What Causes Tooth Fractures?
What Causes Tooth Fractures?
Tooth fractures usually happen when a weakened tooth meets sudden force—such as a fall, biting something hard, or ongoing pressure from teeth grinding. Tooth decay, large fillings, and age-related enamel wear can also make teeth more likely to crack. Prompt dental care helps reduce pain, prevent infection, and limit further breakage.
Common Causes Of Tooth Fractures
A chipped or cracked tooth can happen in a second, but it’s usually linked to a few predictable triggers. Some causes are sudden, like an accident, while others build over time by weakening enamel or internal tooth structure.
Falls And Trauma
Impacts from falls, car accidents, or being hit during sports can chip a tooth or create deeper cracks. The risk is higher in contact sports, especially without a mouthguard.
Biting Or Chewing Hard Objects
Biting down on hard foods (such as nuts, ice, or hard candy) can overwhelm enamel and cause a fracture. Habits like chewing pens or biting nails can also stress teeth over time.
Tooth Decay
Cavities weaken the tooth from the inside out. As decay progresses, the remaining tooth structure becomes more likely to break under normal biting forces.
Bruxism (Teeth Grinding)
Grinding or clenching—often during sleep—puts repeated heavy pressure on teeth. Over time, this can create microcracks that grow into a visible fracture.
Age-Related Enamel Wear
Enamel can thin with age and with years of wear and tear. When enamel is thinner, teeth are more sensitive to pressure and more likely to crack.

Table of Contents
Who Is Most Likely To Experience Tooth Fractures?
Tooth fractures can affect anyone, but they tend to be more common in certain groups. Risk increases with higher impact activities, enamel wear, and conditions that increase bite force.
- Children And Teenagers: Active play, sports, and falls are common reasons for chipped or broken teeth.
- Athletes In Contact Sports: Sports like football, basketball, martial arts, and hockey raise the risk of direct impacts to the mouth.
- Older Adults: Enamel wear, existing dental work, and age-related changes can make teeth more prone to cracking.
- People Who Grind Or Clench: Bruxism increases pressure on teeth and can turn small cracks into larger fractures.
What To Do If A Tooth Breaks
If you suspect a tooth has fractured, quick action can make treatment easier and more comfortable. Use the steps below as first aid, then arrange a dental visit as soon as possible.
- Stay calm and check the area. Look for sharp edges, bleeding, and whether a piece of tooth is missing.
- Save any broken pieces. If you can find the fragment, store it in clean water or milk and bring it to your appointment.
- Rinse gently. Use lukewarm water to rinse and remove debris. Avoid vigorous swishing if there is bleeding.
- Protect the tooth. If the edge is sharp, cover it with dental wax (or sugar-free chewing gum) until you see a dentist.
- Manage pain and swelling. Use a cold compress on the outside of the cheek. Over-the-counter pain relief may help if it’s safe for you.

Treatment Options For Tooth Fractures
Treatment depends on how deep the crack goes and whether the nerve is affected. A dentist will check the tooth, take imaging when needed, and recommend the option that best protects the tooth long-term.
Composite Bonding Or Fillings
Small chips and minor fractures can often be repaired with tooth-colored composite. This restores shape and function with minimal removal of tooth structure.
Dental Crown Or Porcelain Restoration
When a larger portion of the tooth is damaged, a crown may be used to cover and strengthen it. Crowns help protect against further cracking during chewing.
Root Canal Treatment
If the fracture exposes or inflames the pulp (the nerve), root canal treatment may be recommended. Afterward, a crown is often placed to support the tooth.
Extraction And Dental Implant
If the tooth cannot be repaired, removal may be necessary. A dental implant is one common way to replace a missing tooth and restore biting function.
How To Relieve Pain After A Tooth Fracture
Pain is common after a tooth breaks, especially if the crack is deep or the tooth is sensitive. These steps can help until you’re able to see a dentist.
- Apply a cold compress. Hold a cold pack against the cheek for 10–15 minutes at a time to help with swelling and discomfort.
- Use appropriate pain relief. Over-the-counter pain medicine may help. Follow the label directions and avoid placing aspirin directly on the gum.
- Stick to soft foods. Choose softer foods and chew on the opposite side to avoid worsening the fracture.
Precautions To Reduce The Risk Of Tooth Fractures
Many fractures are preventable with a few habit changes and the right protective gear. These steps are especially useful if you have a history of cracked teeth or grinding.
- Wear a mouthguard for sports. A properly fitted mouthguard reduces the risk of impact-related fractures.
- Treat teeth grinding. If you clench or grind, ask your dentist about a night guard and ways to reduce strain on teeth.
- Avoid chewing hard objects. Skip ice, hard candy, and non-food items like pens or fingernails.
- Maintain strong oral hygiene. Brushing, flossing, and treating cavities early helps keep teeth structurally strong.

