Infection Risks After Dental Implants | LYGOS DENTAL
Infection Risks After Dental Implants
Infection after a dental implant usually starts with inflammation of the gum around the implant and can progress to bone loss (peri-implantitis) if ignored. Early signs include increasing pain, swelling, bleeding, bad taste or odor, or pus. Prompt dental care and good home hygiene often stop the problem before the implant is affected.
Dental implants are a reliable way to replace missing teeth, but they still require surgical healing. Like any oral surgery, an implant site can become infected if bacteria build up or the tissues struggle to heal. Knowing what to watch for helps you act early and protect your results.
Table of Contents
What Is A Dental Implant Infection?
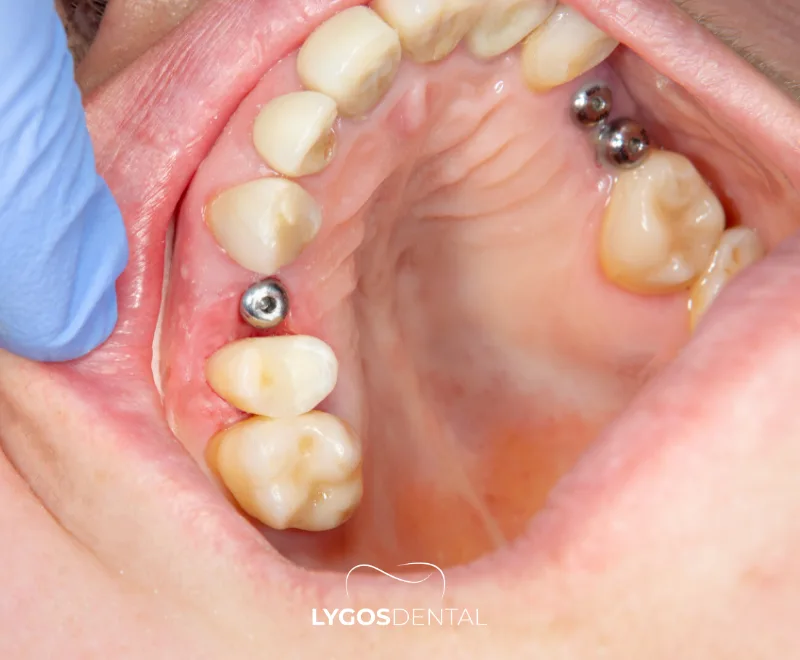
A dental implant infection is inflammation caused by bacteria around an implant. It may involve only the gum tissue (peri-implant mucositis) or, in more advanced cases, the deeper tissues and supporting bone (peri-implantitis). When bone is affected, the implant can loosen over time.
Early Signs And Symptoms
Some soreness is expected after surgery, especially in the first few days. Concern rises when symptoms worsen instead of improving, or when new symptoms appear after the initial healing period.
- Increasing or persistent pain and tenderness around the implant
- Redness, swelling, or bleeding of the gum near the implant
- Bad taste, bad breath, or a feeling of pressure in the area
- Pus (discharge) around the implant or under the gum
- Fever, fatigue, or swollen glands (less common, but urgent when present)
If you notice pus, fever, or rapidly increasing swelling, contact your dentist as soon as possible. These can signal an infection that needs prompt treatment.
Common Causes

Implant infections are usually linked to bacterial biofilm (plaque) accumulating at the gumline or under the gum. Several factors can make this more likely.
- Oral hygiene gaps that allow plaque to collect around the implant or restoration
- Smoking or vaping, which reduces blood flow and slows healing
- Uncontrolled diabetes or other conditions that affect immune response
- Poor fit of a crown or bridge that traps food and makes cleaning difficult
- Early disruption of the healing site (for example, chewing hard foods too soon)
- Incomplete or inappropriate use of prescribed antibiotics (when they are indicated)
Risk Factors That Raise The Chance Of Infection
Some patients are more prone to peri-implant disease. Your dentist may adjust your aftercare plan if any of the following apply.
- Smoking or heavy alcohol use
- A history of gum disease (periodontitis)
- Diabetes that is not well controlled
- Medications or medical conditions that suppress immunity
- High stress, poor sleep, or nutrition that can slow recovery
- Irregular dental maintenance visits after the implant is placed
How Dentists Diagnose An Implant Infection

Diagnosis usually starts with a clinical exam of the gum around the implant. Your dentist may check for bleeding, swelling, pus, and pocket depth around the implant. X-rays can help assess bone levels and rule out other causes of pain.
Treatment Options
Treatment depends on how early the problem is caught. The main goals are to remove bacteria, reduce inflammation, and protect the surrounding bone.
- Professional cleaning and debridement around the implant to remove plaque and hardened deposits
- Antiseptic mouth rinses, such as chlorhexidine, when recommended by your dentist
- Antibiotics when a bacterial infection is confirmed or strongly suspected (your dentist will choose the right option)
- Adjusting the crown or bite if the restoration is trapping plaque or causing excess pressure
- Surgical cleaning and regeneration procedures for advanced peri-implantitis, when needed
Self-treating with leftover antibiotics is risky and can delay proper care. Always follow your dentist’s instructions.
Home Care While You Arrange A Dental Visit
If you suspect an infection, home care can reduce irritation, but it cannot replace professional treatment. Use gentle brushing, keep the area clean, and avoid smoking.
- Rinse gently with warm salt water (avoid aggressive swishing right after surgery)
- Brush carefully with a soft toothbrush and clean between teeth as advised
- Stick to softer foods and avoid chewing directly on the implant area
- Take pain relief only as recommended by your dentist or pharmacist
- Call the clinic urgently if you develop fever, spreading swelling, or trouble swallowing
What Happens If An Implant Infection Is Left Untreated?
When inflammation persists, it can lead to progressive bone loss around the implant (peri-implantitis). Over time, this may reduce support and increase the risk of implant failure. In rare cases, oral infections can spread beyond the mouth and become a wider health issue.
- Ongoing discomfort and swelling
- Bone loss around the implant and gum recession
- Loosening or loss of the implant
- More complex treatment and longer healing time if re-implantation is needed
How To Reduce Infection Risk After Implant Surgery
Most problems are preventable with consistent aftercare and maintenance. Your dentist may tailor advice based on your health history and the type of restoration placed.
- Follow post-op instructions closely, especially in the first 1–2 weeks
- Brush twice daily and clean between teeth with the tools recommended for implants
- Attend follow-up visits so early inflammation is spotted before bone is affected
- Stop smoking before surgery and avoid nicotine during healing
- Manage chronic conditions such as diabetes with your medical team
- Schedule professional implant maintenance cleanings as advised
Book An Appointment
If you think you may have an implant infection—or you want a preventive check—contact our clinic to arrange an appointment. We provide cosmetic dentistry, crowns, dental implants, and general dentistry services.
FAQ
How common is infection after dental implants?
Early infection is uncommon (around 1–5%); peri-implantitis affects about 10% of implants.
What is the 3/2 rule for dental implants?
Place the implant 3 mm apical and 2 mm palatal to the planned crown.
What are the early signs of implant infection?
Pain, swelling, redness, pus/bad taste, bleeding, and increasing tenderness around the implant.
What is the most common complication of dental implants?
Peri-implant mucositis is the most common complication, causing reversible gum inflammation.
What are the disadvantages of dental implants?
Surgery, higher cost, healing time, possible failure, and peri-implantitis are major disadvantages.
Effects of Thyroid Disorders on Dental Health | LYGOS DENTAL
Effects Of Thyroid Disorders On Dental Health
Thyroid disorders can influence oral health by changing saliva flow, inflammation, and the way tissues heal. People with hypothyroidism or hyperthyroidism may notice dry mouth, higher cavity risk, gum bleeding, taste changes, or slower healing after dental work. With regular check-ups and tailored home care, most complications can be reduced.
The thyroid gland helps regulate metabolism and many body systems, including the salivary glands, immune response, and bone turnover. When thyroid hormone levels are too low or too high, changes can show up in the mouth long before someone connects the symptoms to their thyroid.
Table of Contents
What Are Thyroid Disorders?

