Turkey Dental Veneer Prices 2026 | LYGOS DENTAL
Turkey Dental Veneer Prices 2026
Turkey dental veneer prices in 2026 typically start around ₺2,500 per tooth for composite and ₺6,500 per tooth for porcelain, with premium materials like zirconia and E.max costing more. Full smile makeover packages often fall between ₺50,000 and ₺150,000+, depending on the number of teeth, prep work, and what’s included in the package.
Table of Contents
Typical Dental Veneer Costs In Turkey In 2026
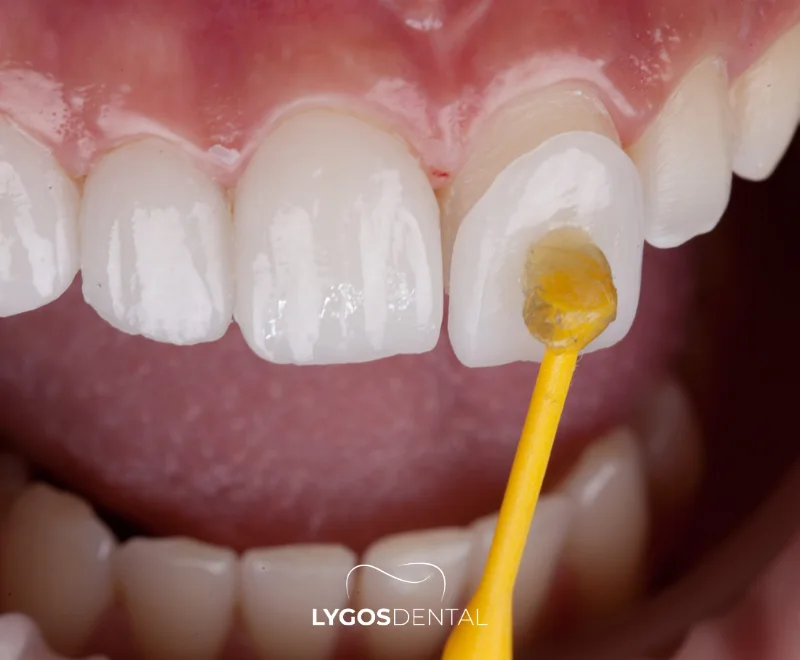
Clinics usually quote veneer pricing per tooth. Your final cost depends on the material, the amount of tooth preparation, and whether extra treatments are needed. Many clinics quote in Turkish lira (TRY) and may also offer EUR or USD pricing for international patients.
| Veneer Type (Per Tooth) | Typical Range (TRY) | Notes |
| Composite veneers | ₺2,500–₺7,500 | Budget-friendly and fast, but less stain‑resistant and shorter‑lasting than ceramics. |
| Porcelain veneers (laminate) | ₺6,500–₺15,000 | Natural look and strong. Lab quality and tooth preparation make a big difference. |
| E.max veneers (lithium disilicate) | ₺4,500–₺12,000 | Highly aesthetic ceramic often used on front teeth; pricing varies by lab and brand. |
| Zirconia veneers | ₺7,000–₺25,500 | Very strong and useful for masking darker teeth, but can look less translucent than E.max in some cases. |
Smile makeover packages are often priced as a bundle for 10–20 teeth rather than a strict per‑tooth total. If you see a very low headline price, ask what’s included (x‑rays, digital smile planning, temporary veneers, aftercare, and any warranty).Turkey Dental Veneer Prices 2025
What Is A Dental Veneer?
A veneer is a thin shell bonded to the front surface of a tooth to improve colour, shape, and minor alignment issues. Veneers can be made from composite resin or ceramics such as porcelain, zirconia, or E.max.
Veneers work best when the underlying tooth is healthy and the bite is stable. If there is active gum disease, untreated decay, or heavy grinding, those issues usually need addressing first to protect the final result.
Veneers Vs Crowns: Know What You’re Paying For
Veneers typically cover the front face of the tooth and can be conservative when planned well. Crowns cover the entire tooth and usually require more shaping.
Some “Turkey teeth” packages marketed online as veneers are actually crowns. Before you book, ask whether the plan is veneers, crowns, or a mix—and how much natural tooth reduction is expected.
Factors That Affect Dental Veneer Pricing