Frequently Asked Questions
What causes fractures in teeth?
Fractures are caused by trauma, biting hard objects, decay, large fillings, or grinding.
Can fractures in teeth heal?
Teeth cannot truly heal; cracks may be stabilized, but damaged structure won’t regrow.
How to prevent a fractured tooth?
Prevent fractures by avoiding hard chewing, treating decay, wearing a nightguard, and regular dental care.
Why would my tooth suddenly break?
A tooth can break suddenly when hidden decay or cracks weaken it, then biting.
Which teeth are most likely to fracture?
Back teeth, especially molars, and heavily filled or root-treated teeth fracture most.
Can you leave a fractured tooth?
Leaving a fractured tooth risks worsening breakage, pain, and infection; see a dentist.
What is a Tooth Cyst?
Tooth Cyst: Symptoms, Causes, And Treatment
A tooth cyst is a fluid-filled sac that forms near a tooth root or within the jawbone, often after long‑standing infection or around an unerupted tooth. Many cysts cause no symptoms and are found on dental X‑rays. Treatment depends on the type and size and may include root canal therapy, surgical removal, or tooth extraction, followed by monitoring.
Tooth cysts are usually benign, but they can expand over time and damage nearby teeth, bone, or nerves. Because early cysts are often painless, regular dental check-ups and X-rays play a big role in finding them before they cause complications.
What Is A Tooth Cyst?
A tooth cyst is a closed sac lined by tissue and filled with fluid or semi‑fluid material. It may develop at the tip of a tooth root, around an unerupted tooth, or elsewhere in the jawbone. Some cysts stay small, while others slowly enlarge and weaken the surrounding bone.
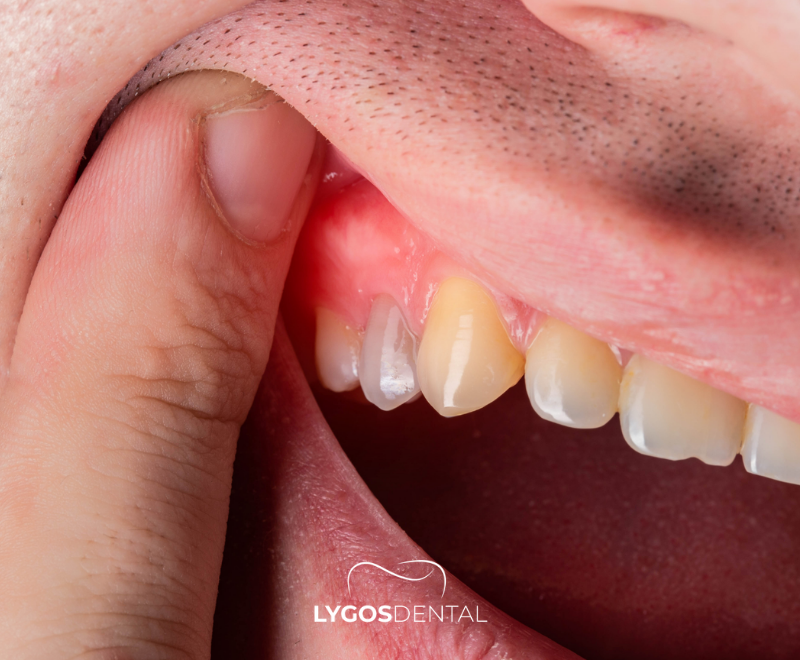
Table of Contents
Common Types Of Tooth Cysts
Dentists may use the term “tooth cyst” broadly, but there are different odontogenic (tooth‑related) cysts. The exact diagnosis matters because it affects treatment and follow-up.
- Radicular (Periapical) Cyst: Often linked to an infected or non‑vital tooth and found near the root tip.
- Dentigerous Cyst: Forms around the crown of an unerupted or impacted tooth, commonly wisdom teeth.
- Other Odontogenic Cysts: Less common types exist and may need specialist evaluation and longer follow‑up.
Symptoms Of A Tooth Cyst
Many tooth cysts cause no obvious symptoms until they grow or become infected. When symptoms do appear, they can look similar to other dental problems, so an exam and imaging are important.
- Swelling in the gum or jaw area
- A dull ache or pressure that may worsen when chewing
- Tenderness of the gum near the affected tooth
- A tooth feeling loose or shifting position as the cyst enlarges
- Changes in tooth color (in some cases)
- Drainage, bad taste, or bad breath if infection develops
What Causes A Tooth Cyst?
Causes depend on the cyst type, but most are related to infection, inflammation, or tooth development. A dentist may also consider past dental trauma, previous treatment, and how the tooth developed in the jaw.
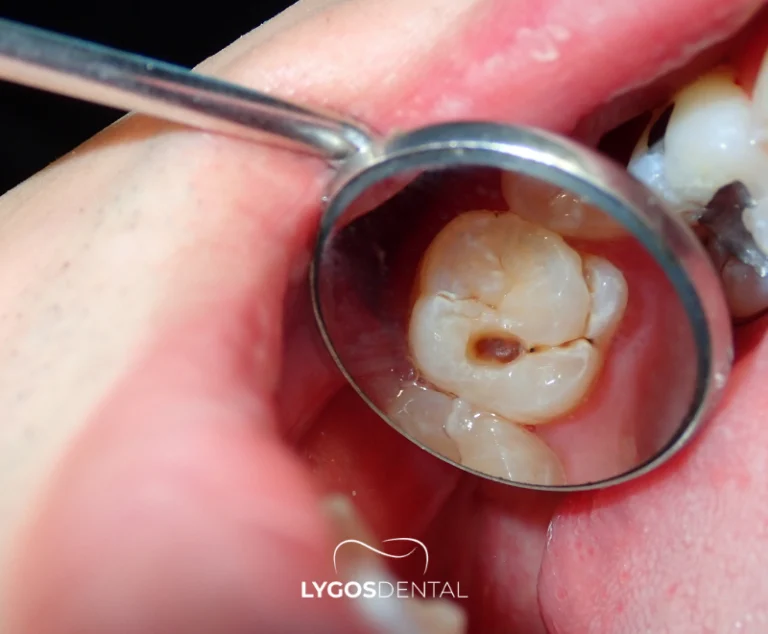
- Untreated tooth decay or deep fillings: Bacteria can reach the pulp and trigger infection near the root.
- Gum or tooth infections: Chronic inflammation can contribute to cyst formation and growth.
- Impacted or unerupted teeth: A cyst may form around a tooth that hasn’t erupted normally.
- Dental trauma: A blow to the tooth can damage the pulp and set the stage for infection‑related cysts.
- Developmental factors: Some cysts arise from tissues involved in tooth development and aren’t caused by poor hygiene.
How Tooth Cyst Treatment Works
Treatment is tailored to the cyst’s size, location, and the health of the tooth involved. Your dentist may refer you to an endodontist (root canal specialist) or an oral and maxillofacial surgeon for complex cases.
1) Diagnosis And Imaging
Most cysts are found on dental X‑rays. Depending on the case, your dentist may use 3D imaging (CBCT) to understand the cyst’s boundaries and its relationship to nearby structures.
2) Root Canal Treatment (When The Tooth Can Be Saved)
If the cyst is associated with an infected tooth, root canal therapy can remove the source of infection. In many cases, addressing the infection allows the surrounding tissue to heal and the lesion to shrink over time.
3) Surgical Removal (Enucleation) Or Decompression
For larger cysts, true cysts that don’t resolve, or cysts linked to impacted teeth, surgical treatment may be recommended. Options include removing the cyst lining (enucleation) or reducing its size first (decompression or marsupialization) to lower surgical risk.
4) Tooth Extraction (When Needed)
If the tooth is severely damaged or cannot be predictably restored, extraction may be the safest option. Your dentist can discuss replacement options such as an implant, bridge, or denture once healing is complete.
5) Antibiotics And Pain Relief
Antibiotics may be prescribed if there are signs of spreading infection, but they don’t remove the cyst itself. Pain relief medications and mouth rinses may also be used as part of your short‑term care plan.

Recovery After Tooth Cyst Surgery
Recovery varies based on the size of the cyst and the procedure performed. Most people can return to normal routines quickly, but full bone healing may take longer.
- Swelling and discomfort: Mild to moderate soreness is common for a few days. Use prescribed medication as directed.
- Stitches and follow-up: If sutures are used, your dentist may remove them in about a week, depending on the material.
- Oral hygiene: Brush gently and follow any rinse instructions to keep the area clean without disturbing healing tissue.
- Diet: Choose soft foods for the first few days and avoid very hot, spicy, or crunchy items if they irritate the area.
- Monitoring: Follow-up visits and repeat X‑rays help confirm healing and reduce the risk of recurrence.
Can You Prevent Tooth Cysts?
Not every tooth cyst can be prevented, especially developmental cysts. Still, you can lower your risk by reducing infections and catching problems early.
- Keep up with regular dental check-ups and recommended X-rays
- Brush twice daily and clean between teeth to reduce decay and gum disease
- Treat tooth pain, swelling, or a broken tooth promptly
- Use a mouthguard for contact sports to reduce dental trauma
- Follow through with planned treatment for impacted teeth when your dentist recommends it
Frequently Asked Questions
What causes a cyst on your tooth?
Pulp infection or impacted teeth trigger cysts from inflammation around tooth roots.
How do you treat a dental cyst?
Treatment includes root canal or extraction plus surgical removal; antibiotics if infected.
Can a dental cyst go away?
Most dental cysts don’t disappear alone; they usually need dental treatment.
What does a tooth cyst feel like?
Often painless; may cause swelling, pressure, tenderness, or a draining salty taste.
Are dental cysts harmful?
Yes; untreated cysts can destroy jawbone, loosen teeth, and cause recurrent infections.
How painful is dental cyst removal?
Removal is usually painless under anesthesia, with mild-to-moderate soreness afterward.
Painless Teeth Cleaning with Airflow
Painless Teeth Cleaning With Airflow
Airflow teeth cleaning (also called air polishing) is a gentle professional cleaning that uses a controlled stream of air, warm water, and fine powder to lift plaque, surface stains, and biofilm. It’s often more comfortable than traditional scraping, especially for sensitive teeth, and it can brighten teeth by removing discoloration from coffee, tea, or smoking.
Daily brushing and flossing matter, but they can’t remove every stain or hardened buildup. A professional cleaning helps protect gum health and keeps breath fresher. If you’ve avoided cleanings because they feel uncomfortable, Airflow is worth asking your dentist about.
What Is Airflow?
Airflow is a modern hygiene technique used during professional cleanings. A handheld device sprays a targeted mix of air, water, and a specially designed powder to break up dental biofilm and remove extrinsic stains on the tooth surface. Because it relies on a spray rather than metal instruments alone, many patients find it more comfortable.
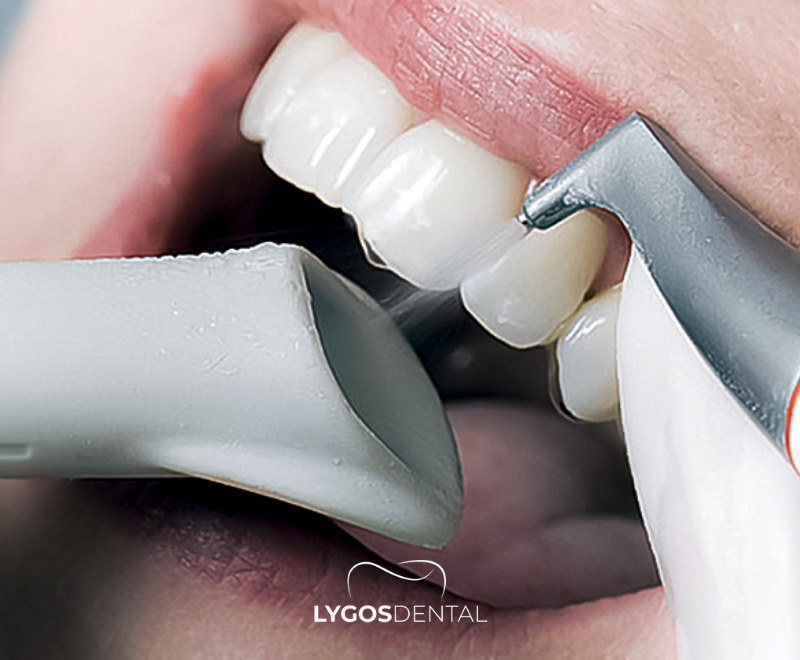
Table of Contents
How Airflow Teeth Cleaning Is Performed
Most appointments are straightforward and usually take around 20–30 minutes, depending on stain and plaque levels. A typical visit looks like this:
- Assessment: Your dentist or hygienist checks your teeth and gums and confirms Airflow is appropriate for you.
- Protection: You’ll wear protective eyewear, and a moisturiser may be applied to keep lips comfortable.
- Airflow cleaning: The spray is guided along tooth surfaces and around gumlines to remove plaque, biofilm, and stains.
- Rinse and review: Your mouth is rinsed and the clinician checks if any areas need extra attention.
- Optional fluoride: If recommended, a fluoride application may be used to support enamel strength.
Benefits Of The Airflow Method
Airflow is popular because it combines comfort with visible results. Key benefits include:
- Comfortable cleaning: Many people report less sensitivity compared with traditional scraping.
- Effective stain removal: Helps lift discoloration from coffee, tea, red wine, and smoking.
- Gentle on enamel: Designed for surface stain and biofilm removal without aggressive abrasion when used correctly.
- Gum-friendly approach: Can feel easier for people with mild gum sensitivity.
- Faster appointments: Often quicker for stain-heavy cases than polishing alone.
- Fresher breath: Reducing bacterial biofilm can help with persistent bad breath.