Thyroid disorders occur when the thyroid gland produces too little hormone, too much hormone, or when structural changes affect how the gland functions. Common conditions include:
- Hypothyroidism: an underactive thyroid that slows many body processes.
- Hyperthyroidism: an overactive thyroid that speeds up metabolism and can raise heart rate.
- Goiter: an enlarged thyroid that may occur with normal, low, or high hormone levels.
- Thyroid nodules and thyroid cancer: growths in the thyroid; most nodules are benign, but some require further testing.
Why Thyroid Health Shows Up In The Mouth
Saliva protects teeth and gums by neutralizing acids, washing away food debris, and helping control bacteria. Thyroid conditions and related autoimmune issues can be linked with reduced salivary flow, which can trigger a chain reaction: more plaque, more irritation in gum tissue, and a higher risk of tooth decay.
Common Oral Signs Of Thyroid Disorders

Dry Mouth And Higher Cavity Risk
Dry mouth (xerostomia) can raise the risk of cavities, plaque buildup, and bad breath because saliva is one of the mouth’s main defenses. If your mouth often feels sticky or you need water to swallow food, mention it at your dental visit.
Gum Inflammation And Periodontal Changes
Hormone imbalance and inflammation can make gums more sensitive. Some people notice swelling, tenderness, or bleeding when brushing or flossing. Gum disease also tends to progress faster when dry mouth and plaque buildup are present.
Changes In Tongue, Taste, And Healing
Thyroid disorders can be associated with changes in taste (dysgeusia), burning or discomfort, and slower healing after extractions or other procedures. In hypothyroidism, tongue enlargement (macroglossia) or general oral tissue swelling may occur in some patients.
Tooth Development Issues In Children
In children and teens, thyroid hormones play a role in growth and development. Hypothyroidism has been linked with delayed tooth eruption and altered tooth development, while hyperthyroidism may be associated with earlier eruption in some cases.
Hypothyroidism And Oral Health
Hypothyroidism can affect oral tissues through reduced metabolic activity and changes in immune and inflammatory responses. Common dental and oral findings may include:
- Dry mouth, which can increase cavities and plaque accumulation.
- Gum inflammation and a higher risk of periodontal problems.
- Tongue enlargement or oral tissue puffiness in some patients.
- Taste changes and, in some cases, delayed wound healing.
If hypothyroidism is poorly controlled, some people are more sensitive to sedatives and other central nervous system–active medications used in dental settings. Always share your diagnosis and medication list with your dentist.
Hyperthyroidism And Dental Issues
Hyperthyroidism can increase sensitivity to stress and certain medications. Oral changes can overlap with those seen in other inflammatory conditions, and may include:
- Gum tenderness or bleeding that feels worse than usual.
- Dry mouth and increased cavity risk in people prone to dehydration or mouth breathing.
- Jaw or tooth sensitivity related to muscle tension or heightened response to stimuli.
- Faster progression of oral problems when plaque control is inconsistent.
In uncontrolled hyperthyroidism or thyrotoxicosis, stimulants such as epinephrine (found in some local anesthetics and retraction cords) can provoke a stronger cardiovascular response. Dentists may use the lowest effective dose or consider alternatives when clinically appropriate.
Effects Of Thyroid Treatments On Oral Health

Levothyroxine And Hormone Replacement
Levothyroxine helps restore normal hormone levels in hypothyroidism. Some people still report dry mouth or taste changes, which can be influenced by dose adjustments, other medications, or coexisting conditions.
Antithyroid Medications
Antithyroid drugs such as methimazole or propylthiouracil can have side effects that matter in dentistry. A rare but serious complication is agranulocytosis, which can present with fever, sore throat, or mouth ulcers due to low white blood cell counts. Any new fever or sore throat while on these medications warrants urgent medical advice.
Radioactive Iodine And Salivary Flow
Some thyroid conditions are treated with radioactive iodine. In certain patients, this can affect salivary glands and contribute to dry mouth. If you have had radioactive iodine treatment, tell your dentist so your prevention plan can be tailored.
Dental Care Recommendations For Thyroid Patients
Most people with thyroid conditions can keep their teeth and gums healthy with consistent preventive care and a few targeted habits:
- Schedule regular check-ups and cleanings (often every six months, or more frequently if gum disease is present).
- Brush twice daily with fluoride toothpaste and clean between teeth once a day.
- Support saliva: sip water, use sugar-free gum or lozenges, and ask about saliva substitutes if needed.
- Limit frequent snacking on sugary or acidic foods and drinks, especially if you have dry mouth.
- Share your full medication list, including thyroid dose, with your dental team before procedures.
- If your hyperthyroidism is not well controlled, ask your physician for clearance before major dental treatment and discuss anesthetic options.
When To Seek Help Quickly
Contact a dentist or doctor promptly if you notice persistent mouth sores, swelling, unusual bleeding, severe dry mouth, or signs of infection. If you take antithyroid medication and develop fever or sore throat, seek urgent medical care because it can signal a rare drop in white blood cells.
FAQ
Thyroid and tooth fractures
Thyroid disease rarely fractures teeth directly; dry mouth and bone loss may contribute.
Hypothyroidism dental treatment
Treat dental patients normally if controlled; postpone elective care when hypothyroidism is untreated.
Oral manifestations of thyroid disorders
Possible signs include dry mouth, burning mouth, taste changes, gum disease, delayed eruption.
Hypothyroidism and dental local anesthesia
Local anesthesia is usually safe when controlled; avoid heavy sedation in severe hypothyroidism.
Can thyroid problems cause dental problems?
Yes, thyroid disorders can worsen dry mouth, periodontal disease, healing, and jawbone metabolism.
Swelling After Wisdom Tooth Extraction | LYGOS DENTAL
Swelling After Wisdom Tooth Extraction
Facial swelling after wisdom tooth extraction is usually normal. It often starts within the first day, peaks around days 2–3, and improves over the next week. Using cold compresses early, keeping your head elevated, and following your dentist’s instructions can help. Seek care if swelling worsens after day 3, lasts beyond a week, or comes with fever or pus.
Table of Contents
Why Your Face Swells After Wisdom Tooth Removal
Swelling is part of the body’s inflammatory response to surgery. During extraction, the gum tissue and, in many cases, the bone around the tooth are disturbed. Your immune system increases blood flow and sends repair cells to the area, which can cause temporary fluid buildup in the cheek and jaw.
The severity of the swelling generally depends on:
What Affects How Much You Swell
Swelling varies from person to person. Common factors include:
- Whether the tooth was impacted or partially erupted
- How long and complex the procedure was
- Your age, general health, and healing speed
- The amount of tissue manipulation needed and the surgical approach used
How Long Swelling Usually Lasts
Most people notice swelling within the first 24 hours. It typically reaches its maximum around 48–72 hours after surgery and then gradually improves.
A simple timeline can help set expectations:
- Day 0–1: Swelling begins and may feel tight or puffy.
- Day 2–3: Swelling is often at its peak; bruising may appear.
- Day 4–7: Swelling steadily decreases and comfort improves.
- After day 7: Mild puffiness can linger, especially after difficult extractions, but it should keep improving.
If swelling is still getting worse after the first few days, or it does not start to improve by about a week, contact your dentist or oral surgeon.
How To Reduce Swelling Safely

