Oral Lesions in Autoimmune Diseases
Oral Lesions in Autoimmune Diseases
Autoimmune diseases can trigger mouth ulcers, soreness, and persistent dryness when immune activity inflames the oral tissues or damages salivary glands. The most common causes include Behçet’s disease, lupus, Sjögren’s syndrome, and pemphigus vulgaris. Management usually combines treating the underlying condition with local pain control and careful oral care.
Autoimmune diseases are long-term conditions in which the immune system mistakenly targets the body’s own tissues. When the mouth is involved, symptoms can feel disproportionally disruptive—pain can make eating, speaking, and toothbrushing difficult.
Oral lesions are not always caused by autoimmune disease, but recurring or unexplained problems in the mouth can be an early clue. A dentist or physician may use these signs, together with other symptoms, to guide testing and diagnosis.
Table of Contents
What Is An Autoimmune Disease?
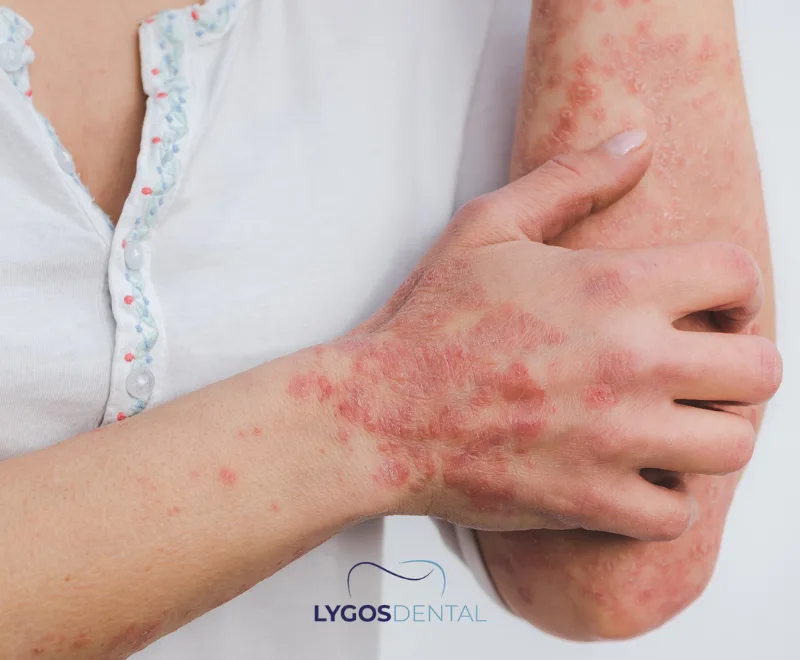
In a healthy immune system, immune cells identify and eliminate harmful threats such as bacteria and viruses. In autoimmune disease, that defense system misidentifies normal cells as “foreign” and creates inflammation that can damage organs and tissues.
Many autoimmune conditions can affect oral health directly (through inflammation of the oral mucosa) or indirectly (through dry mouth, medication effects, or systemic flare-ups).
Common Oral Symptoms
Oral symptoms may involve the oral mucosa, lips, tongue, gums, and salivary glands. People often report one or more of the following:
- Painful, recurring mouth ulcers (aphthae)
- Dry mouth (xerostomia) and thick or foamy saliva
- Gum inflammation, bleeding, or swelling
- Burning or soreness of the tongue
- Changes in taste
- Cracked, dry lips or corners of the mouth
Because these symptoms overlap with common issues such as stress, vitamin deficiencies, infections, and trauma, patterns matter. Ulcers that recur frequently, last longer than expected, or appear with other systemic symptoms deserve a clinical assessment.
Autoimmune Conditions Often Linked To Oral Lesions
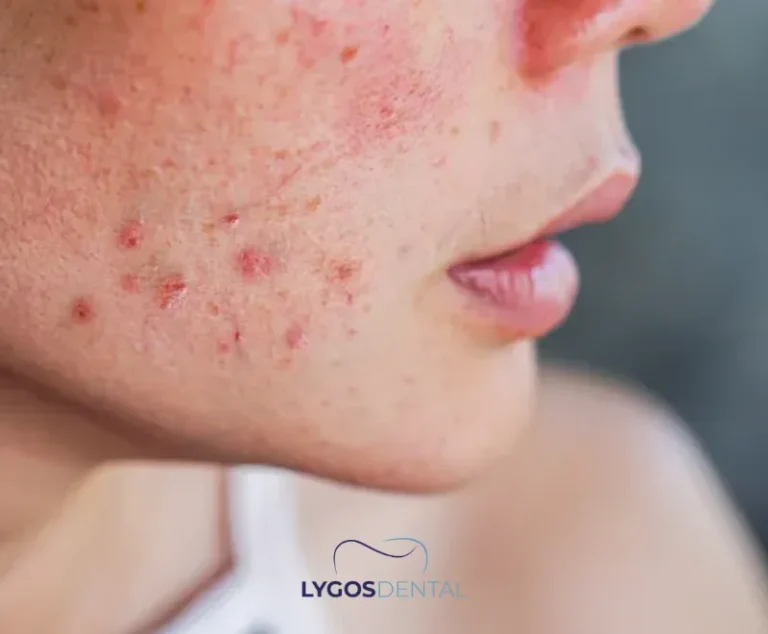
Behçet’s Disease
Behçet’s disease is a multisystem inflammatory condition in which recurrent oral ulcers are a hallmark feature. The ulcers are typically painful, may be multiple at once, and often return in cycles.
Lesions can occur anywhere in the mouth, including the lips, cheeks, tongue, and palate. When oral ulcers are deep and persistent—especially alongside genital ulcers, eye symptoms, or skin lesions—Behçet’s disease becomes an important consideration.
Systemic Lupus Erythematosus (Lupus)
Lupus is a systemic autoimmune disease that can involve skin, joints, kidneys, blood, and the nervous system. Oral ulcers are common and may occur during periods of higher disease activity.
Classic lupus mouth ulcers often appear on the palate and can be red or white. They are sometimes painless, which means they may go unnoticed unless the mouth is examined carefully.
Sjögren’s Syndrome
Sjögren’s syndrome affects the salivary and tear glands, leading to dry mouth and dry eyes. Reduced saliva changes the mouth’s natural protection against acids and microbes.
Dry mouth increases the risk of cavities, gum disease, oral yeast infections, and traumatic irritation from speaking, chewing, or dentures. Some people also notice tongue fissures, burning sensations, and difficulty swallowing dry foods.
Pemphigus Vulgaris
Pemphigus vulgaris is an autoimmune blistering disease. In many patients, the first signs appear inside the mouth as fragile blisters that rupture quickly.
The result is widespread, painful erosions that can make eating and oral hygiene challenging. Prompt diagnosis and specialist treatment are important because symptoms can progress beyond the mouth.
How Lupus, Behçet’s, And Sjögren’s Affect The Mouth

