
What Is The Golden Ratio?
The golden ratio (approximately 1.618) is a mathematical proportion that appears in many natural patterns and has been used in art and design. In dentistry, it’s treated as a reference point for visual balance—helpful during planning, but not a strict rule that every smile must follow.
How Dentists Use Golden Ratio Measurements In The Face
Facial proportions influence how we perceive a smile. During smile design, clinicians may check broad facial relationships—such as facial height to width, midline alignment, and how the lips frame the teeth—before choosing tooth shapes and display.
Common facial guidelines that are sometimes compared with the golden ratio include:
- Facial length ÷ facial width ≈ 1.6
- Inter-pupillary distance ÷ eye width ≈ 1.618
- Nose width ÷ mouth width ≈ 1.618
- Forehead, midface, and lower-face thirds that are visually balanced
How The Golden Ratio Is Measured In Teeth
In smile design, golden ratio calculations are usually discussed for the visible widths of the upper front teeth when viewed from straight on. A commonly cited relationship is:
- Central incisor visible width = 1.0 unit
- Lateral incisor visible width ≈ 0.618 units
- Canine visible width ≈ 0.382 units
These numbers describe how the teeth appear across the smile, not their true anatomical widths. Because tooth rotation, arch form, and camera angle change what is “visible,” dentists treat this as a starting point rather than a target.
Example: If a central incisor appears 8.5 mm wide from the front, a lateral incisor might look about 5.3 mm (8.5 × 0.618) in the same view. The canine’s visible width would be smaller again, because the tooth sits further back in the arch.
What Elements Are Considered In Smile Design?

A complete smile design review looks beyond tooth size. Clinicians typically assess:
- Tooth colour and translucency (often supported by whitening before restorations)
- Tooth size, shape, and symmetry (including line angles and incisal edge position)
- Gum level and gum health (symmetry, inflammation control, and “gummy smile” factors)
- Lip shape and mobility (how much tooth shows at rest and during a full smile)
- Facial shape and smile arc (how the incisal edges follow the lower lip line)
- Age and gender expression preferences (softer vs sharper forms, when appropriate)
How The Golden Ratio Is Applied In A Smile Design Workflow

In modern practice, golden ratio checks are typically built into a broader digital workflow. A typical sequence looks like this:
- 1. Photography and measurements: facial and intraoral photos (often with video) plus digital scans.
- 2. Digital Smile Design (DSD): software simulation to test tooth proportions, midline, and smile arc.
- 3. Treatment planning: selection of procedures such as whitening, veneers, crowns, orthodontics, or gum reshaping.
- 4. Mock-up or trial smile: a temporary preview (when appropriate) to validate aesthetics and speech comfort.
- 5. Final delivery and follow-up: final restorations plus bite checks and hygiene guidance.
Where The Golden Ratio Helps—and Where It Doesn’t
The golden ratio can be useful for communicating “balance” between teeth, especially when planning veneer or crown widths. Still, research across different populations shows that naturally attractive smiles often do not match a single fixed ratio. That’s why many clinicians prefer flexible frameworks (such as percentages or recurring aesthetic proportions) over strict formulas.
For durable results, function and biology must lead the plan. Bite stability, enamel thickness, gum health, and restorative material limits will often set the boundaries for what is realistic—even if a ratio looks ideal on screen.
Golden Ratio In Smile Design FAQ
Why is the golden ratio used in smile design?
Because it provides a simple visual reference for harmony between the front teeth and the face. Used carefully, it can help guide tooth width dominance (central vs lateral vs canine) and support a balanced, natural look.
How is the golden ratio applied to the front teeth?
Clinicians measure the visible widths of the upper front teeth from a straight-on view and compare the proportions as the teeth move toward the corners of the smile. If changes are needed, they may adjust tooth shape, spacing, or alignment through orthodontics or restorations.
Do teeth need to be healthy before starting smile design?
Yes. Any active decay, gum disease, or bite instability should be treated first. Aesthetic dentistry lasts longer when the foundation—clean gums, stable bite, and good oral hygiene—is in place.
Is the golden ratio applied differently for men and women?
The mathematics do not change, but the design choices can. Some patients prefer softer contours and rounded line angles, while others prefer squarer forms and stronger definition. A good plan matches the person’s facial features and preferences rather than forcing a single template.
Laminate Veneer Prices
Laminate Veneer Prices In Turkey For 2026
In Turkey, laminate veneer prices in 2026 vary mainly by material (porcelain vs. e.max), the dentist’s experience, and how many teeth are treated. Many clinics quote roughly ₺9,500–₺26,400 per tooth, with premium cases sometimes higher. A clear treatment plan after an exam is the only way to get an exact figure.
What Is A Laminate Veneer?

A laminate veneer is a thin porcelain shell bonded to the front surface of a tooth to improve color, shape, or alignment. It’s commonly used for stains that don’t respond to whitening, minor chips, uneven edges, and small gaps. Because the veneer sits on the visible surface, it can deliver a natural look with minimal change to the tooth.
Who Is A Good Candidate?
Most patients with healthy enamel, stable gums, and good oral hygiene can be considered for laminate veneers. They may not be the best option if you have untreated gum disease, heavy tooth grinding, or large fillings that weaken the tooth. A clinical exam is essential, since the best plan depends on bite, enamel thickness, and the cosmetic goal.
How Laminate Veneers Are Applied

