Brushing Teeth with the 3-3-3 | LYGOS DENTAL
Brushing Teeth with the 3-3-3
The 3-3-3 rule is a simple reminder to brush regularly and long enough to clean every surface of your teeth. It’s often described as brushing three times a day for about three minutes. Use it flexibly: twice-daily brushing is the baseline for most people, and after acidic meals it’s usually better to wait before brushing.
What The 3-3-3 Rule Means
You’ll see the 3-3-3 rule described in a few different ways online. The most common version is:
- Brush up to 3 times a day (morning, after lunch, and before bed).
- Brush for about 3 minutes to cover every tooth surface and the gumline.
- Brush after meals when practical—especially after lunch or snacks—rather than waiting until the next routine.
Think of it as a structure, not a strict medical requirement. The goal is consistent plaque control without over-brushing or irritating the gums.
How It Fits With Standard Dental Advice

Table of Contents
Major dental organizations generally recommend brushing twice a day for two minutes with fluoride toothpaste. That routine is enough for many people when technique is solid and daily interdental cleaning is in place.
A third brush (usually after lunch) can be helpful if you snack often, wear braces or aligners, or struggle with plaque. The key is gentle brushing with a soft-bristled brush and the right timing after certain foods and drinks.
When To Brush After Eating
After you eat, mouth bacteria start breaking down carbohydrates and the pH in your mouth can drop. That acidic window makes enamel more vulnerable, especially after citrus, soda, sports drinks, wine, or sour candy.
If the meal or drink was acidic, many dentists advise waiting around 30–60 minutes before brushing. This gives saliva time to neutralize acids and lets enamel reharden. If you want to do something right away, rinse with water, chew sugar-free gum, or use an alcohol-free fluoride mouthwash at a different time than brushing.
If the meal wasn’t very acidic, brushing soon after eating can be fine—just keep the pressure light and focus on technique rather than scrubbing.
Correct Technique: The Bass Technique In Plain English
Timing matters, but technique determines results. The Bass Technique is widely used because it targets plaque where it collects most: along the gumline.
How To Do It
- Place the brush at a 45-degree angle toward the gumline.
- Use small, gentle vibrations or short circular motions—avoid hard, back-and-forth scrubbing.
- Spend about 10–20 seconds per small section, then move to the next.
- Brush the outer, inner, and chewing surfaces, then lightly brush your tongue.
If you use an electric toothbrush, let it do the work. Hold it in place on each tooth surface and guide it slowly along the gumline.
Who May Benefit From Brushing Three Times A Day

Brushing three times daily can be useful when your risk of plaque buildup is higher. It’s often a good fit for:
- People who snack frequently or sip sugary drinks through the day.
- Patients with braces, aligners, bridges, or implants who need extra cleaning around hardware.
- Anyone prone to cavities, gingivitis, or persistent bad breath.
- People who struggle to floss consistently and need a stronger routine while they build the habit.
If you already have gum recession, enamel wear, or sensitivity, a dentist can help you tailor the routine so it protects your teeth instead of aggravating them.
Choosing The Right Toothbrush And Toothpaste
Toothbrush
- Choose soft bristles to reduce abrasion and gum irritation.
- A small-to-medium brush head makes it easier to reach back molars.
- Electric toothbrushes can improve plaque removal for many people, especially if timing or technique is inconsistent.
Toothpaste
- Use a fluoride toothpaste. Many adult toothpastes contain about 1,350–1,500 ppm fluoride.
- If you get cavities often, ask your dentist whether a higher-fluoride toothpaste is appropriate.
- Avoid very abrasive whitening pastes if you have sensitivity or visible enamel wear.
A Simple Daily Routine Using The 3-3-3 Idea
Morning
- Brush thoroughly (aim for 2–3 minutes).
- Spit, but avoid rinsing with water right away so fluoride can stay on the teeth longer.
- Clean between teeth (floss or interdental brushes) at some point during the day.
Midday
- If you can brush after lunch, do it gently.
- After acidic foods or drinks, rinse with water first and wait 30–60 minutes before brushing.
- If brushing isn’t possible, water rinse and sugar-free gum can help until you get home.
Night
- Brush before bed—this is the most protective brush of the day.
- Clean between teeth to remove plaque from areas a toothbrush can’t reach.
- Avoid eating or sugary drinks after you’ve brushed.
Signs Your Brushing Routine Needs Adjusting

Even with a structured routine, technique or timing issues can show up. Watch for:
- Bleeding gums that don’t improve after a week or two of gentle brushing and flossing.
- Persistent bad breath despite brushing your tongue.
- Sensitivity, gum recession, or notches near the gumline (possible over-brushing).
- Visible plaque along the gumline or a rough feeling on teeth.
If you notice these signs, a professional cleaning and a quick technique check can make a big difference.
Professional Care At Lygos Dental
Home care works best when it’s supported by regular dental visits. At Lygos Dental, we help patients fine-tune brushing and interdental cleaning based on their mouth, restorations, and risk factors.
If you’re unsure whether the 3-3-3 routine is right for you—or you’re dealing with sensitivity, gum bleeding, or frequent cavities—book a check-up so you can get a plan that’s both effective and safe.
Brushing Teeth With The 3-3-3 Rule FAQ
What is the 333 rule in Korea?
Brush teeth three times daily, within three minutes after meals, for at least three minutes.
What is the 3-3-3 brushing method?
Brush three times daily, within three minutes after meals, for at least three minutes.
What is the 3-3-3 rule for life?
Identify three things you see, three sounds you hear, and move three body parts.
What is the 3-3-3 rule for humans?
Rule: 3 minutes without air, 3 days without water, 3 weeks without food.
Why is the 3-3-3 rule so popular?
Brush three times daily, within three minutes after meals, for at least three minutes.
What is the 3-3-3 rule for health?
Brush three times daily, within three minutes after meals, for at least three minutes.
What Is Dental Wax and How to Use It? | LYGOS DENTAL
What Is Dental Wax and How to Use It?
Orthodontic dental wax is a soft, moldable barrier that covers sharp brackets or wires so they stop rubbing your cheeks, lips, or gums. Dry the metal, warm a pea-sized piece between clean fingers, then press it firmly onto the irritating spot. Swap it out after meals or brushing, or anytime it loosens.
What Dental Wax Is
Dental wax (also called orthodontic wax) is a soft, pliable material designed for people wearing braces and other orthodontic appliances. It temporarily covers sharp edges on brackets, hooks, and wire ends. Once it warms to body temperature, it molds into a smooth layer that reduces friction against the soft tissue inside your mouth.
Most orthodontic waxes are made from food-safe waxes such as paraffin, beeswax, or carnauba wax. They’re usually clear or slightly opaque, and some are lightly flavored. Wax is meant for comfort, not repair—if something is broken or poking, your orthodontist still needs to fix the cause.
When To Use Dental Wax
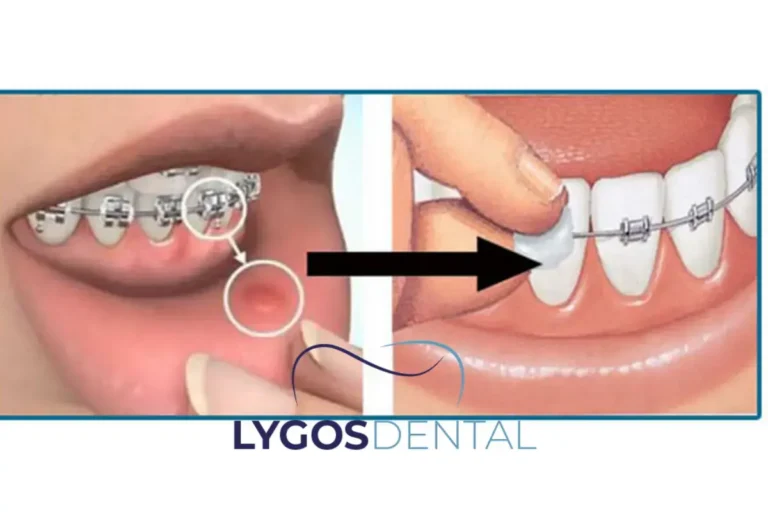
Table of Contents
Wax is most helpful during the first week of braces, after adjustments, or anytime a new component starts rubbing. It can also protect a sore spot while your mouth heals.
- A bracket or hook is rubbing the inside of your cheek or lip
- A wire end feels sharp or is starting to poke
- A new elastic, spring, or appliance creates a pressure point
- You can’t get an urgent appointment the same day and need short-term relief
How To Apply Dental Wax

Using the right technique helps wax stay in place longer and keeps the area cleaner.
Wash Your Hands
Clean hands reduce the chance of introducing bacteria when you touch your braces.
Dry The Area
Wax won’t stick well to wet metal. Use a tissue, gauze, or a cotton swab to dry the bracket or wire.
Use A Small Piece
Pinch off a pea-sized amount. Too much wax can feel bulky and may fall off sooner.
