Dental Bridge vs Partial Denture: Differences and How to Choose
Bridges and Partial Dentures: What They Are and How to Decide Which One Fits You
A dental bridge is fixed in place and replaces one or more missing teeth by attaching to nearby teeth or implants. A partial denture is removable and can replace several missing teeth across the mouth. The right choice depends on the health of your remaining teeth, how many teeth are missing, your bite, and long‑term plans.
Losing a tooth is rarely just about looks. Missing teeth can change how you chew, affect speech, and shift the forces your jaw and remaining teeth have to handle.
Two common ways to restore a gap are dental bridges and partial dentures. Both can work well, but they solve the problem in different ways. A quick exam and a clear plan are what turn “Which is better?” into “Which is right for me?”
Dental Bridges Explained in Simple Terms
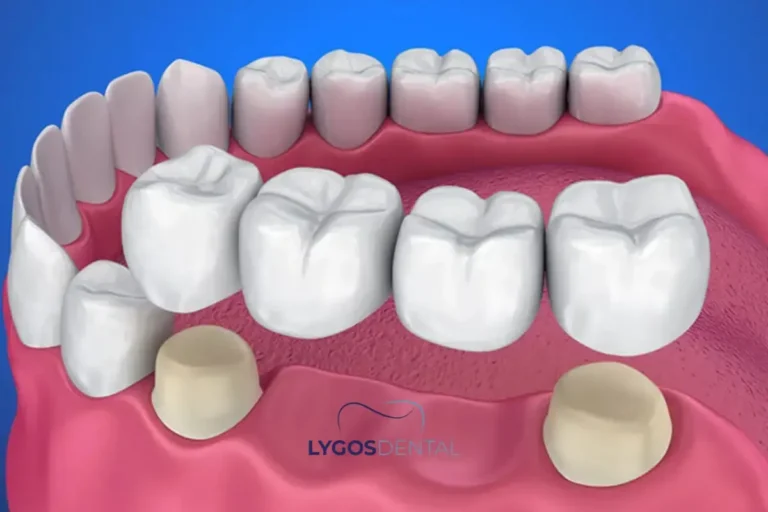
Table of Contents
A dental bridge is a fixed restoration. It replaces a missing tooth (or teeth) by holding an artificial tooth between two supports. In many cases, those supports are the natural teeth next to the gap, prepared to hold crowns.
Because a bridge doesn’t move, it often feels close to having a natural tooth again. You don’t remove it at night, and most daily care looks like normal brushing and flossing. Cleaning under the false tooth takes extra attention, usually with floss threaders or small interdental brushes.
Common Types Of Bridges
Your dentist may recommend a traditional bridge (supported by crowns on both sides), a resin‑bonded bridge for certain front‑tooth cases, or an implant‑supported bridge when implants are the safest long‑term anchor. The best type depends on the gap location, bite forces, and the condition of nearby teeth.
What Partial Dentures Are Like in Everyday Life
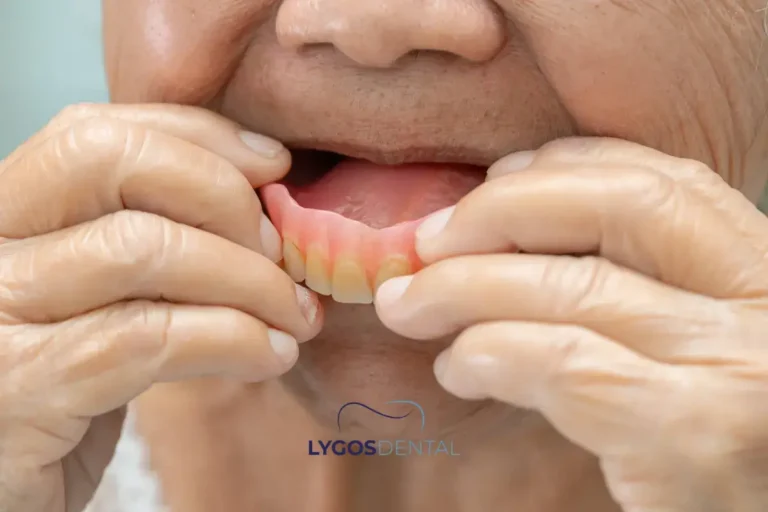
Partial dentures are removable. They can replace several missing teeth, even when the gaps are in different areas of the mouth. A partial denture usually has artificial teeth set into a gum‑colored base, sometimes reinforced with a thin metal framework or flexible material.
You take a partial denture out for cleaning and usually remove it before sleep. Dentists often consider it when many teeth are missing, when the remaining teeth are not ideal bridge supports, or when future tooth loss is possible and flexibility matters.
There can be a short adjustment period for speech and chewing. Most people adapt within days to a few weeks once the fit is properly adjusted.
Bridge Vs Partial Denture: Key Differences
Here’s what typically separates the two options in real life:
- Fixed vs removable: Bridges stay in place; partial dentures are taken out for cleaning.
- Tooth preparation: Bridges often require shaping the teeth next to the gap; partial dentures usually do not require the same level of preparation.
- Cleaning routine: Bridges need careful cleaning under the bridge; partial dentures need daily removal and cleaning.
- Flexibility: A partial denture can often be modified if another tooth is lost later; a bridge usually cannot.
- Cost range: Bridges often cost more because they involve crowns and lab work, though pricing depends on materials and case complexity.
How Dentists Choose Between the Two
There isn’t a single rule that fits everyone. Dentists weigh several clinical factors before recommending a bridge or a partial denture.
What Your Dentist Checks
- Health and strength of the teeth next to the gap
- Gum health and bone support
- Number of missing teeth and their positions
- Bite forces and grinding or clenching habits
- Risk of future tooth loss and whether the plan needs flexibility
In some mouths, a bridge is a neat, long‑lasting solution. In others, using a bridge would mean reshaping healthy teeth or overloading weak ones, which can raise the risk of problems down the road. In those cases, a partial denture can be the safer choice.
Comfort, Looks, and Daily Habits
Comfort is often the first concern. Bridges tend to feel more natural because they’re fixed. Partial dentures can feel bulkier at first, yet a well‑fitted design should sit securely and stop rubbing or clicking.
From an appearance standpoint, both options can look very natural when planned well. Material choices, tooth shade matching, and how the gum line is shaped all play a role.
Daily habits matter, too. If you want a “set it and forget it” routine, a bridge may suit you. If you prefer an option that can be adjusted over time, a partial denture may be more practical.