Treatment usually takes two or three visits. The exact steps depend on whether the case is ‘no-prep’, minimal-prep, or requires small reshaping for a clean fit.
Visit 1: Planning And Preparation
Your dentist evaluates your teeth and bite, discusses the shade and shape you want, and checks gum health. If needed, a very thin layer of enamel is removed to create space for the veneer. Digital scans or impressions are taken and sent to the lab, and temporary veneers may be placed in some cases.
Visit 2: Try-In And Bonding
Once the veneers are ready, your dentist tests the fit and color, then bonds them with dental adhesive systems designed for porcelain. The bonding stage is technique-sensitive and takes time, since each tooth is isolated and cured carefully. Many patients find the process comfortable; local anesthetic can be used if enamel preparation was done.
Advantages And Limitations
Laminate veneers are popular because they can look very natural when planned well. They also have limits, especially if you have habits that put extra force on the front teeth.
Main Advantages
- Natural aesthetics with strong control over shape and shade.
- Conservative approach when compared with full crowns, since less tooth structure is removed.
- Good color stability with quality porcelain and proper polishing.
- Fast cosmetic improvement once planning is complete.
Potential Disadvantages
- Veneers can chip or fracture with trauma, biting hard foods, or nail-biting.
- Costs are higher than many direct composite options.
- Not ideal for uncontrolled bruxism (teeth grinding) unless protective measures are used.
- Because the tooth surface is altered, the procedure is not reversible.
Are Laminate Veneers Permanent?
Laminate veneers are a long-term treatment, not a temporary cosmetic fix. Many last 10–15 years, and longer with good hygiene, regular checkups, and a stable bite. Avoiding edge-biting habits and using a night guard when recommended can make a major difference.
Laminate Veneer Prices In 2026
Prices vary widely between cities and clinics, so published ranges should be treated as a starting point. Your final quote depends on the plan for your smile, the material selected, and any extra treatments needed beforehand.
Typical Price Range Per Tooth
Across Turkish clinics, laminate veneer pricing in 2026 is often quoted in a broad band. Some clinics list porcelain laminate ranges around ₺9,500–₺13,000 per tooth, while premium ceramic options can reach ₺20,000+ per tooth. Examples of published clinic pricing place laminate veneer (yaprak porselen) figures up to roughly ₺26,400 per tooth in 2026.
What The Price Usually Includes
- Initial assessment and smile planning (varies by clinic).
- Tooth preparation when needed, plus digital scan or impression.
- Lab work for the veneer (material and technique affect cost).
- Bonding appointment and final bite checks.
- Short-term follow-up visits in the early adaptation phase (clinic-dependent).
Factors That Affect Laminate Veneer Costs
Two patients can receive the same number of veneers and still receive different quotes. These are the main cost drivers you should compare when choosing a clinic.
- Number of teeth: More units increase total cost, though package pricing is common for 6–10 teeth.
- Material choice: Standard porcelain, e.max (lithium disilicate), or other ceramics affect both aesthetics and price.
- Dentist’s expertise: Cosmetic specialists may charge more, especially for complex cases and shade matching.
- Clinic location and overhead: Larger cities and high-demand districts tend to be priced higher.
- Technology and lab standards: CAD/CAM workflows and premium lab work usually cost more.
- Extra treatments: Cleaning, gum therapy, whitening, or bite adjustments can add to the total.
Frequently Asked Questions
Who Is Suitable For Laminate Veneers?
Patients with healthy teeth and gums, adequate enamel, and realistic expectations are typically good candidates. If you grind your teeth, your dentist may recommend a night guard or a different treatment.
Why Do Prices Vary So Much?
The largest differences come from material type, lab quality, the dentist’s experience, and whether extra procedures are required. Published price lists are rarely final; a clinical exam and a written treatment plan provide the most reliable quote.
How Do You Care For Veneers?
Brush and floss daily, attend regular dental checkups, and avoid using your teeth as tools. If you bite hard foods with your front teeth, switch to cutting food into smaller pieces. When bruxism is present, wearing a night guard can protect veneers and natural teeth.
Aesthetic Dental Treatments Preferred by Celebrities
Aesthetic Dental Treatments Popular With Celebrities
Public figures often choose cosmetic dental treatments that look natural on camera and hold up under a busy schedule. The most common options include smile makeover planning (often called a Hollywood Smile), porcelain veneers, zirconia crowns, composite bonding, and professional whitening. The best choice depends on tooth health, bite, timeline, and the level of change you want.
What A Hollywood Smile Means In Dentistry

A “Hollywood Smile” is a smile makeover plan rather than a single treatment. Dentists combine a few procedures to improve tooth colour, symmetry, and gum balance while keeping the result believable up close and on screen.
Depending on the case, the plan may include whitening, veneers or crowns, minor alignment changes, and gum contouring. The goal is consistency: teeth that look evenly shaped and bright without appearing unnaturally flat or opaque.
Porcelain Veneers
Porcelain veneers are thin, custom-made shells bonded to the front of the teeth. They can change colour, shape, length, and the appearance of minor misalignment in a controlled way.
Veneers are popular for camera work because they resist staining better than many alternatives and can be designed to match facial features. With good oral hygiene, routine check-ups, and protection against grinding, porcelain veneers commonly last around 10–15 years, and sometimes longer.
Zirconia Crowns
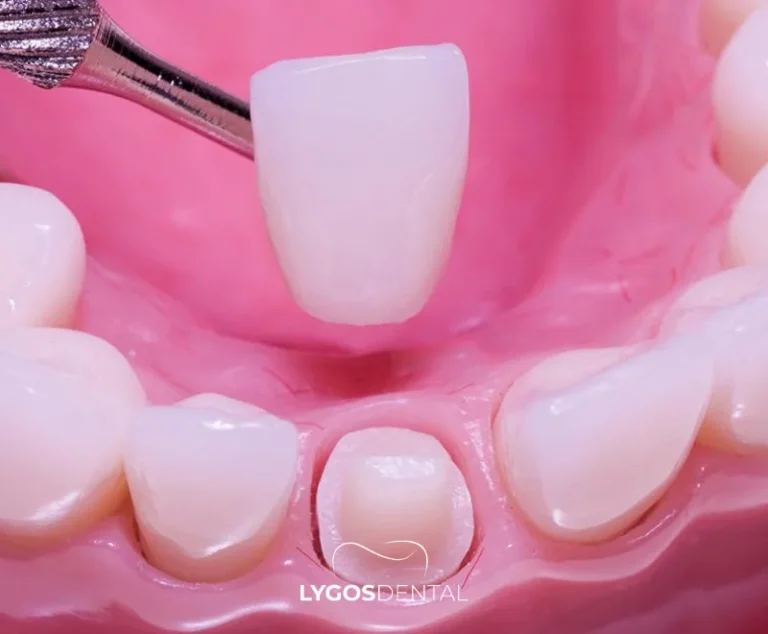
Zirconia crowns cover the entire tooth and are chosen when a tooth needs more structural support than a veneer can provide. They’re valued for strength and for a more natural look compared with older metal-backed crowns.
Modern zirconia materials can transmit light in a way that helps the restoration blend with natural enamel. Your dentist will choose the right type for the tooth position and your bite, since some versions prioritise durability over translucency.
Composite Bonding
Composite bonding uses a tooth-coloured resin to correct small cosmetic issues such as chips, fine cracks, uneven edges, or mild gaps. It’s a conservative option because it often requires little to no removal of natural tooth structure.
Bonding can be completed quickly, which is helpful when someone wants a visible improvement without a long treatment timeline. Like any cosmetic restoration, durability depends on bite forces, habits, and maintenance.
Professional Teeth Whitening
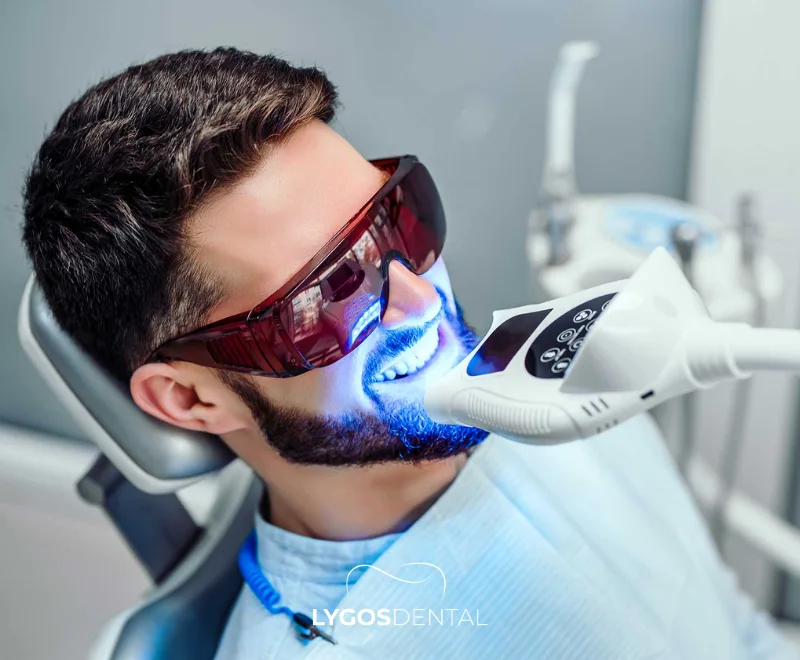
Professional whitening (bleaching) brightens natural tooth enamel using dentist-supervised gels, sometimes combined with light or laser systems. It’s one of the simplest ways to refresh a smile for events, filming, or photography.
Whitening works best for external staining and general yellowing. For deeper discolouration or older fillings and crowns that don’t change colour, your dentist may recommend a combination approach, such as whitening first and then matching restorations to the new shade.
What Celebrities And Public Figures Prioritise
Despite the headlines, most public-facing patients ask for the same things: a natural finish, predictable results, and a treatment plan that fits their schedule. The best cosmetic work is rarely “one-size-fits-all.”
Experienced clinicians usually start with oral health and bite stability, then plan the cosmetic changes. That may mean treating gum inflammation, addressing cavities, or managing grinding before committing to veneers or crowns.
Frequently Asked Questions
Which cosmetic dental treatments are most commonly requested?
Smile makeover planning (Hollywood Smile), porcelain veneers, zirconia crowns, composite bonding, and professional whitening are among the most requested options. Each one targets a different level of change, from subtle refinements to full smile redesigns.
What’s the difference between a Hollywood Smile and a single procedure?
A Hollywood Smile describes a customised plan that may combine multiple treatments. A single procedure, such as whitening or bonding, focuses on one issue and is usually quicker, but it can’t solve every aesthetic concern on its own.
Can these treatments work for anyone?
Many people are suitable candidates, but the right option depends on tooth health, gum condition, and bite forces. A clinical exam is essential, especially for patients with heavy grinding, untreated gum disease, or significant crowding.
How long do porcelain veneers last?
High-quality porcelain veneers commonly last around 10–15 years with proper care. Lifespan is strongly influenced by oral hygiene, regular dental visits, and habits like grinding or using teeth as tools.
How Should Dental Care Be Done in the Summer Months?
Summer Dental Care: How To Protect Teeth And Gums In Hot Weather
Quick answer: Summer heat, travel, and sugary drinks can make cavities and gum irritation more likely. Stay on track by drinking water often, brushing twice daily with fluoride toothpaste, flossing once a day, and limiting acidic or sugary beverages. After acidic foods or drinks, rinse with water and wait 30–60 minutes before brushing.
Why Summer Can Be Hard On Oral Health