Warm And Shape It
Roll it between your fingers for a few seconds until it softens, then form a small ball or flat pad.
Press Onto The Irritating Spot
Place the wax directly over the bracket or wire end and press firmly. Smooth the edges so it forms a comfortable shield.
Replace When Needed
Change the wax if it becomes dirty, loose, or uncomfortable, especially after eating or brushing.
Tips To Make Wax Stay In Place
- Apply wax to dry metal and dry surrounding tissue when possible
- Use fresh wax each time rather than reusing a piece
- Remove wax before brushing and flossing, then reapply afterward
- Carry a small case in your bag for school, work, or travel
- If a wire is poking badly, contact your orthodontist—wax is only a temporary fix
Benefits of Dental Wax
Less Irritation And Pain
Creates a cushion over sharp areas to help prevent cuts and sores.
Easier Speaking And Eating
Reduces rubbing so day-to-day activities feel more normal.
Supports Healing
By limiting friction, it gives ulcers and tender spots time to settle.
Generally Safe If Swallowed
Small accidental pieces typically pass through the digestive system without problems.
Portable And Simple
Comes in a small container and can be applied in minutes.
Common Mistakes To Avoid

- Putting wax on a wet bracket or wire
- Using a large chunk that feels bulky or falls off quickly
- Leaving old, dirty wax in place for too long
- Trying to “fix” a broken bracket with wax instead of booking a repair visit
- Ignoring a poking wire that needs adjustment
Dental Wax FAQs
How to properly use dental wax?
Soften a pea-sized piece, dry area, press wax over irritating spot; replace daily.
How long can you leave dental wax on?
Leave it until it falls off or you remove it; replace when dirty.
When should I use dental wax?
Use it when braces or a sharp tooth edge irritates cheeks, lips, or tongue.
Can dental wax help toothache?
No; it only cushions irritation, so see a dentist for toothache.
Can I eat with dental wax on my tooth?
Yes, but wax may dislodge; remove before hot, sticky, or hard foods.
Can you sleep with dental wax on a tooth?
Yes, if well-adhered; remove and reapply if it loosens to avoid swallowing.
Can I brush with dental wax?
No; remove wax before brushing and flossing, then reapply afterward if needed.
Why Black Lines Form on Teeth and How to Treat Them | LYGOS DENTAL
Why Black Lines Form On Teeth And How To Treat Them
Black lines on teeth are usually caused by surface staining or hardened plaque (tartar) collecting near the gumline or between teeth. Less commonly, a dark line can signal early tooth decay or an aging restoration. A dental exam confirms the cause, and professional cleaning, stain removal, or restorative care can usually clear the line safely.
Thin dark streaks can show up suddenly or build slowly over time, often where plaque is hardest to remove. Some are purely cosmetic, while others are an early warning sign of decay or gum disease. Knowing what the line represents makes it easier to choose the right fix and prevent it from coming back.
What Black Lines On Teeth Usually Mean
Most black lines are a type of extrinsic discoloration—stain sitting on the surface—or darkened tartar at the gum margin. Because tartar is mineralized plaque, it can’t be brushed off at home once it forms. If the line looks like it is “inside” the tooth, spreads, or sits at the edge of a filling or crown, decay or leakage around dental work becomes more likely.
Common Causes Of Black Lines On Teeth
Several issues can create the same visual problem, so appearance alone isn’t a perfect guide. These are the most common causes dentists see:
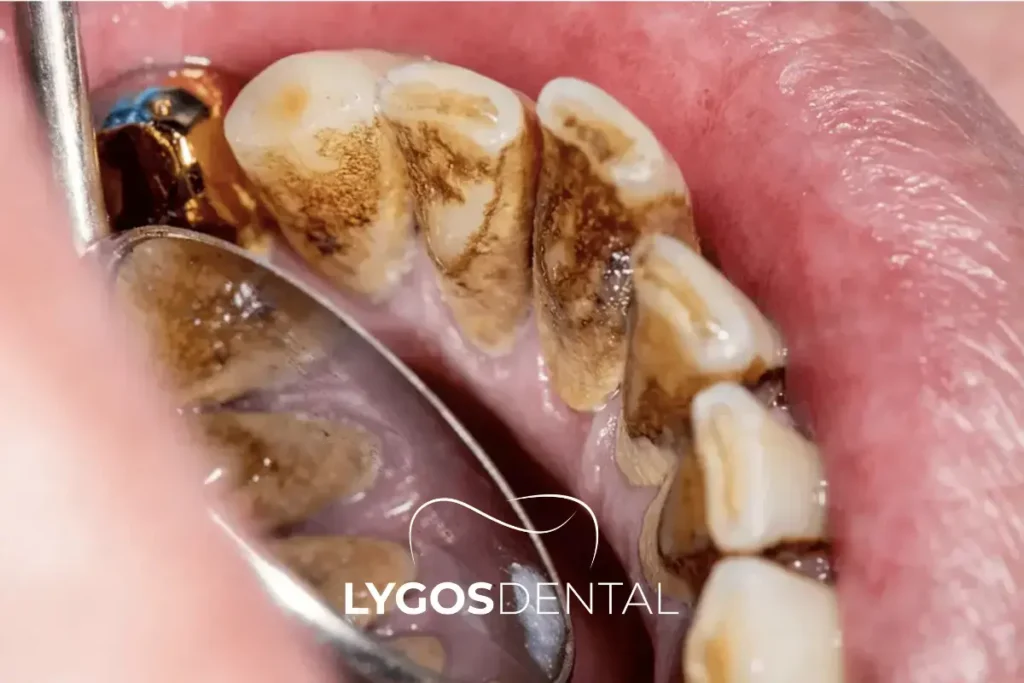
Table of Contents
Tartar And Plaque Buildup
When plaque is left in place, it hardens into tartar (also called dental calculus). Tartar can trap pigments from food, drinks, or smoking and may look brown or black along the gumline. Only a dentist or hygienist can remove it with professional instruments.
Chromogenic Bacteria
Some oral bacteria produce pigments that stick to the tooth surface. This often shows up as black dots or a thin line at the cervical third of the tooth (close to the gumline) and is seen frequently in children, though adults can get it too.
Staining From Foods, Drinks, And Tobacco
Coffee, tea, red wine, cola, and tobacco can leave dark stains that collect in grooves, between teeth, or where plaque is retained. If you drink or smoke frequently, stains can reappear quickly after cleaning.
Early Tooth Decay
A dark line that expands, feels rough, or catches floss can be an early cavity. Decay is more suspicious when the area is soft, sensitive, or located around an old filling.
Gum Recession
As gums recede, the root surface becomes exposed. Root surfaces are more porous than enamel, so they can pick up stain easily, creating a darker line along the gum margin.
Old Metal-Based Restorations
Older crowns or restorations that contain metal can sometimes create a dark edge at the margin. A visible line may also mean the restoration is aging or no longer sealing perfectly.
How Black Lines Tend To Look
Dentists often use the pattern and location to narrow down the cause:
- Thin border along the gumline: commonly tartar, chromogenic stain, or retained plaque.
- Dark streaks between teeth: often plaque retention and surface stain; sometimes early decay.
- Small dark spot that slowly widens: more suspicious for a cavity.
- Dark line around a crown or filling: can be stain at the margin or a restoration issue.
Many surface stains and tartar deposits don’t hurt. If the black line comes with bleeding gums, persistent bad breath, swelling, or sensitivity to cold or sweets, book a dental visit sooner rather than later.
Treatment Options

The best treatment depends on the diagnosis. Your dentist may use one or more of the following:
Professional Cleaning (Scaling And Polishing)
Routine cleaning removes plaque, tartar, and many surface stains. It’s the most effective first step for black calculus or gumline staining.
Air Polishing
Air polishing uses a controlled stream of air, water, and fine powder to lift stubborn extrinsic stains from enamel and hard-to-reach grooves.
Teeth Whitening
When discoloration is embedded in the enamel, whitening can brighten the tooth after the surface is cleaned. Whitening won’t remove tartar and should be done after a professional exam.
Fillings Or Other Restorative Care
If decay is the cause, your dentist removes the damaged area and restores the tooth with a filling or another suitable option.
Replacing A Crown Or Restoration
If the dark line is caused by an older restoration, replacing it with a modern material (often all-ceramic) can improve both the seal and the appearance.
Gum Disease Treatment
If there is gum inflammation or deep tartar below the gumline, treatment may include deeper cleaning (scaling and root planing) and a tailored home-care plan.
How To Prevent Black Lines From Coming Back
Prevention is mostly about reducing plaque retention and limiting stain exposure. These habits make the biggest difference:
- Brush twice daily with fluoride toothpaste, spending extra time at the gumline.
- Clean between teeth daily with floss or interdental brushes.
- Limit frequent sipping of staining drinks; rinse with water afterward.
- Avoid tobacco products.