Thinking Long Term
Long‑term oral health matters more than many people expect. Bridges rely on the teeth next to the gap. If one supporting tooth develops decay, gum disease, or a fracture, the entire bridge can be affected.
Partial dentures are more adaptable. If another tooth is lost later, the denture can often be adjusted rather than replaced from scratch. That flexibility can be valuable for people with ongoing gum issues or a higher risk of future tooth loss.
When Another Option May Make Sense
Some patients are also candidates for dental implants, either as a single replacement tooth or as support for a bridge. Implants can help avoid reshaping nearby teeth, but they require adequate bone and a healing period. A dentist can explain whether implants are realistic in your case and how they compare on cost, time, and maintenance.
Why Professional Guidance Makes a Difference
Choosing between a bridge and a partial denture isn’t only about price or convenience. It’s about how your mouth will function over the next few years, not just next week.
At Lygos Dental, a full exam and straightforward discussion help patients understand the trade‑offs clearly. The aim is a plan that protects the remaining teeth, keeps the bite stable, and fits your daily routine.
Get Information Now!
Contact our team to learn more about cosmetic dentistry, dental crowns, dental implants, and general dentistry, and to book an evaluation for the best tooth‑replacement option for you.
Frequently Asked Questions (FAQs)
Should I get a bridge or a partial denture?
Get a bridge if adjacent teeth are strong; get a partial for multiple gaps.
What are the reasons a dentist would recommend a partial rather than two separate bridges?
Partial is recommended when long spans, weak abutments, cost, or future loss make bridges risky.
Is it better to have a bridge or denture?
Bridge is better for stability and chewing; partial is better for cost and flexibility.
Why would a dentist not recommend a bridge?
Dentists avoid bridges when abutment teeth are unhealthy, insufficient, or spans are too long.
What is the downside of having a dental bridge?
Main downside is shaving adjacent teeth, increasing decay risk and making cleaning harder.
What can I get instead of a bridge?
Instead of a bridge, options include implants, a partial denture, resin-bonded bridge, or orthodontics.
Night Toothache Relief: Easy Drug-Free Solutions That Actually Help
Night Toothache Relief: Easy Drug-Free Solutions That Actually Help
If your tooth hurts more at night, you can often take the edge off with a warm saltwater rinse, a cold compress on the cheek, and sleeping with your head slightly raised. These steps won’t fix the cause, but they can make it easier to rest until a dentist can examine the tooth and treat the problem.
Tooth pain at bedtime can feel brutal. During the day you’re distracted, but once you lie down the ache can suddenly feel louder and more persistent.
If you’re trying to get through the night without reaching for medication right away, there are a few practical, drug-free steps that may help you settle the area and sleep more comfortably until you can get proper dental care.
Why Tooth Pain Feels Worse at Night

Table of Contents
Lying flat can increase blood flow and pressure around the head and jaw. When a tooth nerve is already irritated, that extra pressure can make the pain feel more intense or “throbbing.”
Nighttime is also quiet, so your brain has fewer distractions and focuses more on discomfort. Many people also produce less saliva while sleeping, which can leave the mouth drier and make sensitive teeth feel worse.
Common Causes of Night Tooth Pain
Night toothaches usually have a clear trigger, even if it isn’t obvious at first. Common causes include deep decay, a cracked tooth, a loose filling, gum inflammation, or an infection developing inside the tooth.
Hot or cold sensitivity that turns into constant pain can suggest the nerve is involved. Sharp pain when biting may point to a crack, while a deep, pulsing ache (especially with pressure) can be a sign of significant inflammation or infection.
Drug-Free Ways to Relieve Tooth Pain at Night

These options won’t cure the underlying issue, but they can reduce irritation and take the edge off long enough to rest.
Rinse With Warm Salt Water
Warm salt water can soothe irritated gums and help clear bacteria around the sore area. Mix about ½ teaspoon of salt into 1 cup (8 oz) of warm water, swish gently for 20–30 seconds, then spit it out.
Skip aggressive swishing if the tooth is very sensitive. You can repeat the rinse a few times during the evening, but don’t swallow the salt water.
Use A Cold Compress (Outside Only)
If the cheek feels swollen or tender, apply a cold compress to the outside of your face. Hold it for 10–20 minutes, take a break, then repeat as needed.
Wrap ice or a cold pack in a thin cloth to protect your skin. Avoid putting ice directly on the tooth, especially if the nerve is exposed.
Sleep With Your Head Slightly Elevated
If the tooth throbs when you lie flat, try an extra pillow or a more upright position. Reducing head-down pressure can make pulsing pain feel less intense for some people.
If you tend to sleep on the painful side, switching sides may also help reduce pressure on the area.
Avoid Triggers Before Bed
Sugary snacks, very hot drinks, and icy beverages can spike sensitivity right before sleep. Hard or crunchy foods can also aggravate a cracked tooth or inflamed gumline.
If you need to eat, keep it soft and chew on the other side. It also helps to avoid alcohol-based mouthwash, which can sting irritated tissues.
Clean The Area Gently
Sometimes pain flares because food or plaque is trapped between teeth or along the gumline. Brush gently, floss carefully, and then rinse to calm the area.
If flossing causes sharp pain or significant bleeding, stop forcing it. You don’t want to further irritate already inflamed gum tissue.
When Home Solutions Aren’t Enough
If you’re repeating the same night-toothache routine multiple nights in a row, it’s rarely “just one of those things.” Cavities don’t heal on their own, and infections won’t clear without treatment.
Delaying care because of time, fear, or cost is common, but waiting can make treatment more complex. Think of night pain as an early warning sign worth checking quickly.
When to See a Dentist Immediately
Some symptoms should not be managed at home. Seek urgent dental care (or emergency medical care if needed) if you notice any of the following:
- Swelling in the face, jaw, or gums
- Fever or feeling generally unwell
- A bad taste, pus, or a persistent bad smell
- Pain that spreads to the jaw, ear, or neck
- Difficulty opening your mouth, swallowing, or breathing
These can be signs of an infection that may spread. If symptoms are severe or you’re having trouble breathing or swallowing, treat it as urgent.
Book An Appointment
At Lygos Dental, we treat night tooth pain as a signal, not a nuisance. If you’re losing sleep or the pain keeps returning, booking an exam is the fastest way to get relief and prevent complications.
You can contact us to learn more about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry, and to make an appointment.
Frequently Asked Questions (FAQs)
How to stop a toothache fast at night?
Rinse warm salt water, take labeled ibuprofen/acetaminophen, cold compress; see dentist urgently.
What is the 3 3 3 rule for toothaches?
It means 600mg ibuprofen three times daily for three days, with clinician approval.
What kills nerve pain in a tooth?
Dentist-delivered local anesthetic and cause treatment (root canal/extraction) stop tooth nerve pain.
What to do when your tooth hurts so bad you can’t sleep?
Take labeled ibuprofen/acetaminophen, cold compress, elevate head; contact an emergency dentist.
What helps a toothache in 5 minutes?
Cold compress and warm saltwater rinse can ease pain within minutes; take labeled analgesic.
What makes a toothache worse at night?
Lying flat raises tooth pressure; nighttime clenching and fewer distractions amplify pain.
What Is Sedation Dentistry for Kids? A Simple, Honest Guide for Parents
What Is Sedation Dentistry For Kids? A Simple, Honest Guide For Parents
Sedation dentistry helps some children stay calm and comfortable during dental treatment by using carefully chosen medication. Depending on the option used, a child may remain awake and relaxed, feel very sleepy, or (in specific cases) be fully asleep. It’s typically recommended for significant anxiety, young age, special healthcare needs, or longer procedures.
Taking a child to the dentist can be surprisingly tough. Some kids manage fine until they hear instruments or smell the clinic. Others feel anxious the moment they sit in the chair.
Sedation dentistry isn’t about “knocking a child out” for convenience. It’s used to reduce fear, limit sudden movement, and make treatment safer when a child can’t cope with dental care in the usual way.
What Is Sedation Dentistry For Children?
Table of Contents
Sedation dentistry for children means using medication to help a child relax during dental treatment. The level can range from mild calmness to deep sleep, depending on the child and the procedure.
The aim is simple: a calmer child, safer treatment, and a better overall experience. Sedation is not needed for every patient, and a good dental team will recommend it only when it adds real benefit.
Why Would A Child Need Sedation Dentistry?
Every child responds differently to dental visits. Sedation may be suggested when:
- A child has strong dental fear, panic, or past trauma
- Several treatments are needed in one appointment
- The child is very young and can’t reliably stay still
- There is a sensitive gag reflex that interferes with care
- The child has medical, sensory, or developmental challenges
In the right situation, sedation can protect a child emotionally and reduce the chance of long-term dental anxiety. It can also help the dentist complete care efficiently, which may mean fewer visits overall.
Common Types Of Sedation Used For Kids
Dentists typically start with the mildest option that matches the child’s needs and the planned treatment. Here are the most common approaches:
Nitrous Oxide (Laughing Gas)
This is one of the most common choices. Your child breathes nitrous oxide through a small mask to feel calmer, while staying awake and responsive. The effects fade quickly once the mask is removed.
Oral Sedation
Oral sedation is usually given before the appointment, often as a liquid. It can make a child drowsy and deeply relaxed. Some children remember little of the procedure afterward, which can be helpful if anxiety is a big issue.
IV Sedation
IV sedation is used when a deeper level of relaxation is needed. It works quickly and is closely monitored throughout treatment by trained professionals. This option is typically reserved for more involved procedures or higher anxiety levels.
General Anesthesia
General anesthesia is used in select situations, such as extensive dental work, certain special healthcare needs, or when other options aren’t appropriate. Your child is fully asleep, and the team monitors breathing and vital signs continuously.
How Sedation Dentistry Can Help Long-Term
The emotional side matters. A difficult appointment can leave a child fearful of dental care for years.
When treatment happens in a calmer way, children are more likely to trust the dentist next time. That can make future check-ups and cleanings much easier for the whole family.
Is Sedation Dentistry Safe For Kids?