Who Is Airflow Teeth Cleaning Suitable For?
Airflow is suitable for many adults and teens. It’s commonly recommended if you:
- Have surface stains from coffee, tea, or smoking
- Wear braces or clear aligners and want easier stain and plaque control around appliances
- Have mild gum sensitivity and prefer a gentler-feeling clean
- Have crowns, veneers, or implants and want careful hygiene around restorations (your clinician will choose the right powder and settings)
- Feel anxious about traditional scaling or dislike the scraping sensation
When Airflow May Not Be Recommended
Airflow is safe for most patients, but it may be postponed or adjusted in some situations. Tell your dentist if you have severe or unstable asthma or other significant breathing problems, an active respiratory infection, or a known allergy to ingredients in dental powders. Your clinician may also avoid certain powders for people on a strict low‑sodium diet.
Aftercare Tips Following Airflow Cleaning
To keep the result looking clean for longer and to protect gum health:
- Avoid staining drinks and foods (coffee, tea, red wine) and smoking for at least 2 hours after the visit.
- Skip very hot or very cold drinks for the rest of the day if your teeth are sensitive.
- Brush twice daily and clean between teeth (floss or interdental brushes) to slow plaque build‑up.
- Use a fluoride toothpaste if your dentist recommends it.
- Schedule routine hygiene visits as advised—often every 6 months, and more frequently if you have gum issues.

How Much Does Airflow Cost In Turkey?
Costs vary by city, clinic type, and whether Airflow is done on its own or combined with scaling, polishing, and fluoride. In 2026, some large clinic chains in Turkey publish Airflow packages in the roughly 2,600–3,800 TL range, while more comprehensive “full hygiene” packages can be around 3,700–5,900 TL. The best way to get an accurate figure is to ask for a written quote after an exam.
Airflow Teeth Cleaning: Frequently Asked Questions
Does airflow teeth cleaning hurt?
Airflow cleaning is usually painless, but can feel chilly or sensitive on exposed roots.
Is airflow teeth cleaning better?
Airflow removes biofilm and surface stains better; scaling removes hardened tartar better.
How long does air flow teeth cleaning take?
Airflow cleaning typically takes about 20–30 minutes, depending on staining and plaque.
Is airflow better than scaling?
Airflow is better for biofilm and stains; scaling is better for hardened tartar.
Can airflow damage gums?
Airflow won’t damage healthy gums when used correctly, but may temporarily irritate inflamed tissue.
How long does air flow take?
Airflow usually takes 10–30 minutes per visit, depending on how many teeth.
What Causes Dry Mouth?
What Causes Dry Mouth?
Dry mouth (xerostomia) happens when your salivary glands don’t make enough saliva to keep your mouth comfortably moist. The most common triggers are medications, dehydration, mouth breathing (often during sleep), tobacco or alcohol use, and certain medical conditions such as diabetes or Sjögren’s syndrome. Relief usually starts with finding the cause and protecting your teeth.
What Is Dry Mouth?
Dry mouth is the feeling of oral dryness caused by reduced saliva or changes in saliva quality. Saliva does more than wet your mouth: it helps you chew and swallow, supports taste, buffers acids, and protects teeth and gums. When saliva is low, everyday activities can feel uncomfortable and the risk of dental problems goes up.
Common Symptoms
Dry mouth can show up in different ways. Some people notice it mainly at night, while others feel it throughout the day.
- A sticky or dry feeling in the mouth or throat
- Frequent thirst or needing to sip water to speak
- Bad breath (halitosis)
- Difficulty chewing, swallowing, or wearing dentures comfortably
- Burning sensation, cracked lips, or a sore tongue
- Changes in taste or increased sensitivity to spicy or salty foods
- More cavities, gum irritation, or recurrent oral infections

Table of Contents
The Most Common Causes Of Dry Mouth
Dry mouth is usually a symptom rather than a disease on its own. These are the most frequent reasons saliva drops.
1) Medication Side Effects
Many prescription and over-the-counter medicines can reduce saliva. Common examples include antihistamines, decongestants, antidepressants, some blood pressure medicines, diuretics, and certain pain medicines. If your symptoms started after a new medication or dose change, speak with a clinician before stopping anything.
2) Dehydration And Low Fluid Intake
Not drinking enough fluids is a simple but common cause. Dehydration can follow fever, vomiting or diarrhea, heavy sweating, or just inadequate water intake. Alcohol and too much caffeine can also leave you drier than you expect.
3) Mouth Breathing, Snoring, And Sleep Issues
Sleeping with your mouth open dries oral tissues quickly. Nasal congestion, allergies, chronic sinus problems, or sleep-disordered breathing can make mouth breathing more likely. If you wake up with a dry mouth most mornings, this is worth checking.
4) Tobacco, Alcohol, And Irritants
Smoking and other tobacco use can reduce saliva and irritate oral tissues. Alcohol—whether in drinks or alcohol-based mouthwashes—can also worsen dryness. Spicy foods and very salty snacks may feel more irritating when saliva is low.
5) Health Conditions That Affect Saliva
Several medical conditions are linked with dry mouth. Diabetes is a common one, especially when blood sugar is not well controlled. Autoimmune diseases such as Sjögren’s syndrome can directly affect salivary glands. Neurological conditions or nerve damage in the head and neck area may also interfere with normal saliva signals.
6) Cancer Treatments In The Head And Neck Area
Radiation therapy to the head and neck can damage salivary glands. Chemotherapy may also cause dryness in some people. If you are in cancer treatment or recovery and notice persistent dryness, coordinated care between your oncology team and dentist can help reduce complications.
7) Stress And Anxiety
Stress can change breathing patterns and trigger a “dry” sensation, especially during anxious periods. Some people clench their jaw or breathe through their mouth more when stressed, which can make symptoms worse.