These conditions can look similar at first glance, but their patterns help differentiate them in clinic.
In lupus, ulcers often involve the palate and may be painless. In Behçet’s disease, ulcers tend to be deeper, more painful, and strongly recurrent.
In Sjögren’s syndrome, dryness drives many of the problems—irritation, fissures, higher cavity risk, and recurrent infections—rather than a single “ulcer type”.
Treatment Options
Treatment is tailored to the underlying diagnosis, the severity of symptoms, and how often lesions recur. The main goals are to reduce pain, speed healing, and prevent complications such as infection or tooth decay.
Systemic Treatment (Prescribed By A Specialist)
When oral lesions reflect active autoimmune disease, systemic therapy may be needed to control inflammation. Depending on the condition, clinicians may use corticosteroids, immunosuppressive medicines, or targeted biologic therapies.
Local Treatment And Supportive Care
Local care focuses on comfort and protecting the oral tissues. Options may include topical corticosteroid gels, antiseptic mouth rinses, and short-term anesthetic products.
For Sjögren’s-related dryness, saliva substitutes, moisturizing sprays, and strategies to stimulate saliva can help reduce irritation and lower cavity risk.
Self-Care And Prevention
Simple changes often reduce flare-ups and make lesions less painful. Many patients do better when they avoid spicy or acidic foods during active sores and keep up with gentle, consistent oral hygiene.
If you smoke, stopping can improve healing and reduce irritation. Stress management can also help, as stress is a common trigger for recurrent mouth ulcers in general.
Are Oral Lesions Permanent?
In many autoimmune conditions, oral lesions come and go in flares rather than remaining permanently. Behçet’s disease is well known for recurrent oral ulcers, while lupus mouth ulcers often correlate with disease activity.
In Sjögren’s syndrome, the dryness can be long term, which means the downstream risks—cavities, gum disease, and chronic irritation—may persist without ongoing prevention and dental follow-up.
When To Seek Medical Or Dental Care
Seek evaluation if mouth ulcers recur frequently, last longer than two weeks, or are accompanied by fever, weight loss, rashes, joint pain, eye symptoms, or genital ulcers.
Urgent care is appropriate if you cannot drink enough fluids, pain is severe, or there are signs of infection such as spreading redness, pus, or a high fever.
FAQ
Which autoimmune disease causes mouth lesions?
Behçet’s, lupus, pemphigus, and oral lichen planus can cause mouth lesions.
Which autoimmune disease causes extreme fatigue?
Lupus, rheumatoid arthritis, Sjögren’s, and autoimmune thyroid disease often cause extreme fatigue.
What is the best diet to reverse an autoimmune disease?
No diet reliably reverses autoimmune disease; Mediterranean-style diets can reduce inflammation and symptoms.
How can I get rid of autoimmune mouth sores?
See your clinician; treat the disease, use topical steroids, and avoid triggering foods.
Which autoimmune disease is the most difficult to diagnose?
None is universally hardest; lupus and vasculitis are often difficult due to variability.
Does Tartar Cleaning Damage Tooth Enamel?
Does Tartar Cleaning Damage Tooth Enamel?
Professional tartar cleaning (also called scaling) does not damage tooth enamel when it’s performed by a trained dental professional. The instruments are designed to lift hardened deposits from the tooth surface and along the gumline. Temporary sensitivity can happen after cleaning, but it’s usually caused by exposed dentin or irritated gums—not enamel loss.
Table of Contents
What Tartar Is
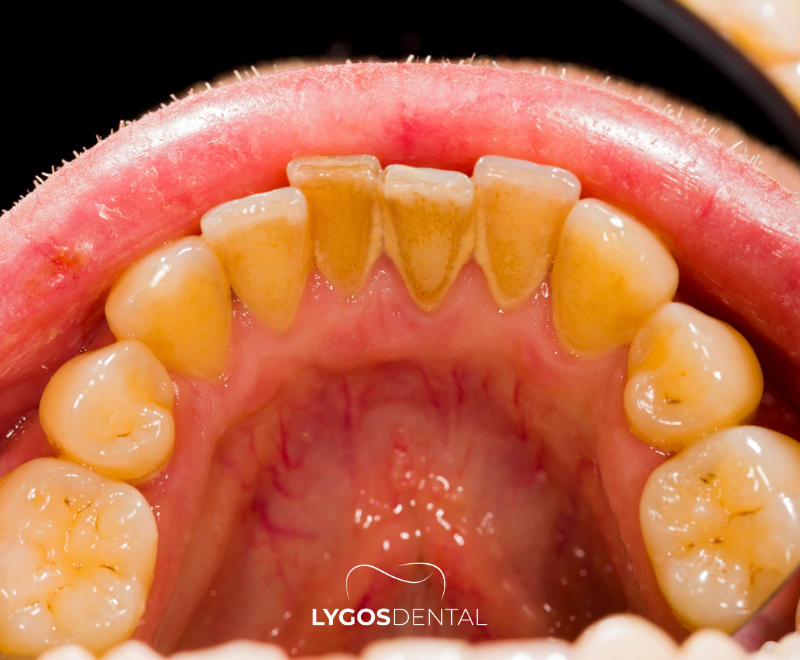
Tartar (calculus) is plaque that has hardened after minerals in saliva bind to it. Unlike soft plaque, tartar cannot be removed fully with brushing alone once it has formed.
It tends to build up near the gumline, between teeth, and behind the lower front teeth—areas that are harder to clean consistently.
Why Dentists Remove Tartar
Tartar traps bacteria against the teeth and gums. Over time, that increases the risk of gum inflammation and can contribute to periodontal (gum) disease.
Removing tartar helps reduce:
- Gum inflammation (gingivitis)
- Bleeding gums and gum recession
- Persistent bad breath
- Progression toward periodontitis and tooth loss
- Visible staining and rough tooth surfaces
Does Tartar Cleaning Harm Enamel?
No—routine tartar removal does not “strip” enamel when it is done properly. Dental professionals use hand scalers and/or ultrasonic scalers to break up and lift calculus from the tooth surface.
These tools are used with controlled pressure and angles, targeting deposits rather than shaving tooth structure. After cleaning, teeth can feel smoother because the hard buildup is gone, not because enamel has been removed.
If you already have enamel wear, exposed roots, or gum recession, you may notice more sensitivity during or after the visit. That sensitivity is related to exposed dentin or root surfaces (roots don’t have enamel), not new enamel damage from the cleaning.
Is Tooth Sensitivity Normal After Tartar Cleaning?

Mild sensitivity is common for a short time after scaling. It typically feels like a quick “zing” with cold air, cold drinks, or brushing.
Why Sensitivity Can Happen
Common reasons include:
- Tartar previously covering sensitive areas near the gumline
- Temporary gum irritation after instruments are used around inflamed tissue
- Existing gum recession exposing dentin or root surfaces
How Long It Lasts And When To Call Your Dentist
Most people feel better within a few days. If discomfort is severe, lasts longer than a week, or is accompanied by swelling, persistent bleeding, or pain when biting, contact your dentist to rule out cavities, cracked teeth, or gum infection.
How Often Should You Get Tartar Cleaning?

There isn’t one perfect schedule for everyone. Many patients do well with a check-up and cleaning about every six months, but the ideal interval depends on your risk factors and oral health history.
Your dentist may recommend more frequent cleanings if you:
- Smoke or use tobacco
- Have a history of gum disease
- Have diabetes or other conditions that affect gum health
- Wear orthodontic appliances or have many restorations that trap plaque
- Build tartar quickly due to saliva composition or genetics
Aftercare Tips To Protect Teeth And Gums
To keep results longer and reduce sensitivity:
- Brush twice daily with a soft-bristled toothbrush and fluoride toothpaste.
- Clean between teeth daily with floss or interdental brushes.
- For 24–48 hours, avoid very cold, very hot, or acidic foods if you feel sensitive.
- If your dentist recommends it, use a desensitizing toothpaste for a week or two.
- Keep regular dental visits so tartar doesn’t have time to harden again.
FAQ
Does tartar removal damage tooth enamel?
No; professional tartar removal doesn’t damage enamel when performed correctly.
Can I restore my tooth enamel?
No; enamel can’t regrow, but fluoride can remineralize early enamel weakening.
Why do dentists recommend deep cleaning?
Because it removes buildup below gums, reduces pockets, and treats periodontal disease.
How can tartar be removed without damaging tooth enamel?
By professional scaling with proper instruments and technique, avoiding DIY scraping.
What happens if tartar is not removed?
Tartar causes gum disease, bad breath, recession, and bone loss, increasing tooth-loss risk.
Dental Health Problems After Menopause
Dental Health Problems After Menopause
After menopause, lower estrogen can reduce saliva, make gums more sensitive, and contribute to bone loss in the jaw. Many women notice dry mouth, gum bleeding, burning sensations, or more cavities. With consistent home care, targeted products for dryness, and routine dental checkups, these changes are often manageable and preventable.
Table of Contents
Why Menopause Affects Oral Health
Estrogen helps maintain healthy oral tissues and supports normal bone turnover. When estrogen levels fall during menopause, the mouth may feel drier and soft tissues can become thinner or more reactive. At the same time, age-related changes and reduced bone density can affect the jaw, which supports the teeth.
Common Dental And Oral Problems