Yes—when it’s planned properly and provided by trained professionals, pediatric dental sedation is generally considered safe. Before recommending sedation, the dental team reviews your child’s medical history, age, weight, medications, and any health conditions.
During treatment, the team monitors breathing, heart rate, and oxygen levels. The most important safety step is choosing a clinic that has appropriate training, monitoring equipment, and clear emergency protocols.
How Parents Can Prepare Their Child

Follow the clinic’s instructions closely—especially rules about eating and drinking before the appointment. These guidelines exist to reduce risk and keep sedation predictable.
When you talk about the visit, keep it simple and calm. Avoid building suspense with words like “pain” or “needle.” After treatment, it’s common for children to feel tired, emotional, or a little confused for a few hours.
Book An Appointment Or Ask A Question
If you’d like to talk through sedation options, share your child’s concerns, or plan treatment, contact the clinic to get individualized guidance. Many practices can also explain related services such as general dentistry, crowns, implants, or cosmetic dentistry.
Frequently Asked Questions (FAQs)
What happens when a child is sedated?
Sedation relaxes or makes the child sleepy, reducing anxiety and movement during treatment.
What is the minimum age for dental sedation?
No fixed minimum age; dentists assess health, weight, and procedure individually.
What type of sedation is used for children?
Nitrous oxide, oral sedatives, IV sedation, or general anesthesia are used for children.
What are the risks of sedation in children?
Risks include breathing problems, low oxygen, allergic reactions, nausea, vomiting, and rare emergencies.
How safe is sedation dentistry for kids?
Sedation dentistry is very safe when performed by trained teams with continuous monitoring.
How long does sedation last for kids?
Duration ranges from minutes (nitrous) to several hours, depending on medication and dose.
How to Clean Your Teeth Without a Toothbrush?
How to Clean Your Teeth Without a Toothbrush?
Forgot your toothbrush—start by rinsing with water to loosen food debris, then gently wipe teeth and gumline with a clean finger wrapped in tissue or cloth. Sugar-free gum boosts saliva, and saltwater or mouthwash can cut bacteria and odor. Crunchy produce may help remove bits. Brush with fluoride toothpaste as soon as you can.
Most people have been caught without a toothbrush at least once—during travel, an overnight stay, or a busy day that ran longer than planned. Missing one brushing session isn’t a disaster, but letting plaque and food debris sit for too long can quickly lead to bad breath and irritated gums.
A toothbrush and fluoride toothpaste are still the best tools for daily oral care. Until you can replace them, the methods below can help you stay comfortable and keep your mouth cleaner in the short term.
Can You Clean Your Teeth Without A Brush?
Yes—well enough to get by for a short period. The goal isn’t a perfect deep clean. It’s to remove obvious debris, lower acidity after eating, and reduce the bacterial film that contributes to odor and gum inflammation.
Quick Ways To Clean Your Teeth Without A Toothbrush
1. Rinse With Water
If nothing else is available, a thorough rinse is your best starting point. Swish plain water around your mouth for 20–30 seconds, spit, and repeat once or twice.
- Dislodges food particles
- Dilutes acids after meals
- Helps keep gums calmer
- Reduces the “dry mouth” feeling that makes breath worse
2. Use A Clean Finger As A Mini Brush
It’s not elegant, but it can work surprisingly well—especially along the gumline—if your hands are clean.
- Wash your hands with soap and water.
- Wrap your index finger with tissue, a clean cloth, or a handkerchief.
- If you have toothpaste, use a pea-sized amount (or less).
- Rub teeth gently in small circles, focusing on the gumline and chewing surfaces.
- Rinse with water.
3. Chew Sugar Free Gum
Table of Contents
Sugar-free gum can help when you’re away from a sink. Chewing increases saliva, which is your mouth’s natural way of washing away debris.
- Helps rinse away leftover food
- Neutralizes acids
- Freshens breath
- Supports a moist mouth environment
If you have a choice, gum sweetened with xylitol is a popular option because it isn’t fermentable like sugar.
4. Eat Crunchy Fruits And Vegetables
You may have heard apples called “nature’s toothbrush.” That’s an overstatement, but crisp produce can lightly scrub tooth surfaces and help remove stuck-on bits of food.
- Apples
- Carrots
- Celery
- Cucumber
This doesn’t replace brushing, and it won’t remove plaque from between teeth, but it can make your mouth feel noticeably fresher.
5. Rinse With Mouthwash Or Saltwater
If you have mouthwash available, follow the label instructions and avoid swallowing it. If you don’t, saltwater is a simple alternative.
To make a salt rinse, dissolve a small pinch of salt in a glass of warm water, swish for 20–30 seconds, and spit. Many people find it
soothing for tender gums.
6. Wipe With A Clean Cloth
Before modern toothbrushes, cleaning with cloth was common. It’s still a practical emergency option.
- Wrap a clean cloth or paper towel around your finger.
- Dampen it with water (a tiny amount of toothpaste is fine if you have it).
- Gently wipe the front, back, and chewing surfaces of each tooth.
- Rinse afterward.
How People Cleaned Their Teeth Before Modern Toothbrushes