These are the main variables that move the cost up or down:
- Material and lab system: ceramics differ in translucency, strength, and manufacturing process.
- Number of teeth: treating more teeth increases total cost, though packages can reduce the per‑tooth price.
- Case complexity: dark discolouration, old fillings, gaps, and worn edges can require a more detailed plan.
- Extra treatments: fillings, gum contouring, bite adjustment, root canal treatment, or whitening may add cost.
- Dentist and clinic standards: experience, digital planning, and lab partnerships can affect both price and outcome.
- Clinic location: larger cities and tourist areas can be priced higher due to overhead and demand.
- Aftercare and warranty: follow‑up visits, a night guard for bruxism, and clear support policies are worth checking.
Turkey Vs Europe, The UK, And The USA
Turkey is often more affordable due to lower operating costs and currency effects, while many clinics use similar ceramic systems and digital workflows. Cost alone should not drive the decision—look at treatment planning, hygiene standards, and aftercare.
| Location | Common Per‑Tooth Range For Porcelain Veneers | What This Usually Reflects |
| Turkey | $200–$400 | High patient volume and lower overhead; prices vary by city, material, and inclusions. |
| United Kingdom | £700–£1,400 | Higher clinic and lab costs; pricing varies widely by region and ceramist level. |
| United States | $900–$2,500 | Higher chair time and lab fees; complex cases and premium labs increase costs. |
| Western Europe | €700–€1,300 | Country and city make a large difference; private cosmetic fees are typically higher than Turkey. |
These ranges are broad market averages. A proper quote should be based on an exam, x‑rays, and a clear treatment plan.
Price Differences Based On Clinic Location In Turkey
Dental veneer prices in Turkey can vary by city and district. Prices are often higher in major cities and popular tourist areas.
- Istanbul, Ankara, Izmir: often priced higher due to demand, clinic concentration, and higher operating costs.
- Antalya, Bodrum, Alanya: competitive pricing is common because of health tourism volume and package-style offers.
- Smaller cities: lower overhead can make pricing more affordable, but clinic selection matters even more.
Choose a clinic based on safety and results—not only price. Ask about sterilisation protocols, the lab they use, and what happens if a veneer chips or needs adjustment.
What’s Usually Included In Veneer Packages
Packages and quotes differ from clinic to clinic. A transparent plan usually makes it clear what you’re paying for.
- Consultation and smile assessment (photos, measurements, bite evaluation)
- X‑rays or scans if needed for planning
- Digital smile design or wax‑up (where offered)
- Temporary veneers (if required during lab work)
- Laboratory production and bonding appointment
- Post‑treatment check and minor bite adjustments
- Written aftercare guidance and clear warranty terms
Travel items (hotel, transfers) may be bundled for international patients. Medication, additional treatments, and long‑term maintenance (like a night guard) are often priced separately.
How Long Does The Dental Veneer Process Take?
Timing depends on how many teeth are being treated and whether you need extra procedures first. For straightforward veneer cases, many patients complete treatment in two main visits over several days.
Smile makeovers can take longer when gum shaping, bite changes, or healing time is needed. If you’re travelling, build in time for a final check and small adjustments before you fly home.
How Long Do Dental Veneers Last?
Longevity depends on the material, bite forces, and daily habits. As a general guide:
- Porcelain and zirconia veneers: often 10–15 years, and sometimes longer with good maintenance.
- Composite veneers: commonly 5–7 years and may need polishing or repair sooner.
To extend veneer life, keep up with routine cleanings, avoid biting hard objects, and consider a night guard if you clench or grind.
Choosing The Right Clinic And Dentist
Veneers are a precision treatment. The safest results come from careful planning, conservative tooth preparation, and good communication about the look you want.
- Ask to see real before‑and‑after cases with similar teeth to yours (not only perfect marketing photos).
- Request a written plan that lists the material, brand/lab, and exactly how many teeth are being treated.
- Check how the clinic handles occlusion (bite) and whether they provide a mock‑up or trial smile where possible.
- Confirm sterilisation standards and whether the clinic is equipped for proper diagnostics and emergency care.
- Clarify aftercare: follow‑ups, repairs, warranty terms, and what support is available once you’re back home.
Request A Quote
To receive a personalised estimate, share clear photos of your teeth and any recent x‑rays if available. A reliable clinic will confirm the final plan only after an in‑person exam.
Get Information Now!
You can contact us to learn more about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry, book an appointment, and request pricing details.
FAQ
How much does a full set of veneers cost in Turkey?
$5,000–$12,000 for 20 porcelain veneers; $300–$600 per tooth.
Which country makes the cheapest veneers?
Turkey is often cheapest; India, Thailand, and Mexico are also low-cost.
How long do Turkish veneers last?
10–15 years with good care; many last 15–20.
Do veneers in Turkey look natural?
Yes, when custom-shaded, well-contoured, and made from translucent ceramics.
Why Do Tongue Sores Occur? | LYGOS DENTAL
Why Do Tongue Sores Occur?
Tongue sores usually occur when the tongue’s surface becomes irritated or inflamed—most often from accidental biting, sharp teeth, spicy or acidic foods, or canker sores. Less commonly, infections, vitamin B12/iron/folate deficiency, allergies, or autoimmune conditions play a role. A sore that doesn’t improve within two weeks should be checked.
Table of Contents
What Is A Tongue Sore?
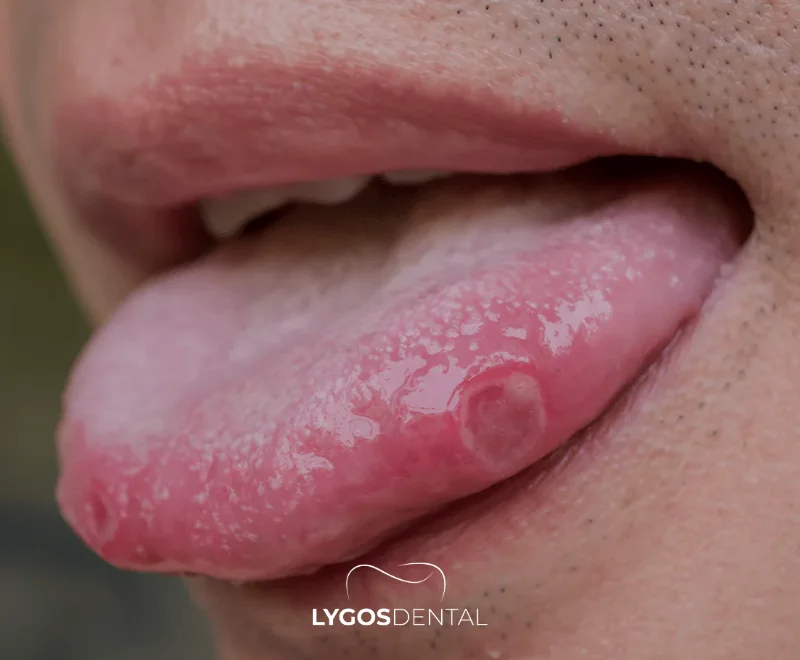
A tongue sore is a tender spot, ulcer, or inflamed area on the tongue that can sting or hurt, especially when you eat, drink, or speak. Some sores look like a small red patch, while others form a shallow crater (ulcer) with a white or yellow center. Many are harmless and temporary, but recurring or slow-healing sores can sometimes point to an underlying issue.
Common Causes Of Tongue Sores
Tongue tissue is sensitive and can react quickly to irritation. The causes below are the most common reasons people develop a painful sore on the tongue.
Minor Irritation And Trauma
Everyday injuries are a leading cause of tongue soreness. This includes biting your tongue, rubbing against a sharp tooth or filling, irritation from braces, or pressure from an ill‑fitting denture.
- Accidental biting during eating or sleeping
- Hard, sharp, or crunchy foods (chips, crusty bread)
- Burns from very hot foods or drinks
- Friction from dental appliances (braces, aligners, dentures)
Canker Sores (Aphthous Ulcers)
Canker sores are small, round or oval ulcers that can appear on the tongue and other soft tissues in the mouth. They are not contagious, but they can be very painful. Many cases heal on their own within about 7–14 days.
Common triggers include:
- Stress and poor sleep
- Minor mouth trauma
- Certain foods (especially acidic foods)
- Hormonal changes
- A family tendency to get canker sores
Food And Chemical Irritants
Spicy, acidic, or very salty foods can inflame the tongue’s surface and make small breaks in the tissue feel worse. Alcohol-containing mouthwashes and strong whitening products can also irritate sensitive mouths.
Infections (Viral, Fungal, Or Bacterial)
Some tongue sores are related to infections. Cold sores (herpes simplex) can cause painful blisters and ulcers in or around the mouth and may be contagious. Oral thrush (a yeast infection) can also cause soreness and a burning feeling, often with white patches.
If you suspect an infection, avoid sharing utensils, cups, or towels until you’re assessed.
Vitamin And Mineral Deficiencies
Low levels of vitamin B12, iron, or folate can affect the lining of the mouth and contribute to a sore or inflamed tongue. If tongue sores are frequent, a clinician may recommend blood tests to check for deficiencies.
Stress, Smoking, And Alcohol
Chronic stress can be linked to recurring mouth ulcers for some people. Tobacco and alcohol can irritate the oral tissues and slow healing, especially if sores keep returning.
Allergies And Sensitivities
Some people react to ingredients in toothpaste, mouthwash, or certain foods. Flavourings, strong detergents, and preservatives can trigger soreness or ulcer-like lesions in sensitive individuals.
Medical Conditions That Can Show Up In The Mouth
Recurrent tongue sores can occur with certain systemic conditions such as Behçet’s disease, coeliac disease, inflammatory bowel disease (Crohn’s disease), and lupus. These conditions usually come with other symptoms beyond the mouth, so a broader medical review may be needed if sores are persistent or frequent.
Symptoms You Might Notice

Tongue sores can look and feel different depending on the cause. Common symptoms include:
- A red, tender spot on the tongue
- A shallow ulcer with a white or yellow center
- Burning or stinging sensations
- Pain when eating, drinking, or speaking
- Swelling or a rough feeling on the tongue
- Changes in taste or increased sensitivity to certain foods
What Helps Tongue Sores At Home?
Most minor tongue sores improve with simple care and a little time. The goal is to reduce irritation, keep the area clean, and manage pain while the tissue heals.
Home care options include:
- Salt-water rinse (½ teaspoon of salt in a glass of warm water) 2–3 times a day
- Baking soda rinse to soothe irritation and balance oral pH
- A cold compress or sucking on ice chips to reduce discomfort
- A bland, soft diet for a few days (avoid spicy, acidic, and very hot foods)
- Gentle brushing and flossing; switch to a soft-bristled toothbrush if needed
Some people also find aloe vera gel or a small amount of honey soothing when applied to the sore. (Honey should not be given to children under 12 months.)
When To See A Dentist Or Doctor
Get professional advice if a tongue sore is severe, keeps coming back, or doesn’t improve as expected. A clinician can check for dental causes (like a sharp edge), signs of infection, and less common conditions that need treatment.
Seek an assessment sooner if you notice:
- A sore that lasts longer than two weeks
- Rapidly increasing size, significant swelling, or worsening pain
- Bleeding, numbness, or a hard lump in the tongue or neck
- Fever, rash, or difficulty swallowing
- Unexplained weight loss or persistent hoarseness
Medications and Treatments for Tongue Sores