Gum Disease (Gingivitis And Periodontitis)
Hormonal shifts can make gums more prone to inflammation and tenderness. You might notice swelling, bleeding during brushing, bad breath, or gum recession. Untreated periodontitis can damage the bone around teeth and raise the risk of tooth loss.
Dry Mouth (Xerostomia)
A drop in saliva flow is common and can change how the mouth feels day to day. Saliva protects teeth by washing away food debris and buffering acids. When saliva is low, cavities, plaque buildup, and oral infections become more likely.
Burning Mouth Syndrome
Some women develop a persistent burning, tingling, or scalded feeling on the tongue, lips, or palate. Symptoms can fluctuate and may come with altered taste or a dry sensation. Because triggers vary, it’s worth discussing symptoms with a dentist or physician to rule out other causes.
Tooth Decay
Dry mouth and changes in oral bacteria can increase the chance of cavities. Existing fillings may also start to leak over time, which can hide decay around edges. Regular exams and fluoride support are especially helpful during this stage.
Loose Teeth And Tooth Loss
Bone density changes after menopause can affect the jawbone as well as the spine and hips. If periodontal disease is present, bone loss can progress faster and weaken tooth support. Early gum treatment and bone health monitoring help reduce long-term risk.
Dry Mouth And Menopause
Dry mouth can affect speaking, swallowing, sleep quality, and comfort while eating. It may also lead to mouth sores, cracked lips, bad breath, or a higher rate of cavities. If dryness is persistent, it’s important to treat it as a medical and dental issue rather than a minor annoyance.
Practical steps that often help:
- Sip water regularly and keep water nearby at night.
- Chew sugar-free gum or use xylitol lozenges to stimulate saliva (if appropriate for you).
- Limit alcohol and caffeine if they worsen dryness.
- Use saliva substitutes, moisturizing gels, or dry-mouth rinses.
- Ask your dentist about high-fluoride toothpaste or in-office fluoride treatments.
If you also take medications that can reduce saliva, your dentist can suggest a tailored plan. Seek prompt care if you develop frequent cavities, oral thrush, or painful cracking at the corners of the mouth.
Osteoporosis, Jawbone Changes, And Tooth Stability

Postmenopausal osteoporosis can reduce overall bone strength, and the jawbone is not exempt. Lower jawbone density may contribute to loose teeth and can influence planning for implants or dentures. Coordination between your dentist and physician is useful when bone density is changing or treatment is underway.
Supportive habits for bone and oral health:
- Follow your clinician’s guidance on calcium and vitamin D intake.
- Do regular weight-bearing and strength-based exercise if medically appropriate.
- Keep periodontal disease under control with professional cleanings.
- Ask whether a bone density test is right for you, especially if you have risk factors.
Gum Care During And After Menopause
Gums may feel more sensitive, and brushing that once felt fine can suddenly cause bleeding. Bleeding is a sign of inflammation, not something to ignore. A consistent routine usually improves symptoms within a few weeks, but persistent bleeding should be checked.
A gum-friendly daily routine:
- Brush twice daily with a soft-bristled brush and gentle technique.
- Clean between teeth daily with floss or interdental brushes.
- Use an alcohol-free mouthwash if your mouth is dry.
- Replace your toothbrush every 3 months, or sooner if bristles fray.
Professional cleanings and periodontal assessments remain important every six months, or more often if advised. If you smoke or have diabetes, ask your dental team for extra prevention strategies.
How Menopause-Related Medications Can Affect Teeth

Hormone Therapy
Hormone therapy can improve some menopause symptoms, and its oral effects vary from person to person. If you notice new dry mouth or gum sensitivity after starting or changing therapy, note the timing and share it with your clinician. Avoid stopping any prescribed medication without medical advice.
Antidepressants And Anti-Anxiety Medications
Several common medications can reduce saliva flow and worsen dry mouth. If you rely on these medicines, preventive dental care becomes even more important. Your dentist may recommend fluoride support and more frequent checkups.
Osteoporosis Medications (Including Bisphosphonates)
Antiresorptive medicines used for osteoporosis are important for fracture prevention. In rare cases, they are associated with a jaw complication called medication-related osteonecrosis of the jaw, especially after invasive dental procedures. Always tell your dentist if you take these medicines, and ask your prescriber and dentist for guidance before extractions or implant surgery.
When To See A Dentist
Book a dental visit if you notice ongoing gum bleeding, persistent mouth dryness, or a burning sensation that lasts more than two weeks. Tooth pain, loose teeth, swelling, or sores that don’t heal should be assessed promptly. Early treatment is usually simpler and helps prevent bigger problems.
FAQ
Why do dental and gum problems increase after menopause?
Hormonal estrogen decline reduces saliva and bone support, increasing inflammation and dryness.
Does menopause increase the risk of gum disease?
Yes; menopause-related estrogen loss increases periodontal inflammation and bone loss risk.
Is tooth sensitivity normal during menopause?
Yes; dryness and gum recession can make teeth temporarily more sensitive.
How often should dental checkups be performed after menopause?
Every 6 months, or every 3–4 months if gum disease risk is high.
Is Whitening Teeth with Vinegar Harmful?
Is Whitening Teeth With Vinegar Harmful?
Yes, whitening teeth with vinegar can be harmful because vinegar is acidic and can soften and erode enamel. Even if teeth look slightly brighter at first, repeated exposure may increase sensitivity, irritate gums, and make teeth more prone to staining and cavities. Safer whitening methods exist, including dentist-approved products and professional treatments.
Table of Contents
Why People Try Vinegar For Teeth Whitening

Interest in a brighter smile has made “natural” whitening hacks popular, and vinegar is one of the most shared. Most people use apple cider vinegar, but white vinegar is also mentioned in online recipes.
The idea is simple: acid can loosen some surface stains and plaque, so a quick rinse may make teeth look cleaner. Some people apply vinegar with cotton, dilute it in water as a mouth rinse, or mix it with baking soda and brush.
How Vinegar Affects Tooth Enamel
Vinegar has a low pH, which means it is acidic. When teeth are exposed to acids, enamel can temporarily soften. If acid exposure is frequent or prolonged, enamel can wear away over time.
Enamel does not grow back. Once it thins, the underlying dentin becomes more exposed, which can make teeth look more yellow, feel more sensitive, and become easier to damage.
Does Vinegar Actually Whiten Teeth?
Vinegar may reduce some extrinsic (surface) staining, especially from foods and drinks. Any visible change is usually minor and short-lived.
The trade-off matters. A method that “whitens” by weakening enamel can backfire, because thinner enamel can reveal yellow dentin and increase new staining. A safe whitening approach should improve colour without sacrificing tooth structure.
Main Risks Of Whitening Teeth With Vinegar

Enamel erosion: Acid can gradually wear down enamel, leading to permanent changes in tooth strength and appearance.
Tooth sensitivity: As enamel thins, teeth may react more strongly to cold, hot, sweet, or acidic foods and drinks.
Gum irritation: Vinegar can sting and inflame gum tissue, especially if gums are already sensitive or there are small cuts.
Higher cavity risk: Weaker enamel offers less protection against decay. If brushing becomes painful due to sensitivity, plaque can build up faster.
Uneven results: Stain removal can be patchy, and erosion can create a dull or translucent look at the edges of teeth.
Common Mistakes That Make The Damage Worse
Using vinegar daily or for long rinses. Even “diluted” vinegar is still acidic, and repeated exposure increases risk.
Brushing immediately after using vinegar. Acid can soften enamel, and brushing straight away may increase wear. If you’ve had something acidic, rinse with water and wait before brushing.
Combining vinegar with baking soda. The mix can feel “cleaning,” but it can increase abrasion and is not a controlled whitening system.
Copying social media recipes. Whitening is not one-size-fits-all; existing sensitivity, restorations, and gum health change what is safe.
Safer Alternatives To Vinegar For A Whiter Smile