Humans have tried to keep teeth clean for thousands of years. Different cultures used simple tools and natural materials to scrape or wipe away debris.
- Miswak or other chewing sticks
- Cloth strips
- Toothpicks made from plant twigs
- Herbal powders and pastes
- Salt and ash mixtures
Some traditional tools, like miswak, are still used today. If you try natural powders, avoid anything overly abrasive that could wear enamel over time.
Why You Still Need A Real Toothbrush
 These methods can help you get through a day or two, but they’re not a long-term substitute. Plaque can harden into tartar within roughly 48–72 hours, and tartar usually needs professional removal.
These methods can help you get through a day or two, but they’re not a long-term substitute. Plaque can harden into tartar within roughly 48–72 hours, and tartar usually needs professional removal.
Brushing twice daily with fluoride toothpaste remains the most reliable routine because it removes plaque, strengthens enamel, and lowers the risk of cavities and gum disease.
When To Get Dental Advice
If you’re without a toothbrush for more than a couple of days, try to replace it as soon as possible. See a dentist sooner if you have persistent gum bleeding, swelling, severe bad breath that doesn’t improve, or tooth pain.
Frequently Asked Questions
How to clean teeth at home without a toothbrush?
Floss well, rinse with fluoridated mouthwash, and wipe teeth with clean gauze or cloth.
Can you clean teeth without brushing?
Yes, partially; floss and fluoride rinses help, but brushing removes plaque best.
What cleans teeth naturally?
Saliva and crunchy vegetables help, but fluoride and mechanical cleaning protect teeth best.
Should I brush my tongue?
Yes; gently brush or scrape to reduce bacteria and bad breath without injury.
Can I use my finger to brush?
Yes, in emergencies; use clean finger with fluoride toothpaste, but it’s less effective.
What to Pay Attention to After Tooth Preparation
After Tooth Preparation: What To Pay Attention To
After tooth preparation for a crown, veneer, or similar restoration, mild sensitivity and gum tenderness are common. Protect the tooth (and any temporary crown), choose soft foods, and keep the area clean with gentle brushing and careful flossing. Call your dentist if pain worsens, swelling increases, the temporary comes off, or your bite feels uneven.
What To Expect After Tooth Preparation
Once the numbness wears off, the tooth can feel a little “different.” You may notice sensitivity to temperature, pressure, or sweets, plus mild gum soreness if the gumline was touched during the procedure. These symptoms usually ease as the tooth and gums settle.
Why Sensitivity Happens
Table of Contents
To make room for a crown, veneer, or onlay, your dentist removes a small amount of enamel so the final restoration can fit precisely. That can temporarily expose the tooth to temperature changes and pressure. If the gum tissue was gently retracted or shaped, it can also feel tender for a few days.
What To Do In The First 24 Hours
Be Gentle With The Tooth
If you have a temporary crown or temporary veneer, avoid chewing on that side at first. Temporaries protect the tooth, but they are not as strong as the final restoration.
Wait Until Numbness Is Gone Before Eating
Eating while numb makes it easy to bite your cheek, lip, or tongue. Once sensation returns, start with soft foods and chew slowly.
Choose Tooth-Friendly Foods And Drinks
For the first couple of days, these choices tend to feel best:
- Soft foods: soup, pasta, eggs, yogurt, cooked vegetables
- Cut foods into small pieces if the temporary is on a front tooth
- Lukewarm drinks rather than very hot or ice-cold beverages
- Avoid sticky or hard foods (caramel, chewing gum, nuts, hard candy)
Keep The Area Clean Without Irritating It
Good hygiene helps the tooth and gums recover, especially while you’re waiting for the final restoration. Use a soft toothbrush and gentle pressure around the prepared tooth.
When flossing next to a temporary crown, bring the floss down, clean the sides, then slide it out to the side rather than snapping it up. That small technique can help prevent the temporary from loosening.
Managing Sensitivity And Soreness
A quick “zing” with cold water or hot coffee is common for a short period. If you need relief, a desensitizing toothpaste and an over-the-counter pain reliever can help, as directed on the label (or by your dentist).
If the tooth is extremely sensitive to biting, or the bite feels high on the temporary, contact your clinic. A simple bite adjustment can make a big difference.
If Your Gums Were Trimmed Or Shaped

Gums usually heal fast, but they can feel tender for a few days. Gentle care is the goal—keep the area clean and avoid foods that sting.
Helpful habits include:
- Warm saltwater rinses starting the day after the procedure
- Avoiding spicy, hard, or very acidic foods until tenderness settles
- Using a soft toothbrush along the gumline
- Using a cold compress on the outside of the cheek if there’s mild swelling
Typical Healing Timeline

Most people feel close to normal within a few days. As a general guide:
- Tooth sensitivity: often improves within 2–5 days
- Mild gum irritation: often improves within 3–7 days
- If stitches were placed: many heal within about 7–10 days (timing varies by material)
Once your permanent crown or veneer is placed, the tooth is fully covered again and sensitivity often drops further.
When To Call Your Dentist
Contact your clinic if you notice any of the following:
- Pain that becomes severe or keeps getting worse
- Swelling that increases instead of settling down
- A temporary crown/veneer that feels loose or falls off
- Sensitivity that lasts longer than a week without improving
- A bite that feels uneven or “off”
Small issues are usually easy to fix when they’re caught early.
Get Information Now
Contact us to learn more about cosmetic dentistry, dental crowns, dental implants, and general dentistry. We can help you book an appointment and answer questions about your treatment plan.
Frequently Asked Questions (FAQs)
What is the best thing to do after a tooth extraction?
Apply firm gauze pressure and rest, following your dentist’s aftercare instructions.
What is the most crucial time after tooth extraction?
First 24 hours are most crucial, because the blood clot forms and stabilizes.
What should you not do after a tooth extraction?
Do not smoke, use straws, spit, or rinse vigorously for at least 24 hours.
Why is day 3 the worst after tooth extraction?
Day 3 often feels worst because inflammation peaks and jaw soreness increases temporarily.
What are the red flags after tooth extraction?
Uncontrolled bleeding, worsening pain, swelling, fever, pus, foul taste, or breathing difficulty are red flags.
Does drinking water help heal tooth extraction?
Yes, drinking water supports healing by preventing dehydration; sip gently without suction.
What Happens If a Tooth That Should Be Extracted Is Not Removed?
What Happens If a Tooth That Should Be Extracted Is Not Removed?
If a tooth that needs extraction is left untreated, infection can spread to the gums and jawbone, pain often returns with greater intensity, and the supporting bone may start to break down. In some cases, oral bacteria can affect overall health. Seeing a dentist early reduces the risk of abscesses and emergency treatment.
Dentists recommend extraction only when a tooth can’t be saved safely. When a severely decayed, infected, or badly damaged tooth stays in place, the problem can move beyond the tooth itself and involve the gums, bone, and nearby tissues. Even if symptoms come and go, the underlying cause usually continues to progress.
Why A Dentist May Recommend Tooth Extraction
Most teeth can be treated with fillings, root canal therapy, crowns, or periodontal care. Extraction becomes the safest option when keeping the tooth would put the rest of your mouth at risk.
Common reasons a tooth may need to be removed include:
- Advanced decay that can’t be restored
- Repeated or severe infections
- Deep fractures below the gumline
- Severe gum disease with significant bone loss
- Impacted or problematic wisdom teeth
- Orthodontic treatment that requires space
What Can Happen If A Tooth That Needs Extraction Is Not Removed