Treatment depends on the underlying cause. After an exam, a dentist or doctor may recommend one or more of the options below.
- Protective gels or mouth rinses to reduce pain and irritation
- Topical steroid medications for painful canker sores (when appropriate)
- Antiviral medication if lesions are due to herpes
- Antifungal treatment for oral thrush
- Vitamin or iron supplementation if a deficiency is confirmed
- Adjusting or polishing a sharp tooth, filling, or denture edge that is repeatedly rubbing the tongue
- Low-level laser therapy in selected cases of recurrent ulcers (availability varies)
How To Prevent Tongue Sores
Not every tongue sore is preventable, but a few habits lower the odds of recurrence. Focus on reducing irritation and supporting good oral and general health.
- Keep up with regular dental checkups and cleanings
- Treat sharp teeth, rough fillings, or ill-fitting appliances promptly
- Limit spicy and acidic trigger foods during flare-ups
- Stay hydrated and consider a saliva-friendly routine if you have dry mouth
- Manage stress and prioritize sleep
- Avoid tobacco and limit alcohol
- Eat a balanced diet; ask about blood tests if you have repeated mouth ulcers
FAQ
What causes sores on your tongue?
Aphthous ulcers, trauma, infections, allergies, irritants, and nutritional deficiencies commonly cause tongue sores.
How can you get rid of tongue sores?
Rinse saltwater, avoid irritants, use topical anesthetic, and see a dentist if persistent.
How long do tongue sores usually last?
Most heal within 7–14 days; longer than two weeks needs evaluation.
How should I treat a tongue sore?
Use saltwater rinses, topical numbing gel, soft foods, and avoid spicy or acidic items.
Can stress cause sores on my tongue?
Yes, stress can trigger or worsen aphthous ulcers on the tongue.
Why Are Dental Crowns So Expensive? | LYGOS DENTAL
Why Are Dental Crowns So Expensive?
Dental crowns cost more because they’re custom-made restorations that involve clinical time, precise tooth preparation, digital scans or impressions, temporary crowns, and lab fabrication. Material choice (ceramic, zirconia, gold), the skill of the dentist and technician, clinic overhead, and insurance limits all affect the final price.
Table of Contents
What A Dental Crown Is And When You Need One
A dental crown is a tooth-shaped “cap” that covers and protects a damaged tooth or restores a dental implant. Unlike a veneer, which bonds to the front surface only, a crown wraps around the whole tooth above the gumline.
Dentists recommend crowns when a tooth needs strength as well as a better appearance. Common reasons include a large filling that weakens the tooth, cracks or fractures, severe wear, or protection after root canal treatment.
Crowns may also be used to:
- Restore a broken tooth that can’t be repaired with a simple filling
- Hold a dental bridge in place
- Cover a badly misshapen or severely discolored tooth when other options won’t last
- Protect a tooth that has been heavily worn down
What You’re Paying For In A Crown Procedure
A crown isn’t a single product—it’s a sequence of appointments and steps that need accuracy. Your quote usually includes more than the crown itself, such as:
- Diagnosis and treatment planning (exam, X-rays, and sometimes digital scans)
- Tooth preparation and shaping so the crown fits properly
- Impressions or intraoral scanning, plus bite records
- A temporary crown to protect the tooth while the final crown is made
- Dental laboratory design and fabrication (or in-office milling when available)
- Final fitting, cementation, and any adjustments for comfort and bite
Key Factors That Drive Crown Pricing
Material And Manufacturing Quality
Crown materials vary in cost, appearance, and strength. Higher-end ceramics can look extremely natural, but they often require premium materials and more detailed lab work.
Common crown options include:
- All-ceramic or porcelain crowns (natural look, often chosen for front teeth)
- Zirconia crowns (very strong, often used for back teeth or people who grind)
- Porcelain-fused-to-metal (PFM) crowns (a metal core with porcelain on top)
- Full metal crowns such as gold alloys (durable, less common for visible teeth)
- Resin/composite crowns (typically used as temporary or lower-cost options)
Dental Lab Fees And Craftsmanship
Most crowns are made by a dental laboratory, and you’re paying for skilled technical work and quality control. A lab that focuses on lifelike shading, accurate margins, and strong materials will typically charge more than a low-cost, high-volume lab.
Digital Dentistry And Equipment Costs
Digital scanners and CAD/CAM systems can improve fit and reduce remakes, but the equipment and maintenance are expensive. Some clinics pass part of that investment into the crown fee, especially for same-day crowns.
Case Complexity And Extra Treatments
A crown can be straightforward, or it can involve extra steps to make the tooth stable and healthy. Costs often increase when you also need a buildup, post-and-core, gum treatment, or root canal therapy.
Dentist Experience And Remakes
Crowns depend heavily on preparation design, bite management, and finishing. Experienced clinicians may charge more, but their work can reduce the risk of sensitivity, poor fit, and early failure. If a crown needs to be remade due to fit or aesthetics, that adds time and lab cost.
Clinic Location And Overhead
Practice overhead matters. City-center rent, staffing, sterilization standards, modern imaging, and high-quality materials all influence pricing. Even with the same crown material, fees can vary widely by region.
Insurance And Coverage Limits
Dental insurance may cover crowns when they’re medically necessary, but coverage varies by plan. Many policies pay a percentage after deductibles and apply annual maximums, which can leave a large out-of-pocket balance.
If a crown is considered cosmetic, coverage may be limited or excluded. It’s worth asking for a pre-treatment estimate so you know what your plan is likely to pay before you schedule treatment.
How To Lower Your Out-Of-Pocket Cost Without Cutting Corners
If cost is a concern, these steps can help you make a safer, smarter decision:
- Ask for an itemized treatment plan (crown, buildup, temporary, imaging, lab fees)
- Check in-network options and request a pre-authorization or pre-treatment estimate
- Discuss material choices that fit your case and budget (for example, PFM vs all-ceramic in some situations)
- Ask about payment plans or whether you can use HSA/FSA funds if applicable
- Protect your investment with good hygiene and a night guard if you clench or grind
Alternatives To Crowns When Appropriate
A crown isn’t always the only option. The right alternative depends on how much tooth structure is missing and where the tooth sits in your bite.
- Bonding or a filling for small chips and limited decay
- Inlays or onlays for moderate damage where the tooth walls are still strong
- Veneers for front-tooth cosmetic concerns when the tooth doesn’t need full coverage
- Whitening for discoloration when the tooth structure is otherwise healthy
A dentist should confirm whether an alternative will hold up long-term. Choosing a cheaper option that fails early can end up costing more overall.
Get Information Now
Contact us to learn more about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry. We can review your options and explain what affects your treatment cost.
FAQ
Why do dentists charge such high fees for crowns?
Crowns cost more due to labs, materials, equipment, staff, time, and overhead.
Why do dentists insist on placing crowns?
Crowns protect weakened teeth from fracture, restore function, and seal large restorations.
Are crowns more expensive than root canal treatment?
Yes; crowns often cost similar or more than a root canal per tooth.
The Effects of Stress on Dental Health | LYGOS DENTAL
The Effects of Stress on Dental Health
Stress can affect your teeth and gums by increasing jaw clenching, reducing saliva, and making the immune response less effective. It can also lead to skipped brushing, more sugary snacks, and more frequent mouth sores. Over time, this may cause sensitivity, cavities, gum bleeding, and jaw pain. Stress control and consistent dental care help protect your smile.
Stress is part of modern life, but its impact isn’t limited to sleep, mood, or blood pressure. Your mouth often shows the effects early, sometimes before you notice anything else.
From teeth grinding to dry mouth, stress can create conditions that make cavities, gum irritation, and mouth sores more likely. Knowing what to watch for helps you protect your dental health even during busy or difficult periods.
Table of Contents
What Is The Connection Between Stress And Dental Health?
When you’re stressed, your body releases stress hormones such as cortisol and activates the “fight-or-flight” response. This can influence inflammation and how well your immune system responds to bacteria in the mouth.
Stress also changes daily routines. People often brush and floss less carefully, snack more frequently, or reach for sugary drinks. Those habit shifts, combined with dry mouth or jaw clenching, can accelerate dental problems.
Dental Health Problems Linked To Stress