Summer routines often include more snacks, iced drinks, and longer days out of the house. Those habits can raise your exposure to sugar and acid, which weakens enamel over time.
Hot weather also increases fluid loss. When you’re dehydrated, saliva flow may drop, leaving the mouth drier and less able to wash away acids and bacteria.
Daily Summer Oral Hygiene Basics
Hydrate To Prevent Dry Mouth
Water helps maintain saliva flow, which naturally protects enamel and supports healthy gums. Sip water throughout the day, especially after time in the sun, exercise, or air travel.
If your mouth still feels dry, sugar-free gum can help stimulate saliva. Persistent dry mouth is worth discussing with a dentist, especially if you notice bad breath or more sensitivity.
Brush And Floss Consistently
Keep the basics simple and non-negotiable, even on busy days:
- Brush for two minutes, morning and night, using a soft-bristled brush.
- Use fluoride toothpaste to strengthen enamel.
- Clean between teeth daily with floss or interdental brushes.
- If you use mouthwash, choose a fluoride option and use it at a different time than brushing.
Timing Matters After Acidic Foods And Drinks
Cold sodas, citrus juices, sports drinks, and many iced coffees are acidic. Acid softens enamel for a short time, so brushing right away can be too abrasive.
Rinse with water first, then wait at least 30 minutes (up to an hour after very acidic drinks) before brushing.
Smarter Choices For Summer Drinks
Frequent sipping is tougher on teeth than having a drink with a meal. The mouth stays acidic longer, which increases the risk of enamel wear and decay.
To reduce damage when you do have sugary or acidic drinks:
- Use a straw to limit contact with teeth, especially for iced coffee and soda.
- Avoid slowly sipping over long periods; finish the drink in a shorter window.
- Rinse your mouth with water afterward.
- Choose water, milk, or unsweetened options more often.
Ice Cream And Sweets Without The Damage