Table of Contents
1) Infection Can Spread
Bacteria from an untreated tooth can spread into the gums and surrounding tissues. What starts as a localized infection may develop into a dental abscess, facial swelling, or a spreading infection that needs urgent care.
2) Pain Often Gets Worse, Not Better
A damaged or infected tooth rarely heals on its own. As the nerve becomes more irritated, you may feel throbbing pressure, sensitivity to temperature, and pain that radiates to the jaw, ear, or head.
3) Bone Loss And Loosening Teeth
Infection can damage the bone that supports the tooth. As the bone weakens, the tooth may become loose and the area may be harder to treat later. In severe situations, the tooth can break down or fall out, which can injure nearby tissue.
4) Possible Effects On Overall Health
Oral infections are not confined to the mouth. When bacteria enter the bloodstream or sinuses, they can contribute to wider health complications, especially in people with underlying medical conditions. This is one reason dental teams emphasize early treatment and infection control.
Health Issues That May Be Linked To Severe Untreated Tooth Decay
Research has found associations between poor oral health and certain systemic conditions. A decayed or infected tooth may contribute to complications such as:
- Sinus infections (particularly from upper back teeth)
- Cardiovascular inflammation in susceptible individuals
- Respiratory infections related to oral bacteria
- Worsening blood sugar control in people with diabetes
- Rarely, infections that spread to other parts of the body
These risks vary from person to person, but the safest approach is to treat infection early and avoid letting it linger.
What Happens If The Tooth Is Extracted But Not Replaced
Leaving an extraction space empty can cause changes in your bite and jaw over time. Replacing the tooth helps maintain function and reduces long-term complications.
1) Shifting Teeth And Bite Changes
Teeth naturally drift toward open spaces. Over time, this movement can cause crowding, misalignment, and uneven contact between the upper and lower teeth.
2) Jawbone Shrinkage (Bone Resorption)
The jawbone depends on stimulation from tooth roots. When a tooth is missing, the bone in that area can start to thin and shrink, which may affect facial support and make future implant placement more complex.
3) Chewing And Speech Difficulties
Missing teeth can make chewing less efficient and may cause you to avoid certain foods. If front teeth are missing, speech sounds may also change.
4) TMJ Stress And Muscle Strain
An unbalanced bite can strain the jaw joint and surrounding muscles. Some people notice jaw clicking, headaches, or persistent jaw fatigue.
When Extraction Is Usually The Only Safe Option
A dentist may recommend extraction when the tooth is beyond repair or when saving it would risk repeated infection or structural failure. This often includes cases where:
- Decay reaches a point where there isn’t enough healthy tooth structure to restore
- Infection involves the root and surrounding bone and keeps returning
- A fracture extends vertically or below the gumline
- The tooth causes chronic pain despite appropriate treatment
- Wisdom teeth are impacted or damaging neighboring teeth
- Orthodontic planning requires space for proper alignment
Which Teeth Are Typically The Hardest To Remove
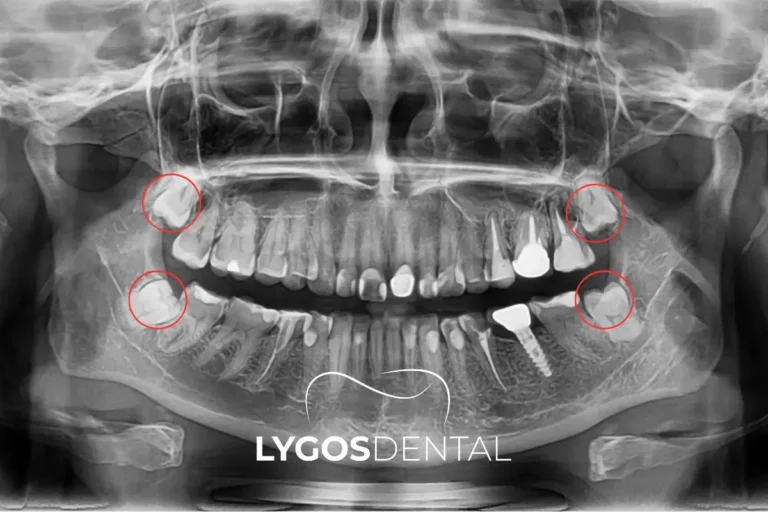
Wisdom teeth—especially impacted ones—are often the most complex. Their position at the back of the mouth, limited access, and varied root shapes can make removal more challenging. Some molars with multiple or curved roots can also require a surgical approach.
When To Seek Urgent Dental Care
Contact a dentist promptly if you have facial swelling, fever, trouble swallowing, a bad taste with pus drainage, or pain that spreads and doesn’t improve. These can be signs of a progressing infection that should not be ignored.
Frequently Asked Questions
What happens if a tooth is not extracted?
Infection and damage can worsen, spreading to bone, causing abscess, pain, and tooth loss.
What happens if you wait too long to pull a tooth?
Waiting can increase infection, pain, root damage, and make extraction more difficult.
How long will a tooth hurt before the nerve dies?
Nerve death can take days to months, and pain may persist intermittently.
What stops tooth nerve pain immediately?
Dental local anesthetic stops tooth nerve pain immediately; see a dentist urgently.
What does a damaged tooth nerve feel like?
Damaged tooth nerve feels like sharp, lingering pain to hot, cold, or biting.
What’s the best painkiller for tooth nerve pain?
Ibuprofen is usually best; acetaminophen helps if NSAIDs aren’t safe.
Alveolar Arch: Its Role in Oral Health and Function
Alveolar Arch: Its Role In Oral Health And Function
The alveolar arch is the tooth‑bearing part of the upper and lower jawbones. It holds each tooth in a socket, helps the bite distribute chewing forces, and supports the shape of the lips and lower face. When the arch loses bone—often from gum disease or missing teeth—teeth may shift, loosen, and function can change.
Most people think of oral health as teeth and gums, but those tissues rely on a hidden foundation: the alveolar arch. This curved ridge of bone supports the tooth sockets, guides how the upper and lower teeth meet, and plays a direct role in chewing and speech.
Because the alveolar arch responds to everyday forces, it can strengthen with healthy stimulation and shrink when teeth are lost or inflammation persists. Understanding this structure helps explain why timely periodontal care, tooth replacement, and orthodontic planning matter.
What Is The Alveolar Arch?
The alveolar arch is the bony ridge of the maxilla (upper jaw) and mandible (lower jaw) that contains the tooth sockets (alveoli). Each tooth root sits in its own socket, anchored by periodontal ligament fibers and surrounded by alveolar bone.
Clinicians may also use related terms such as the alveolar process (the tooth‑bearing portion of the jaw) and the alveolar ridge/crest (the highest edge of that bone around the teeth). Together, these structures provide the support needed for stable, comfortable function.
Why The Alveolar Arch Matters
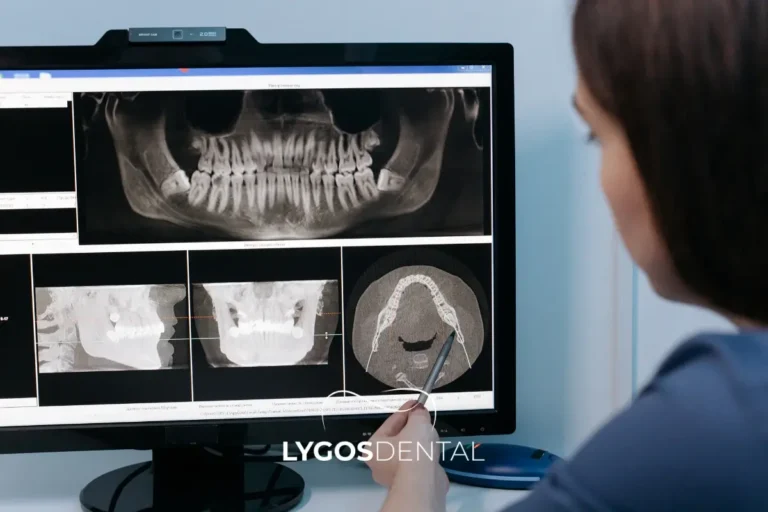
Table of Contents
It Keeps Teeth Stable
Healthy alveolar bone maintains firm support around the roots. When bone height or density decreases, teeth can loosen, migrate, or become more sensitive to bite forces.
It Helps Maintain Facial Shape
The arch supports soft tissues of the mouth and lower face. Bone loss after tooth loss or advanced gum disease can contribute to a flatter profile around the lips and cheeks over time.
It Supports A Balanced Bite
The size and curvature of the upper and lower arches affect how teeth fit together. A narrow arch can increase crowding, while an uneven arch form can contribute to crossbites, open bites, or excessive tooth wear.
It Influences Speech And Chewing
The arch helps guide tongue space and the path of chewing. When the arch is irregular or teeth shift, some sounds may be harder to form clearly and food may not break down as efficiently.
How The Alveolar Arch Develops