Dentist-Approved At-Home Options
Over-the-counter whitening products can help when used as directed. Look for products designed for teeth (not DIY acids), and follow label instructions closely.
Whitening toothpastes can polish surface stains and may be a good starting point if you want mild improvement without bleaching.
Professional Whitening
If you want a noticeable colour change, professional whitening is the safest route. Dentists can check for cavities, gum inflammation, and enamel wear before whitening, then choose a method that fits your teeth.
In-office whitening and dentist-supervised take-home trays use controlled peroxide-based gels. This approach is more predictable and easier to adjust if sensitivity occurs.
Habits That Help Teeth Look Brighter Naturally
A lot of “yellowing” comes from surface staining. Daily brushing with fluoride toothpaste, flossing, and regular cleanings often make teeth look noticeably fresher.
If tea, coffee, red wine, or smoking is part of your routine, reducing frequency and rinsing with water afterward can help slow staining.
When To Talk To A Dentist First
If you have sensitivity, visible enamel wear, gum recession, or frequent cavities, skip DIY whitening. The same goes for people with crowns, veneers, or bonding on front teeth, because these restorations will not whiten in the same way as natural enamel.
A dentist can identify whether the colour change is surface staining, enamel thinning, or an internal issue. That diagnosis determines the safest way to improve your smile.
FAQ
Can I whiten my teeth with vinegar?
No; vinegar is acidic and can erode enamel, increasing sensitivity and decay risk.
What is the healthiest way to whiten your teeth?
Dentist-supervised peroxide whitening with custom trays is healthiest and least damaging.
Can white vinegar damage your teeth?
Yes; white vinegar can erode enamel, worsen sensitivity, and irritate gums.
What is the best natural teeth whitener?
None truly whitens naturally; best is professional cleaning plus fluoride brushing to prevent stains.
What happens if I brush my teeth with apple cider vinegar?
It can strip enamel, cause burning, increase sensitivity, and raise cavity risk.
When Do Permanent Teeth Erupt in Children?
When Do Permanent Teeth Erupt In Children?
Most children start getting permanent (adult) teeth at about age 6, often with the first molars and the lower front teeth. Eruption continues through the early teen years, with most permanent teeth in place by 12–13. Third molars (wisdom teeth) may appear later, typically between 17–25.
Table of Contents
Typical Timeline For Losing Baby Teeth
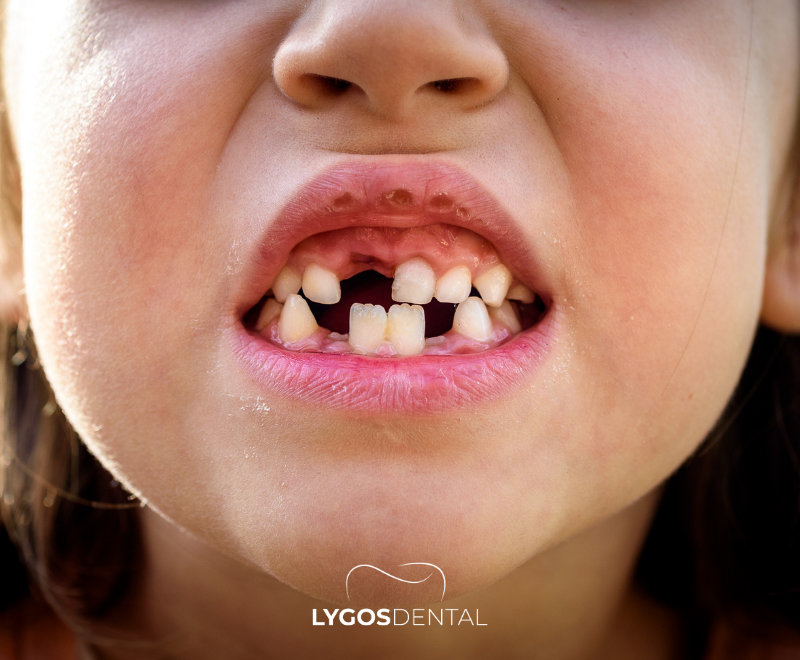
Baby teeth help with chewing, speech, and jaw growth, and they hold space for the adult teeth that follow. Most children start losing baby teeth around age 6, though it can happen a little earlier or later. This period is called the mixed dentition stage because baby teeth and permanent teeth are both present.
When Permanent Teeth Start Coming In
Permanent teeth usually begin erupting between ages 5 and 7, with age 6 as the most common starting point. The first teeth you may notice are the first permanent molars (often called the “6-year molars”) and the lower central incisors. Timing varies by child and can be influenced by genetics, overall growth, and oral health.
Order Of Permanent Tooth Eruption

Children don’t all follow the exact same schedule, but the sequence is fairly consistent. Below are typical age ranges for eruption (upper and lower jaws can differ):
- First permanent molars (6-year molars): 6–7 years
- Lower central incisors: 6–7 years
- Upper central incisors: 7–8 years
- Lateral incisors: 7–9 years
- First premolars (bicuspids): 9–12 years
- Canines (cuspids): 9–12 years
- Second premolars: 10–12 years
- Second molars: 11–13 years
- Third molars (wisdom teeth): 17–25 years (varies widely)
If the order looks different in your child, it doesn’t automatically mean there’s a problem. Dentists focus on patterns such as crowding, teeth that are “stuck,” or large delays between teeth on the right and left sides.
What Are 6-Year Molars And Why Do They Matter?
The 6-year molars are the first permanent molars to erupt, and they do not replace any baby tooth. They come in behind the baby molars, so it’s easy to mistake them for “new baby teeth.” Because they arrive early and have deep grooves, they’re at higher risk for cavities if brushing is inconsistent.
Ask your dentist whether fissure sealants are appropriate once these molars are fully erupted. Sealants can help protect the biting surfaces from decay, especially in children who are prone to cavities.
What If Permanent Teeth Erupt Early Or Late?
A few months’ difference is usually normal. It’s worth booking a dental check if your child is 7–8 and hasn’t started losing any baby teeth, or if a permanent tooth is visible but can’t come through the gum properly.
Common reasons for delayed eruption include:
- Limited space or crowding in the jaw
- Baby tooth roots not resorbing on time
- Extra (supernumerary) teeth blocking eruption
- Teeth developing in an unusual position
- Less commonly, medical or hormonal factors affecting growth
Your dentist may recommend an exam and X-rays to confirm that the adult teeth are present and to check their position. In some cases, removing a retained baby tooth can help the permanent tooth erupt normally.
How To Protect Newly Erupted Permanent Teeth
Newly erupted teeth can be harder for children to clean, especially the back molars. Strong daily habits during the mixed dentition years make a long-term difference.
- Brush twice a day with fluoride toothpaste (a parent should supervise until the child can brush effectively).
- Floss daily once teeth touch, especially around molars.
- Limit frequent sugary snacks and drinks between meals.
- Keep up routine dental visits so eruption, spacing, and bite development can be monitored.
- Consider fluoride varnish and fissure sealants if recommended by your dentist.
FAQ
When do permanent teeth usually start coming in?
Around age 6, first molars and lower incisors usually erupt.
Are there teeth that come in at age 7?
Yes; permanent lateral incisors commonly erupt around age 7–8.
Which vitamins help teeth grow?
No vitamins grow adult teeth; vitamin D and A support tooth development.
Differences Between Implants and Dental Bridges
Differences Between Implants And Dental Bridges
Dental implants replace a missing tooth with a titanium post placed in the jawbone and a crown on top, while a dental bridge fills the gap by anchoring a false tooth to the neighboring teeth. Implants usually last longer and help preserve bone, but they take more time and cost more upfront than bridges.
Table of Contents
What Are Dental Implants And Dental Bridges?
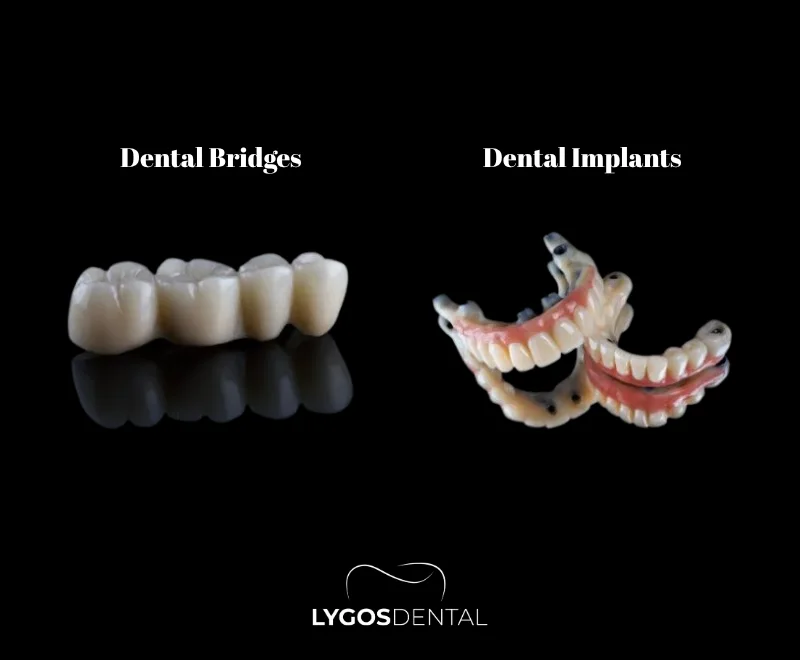
A dental implant is a screw-shaped post made from titanium or another biocompatible material that is placed into the jawbone to act like a tooth root. After healing, a crown (often porcelain or zirconia) is attached to restore the look and function of a natural tooth.
A dental bridge is a fixed prosthesis that replaces one or more missing teeth by using the teeth next to the gap for support. Those neighboring teeth are shaped to hold crowns, and the replacement tooth (pontic) is connected between them.
How Each Treatment Is Done
Implant Treatment Steps
Implant treatment involves a minor surgical procedure to place the implant into the jawbone. The implant then needs time to bond with the bone (osseointegration), which commonly takes several months. Once the site is stable, the dentist fits the final crown onto the implant.
Dental Bridge Treatment Steps
For a dental bridge, the dentist prepares the teeth on either side of the missing tooth and takes impressions or digital scans. A dental lab fabricates the bridge, and the dentist bonds it in place at a follow-up visit. Because there is no implant surgery, treatment is typically completed faster.
Key Differences At A Glance