Stress can contribute to several oral health issues. These are the most common problems dentists see when stress levels run high:
Teeth Grinding And Clenching (Bruxism)
Many people grind or clench their teeth during sleep or while concentrating. Over time, this can wear enamel, cause cracks, trigger headaches, and lead to jaw or TMJ pain.
Gum Inflammation And Gum Disease
Ongoing stress may make gums more sensitive to plaque and inflammation. If brushing and flossing slip, gingivitis can progress and gum pockets may deepen.
Dry Mouth (Xerostomia)
Stress and anxiety can reduce or change saliva flow. With less saliva to wash away food and neutralize acids, bad breath and cavities become more likely.
Mouth Sores And Cold Sores
Stress can be a trigger for canker sores, and it can also contribute to cold sore flare-ups in people who carry the virus. Sores may feel more painful and take longer to settle when you’re run down.
Tooth Decay
Cavities become more likely when dry mouth, frequent snacking, and inconsistent brushing happen at the same time. Early decay may show up as sensitivity, rough spots, or dark areas on a tooth.
How To Manage Stress And Protect Your Oral Health

You don’t need a perfect routine to protect your teeth—you need a consistent one. These steps make a real difference during stressful seasons:
- Brush twice a day with fluoride toothpaste and clean between teeth daily.
- If you notice jaw tightness or morning headaches, ask your dentist about a custom night guard.
- Stay hydrated and limit caffeine and alcohol if dry mouth is a problem.
- Choose tooth-friendly snacks (cheese, nuts, yogurt, crunchy vegetables) instead of sticky sweets.
- Keep regular dental checkups so problems are caught early, before they become painful or expensive.
Stress And Mouth Sores: Canker Sores Vs. Cold Sores
Canker sores are small ulcers that form inside the mouth. They are not contagious, but they can be painful—especially with spicy or acidic foods.
Cold sores usually appear on or around the lips and are linked to the herpes simplex virus. Stress, illness, and sun exposure can all contribute to flare-ups.
If sores are frequent, unusually large, or last longer than two weeks, it’s worth getting checked. Your dentist can help rule out irritation from braces, nutritional issues, or other causes.
Indirect Effects On Tooth Color And Smile Aesthetics
Stress-related grinding can flatten biting edges and create tiny cracks that trap stain. Dry mouth can also make plaque build up faster, which may dull the look of teeth.
If you’re seeing more yellowing, focus on hydration, daily plaque removal, and limiting frequent sipping of coffee, tea, or soda. Your dentist can recommend safe whitening options if needed.
Stress-Relief Habits That Support Oral Health
Simple habits that lower stress can reduce clenching and help you stick to oral care. Aim for small, repeatable routines rather than big lifestyle overhauls.
- A short daily walk, stretching, or light exercise to lower muscle tension
- Breathing exercises or meditation, especially before bed
- Better sleep hygiene (consistent bedtime, less screen time late at night)
- Cutting back on tobacco and limiting alcohol, which can worsen dry mouth
When To See A Dentist
Make an appointment if you notice any of the following:
- Tooth sensitivity that doesn’t improve after a week
- Jaw pain, clicking, or headaches on waking
- Bleeding gums or persistent bad breath
- New cracks, chips, or flat spots on teeth
- Mouth sores that last longer than two weeks
Book An Appointment
If you’d like support with cosmetic dentistry, dental crowns, dental implants, or general dentistry, reach out to our team to schedule a visit.
FAQ
Can stress affect dental health?
Yes; stress increases bruxism, dry mouth, gum inflammation, and cavity risk.
How is stress-related teeth grinding treated?
Treat with nightguard, stress management, jaw therapy, sleep optimization, and dental bite correction.
How can I tell if I grind my teeth?
Signs include morning jaw pain, headaches, tooth wear, cracks, and partner-reported grinding sounds.
Can an Infected Tooth Be Extracted? | LYGOS DENTAL
Can an Infected Tooth Be Extracted?
Yes. Dentists can usually extract an infected or abscessed tooth, but the safest timing depends on how far the infection has spread and whether the tooth can be saved. Your dentist may first reduce swelling and pain, sometimes with drainage or medication, then remove the tooth under local anesthesia and give clear aftercare instructions.
A tooth infection is not something to “wait out.” Besides causing intense pain, it can spread into the jaw, face, and other areas. If you have facial swelling, fever, trouble swallowing, or difficulty breathing, seek urgent dental or medical care.
Table of Contents
What Is An Infected Tooth?
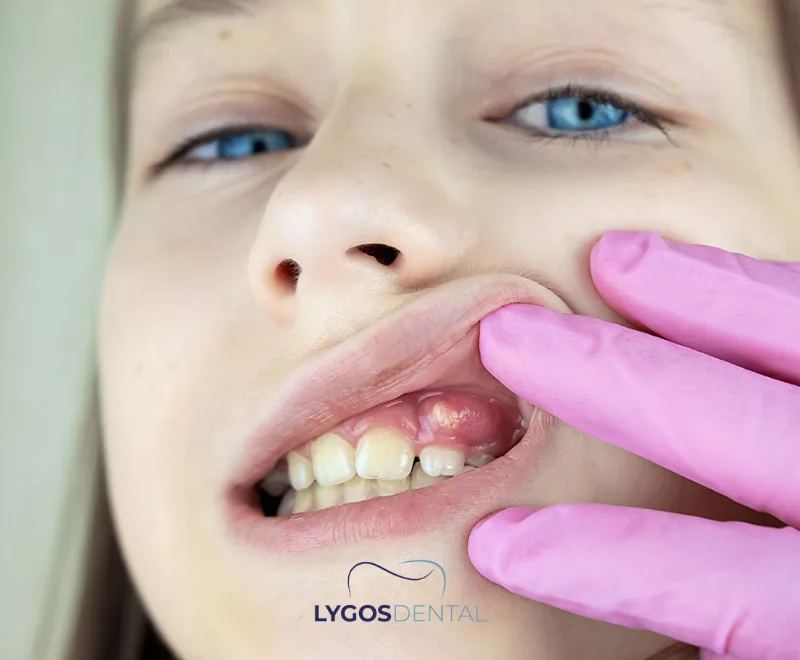
An infected tooth develops when bacteria reach the pulp (the inner tissue containing nerves and blood vessels) or the tissues around the root. This often happens after deep decay, a cracked tooth, a failed filling, or advanced gum disease. When infection builds pressure inside the tooth or around the root, you can develop an abscess (a pocket of pus).
Common Symptoms
People describe symptoms differently, but these are common signs of a dental infection:
- Persistent throbbing toothache or pain when biting
- Sensitivity to hot, cold, or sweet foods and drinks
- Swollen, tender gums or a pimple-like bump on the gum (draining abscess)
- Bad taste in the mouth or bad breath that doesn’t improve with brushing
- Swelling of the jaw, cheek, or face; sometimes enlarged lymph nodes
If these symptoms are present, a dentist will usually examine the tooth and take an X‑ray to see how far the infection extends.
Can An Infected Tooth Be Extracted Safely?
In most cases, yes—an infected tooth can be extracted safely. The decision comes down to three practical questions:
- Can the tooth be predictably saved with treatment such as root canal therapy and a crown?
- Is the infection localized, or is there significant facial swelling or spreading infection?
- How complex is the extraction (simple removal vs. surgical extraction), and what is your overall medical history?
When a Tooth Is Usually Saved Instead Of Removed
If enough healthy tooth structure remains and the roots are stable, your dentist may recommend root canal treatment to remove the infected pulp and seal the tooth. This preserves your natural bite and can be the best option for many molars and premolars.
When Extraction Is Often The Best Option
Extraction is more likely when the tooth is badly broken, severely decayed below the gumline, has advanced bone loss, or has a crack that extends into the root. Your dentist may also recommend extraction if the tooth has repeated infections or cannot be restored reliably.
How Dentists Manage Infection Before Extraction
If there is significant swelling, drainage, or signs the infection is spreading, your dentist may focus on calming things down first. Depending on the situation, this can include:
- Draining the abscess (when needed) to relieve pressure
- Medication for pain and inflammation
- Antibiotics in specific cases—especially when there is fever, facial swelling, or risk of spread
Antibiotics are not always required for every tooth infection. The right approach depends on your symptoms and exam findings.
What Happens During An Infected Tooth Extraction
Most extractions are done with local anesthesia, so you should feel pressure but not sharp pain. A typical visit may include:
- Numbing the area and checking that you’re comfortable
- Loosening the tooth and removing it (or performing a small surgical procedure if the tooth is broken or impacted)
- Cleaning the socket and placing gauze to control bleeding
- Post‑op instructions and, when appropriate, a plan to replace the tooth (implant, bridge, or other option)
Healing And Aftercare
Healing is usually straightforward when aftercare is followed. Common guidance includes:
- Bite on gauze as directed and avoid vigorous rinsing for the first 24 hours to protect the blood clot
- Use cold compresses for swelling during the first day, then switch to gentle warmth if advised
- Stick to soft foods, avoid smoking and straws, and keep the area clean with gentle rinses after the first day
- Take prescribed medications exactly as directed
Call your dentist promptly if you have worsening swelling after the first 48–72 hours, uncontrolled bleeding, severe increasing pain, fever, or pus-like drainage.
Possible Risks And Complications
Dentists extract infected teeth every day, but any procedure carries some risk. Potential complications include:
- Dry socket (painful clot loss), more common after lower molar extractions
- Temporary swelling, bruising, or stiffness
- Infection that persists or returns, especially if drainage is limited
- Sinus involvement for upper back teeth, in rare cases
- Nerve irritation or numbness, usually temporary, for certain lower teeth
A proper exam and imaging help reduce these risks and guide the safest plan.
Cost Factors
Extraction fees vary widely by country, clinic type, and complexity. The final cost typically depends on:
- Simple vs. surgical extraction
- Tooth location (front teeth are often simpler than molars)
- Need for imaging, medication, or drainage
- Sedation options, if chosen
- Follow‑up care and tooth replacement planning
For an accurate estimate, you’ll need an in‑person evaluation.
FAQ
What happens if an infected tooth is extracted?
Extraction removes the source; infection usually resolves with drainage and sometimes antibiotics.
Will a dentist extract an infected tooth?
Yes, dentists can extract infected teeth, often with antibiotics or drainage first.
What are the symptoms of sepsis caused by a tooth infection?
High fever, fast heart rate, fast breathing, confusion, severe weakness, low blood pressure.
How does a serious tooth infection feel?
It feels like worsening throbbing tooth pain with swelling, pressure, bad taste, sometimes fever.
What is the 3-3-3 rule for toothache?
It’s a common pain tip: 600mg ibuprofen three times daily for three days maximum.
How to Relieve a Toothache That Keeps You Awake
How To Relieve A Toothache That Keeps You Awake
If a toothache keeps you awake, start with safe, temporary relief: rinse with warm salt water, apply a cold compress to the cheek, and use an over-the-counter pain reliever as directed on the label. Sleep with your head slightly elevated and avoid sugary or very hot foods. If you have swelling, fever, or worsening pain, contact a dentist urgently.
Nighttime tooth pain can feel intense because you have fewer distractions, and lying down may increase blood flow and pressure in the head. The tips below can help you get through the night, but they do not replace a dental exam. Persistent or severe pain usually means there is an underlying issue that needs treatment.
Table of Contents
Why Tooth Pain Often Feels Worse At Night