Arch development begins as primary (baby) teeth erupt and continues through adolescence as the jaws grow and permanent teeth come in. Genetics influence arch shape, but habits can change it, especially during growth.
- Thumb‑sucking or prolonged pacifier use (may narrow the upper arch)
- Mouth breathing and chronic nasal obstruction (can affect jaw posture and arch form)
- Premature tooth loss (may allow neighboring teeth to drift)
In adulthood, the alveolar bone remains biologically active. It is maintained by healthy chewing forces and periodontal health, and it tends to resorb in areas where teeth are missing.
Common Problems That Affect The Alveolar Arch
Periodontal Disease And Bone Loss
Untreated gum disease can destroy the supporting tissues and reduce alveolar bone height. As support decreases, teeth may become mobile and bite relationships can change.
Tooth Loss, Extractions, And Trauma
After an extraction, the bone in that region commonly shrinks, especially during the first months. Without a timely replacement plan, the ridge can lose volume and make future implant or denture fit more challenging.
Developmental Differences
Some people naturally have narrower or wider arches, which can affect spacing, crowding, and airway comfort. Early assessment during childhood can help guide orthodontic timing and reduce complications.
Orthodontic And Bite Concerns
Crossbites, crowding, and open bites often relate to how the arches developed and how teeth erupted within them. Orthodontic treatment aims to align teeth within a stable arch form while respecting bone limits.
How Dentists Evaluate The Alveolar Arch
Dentists assess the alveolar arch through a clinical exam and imaging. X‑rays help measure bone levels and detect changes around the roots, while 3D imaging (CBCT) may be used when planning implants, grafting, or complex orthodontics.
Your dentist will also evaluate gum health, tooth mobility, bite contacts, and any signs of parafunction such as clenching or grinding. These findings guide prevention and treatment choices.
Treatment Options
Periodontal Therapy
Early treatment of gum inflammation helps preserve bone support. Depending on severity, care may include deep cleaning, targeted antimicrobial therapy, and ongoing maintenance visits.
Orthodontic Expansion And Alignment
When arch width contributes to crowding or crossbite, orthodontic appliances can create space and improve how the arches relate. Treatment is planned to move teeth safely within the available bone.
Bone Grafting
If bone volume is insufficient—often after tooth loss or long‑standing periodontal disease—grafting can rebuild the ridge. This may be done to support implants or to restore arch contour for better function and aesthetics.
Dental Implants And Restorations
Implants can help maintain bone by transferring chewing forces into the jaw, while bridges or dentures restore function and prevent drifting. The best option depends on bone levels, bite, and general health factors.
How To Protect The Alveolar Arch
Protecting the alveolar arch comes down to controlling inflammation and keeping teeth functioning. Consistent home care, regular professional cleanings, and early treatment of gum bleeding are the most effective steps.
If a tooth is lost, discuss replacement timelines soon after extraction to reduce bone shrinkage. For people who grind their teeth, a night guard may help limit excessive forces that stress teeth and supporting bone.
When To Seek Professional Advice
Book an evaluation if you notice persistent gum bleeding, loosening teeth, shifting bite, or difficulty chewing. These signs may indicate changes in the supporting bone that are easier to manage when caught early.
Frequently Asked Questions
What is the alveolar arch?
The alveolar arch is the curved jawbone ridge that houses the tooth sockets.
What is the function of the alveolar bone in the teeth?
Alveolar bone supports and anchors teeth via the periodontal ligament and absorbs biting forces.
What is the primary function of the alveolar ridge?
The alveolar ridge provides the bony foundation for teeth and supports dentures after loss.
What is the function of the alveolar process?
The alveolar process forms the tooth sockets and maintains tooth support in the jaw.
What does alveolar mean in dental?
Alveolar means relating to the tooth sockets and the supporting jawbone around them.
What happens when alveolar bone is lost?
Alveolar bone loss causes tooth looseness, ridge resorption, impaired chewing, and harder implant placement.
What Is the 7–4 Rule and Why Is It Important in Pediatric Dentistry?
What Is The 7–4 Rule In Pediatric Dentistry?
The 7–4 rule is a quick way to estimate baby tooth eruption: many babies get their first tooth around 7 months, then gain roughly four new teeth every four months until most have 20 primary teeth by about age 2½–3. It’s a guide, not a diagnosis. If eruption seems very delayed, a dental check is wise.
What The 7–4 Rule Means
The name can be confusing because different clinics describe it in slightly different ways. In everyday pediatric dentistry, it’s best understood as a memory aid for early tooth eruption: teething often begins around seven months, then new teeth tend to appear in “bursts” over the next couple of years.
Some people summarize it as “four teeth every four months,” while others use a simple subtraction shortcut to estimate how many teeth a child may have at a given month. Either way, the point is the same: it helps parents notice patterns, not count teeth with scientific precision.
What The Rule Does Not Mean