First 24 Hours
Focus on cold therapy and rest. Cold helps limit fluid buildup in the tissues.
- Use a cold compress on the cheek: 15–20 minutes on, then 15–20 minutes off, repeating as tolerated.
- Rest and avoid strenuous activity.
- Sleep with your head slightly elevated to reduce fluid pooling.
After 24 Hours
Once the first day has passed, gentle warmth and good oral hygiene can support comfort and healing.
- Rinse gently with warm salt water 3–4 times per day (or as directed). Avoid vigorous swishing.
- Stay well hydrated and choose soft foods. Cool or room-temperature foods are usually best early on.
- Take prescribed medications exactly as directed, including any anti-inflammatory medicine or antibiotics.
What To Avoid After Extraction
These habits can increase swelling, disrupt the clot, or slow healing:
- Smoking or vaping
- Alcohol during the early healing period
- Hot foods and drinks in the first day or two
- Straws, forceful spitting, or aggressive rinsing during the first 24 hours
- Hard, crunchy, or grainy foods that can irritate the surgical site
- Touching the area with fingers or probing it with your tongue
Does Swelling Mean Something Is Wrong?
Swelling by itself is expected after wisdom tooth removal. What matters is the pattern. Normal swelling tends to peak around days 2–3 and then improves. A sudden increase in swelling, worsening pain, or new symptoms can point to a problem such as infection or a dry socket.
When To Contact A Dentist
Call your dentist or oral surgeon promptly if you notice any of the following:
- Swelling that keeps increasing after day 3, or swelling that lasts longer than about 7 days without improvement
- Fever, chills, or feeling unwell
- Pus, foul odor, or a persistent bad taste
- Severe one-sided swelling or noticeable facial asymmetry that is worsening
- Trouble swallowing, breathing, or opening the mouth
- Numbness that does not start to improve or gets worse
FAQ
How long does the swelling last after a wisdom tooth extraction?
Swelling peaks day 2–3 and improves within 3–5 days.
Why is the third day the worst after a tooth extraction?
Inflammation and tissue fluid peak around day three, making pain and swelling strongest.
What are the symptoms to watch for after a wisdom tooth extraction?
Watch for uncontrolled bleeding, worsening pain, fever, pus, foul taste, severe swelling, breathing trouble.
Can I tell if I have dry socket on the third day?
Yes; severe throbbing pain, bad odor/taste, and visible socket bone suggest dry socket.
How can I tell if I have an infection after a wisdom tooth extraction?
Infection signs include fever, worsening swelling, pus, increasing pain, and foul discharge.
Turkey Dental Treatment and Post-Treatment Holiday Guide
Turkey Dental Treatment and Post-Treatment Holiday Guide
If you’re coming to Turkey for dental treatment, plan your trip around recovery. Use the first 48–72 hours for rest, soft foods, and follow-up checks, then add gentle sightseeing. Choose a city that fits both your clinic and holiday style—city breaks in Istanbul, beach time in Antalya, or Aegean calm in Izmir and Çeşme.
Table of Contents
Why People Choose Dental Treatment In Turkey
Turkey is a well-known dental tourism destination because many private clinics combine modern equipment, experienced clinicians, and packages that simplify travel. Prices can be lower than in many European countries and the US, but the exact savings depend on the clinic, materials, and the complexity of your case.
Before you book, ask for a written treatment plan that lists the number of visits, the brands/materials used, warranty terms, and what is included in the quote. If you have medical conditions or take regular medication, share that information early so your dentist can plan safely.
How To Schedule Treatment And Holiday Time
Match your holiday to the type of dental work.
Some treatments fit neatly into a short trip, while others need staged visits. Teeth whitening and simple cosmetic procedures may be completed in a couple of appointments. Implants, bone grafts, and complex restorative work often need more time, follow-up checks, and sometimes a second visit after healing.
Build in recovery days from the start.
Plan at least a few low-key days right after any surgical procedure. Swelling and discomfort tend to peak early, so keep your schedule flexible for rest, medication timing, and a follow-up appointment if needed.
Most Popular Bases For Treatment And A Short Break

Istanbul
Best for a city break. Choose calm, walkable plans after treatment: a Bosphorus cruise, museums with elevators, and short neighborhood strolls.
Antalya
Ideal for a resort-style recovery. Many hotels make it easy to rest, hydrate, and eat soft foods while staying close to clinics.
Izmir And Çeşme
Good for a relaxed Aegean pace. Alaçatı and Çeşme are comfortable once you feel better, with plenty of gentle dining options.
Muğla: Bodrum, Marmaris, Fethiye
A strong pick for post-procedure downtime by the sea. Keep boat trips and long hikes for later in your recovery.
Ankara
Often chosen for clinic access and healthcare infrastructure. It also works as a hub if you’re connecting onward to Cappadocia.
Recovery Guidelines For A Comfortable Holiday
First 48–72 hours
- Keep activity light. Skip heavy lifting, intense workouts, and long walking tours.
- Sleep with your head slightly elevated if you have swelling.
- Follow your dentist’s instructions for pain relief, antibiotics (if prescribed), and oral hygiene.
- Stay hydrated. Cabin air, summer heat, and salty foods can make you feel worse.
Days 4–7
- Add gentle sightseeing: short walks, shaded cafés, and seated attractions.
- Choose low-risk activities. Avoid contact sports, diving, and anything that could bump your jaw.
- Keep a buffer for check-ups and unexpected sensitivity.
When flying or taking long transfers
If you’ve had an extraction, implant surgery, or bone grafting, ask your dentist whether you should delay flying. Many clinicians advise avoiding flights in the first few days after oral surgery, especially after more complex procedures. If you must travel, carry your medications in your hand luggage and plan for easy meals on the go.
Food And Drink After Dental Treatment
What usually works well
Soft, lukewarm foods are easier on healing gums. Good options in Turkey include lentil soup, yogurt, well-cooked vegetables, soft egg dishes, and flaky fish. If chewing is uncomfortable, ask the restaurant to serve food without crusty bread, seeds, or hard garnishes.
What to limit early on
- Very hot or very cold foods if you have sensitivity.
- Spicy or acidic dishes if your gums feel sore.
- Alcohol and carbonated drinks if your dentist advised avoiding them after surgery.
- Hard snacks (nuts, chips, crackers) that can irritate the area or get trapped.
Choosing A Clinic With Travel In Mind