Why Dry Mouth Shouldn’t Be Ignored
Saliva protects teeth and soft tissues. When it’s low, plaque builds up faster and acids stay in contact with enamel longer. That can lead to cavities, gum inflammation, mouth sores, and fungal infections. Dry mouth can also affect appetite and sleep, which then feeds the problem.
How Dry Mouth Is Diagnosed
Diagnosis usually starts with a medical and dental history, including a review of all medications and supplements. A clinician may examine your mouth for dryness, irritation, tooth decay, or signs of infection. If an underlying condition is suspected, they might recommend blood tests, salivary flow assessment, or referral to a specialist.
Treatment Options For Dry Mouth
The best treatment depends on the cause. Most people improve with a mix of daily habits and targeted medical care.
Daily Relief You Can Start Right Away
- Sip water regularly instead of drinking a lot at once.
- Chew sugar-free gum or use sugar-free lozenges to stimulate saliva (xylitol is commonly used).
- Use a humidifier at night if your bedroom air is dry.
- Avoid alcohol-based mouthwashes; choose products labeled for dry mouth.
- Limit tobacco and alcohol, and be mindful of caffeine if it worsens dryness.
- Choose softer, moist foods and add sauces or soups if chewing feels difficult.
Dental Protection And Oral Hygiene
Good oral hygiene becomes even more important when saliva is low. Brush twice daily with fluoride toothpaste and clean between teeth every day. Your dentist may recommend fluoride treatments or specific products if you’re getting cavities more easily.
Medical Treatments
If a medication is the trigger, a clinician may be able to adjust the dose, switch to an alternative, or change the timing—without compromising your overall care. For some people, prescription saliva-stimulating medicines (such as pilocarpine or cevimeline) may be considered. Saliva substitutes, gels, and sprays can also provide short-term comfort, especially at night.

Measures To Help Prevent Dry Mouth
You can’t prevent every cause of dry mouth, but a few habits lower the chances of long-lasting symptoms.
- Stay hydrated and increase fluids during exercise, heat, or illness.
- Breathe through your nose when possible; treat nasal congestion and allergies promptly.
- Keep regular dental check-ups so early decay and gum problems are caught quickly.
- Review medication lists periodically with your healthcare team, especially if symptoms change.
- If you snore heavily or feel unrested, consider screening for sleep-related breathing issues.
Natural Solutions That May Help
Some home approaches can be soothing. Use them as comfort measures, and seek medical advice if symptoms persist.
- Aloe vera: Some people find aloe vera juice or gel products soothing, but choose reputable products and avoid anything that irritates your stomach.
- Herbal teas: Unsweetened mint or chamomile tea can feel calming and may reduce the urge to mouth-breathe.
- Honey: A small amount can coat and soothe tissues, but use it sparingly and brush well to protect teeth.
- Saline rinses: Gentle saltwater rinses can reduce irritation without the sting of alcohol-based mouthwash.
When To See A Doctor Or Dentist
Get professional advice if dry mouth lasts more than a couple of weeks, keeps waking you at night, or is getting worse. You should also book an appointment if you notice mouth pain, swelling, sores that don’t heal, new tooth sensitivity, or frequent cavities. If you have diabetes, an autoimmune condition, or you’re receiving cancer treatment, early support can prevent complications.
FAQ: What Causes Dry Mouth?
What can dry mouth be a symptom of?
Dry mouth can signal dehydration, medication side effects, anxiety, diabetes, or Sjögren’s syndrome.
How do you get rid of a very dry mouth?
Sip water often, chew sugar-free gum, avoid alcohol/caffeine, use saliva substitutes, see a doctor.
How can I stop my mouth from being so dry?
Increase hydration, breathe through your nose, use a humidifier, review medicines with clinician.
What are you lacking if you have a dry mouth?
You’re often lacking fluids; sometimes saliva production is reduced from medications or gland disease.
Is there a disease that causes dry mouth?
Yes—Sjögren’s syndrome, diabetes, HIV, Parkinson’s, and radiation damage can cause dry mouth.
Why is my mouth so dry and I feel tired?
Dehydration, sleep apnea, diabetes, anemia, infections, or medications; seek medical evaluation if persistent.
Tooth Lesion Symptoms
What Are The Symptoms Of A Tooth Lesion?
A tooth lesion is damage to enamel or dentin, often from decay, wear, or trauma. Early lesions may cause no symptoms, but as they deepen you may notice cold or sweet sensitivity, tooth discoloration, pain when biting, visible chips or cracks, or gum recession near the affected area. A dental exam (often with X‑rays) confirms the cause and severity.
What Is A Tooth Lesion?
A tooth lesion is an area where the tooth structure has been weakened or lost. Some lesions are caused by tooth decay (caries), while others come from grinding, acidic erosion, aggressive brushing, or a crack after trauma. Lesions can affect enamel, dentin, and—when advanced—the inner nerve tissue.
Early Symptoms Of A Tooth Lesion
Many tooth lesions start silently. When symptoms do appear early, they are usually mild and easy to overlook.
-
- Tooth sensitivity to cold, hot, or sweet foods and drinks.
- A small rough spot, notch, or area that catches floss.
- Light discoloration (a white, yellow, or brown spot), especially along grooves or near the gumline.
- Occasional discomfort when biting, chewing, or brushing.
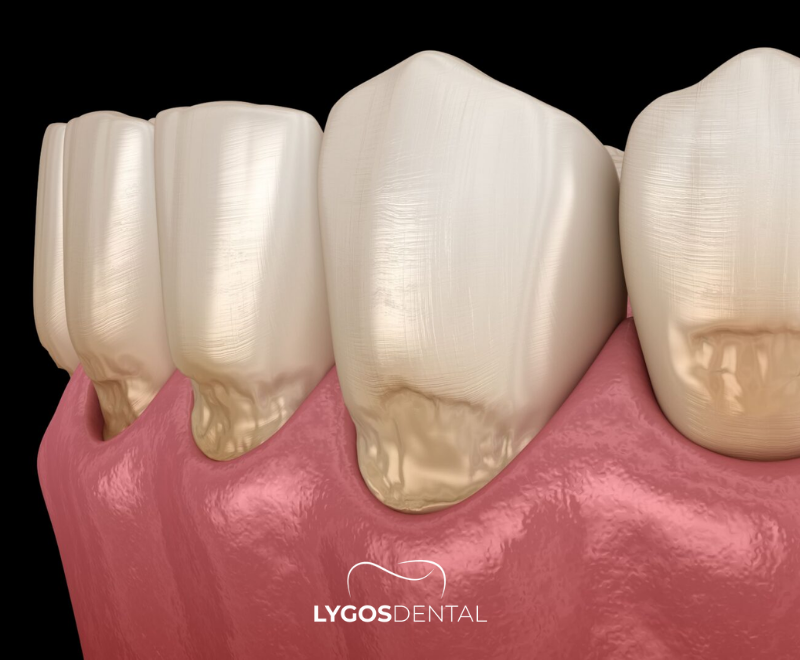
Table of Contents
Later Or More Noticeable Symptoms
As a lesion progresses, symptoms tend to become more consistent and harder to ignore.
- Sharp pain or lingering sensitivity after cold or sweet foods.
- Pain when biting down, especially on one specific tooth.
- Visible cracks, chips, or a piece of tooth that feels missing.
- Darkening of the tooth (brown or black areas) or a shadow under enamel.
- Gum recession around the affected tooth, which can expose the root and increase sensitivity.
- Bad taste, food trapping, or swelling around the tooth (possible sign of infection).
What Causes Tooth Lesions?
Tooth lesions have several common causes. Knowing the likely cause helps your dentist choose the right treatment and prevent recurrence.
- Tooth decay from plaque buildup and frequent sugar intake.
- Acid erosion from acidic foods/drinks or gastric reflux.
- Teeth grinding (bruxism) and heavy bite forces that create micro‑cracks.
- Trauma (a fall, sports injury, or biting something hard).
- Aggressive brushing or abrasive toothpaste, especially near the gumline.