- Keep regular dental cleanings as advised by your dentist (often every 6 months, but it varies).
- Ask your dentist whether an antiseptic rinse is appropriate for you if bacterial staining is suspected.
When To See A Dentist
Book an appointment if the line is new and spreading, you notice sensitivity, or there’s a dark edge around a filling or crown. Seek prompt care for swelling, pus, fever, or significant pain. A quick exam can rule out cavities and gum problems and save you from bigger treatment later.
Frequently Asked Questions
How to get rid of black lines on a tooth?
Remove black lines by professional cleaning, polishing, or treating decay at a dentist.
How to treat black marks on teeth?
Treat black marks with brushing, flossing, whitening, and dental evaluation for stains or decay.
What causes black lines on teeth?
Black lines are caused by stain, tartar buildup, enamel cracks, or cavities.
Are black lines on teeth reversible?
Some black lines are reversible with cleaning; lines from cracks or decay aren’t.
Do black lines require a filling?
Black lines require a filling if they indicate tooth decay, not simple staining.
Does Tooth Decay Damage the Heart? | LYGOS DENTAL
Does Tooth Decay Damage the Heart?
Untreated tooth decay can contribute to health problems beyond the mouth. When a cavity progresses to infection, mouth bacteria and inflammation may enter the bloodstream. This is linked to higher cardiovascular risk, and in rare cases can trigger a serious heart infection (endocarditis) in vulnerable patients. Prompt dental treatment and good daily hygiene help lower these risks.
How Tooth Decay Can Affect the Rest of Your Body
A cavity starts when bacteria in dental plaque break down enamel. If decay continues, it can reach the dentin and pulp, where nerves and blood vessels sit. At that stage, the tooth may become infected or develop an abscess.
Infection and gum inflammation make it easier for bacteria to enter the bloodstream. This can happen during everyday activities such as chewing or brushing, especially if the gums bleed easily.
What the Research Suggests About the Heart Connection

Table of Contents
Studies consistently show a link between poor oral health—especially gum disease—and cardiovascular disease. Researchers believe inflammation and short bursts of bacteria in the blood (bacteremia) may play a role. That said, a link does not prove that cavities directly cause heart disease.
Tooth decay matters because it can increase inflammation and, when it turns into a deep infection, it may raise the chance of bacteria reaching the bloodstream. For most healthy people, this is unlikely to cause a heart problem, but it becomes more important if you already have certain heart conditions.
Potential Heart-Related Risks Associated With Dental Infections
Systemic Inflammation
Ongoing gum inflammation or untreated dental infection can contribute to higher inflammatory markers in the body. Inflammation is a known factor in cardiovascular disease, so keeping oral inflammation under control is a sensible prevention step.
Infective Endocarditis in High-Risk Patients
Infective endocarditis is a rare but serious infection of the heart’s inner lining or valves. It can occur when bacteria from the mouth enter the bloodstream and attach to damaged heart tissue or artificial valves. People with specific cardiac conditions may need special precautions before certain dental procedures.
Worsening of Existing Cardiovascular Risk Factors
Oral health problems often cluster with other risk factors such as smoking, diabetes, and limited access to preventive care. Treating decay and gum disease won’t replace medical care for heart disease, but it supports overall health and can reduce one avoidable source of inflammation.
Signs a Cavity or Tooth Infection Needs Urgent Care
Contact a dentist promptly if you notice any of the following:
- Toothache that lasts more than a day or worsens
- Swelling of the gums, face, or jaw
- Pus, a bad taste, or persistent bad breath
- Fever, fatigue, or feeling unwell alongside dental pain
- Pain when biting or difficulty chewing
Who Is at Higher Risk of Heart Complications?
Extra caution is recommended if you have:
- A prosthetic heart valve or a history of infective endocarditis
- Certain congenital heart conditions (your cardiologist can confirm)
- A weakened immune system (for example, from medication or illness)
- Diabetes that is difficult to control
- Moderate to severe gum disease
How to Protect Your Teeth and Support Heart Health
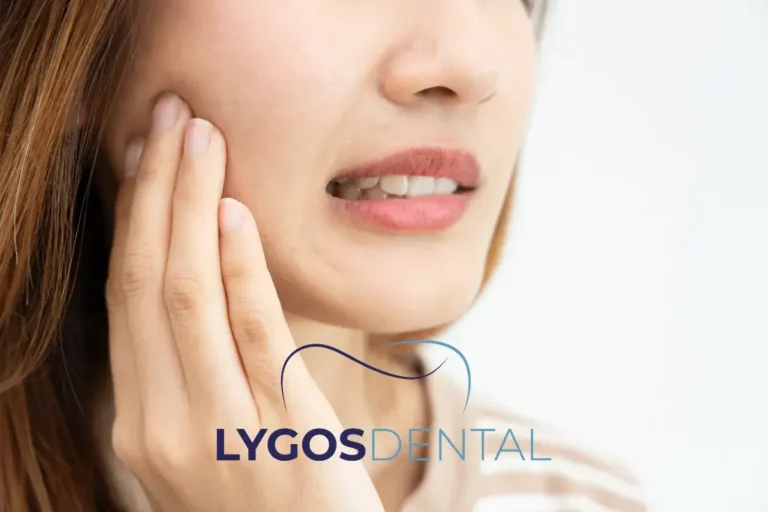
Treat Cavities Early
A filling or crown can stop decay from progressing and reduce the chance of infection. If you have swelling or severe pain, you may need urgent treatment for an abscess.
Keep Daily Oral Care Simple and Consistent
Brush twice a day with fluoride toothpaste, clean between your teeth daily (floss or interdental brushes), and consider an antiseptic mouthwash if your dentist recommends it.
Get Regular Dental Check-Ups
Routine visits help catch early decay, gum inflammation, and bite issues before they turn into infections. If you have a heart condition, tell your dentist and bring your current medication list.
Support a Low-Inflammation Lifestyle
A balanced diet, less added sugar, not smoking, and managing conditions like diabetes protect both oral health and the cardiovascular system.
When to See a Dentist
Book an appointment if you suspect a cavity, have sensitivity that persists, or notice gum bleeding. If you have a high-risk heart condition and need dental work, ask your cardiologist and dentist whether antibiotic precautions are appropriate for you.
At Lygos Dental, we provide modern diagnostic tests, comfortable treatment options, and personalized care plans to help protect your oral health.
Key Takeaway
Tooth decay doesn’t automatically lead to heart disease, but untreated cavities can progress to infection and add to inflammation in the body. Good oral hygiene, timely dental treatment, and coordination with your cardiologist (when needed) are practical steps to reduce avoidable risks.
Get Information Now
You can contact us to learn more about Cosmetic Dentistry, Dental Crown, Dental Implant, and General Dentistry, to make an appointment, or to ask questions about our services.
Frequently Asked Questions
Can a tooth decay be fixed?
Yes, early decay can remineralize; cavities require fillings or crowns.
What is the main cause of tooth decay?
Bacterial acids from sugar breakdown erode enamel and dentin.
What are the 5 stages of tooth decay?
Demineralization, enamel decay, dentin decay, pulp infection, and abscess formation.
When is it too late to stop tooth decay?
It’s too late once decay reaches pulp causing irreversible infection or collapse.
Is tooth decay your fault?
No, decay isn’t solely your fault; biology, diet, habits, and access contribute.
How painful is tooth decay?
Pain ranges from none early to severe, throbbing pain in advanced decay
Gum Problems in the Elderly
Gum Problems in the Elderly
Gum problems are common in older adults and can progress from mild gum inflammation to advanced periodontitis and tooth loss. Watch for bleeding, swelling, bad breath, receding gums, and loose teeth. With timely dental care, good daily cleaning, and management of dry mouth and chronic conditions, most cases can be controlled.
As we age, gum tissue can become more vulnerable to inflammation and infection. Changes in dexterity, medications that cause dry mouth, and long-term health conditions can make gum disease easier to develop and harder to notice early.
The good news is that most gum problems respond well to early treatment and consistent home care. The sections below cover symptoms to watch for, common risk factors, treatment options, and practical tips for seniors and caregivers.