- Confirm the clinic’s location, airport transfer options, and how you’ll reach them for follow-up visits.
- Ask which materials and lab work are used (implant brand, crown type, veneer material) and request documentation.
- Check whether a translator is available if you prefer care in English.
- Prioritize clear consent, realistic timelines, and a plan for complications once you return home.
Why Combining Treatment With A Holiday Can Work
A calm environment can make recovery feel easier, and Turkey offers both coastal downtime and culture-rich city breaks. The key is to treat recovery time as part of the trip, not an afterthought. If your itinerary is gentle and your clinic schedule is realistic, you can come home with both a healthier smile and a good travel experience.
FAQ
Turkey dental treatment and post-treatment vacation guide Antalya
Schedule treatment early, rest 48 hours, avoid swimming 24–48 hours, attend follow-ups.
Best All on 4 in Turkey
Choose an experienced implant team using CBCT planning, proven brands, and written guarantees.
How much does a new set of teeth cost in Turkey?
Full-mouth fixed implant teeth in Turkey cost about £5,200–£12,600.
Affordable veneers in Turkey
Veneers in Turkey cost about $150–$450 per tooth, depending on material.
What is the cost of getting dental implants in Turkey?
A single dental implant in Turkey costs about $500–$900 including abutment and crown.
What to Eat During Orthodontic Treatment | LYGOS DENTAL
What to Eat During Orthodontic Treatment
Stick to soft, nutrient-dense foods that won’t bend wires or pop brackets—yogurt, eggs, soups, pasta, cooked vegetables, and smoothies. Cut firmer foods into small pieces, chew slowly, and avoid sticky, hard, or crunchy snacks. These choices reduce soreness, protect your appliance, and help treatment stay on schedule.
Table of Contents
Orthodontic Treatment: What It Is And Who It Helps
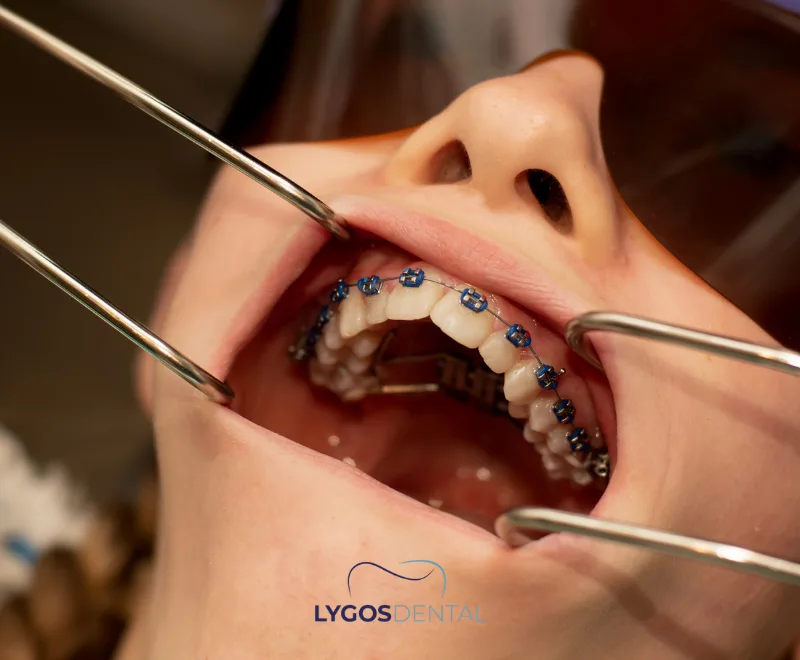 Orthodontic treatment moves teeth and, when needed, the jaw into healthier alignment. It can improve bite function, speech clarity, cleaning access, and overall smile aesthetics. Treatment may involve metal or ceramic braces, lingual braces, or clear aligners such as Invisalign. Because brackets, wires, and attachments sit on the teeth, food choices matter from day one.
Orthodontic treatment moves teeth and, when needed, the jaw into healthier alignment. It can improve bite function, speech clarity, cleaning access, and overall smile aesthetics. Treatment may involve metal or ceramic braces, lingual braces, or clear aligners such as Invisalign. Because brackets, wires, and attachments sit on the teeth, food choices matter from day one.
Why Diet Matters During Orthodontic Treatment
Brackets and wires create new pressure points in the mouth. Hard or sticky foods can break appliances, irritate soft tissues, and make cleaning harder. Poor choices may lead to plaque buildup, enamel damage, or gum inflammation. A braces-friendly diet can help you:
- Lower the risk of broken brackets, bent wires, or lost aligner attachments
- Reduce cheek and gum irritation
- Keep brushing and flossing easier and more effective
- Support healthy gums and enamel throughout treatment
- Avoid unnecessary delays in your treatment plan
What To Eat In The First Week After Getting Braces
 Tenderness is common for the first few days and after adjustment appointments. Choose soft foods that require minimal chewing, and keep foods lukewarm to avoid triggering sensitivity.
Tenderness is common for the first few days and after adjustment appointments. Choose soft foods that require minimal chewing, and keep foods lukewarm to avoid triggering sensitivity.
- Yogurt or kefir: cool and soothing for sore gums
- Soups and broths: blended vegetable soups or chicken broth are easy to eat
- Mashed potatoes or other purées: filling and gentle on brackets
- Soft fruits: bananas, ripe pears, or avocado
- Cooked vegetables: zucchini, broccoli, pumpkin, or well-steamed carrots
- Oatmeal or soft cereal soaked in milk
Best Braces-Friendly Foods For Everyday Meals
Once the initial soreness eases, you can expand your menu. Aim for foods that are soft, easy to chew, and not likely to stick to brackets or get trapped around wires.
Dairy And Calcium-Rich Options
Milk, cheese, yogurt, and ayran/buttermilk support enamel and are generally easy to eat with braces.
Protein That’s Easy On Braces
Eggs (boiled, scrambled, omelets), flaky fish, tofu, and tender ground meat are practical protein choices. If you eat chicken or beef, choose softer cuts and chop them into small pieces.
Soft Grains And Starches
Pasta, rice, couscous, soft bread without a hard crust, and well-cooked oats are usually safe. Avoid biting into hard rolls or crusty baguettes.
Fruits And Vegetables
Soft fruits are easiest. For firmer produce, slice thinly, grate it, or cook it until tender.
- Smoothies made with berries, banana, yogurt, and oats
- Apples or carrots: cook, grate, or slice into very small pieces
- Leafy greens: add to soups, omelets, or smoothies
Soups, Stews, And One-Bowl Meals
Lentil soup, vegetable soup, and soft stews can deliver vegetables and protein without heavy chewing. Let hot soups cool slightly before eating.
Snacks And Desserts
Try hummus, soft muffins, pudding, custard, or ripe fruit. If you choose ice cream, rinse with water afterward to reduce sugar sitting on the teeth.
Foods to Avoid with Braces
Some foods commonly break brackets, bend wires, or get stuck in places that are hard to clean. Limiting them helps prevent emergency visits and keeps progress steady.
Hard Foods
- Nuts, popcorn kernels, hard candy, ice
- Crusty bread, hard pizza crusts
- Whole raw apples or large raw carrot sticks
Sticky Or Chewy Foods
- Caramel, taffy, gummy candies, Turkish delight
- Chewing gum
- Very chewy bagels or jerky
Crunchy Snacks
- Chips, crackers, pretzels
- Granola clusters and hard cereals
Foods With Pits, Bones, Or Shells
- Cherries, olives, and other fruits with pits (remove pits first)
- Bone-in meats (cut meat off the bone before eating)
Sugary And Acidic Drinks
Soda and frequent acidic drinks can increase enamel wear, especially around brackets. If you drink them occasionally, use a straw and rinse with water afterward.
Foods That Can Help Relieve Braces Soreness
 When your teeth feel tender after braces are placed or tightened, focus on temperature and texture.
When your teeth feel tender after braces are placed or tightened, focus on temperature and texture.
Cool Options
- Cold yogurt, kefir, or smoothies
- Soft ice cream or frozen yogurt (in moderation)
- Chilled applesauce
Warm (Not Hot) Options
- Vegetable soup, chicken broth, or lentil soup
- Mashed potatoes, soft pasta, or rice
- Warm oatmeal
Practical Eating Tips To Protect Your Braces
- Cut food into small, bite-sized pieces and chew slowly.
- Try to chew with your back teeth rather than biting with the front teeth.
- Rinse with water after meals to clear food from around brackets and wires.
- Brush and floss carefully, especially after sugary or starchy foods.
- If something feels stuck, use an interdental brush or water flosser instead of toothpicks.
- If you wear aligners, remove them for meals and drinks other than water, then clean your teeth before putting them back in.
Orthodontic treatment takes time, but eating well makes it easier. Soft, braces-safe foods support comfort and oral hygiene, while avoiding hard and sticky items protects your appliance. If you’re unsure whether a food is safe, ask your orthodontist at your next visit.
Get More Information
To book an appointment or ask questions about braces, aligners, cosmetic dentistry, dental crowns, implants, or general dentistry, contact our clinic.
FAQ
What should I eat during braces treatment?
Eat soft, non-sticky foods: yogurt, eggs, pasta, rice, cooked vegetables, soft fruits.
What should I avoid eating while wearing braces?
Avoid hard, sticky, chewy foods: nuts, popcorn, caramel, gum, ice, hard candy.
Can I bite into and eat a hamburger while wearing braces?
Yes, if you cut it into small pieces and avoid biting directly.
What drinks should I avoid while wearing braces?
Avoid sugary or acidic drinks: soda, energy drinks, sports drinks, and frequent juice.
Can I eat cookies while wearing braces?
Yes, choose soft cookies; avoid hard, crunchy cookies and biting with front teeth.
Jaw Exercises for TMJ Patients | LYGOS DENTAL
Jaw Exercises for TMJ Patients
Gentle jaw exercises can help many people with TMJ/TMD reduce muscle tension and improve comfortable mouth opening. Work only within a pain‑free range, move slowly, and stop if you feel sharp pain, locking, or worsening symptoms. Pair exercises with good jaw posture and simple self‑care like heat or cold as advised by your clinician.
Temporomandibular disorders (often shortened to TMD or “TMJ pain”) can make chewing, speaking, and yawning uncomfortable. Alongside professional guidance, simple home exercises may support recovery by improving control and reducing muscle guarding.
Table of Contents
What TMJ Is
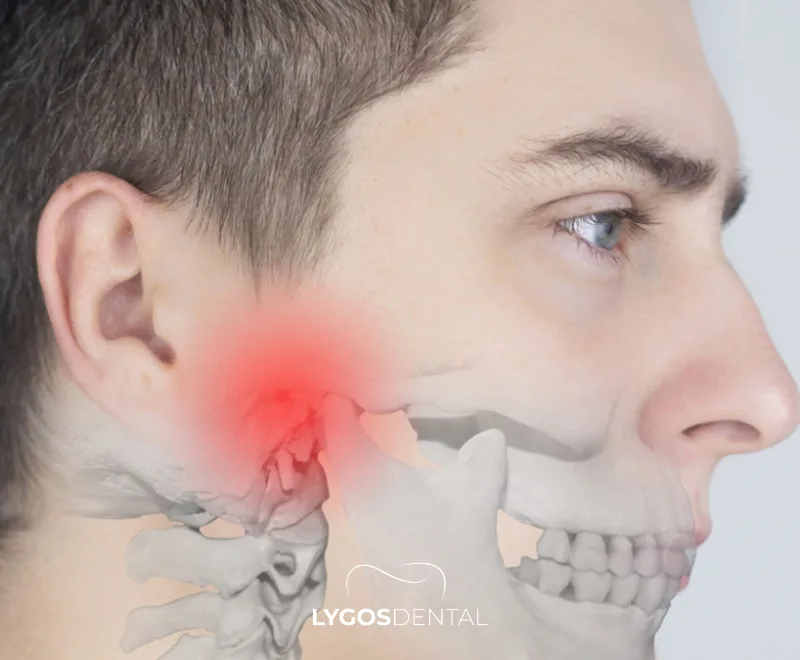
The temporomandibular joint connects your lower jaw (mandible) to your skull and works with a group of chewing muscles. When the joint itself, the surrounding muscles, or both become irritated or overworked, symptoms such as pain, stiffness, and clicking can appear.
Common Symptoms of TMJ Disorders
TMJ/TMD symptoms vary, but common signs include:
- Jaw pain or tenderness (one or both sides)
- Pain or fatigue while chewing
- Tightness in the face or jaw muscles
- Limited or uneven mouth opening
- Clicking, popping, or grinding sounds with jaw movement
- Ear-area pressure or pain (without an ear infection)
- Headaches, neck pain, or facial pain that seems linked to jaw use
How Exercises Support TMJ Treatment