Risk Factors For Tooth Lesions
Risk factors increase the chance of developing a lesion or speed up its progression.
- Poor oral hygiene (infrequent brushing, no flossing, irregular dental cleanings).
- A diet high in sugary or acidic snacks and drinks.
- Dry mouth (from medications, dehydration, or certain health conditions).
- Smoking or tobacco use, which increases gum disease risk and can worsen oral health.
- Bruxism (night grinding) or a misaligned bite.
- Naturally thinner enamel or a personal history of frequent cavities.
- Age-related enamel wear.
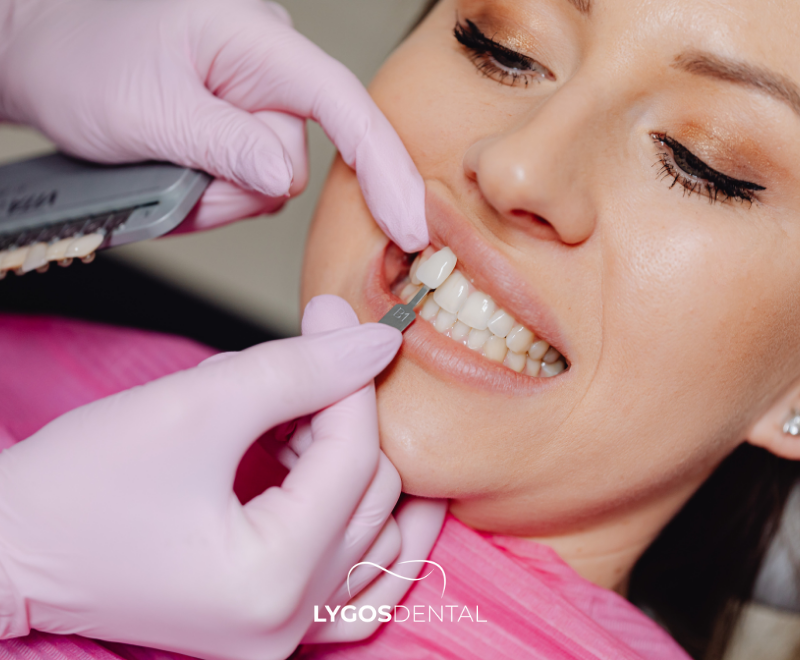
How Dentists Diagnose Tooth Lesions
Tooth lesions are usually found during routine checkups, even before they cause pain.
- Clinical exam: your dentist checks for color changes, soft areas, cracks, worn spots, and gum recession.
- Dental X‑rays: help detect decay between teeth and evaluate deeper damage not visible to the eye.
- Bite and sensitivity checks: identify pain triggers and confirm whether the tooth has a crack or inflamed nerve.
How Tooth Lesions Are Treated
Treatment depends on the type of lesion and how deep it goes. Earlier treatment is usually simpler and helps preserve more natural tooth structure.
- Fluoride or remineralization care: may help early enamel lesions and reduce sensitivity.
- Dental filling (restoration): removes damaged areas and rebuilds the tooth’s shape and function.
- Root canal treatment: used when the nerve is infected or irreversibly inflamed, followed by a restoration.
- Crown or onlay: protects a tooth that has lost a large amount of structure or has a significant crack.
Recovery And Aftercare
Recovery varies by procedure, but most people return to normal routines quickly.
- Keep up daily brushing and flossing to prevent new decay around restorations.
- Avoid very hard or sticky foods for a short period if your dentist advises it.
- Use medications only as directed if you have pain or swelling after treatment.
- Contact your dentist if pain worsens, you develop swelling, or your bite feels off.
When To See A Dentist
Book a dental visit if you notice new sensitivity, pain when chewing, visible cracks, or discoloration that doesn’t improve. Regular checkups are still the best way to catch lesions early—often before they become painful.
Tooth Lesion Symptoms: Frequently Asked Questions
What is a tooth lesion?
A tooth lesion is damaged tooth tissue from decay, erosion, trauma, or infection.
What is the 3-3-3 rule for toothache?
Use pain relief or saltwater rinses every 3 hours; see dentist within 3 days.
How to get rid of tooth lesion?
See a dentist; treatment ranges from fluoride remineralization to fillings, crowns, or root canals.
How to treat lesions on teeth?
A dentist treats them with fluoride, fillings, bonding, crowns, or root canal therapy.
What is the most common oral lesion?
Recurrent aphthous ulcers (canker sores) are the most common oral mucosal lesion.
Can tooth lesions be reversed?
Early enamel caries can be reversed by remineralization; cavitated lesions require restoration.
How Long Does Pain Last After a Filling?
How Long Does Pain Last After a Filling?
Most people feel mild soreness or temperature sensitivity after a dental filling for a few hours up to 1–3 days. Deeper fillings can stay tender for a couple of weeks as the tooth settles. Pain that worsens, lasts beyond two weeks, or comes with swelling, fever, or a bad taste needs a dental check.
Dental fillings repair cavities and strengthen a tooth, but it’s normal to feel a bit “off” afterward—especially when eating or drinking something hot or cold. The key is whether the discomfort is improving each day. Below is what to expect, why it happens, and how to get relief.
Is Pain After a Filling Normal?
Yes. A filling can irritate the tooth for a short period because the dentist has cleaned decay, dried the tooth, and placed restorative material. It’s common to notice temporary sensitivity to cold, heat, sweets, or biting pressure. This tends to fade as the tooth and surrounding tissues calm down.
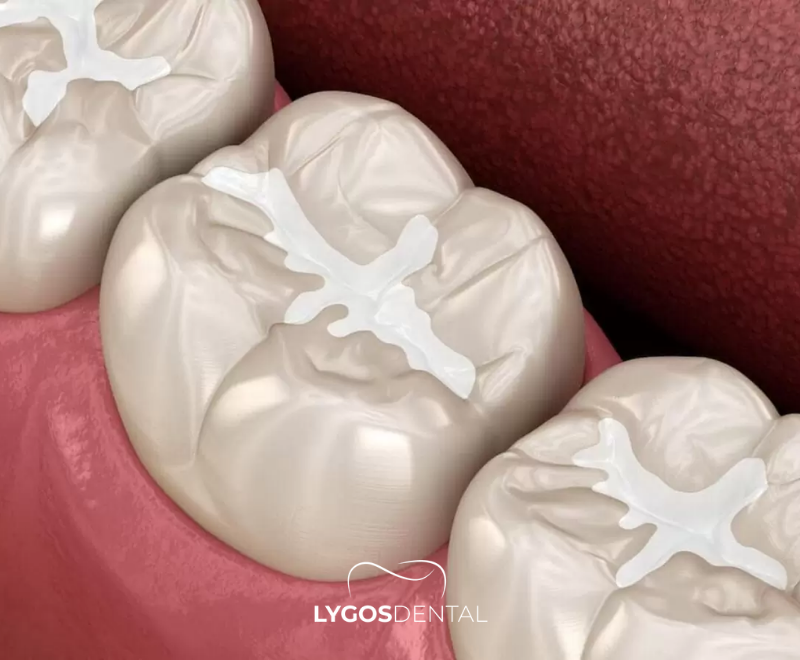
Table of Contents
How Long Does Pain Last After a Filling?
Timelines vary based on how deep the cavity was, which tooth was treated, and whether your bite feels balanced. These ranges are typical:
- Mild sensitivity or aching: often improves within 24–72 hours.
- Deep fillings (close to the nerve): can stay tender for 1–2 weeks and should gradually feel better.
- Pain that persists or gets worse: discomfort beyond two weeks, or pain that intensifies day by day, deserves a dental evaluation.
What Causes Pain After a Filling?
When pain lasts longer than expected, the cause is often mechanical (how the filling meets your bite) or nerve-related. Common reasons include:
- Filling too high: A slightly “tall” filling can create extra pressure when you chew, leading to sharp pain or jaw soreness.
- Irritation close to the nerve: If decay was deep, the nerve can stay inflamed for a while, causing lingering temperature sensitivity.
- Material sensitivity: Some people are more sensitive to certain filling materials, which can trigger short-term discomfort.
- Cracks or micro-leaks: If the tooth has tiny cracks or the seal isn’t perfect, the tooth may remain sensitive.
- New decay under the filling: Less common early on, but a poor seal can allow bacteria to create recurrent decay over time.
How To Relieve Pain After a Filling
For most people, simple steps are enough while the tooth settles:
- Use OTC pain relief if appropriate: Ibuprofen or acetaminophen can help. Follow the label directions and any advice from your dentist or pharmacist.
- Avoid extreme temperatures: Choose lukewarm foods and drinks for a day or two if cold or hot triggers sensitivity.
- Chew on the other side: Give the filled tooth a short break from hard or sticky foods.
- Try a sensitive toothpaste: A fluoride or desensitizing toothpaste can reduce sensitivity with regular use.
- Get your bite checked: If chewing feels “off,” call your dentist. A quick bite adjustment often solves the problem fast.
Home Remedies For Pain After a Filling
Home care can ease mild irritation, but it shouldn’t replace professional help when symptoms are severe or worsening:
- Warm saltwater rinse: Swish gently for 20–30 seconds to soothe tender gums and keep the area clean.
- Cold compress on the cheek: Apply for 10 minutes at a time to reduce soreness.
- Clove oil (use carefully): If you use it, dilute it and apply a small amount to the tooth area—not the gums. Stop if it irritates your mouth.
- Soft foods for 24 hours: Soups, yogurt, eggs, and pasta can reduce pressure on the tooth.