Ice cream and summer desserts often combine sugar with cold temperatures, which can trigger sensitivity and feed decay-causing bacteria.
Practical ways to lower the risk:
- Enjoy sweets with a main meal rather than grazing between meals.
- Drink water afterward to help neutralize acids and rinse sugar away.
- Wait 30–60 minutes before brushing if the dessert was acidic or very sugary.
- Pick smaller portions or less frequent treats when possible.
Keeping Up With Brushing While Traveling
Vacations can disrupt routines, so make oral care easy to follow. Pack your kit where you can see it, like the top of your toiletry bag.
Helpful habits on the road:
- Keep a travel toothbrush and toothpaste in your day bag for long outings.
- Set a nightly phone reminder so brushing doesn’t get skipped.
- For children, use a simple reward chart or a short song timer to keep brushing consistent.
If you’re leaving for a long trip, a dental check-up beforehand can prevent surprises like a lost filling or a flare-up of sensitivity.
Travel Oral Care Kit Checklist
A small, well-chosen kit makes it easier to keep your mouth healthy away from home:
- Compact soft-bristled toothbrush (plus a spare, if possible)
- Fluoride toothpaste (travel size)
- Floss or interdental brushes
- Travel case to keep the brush dry and clean
- Fluoride mouthwash (optional, used separately from brushing)
- Sugar-free gum for dry mouth days
Frequently Asked Questions
Why Do Teeth Seem To Decay Faster In Summer?
Sugar and acid show up more often in summer diets—think sodas, fruit juices, and desserts. Heat and dehydration can also reduce saliva, which normally helps neutralize acids and control bacteria.
How Can I Avoid Forgetting To Brush On Vacation?
Pack travel-size essentials and keep them visible. A simple reminder on your phone helps, and brushing right after dinner can be easier than waiting until you’re exhausted at bedtime.
Does Ice Cream Harm Teeth?
Ice cream can contribute to cavities because it contains sugar, and the cold can trigger sensitivity in already exposed or worn enamel. Enjoying it with meals and rinsing with water afterward helps reduce the impact.
Does Sunbathing Affect Oral Health?
Sunbathing itself doesn’t damage teeth, but dehydration from long hours in the sun can lead to dry mouth. Drinking water regularly helps protect saliva flow and lowers the risk of bad breath and irritation.
Why Do Teeth Get Stained?
Why Do Teeth Get Stained?
Teeth stain when pigments from food, drinks, and tobacco cling to the enamel, or when changes happen inside the tooth, such as medication-related discoloration, fluorosis, trauma, or natural enamel thinning with age. Surface stains often improve with professional cleaning or whitening, while deeper stains may need cosmetic dental treatment.
What A Tooth Stain Is
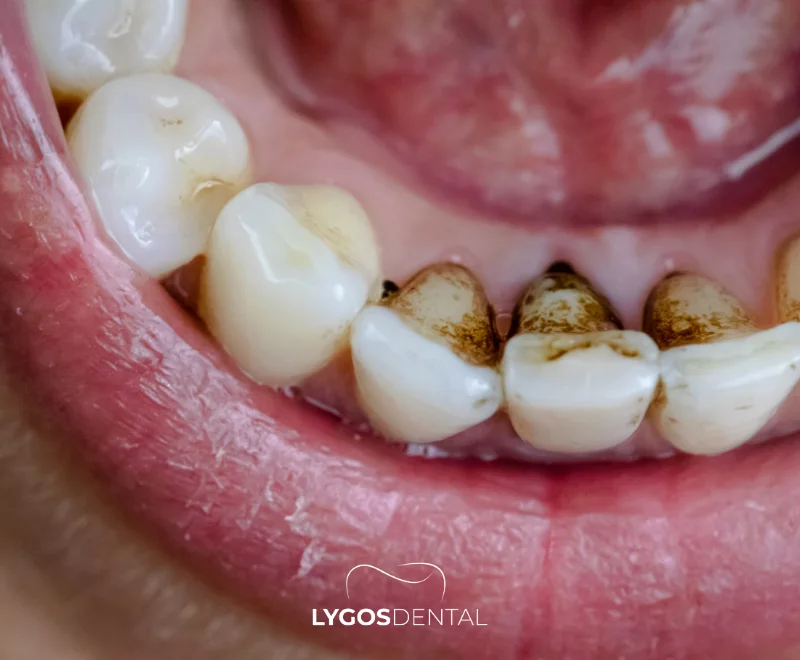
A tooth stain is a change in tooth color that affects the enamel surface or the layers beneath it. Stains can look yellow, brown, gray, or almost black, and they may appear evenly or as patches. Some discoloration is purely cosmetic, but sudden or uneven changes can also point to enamel wear or decay.
Main Reasons Teeth Get Stained
Most staining falls into two categories: extrinsic (on the surface) and intrinsic (within the tooth). Understanding the difference helps you choose the right solution and avoid wasting money on treatments that won’t work for your stain type.
Extrinsic Stains
Extrinsic stains sit on the enamel and are usually linked to daily habits. Dark beverages and tobacco are the usual culprits, but heavily pigmented foods can contribute too. These stains often respond well to professional cleaning and dentist-supervised whitening.
- Coffee and tea (tannins and dark pigments bind to enamel)
- Red wine and cola
- Berries, curries, tomato-based sauces, and other strongly colored foods
- Smoking and other tobacco use (nicotine and tar leave persistent yellow-brown buildup)
Intrinsic Stains
Intrinsic stains form below the enamel, inside the tooth structure. They may appear as overall darkening, gray tones, or bands, and they typically don’t lift with over-the-counter whitening products. A dentist can confirm the cause and recommend options such as internal bleaching, bonding, veneers, or crowns.
- Certain antibiotics during tooth development (for example, tetracycline)
- Excess fluoride exposure while teeth are forming (fluorosis)
- Dental trauma that affects the tooth’s internal tissues
- Developmental enamel defects or inherited factors
Common Types Of Tooth Discoloration
The color and pattern can give clues about the cause, although a dental exam is the best way to confirm it.
- Yellowing: Often linked to enamel thinning with age, revealing the naturally darker dentin underneath
- Brown stains: Common with coffee, tea, and tobacco; can also appear where plaque collects
- Black stains: May be associated with heavy tobacco use, long-term buildup, or certain bacteria in plaque
- White spots: Can be fluorosis or early demineralization (sometimes the first stage before a cavity)
How Tea, Coffee, And Tobacco Contribute