- Support: Implants are anchored in the jawbone; bridges rely on the neighboring teeth.
- Impact on nearby teeth: Implants usually do not require altering adjacent teeth; bridges typically require shaping them.
- Bone support: Implants can help slow jawbone shrinkage in the missing-tooth area; bridges do not replace the root, so bone changes may continue.
- Longevity: Implants often last longer with good oral hygiene; bridges commonly need replacement over time.
- Treatment time: Implants take longer because healing is required; bridges are usually finished within a shorter period.
Advantages And Disadvantages
Advantages Of Implants
- Help preserve jawbone in the missing-tooth area.
- Do not typically require reducing neighboring teeth.
- Strong, stable chewing function.
- Natural-looking results when properly planned.
Possible Downsides Of Implants
- Require a surgical procedure and healing time.
- Not ideal for everyone (for example, limited bone volume or certain medical risks).
- Higher upfront cost compared with many bridge options.
Advantages Of Dental Bridges
- No implant surgery is needed.
- Faster path to a fixed tooth replacement in many cases.
- Often lower upfront cost.
Possible Downsides Of Dental Bridges
- Neighboring teeth usually need to be shaped, which can affect otherwise healthy tooth structure.
- Do not replace the tooth root, so bone changes may continue under the missing-tooth area.
- May need replacement after years of wear, decay, or gum changes.
Treatment Time And Recovery
With implants, the overall timeline depends on healing and bone integration, so treatment may take several months from start to final crown. Mild swelling or discomfort can occur after placement, and following aftercare instructions helps reduce complications.
With bridges, most patients return to normal routines quickly because there is no surgical site to heal. Some temporary sensitivity can happen after tooth preparation, especially if the prepared teeth were already sensitive.
Costs And Long-Term Value

Implants are usually more expensive upfront because they involve surgical placement, components, and a longer clinical process. Bridges can be more economical at the start, particularly when multiple adjacent teeth are being replaced.
Over the long term, value depends on maintenance, gum health, bite forces, and whether the restoration needs to be replaced. A dentist can explain expected lifespan and maintenance costs for your specific case.
Which Option May Be Right For You?
Implants may be preferred when you want to avoid involving the neighboring teeth and you have enough bone support for predictable placement. Bridges may be considered when you need a quicker fixed option, when implant surgery is not suitable, or when adjacent teeth already need crowns.
The best choice depends on medical history, smoking habits, bone quality, gum health, and your budget. A clinical exam and imaging are essential before deciding.
Care Tips To Protect Your Restoration
Brush twice daily with a soft toothbrush and use interdental cleaning (floss, floss threaders, or interdental brushes) as advised by your dentist. Professional cleanings and routine check-ups help detect early issues such as gum inflammation, bite changes, or decay around bridge margins.
If you grind your teeth, ask about a night guard. Avoid using your teeth as tools and be cautious with very hard foods, especially during the first weeks after treatment.
FAQ
Is a dental implant better than a bridge?
Often yes; implants spare adjacent teeth and bone, but bridges can be suitable.
Which is more expensive, a bridge or an implant?
Usually an implant costs more upfront than a bridge.
Do the teeth under a bridge decay?
Yes; abutment teeth can decay at the margins if hygiene is poor.
What is the 2-2-2 rule in dentistry?
Brush twice daily for two minutes, and visit a dentist twice yearly.
What can I do instead of a bridge?
Consider an implant, removable partial denture, resin-bonded bridge, or orthodontic space closure.
Dental Treatments with CAD/CAM Technology
Dental Treatments With CAD/CAM Technology
CAD/CAM dentistry uses a digital scanner to capture your teeth, then designs and mills restorations such as crowns, veneers, inlays/onlays, and implant crowns with high precision. Many cases can be completed faster than traditional lab workflows, often with a more comfortable impression process and a highly natural look—depending on your bite, materials, and clinical needs.
Dentistry has moved quickly toward digital workflows, and CAD/CAM has become one of the most practical upgrades for both patients and clinics. Instead of taking a putty impression and waiting days for a lab, many restorations can be planned digitally and produced with tighter tolerances.
This guide explains what CAD/CAM technology is, where it is used in modern dentistry, and what to expect in terms of benefits, limitations, and pricing.
Table of Contents
What Is CAD/CAM Technology?
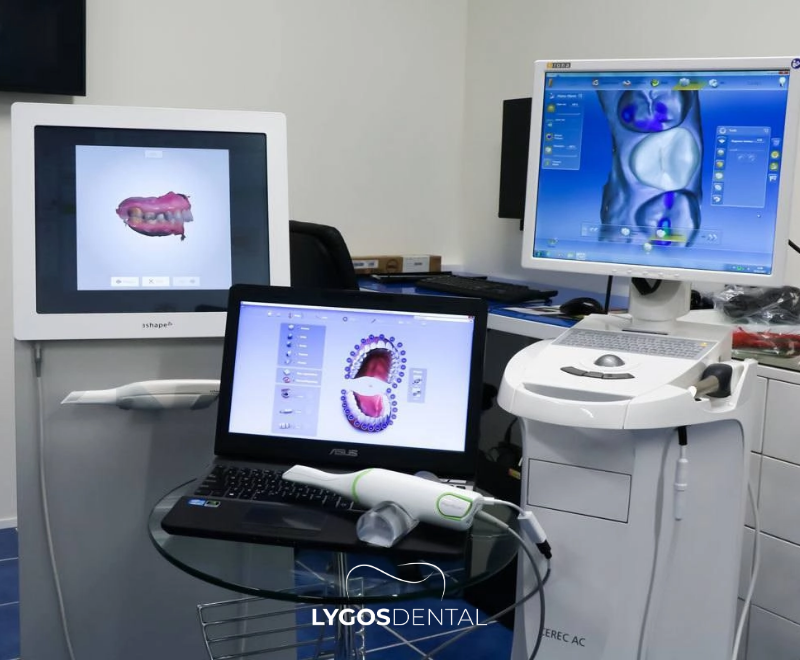
CAD/CAM stands for Computer‑Aided Design (CAD) and Computer‑Aided Manufacturing (CAM). In dentistry, it typically includes three steps:
- Digital scanning of teeth and gums with an intraoral scanner (or a scan of a physical model).
- Designing the restoration on a computer using specialized software.
- Manufacturing the piece by milling or 3D printing, then finishing and bonding or cementing it.
Common CAD/CAM materials include ceramics such as zirconia, lithium disilicate (e.g., E.max), and other high‑strength porcelain options.
Where CAD/CAM Is Used In Dentistry
CAD/CAM can support a wide range of restorative and aesthetic treatments. The most common applications include:
Crowns And Bridges: Single‑tooth crowns and multi‑unit bridges can be designed to match your bite and smile line more precisely.
Veneers (Laminates): Thin ceramic shells for front teeth can be digitally planned for shape, symmetry, and shade.
Inlays And Onlays: Custom restorations for larger cavities or fractured cusps when a standard filling is not ideal.
Implant‑Supported Restorations: Implant crowns, bridges, and full‑arch prostheses can be designed with careful attention to emergence profile and screw/cement access.
Orthodontic Appliances: Clear aligner workflows and some retainers can be planned digitally and produced with high consistency.
Key Advantages For Patients
- Faster turnaround: many cases can be delivered sooner, and some clinics offer same‑day options for selected restorations.
- High precision: digital scanning and manufacturing can reduce distortion and improve the fit of margins and contacts.
- More comfortable impressions: scanners can replace messy impression materials in most cases.
- Natural aesthetics: modern ceramics can closely mimic enamel translucency and color.
- Biocompatible materials: zirconia and other ceramics are widely used and well tolerated for many patients.
Your dentist may still recommend a conventional approach for certain situations, such as complex bite issues, extensive gum treatment needs, or when a lab‑crafted restoration is clinically preferable.
CAD/CAM Vs Traditional Dentistry
Both methods can produce excellent results. The difference is often the workflow and speed rather than the final goal.
| Feature | Traditional Method | CAD/CAM Method |
| Impressions | Putty/paste impressions (can trigger gag reflex) | Digital scan with an intraoral scanner (typically more comfortable) |
| Production Time | Often several days (lab turnaround) | Often faster; sometimes same‑day for selected cases |
| Accuracy | More steps where distortion can occur | Digital workflow can improve consistency and fit |
| Aesthetics | Depends on lab and materials | Digital planning + modern ceramics can improve predictability |
| Appointments | Commonly 2+ visits | Can be fewer visits depending on the case |
Who Is CAD/CAM Suitable For?
CAD/CAM is suitable for many people, but case selection matters. It is commonly recommended for patients who:
- Want a natural-looking, aesthetic restoration for visible teeth.
- Need a precise crown, veneer, inlay/onlay, or implant restoration.
- Prefer a shorter, more streamlined treatment process.
- Have had problems with impressions in the past (gag reflex, discomfort).
A clinical examination, X‑rays, and sometimes a digital bite analysis help your dentist decide whether a CAD/CAM restoration is the best option for your mouth and bite.
CAD/CAM Dental Treatment Prices In 2026