Table of Contents
The 7–4 rule doesn’t replace an eruption chart, and it doesn’t predict the exact order or the exact month a tooth will show up. Healthy children can be early or late teether’s by several months. A dentist looks at the whole picture—growth, family history, diet, oral habits, and the health of the gums.
Typical Baby Tooth Milestones

Most primary teeth erupt between about 6 months and 3 years. To keep this practical, these milestones are often used as a quick check:
- Around 6–10 months: the first lower front teeth (central incisors) often appear.
- Around 8–13 months: upper front teeth commonly follow.
- Around 12–23 months: first molars and canines usually come in.
- Around 20–33 months: second molars typically complete the set.
- By about 2½–3 years: many children have all 20 primary teeth.
If you want exact ranges by tooth, ask your dentist for a tooth eruption chart. Charts are especially helpful if you’re tracking spacing, crowding, or the timing of molars.
Why The 7–4 Rule Matters
Primary teeth are not “practice teeth.” They help children chew comfortably, speak clearly, and guide the position of permanent teeth. When eruption is far outside the expected window, it can signal issues worth checking—such as a tooth that’s blocked, a missing tooth, or (less commonly) a medical or nutritional factor affecting development.
The rule is also useful because it encourages earlier preventive care. A quick pediatric dental visit can catch early cavities, review brushing technique, and help parents prevent problems before they become painful.
When To See A Pediatric Dentist

A dentist can reassure you when timing is normal for your child, and they can investigate when something looks unusual. Consider booking a visit sooner if any of these apply:
- No teeth have erupted by 12 months, or there’s a sudden stall after teething has started.
- A tooth seems stuck (the gum is swollen for weeks without eruption) or erupts in an unusual position.
- Your child has pain, swelling, fever, or a bad taste that could suggest infection.
- Early loss of a baby tooth from decay or injury.
- You notice persistent mouth breathing, thumb sucking beyond toddler years, or other habits affecting jaw development.
Many pediatric dental teams recommend the first dental visit by age one or within six months of the first tooth. That early appointment is usually short and gentle, and it sets the stage for stress-free checkups later.
How To Protect Your Child’s Teeth From The Start
Daily Cleaning
Start cleaning as soon as the first tooth appears. Use a soft, age-appropriate toothbrush and a tiny smear of fluoride toothpaste. As your child learns to spit (usually around age 3), you can move toward a pea-sized amount.
Food And Drinks
Frequent sugar is a bigger risk than the occasional treat. Keep sweet drinks and snacks to mealtimes when possible, and offer water between meals. Avoid sending a child to bed with milk or juice in a bottle, because sugar can sit on teeth for hours.
Regular Checkups
Routine visits help track eruption, monitor bite development, and catch early signs of decay. Your dentist may also recommend fluoride varnish, and later, sealants when permanent molars erupt.
Frequently Asked Question
What is the alveolar arch?
The alveolar arch is the curved jawbone ridge that houses the tooth sockets.
What is the function of the alveolar bone in the teeth?
Alveolar bone supports and anchors teeth via the periodontal ligament and absorbs biting forces.
What is the primary function of the alveolar ridge?
The alveolar ridge provides the bony foundation for teeth and supports dentures after loss.
What is the function of the alveolar process?
The alveolar process forms the tooth sockets and maintains tooth support in the jaw.
What does alveolar mean in dental?
Alveolar means relating to the tooth sockets and the supporting jawbone around them.
What happens when alveolar bone is lost?
Alveolar bone loss causes tooth looseness, ridge resorption, impaired chewing, and harder implant placement.
What Is the 2-2-2 Rule for Brushing Teeth?
What Is the 2-2-2 Rule for Brushing Teeth?
The 2-2-2 rule is a quick way to remember healthy brushing habits: brush your teeth two times a day, for two minutes each time, and schedule dental checkups on a regular basis—often twice a year. Done consistently, it helps control plaque, protect gums, and catch small problems early.
What The 2-2-2 Rule Means
This rule bundles three basics into one easy reminder. It’s simple, but it covers the habits dentists see people miss most often.
Brush Twice A Day
Aim for a morning brush and a brush before bed. Night brushing matters because saliva flow drops while you sleep, which gives bacteria an easier time.
Brush For Two Minutes
Most people stop too soon without realizing it. Two full minutes gives you enough time to clean the gumline and reach every surface, including the back teeth.
See Your Dentist Regularly
Many clinics recommend a checkup and cleaning every six months, but the best interval depends on your cavity and gum-risk. Your dentist may suggest visits more or less often based on your mouth, medical history, and home care.
Why The Rule Works
Plaque forms constantly, and it hardens into tartar if it isn’t removed. Twice-daily brushing and routine professional cleanings keep plaque from building up and give your dentist a chance to spot early decay or gum inflammation.
Step-By-Step Brushing Technique