Tea and coffee contain tannins that help pigments stick to enamel. Over time, those pigments build up, especially in grooves and between teeth. Tobacco stains tend to be tougher because tar and nicotine form a sticky film that attracts more discoloration and plaque.
Are Tooth Stains Permanent?
Some stains are temporary, while others are stubborn. Surface stains are often removable with a professional scale and polish, and many people see additional improvement with dentist-supervised whitening. Intrinsic stains can be long-lasting, but cosmetic dentistry offers effective ways to mask or correct them.
How To Prevent Tooth Stains
Prevention is usually easier than reversal. A few consistent habits can reduce staining without changing your diet dramatically.
- Brush twice a day with fluoride toothpaste and clean between teeth daily
- Rinse with water after coffee, tea, or deeply colored foods
- Use a straw for cold, dark beverages to limit contact with front teeth
- Avoid brushing immediately after acidic drinks; wait about 30 minutes to protect enamel
- Limit tobacco use or quit for the biggest long-term improvement
- Book routine dental cleanings as recommended by your dentist
Treatment Options That Actually Work
The best treatment depends on whether the stain is surface-level or internal. If you’re unsure, a quick dental check can prevent wasted time and sensitivity from unnecessary whitening products.
- Professional cleaning: Removes plaque and many surface stains
- Dentist-supervised whitening: Stronger and more predictable than most at-home kits
- Bonding or veneers: Covers discoloration and can also improve shape
- Crowns: Used when a tooth is heavily damaged or discolored
Frequently Asked Questions
Do Tooth Stains Go Away On Their Own?
Usually not. Some mild surface discoloration can fade if you stop the habit causing it, but most stains need cleaning or whitening to improve.
Why Do Children Get Tooth Stains?
Common reasons include plaque buildup, certain medications, and fluoride exposure while teeth are developing. A pediatric dentist can identify the cause and advise safe treatment.
Do Stains Cause Cavities?
Stains don’t directly create cavities. Still, the buildup that causes staining—like plaque—can raise the risk of decay if it isn’t removed regularly.
Is Whitening With Lemon Or Baking Soda Safe?
No. Acid and abrasives can wear enamel, increase sensitivity, and make teeth look more yellow over time. Dentist-guided options are safer and more reliable.
Which Foods And Drinks Stain Teeth Most?
Coffee, tea, red wine, cola, berries, and richly colored sauces are frequent causes. Consuming them less often, rinsing with water, and keeping up with cleanings can make a noticeable difference.
How Can Fear of The Dentist be Overcome?
How Can Fear Of The Dentist Be Overcome?
Fear of the dentist can be reduced by understanding what triggers your anxiety, choosing a dentist who explains each step, and using practical calming techniques before and during appointments. Modern pain-control methods, gradual exposure, and therapy such as CBT can help. For severe phobia, sedation may be an option after clinical assessment.
Table of Contents
Why Dental Fear Happens
Dental fear ranges from mild nervousness to dental phobia, where people avoid care even when they are in pain. It often builds after one bad experience, but it can also develop without a clear trigger.
Common triggers include:
- Past painful or distressing treatment experiences.
- Expectation of pain based on old beliefs, social media, or stories from friends and family.
- Feeling a loss of control while lying back in the chair.
- Embarrassment or shame about oral health, especially after delayed checkups.
- Sensitivity to sounds, smells, or the sight of dental instruments.
Signs And Symptoms Of Dental Phobia
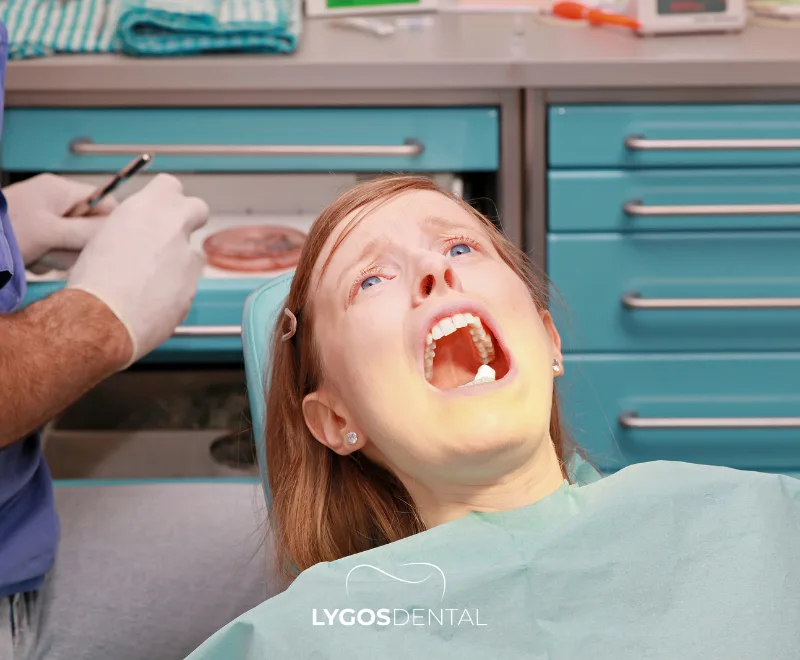
Dental anxiety can show up in the body, in thoughts, and in behavior. When it starts affecting sleep, daily life, or keeps you from seeking care, it is worth addressing directly.
- Nausea, sweating, trembling, or a racing heartbeat before an appointment.
- Panic-like feelings in the waiting room or when sitting in the chair.
- Repeatedly canceling or postponing visits.
- Avoiding the dentist even as tooth or gum problems get worse.
- Difficulty sleeping because you are anticipating treatment.
How Dental Anxiety Starts In Children
Many adult fears begin early. A child’s first dental visits, and the way adults talk about dentistry, can shape long-term attitudes toward care.
In children, fear often develops from:
- Parental anxiety or negative comments about dentists.
- A painful first experience or a rushed appointment.
- Arriving without preparation, so the child does not know what to expect.
- Using the dentist as a threat (for example, “If you misbehave, you’ll go to the dentist”).
Supportive language, short introductory visits, and a calm parent in the room can prevent fear from taking hold. If a child is very anxious, ask the dental team about child-friendly approaches and pacing.
Practical Ways To Reduce Dental Anxiety

What you do before the appointment often matters as much as what happens in the chair.
Before your visit
- Choose a dentist who is comfortable treating anxious patients and is willing to answer questions.
- Book an early-day appointment so you spend less time anticipating it.
- Ask for a step-by-step explanation and agree on a stop signal (such as raising your hand).
- Avoid caffeine on the day of the visit if it increases your jitters.
- Practice slow breathing for a few minutes before you arrive.
During treatment
- Use paced breathing: inhale through the nose, exhale slowly through the mouth.
- Bring headphones or listen to calming audio if the clinic allows it.
- Ask for short breaks so you do not feel trapped.
- Tell the dentist where you feel sensitive; numbing can be adjusted.
Evidence-based psychological approaches
For persistent or severe anxiety, psychological strategies can make a lasting difference, especially when paired with a supportive dental team.
- Cognitive Behavioral Therapy (CBT): helps reframe catastrophic thoughts and builds coping skills.
- Graded exposure: gradual steps such as a clinic visit, a short exam, then a simple procedure.
- Relaxation training: breathwork, progressive muscle relaxation, or brief mindfulness exercises.
- Desensitization: getting used to triggers like the sound of instruments in a controlled way.
Modern Options That Make Treatment More Comfortable
Dentistry has changed a lot. Many clinics now use techniques that reduce discomfort and shorten treatment time, which can be reassuring if you have had older, painful experiences.
Examples you can ask about include:
- Laser dentistry for selected procedures, which may reduce noise and vibration compared with traditional drilling.
- Needle-free anesthetic systems offered by some clinics for certain cases (availability varies).
- Digital impressions with 3D scanners instead of traditional impression trays.
Sedation And General Anesthesia

When fear is intense, sedation can help you get essential care while staying calmer. Your dentist will review your medical history and explain benefits and risks before recommending any option.
Common approaches
- Sedation: you remain responsive but deeply relaxed, and you may remember little of the procedure.
- General anesthesia: you are fully asleep; it is typically reserved for specific situations and requires an appropriately equipped setting and qualified professionals.
If you are considering sedation or general anesthesia, discuss the plan in detail, including monitoring, recovery time, and whether you will need someone to take you home.
When To Get Extra Support
If you avoid dental care for years, have panic attacks, or feel unable to sit through even an exam, consider asking for help beyond self-management. A dentist experienced with anxious patients, a therapist, or both can work together so you can receive care without feeling overwhelmed.
Frequently Asked Questions
How do I get over my fear of the dentist?
Use gradual exposure, discuss fears, choose a gentle dentist, and practice relaxation techniques.
How do you treat dental fear?
Treat with education, behavioral therapy, desensitization, supportive communication, and sedation when appropriate.
What phobia is the fear of dentists?
Dental phobia is called odontophobia.
Is it common to be scared of the dentist?
Yes, dental anxiety is common, affecting many children and adults.
What can I take to calm my nerves before a dentist?
Ask your dentist about nitrous oxide or a prescribed anxiolytic; avoid alcohol.
Things You Need to Know Before Getting Braces
Things You Need To Know Before Getting Braces
Braces straighten teeth and improve how your bite works, which can make cleaning easier and reduce uneven wear over time. Before starting, you’ll need an orthodontic exam to confirm the problem, choose the right appliance (metal, ceramic, lingual, or clear aligners), and treat any cavities or gum issues. Good hygiene and regular checkups are key to a smooth result.
A straight smile isn’t only about appearance. When teeth and jaws don’t line up well, you may be more prone to plaque buildup, gum irritation, or uneven tooth wear. Orthodontic treatment can address both cosmetic and functional concerns, but it works best when you know what to expect from day one.
Who Can Get Braces