Pricing varies by material, case complexity, number of teeth, and the clinic’s equipment and lab setup. In Turkey, many clinics quote in EUR or USD for international patients, so exchange rates can affect the final cost.
Typical price drivers include:
- Material choice (zirconia, lithium disilicate, multilayer ceramics, etc.).
- Tooth preparation complexity and whether temporary restorations are needed.
- Number of units (single tooth vs multi‑unit bridge).
- Additional treatments (gum shaping, root canal treatment, bite adjustments).
- Clinic location and clinician experience.
Indicative per‑tooth price ranges in Turkey (2026):
| Procedure (Typical Example) | Approximate Range (TRY) |
| Zirconia Crown (per tooth) | ₺6,700 – ₺10,300 |
| Porcelain Veneer (per tooth) | ₺8,700 – ₺15,200 |
| Composite Veneer (per tooth) | ₺7,800 – ₺10,800 |
| E.max / Lithium Disilicate Veneer (per tooth) | ₺13,000 – ₺26,000 |
| Inlay (per tooth) | ₺5,900 – ₺17,800 |
| Onlay (per tooth) | ₺8,900 – ₺23,700 |
| Single Implant Package (implant + abutment + crown) | ₺17,400 – ₺34,700 |
These figures are broad estimates. A written treatment plan after examination is the only reliable way to confirm pricing for your specific case.
FAQ
What is CAD/CAM technology?
Computer-aided design and manufacturing create precise dental restorations from digital scans.
Types of CAD/CAM Systems in Dentistry
Systems include chairside, lab-based, and centralized milling/printing workflows with intraoral scanners.
Advantages and Disadvantages of CAD/CAM in Dentistry
Pros: speed, precision, consistency; cons: high cost, training needs, material and esthetic limits.
Is CAD/CAM technology safe?
Yes; it’s widely used and safe when clinicians follow proper scanning, design, and fabrication protocols.
What treatments can be performed with CAD/CAM?
It can make crowns, bridges, inlays/onlays, veneers, implant abutments, guides, and dentures.
Symptoms of Gum Inflammation (Gingivitis Symptoms)
Symptoms Of Gum Inflammation (Gingivitis Symptoms)
Gum inflammation (gingivitis) is an early stage of gum disease caused mainly by plaque buildup at the gumline. Common signs include red or swollen gums, bleeding when brushing or flossing, persistent bad breath, tenderness, and gum recession. With early dental care and consistent home hygiene, gingivitis is usually reversible.
Oral health plays a major role in overall wellbeing, and gum disease often starts quietly. Gingivitis can look minor at first, but it’s a clear signal that the gumline is under attack from bacteria. Spotting the signs early can help you avoid deeper infections that affect the bone and support around the teeth.
Table of Contents
What Is Gum Inflammation?
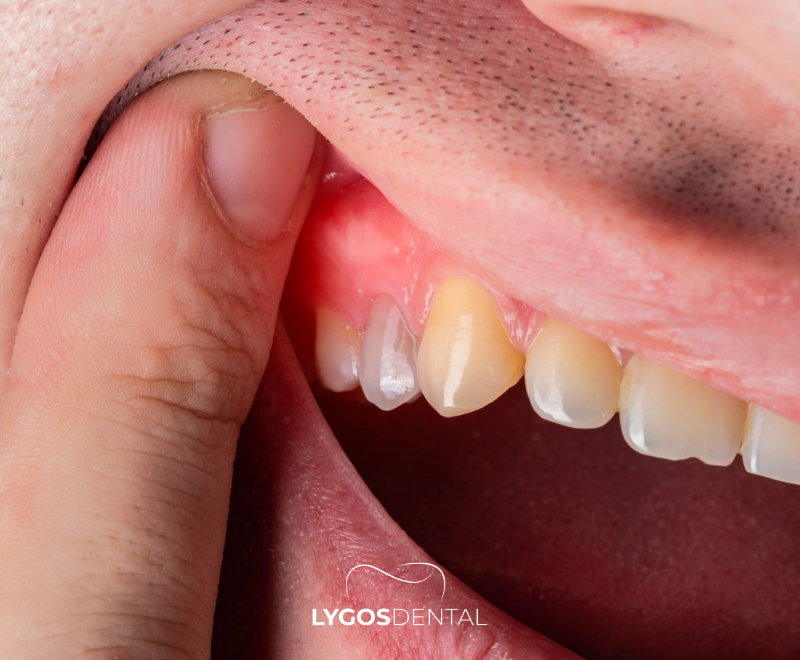
Gum inflammation is the irritation and swelling of the gum tissue. The medical term is gingivitis, and it most often develops when bacterial plaque isn’t removed effectively from the teeth and gumline. Over time, the gums react by becoming red, puffy, and prone to bleeding.
The good news is that gingivitis is typically reversible when addressed early with professional cleaning and improved daily care. When it’s ignored, it can progress to periodontitis, a more serious form of gum disease that may lead to bone loss and loose teeth.
Common Causes And Risk Factors
Plaque buildup is the main trigger, but several factors can raise the risk or make symptoms worse. Some are lifestyle-related, while others are linked to hormonal changes or health conditions. If you’re seeing symptoms repeatedly, it’s worth looking at both your routine and your medical background.
- Inconsistent brushing and flossing, or difficulty cleaning around crowns, bridges, braces, or implants
- Smoking or tobacco use
- Hormonal shifts (for example, pregnancy)
- Dry mouth, which reduces saliva’s natural cleansing effect
- Diabetes and other conditions that can affect immune response
- Certain medications that reduce saliva or irritate gum tissue
Most Common Gingivitis Symptoms
Gingivitis can vary from person to person, but the core signs are fairly consistent. Many people notice bleeding first, especially when brushing or flossing. If you have several of the symptoms below, a dental exam is the safest way to confirm what’s going on.
- Red, swollen, or shiny-looking gums (healthy gums are typically firm and pink)
- Bleeding when brushing, flossing, or biting into firm foods
- Bad breath that doesn’t improve with brushing and tongue cleaning
- Tenderness at the gumline or discomfort when chewing
- Gum recession (teeth may look longer)
- Increased sensitivity to hot, cold, or sweet foods
- A bad taste in the mouth
Does Gum Inflammation Cause Bad Breath?