Table of Contents
If you want a simple routine that covers the whole mouth, follow this sequence:
- Start on the outer surfaces of the upper teeth, then the lower teeth.
- Move to the inner surfaces, where plaque often collects near the gumline.
- Brush the chewing surfaces with short, controlled strokes.
- Angle the bristles about 45 degrees toward the gumline and use small circles or gentle back-and-forth motions.
- Brush your tongue (or use a tongue scraper) to reduce bacteria and improve breath.
Keep pressure light. Scrubbing harder doesn’t clean better, and it can irritate gums or wear enamel over time.
Habits That Improve Results
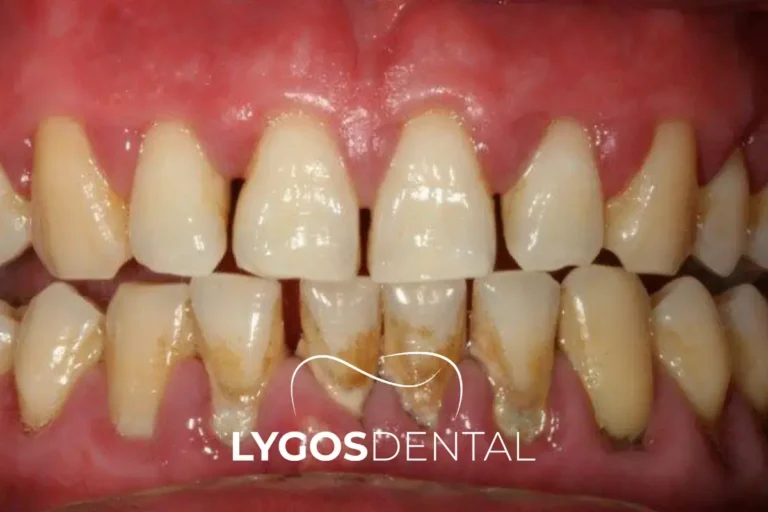
Small choices make a big difference in how well brushing protects your teeth:
- Use a soft-bristled toothbrush that fits comfortably in your mouth.
- Replace your toothbrush (or brush head) every 3–4 months, or sooner if bristles fray.
- Use a fluoride toothpaste to help strengthen enamel.
- Floss once a day to clean between teeth where a brush can’t reach.
- After acidic food or drinks, wait about 30 minutes before brushing to protect softened enamel. Rinse with water in the meantime.
What Happens If You Skip Brushing For One Night?
One missed night won’t ruin your teeth. Still, plaque builds quickly overnight, and you may notice morning breath or gum tenderness.
If skipping becomes frequent, the risk climbs—more tartar, more inflammation, and a higher chance of cavities.
How Often Should You Brush?
For most people, twice daily is the sweet spot. A third gentle brush after lunch can help, especially if you’re prone to cavities or wear aligners.
If you brush more often, keep it gentle and avoid brushing right after acidic meals. Overbrushing with heavy pressure can irritate gums.
A Practical Order For Brushing
Any order is fine as long as you cover every surface. Many dentists suggest a consistent pattern so nothing gets missed:
-
- Upper teeth, outer surfaces: right to left.
- Lower teeth, outer surfaces: right to left.
- Upper and lower teeth, inner surfaces.
- Chewing surfaces, then tongue.
Why This Matters For Long-Term Oral Health
The 2-2-2 rule is memorable, realistic, and easy to teach to kids and adults. Over time, it can mean fewer fillings, less gum bleeding, and fewer urgent dental visits.
At Lygos Dental, our clinicians often share this framework with patients who want a simple routine they can stick to.
Make An Appointment
If you’d like a personalized cleaning schedule or help improving your home-care routine, contact our team to book a visit.
Services include cosmetic dentistry, dental crowns, dental implants, and general dentistry.
Frequently Asked Questions
What is the 2-2-2 rule in dentistry?
Brush twice daily for two minutes, and visit your dentist twice yearly.
What is the 333 rule for brushing teeth?
Brush within three minutes after eating, for three minutes, three times daily.
What is the 222 rule in dentistry?
Brush twice daily for two minutes, and get dental checkups twice yearly.
What is the 222 rule for brushing teeth?
Brush twice daily for two minutes, using about 2 centimeters of toothpaste.
What is the 20 20 20 rule for dental hygiene?
It’s a 60-minute hygiene visit split into 20-minute history, scaling, and polish/exam blocks.
What does 323 and 333 and 222 mean in dentist terms?
323 is pocket-depth mm; 333 is brush 3×/day 3 minutes; 222 is 2×/day 2 minutes.
What Is Buccal Mucosal Cancer
What Is Buccal Mucosal Cancer
Buccal mucosal cancer (inner cheek cancer) is an oral cancer that starts in the lining of the cheeks, most often in squamous cells. It can appear as a sore, red or white patch, or a lump that doesn’t heal. Early evaluation and biopsy are vital because treatment is usually most effective before the cancer spreads.
What Is The Buccal Mucosa?
The buccal mucosa is the soft, moist tissue that lines the inside of each cheek. It helps protect the mouth from friction, bacteria, and everyday irritation, while supporting speech and chewing. Small injuries in this area often heal quickly, but long-term irritation can damage cells over time.
How Buccal Mucosal Cancer Develops

Table of Contents
Buccal mucosal cancer usually begins when the DNA inside lining cells is damaged repeatedly. Over time, abnormal cells can grow out of control and form a tumor. If it isn’t detected early, the cancer may spread deeper into the cheek, nearby structures such as the jaw, or to lymph nodes in the neck.
Common Risk Factors
Risk varies from person to person, but these factors are commonly linked to oral cavity cancers:
- Tobacco Use: Smoking and smokeless tobacco (including chewing tobacco) expose the mouth to carcinogenic chemicals and greatly increase risk.
- Alcohol Consumption: Heavy, frequent alcohol use irritates the mucosa and can magnify the harmful effects of tobacco.
- Chronic Irritation: Sharp teeth, poorly fitting dentures, or repeated cheek biting can cause ongoing inflammation. Irritation alone doesn’t cause cancer, but it can contribute to long-term tissue damage.
- HPV Infection: Certain high-risk HPV types are strongly linked to cancers in the throat (oropharynx). HPV can also play a role in some oral cancers, depending on the site and individual factors.
- Poor Oral Hygiene: Untreated gum disease, chronic inflammation, and persistent infections can weaken the mouth’s natural defenses.
Symptoms Of Inner Cheek Cancer
Buccal mucosal cancer may start subtly. Common warning signs include:
- A sore inside the cheek that doesn’t heal
- White or red patches on the inner cheek
- A lump, thickening, or rough area in the cheek
- Pain or tenderness when chewing
- Difficulty opening the mouth fully
- Unexplained bleeding in the mouth
- Numbness in the cheek or nearby areas
If you notice any of these symptoms lasting longer than two weeks, arrange an evaluation with a dentist, oral and maxillofacial surgeon, or an ENT specialist.
Diagnosis And Treatment

A dental professional will usually start with a thorough oral exam and review of your symptoms and risk factors. If a suspicious area is found, a biopsy is the only way to confirm whether cancer is present. Imaging tests (such as CT, MRI, or PET/CT) may be used to understand the tumor’s size and whether it has spread.
Treatment Options
Treatment depends on the tumor’s stage, location, and your overall health. Options may include:
- Surgery: Often the first-line treatment for early disease, aiming to remove the tumor with a margin of healthy tissue.
- Radiation Therapy: May be used after surgery or as a primary treatment in selected cases to destroy cancer cells or shrink a tumor.
- Chemotherapy: Can be combined with radiation or used when cancer has spread or is at higher risk of returning.
- Targeted Therapy Or Immunotherapy: In some advanced or recurrent cases, oncologists may consider medicines that target specific pathways or help the immune system respond to cancer.
- Reconstruction And Rehabilitation: If tissue is removed, reconstructive procedures, speech therapy, and dental rehabilitation can help restore function and appearance.
Many patients do best with a coordinated care team that may include an oral surgeon, head and neck surgeon, medical oncologist, radiation oncologist, and dentist.
How to Reduce the Risk of Inner Cheek Cancer

You can lower your risk by focusing on habits that protect the oral tissues:
- Quit smoking and avoid all tobacco products
- Limit alcohol consumption
- Brush and floss consistently and treat gum disease early
- Fix dental problems that cause ongoing irritation (sharp teeth, broken fillings, poorly fitting dentures)
- Schedule regular dental check-ups so changes can be noticed early
At Lygos Dental, oral cancer screening can be included as part of routine exams to help identify suspicious changes early.
Book An Appointment
If you’d like to discuss symptoms, request an oral screening, or learn more about our services, you can contact our clinic to schedule an appointment.
Frequently Asked Questions
What is the cause of buccal mucosa cancer?
Causes include tobacco, heavy alcohol, betel nut chewing, and HPV infection.
What is the survival rate for buccal mucosa cancer?
Five-year relative survival is about 69.5% overall; localized disease about 88.4%.
How fast does buccal mucosa cancer spread?
It can spread quickly, first locally, then to nearby neck lymph nodes.
What are the symptoms of Stage 1 buccal mucosa cancer?
Stage 1 may cause a small persistent cheek sore/ulcer, red/white patch, or lump.
What are the 7 warning signs of mouth cancer?
Nonhealing sore, red/white patch, lump, bleeding, numbness, trouble swallowing/chewing, loose teeth.
Is buccal mucosa cancer curable?
Yes—early-stage buccal mucosa cancer is often curable with surgery and/or radiotherapy.