Braces can be an option for children, teens, and adults. What matters most is your dental development, jaw alignment, and overall oral health. An orthodontist will check your teeth, gums, and bite, then recommend a plan that matches your needs and lifestyle.
Braces are commonly recommended for:
- Children (often when most adult teeth have erupted, commonly around ages 9–14)
- Teenagers
- Adults of any age
- People with healthy teeth and a stable jaw structure
- Patients whose gums are free from active disease
When Braces Are Recommended
Orthodontic treatment is used to correct bite problems and alignment issues. Some people start for cosmetic reasons, but many cases also have a functional goal—helping the teeth meet properly and reducing strain on certain teeth or jaw areas.
Common reasons an orthodontist may recommend braces include:
- Crowded, rotated, or misaligned teeth
- Gaps between teeth (diastema)
- Bite problems such as open bite, deep bite, crossbite, or underbite
- Protruding or recessed front teeth
- Wear patterns linked to an uneven bite
- Changes related to habits such as thumb-sucking or long-term mouth breathing
Types Of Braces
There are several orthodontic options today. The best choice depends on how complex your case is, how visible you want the appliance to be, and whether you can follow daily wear instructions for removable systems.
Metal Braces
The classic option. Metal brackets are durable, effective for a wide range of cases, and often the most budget-friendly choice.
Ceramic (Clear) Braces
Tooth-colored brackets that are less noticeable than metal. They can be a good fit for adults who want a subtler look, though they may require a bit more care to avoid staining.
Lingual Braces
Placed on the back of the teeth, so they’re hidden from view. They can be helpful for people who want an invisible option, but they may take longer to get used to and can be harder to clean.
Clear Aligners (For Example, Invisalign®)
Removable trays that gradually move teeth. They’re discreet and can be easier for brushing and flossing, but they only work well when you wear them as directed and attend regular follow-ups. They’re typically best for mild to moderate corrections.
How Long Braces Treatment Takes
Treatment time varies from person to person. Your orthodontist will estimate a timeline after reviewing your bite, the amount of movement needed, and your overall dental health.
Typical ranges are:
- Mild cases: about 6–12 months
- Moderate cases: about 12–18 months
- More complex cases: 24 months or longer
What can affect the timeline:
- Age and how your teeth respond to movement
- Severity of crowding or bite problems
- Keeping appointments for adjustments or new aligners
- Daily habits, including oral hygiene and following wear instructions
Checklist Before Your Braces Go On
Starting with a healthy mouth makes treatment easier and lowers the risk of complications. Your dentist or orthodontist may coordinate a few steps before placement.
- Professional cleaning to remove plaque and tartar
- Treating cavities before brackets or aligners begin
- Addressing gum inflammation or periodontal issues
- Planning for diet changes (hard, sticky, and crunchy foods can damage brackets and wires)
- Setting expectations: mild soreness is common in the first days, and progress takes time
Caring For Braces After Placement

Daily care plays a major role in how your teeth look when the braces come off. Good hygiene helps prevent white spot lesions, cavities, and gum irritation during treatment.
- Brush carefully after meals and before bed; take extra time around brackets and the gumline
- Use interdental brushes, floss threaders, or a water flosser to clean between teeth
- Avoid foods that can bend wires or break brackets (ice, hard nuts, sticky candy, chewing gum)
- Attend scheduled adjustment visits so your orthodontist can keep teeth moving safely
- If you play contact sports, wear a mouthguard designed for braces
If you feel sore after an adjustment, soft foods and orthodontic wax can help. Over-the-counter pain relief may be an option if it’s safe for you—follow label directions and your clinician’s advice.
Frequently Asked Questions
Does getting braces hurt?
You won’t feel pain while they’re being placed. It’s normal to feel pressure or soreness for a few days afterward and after adjustments. Most people adapt within a week.
Should cavities be treated before getting braces?
Yes. Cavities and active gum problems should be treated first. Braces make some areas harder to clean, so starting with healthy teeth lowers the risk of decay during treatment.
What affects the cost of braces?
Price depends on the type of appliance, how long treatment lasts, case complexity, and where you receive care. Clear aligners and lingual braces tend to cost more than standard metal braces in many clinics.
Will braces affect my speech?
Traditional braces usually cause minimal speech changes. You may notice a short adjustment period with lingual braces or clear aligners, but most people adapt quickly with practice.
How Does Diet Affect Dental Health?
How Does Diet Affect Dental Health?
Diet affects dental health by changing how often your teeth face acid attacks and whether your body gets the minerals and vitamins needed to maintain enamel and healthy gums. Sugary and acidic foods feed bacteria and lower mouth pH, raising cavity risk—especially with frequent snacking. Calcium, phosphorus, vitamin D, and vitamin C support stronger teeth and gum tissue.
Oral health is closely tied to everyday eating and drinking habits. The foods you choose, the drinks you sip, and how often you snack all influence enamel strength, saliva flow, and the bacteria that cause tooth decay. Small changes at the table can make a noticeable difference at the dentist.
What Is The Relationship Between Diet And Dental Health?

Teeth are living structures supported by minerals and nutrients from your diet. Enamel relies on a steady supply of calcium and phosphorus, while vitamin D helps your body absorb and use these minerals effectively. Gum tissue benefits from vitamin C and protein, which support collagen and healing.
Food timing matters as much as food choice. Each time you eat or drink something with fermentable carbs (like sugar or refined starch), bacteria can produce acids that soften enamel. When you graze throughout the day, your mouth gets less recovery time, so enamel stays under stress longer.
How Do Sugary Foods Harm Teeth?
Mouth bacteria thrive on sugar. As they break it down, they release acids that pull minerals out of enamel. Over time, repeated acid exposure can lead to white spots, sensitivity, and cavities.
Some options are tougher on teeth because they combine sugar with acidity or stickiness. Sodas, sports/energy drinks, sweetened iced teas, and packaged fruit juices can bathe teeth in acid. Sticky sweets, dried fruit, and chewy candies cling to enamel and keep fueling bacteria.
Why Snacking Frequency Matters