For many patients, first-line care is conservative: self-care, splints/night guards when appropriate, and physical therapy. Targeted exercises may help by improving movement patterns, strengthening supporting muscles, and easing protective muscle spasms.
Benefits you may notice with consistent practice include:
- Better jaw control during opening and closing
- Less muscle tightness and fewer spasms
- Improved comfortable mouth opening over time
- Reduced sensitivity during daily activities like eating or talking
Safe Jaw Exercises You Can Do at Home
Do these exercises slowly and gently. A mild stretch or light muscle effort is okay, but sharp pain is not. Start once daily and build up to 2–3 short sessions if tolerated.
1) Controlled Jaw Opening and Closing
- Sit or stand tall with your head centered (avoid jutting the chin forward).
- Let your jaw relax and slowly open your mouth to a comfortable, pain‑free limit.
- Pause briefly, then close slowly without clenching your teeth at the end.
Suggested dose: 8–10 repetitions, 1–2 times per day.
2) Resisted Jaw Opening (Gentle)
- Place two fingers or the heel of your hand under your chin.
- Begin to open your mouth slowly while applying very light upward resistance.
- Hold the effort for 2–3 seconds, then relax and close slowly.
Suggested dose: 5–8 repetitions, once daily to start.
3) Side‑to‑Side Jaw Glides
- Keep your lips relaxed and teeth slightly apart.
- Move your lower jaw slowly to the right, then return to center.
- Move your lower jaw slowly to the left, then return to center.
Suggested dose: 5 repetitions per side, 1–2 times per day.
4) Tongue‑Up Opening (Resting Tongue on the Palate)
- Rest the tip of your tongue gently on the roof of your mouth, just behind the front teeth.
- Keeping the tongue in place, open your mouth slowly to a comfortable range.
- Close slowly and return to a relaxed jaw position.
Suggested dose: 6–10 repetitions, 1–2 times per day.
5) Relaxed Jaw Position (60‑Second Reset)
- Let your lips come together lightly.
- Keep your teeth slightly apart, with the tongue resting softly on the palate.
- Breathe slowly for 30–60 seconds and release tension from the cheeks and temples.
Suggested dose: 1–3 times per day, especially during stress or after long talking/chewing.
Safety Tips and Precautions
Exercises work best when your technique is calm and controlled. These tips help you stay safe and consistent:
- Stay in a pain‑free range. Stop if pain spikes, the jaw catches/locks, or symptoms worsen afterward.
- Move slowly. Fast or forceful stretching can irritate the joint and surrounding muscles.
- Use heat or cold if it helps (many people prefer moist heat for muscle tightness, cold for soreness after flare-ups).
- Avoid gum chewing, wide yawns, and hard or very chewy foods during flare-ups.
- Check your form in a mirror and keep your head and neck aligned.
When to See a Dentist or Doctor