When you lie flat, blood pressure can rise in the head and jaw, which may make inflamed tissues throb. You may also notice pain more at night because the house is quiet and you are not focused on other tasks. Dry mouth during sleep can worsen gum irritation and make sensitive teeth feel sharper.
Common Causes Of A Toothache That Disrupts Sleep
- Tooth decay: A cavity can reach the inner tooth, irritating the nerve and causing sharp or lingering pain.
- Gum inflammation or infection: Gingivitis or periodontitis can trigger soreness, swelling, and tenderness around the tooth.
- Cracked, broken, or loose fillings: Damage can expose sensitive layers and create pain with biting or temperature changes.
- Tooth abscess: Infection around the tooth root can cause severe, pulsing pain and sensitivity.
- Teeth grinding (bruxism): Night grinding strains teeth and jaw muscles and can make teeth feel achy in the morning.
- Sinus pressure: Congested sinuses can refer pain to the upper back teeth, especially when you lie down.
- Erupting or impacted wisdom teeth: Pressure and trapped food can inflame the gums at the back of the mouth.
What To Do Right Now To Calm Nighttime Tooth Pain
1) Rinse Gently
Swish warm salt water for 30 seconds, then spit it out. This can help reduce irritation and wash away debris. Avoid vigorous gargling if your gums are sore.
2) Use A Cold Compress On The Cheek
Hold a cold pack on the outside of the cheek for 10–15 minutes, then take a break. Cold can reduce swelling and dull pain signals. Do not place ice directly on the tooth or gum tissue.
3) Take An Over-The-Counter Pain Reliever Safely
If you can take it safely, use an over-the-counter pain reliever according to the product label or your clinician’s advice. Avoid doubling up medications that contain the same active ingredient. If you are pregnant, on blood thinners, or have stomach, kidney, or liver conditions, check with a healthcare professional first.
4) Elevate Your Head
Prop up your head with an extra pillow to reduce throbbing. Sleeping slightly upright can decrease pressure in the painful area and make it easier to doze off.
5) Avoid Triggers Before Bed
Skip very hot, very cold, or sugary foods and drinks. If chewing hurts, eat softer foods and chew on the opposite side. If something is stuck, use floss gently—do not dig into the gum with sharp objects.
What Not To Do
- Do not place aspirin directly on the tooth or gums; it can burn soft tissue.
- Do not apply heat to a swollen face, as warmth may worsen some infections.
- Do not ignore persistent pain—temporary relief can mask a problem that needs treatment.
- Do not use alcohol as a mouth rinse, especially on irritated gums.
When To Seek Urgent Dental Care
Book an urgent dental appointment if pain is severe, wakes you repeatedly, or lasts more than 24–48 hours. Seek urgent help sooner if you notice facial swelling, fever, a bad taste or pus, difficulty swallowing or breathing, or pain after a recent dental procedure that is getting worse.
Dental Treatments That Stop Toothache At The Source
Your dentist will identify the cause and recommend treatment. Fixing the underlying issue is the only reliable way to stop the pain from returning.
- Filling or crown: Repairs decay or fractures and protects the tooth.
- Root canal treatment: Removes infected nerve tissue and seals the tooth when the pulp is affected.
- Gum therapy: Deep cleaning and targeted care reduce infection around the roots.
- Extraction: May be recommended if a tooth cannot be saved.
- Night guard: Protects teeth if grinding is the trigger.
Home Remedies: Helpful Support, Not A Cure