When Pain After a Filling Needs A Dentist
Call your dentist if you notice any of the following, especially if symptoms are not improving:
- Severe, throbbing, or worsening pain that doesn’t respond to over-the-counter medication.
- Pain when biting that feels sharp or “electric,” which may suggest a bite issue or deeper tooth irritation.
- Swelling, pus, a bad taste, or a pimple-like bump on the gum (possible infection).
- Fever, facial swelling, or trouble swallowing—seek urgent care.
- Sensitivity that stays intense for more than two weeks.
If you’re unsure, it’s better to get the tooth checked. A quick exam can confirm whether the filling simply needs time, needs a bite adjustment, or requires further treatment.
Frequently Asked Questions
How long should my tooth hurt after a filling?
Mild sensitivity should improve within 1–2 weeks; persistent or worsening pain needs dentist review.
What are the signs of a failed filling?
Persistent pain, new sensitivity, visible gaps/cracks, loose filling, food trapping, or bad taste.
What is the 3-3-3 rule for toothache?
It’s a popular mnemonic: 600 mg ibuprofen three times daily for up to three days.
How do I relieve tooth pain after a filling?
Use ibuprofen/acetaminophen if safe, avoid chewing there, and use cold compresses.
Why is my toothache getting worse after a filling?
Worsening pain suggests high bite, nerve inflammation, crack, or infection—see your dentist promptly.
Why does my filling only hurt at night?
Night pain often worsens lying down or grinding, increasing pressure on an inflamed nerve.
What is Surgical Tooth Extraction
Surgical Tooth Extraction: What It Is, When It’s Needed, And Recovery
Surgical tooth extraction is a minor oral surgery used when a tooth can’t be removed with a standard “simple” extraction—most often because it’s impacted, badly broken, or the roots are difficult to access. The dentist makes a small incision, may remove a little bone, and sometimes divides the tooth into sections before removal, then closes the area with stitches.
What Surgical Tooth Extraction Means
Surgical tooth extraction is used when pulling a tooth straight out isn’t safe or possible. It’s commonly needed for impacted wisdom teeth, teeth that have broken at the gumline, or roots that are curved, deep, or fragile. The procedure is usually done under local anesthesia, and sedation can be an option for anxious patients.
Surgical vs Simple Tooth Extraction
A simple extraction removes a fully visible tooth using elevators and forceps, with no gum incision. A surgical extraction involves accessing the tooth through the gum, and sometimes the surrounding bone, to remove it with minimal trauma.
Surgical cases can take longer and may cause more swelling than a simple extraction. Most people still return to routine activities within a few days, depending on the tooth and the level of surgery.
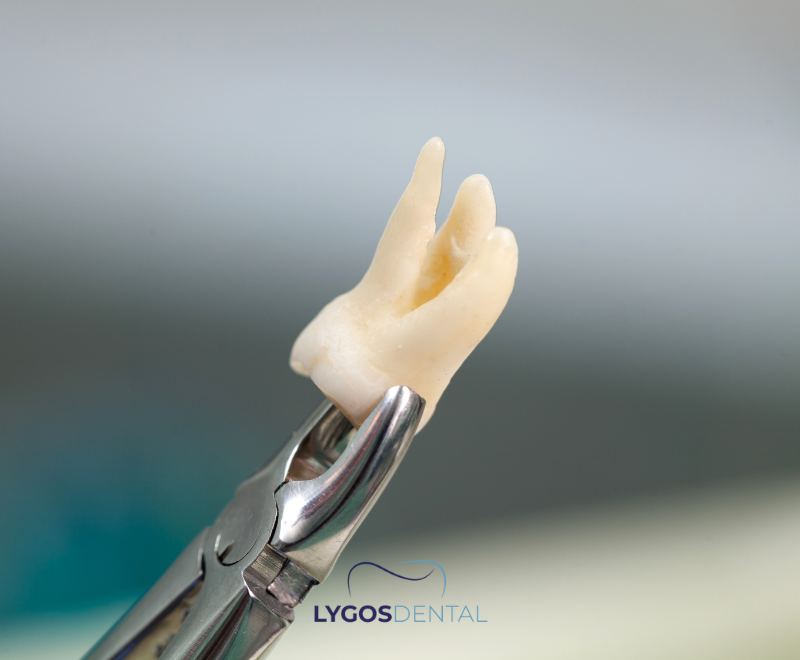
Table of Contents
When Surgical Extraction Is Needed
Dentists usually recommend a surgical approach in situations like these:
- Impacted teeth: The tooth is trapped under gum or bone, which is common with wisdom teeth.
- Severely broken teeth: The crown has fractured and there isn’t enough tooth above the gum to grip safely.
- Root fractures or complex root shape: A cracked root or sharply curved roots can make simple extraction unreliable.
- Advanced decay or infection: The tooth structure is too weak, or the surrounding tissue needs careful management.
- Certain orthodontic plans: Extractions may be needed for space, and a surgical approach is chosen if access is difficult.
- Severe gum or periodontal disease with mobility issues: Inflamed tissue and bone loss can complicate removal and healing.
How The Procedure Works
Exact steps vary by tooth position and imaging findings, but the flow is usually consistent:
- Numbing and comfort planning: Local anesthesia is used. Depending on the case, the clinic may offer sedation.
- Access: A small incision is made in the gum to reach the tooth. If needed, a small amount of bone is removed.
- Removal: The tooth may be lifted out in one piece or divided into sections to protect nearby tissue.
- Cleaning and closure: The socket is cleaned, and stitches may be placed to support healing.
- Aftercare instructions: You’ll be given guidance on pain control, diet, and oral hygiene, plus a follow-up plan if needed.
Recovery Timeline And Aftercare
Most surgical extraction sites heal in stages. Soft tissue often settles within 7–10 days, while deeper healing can take a few weeks, especially after impacted tooth removal.
First 24 Hours
Expect some bleeding, swelling, and soreness. Bite gently on gauze as directed, rest, and use cold packs on the outside of the cheek in short intervals. Avoid spitting, smoking, or using a straw, since suction can dislodge the blood clot.
Days 2–3
Swelling usually peaks and then starts to improve. Keep up with prescribed or recommended pain relief, and stay hydrated. If your dentist recommends it, gentle salt-water rinses can help keep the area clean.
First Week
Stick to soft foods, then slowly return to normal eating as comfort allows. Brush normally but gently around the site, and avoid poking the socket. Heavy exercise can raise bleeding risk, so keep activity light for a few days.
Weeks 2–4
Tenderness and food trapping usually reduce as the gum closes. If you had stitches, they may dissolve on their own or be removed at a follow-up visit, depending on the type used.
Risks And Possible Complications
Surgical extractions are routine, but complications can happen. Your dentist balances these risks against the benefits of removal.
- Dry socket (alveolar osteitis): Clot loss can cause increasing pain a few days after extraction.
- Infection: Persistent swelling, fever, or pus can signal infection and needs assessment.
- Prolonged bleeding: Oozing is common early on, but heavy bleeding should be addressed promptly.
- Nerve irritation: Lower wisdom teeth sit near nerves; temporary numbness is possible in some cases.
- Sinus communication: Upper back teeth can be close to the sinus, which may require specific aftercare.
When To Contact A Dentist Urgently
- Bleeding that doesn’t slow after firm gauze pressure
- Pain that worsens after day 3, especially with a bad taste or odor
- Fever, chills, or rapidly increasing swelling
- Trouble swallowing or breathing
- Numbness that doesn’t improve
Surgical Tooth Extraction Cost In Turkey
Pricing depends on the tooth’s position, whether it’s impacted, the imaging required (such as panoramic X‑ray or CBCT), the anesthesia or sedation choice, and the clinic’s location and expertise. Because the procedure can range from straightforward to highly complex, clinics typically quote after an exam.
As a rough reference, Turkish clinics and price guides for 2026 describe standard extractions starting from around 1,800–2,600 TL, while more complex or impacted (surgically removed) teeth may be several times higher, commonly falling in the mid‑thousands of TL depending on complexity. International patient packages may be priced differently if they include consultations, imaging, medications, and follow-up care.
Frequently Asked Questions
When is surgical tooth extraction necessary?
Surgical extraction is necessary when the tooth is impacted, broken, or not accessible for forceps.
What is the recovery time for a surgical tooth extraction?
Most people resume routine activities in 2–3 days; full bone healing takes weeks.
What to expect after a surgical tooth extraction?
Expect bleeding first hours, swelling 1–2 days, soreness, and gradual improvement over a week.
When can I go back to work after a surgical tooth extraction?
Desk work is often possible in 1–2 days; heavy labor may need 3–5.
Why does my tooth need to be surgically removed?
Your tooth needs surgery because it’s trapped, fractured, or too damaged for simple removal.
Is surgical extraction different from normal extraction?
Yes; surgical extraction uses an incision and sometimes sectioning, unlike simple forceps removal.
Dental Crown Fell Off?
My Dental Crown Fell Off: What Should I Do?
Save the crown, rinse it gently, and book a dental appointment as soon as you can. Keep the exposed tooth clean and avoid chewing on that side. If the crown fits, you may use over-the-counter temporary dental cement for short-term protection. Skip household glues, and seek urgent care for swelling, severe pain, or fever.
First, Check For Urgent Problems
A lost crown is usually fixable, but some symptoms should be treated as urgent. Contact an emergency dentist (or urgent dental service) if you notice any of the following:
- Facial swelling, a pimple-like bump on the gum, or pus
- Severe, worsening toothache that doesn’t settle with typical pain relief
- Fever, feeling unwell, or swollen lymph nodes
- Bleeding that won’t stop, or the crown came off after a significant injury
- Trouble swallowing or breathing (call emergency services)
Table of Contents
Step-By-Step: What To Do When A Crown Comes Off
Most of the time, your goal is simple: protect the tooth and keep the crown safe so your dentist can assess it.
- Find the crown and store it safely.
Place it in a small container or tissue so it doesn’t get lost. Try not to swallow it if it came loose while eating.
- Rinse your mouth and the crown.
Use lukewarm water. Avoid scrubbing the crown aggressively—just remove obvious debris.
- Look at the tooth and the crown.
If you see a broken piece of tooth, sharp edges, or the crown is cracked, don’t try to force it back on.
- Protect the area.
If the tooth feels sharp, cover the edge with orthodontic wax (or sugar-free chewing gum as a very short-term option).
- Call your dentist and arrange the soonest appointment.
A crown can sometimes be re-cemented, but the tooth may need treatment first if there’s decay or damage underneath.
Can I Put The Crown Back On At Home?
You can sometimes place a crown back temporarily, but it’s not a permanent repair. The safest at-home option is an over-the-counter temporary dental cement or an emergency dental repair kit from a pharmacy.
How To Do A Temporary Refit Safely
- Wash your hands, then gently dry the tooth and the inside of the crown with clean tissue.
- Apply a small amount of temporary dental cement inside the crown (a thin layer is usually enough).
- Seat the crown carefully in the right direction. Bite down gently to help it settle.
- Wipe away any excess material and avoid eating on that side.
- See a dentist as soon as possible, even if it feels fine.
What To Avoid
- Do not use superglue or household adhesives. They can irritate tissue and make professional re-cementing harder.
- Do not force the crown into place if it doesn’t seat easily.
- Do not ignore the problem for days. Teeth can shift and the exposed tooth can decay quickly.