Symptoms Of Gum Problems In The Elderly
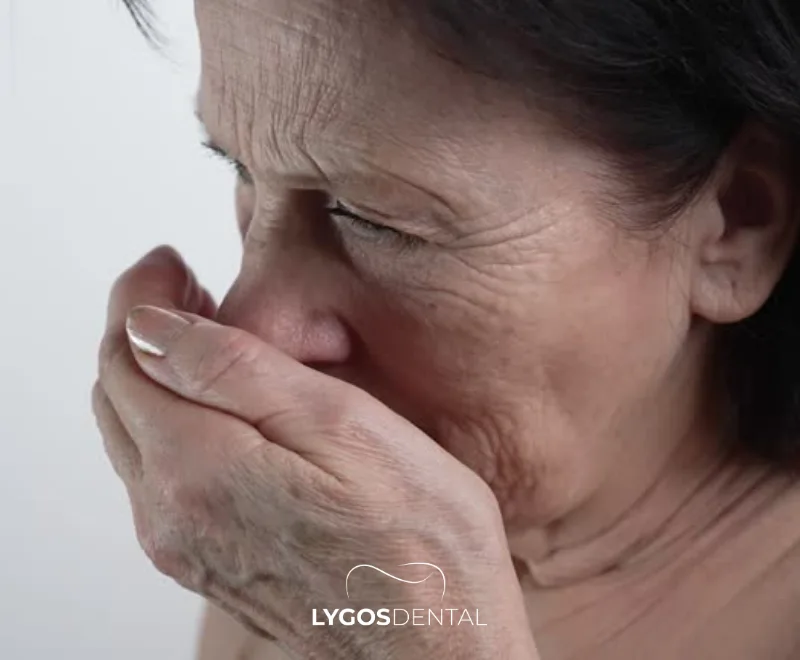
Table of Contents
Gum disease often starts quietly. If symptoms are missed, it can progress and increase the risk of tooth loosening or tooth loss.
- Red, swollen, or tender gums
- Bleeding during brushing or flossing
- Persistent bad breath or a bad taste
- Gums pulling away from the teeth (gum recession)
- Sensitive teeth or exposed roots
- Teeth that feel loose or a bite that feels different
If you notice these changes, schedule a dental visit. Earlier care usually means simpler treatment and better comfort.
Risk Factors For Gum Problems In The Elderly
Several factors can increase the likelihood of gum disease in older adults. Knowing what applies to you helps you prevent flare-ups and catch issues sooner.
- Age-related tissue changes: gums may thin and attachments can weaken over time
- Oral hygiene challenges: arthritis, tremor, or reduced mobility can make brushing and flossing harder
- Smoking or tobacco use: reduces blood flow to the gums and slows healing
- Diabetes and other chronic conditions: can raise inflammation and affect infection control
- Dry mouth (often medication-related): less saliva makes plaque build up faster
- Nutritional gaps: low intake of key nutrients can affect gum resilience and healing
Common Types Of Gum Disease In Older Adults
Treatment options vary depending on the stage of the disease and the patient’s general condition. Key treatment methods include:
- Professional dental cleaning (prophylaxis): To remove plaque and tartar buildup.
- Deep cleaning (scaling and root planing): To remove inflamed tissues below the gumline.
- Antibiotic therapy: Short-term antibiotic use may be required to control infections.
- Surgical interventions: In advanced cases involving gum recession or bone loss.
- Regular follow-up: Ongoing dental check-ups are critical after treatment.
These interventions are crucial for halting the progression of gum disease and maintaining oral health in the elderly.
Dental Implants in the Elderly
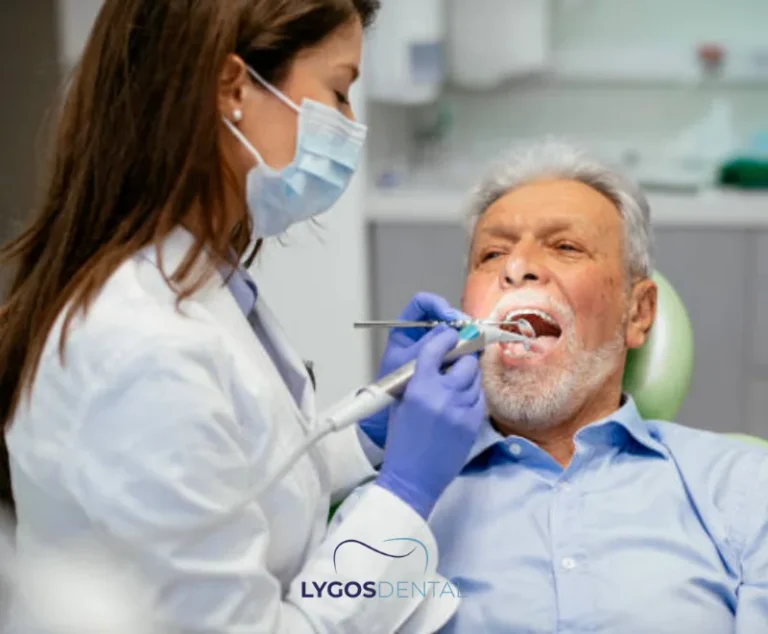
Since tooth loss is common in older age, dental implants have become a popular replacement option. However, gum health must be stabilized before implant placement. Infected gums can prevent successful integration of implants and lead to treatment failure. Therefore:
- Gum disease should be treated first
- Proper oral hygiene must be ensured
- Bone structure suitability must be assessed
When properly planned, implant treatment can provide both aesthetic and functional benefits for seniors.
At-Home Gum Care for the Elderly
The two most common gum conditions are gingivitis and periodontitis. Both start with plaque (bacterial buildup), but they affect different levels of the supporting tissues.
Gingivitis
Gingivitis is inflammation of the gums. It often causes redness and bleeding, but it has not yet damaged the bone that supports the teeth. With thorough cleaning and improved daily care, gingivitis is usually reversible.
Periodontitis
Periodontitis develops when inflammation spreads deeper under the gumline. It can lead to gum recession, bone loss, and tooth mobility. Treatment can stop or slow progression, but lost bone and attachment do not fully grow back without advanced procedures.
How Gum Disease Can Affect Overall Health
Gum infections can contribute to ongoing inflammation in the body. Studies have found associations between periodontitis and conditions such as cardiovascular disease, diabetes control, and some respiratory infections. Treating gum disease is one practical step toward better overall health, especially for people with chronic illnesses.
Treatment Options For Gum Problems In The Elderly
Treatment depends on severity, overall health, and the ability to keep the mouth clean during healing. A dentist or periodontist will usually start with the least invasive option and reassess after healing.
- Professional cleaning: removes plaque and tartar above the gumline
- Scaling and root planing (deep cleaning): clears deposits below the gumline and smooths root surfaces
- Targeted medications: antimicrobial rinses or short-term antibiotics when infection control is needed
- Gum or bone procedures: considered for advanced recession, deep pockets, or significant bone loss
- Maintenance visits: regular check-ups help prevent relapse after treatment
When To Contact A Dentist Quickly
Seek prompt dental advice if there is facial swelling, pus, fever, severe pain, sudden tooth mobility, or bleeding that does not stop. These can be signs of an abscess or a fast-moving infection.
Dental Implants In The Elderly

Dental implants can be a reliable option for replacing missing teeth in seniors, but the gums and supporting bone must be healthy enough for predictable healing. Active gum infection raises the risk of implant complications.
- Treat gum disease first and confirm stability
- Review medications and medical conditions that may affect healing
- Assess bone volume and quality with dental imaging
- Plan maintenance care to prevent inflammation around implants (peri-implant disease)
At-Home Gum Care Tips For Older Adults
Daily habits make the biggest long-term difference. If brushing and flossing are difficult, small tool changes often help more than trying harder with the same routine.
- Brush twice a day with a soft-bristled toothbrush; an electric brush can make technique easier
- Clean between teeth daily using floss, floss holders, or interdental brushes (choose what you can use consistently)
- Use fluoride toothpaste and ask your dentist whether an antimicrobial rinse is appropriate
- Stay hydrated and manage dry mouth; discuss saliva substitutes or medication adjustments with your clinician when needed
- Choose a balanced diet with adequate protein, fruits, and vegetables; limit frequent sugary snacks
- Avoid tobacco and reduce alcohol, since both can irritate tissues and slow healing
- Keep regular dental visits for early detection and maintenance
Tips For Caregivers
For seniors who need help, try brushing at the same time each day, use a small-headed soft brush, and keep lighting bright. If there are dentures, clean them daily and remove them at night unless the dentist advises otherwise.
Gum Problems In The Elderly FAQ
When is it too late to reverse gum disease?
It’s too late once periodontitis causes irreversible attachment or bone loss.
What is the best home remedy for gum disease?
Brushing twice daily and cleaning between teeth is the best home care for gum disease.
Can you repair receding gums?
Yes—receding gums can be repaired with periodontal treatment and gum graft surgery.
What toothpaste is good for receding gums?
A stannous-fluoride toothpaste helps reduce gingivitis and protect exposed roots.
Can I live a long life with gum disease?
Yes—with treatment and maintenance, gum disease can be controlled long-term.
How long do you have gum disease before teeth fall out?
Untreated periodontitis can lead to tooth loss over years to decades.
What is Anodontia
Anodontia: Causes, Symptoms, Diagnosis, And Treatment
Anodontia is a rare condition where a person is born without some or all teeth because tooth development never occurs. It is usually linked to genetics and may appear alone or with syndromes like ectodermal dysplasia. Dentists confirm it with an exam and dental X-rays, then plan treatment such as dentures, implants, or orthodontics.
Missing teeth can affect appearance, speech, and how well you chew. While many cases are caused by injury or decay, some people are born without certain teeth—or, more rarely, without any teeth at all.