Some home options may offer short-term comfort while you arrange dental care. Use them cautiously and stop if they irritate your mouth.
- Clove oil (diluted): Dab a small amount on a cotton swab and apply to the tooth, not the gums.
- Peppermint tea bag: Let it cool, then hold it against the sore area for a few minutes.
- Warm water rinse: Simple warm water can soothe when salt water feels too strong.
How To Reduce The Chances Of Another Nighttime Toothache
Brush twice daily with a fluoride toothpaste and clean between teeth once a day. If you have sensitive teeth, choose a sensitivity-focused toothpaste and use a soft-bristled brush with gentle pressure. Limit frequent sipping of acidic or sugary drinks, and keep regular dental checkups so small issues do not turn into emergencies.
Need Help Today?
If you have persistent tooth pain, schedule a dental evaluation as soon as possible. A prompt exam can prevent complications and get you lasting relief.
FAQ
What should you do if you can’t sleep due to toothache?
Take ibuprofen/acetaminophen if safe, use cold compress, saltwater rinse, elevate head, call dentist.
What should you do for severe toothache at night?
Seek urgent dental care; take ibuprofen/acetaminophen if safe, rinse with saltwater, cold compress.
What is the 3-3-3 rule for toothache?
600 mg ibuprofen three times daily for three days maximum, if safe for you.
What relieves nerve pain in the tooth?
Root canal or extraction relieves tooth nerve pain; until then use ibuprofen/acetaminophen if safe.
Advantages of Zirconium Dental Crowns
Advantages Of Zirconium Dental Crowns
Zirconium (zirconia) dental crowns are all-ceramic restorations known for a natural, light-reflecting look and strong bite resistance. They are gum-friendly, metal-free, and less likely to cause temperature sensitivity than metal-supported options. For many patients, they provide a durable, aesthetic solution for damaged, stained, or heavily restored teeth.
Table of Contents
What Are Zirconium Dental Crowns?
A zirconium dental crown is made from zirconium dioxide (zirconia), a white, high-strength ceramic used widely in modern dentistry. Because it contains no metal, it avoids the dark gum-line shadow sometimes seen with metal-supported crowns. Its semi-translucent structure helps the crown blend with nearby teeth for a more natural finish.
When Are Zirconium Crowns Recommended?
Zirconium crowns are commonly used when a tooth needs both strength and an aesthetic upgrade, such as:
- Severely discolored or darkened teeth that don’t respond well to whitening
- Broken, cracked, or worn teeth that need full coverage
- Cosmetic reshaping when orthodontics isn’t preferred or isn’t suitable
- Replacing old crowns that look unnatural or irritate the gums
Key Advantages Of Zirconium Crowns

Zirconium crowns are suitable for individuals of all ages with high aesthetic concerns. They are especially recommended for people with:
- Aesthetic expectations,
- Crooked or misaligned teeth,
- Tooth discoloration issues,
- Wide gaps between teeth,
- Broken or worn tooth structure,
- Dissatisfaction with previous metal-supported crowns.
Thanks to the advantages of zirconium crowns, they can also be safely used for individuals with sensitive gums.
Zirconium Dental Crown Prices in 2025
As of 2025, the cost of zirconium dental crowns can vary depending on the quality of material used, the number of crowns, the dentist’s experience, and the clinic’s location.
Generally, the price for a single zirconium crown ranges between 3,000 TL and 7,500 TL. Some clinics may also offer package deals for multiple teeth (e.g., 6 or 8 crowns).
Considering the advantages of zirconium crowns, their long lifespan and aesthetic benefits make them a cost-effective investment.
Post-Treatment Care for Zirconium Crowns
Natural-Looking Aesthetics
Zirconia can be layered or shaded to match surrounding teeth closely. Because it is metal-free, it doesn’t create gray reflections at the gum margin. This is especially valuable for visible front teeth and smile makeovers.
High Strength And Long-Term Performance
Zirconium crowns are designed to handle chewing forces well and can be suitable for both front and back teeth. Longevity depends on bite habits, crown design, and oral hygiene, but many patients use them for years without issues. Your dentist will check your bite to reduce the risk of chipping or wear.
Gum Compatibility And Low Allergy Risk
Zirconia is biocompatible, meaning it is generally well tolerated by soft tissues. For patients who are sensitive to metals or have a history of gum irritation, zirconium crowns are often a comfortable option. A precise fit and good plaque control still matter for keeping gums healthy.
Lower Temperature Sensitivity
Compared with metal-supported crowns, zirconium typically transmits temperature less. That can help reduce discomfort with hot or cold foods, particularly for people with sensitive teeth. Sensitivity can still occur if the tooth nerve is inflamed or if the bite needs adjustment.
Stain Resistance And Easy Maintenance
Zirconium crowns are resistant to staining from everyday foods and drinks such as tea and coffee. They don’t discolor the way some older materials can over time. Routine brushing, flossing, and professional cleaning keep the margins healthy and the smile bright.
Zirconium Vs Porcelain Crowns

The right crown depends on aesthetics, bite forces, gum health, and budget. Traditional porcelain crowns are often supported by metal, which can create a dark line near the gums and may affect light reflection. Zirconium crowns are fully ceramic, so they typically offer a more natural look at the gumline.
For front teeth, zirconium is frequently chosen for its light-handling and lifelike appearance. For back teeth, the decision may depend on your bite, grinding habits, and how much tooth structure remains. A dentist can recommend the most suitable material after an examination.
Who Is Suitable For Zirconium Crowns?
Zirconium crowns can be a good fit for many adults who want a durable, natural-looking result, including those with:
- High aesthetic expectations (especially for front teeth)
- Misaligned teeth that need cosmetic correction
- Persistent tooth discoloration
- Gaps that require restorative reshaping
- Broken, chipped, or heavily filled teeth
- Unwanted appearance or gum irritation from older metal-supported crowns
They can also be appropriate for people with sensitive gums, as long as daily cleaning and regular check-ups are maintained.
Zirconium Dental Crown Prices In 2026
Pricing varies by clinic, location, dentist experience, lab quality, and the type of zirconia used (standard, multilayer, or premium options). The final cost can also change if additional treatments are needed, such as root canal therapy, gum treatment, or a build-up under the crown.
In Turkey, clinics may quote a per-tooth zirconium crown price in a broad range—often roughly 7,500 TL to 15,000 TL. Some clinics offer package pricing when multiple crowns are planned. For an accurate quote, a clinical examination and treatment plan are essential.
Aftercare And Maintenance
Good aftercare helps crowns last longer and keeps the gums around them healthy:
- Brush twice daily and clean between teeth with floss or interdental brushes
- Use an alcohol-free mouthwash if recommended by your dentist
- Attend routine check-ups and professional cleanings (commonly twice a year)
- Avoid chewing very hard items such as ice or unpopped kernels
- If you grind your teeth, ask about a night guard to protect the crowns and your natural teeth
Book A Consultation
If you’re considering zirconium crowns, a consultation helps confirm whether they’re the right option for your teeth and bite. Your dentist can explain the expected outcome, number of appointments, and alternative treatments based on your needs.
FAQ
What are the disadvantages of zirconia crowns?
Disadvantages include lower translucency, difficult adjustments, potential opposing-tooth wear, and possible cementation issues.
How long do zirconia crowns last?
Usually 10–15 years; many last 15–20+ with good hygiene and bite.
Why do zirconia crowns fall out?
They fall out from poor fit, cement failure, decay, short tooth prep, or bruxism.
Do teeth decay under crowns?
Yes; decay can occur at crown margins if the seal leaks or hygiene is poor.
What is the best toothpaste for zirconia crowns?
Use a non-abrasive fluoride toothpaste; avoid harsh whitening or charcoal pastes.
Common Oral and Dental Health Mistakes
Common Oral And Dental Health Mistakes
Most dental problems start with everyday habits: rushing your brushing, scrubbing with a hard brush, skipping interdental cleaning, sipping sugary or acidic drinks, and delaying dental check-ups. Gentle brushing for two minutes with fluoride toothpaste, daily flossing, smarter snacking, and regular exams help protect enamel, gums, and breath.
Table of Contents
Tooth Brushing Mistakes
Brushing Too Quickly
Brushing for a few seconds rarely removes plaque along the gumline and between teeth.
Aim for about two minutes, covering every surface: outer, inner, and chewing surfaces, plus the tongue for fresher breath.
Brushing Too Hard Or Using Hard Bristles