Why Dental Crowns Come Loose
Crowns can last many years, but they can still come off. Common causes include:
- Cement breaking down over time
- Tooth decay at the crown margin
- A crack or fracture in the tooth underneath
- Biting something hard, sticky foods, or clenching and grinding
- A crown that no longer fits as the tooth or gum line changes
What Your Dentist Will Do
Your dentist will check both the crown and the tooth to decide whether the same crown can be reused. If everything is intact, they may clean the crown, remove old cement, and re-cement it.
If there is decay, a crack, or not enough healthy tooth structure to hold the crown, you may need treatment first. That could mean a new filling/core build-up, root canal treatment, or a replacement crown.
How To Protect The Tooth Until Your Appointment
An uncovered tooth can feel sensitive to cold, heat, and sweet foods. These tips help you stay comfortable and reduce risk until you’re seen:
- Chew on the other side and avoid hard or sticky foods.
- Brush gently around the area and keep flossing, but slide floss out rather than snapping it up.
- If the tooth is sensitive, use toothpaste for sensitive teeth. You can dab a small amount directly onto the tooth and leave it for a few minutes.
- Use pain relief only as directed on the label, and avoid placing aspirin directly on the gum or tooth.
How To Prevent A Crown From Falling Off Again
Once your dentist has fixed the cause, a few habits can help your crown stay put longer:
- Avoid crunching ice and hard sweets, and be careful with sticky candies.
- If you grind your teeth, ask about a night guard.
- Keep up with routine checkups so early decay around the crown can be caught.
- Maintain daily brushing and interdental cleaning to reduce plaque at the crown edges.
FAQ
Is it common for dental crowns to fall off?
Yes, crowns sometimes fall off, especially if cement fails or tooth decays.
How long can you go without a crown that fell out?
A few days at most; see a dentist promptly and protect the tooth.
Can you put a crown back in after it falls out?
Yes, if the crown is intact, a dentist can usually recement it.
Can I still eat if my crown falls out?
Yes, eat soft foods and avoid chewing on that side.
What will a dentist do if a crown falls off?
A dentist will assess damage, clean surfaces, and recement or replace the crown.
What is the average lifespan of a dental crown?
About 10–15 years on average, though some last longer with good care.
What is Preventive Dentistry?
Preventive Dentistry
Preventive dentistry focuses on stopping dental problems before they start. It combines regular exams, professional cleanings, fluoride and sealants when needed, plus daily brushing, flossing, and smart diet habits. The goal is to reduce cavities and gum disease, catch issues early, and protect overall health while keeping treatment simpler and less costly.
What Preventive Dentistry Means
Preventive dentistry focuses on keeping teeth and gums healthy by reducing the chance of problems such as cavities, gum disease, and enamel wear. It blends professional care with daily routines at home. The aim is simple: protect your mouth now and avoid complex treatment later.
Table of Contents
Why Preventive Care Matters
Many dental issues start quietly, then become painful or expensive once they progress. Regular prevention helps spot early warning signs and deal with them while treatment is still straightforward. Oral health also connects with overall wellbeing, and research has found links between gum inflammation and systemic conditions, so keeping gums healthy is part of looking after the whole body.
Common Preventive Dentistry Services
A dentist tailors preventive care to your age, risk level, and medical history. These are the most common services:
- Dental exams and risk checks (including gum screening) to catch problems early
- X-rays when clinically needed to see areas that are hard to check by eye
- Professional cleaning (scale and polish) to remove plaque and tartar that brushing cannot reach
- Fluoride treatments to strengthen enamel and lower cavity risk
- Fissure sealants for deep grooves on back teeth, commonly used for children and teens
- Personalised advice on brushing, flossing, diet, dry mouth, and sensitivity
For many people, a check-up every six months works well, though some may need visits more or less often depending on their risk and the dentist’s advice.