When patients ask, “What is anodontia?”, the simplest answer is that it’s a congenital tooth-development disorder. With early diagnosis and a tailored plan, most functional and aesthetic concerns can be managed effectively.
What Is Anodontia?
Anodontia is the congenital absence of teeth due to disrupted tooth development during early growth. It can involve primary teeth, permanent teeth, or both. The condition ranges from missing a small number of teeth to the complete absence of all teeth.
Types Of Anodontia
Clinicians often group congenital tooth absence by how many teeth are missing. These categories help dentists plan timing, prosthetics, and long-term follow-up.
Complete Anodontia
- No teeth develop in the upper and lower jaws. This is extremely rare and often associated with genetic syndromes.
Partial Anodontia (Hypodontia)
- One or more teeth fail to develop. This is the most common pattern of congenital tooth absence.
Oligodontia
- Six or more teeth are missing (excluding wisdom teeth in many clinical definitions). It may occur on its own or with other congenital findings.
Symptoms Of Anodontia
Symptoms vary by severity and the age at which missing teeth become noticeable. Common signs include:
- Delayed eruption of baby teeth or permanent teeth.
- Visible gaps where teeth are expected to appear.
- Chewing difficulty and changes in diet choices.
- Speech differences, especially with missing front teeth.
- Changes in jaw growth or facial profile in more severe cases.
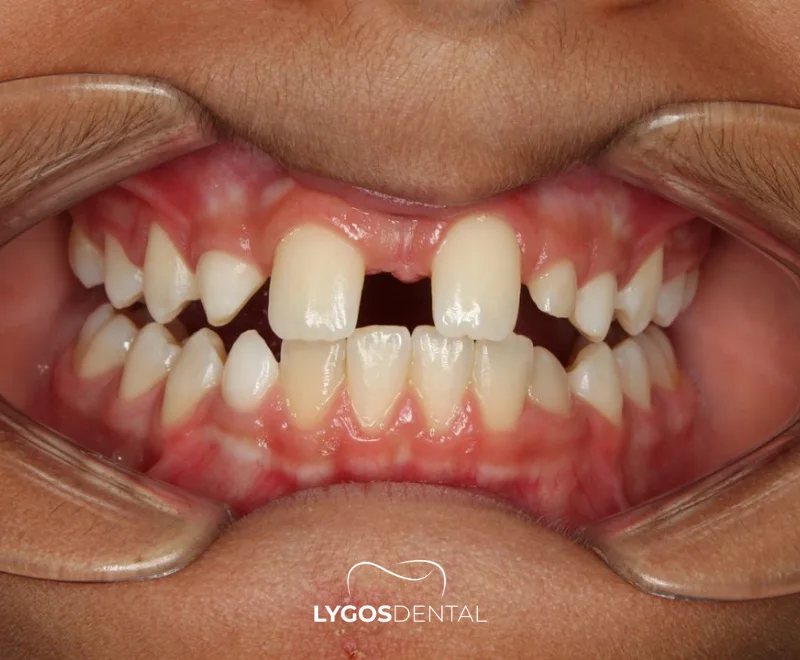
Table of Contents
Causes And Risk Factors
Anodontia is most often genetic. It can run in families or occur as part of a broader syndrome that affects ectodermal structures (such as hair, skin, sweat glands, and nails).
Potential contributors include:
- Genetic variants linked to tooth development (for example, EDA, WNT10A, PAX9, and MSX1).
- Syndromes such as ectodermal dysplasia.
- Less commonly, exposures during pregnancy that disrupt fetal development (for example, certain medications, radiation, or severe infections).
How Is Anodontia Diagnosed?
Diagnosis usually begins when tooth eruption is delayed or when teeth appear to be missing. A dentist confirms whether teeth are absent or simply unerupted using clinical and imaging findings.
- Dental examination to assess gums, spacing, bite, and jaw growth.
- Radiographic imaging (often a panoramic X-ray; sometimes CT/CBCT when detailed planning is needed).
- Genetic evaluation when a syndrome is suspected or there is a strong family history.

Treatment Methods For Anodontia
Treatment is individualized and depends on age, the number of missing teeth, jaw development, and overall oral health. Care is often coordinated between pediatric dentistry, orthodontics, prosthodontics, and sometimes medical genetics.
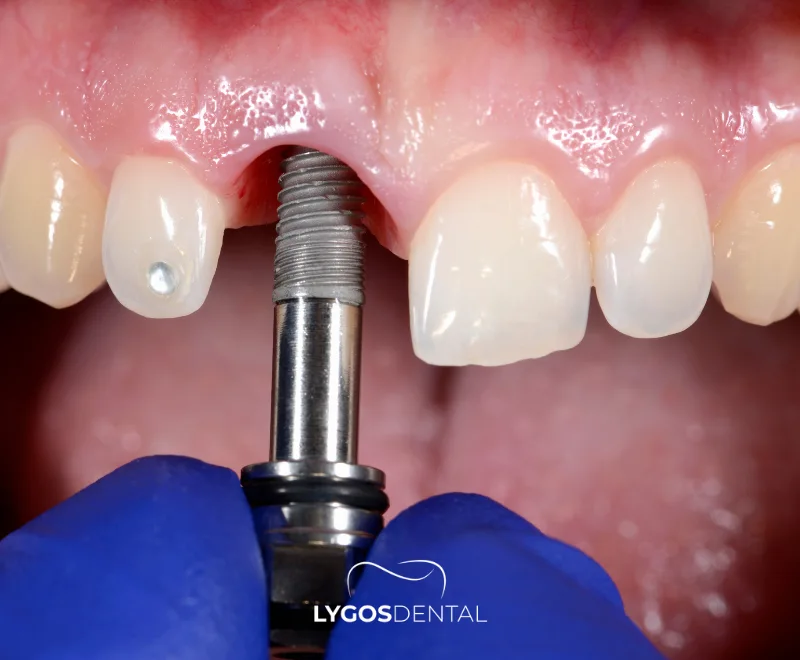
- Prosthetic treatment: removable partial dentures, complete dentures, or overdentures to restore function and appearance.
- Implant treatment: dental implants may be an option once jaw growth is appropriate and bone volume is sufficient.
- Orthodontic treatment: space management, bite correction, and support for prosthetic planning.
- Follow-up and adjustments: relines, remakes, or repairs may be needed over time—especially in growing patients.
- Genetic counseling: helpful for families when an inherited pattern is likely.
Anodontia FAQ
When is it too late to reverse gum disease?
It’s too late once periodontitis causes irreversible attachment or bone loss.
What is the best home remedy for gum disease?
Brushing twice daily and cleaning between teeth is the best home care for gum disease.
Can you repair receding gums?
Yes—receding gums can be repaired with periodontal treatment and gum graft surgery.
What toothpaste is good for receding gums?
A stannous-fluoride toothpaste helps reduce gingivitis and protect exposed roots.
Can I live a long life with gum disease?
Yes—with treatment and maintenance, gum disease can be controlled long-term.
How long do you have gum disease before teeth fall out?
Untreated periodontitis can lead to tooth loss over years to decades.
Gappy Teeth
Gappy Teeth: Causes, Treatment & Prevention
Gappy teeth (diastema) are visible spaces between two teeth, most often the upper front teeth. They’re commonly caused by genetics, tooth-size/jaw-size mismatch, missing teeth, gum disease, or habits like tongue thrusting. Treatment ranges from orthodontics and bonding to veneers, crowns, or replacing missing teeth. Good hygiene and early dental advice help prevent gaps related to gum disease and shifting.
What Are Gappy Teeth (Diastema)?
Gappy teeth—clinically called diastema—describe a space between two teeth. The most recognizable gap sits between the two upper front teeth, but spacing can occur anywhere along the arch.
Diastema is common during childhood and often narrows as permanent teeth come in. In adults, a gap may remain stable for years or gradually widen if the underlying cause isn’t addressed.
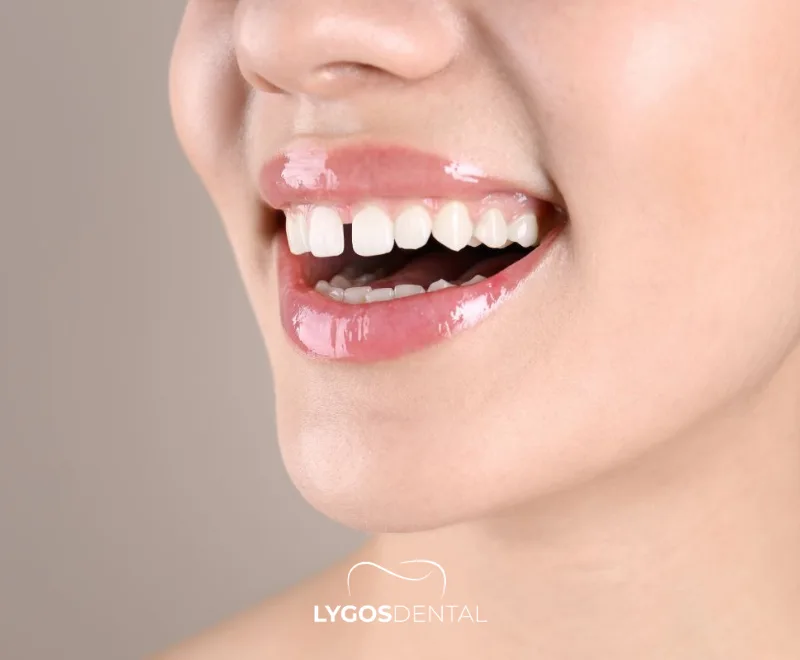
Table of Contents
Common Causes Of Gappy Teeth
More than one factor can contribute to spacing. A dentist or orthodontist will look for the primary cause before recommending treatment.