Scrubbing aggressively or using a hard-bristled brush can wear enamel and irritate gums.
Use a soft-bristled brush and gentle pressure. If your bristles splay out quickly, you’re likely brushing too hard.
Not Replacing Your Toothbrush Regularly
A worn brush cleans less effectively and can harbor bacteria.
Replace your toothbrush or electric brush head every 3–4 months, or sooner if the bristles are frayed or after illness.
Brushing Right After Acidic Foods Or Drinks
Acidic items like citrus, soda, sports drinks, wine, and sour candies can temporarily soften enamel.
Brushing immediately afterwards may increase enamel wear. Rinse with water first and wait about 30–60 minutes before brushing.
Brushing Before Or After Breakfast
Brushing before breakfast removes overnight plaque and leaves a protective fluoride layer on the teeth.
If you prefer brushing after breakfast, wait about 30 minutes after eating (especially after coffee, juice, or fruit) so enamel isn’t softened by acids.
Ignoring Your Gumline
Plaque tends to collect where teeth meet gums, which can trigger bleeding and inflammation.
Angle your brush slightly toward the gumline and make small, gentle strokes rather than wide scrubbing motions.
Skipping Your Tongue
The tongue can hold bacteria that contribute to bad breath and coating.
Brush your tongue gently or use a tongue scraper once a day.
Flossing And Interdental Cleaning Mistakes
Not Flossing At All
A toothbrush can’t clean between teeth where plaque often hides.
Clean between teeth daily using floss, interdental brushes, or water flossers—choose what you can do consistently.
Flossing Too Hard
Snapping floss down can cut gums and make flossing unpleasant.
Guide floss gently between teeth, curve it into a “C” shape around each tooth, and slide it up and down.
Only Flossing When Food Gets Stuck
Interdental cleaning isn’t just for removing food—it removes plaque that contributes to cavities and gum disease.
Make it a daily habit, even if you don’t feel anything stuck.
Mouthwash Mistakes
Using Mouthwash As A Substitute For Brushing
Mouthwash can support oral hygiene, but it doesn’t remove plaque like brushing and flossing.
Use it as an add-on, not a replacement—especially if you’re prone to gum inflammation or cavities.
Rinsing Right After Brushing With Fluoride Toothpaste
Rinsing immediately after brushing can wash away fluoride, reducing its protective benefit.
Spit out toothpaste after brushing and avoid rinsing for a while so fluoride can stay on the teeth longer.
Overusing Strong Antiseptic Mouthwashes
Frequent use of strong antiseptic rinses can cause dryness or irritation for some people.
Follow the label directions. If your dentist recommends one, it’s often for short-term use.
Diet And Lifestyle Mistakes
Frequent Snacking And Sipping Sugary Drinks
Each snack or sugary drink can start an “acid attack” that weakens enamel.
Try to limit grazing. Drink water between meals and keep sugary or acidic drinks to mealtimes when possible.
Too Many Acidic Foods And Drinks
Acidic choices can soften enamel, especially when consumed often.
Use a straw for acidic drinks, rinse with water after, and avoid brushing right away.
Not Drinking Enough Water
Saliva helps neutralize acids and wash away food particles.
Staying hydrated supports saliva flow and can help reduce dry mouth and bad breath.
Smoking Or Vaping
Tobacco and nicotine products can increase staining, dry mouth, gum disease risk, and slower healing.
Quitting or cutting back can improve gum health and reduce oral health complications over time.
Skipping Dental Visits And Early Warning Signs
Waiting Until Pain Starts
Many dental problems don’t hurt until they’re advanced.
Regular check-ups help catch decay and gum disease early, when treatment is simpler and less costly.
Ignoring Bleeding Gums
Bleeding during brushing or flossing is often a sign of gum inflammation.
If it persists for more than a week or two despite improved cleaning, book a dental visit to assess gum health.
Not Addressing Tooth Sensitivity
Sensitivity can come from enamel wear, exposed roots, cavities, or grinding.
Don’t self-diagnose—use a sensitivity toothpaste and schedule an exam if it continues.
Tooth Whitening And DIY Treatments Mistakes
Overusing Whitening Products
Overuse can increase sensitivity and irritate gums.
Follow the recommended schedule and take breaks if you notice discomfort.
Trying Harsh DIY “Hacks”
Abrasive or acidic DIY methods can damage enamel.
If you want whiter teeth, ask your dentist about safer options and realistic results.
Grinding, Clenching, And Jaw Habits
Ignoring Night Grinding
Grinding can flatten teeth, cause cracks, and lead to jaw soreness or headaches.
If you wake with jaw pain or notice tooth wear, ask about a night guard or other treatment.
Chewing Ice Or Hard Objects
Chewing hard items can chip enamel and crack fillings.
Choose softer snacks and avoid using your teeth as tools.
FAQ
Dental problems and solutions
Common problems: cavities, gum disease, sensitivity; solutions: hygiene, fluoride, dentist treatment.
How often should I brush my teeth?
Twice daily for two minutes, and after sugary meals if possible.
Oral and dental problems
Include cavities, gingivitis, periodontitis, bad breath, erosion, ulcers, and tooth loss.
What are the 5 oral health diseases?
Dental caries, gingivitis, periodontitis, oral cancer, and oral candidiasis are five.
Definition of oral hygiene
Oral hygiene is daily practices that keep teeth and gums clean and healthy.
How to Prevent Gum Recession in Smokers
How To Prevent Gum Recession In Smokers
Gum recession in smokers often develops quietly because smoking reduces blood flow and can hide bleeding. Prevention focuses on gentle brushing, daily interdental cleaning, professional cleanings, and early gum checks. Quitting tobacco is the biggest step: it improves healing and lowers ongoing risk, even if already-receded gums do not grow back.
Table of Contents
Why Smoking Raises The Risk Of Gum Recession
Smoking affects the gums in a few connected ways. Nicotine constricts blood vessels, so less oxygen and fewer nutrients reach gum tissue. That slows repair and makes the gums more vulnerable to ongoing irritation.
Tobacco also changes the mouth’s bacterial balance and weakens immune response. As a result, plaque hardens into tartar more easily, infections become harder to control, and gum disease is more likely to progress.
Many smokers also bleed less during brushing because of reduced circulation. That can mask inflammation and delay diagnosis, which is one reason recession may be noticed late.
Common Causes Of Gum Recession In Smokers

- Plaque and tartar buildup along the gumline (often worse with dry mouth).
- Gum disease (gingivitis and periodontitis) that progresses faster and responds less predictably to treatment.
- Aggressive brushing or a hard-bristled toothbrush, which can wear down the gum margin.
- Grinding or clenching, which can increase stress on the supporting tissues.
- Poorly fitting dental work or bite issues that trap plaque or irritate the gums.
Early Signs You Shouldn’t Ignore
Recession is usually gradual. If you smoke, it’s worth checking your gums regularly in good light.
- Tooth sensitivity to cold, hot, or sweet foods.
- Teeth looking “longer” or roots becoming visible.
- Notches near the gumline or a change in the way the gums hug the tooth.
- Food getting stuck more often between teeth.
- Persistent bad breath or a bad taste that returns quickly after brushing.
- Bleeding, swelling, or tenderness—even if it’s mild or occasional.
A Daily Routine That Protects Your Gums
Brush Gently, Twice A Day
Use a soft-bristled toothbrush and small circular motions at the gumline. Aim for two minutes. Hard scrubbing can make recession worse, especially if the gums are already inflamed.
Clean Between Teeth Every Day
Floss, interdental brushes, or a water flosser can remove plaque where brushes miss. Choose the option you can do consistently; technique matters more than the tool.
Use Mouthwash With A Purpose
An antiseptic mouthwash can reduce bacterial load, while fluoride rinses support enamel. If you have dry mouth, look for alcohol-free options and ask your dentist what fits your situation.
Don’t Skip Tongue Cleaning
A tongue scraper or brushing the tongue can reduce odor-causing bacteria and help overall oral hygiene.
Professional Care That Makes The Biggest Difference