Home exercises can be useful, but some symptoms need professional assessment. Seek care if you notice:
- Severe or persistent pain that doesn’t improve with self‑care
- A sudden change in your bite or new difficulty bringing teeth together
- Jaw locking (open or closed) or frequent catching during movement
- Significant limitation in mouth opening
- Swelling, fever, trauma, or signs of infection
- Symptoms that steadily worsen over days or weeks
A dentist, physiotherapist, or oral and maxillofacial surgeon can help confirm the cause of your symptoms and tailor a plan that may include splint therapy, medication advice, manual therapy, posture work, and targeted strengthening.
FAQ
Permanently treating TMJ
Permanent cure is uncommon; manage with splints, physiotherapy, stress reduction, and treating causes.
TMJ exercises at home
Do gentle controlled opening, tongue-to-palate, and isometric holds, 5–10 reps.
TMJ exercises for jaw clicking
Controlled opening with tongue on palate and gentle lateral movements may reduce clicking.
Relaxing jaw exercise
Place tongue on palate, lips closed, teeth apart, breathe slowly for 2 minutes.
TMJ exercises before bed
Do warm compress 10 minutes, then gentle stretches and slow diaphragmatic breathing.
Methods to Prevent Baby Tooth Decay | LYGOS DENTAL
Methods To Prevent Baby Tooth Decay
Baby tooth decay is preventable with early cleaning, the right amount of fluoride toothpaste, a low-sugar routine, and an age-one dental visit. Start wiping gums and brushing as soon as the first tooth erupts, brush twice daily with caregiver help, avoid bedtime bottles with anything but water, and keep regular check-ups to catch early spots before they turn into cavities.
Table of Contents
Why Baby Teeth Matter
Baby teeth are not “practice teeth.” They hold space for permanent teeth, support clear speech, and help children chew comfortably. When baby teeth decay, children can feel pain, have trouble eating, and may need dental treatment that could have been avoided.
When To Start Cleaning Baby Teeth

Begin oral care before your child can even brush. Wipe the gums with a clean, damp gauze or soft cloth after feedings if you like, and start cleaning as soon as the first tooth appears (often around 6–10 months). Early routines make brushing feel normal and lower cavity risk.
Brushing And Fluoride Toothpaste

Brushing removes plaque, the sticky film that feeds cavity-causing bacteria. Young children need hands-on help, so plan to brush for them or with them until they can reliably spit and brush well on their own.
Step-By-Step Brushing For Infants And Toddlers
- Brush twice a day: after breakfast and before bed.
- Use gentle, small circular motions along the gumline and on all tooth surfaces.
- Choose a small, soft-bristled brush (or a baby finger brush for early months).
- Lift the lip to reach the upper front teeth—these are common cavity spots.
- Make it quick and calm. A song or timer helps.
How Much Toothpaste To Use
Use fluoride toothpaste, but keep the amount small. For children under 3, use a smear the size of a grain of rice. From 3 to 6, use no more than a pea-sized amount. Always supervise brushing and store toothpaste out of reach.
Food And Drink Habits That Protect Baby Teeth
Cavities are not caused by sugar alone—it’s the frequency and timing that matter. Sipping sweet drinks over long periods or having sugary snacks right before sleep keeps acids on the teeth for hours.
Limit Sugary Snacks And Drinks
- Keep sweets as an occasional treat, not a daily routine.
- Avoid juice, sweetened milk, and other sugary drinks in bottles or sippy cups.
- Offer water between meals and after snacks.
- Choose tooth-friendly snacks like plain yogurt, cheese, eggs, vegetables, and fresh fruit.
Avoid Bedtime Bottles With Sugar
Put your child to bed with water only. Milk, formula, juice, and sweetened drinks can pool around the teeth during sleep, raising the risk of early childhood cavities—especially on the upper front teeth.
First Dental Visit And Regular Check-Ups
Schedule the first dental visit within six months of the first tooth erupting, and no later than your child’s first birthday. These early visits focus on prevention: checking development, spotting early white marks, and helping you fine-tune brushing and diet.
Extra Measures Your Dentist May Recommend

Some children benefit from added protection, depending on diet, enamel strength, and cavity risk. Your dentist may suggest:
- Fluoride varnish to strengthen enamel.
- Silver diamine fluoride (SDF) to slow or stop early cavities when appropriate.
- Age-appropriate flossing once teeth touch.
- Sealants on back teeth when they erupt (common later in childhood).
At-Home Routine Checklist
- Brush twice daily with a caregiver’s help.
- Use the correct fluoride toothpaste amount for your child’s age.
- Avoid frequent sipping of sweet drinks; choose water between meals.
- Keep snacks mostly low-sugar and stick to set snack times.
- Book regular dental check-ups and follow professional advice.
FAQ
How can I prevent my baby’s teeth from decaying?
Brush erupted teeth twice daily with fluoride; avoid bedtime bottles; limit sugar.
What is the 2-2-2 rule in dentistry?
Brush 2 minutes twice daily and see dentist twice yearly.
What food causes tooth decay the most?
Frequent sugary, sticky foods like candy and cookies cause the most decay.
Why does my 2-year-old child constantly experience tooth decay?
Frequent sugars, bedtime milk/juice, and inadequate fluoride brushing commonly drive toddler cavities.
What should I do to prevent tooth decay 100%?
You cannot prevent cavities 100%; minimize risk with fluoride brushing, flossing, less sugar, checkups.
Porcelain Veneers in Turkey vs Spain | LYGOS DENTAL
Porcelain Veneers In Turkey Vs Spain
Porcelain veneers can improve tooth colour, shape, and minor alignment in a short timeframe. Turkey is often chosen for lower per-veneer costs with modern clinics in major cities, while Spain typically costs more but appeals to patients who prefer treatment within the EU. The best option depends on case complexity, aftercare plans, and clinic quality rather than price alone.
Table of Contents
What Porcelain Veneers Are

Porcelain veneers are thin ceramic shells bonded to the front surface of teeth. They can correct stains that do not respond well to whitening, small chips, worn edges, uneven tooth shapes, and gaps.
Veneers are not the right solution for every case. Active gum disease, untreated cavities, heavy grinding, or significant bite issues may require other treatment first.
Why Patients Choose Veneers
- A natural look: modern ceramics mimic enamel translucency and reflect light similarly to natural teeth.
- Durability: with good oral hygiene and regular check-ups, veneers often last many years.
- Conservative change: many cases need only minimal shaping of the tooth surface, compared with full crowns.
- Fast results: planning, preparation, and final bonding are typically completed in a short treatment window.
Materials And Laboratory Quality
The final result depends on both the ceramic material and the lab work. Clinics in Turkey and Spain commonly use digital impressions, shade matching, and high-precision milling or layering techniques.
Common veneer options include:
Zirconia-Based Ceramics
Zirconia is known for strength. It can be a good choice when extra durability is needed, though achieving the most lifelike translucency may require advanced layering and careful shade work.
Laminate (Feldspathic) Porcelain
Laminate veneers are very thin and can look highly natural. They are often used for smile design cases where the goal is a bright but realistic finish with minimal bulk.
Full-Ceramic Veneers
Full-ceramic options without metal support avoid grey shading at the gumline and are widely used for front teeth. The exact brand and technique vary by clinic and lab.
Treatment Steps And Typical Timeline
Most veneer treatments follow a structured plan, whether you do it in Turkey or Spain:
- Consultation and planning: exam, X-rays when needed, and a smile plan based on your face and bite.
- Tooth preparation: a thin layer of enamel may be shaped to create space for the veneer.
- Impressions and lab work: digital scans or impressions are sent to the lab for fabrication.
- Temporary veneers: optional, used to protect teeth and preview the look while the final set is made.
- Bonding and adjustments: veneers are cemented and the bite is checked to reduce the risk of chipping.
Timelines vary by case and lab capacity. Many clinics schedule veneer treatment across several visits over about one to two weeks, especially for international patients.
Getting Veneers Abroad: Pros And Cons