It’s not only the amount of sugar—it’s the number of times teeth are exposed. Frequent snacking keeps mouth pH low for longer periods. Saliva needs time to neutralize acids and start remineralizing enamel.
If you snack, keep it structured. Aim for tooth-friendlier options and avoid slowly sipping sweet drinks over hours. Water between meals helps rinse away food particles and supports a healthier pH balance.
Foods And Drinks That Support Dental Health
A tooth-supportive diet focuses on minerals, vitamins, and foods that stimulate saliva.
- Dairy or fortified alternatives (milk, yogurt, cheese): calcium and phosphorus to support enamel.
- Leafy greens (spinach, kale): minerals plus antioxidants.
- Eggs and oily fish (salmon, sardines): vitamin D and protein.
- Nuts, beans, and lean meats: phosphorus, protein, zinc, and iron to support oral tissues.
- Crunchy produce (apples, carrots, celery): fiber that helps mechanically clean teeth and boosts saliva.
- Water: rinses the mouth and helps dilute acids.
Can Poor Nutrition Lead To Dental Problems?
Yes. Diets low in key nutrients can weaken enamel and reduce the mouth’s ability to repair itself. Low vitamin D or calcium intake may affect mineral support for teeth, while low vitamin C can make gums more prone to bleeding and slower to heal.
When protein intake is consistently low, immune defenses can suffer, which may increase the risk of oral infections. Iron and zinc deficiencies may also be linked with mouth sores or altered taste in some people.
Children, older adults, and people with restricted diets benefit from extra attention to nutrient intake and regular dental checkups.
Which Foods Should Be Limited For Gum Health?
Gum health depends on stable blood flow, low inflammation, and good daily plaque control. Certain foods and drinks can make that harder by increasing acid exposure or promoting plaque buildup.
Try to limit:
- Acidic drinks such as soda, cola, energy drinks, and frequent citrus juices.
- Refined carbohydrates (white bread, chips, crackers, cookies) that break down into sugars quickly.
- Sticky sweets and frequent grazing on sugary snacks.
- Very salty processed foods that can contribute to dry mouth in some people.
Severe gum disease has been associated with chronic conditions like diabetes and cardiovascular disease, so protecting gum health is part of looking after overall wellbeing.
What Should You Eat For Healthy Teeth?

Brushing and flossing are essential, but diet helps set the baseline for how resilient your teeth and gums are. A practical approach is to build meals around nutrient-dense foods and keep sugary exposure predictable and limited.
A tooth-friendly plate often includes:
- Calcium-rich foods (milk, yogurt, cheese, calcium-fortified alternatives).
- Vitamin D sources (egg yolks, salmon, sardines, fortified foods) to support calcium use.
- Vitamin C sources (citrus, kiwi, berries, bell peppers) to support gum tissue.
- Fiber-rich fruits and vegetables to boost saliva and reduce food residue.
- Water as the default drink.
If you want something sweet, having it with a meal is usually better than nibbling over a long period. Afterward, rinse with water. If brushing isn’t possible right away, sugar-free gum (especially xylitol-sweetened) can stimulate saliva.
Simple Daily Habits That Protect Your Mouth
- Keep sweet drinks occasional, and avoid sipping them slowly over time.
- Choose snacks that don’t cling to teeth (cheese, nuts, plain yogurt, fresh fruit).
- Wait 30 minutes after acidic foods or drinks before brushing to avoid brushing softened enamel.
- If you have dry mouth, speak with a dentist or doctor—medications and dehydration can play a role.
How Does Diet Affect Dental Health? Frequently Asked Questions
Does Diet Really Affect Tooth Decay?
Yes. Tooth decay is driven by repeated acid exposure created when bacteria metabolize sugars and refined carbs. Higher frequency of sugary or acidic foods and drinks increases risk, especially when oral hygiene and fluoride exposure are limited.
Which Vitamins And Minerals Are Most Important For Dental Health?
Calcium and phosphorus help maintain enamel, and vitamin D supports how your body uses those minerals. Vitamin C supports gum tissue and healing. Vitamin A and several B vitamins also play roles in oral tissue health and immune function.
Are “Sugar-Free” Snacks Always Safe For Teeth?
Not always. Some sugar-free products still contain fermentable starches that can turn into acids in the mouth. Look for snacks that are low in added sugars and don’t stick to teeth. If chewing gum, xylitol-sweetened options are generally considered tooth-friendlier.
How Much Water Should I Drink For Better Oral Health?
Hydration needs vary by body size, activity, and climate. Many public health guidelines suggest roughly 6–8 cups of fluids a day for most adults, and a useful rule of thumb is aiming for pale yellow urine. From an oral health perspective, choosing water often—and using it to rinse after meals—helps reduce acid and food residue.
How Do Dairy Products Help Teeth?
Milk, yogurt, and cheese provide calcium and phosphorus, which help maintain enamel mineral balance. Cheese can also stimulate saliva, supporting a healthier mouth pH after eating.
Is Fluoride Toothpaste Harmful?
Is Fluoride Toothpaste Harmful?
Fluoride toothpaste is considered safe for most people when used as directed. It strengthens enamel, helps reverse early decay, and lowers cavity risk. Problems usually come from frequent swallowing or long-term excessive fluoride exposure, which can cause mild dental fluorosis in young children. Use the right amount for age and spit after brushing.
Oral health is closely linked to overall health, and fluoride toothpaste is one of the most widely used tools for preventing tooth decay. Still, you may have seen concerns online about fluoride’s safety. The real question isn’t whether fluoride exists in toothpaste, but whether it’s used in the right way and dose.
What Is Fluoride?

Fluoride is a naturally occurring mineral found in water, soil, and some foods. In dentistry, it’s valued because it helps the outer layer of the tooth (enamel) resist acid attacks from plaque bacteria and sugar.
Does Fluoride Toothpaste Work?
Yes. Research consistently shows that brushing with fluoride toothpaste reduces cavities. Fluoride supports remineralization (repair of early enamel damage) and makes enamel more resistant to future demineralization.
Over-the-counter toothpastes commonly contain about 1,000–1,500 ppm fluoride, a range considered effective for cavity prevention.
Benefits Of Fluoride Toothpaste

Strengthens tooth enamel
Fluoride integrates with enamel and helps it withstand acids produced after eating or drinking sugary foods.
Helps prevent cavities
By slowing demineralization and supporting repair, fluoride lowers the chance that early weak spots develop into cavities.
Supports remineralization
Early enamel changes can often be stabilized when fluoride is available regularly through brushing.
May reduce sensitivity in some formulas
Certain fluoride toothpastes are designed to help protect exposed areas, which can reduce sensitivity for some people.
What Are The Risks Of Too Much Fluoride?
Like many helpful ingredients, fluoride can cause problems when intake is excessive. With toothpaste, the main risk is repeated swallowing by young children or very frequent use of high‑fluoride products without professional guidance.
Dental fluorosis
During tooth development (typically in early childhood), swallowing too much fluoride over time can lead to dental fluorosis. Mild fluorosis often appears as faint white streaks or spots and is mainly cosmetic.
Stomach upset from swallowing toothpaste
Swallowing large amounts of toothpaste at once may cause nausea, vomiting, or stomach pain. This is one reason adult supervision matters for young children.
High‑fluoride toothpaste without dental advice
Prescription-strength toothpastes may contain much higher fluoride levels (for example, 5,000 ppm) and are intended for people at higher cavity risk. These should be used only when recommended by a dentist.
Is Fluoride Toothpaste Safe For Children?