Home care is essential, but it can’t remove tartar once it hardens. Regular professional cleanings help keep gum inflammation under control.
If you smoke, many dentists recommend cleanings and gum checks at least every 6 months, and sometimes more often depending on your gum measurements and tartar buildup.
If early gum disease is found, treatment may include deep cleaning (scaling and root planing), targeted antibacterial care, and a review of your brushing technique.
Quitting Smoking: What Improves And What Doesn’t
Stopping tobacco use is the strongest long-term move for gum health. Circulation and immune response improve over time, which supports healing and makes periodontal treatment more effective.
Quitting does not “regrow” gums that have already receded, but it can slow or stop further damage. If recession has created significant sensitivity or exposed roots, your dentist can discuss options such as bonding, grafting, or desensitizing treatments.
Nutrition That Supports Gum Tissue

Diet won’t replace dental treatment, but it can support gum repair and immune function—especially if smoking has left the tissues irritated.
- Vitamin C: supports collagen formation in gum tissue.
- Vitamin D and calcium: support bone and tooth structure.
- Zinc: supports healing and immune function.
- Magnesium and vitamin K: support mineral balance and normal tissue repair.
If you’re considering supplements, discuss them with a clinician—especially if you take blood thinners, have kidney disease, or are pregnant.
When To See A Dentist Soon
Book an appointment sooner rather than later if you notice sensitivity, visible root surfaces, loose teeth, pus, persistent swelling, or bad breath that doesn’t improve with better cleaning. Early treatment is usually simpler and more predictable.
FAQ
Do receding gums grow back?
No; receding gums don’t regrow naturally, but grafting can restore gum tissue.
What is the best toothpaste for receding gums?
Use low-abrasive fluoride toothpaste; stannous fluoride may reduce gingival inflammation and sensitivity.
Do gums heal after quitting smoking?
Yes; blood flow improves, inflammation decreases, but recession won’t reverse.
If gums recede, will teeth fall out?
Not inevitably; risk rises if periodontal disease progresses and bone loss occurs.
How can smokers strengthen their gums?
Quit smoking, brush twice daily, floss, get cleanings, and treat gum disease promptly.
Changes in Dental Structure by Age
Changes In Dental Structure By Age
Teeth change throughout life—from the eruption of baby teeth to enamel wear, gum recession, and a higher risk of tooth loss later on. Knowing what’s typical at each age helps you spot problems early, plan checkups, and adjust daily care. With consistent hygiene, smart nutrition, and timely dental visits, most age-related issues can be prevented or managed.
Dental health isn’t static. As the jaw grows, teeth erupt, and tissues respond to diet, hormones, and daily use, the structure and function of the mouth shifts in predictable ways.
Understanding these changes makes it easier to protect your smile at every stage—whether you’re caring for a teething baby, supporting a teenager with braces, or managing sensitivity and gum health later in life.
Table of Contents
Tooth Development In Infancy (0–3 Years)

What Typically Changes
- Primary (baby) teeth usually begin erupting around 6 months, often starting with the lower front teeth.
- By about age 3, most children have 20 primary teeth, which support chewing, speech, and jaw development.
- Teething may cause drooling and irritability. If a child has a significant fever or seems unwell, it’s best to consult a pediatrician.
Care Tips That Matter
- Clean gums with a soft, damp cloth; once teeth appear, use a small, soft toothbrush.
- Avoid putting babies to bed with bottles containing milk or sugary drinks to reduce early cavities.
- Schedule the first dental visit by age 1, or within six months of the first tooth erupting.
Tooth Transition And Permanent Teeth Formation In Children (4–12 Years)
What Typically Changes
- Around age 6, baby teeth begin to loosen and fall out as permanent teeth erupt.
- The first permanent molars (often called “6‑year molars”) typically appear behind baby teeth and do not replace any tooth.
- Jaw growth continues, which influences spacing, crowding, and bite alignment.
Care Tips That Matter
- Help children brush twice daily and clean between teeth as contact points tighten.
- Watch for early signs of crowding or an uneven bite; many orthodontic concerns are easier to address when caught early.
- Keep checkups regular to detect cavities quickly, especially as new permanent molars come in.
Dental Health During Adolescence (13–18 Years)

What Typically Changes
- Hormonal changes can make gums more reactive, increasing the likelihood of bleeding or inflammation when plaque builds up.
- Most permanent teeth are in place, so orthodontic treatment is often timed for this period.
- Diet choices and busy schedules can raise cavity risk, especially with frequent sugary or acidic snacks and drinks.
Care Tips That Matter
- Focus on thorough brushing along the gumline and around orthodontic appliances if present.
- Encourage consistent routines—morning and night brushing is non‑negotiable during these years.
- Limit frequent sipping of acidic beverages; rinse with water after snacks when brushing isn’t possible.
Changes In Dental Structure In Adulthood (19–40 Years)
What Typically Changes
- Daily chewing and lifestyle factors can gradually wear enamel, especially with acidic diets or reflux.
- Stress-related clenching or grinding may cause flattening of tooth surfaces, chips, or jaw discomfort.
- Wisdom teeth may erupt or create crowding and inflammation in some adults.
Care Tips That Matter
- Book routine cleanings and exams to catch early decay, gum inflammation, and bite issues.
- If you grind your teeth, ask about a night guard to protect enamel and reduce strain on the jaw.
- Use protective gear for contact sports and address sensitivity early rather than avoiding one side when chewing.
Dental Problems And Precautions In Middle Age (41–60 Years)

What Typically Changes
- Gum recession becomes more common, exposing root surfaces that are more vulnerable to decay and sensitivity.
- Long-term plaque buildup can progress to periodontal disease, which is a leading contributor to tooth loss.
- Certain medications and hormonal changes may contribute to dry mouth, increasing cavity risk.
Care Tips That Matter
- Prioritize professional periodontal checks; gum issues are easier to stabilize when treated early.
- Choose low‑abrasive toothpaste and a soft brush if enamel feels thinner or sensitivity increases.
- If teeth are missing, discuss replacement options such as bridges or implants to support chewing and prevent shifting.
Tooth Loss And Denture Use In Older Age (60+ Years)
What Typically Changes
- The risk of root decay rises as gums recede and dry mouth becomes more common.
- Tooth loss can affect nutrition, speech, and confidence, especially when chewing becomes less efficient.
- Dentures, bridges, and implants may be needed to restore function and comfort.
Care Tips That Matter
- Clean dentures daily and remove them as advised to reduce irritation and infection risk.
- Maintain dental visits even with dentures—oral cancer screenings and gum checks still matter.
- Support oral health with balanced nutrition and hydration, especially if dry mouth is an issue.
How Often To See A Dentist
Most people benefit from regular exams and professional cleanings. Your dentist may recommend more frequent visits if you have gum disease, dry mouth, a history of cavities, or ongoing orthodontic treatment.
Book An Appointment
If you’d like tailored advice on cosmetic dentistry, dental crowns, implants, or general dentistry, contact our clinic to schedule an appointment.
FAQ
Does tooth structure change with age?
Yes; enamel wears, teeth darken, and dentin thickens as you age.
Which vitamins help teeth grow?
No vitamins make adult teeth grow; vitamin D and A support developing teeth.
At what age do teeth start to decay?
Decay can start as soon as teeth erupt, even in early childhood.
Do your teeth become more crooked as you age?
Yes; teeth often shift and crowd gradually with age, especially without retainers.