- Genetics and tooth–jaw size mismatch: Teeth that are relatively small for the jaw can leave extra space.
- Missing or undersized teeth: A missing tooth (or a “peg” lateral incisor) can let neighboring teeth drift.
- Large labial frenum: The band of tissue connecting the upper lip to the gum can sit low or thick and keep the front teeth apart.
- Gum disease (periodontal disease): Bone loss around teeth can make them loosen and shift, creating or worsening gaps.
- Childhood habits: Thumb sucking, prolonged pacifier use, or tongue thrusting can push teeth forward and apart over time.
- Tooth movement over time: Teeth can shift with age, after tooth loss, or if retainers aren’t worn after orthodontic treatment.
Possible Oral Health Issues Linked To Tooth Gaps
A diastema is often harmless, but the space can make plaque control trickier—especially if the gap sits next to inflamed or receding gums.
If spacing is caused by gum disease or missing teeth, treating the underlying condition matters more than the gap itself. In some cases, gaps also accompany bite problems that can contribute to uneven wear or jaw discomfort.
Speech changes are possible, particularly with larger gaps at the front, although not everyone is affected.
Treatment Options For Gappy Teeth
The right approach depends on the cause, the size of the space, and your bite. Your clinician may combine treatments to get a stable result.
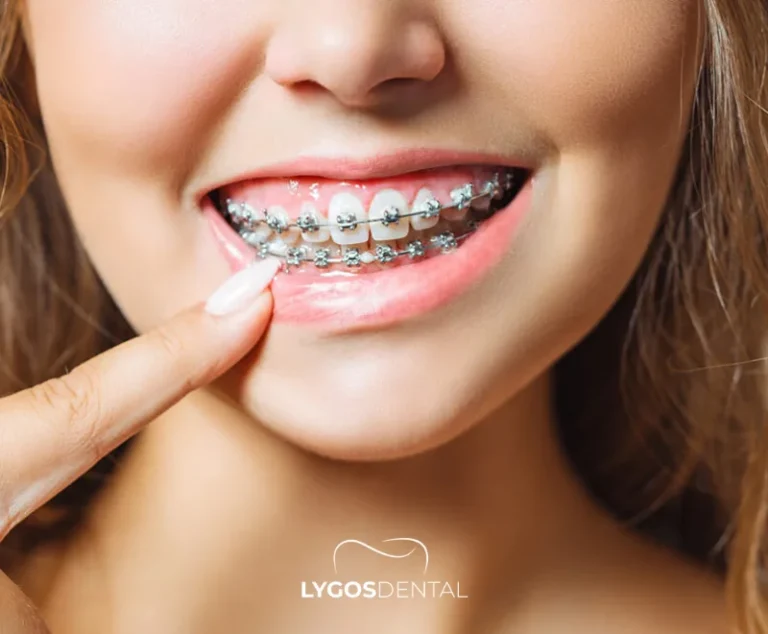
Orthodontics: Braces Or Clear Aligners
Orthodontic treatment gently moves teeth into position and is often the best choice when there are multiple gaps or broader alignment issues. Retention (wearing a retainer) is essential to reduce the risk of the gap reopening.
Composite Bonding
For small gaps, bonding can close spaces quickly by adding tooth-colored resin to the sides of the teeth. It’s conservative and typically completed in one visit, though it may stain or chip over time and can require maintenance.
Veneers
Porcelain or composite veneers can reshape the visible surface of the teeth to disguise a gap and improve symmetry. Veneers are mainly a cosmetic solution and usually require some enamel preparation.
Crowns
Crowns may be recommended when a tooth is heavily filled, weak, or needs a larger shape change than bonding or veneers can provide. They cover the entire tooth, so the preparation is more extensive.
Frenectomy
If a thick or low labial frenum is keeping the front teeth apart, a minor procedure called a frenectomy may be advised. It’s often paired with orthodontics or restorative work to close the space and help it stay closed.
Replacing Missing Teeth: Implants Or Bridges
When spacing is driven by a missing tooth, replacing it can prevent further drifting and restore function. Your dentist may suggest an implant, a fixed bridge, or another appropriate option based on bone, bite, and overall health.

At-Home Approaches: What Helps And What To Avoid
Be cautious with online “quick fixes.” Any method that moves teeth should be supervised by a dental professional.
Myofunctional therapy (tongue and swallowing training) can be helpful when tongue thrusting is part of the problem, but it usually complements orthodontic care rather than replacing it.
Daily brushing, flossing (or interdental brushes), and regular cleanings support gum health, which can reduce the risk of spacing that worsens due to inflammation or bone loss.
Avoid:
- DIY elastic bands or “gap bands”: These can slip under the gums, damage the supporting tissues, and may lead to serious gum and bone loss.
- Attempting to file teeth at home to “make room” for bonding or alignment: This can permanently damage enamel.
- Relying on oil pulling or supplements to close a gap: These may support general oral hygiene habits, but they do not move teeth.
How To Help Prevent Gaps From Developing Or Worsening
Not all diastemas are preventable, especially those driven by genetics. These steps can lower the risk of gaps related to disease and shifting:
- Keep gums healthy: Brush twice daily, clean between teeth, and get regular dental check-ups and professional cleanings.
- Treat gum disease early: Bleeding gums, persistent bad breath, and gum recession should be checked promptly.
- Replace missing teeth in a timely way to reduce drifting and bite changes.
- Manage childhood habits: Address thumb sucking, extended pacifier use, and tongue thrusting early with professional guidance.
- Wear retainers as prescribed after orthodontic treatment.
When To See A Dentist Or Orthodontist
Book an assessment if a gap is getting larger, if you notice gum bleeding or looseness, or if food traps are becoming a daily issue.
You should also get advice before choosing a cosmetic fix. Closing a gap without checking the bite can create problems elsewhere, such as chipping, uneven wear, or gum irritation.
Gappy Teeth FAQ
How to stop gaps from forming in teeth?
Prevent gaps by maintaining gum health, treating bite issues, and wearing retainers after orthodontics.
What causes gappy teeth?
Gappy teeth result from genetics, tooth-size/jaw mismatch, gum disease, missing teeth, habits.
Can gappy teeth be fixed?
Yes, gaps can be closed with orthodontics, bonding, veneers, crowns, or implants.
Do gaps in teeth cause problems?
Sometimes gaps trap food, affect speech, shift teeth, and worsen bite.
What is the best teeth gap treatment?
Best treatment is orthodontic alignment for larger gaps; bonding or veneers for small gaps.
How to reduce gaps in teeth naturally?
You cannot naturally close most gaps; stop habits and treat gum disease promptly.
What is Amalgam Filling?
Amalgam Filling: Is It Safe and When Is It Used?
An amalgam filling is a long-lasting “silver” dental filling used mainly for back teeth. It’s made from a blend of metals, including mercury that binds the alloy into a strong material. Most health authorities consider amalgam safe for the general population, while some higher‑risk groups may be advised to choose alternatives.
What Is an Amalgam Filling?
Dental amalgam is a restorative material used to repair a tooth after decay has been removed. Because it resists wear and pressure, it is commonly used for molars and premolars where chewing forces are highest. The dentist shapes the material inside the prepared cavity and it hardens into a solid filling.