Yes. When plaque and bacteria accumulate around the gumline, they release compounds that can cause persistent bad breath. If the odor returns quickly after brushing, or if it comes with bleeding or swollen gums, it’s often a sign that the problem is coming from the gums rather than the tongue alone.
Professional cleaning and treating the underlying gum inflammation usually makes a noticeable difference. If bad breath persists after treatment, your dentist may also check for cavities, dry mouth, tonsil stones, or other causes.
Does Gingivitis Cause Pain?
Gingivitis doesn’t always hurt, especially in the early stages. That’s one reason it can be easy to miss. Some people feel mild soreness or a “raw” sensation at the gumline, while others notice sensitivity when eating or drinking.
If you’re experiencing significant pain, throbbing, swelling that spreads, or a pimple-like bump on the gum, it may point to a deeper infection and should be assessed promptly.
What Can Happen If Gingivitis Is Left Untreated?
Untreated gingivitis can move beyond the surface gums and affect the supporting tissues around the teeth. At that point, home care alone usually isn’t enough. Early treatment is simpler, less invasive, and typically more affordable than advanced gum therapy.
- Periodontitis (infection that can damage the bone supporting the teeth)
- Gum recession and pockets around teeth that trap bacteria
- Loose teeth and, in advanced cases, tooth loss
- Gum abscesses or pus drainage
When Should You See A Dentist?
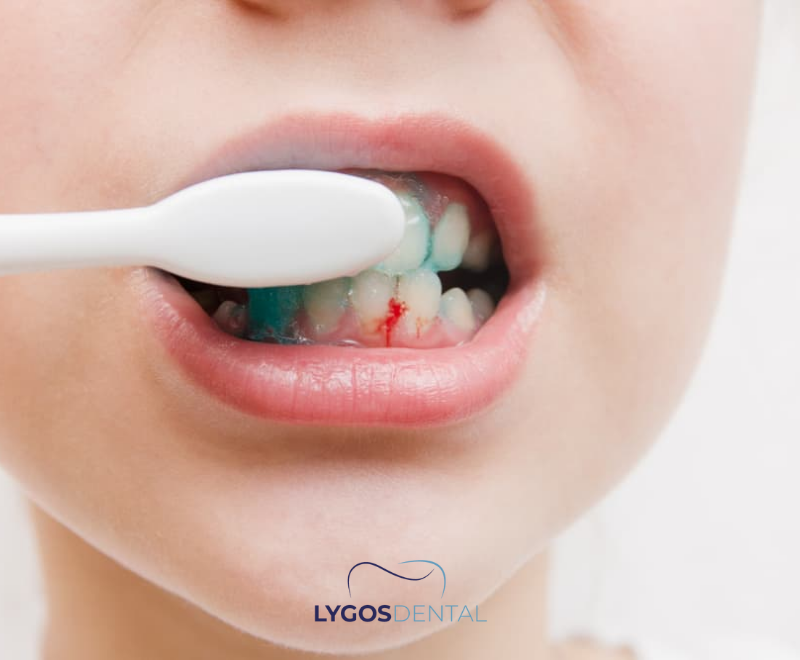
Book a dental checkup if you notice any of the following signs, especially if they last more than a week or keep coming back. A dentist can confirm whether it’s gingivitis, check for periodontitis, and recommend the right cleaning and home-care plan.
- Bleeding gums during brushing or flossing
- Redness, swelling, or tenderness at the gumline
- Bad breath or a bad taste that doesn’t go away
- Gum recession or teeth that look longer
- Sensitivity, discomfort when chewing, or teeth that feel loose
How To Reduce Gum Inflammation At Home
Home care can make a real difference, but it works best when combined with professional cleaning if plaque has hardened into tartar. Aim for gentle, consistent hygiene rather than aggressive brushing, which can irritate gums further.
- Brush twice daily for two minutes with a soft-bristled toothbrush
- Clean between teeth daily with floss or interdental brushes
- Pay special attention to the gumline and the back molars
- Replace your toothbrush head regularly, especially if bristles flare
- If you smoke, consider quitting support—tobacco is strongly linked to gum disease
Need Professional Support?
If you suspect gum inflammation or want a preventive checkup, contact our clinic to schedule an appointment. We can also advise on cosmetic dentistry, dental crowns, dental implants, and general dentistry services based on your needs.
FAQ
What is gum disease?
Gum disease is infection and inflammation of gums and supporting bone around teeth.
What is the most common symptom of gum disease?
Bleeding gums when brushing or flossing is the most common symptom.
How is gum disease treated?
Professional cleaning, improved home care, and sometimes antibiotics or gum surgery.
What happens if it is not treated?
It can cause recession, bone loss, loose teeth, abscesses, and tooth loss.
How long does it take for gum disease to heal?
Gingivitis can improve in 1–2 weeks; periodontitis needs ongoing care.
How Does a Vegan Diet Affect Dental Health?
How Does A Vegan Diet Affect Dental Health?
A well-planned vegan diet can support good dental health, but it may increase enamel wear or gum issues if it’s high in acids and sugars or low in calcium, vitamin D, and B12. With fortified foods, supplements when needed, and consistent oral hygiene, most vegans can maintain healthy teeth and gums.
Vegan eating patterns can be very tooth-friendly when they focus on whole foods, adequate minerals, and good oral routines. Problems usually come from frequent acidic drinks, sticky sugars, and nutrient gaps that affect enamel and gum tissues. The sections below cover the most common risks and the practical steps that help vegans keep their smile healthy.
Table of Contents
Does A Vegan Diet Harm Dental Health?
A vegan diet is not automatically harmful to teeth or gums. Oral health is shaped more by overall diet quality, snacking frequency, fluoride exposure, and daily hygiene than by the absence of animal foods alone.
That said, a poorly planned vegan diet can increase risk in a few predictable ways. Low calcium or vitamin D can affect the strength of teeth and supporting bone, while low vitamin B12 may be linked with mouth ulcers and gum issues. Highly processed vegan snacks and frequent fruit juices can also raise the mouth’s acid and sugar load.
How A Plant-Based Diet Influences Teeth

Acid Exposure And Enamel Erosion
Many plant-based staples are acidic or become acidic in the mouth, especially when eaten often. Citrus fruits, vinegar-based foods, wine, kombucha, and fruit juices can soften enamel over time. Starchy foods that linger on the teeth may also feed acid-producing bacteria, increasing cavity risk.
Saliva-Friendly Whole Foods
Whole, fibrous foods can work in your favor. Crunchy vegetables, nuts, and seeds stimulate saliva, which helps neutralize acids and wash away food particles. Water-rich foods and steady hydration support saliva flow, an important defense against both decay and bad breath.
Key Nutrients Vegans Should Watch For Oral Health
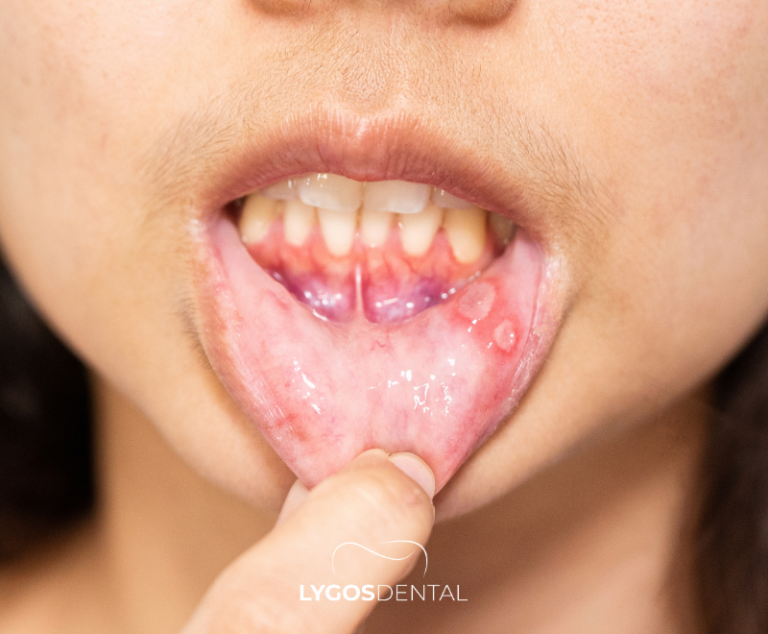
Calcium And Vitamin D
Calcium helps maintain strong teeth and jawbone, while vitamin D supports calcium absorption. Without dairy, vegans usually rely on a mix of naturally calcium-rich foods and fortified products.
Practical vegan sources include:
- Calcium-set tofu, fortified plant milks and yogurts
- Tahini (sesame), chia seeds, almonds
- Kale, broccoli, bok choy, and other leafy greens
- Vitamin D from sensible sun exposure, fortified foods, or supplements when needed
Vitamin B12 And Gum Health
Vitamin B12 is essential for healthy blood cells and nerve function, and it supports immune response in the mouth. Because B12 is limited in unfortified plant foods, deficiency is more common in strict vegans who do not use fortified foods or supplements.
Low B12 has been associated with oral symptoms such as:
- Mouth ulcers or sore spots
- A burning or tingling sensation on the tongue
- Gum tenderness or easier bleeding
A reliable B12 supplement or regular intake of B12-fortified foods is the most consistent way to prevent deficiency.
Omega-3s And Inflammation
Omega-3 fats play a role in inflammation control, which matters for gum health. Plant foods mainly provide ALA from flax, chia, walnuts, and hemp, while DHA and EPA are available from algae-based supplements.
Iron And Zinc
Iron and zinc support immune function and tissue repair. If either is consistently low, some people notice more frequent mouth sores or slower healing after dental work.
Plant-based sources to prioritize:
- Lentils, beans, chickpeas, and pumpkin seeds
- Whole grains and oats
- Cashews and tahini
- Vitamin C–rich foods with meals to improve iron absorption
Daily Habits That Protect Vegan Smiles