Advantages
- Potential savings compared with some Western European markets, particularly for multiple veneers.
- Access to high-volume cosmetic dentistry teams that focus on smile design.
- Combining treatment with travel, if your schedule allows for follow-up visits.
Disadvantages
- Follow-up logistics: if a veneer needs adjustment or repair, returning to the same clinic may be inconvenient.
- Communication: language differences can affect expectations around shade, shape, and final outcome.
- Total trip cost: flights, accommodation, and time off work can reduce the price gap.
Price Comparison: Turkey Vs Spain
Prices depend on the ceramic type, the number of veneers, the complexity of your bite, and what is included (consultation, imaging, temporaries, warranty, and aftercare). Clinics may also price differently for single veneers versus full smile cases.
Typical per-veneer ranges you may see advertised:
- Turkey: about €150–€400 per veneer in many clinics, with large variation by city and lab quality.
- Spain: about €300–€600 per veneer, with higher prices common in major cities and premium cosmetic practices.
Always ask for a written treatment plan that lists the material type, the number of veneers, what is included in the package, and the policy for remakes or repairs.
How To Choose A Clinic Safely
- Check credentials: confirm the dentist’s training, licensing, and experience with veneers.
- Review planning standards: look for clear smile design steps, previews (mock-up), and bite assessment.
- Ask about the lab: in-house vs external, turnaround time, and how shade matching is handled.
- Confirm hygiene and documentation: sterilisation protocols and a clear consent process.
- Get aftercare in writing: follow-up schedule, warranty terms, and what happens if a veneer chips or debonds.
- Plan for protectors: if you grind your teeth, a night guard can protect your investment.
FAQ
Is it worth going to Turkey to get veneers?
Yes, if savings are substantial and aftercare and warranties are confirmed.
How much do porcelain veneers cost in Spain?
€350–€600 per tooth is common; some clinics quote from about €450.
How much does a full set of veneers cost in Turkey?
$2,000–$9,000 for 16–20 veneers, depending on material and clinic.
How long does it take to get porcelain veneers in Turkey?
5–7 days over two visits; some cases finish within one week.
Emax Veneer 2026 | LYGOS DENTAL
Emax Veneers 2026
Emax veneers are ultra-thin lithium disilicate ceramic shells bonded to the front of teeth to improve color, shape, and small spacing or alignment concerns. In 2026, digital scanning and smile design tools help dentists plan results more precisely, often with minimal enamel reduction. With good oral hygiene, many patients keep their veneers for around 10–15 years.
Dental aesthetics is no longer only about “white teeth.” For many people, it affects confidence, first impressions, and how comfortably they speak and smile.
Emax veneers remain a popular option because they can look very natural while offering strong, long-lasting ceramic performance. This guide covers what they are, what’s new in 2026, who they suit best, how the treatment works, and what usually affects cost.
Table of Contents
What Are Emax Veneers?
Emax veneers are thin ceramic shells that are bonded to the front surface of the teeth. They are typically made from lithium disilicate glass-ceramic, a material known for its strength and lifelike translucency.
Because lithium disilicate transmits light in a way that resembles natural enamel, Emax veneers can blend smoothly with neighboring teeth. They also tend to stay color-stable and resist staining when properly cared for.
Compared with many traditional porcelain veneers, Emax can often be produced in thinner sections. That can mean less tooth reduction in suitable cases, which helps preserve natural enamel.
Emax Veneer Trends In 2026
Aesthetic dentistry keeps moving toward more personalized, minimally invasive results. For Emax veneers, the biggest changes come from digital planning and improved ceramic characterization.
Digital Smile Design (DSD) And 3D Scanning
Dentists increasingly use high-resolution photos and 3D scans to map facial proportions, lip movement, and tooth position. This makes it easier to preview the smile design and communicate expectations before any tooth preparation begins.
Ultra-Thin And Minimal-Prep Veneers
In appropriate cases, Emax veneers may be fabricated as very thin restorations (often around 0.2–0.3 mm). When bite and alignment allow, the dentist may reduce little enamel—or sometimes none—while still achieving a natural shape.
More Natural Surface Texture And Shade Layering
Modern ceramics and lab techniques can recreate subtle details like translucency at the incisal edge, soft texture, and realistic light reflection. The goal in 2026 is a “your teeth, but better” look rather than an overly uniform, opaque finish.
Software-Assisted Planning
Planning software can propose veneer shapes based on facial and dental measurements, then the dentist fine-tunes the final design. This can speed up mock-ups and help standardize accuracy, especially in clinics that use an in-house CAD/CAM workflow.
Who Are Emax Veneers Suitable For?
Emax veneers work best for patients who want an aesthetic upgrade while keeping as much natural tooth structure as possible. A dentist will still check bite, gum health, and enamel quality before recommending them.
Good Candidates
- People who want a longer-lasting alternative to repeated whitening for stubborn discoloration.
- Patients with small chips, hairline cracks, or worn incisal edges on front teeth.
- Those with mild gaps between teeth (diastema).
- Teeth that are slightly uneven, asymmetric, or irregularly shaped.
- Patients seeking a brighter, more youthful smile while keeping a natural look.
When Emax Veneers May Not Be The Right Choice
- Severe teeth grinding (bruxism) without protection (for example, a night guard).
- Active gum disease or untreated decay.
- Significant bite misalignment that would overload veneers.
- Very limited enamel for bonding (your dentist will assess this).
If any of these issues apply, dentists usually treat the underlying problem first—then reassess veneer options.
Emax Veneer Procedure Step By Step
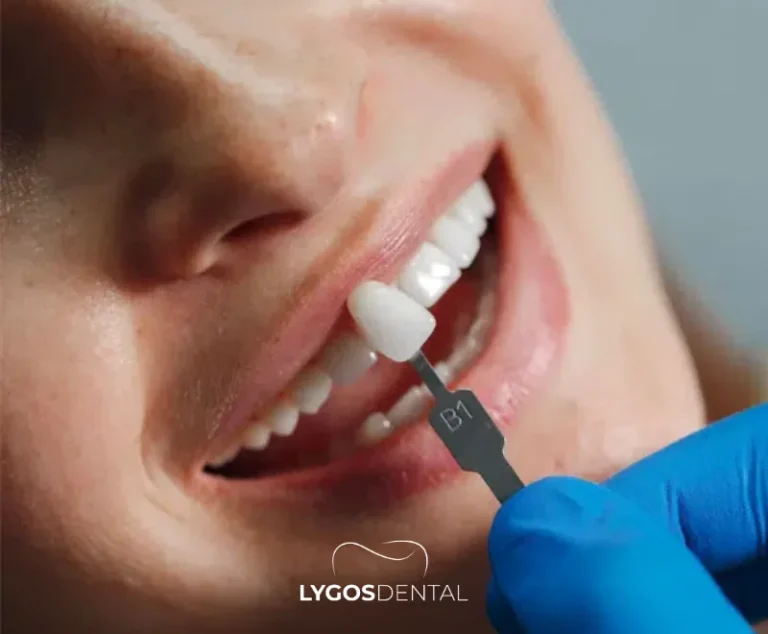
- Consultation And Digital Planning
The dentist examines the teeth and gums, discusses goals, and takes digital impressions or 3D scans. A mock-up or preview may be created to show likely results.
- Tooth Preparation (If Needed)
A small amount of enamel may be reduced to create space for the veneer. With ultra-thin designs, preparation can be minimal in suitable cases.
- Temporary Veneers
Temporary veneers may be placed while the lab fabricates the final restorations, especially when tooth reduction was required.
- Try-In And Bonding
The dentist checks fit and shade, then bonds the veneers using adhesive protocols designed for ceramic. Final shaping and polishing help achieve a natural finish.
- Aftercare And Follow-Up
Most patients can eat normally soon after bonding, but it helps to avoid very hard foods and stain-heavy drinks at first. Regular check-ups and good daily hygiene support long-term success.
How Long Do Emax Veneers Last?