Daily Habits That Help Prevent Cavities
Home care is where prevention really happens. Small routines done consistently make the biggest difference.
- Brush twice a day with fluoride toothpaste and spend at least two minutes each time
- Clean between teeth daily using floss or interdental brushes
- Keep sugary snacks and acidic drinks to occasional treats, especially between meals
- Drink water regularly, particularly after meals, to help wash away food acids
- Choose tooth-friendly foods (cheese, yoghurt, nuts, fibrous vegetables) more often
- Avoid tobacco and limit alcohol, since both raise the risk of gum disease and oral problems
Preventive Dentistry For Adults
Adult preventive care often focuses on gum health, existing restorations, and lifestyle factors. Many adults also deal with dry mouth from medications, which increases cavity risk. If you have crowns, bridges, implants, or dentures, cleaning routines and regular reviews help protect the investment and prevent inflammation around these areas.

Preventive Dentistry For Children
Starting early builds habits that last. Children benefit from age-appropriate brushing instruction, diet guidance, fluoride where indicated, and sealants on the back teeth once they erupt. Parents play a key role by supervising brushing until a child has the dexterity to do it well on their own.
Who Benefits Most From Extra Preventive Support
Preventive dentistry suits everyone, yet some people may need closer follow-up or more frequent cleanings:
- Children and teenagers, especially during orthodontic treatment
- Pregnant women, since hormonal changes can increase gum sensitivity
- People with diabetes or conditions that affect immunity
- Smokers and people with a history of gum disease
- Anyone with implants, dentures, or complex dental work
- People with persistent dry mouth or a high cavity rate
Frequently Asked Questions
What is preventive dentistry?
Preventive dentistry is care that prevents disease, including cleanings, exams, fluoride, sealants.
What is preventative dental?
Preventative dental means preventive dental care—services that stop cavities and gum disease.
What is the difference between general dental and preventative dental?
General dental covers all routine care; preventative dental focuses specifically on preventing disease.
What are the three levels of prevention in dentistry?
Primary prevents disease onset; secondary detects early; tertiary limits damage and restores function.
Are preventative fillings worth it?
Often no: sealants or remineralization are preferred unless decay already requires a filling.
What is the difference between preventive and restorative dentistry?
Preventive dentistry avoids disease; restorative dentistry repairs existing damage with fillings, crowns, or implants.
How To Fix Crooked Teeth
How To Fix Crooked Teeth
Crooked teeth are usually corrected with orthodontic treatment such as braces or clear aligners. An orthodontist checks crowding, bite, and jaw position, then creates a plan that gently moves teeth into alignment. Afterward, wearing a retainer as directed helps keep the result stable, along with good oral hygiene and regular check-ups.
Crooked teeth can affect confidence, but they can also make daily cleaning harder and put extra stress on the bite. The right fix depends on the cause, the amount of crowding or spacing, and whether the bite or jaw needs correction.
What Causes Crooked Teeth?
Teeth can become misaligned for several reasons, including genetics, crowding as adult teeth erupt, and jaw growth patterns. Childhood habits such as thumb sucking or prolonged pacifier use may push teeth out of position. Early or late loss of baby teeth, missing teeth, and mouth breathing related to airway issues can also contribute.

Table of Contents
Do Crooked Teeth Lead To Health Problems?
Yes. Misaligned teeth are not only a cosmetic concern; they can also affect oral health and comfort.
- Harder-to-clean areas that can trap plaque and tartar
- Higher risk of cavities and gum disease
- Uneven wear or difficulty chewing properly
- Jaw discomfort or joint strain in some cases
- Speech issues for certain bite patterns
Addressing alignment early can reduce these risks and make long-term maintenance easier.
Orthodontic Treatments For Straightening Crooked Teeth
Orthodontic treatment moves teeth gradually into a healthier position. Your orthodontist may recommend one of the following options based on your bite, aesthetics, and lifestyle:
- Metal Braces: A strong, reliable option that works well for mild to complex cases.
- Ceramic Braces: Similar to metal braces, but less noticeable because the brackets blend with tooth color.
- Lingual Braces: Braces placed behind the teeth, hidden from view, with suitability depending on bite and anatomy.
- Functional Appliances: Devices often used in growing patients to guide jaw development and improve alignment.
An orthodontic exam and X-rays help confirm which approach fits your needs.

Treating Crooked Teeth With Clear Aligners
Clear aligners are a popular, comfortable alternative for many people because they are nearly invisible and removable. They can work well for mild to moderate crowding or spacing, as long as they are worn for the recommended hours each day. Some complex bite problems may still require braces or a combined approach, so suitability should be confirmed by an orthodontist.
What To Consider After Straightening Crooked Teeth?
Retention is what protects your result. Teeth naturally try to shift over time, especially in the first months after treatment. Following your provider’s retainer plan and keeping up with hygiene and check-ups makes relapse much less likely.
Key points to keep in mind:
- Use a retainer: Wear it for the duration and schedule recommended by your orthodontist.
- Keep up oral hygiene: Brush and floss consistently, and use any cleaning tools suggested for retainers or attachments.
- Be mindful with food: If you have fixed retainers or braces, avoid very hard or sticky foods that can damage appliances.
- Attend regular check-ups: Routine visits help spot early shifting, gum issues, or wear.
- Limit smoking and alcohol: These habits can worsen gum health and staining, and can complicate maintenance.
Healthy gums and stable retention are the foundation of long-lasting straight teeth.

How Much Does Crooked Teeth Treatment Cost?
Treatment cost varies with the severity of misalignment, how long treatment is expected to take, and the method used. In many clinics, metal braces tend to be the lower-cost option, while clear aligners and less visible brace types may cost more.
Location, the orthodontist’s experience, and whether you need additional procedures can also affect pricing. For an accurate estimate, book a consultation so the provider can assess your bite and outline a full treatment plan.
FAQ: How To Fix Crooked Teeth?
When is it too late to fix crooked teeth?
Never, if your gums and bone are healthy enough for orthodontic treatment.
How can I fix my crooked teeth naturally?
You can’t reliably fix crooked teeth naturally; braces or aligners are needed to move teeth.
Can you fix crooked teeth?
Yes, orthodontics like braces or clear aligners can straighten most crooked teeth.
Is it worth fixing crooked teeth?
Yes, straightening can improve bite, cleaning, wear, and confidence for many people.
Is crooked teeth a turnoff?
Sometimes, but many people focus more on health, hygiene, and confidence.