- Limit frequent sipping on fruit juice, soda, kombucha, and other acidic drinks.
- After acidic foods or drinks, rinse with water and wait about 30 minutes before brushing.
- Brush twice daily with a fluoride toothpaste and clean between teeth every day (floss or interdental brushes).
- Choose snacks that are less sticky and less sugary; pair fruit with nuts or meals rather than grazing all day.
- Chew sugar-free gum after meals if you’re prone to dry mouth (it can boost saliva).
- Schedule routine dental check-ups and professional cleanings (often every six months, or as advised).
Are Vegan Toothpastes Effective?
Vegan toothpaste can be just as effective as conventional options when it contains proven anti-cavity ingredients. Many vegan formulas include fluoride, which strengthens enamel and reduces decay risk. Some are fluoride-free, so check the label and follow your dentist’s guidance if you’re choosing an alternative active ingredient.
When To See A Dentist
Book a dental visit sooner than your next routine check-up if you notice persistent bleeding gums, new sensitivity, mouth ulcers that do not heal, a burning tongue sensation, or ongoing dry mouth. These symptoms can have several causes, including nutrient deficiencies, irritation, or gum disease, and are worth evaluating early.
Book An Appointment
Contact us to learn more about cosmetic dentistry, dental crowns, dental implants, and general dentistry. We can help you choose an oral care plan that fits your diet and your goals.
FAQ
Vegan nutrition and dental health
Vegan diets can support dental health with adequate calcium, vitamin D, B12, and hygiene.
Does vegetarian nutrition cause tooth decay?
No; decay is caused by sugars, acids, and plaque, not vegetarianism.
Dental problems in vegetarians
Vegetarians may have erosion or cavities if diets are acidic or sugary.
Are vegetarians’ teeth healthier?
Not automatically; oral health depends on hygiene, fluoride, and sugar frequency.
Why Does Tartar Form?
Why Does Tartar Form?
Tartar (also called dental calculus) forms when plaque is left on teeth long enough to harden. Minerals in saliva “set” the sticky film into a rough deposit—often near the gumline and between teeth. Good brushing, daily flossing, and regular professional cleanings stop plaque before it turns into tartar and irritates gums.
Table of Contents
What Tartar Is
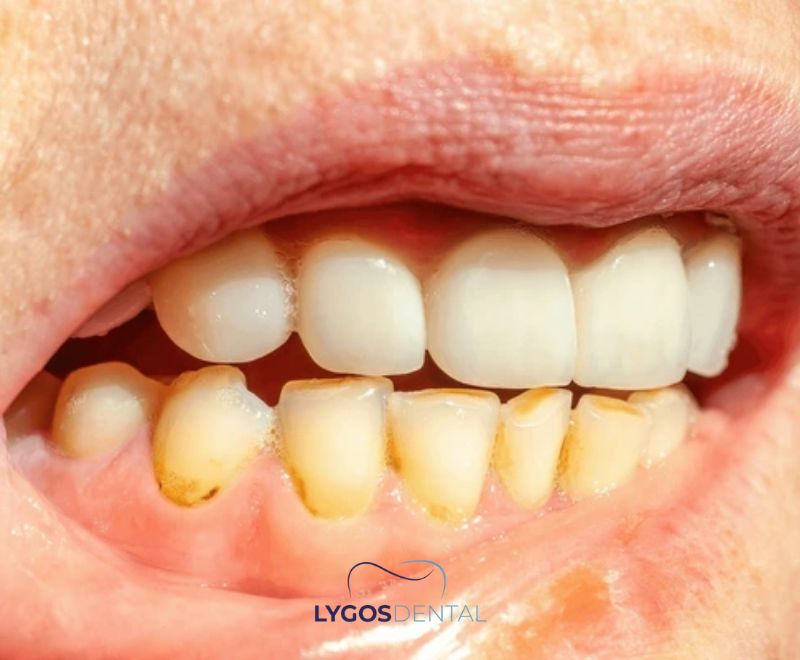
Plaque is a soft, sticky layer of bacteria and food particles that forms on teeth every day. When plaque isn’t removed thoroughly, it can mineralise and become tartar. Unlike plaque, tartar bonds to the tooth surface and creates a rough area where new plaque sticks more easily.
Tartar tends to build up most around the gumline, behind the lower front teeth, and on the outer surfaces of upper back teeth. Over time it can contribute to gum inflammation, persistent bad breath, and a higher risk of cavities.
Why Tartar Forms
Plaque Left On Teeth
The most common reason is missed plaque during daily cleaning. If brushing is rushed or irregular, plaque remains along the gumline and between teeth. As it hardens, it becomes tartar that can’t be removed with a toothbrush.
Saliva Minerals And Dry Mouth
Saliva naturally contains minerals such as calcium and phosphate. People with higher mineral content in their saliva may develop tartar more quickly. Dry mouth (from dehydration, some medications, or mouth breathing) reduces saliva’s cleansing effect and can speed up buildup.
Smoking And Tobacco Use
Smoking and other tobacco use can increase plaque and stain deposits. It also irritates gum tissue and can mask early gum disease by reducing visible bleeding. That combination often leads to heavier tartar accumulation over time.
Diet High In Sugar And Starch
Sugary and starchy foods feed plaque-forming bacteria, especially when snacking is frequent. Sticky foods and sweet drinks can linger on tooth surfaces and between teeth. The longer plaque sits, the more likely it is to harden into tartar.
Skipping Interdental Cleaning
A toothbrush can’t fully reach the tight spaces between teeth. When floss or interdental brushes aren’t used, plaque builds up in these areas and near the gumline. This is why many people notice tartar first between teeth and behind the lower front teeth.
Signs You May Have Tartar
Tartar can look different depending on where it sits and how long it has been there. Common signs include:
- Yellow, tan, or brown deposits on teeth (often near the gums)
- A rough feeling on the tooth surface that doesn’t brush away
- Bad breath that keeps coming back
- Bleeding or tender gums when brushing or flossing
- Red, swollen gums or gum recession
- Increased tooth sensitivity or more frequent cavities
Habits That Speed Up Tartar Buildup

Small routine choices can make a big difference. These habits commonly increase plaque retention and tartar formation:
- Brushing less than twice a day, or brushing for too short a time
- Skipping floss or interdental brushes
- Not cleaning the gumline gently but thoroughly
- Frequent late-night snacking without brushing afterwards
- Regular smoking or vaping with nicotine products
- High intake of sugary drinks, sweet snacks, or refined carbohydrates
How Dentists Remove Tartar
Once plaque becomes tartar, home care can’t lift it off. A dentist or dental hygienist removes it using professional instruments, often with ultrasonic scaling. Teeth are then polished to smooth the surface and make plaque less likely to stick.
If tartar extends below the gumline or there are signs of gum disease, you may need a deeper cleaning (sometimes called periodontal scaling and root planing). Your dentist will recommend the right approach based on your gum health.
Many people do well with a professional cleaning every 6–12 months. If you build tartar quickly or have gum disease risk factors, your dentist may advise more frequent visits.
How To Prevent Tartar From Coming Back
Prevention comes down to stopping plaque before it hardens. A simple routine works best when it’s consistent:
- Brush twice daily for two minutes with a fluoride toothpaste, paying special attention to the gumline.
- Floss once a day or use interdental brushes if you have wider spaces, bridges, or braces.
- Consider an electric toothbrush if you struggle with technique or plaque control.
- Rinse with water after meals and stay well hydrated to support healthy saliva flow.
- Limit frequent sugary snacks and drinks; keep sweet foods to mealtimes when possible.
- Schedule regular dental check-ups and cleanings so tartar is removed early.
When To See A Dentist
Book an appointment if you notice bleeding gums, persistent bad breath, gum swelling, tooth looseness, or pain when chewing. These can be signs of gingivitis or more advanced gum disease, which needs professional care. Early treatment is usually simpler and helps protect the bone supporting your teeth.
FAQ
How can you prevent tartar buildup?
Brush with fluoride twice daily, clean between teeth daily, and get regular professional cleanings.
What is the main cause of tartar?
Tartar forms when plaque isn’t removed and mineralizes from saliva.
Is it okay to scrape tartar off your teeth?
No; DIY scraping can damage enamel and gums and worsen infection risk.
What happens if tartar is not cleaned?
It can cause gum disease, bad breath, recession, bone loss, and tooth loss.
Will teeth fall out if tartar is cleaned?
No; cleaning doesn’t loosen healthy teeth, but it can reveal existing periodontal looseness.