With careful bonding, good oral hygiene, and regular dental visits, Emax veneers commonly last around 10–15 years. Longevity depends on bite forces, habits like nail-biting or ice chewing, and whether grinding is controlled with a night guard.
Emax Veneer Costs In 2026
Pricing varies widely based on the clinic’s location, the dentist’s experience, lab quality, and how complex the case is. Extra procedures—such as gum reshaping, treating gum disease, or correcting bite issues—can also change the total.
In Turkey, clinics often quote per-tooth pricing. As a practical benchmark, many providers advertise ceramic laminate / Emax-style veneers in roughly the 9,500–20,000 TL range per tooth (figures commonly published for 2025 through early 2026), depending on the city, lab, and case complexity. Your final quote should come from an exam and a written treatment plan.
Why Choose Emax Veneers?
- Natural translucency that mimics enamel for a realistic smile.
- Strong ceramic performance that resists chipping when properly designed and bonded.
- Color stability and stain resistance with everyday brushing and flossing.
- Potential for minimal tooth reduction in suitable cases.
- Good gum compatibility when margins are designed and finished correctly.
Care And Maintenance Tips
- Brush twice daily with a non-abrasive toothpaste and a soft-bristled brush.
- Floss daily; consider interdental brushes if recommended by your dentist.
- Avoid using teeth as tools (opening packaging, biting pens).
- If you grind your teeth, wear a night guard as advised.
- Schedule professional cleanings and check-ups at least twice a year.
Book A Consultation
If you’re considering veneers, a consultation is the fastest way to confirm suitability and get an accurate quote. Bring ph
FAQ
How long do Emax veneers last?
Typically 10–15 years; many last longer with good care and a nightguard.
What is the 4-8-10 rule for veneers?
Guideline: veneer 4 incisors, 8 to canines, 10 to premolars for smile width.
What is better than Emax veneers?
Nothing universally; zirconia is stronger, feldspathic porcelain can look even more lifelike.
Do Emax veneers look natural?
Yes; lithium disilicate’s translucency and color matching can look very natural.
What should be avoided with Emax veneers?
Avoid biting hard objects, chewing ice, nail-biting, and untreated grinding/clenching.
Invisalign Prices in Turkey vs UK | LYGOS DENTAL
Invisalign Prices in Turkey vs UK
Invisalign is usually cheaper in Turkey than in the UK because clinic overheads and local operating costs are lower. In the UK, private Invisalign often sits around £1,500–£5,500+, while Turkish clinics commonly quote from roughly ₺40,000 for mild cases to ₺120,000+ for full treatment. Your final price depends on case complexity, provider expertise, and what’s included.
Table of Contents
How Invisalign Treatment Works
Invisalign is an orthodontic system that straightens teeth using a series of clear, removable aligners. Each aligner is custom-made and designed to move teeth in small, planned steps. Most people wear each set for around 1–2 weeks, then switch to the next one.
Treatment typically starts with a 3D scan and a digital plan showing how teeth are expected to move over time. Aligners are worn for 20–22 hours per day and removed for meals and brushing. Depending on the bite and alignment, treatment often takes about 6–18 months, though complex cases can take longer.
Typical Invisalign Prices In Turkey And The UK
Exact fees vary by clinic and case, so these ranges are best used as a starting point for budgeting. A proper quote should be based on a full exam, digital scan, and a clinician-led treatment plan.
Turkey: Common Price Range
Turkey is widely chosen for clear aligners because private dentistry can be priced lower than in many Western European markets. Clinics commonly advertise entry-level Invisalign pricing from around ₺40,000 for straightforward cases, with comprehensive treatment often rising to ₺120,000+ depending on complexity and what’s included.
Some providers price Invisalign in foreign currency (or benchmark it against foreign currency) while quoting patients in Turkish Lira, which can create wide variation between clinics and cities.
UK: Common Price Range
In the UK, private Invisalign fees commonly range from about £1,500 to £5,500+ depending on the package (minor correction vs comprehensive). In higher-cost areas, especially central London, complex cases can exceed the upper end of standard ranges.
When comparing quotes, check whether retainers, refinement aligners, review appointments, and any whitening or bonding are included or billed separately.
Why Invisalign Is Often Cheaper In Turkey
The Invisalign aligners themselves are produced through Invisalign’s global manufacturing network, so the brand and materials are consistent. The price difference usually comes from local business costs and how treatment is packaged and delivered.
In Turkey, clinic rent, staffing costs, and day-to-day operating expenses are typically lower than in the UK. Turkey also has a highly competitive private dental market in major cities, and many clinics structure pricing to attract international patients.
What Can Change The Final Quote

Invisalign pricing is not one-size-fits-all. Two people treated in the same clinic can receive very different quotes because the plan, number of aligners, and chair time can differ.
Key cost drivers usually include:
- Case complexity (crowding, spacing, bite correction, jaw relationship).
- Treatment scope (single arch vs both arches).
- Number of aligners and whether refinements are expected.
- Attachments, IPR (interproximal reduction), or other adjuncts required for the plan.
- Provider experience and Invisalign certification level.
- What’s included (scans, reviews, retainers, refinements, emergency visits, aftercare).
- Clinic location and overheads (city-centre practices generally charge more).
Clinic Standards And Safety: Turkey Vs UK
Both countries have excellent providers, and both have clinics that vary in quality. The practical difference for many patients is how regulation, follow-up care, and accountability are handled locally.
In the UK, you can verify whether a dentist or orthodontist is registered via the General Dental Council (GDC). Dental practices in England are regulated by the Care Quality Commission (CQC), and inspection information is publicly available. These checks make it easier to validate credentials before committing.
In Turkey, reputable clinics will share clinician qualifications, Invisalign provider status, and clear treatment documentation. Turkey’s dental sector also publishes official tariff guidance through the Turkish Dental Association, although private clinic pricing can still vary widely.
If You’re Considering Invisalign In Turkey: Practical Planning Tips
Travelling for aligners can work well when the plan is designed around realistic review schedules. The key is making sure you can get timely advice if something needs adjusting.
Before you book, ask for:
- A written treatment plan and itemised quote (what is included and what is not).
- How many in-person visits are expected, and how remote monitoring is handled.
- Retainer plan after treatment (type, cost, and replacement policy).
- What happens if you lose an aligner or need refinements after you return home.
- Photographs of similar cases treated by the provider (with patient consent).
Get Information Now!
To request a personalised Invisalign estimate, share recent photos of your teeth (front and side), and your main concern (crowding, gaps, bite). A clinic can then confirm whether Invisalign is suitable and provide a tailored plan after a digital scan and clinical exam.
If you’re also exploring cosmetic dentistry, crowns, implants, or general dentistry, you can request an itemised treatment plan so you can compare services on a like-for-like basis.
FAQ
Is Invisalign cheaper in Turkey?
Yes, Invisalign is usually cheaper in Turkey than in the UK.
Which country has the cheapest Invisalign?
No country is consistently cheapest; pricing varies by clinic, case complexity, and promotions.
Do dentists in the UK work on teeth from Turkey?
Yes, UK dentists often treat complications from dental work abroad, but warranties rarely transfer.
Why is Invisalign so expensive in the UK?
UK Invisalign costs reflect Align fees plus higher clinical time, overheads, and economic conditions.