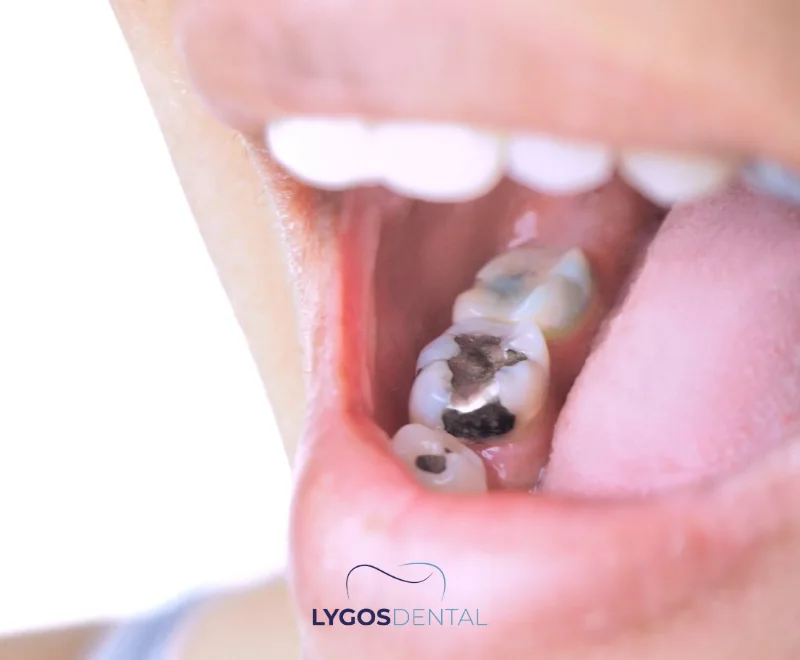
Table of Contents
What Is Amalgam Made Of?
Amalgam is a metal alloy made by mixing liquid mercury with a powdered alloy of other metals. Typical ingredients include silver, tin, and copper, along with mercury to bind the mix. Once placed, the material sets and becomes firm, which is one reason it has a long clinical track record.
Why Dentists Still Use Amalgam
Amalgam remains a practical option in certain situations. It tolerates moisture better than some tooth‑colored materials during placement and can be faster to place in difficult-to-isolate cavities. In large cavities on back teeth, it can offer dependable longevity at a lower cost than many alternatives.
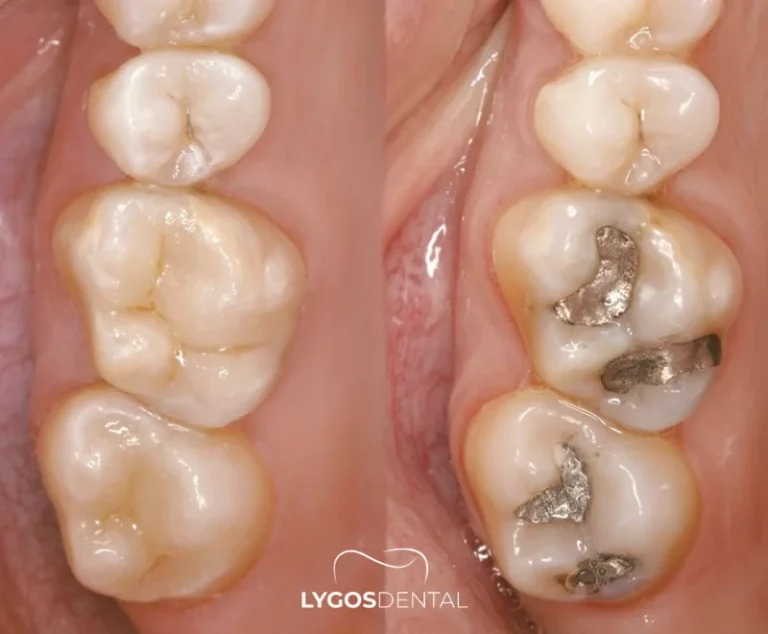
Safety and Mercury Concerns
The main debate around amalgam relates to mercury, which is part of the material. In a set filling, mercury is bound within the restoration, but small amounts of mercury vapor can be released, especially when the filling is placed or removed. Most patients do not experience health problems from amalgam, yet medical guidance can differ for certain groups.
What major health bodies say
Major dental and public health organizations generally state that dental amalgam is a safe and effective filling material for the general population. Some authorities also note that people with allergies to any amalgam components should avoid it. Guidance often emphasizes that removing an intact, well-functioning filling only to “get rid of mercury” is usually not recommended.
Who may be advised to consider alternatives
Some higher‑risk groups may be advised to use non‑amalgam materials whenever suitable. This may include people with known mercury or metal allergies and certain patients with specific health conditions, based on clinical judgment. Pregnant or nursing patients and children may also be offered alternatives depending on local guidance and availability.
Should you remove old amalgam fillings?
If an amalgam filling is intact, not leaking, and there is no decay underneath it, replacement is rarely urgent. Removing a filling can temporarily increase exposure to mercury vapor and may require taking away additional healthy tooth structure. Replacement is typically considered when the filling is cracked, worn, recurrent decay is present, or for a clear medical reason discussed with your dentist.

Amalgam vs Other Filling Types
Choosing a filling material is a balance between strength, appearance, tooth location, and budget. Amalgam is usually stronger than many tooth‑colored options in high‑load areas, but it is also more visible. Your dentist will weigh factors like cavity size, bite forces, and your aesthetic preferences.
- Composite (tooth‑colored): blends with natural teeth and is popular for visible areas, but can be more technique‑sensitive and may wear faster in large back‑tooth cavities.
- Ceramic/inlay restorations: offer excellent aesthetics and stain resistance, but they typically cost more and often require lab work.
- Glass ionomer: can release fluoride and is useful in specific cases, yet it is generally less durable under heavy chewing forces.
Advantages and Disadvantages
Advantages
- Durability: often performs well for years on back teeth under heavy chewing forces.
- Cost: tends to be more affordable than many tooth‑colored or lab-made restorations.
- Placement: can be less sensitive to minor moisture during placement in some clinical situations.
Disadvantages
- Appearance: the silver color is noticeable, so it’s rarely chosen for front teeth.
- Tooth preparation: it may require removing a little more tooth structure to create mechanical retention.
- Mercury concerns: while considered safe for most people, it may not be the best first choice for some higher‑risk patients.
What to Do After Getting an Amalgam Filling
Follow your dentist’s instructions for the first day after treatment. Avoid very hard foods on the treated side until the filling has fully set and your bite feels normal. If you notice a high spot, sharp edge, or pain when chewing, schedule a quick adjustment.
- Brush and floss normally, but be gentle around the area if your gums are sore.
- Avoid chewing ice or very hard foods that could crack any filling material.
- Tell your dentist if you grind your teeth; a night guard may protect restorations.
Cost of Amalgam Fillings
Pricing varies by country, clinic, and the size of the cavity (single‑surface, two‑surface, or three‑surface restorations). Extra needs—such as X‑rays, anesthesia, or treating deeper decay—can also change the total cost. Ask for a written estimate that lists the procedure, material, and any follow‑up visits.
Example: 2026 fee tariff in Turkey
In Türkiye, many clinics reference the Turkish Dental Association’s annual fee tariff as a baseline, though actual clinic fees may differ. In the 2026 tariff, VAT‑included fees for amalgam fillings are listed by surface: one‑surface 2,845 TL, two‑surface 3,805 TL, and three‑surface 4,845 TL. Your dentist can confirm which category your cavity fits and whether additional procedures are needed.
Amalgam Fillings FAQ
Is it safe to use amalgam fillings?
Yes, amalgam is safe for most patients; high-risk groups may need alternatives.
Why did dentists stop using amalgam fillings?
Dentists reduced use due to mercury regulations, aesthetics, and improved tooth-colored composite alternatives.
Is it worth getting amalgam fillings removed?
No, removing intact amalgam isn’t recommended unless failing, leaking, or mercury allergy is diagnosed.
At what age can amalgam be used?
Age 15+: amalgam is allowed; under 15 only when strictly necessary.
Are NHS dentists still using amalgam?
Yes, NHS dentists may still place amalgam fillings when clinically justified and permitted.
How To Clean Teeth
How To Clean Teeth
Clean teeth by brushing twice daily for two minutes with a soft brush, cleaning between teeth with floss or interdental brushes, and removing bacteria from the tongue. Use fluoride toothpaste, limit frequent sugary snacks, and see a dentist for regular professional cleanings to remove tartar you can’t brush away.
Why Teeth Cleaning Matters
Teeth cleaning protects more than your smile. Daily plaque control lowers the risk of cavities, gum inflammation, and persistent bad breath. Healthy gums also matter for general health, since untreated gum disease can contribute to wider health problems.
-
- Helps prevent cavities by reducing plaque and food debris.
- Lowers the risk of gingivitis and more advanced gum disease.
- Supports fresher breath by reducing odor-causing bacteria.
- Keeps teeth stronger for chewing and comfortable eating.
- Helps keep natural tooth color brighter by limiting surface stains.
Table of Contents
How To Clean Teeth At Home
A consistent routine beats intense, occasional cleaning. Focus on technique, timing, and the areas people miss most.
Brush Twice A Day With The Right Technique
Brush in the morning and before bed for about two minutes each time. Angle the bristles toward the gumline and use small, gentle circles. Cover the outer, inner, and chewing surfaces of every tooth. Heavy pressure can irritate gums and wear enamel over time.
- Use a soft-bristled manual brush or an electric toothbrush with a gentle mode.
- Replace the brush head every 3 months, or sooner if bristles splay.
- Spit out excess toothpaste after brushing; avoid rinsing heavily right away to keep fluoride on the teeth.