In general, yes—when the amount matches the child’s age and brushing is supervised. Many dental and public health bodies advise using fluoride toothpaste from the eruption of the first tooth, while focusing on minimizing swallowing.
Recommended amount by age
- Under age 3: use a smear the size of a grain of rice.
• Ages 3–6: use no more than a pea-sized amount.
• Under age 2: ask your dentist or doctor for guidance, especially if your child is likely to swallow toothpaste.
Practical tips for parents
Help your child brush, keep toothpaste out of reach between uses, and encourage spitting rather than rinsing and swallowing. If your child repeatedly swallows toothpaste, speak with a pediatric dentist about the best approach for your situation.
How To Use Fluoride Toothpaste Safely
- Use the right amount. More foam doesn’t mean better cleaning.
- Brush twice daily for about two minutes and spit out afterward.
- Supervise young children to prevent swallowing.
- Check the label for fluoride concentration. For everyday cavity protection, many products are in the 1,000–1,500 ppm range.
- Ask your dentist before using high‑fluoride products or if you have a history of frequent cavities.
Bottom Line
Fluoride toothpaste is not harmful for most people when used correctly. It remains one of the simplest, best-supported ways to protect enamel and reduce cavities. The key is dosage—especially for young children—and using higher-strength products only under professional guidance.
Frequently Asked Questions
What is fluoride toothpaste?
Fluoride toothpaste contains fluoride compounds that help strengthen enamel and reduce the risk of tooth decay when used regularly.
Is fluoride toothpaste harmful?
Not when used as directed. The main concerns involve swallowing toothpaste frequently (especially in young children) or using high‑fluoride products without dental advice.
Can children use fluoride toothpaste?
Yes, with age-appropriate amounts and adult supervision. Use a rice-grain smear under age 3 and a pea-sized amount from ages 3–6.
What happens if too much fluoride is ingested?
Over time, excess swallowed fluoride in early childhood can cause dental fluorosis. Swallowing a large amount at once can also cause stomach upset.
Does Nighttime Teeth Grinding Break Teeth?
Does Nighttime Teeth Grinding Break Teeth?
Yes—nighttime teeth grinding (sleep bruxism) can damage teeth over time. Repeated clenching and grinding may wear down enamel, create small cracks, and break dental work like fillings or crowns. In more severe cases, teeth can chip or fracture. Early signs and a dentist‑made night guard can help prevent permanent damage.
What Nighttime Teeth Grinding Is

Nighttime teeth grinding is a form of bruxism that happens during sleep. Many people aren’t aware they do it until a partner hears grinding sounds or a dentist notices wear.
Sleep bruxism can range from occasional clenching to frequent grinding episodes. When it happens regularly, the jaw muscles and teeth absorb forces that are higher and longer-lasting than normal chewing.
Can Sleep Bruxism Crack Or Break Teeth?
It can. Repeated pressure can flatten biting surfaces, expose dentin, and make teeth more sensitive. Over time, that stress may lead to enamel cracks, chips, or fractures—especially if a tooth already has a large filling or a weak cusp.
Bruxism can also damage dental work. Fillings may loosen or crack, crowns can chip, and veneers may fail. If you’ve invested in restorative work, protecting it is a big reason to address grinding early.
Signs You Might Be Grinding At Night
Sleep bruxism often shows up through symptoms rather than obvious awareness. Common signs include:
- Jaw or facial muscle soreness when you wake up
- Morning headaches, especially around the temples
- Tooth sensitivity (hot, cold, or sweet)
- Flattened, chipped, or worn-looking teeth
- Pain or pressure near the ears
- A partner hearing grinding or clicking sounds during sleep
Common Causes And Risk Factors

Bruxism doesn’t have a single cause. For many people, several factors stack together.
Stress and anxiety
High stress can increase clenching, both during the day and at night. People often notice flare-ups during busy periods or after major life changes.
Sleep disruption
Sleep problems such as snoring or obstructive sleep apnea may be linked with sleep bruxism. If you also wake up tired, gasp, or snore loudly, it’s worth mentioning to a clinician.
Bite and dental factors
A misaligned bite, missing teeth, or poorly fitting restorations can contribute to jaw strain in some cases. Your dentist can assess whether your bite needs adjustment.
Medications and health conditions
Certain medications and neurological conditions have been associated with bruxism. If grinding started after a medication change, discuss it with the prescribing clinician rather than stopping it on your own.
What To Do If You Suspect Bruxism

Start with a dental exam. Dentists look for wear patterns, cracks, gum recession, and changes in the jaw muscles.
Treatment is usually aimed at protecting teeth and reducing triggers. A plan may include:
- A custom night guard (occlusal splint) to separate the teeth and reduce damage
- Repairing cracked teeth or worn restorations before they worsen
- Jaw relaxation exercises or physical therapy when muscle pain is present
- Stress management strategies if tension is a major trigger
- Evaluation for sleep apnea when symptoms point in that direction
Prevention And Self‑Care Tips
You can’t always stop sleep bruxism on willpower alone, but you can reduce the load on your teeth and jaw.
- Avoid chewing gum and limit very hard or chewy foods if your jaw feels tired.
- Cut back on caffeine and alcohol in the evening if you notice they worsen clenching.
- Build a wind-down routine: warm shower, light stretching, or slow breathing.
- Use heat on sore jaw muscles for 10–15 minutes before bed.
- If you wake with jaw tension, try gentle jaw opening and side-to-side movements—no force.
Frequently Asked Questions
Can nighttime teeth grinding cause gum problems?
It can contribute. Grinding may accelerate gum recession in some people, especially if there’s existing inflammation or aggressive brushing. A dentist can tell whether recession is linked to bruxism, brushing habits, or gum disease.
Does nighttime teeth grinding happen in children?
Yes. It can be seen in children and often improves as they grow. If a child has tooth wear, jaw pain, or disturbed sleep, a pediatric dentist can guide next steps.
Should a night guard be worn every night?
If your dentist prescribed one for sleep bruxism, consistent use offers the best protection. Your dentist can also check the fit over time and replace it if it wears down.
Can bruxism cause headaches?
Yes. Many people with sleep bruxism report morning headaches or tightness in the temples due to overworked jaw muscles.
Can bruxism be cured?
Some cases settle when triggers change, while others need long-term management. Even when grinding continues, protecting teeth and addressing contributing factors usually reduces damage and symptoms.