Clean Between Teeth Every Day
A toothbrush can’t reach tight contacts between teeth. Floss or interdental brushes remove plaque where cavities and gum problems often start. If your gums bleed at first, keep going gently; bleeding usually improves as the area becomes healthier. If bleeding persists, book a dental check.
- Floss once a day, sliding it gently under the gumline on each side of the tooth.
- Use interdental brushes if spaces are wider or if you have bridges or orthodontic wires.
- For sensitive gums, try floss picks or water flossers as a support, not a full replacement.
Don’t Skip The Tongue
A coated tongue holds bacteria that can cause bad breath and affect taste. Use a tongue scraper or brush the tongue lightly from back to front. Do this once a day, especially before bed.
Use Mouthwash The Right Way
Mouthwash can help with breath and bacterial control, but it doesn’t replace brushing and flossing. Choose an alcohol-free option if you get dryness or sensitivity. If you use a fluoride mouthwash, try it at a different time from brushing so you don’t wash away toothpaste fluoride.
Diet Habits That Keep Teeth Cleaner
What you snack on—and how often—matters. Sugary or acidic foods feed plaque bacteria and soften enamel. Water is your best everyday drink for the mouth, and crunchy fruits and vegetables can help gently clean tooth surfaces between meals.
- Limit frequent sipping on sweet drinks, including fruit juice and sweetened coffee.
- Keep sugary snacks to mealtimes when possible.
- Rinse with water after acidic foods or drinks, then wait about 30 minutes before brushing.
Professional Teeth Cleaning
Even with a solid routine, tartar can build up in places you can’t reach. Professional cleaning removes hardened deposits and gives your dentist a chance to spot early gum or tooth problems.
What Happens During A Dental Cleaning
- Tartar removal (scaling) using hand instruments or ultrasonic tools.
- Polishing to smooth tooth surfaces and reduce surface stains.
- Targeted gum assessment, including checks for inflammation and pockets.
- Optional fluoride application when it suits your risk level and sensitivity.
How To Clean Teeth For Babies And Children
Early habits make a big difference. Start cleaning as soon as the first tooth appears, and build routines that fit your child’s age and coordination.
Age-Based Tips
0–12 months: Wipe gums and new teeth gently with a clean, damp gauze or soft cloth after feeds.
1–3 years: Use a small, soft brush. A smear of fluoride toothpaste is usually enough.
4–6 years: Use a pea-sized amount of toothpaste. Supervise brushing and help with hard-to-reach areas.
7+ years: Keep supervision as needed and introduce daily flossing when teeth touch.
Limit frequent sugary snacks and drinks, and keep routine dental visits so kids learn that checkups are normal.
Best Products For Teeth Cleaning
The “best” product is the one you can use correctly every day. Choose tools that match your mouth, your dexterity, and any dental work you have.
Toothbrush: Soft bristles are safest for most people. Electric brushes can make timing and coverage easier.
Toothpaste: Fluoride toothpaste helps strengthen enamel and reduce cavity risk. For sensitivity, look for desensitizing formulas.
Interdental cleaning: Floss for tight spaces; interdental brushes for wider gaps; water flossers can be useful for braces and implants.
Mouthwash: Antibacterial or fluoride mouthwash can help, depending on your needs. Alcohol-free options suit dry mouths.
Tongue cleaner: A scraper is simple and effective for reducing tongue coating and odor.
Common Mistakes To Avoid
- Brushing too hard or using a hard-bristled brush.
- Rushing the routine and missing back teeth and gumlines.
- Skipping flossing because gums bleed (bleeding can be a sign you need it).
- Brushing immediately after acidic drinks instead of waiting a bit.
- Using mouthwash as a substitute for brushing and flossing.
When To See A Dentist
Book a visit if you notice bleeding that doesn’t improve, persistent bad breath, tooth sensitivity, pain when chewing, or loose teeth. These can be early signs of decay, gum disease, or bite problems that need treatment. Professional advice also helps if you have crowns, implants, orthodontics, or a history of gum issues.
Frequently Asked Questions
What is the correct way to clean your teeth?
Brush twice daily 2 minutes with fluoride toothpaste, soft brush, and floss daily.
How can I remove dirty from my teeth?
Brush and floss; schedule a dental cleaning to remove plaque and tartar safely.
How do you clean yellow teeth?
Professional cleaning and whitening work best; brush with fluoride and limit staining foods.
What naturally cleans teeth?
Fluoride toothpaste and saliva naturally clean teeth; chew sugar-free gum after meals.
What drink cleans teeth?
Plain water helps rinse teeth; unsweetened tea offers mild stain-fighting polyphenols.
How can I clean my teeth at home?
Brush twice daily, floss nightly, use fluoride toothpaste, and rinse after sugary foods.
What is Tooth Enamel?
What Is Tooth Enamel? Protection And Care
Tooth enamel is the thin, hard outer coating on your teeth. It shields the softer dentin and nerves from acid, temperature changes, and daily chewing. Enamel can’t regrow once it’s lost, so preventing erosion with fluoride, gentle brushing, and a lower-acid diet is the best way to keep teeth strong.
What Is Tooth Enamel?
Tooth enamel is the hard, protective layer that covers the crown (the visible part) of each tooth. It’s the hardest tissue in the human body, yet it can still wear down or erode over time.
Enamel is made mostly of minerals, mainly a calcium‑phosphate crystal called hydroxyapatite. Because enamel is slightly translucent, the color of the dentin underneath can influence how white or yellow a tooth looks.

Table of Contents
What Does Tooth Enamel Do?
Enamel works like a shield. When it’s intact, it protects teeth during everyday eating and drinking and helps you avoid sensitivity and decay.
- Guards the inner tooth from acids produced by bacteria and from acidic foods and drinks
- Protects against temperature sensitivity (hot, cold, and sweet triggers)
- Supports chewing by reducing mechanical wear
- Helps teeth look brighter by covering the naturally yellow dentin layer
Signs Of Tooth Enamel Loss
Enamel loss often happens gradually, so early clues matter. Common signs include:
- New or increased sensitivity to hot, cold, or sweet foods and drinks
- A rough, worn, or “dull” feeling on the tooth surface
- Teeth looking more yellow as dentin becomes more visible
- Small chips, cracks, or edges that seem thinner than before
- Changes in tooth shape, such as flattening on biting surfaces
If you notice these changes, a dental exam can help identify the cause and stop further damage.
How To Prevent Tooth Enamel Erosion
Daily Care Habits
- Brush twice a day with a soft‑bristled toothbrush and fluoride toothpaste.
- Use gentle pressure. Scrubbing hard can wear enamel and irritate gums.
- Floss daily to remove plaque between teeth where a brush can’t reach.
- After acidic foods or drinks, rinse with water and wait 30–60 minutes before brushing.
Diet And Drink Choices
- Limit frequent sipping of soft drinks, sports drinks, and fruit juices. Frequency matters as much as quantity.
- Drink acidic beverages through a straw to reduce contact with teeth.
- Balance acids with enamel‑friendly foods, especially calcium‑ and phosphate‑rich options (milk, yogurt, cheese, leafy greens, nuts).
- Choose water between meals to help neutralize acids and support saliva flow.
Habits That Can Damage Enamel
- Avoid chewing ice, hard candy, or other hard objects that can chip enamel.
- If you grind or clench your teeth, ask about a custom night guard to reduce wear.
- Use whitening products carefully. Overuse can increase sensitivity, especially if enamel is already thin.
Dental Visits And Preventive Treatments
- Schedule regular check‑ups so enamel wear is spotted early.
- Ask your dentist about fluoride varnish or other remineralization options if you’re at higher risk for erosion or cavities.
- If you have dry mouth, reflux, or frequent vomiting, treat the underlying cause—these can speed up enamel erosion.

Can Tooth Enamel Erosion Be Treated?
Enamel doesn’t grow back once it’s lost, but early erosion can often be stabilized and the tooth can be strengthened. Fluoride treatments and targeted remineralization can help protect vulnerable areas and reduce sensitivity.
If enamel loss is more advanced, a dentist may recommend treatments that cover or rebuild the tooth surface, such as bonding (fillings), veneers, or crowns. If grinding is contributing to wear, a night guard can protect your teeth while you sleep.
Tooth Enamel FAQ
What is enamel protection for teeth?
Enamel protection means preventing demineralization and promoting remineralization, mainly with fluoride and habits.
What is the best enamel protection?
Fluoride toothpaste and minimizing acidic exposure provide the best proven enamel protection.
When is it too late to repair enamel?
It’s too late when enamel is worn away; only early demineralization can remineralize.
How to protect and restore teeth enamel?
Use fluoride, limit acids/sugar, brush gently, and get dentist-applied remineralization treatments.
Can I restore enamel on my teeth?
You can remineralize weakened enamel, but you cannot regrow lost enamel.
Is enamel coating healthy?
Dental enamel coatings like sealants/varnish are safe and effective when professionally applied.
