Scarlett Johansson Teeth Veneers | LYGOS DENTAL
Scarlett Johansson Teeth Veneers
There’s no verified public confirmation that Scarlett Johansson has veneers. What people notice in photos—whiter, more even teeth—can come from veneers, whitening, orthodontics, or professional photography. This guide explains the common cosmetic dentistry options behind a “Hollywood smile,” how veneers work, material choices, lifespan, risks, and what to expect from treatment in Turkey.
Why People Talk About Scarlett Johansson’s Smile
Scarlett Johansson’s on-camera smile has looked brighter and more uniform over different stages of her career. That kind of change often leads to online speculation about veneers. Still, celebrity dental work is rarely confirmed, and photos alone can be misleading due to lighting, angles, retouching, and makeup.
Did Scarlett Johansson Get Veneers?
There is no official statement or reliable public record that confirms veneers or any specific dental procedure. If a change is visible, it could be explained by routine cosmetic dentistry such as whitening, edge bonding, minor reshaping, orthodontic alignment, or veneers. Only a treating clinician and the patient would know what was actually done.
What Veneers Are And What They Fix

Table of Contents
Veneers are thin shells bonded to the front surface of teeth to change their shape, color, or symmetry. They’re commonly used to mask discoloration that doesn’t respond well to whitening, close small gaps, and refine chipped or worn edges. Veneers are a cosmetic solution, not a substitute for treating active decay or gum disease.
Benefits People Seek From Veneers
- Brighter, stain-resistant color that stays consistent across the smile
- More even tooth shape and length for a balanced smile line
- Minor alignment and spacing improvements without braces in select cases
- A smooth, uniform finish that photographs well
Common Veneer Materials
Material choice affects translucency, strength, repairability, and cost. A reputable clinic will recommend the material that fits your bite, tooth preparation needs, and aesthetic goals.
Porcelain (Ceramic) Veneers
Porcelain veneers are popular for a natural, enamel-like translucency and good stain resistance. They’re lab-made and usually require careful planning, including shade selection and a smile design step.
Zirconia-Based Veneers
Zirconia offers high strength and can be useful where extra durability is needed. Because zirconia can look more opaque, the lab technique and material selection matter for a natural finish.
Composite Veneers (Direct Bonding-Style Veneers)
Composite veneers are built chairside with tooth-colored resin. They can be more affordable and are often less invasive, but they usually stain and wear faster than porcelain. They can be easier to repair if small chips occur.
“Before And After” Photos: How To Read Them Safely

Before-and-after comparisons online can exaggerate differences. Professional photos may use different lighting, lenses, and color grading, and many public images are retouched. If you’re assessing your own candidacy for veneers, rely on an in-person exam and diagnostic photos taken in controlled conditions.
What The Veneer Process Typically Looks Like
Most veneer cases follow a structured sequence: consultation, digital scans or impressions, smile design, and trial options such as a wax-up or mock-up. Depending on the plan, teeth may need minimal enamel reduction, then temporaries may be placed while the final veneers are fabricated. Final bonding is done with careful isolation and bite checks to protect the edges from early chipping.
How Long Veneers Last
With good case selection and care, veneers can last many years. Longevity depends on habits (grinding, nail biting), bite forces, oral hygiene, and regular dental follow-up. A night guard is often recommended for patients who clench or grind.
Risks And Limitations To Understand
Veneers are not “one-size-fits-all.” They can involve irreversible enamel reduction, and poor planning can lead to gum irritation, sensitivity, or a bulky appearance. Chipping, debonding, and edge wear are possible, especially if the bite is not managed properly.
Cost Of Dental Veneers In Turkey
Turkey is a popular destination for cosmetic dentistry, mainly due to a high volume of clinics and competitive pricing. Veneer pricing varies widely by material, number of teeth treated, laboratory quality, clinician experience, and whether a full smile design is included. When comparing quotes, ask what’s included (consultation, scans, temporaries, aftercare, and any revisions).
Questions To Ask Any Clinic Before Booking
- Which veneer material do you recommend for my bite, and why?
- How much enamel reduction is planned, and can I see a mock-up first?
- Who makes the veneers (in-house lab or external lab), and what is the turnaround time?
- What happens if a veneer chips or debonds after I return home?
- Do you provide a night guard if grinding is suspected?
FAQ About Scarlett Johansson Teeth Veneers
Does Scarlett Johansson wear veneers?
No confirmed evidence; Scarlett Johansson hasn’t publicly confirmed wearing veneers.
What surgery did Scarlett Johansson have?
None; she has publicly denied having plastic surgery.
Did Scarlett Johansson have her teeth fixed?
No confirmed evidence; she hasn’t publicly confirmed having her teeth fixed.
Does Gwen Scarlett Johansson wear dentures?
No confirmed evidence; she hasn’t publicly confirmed wearing dentures.
Has Scarlett Johansson had her teeth done?
No confirmed evidence; she hasn’t publicly confirmed having her teeth done.
Side Effects of Teeth Whitening Products | LYGOS DENTAL
Side Effects of Teeth Whitening Products
Teeth whitening can brighten stains, but it can also trigger short-term tooth sensitivity and gum irritation—especially if trays or strips touch the gums or the product is overused. Less common issues include uneven color around fillings or crowns, dry mouth, and enamel wear from repeated treatments. Using the right strength and timing helps reduce these risks.
Teeth whitening is one of the most popular cosmetic dental treatments because it’s quick and usually affordable. Most products work by using peroxide-based ingredients to break down stain compounds in the enamel and dentin. The trade-off is that whitening can temporarily irritate teeth and soft tissues, particularly if you already have sensitivity or gum inflammation.
What Are Teeth Whitening Products?
Teeth whitening products are designed to lighten tooth color and reduce surface or deeper stains from foods, drinks, smoking, or age. Common active ingredients include hydrogen peroxide and carbamide peroxide (which releases hydrogen peroxide). You’ll see them in whitening toothpaste, strips, paint-on gels, tray-based kits, and in-office treatments performed by a dentist.
Whitening changes tooth color, but it does not change the color of existing dental work such as fillings, crowns, veneers, or bonding. That difference matters when you’re aiming for an even shade across your smile.
Common Side Effects Of Teeth Whitening Products
Most people can whiten safely when they follow instructions and avoid overusing products. Still, these side effects show up often enough that it’s worth planning for them—especially if you have recession, thin enamel, or a history of sensitivity.
Tooth sensitivity
Sensitivity is the most common complaint. Whitening can temporarily open pathways in the tooth structure, making nerves react more strongly to cold, heat, air, and sugary foods. It typically peaks during treatment and settles within a few days after you stop.
Gum irritation
If gel touches the gums, it can cause redness, soreness, or a brief burning sensation. This is more likely with ill-fitting trays or when too much gel is applied. Mild irritation usually improves quickly once the product is removed.
Uneven whitening
Natural teeth can lighten, but restorations won’t. If you have visible fillings, crowns, or bonding, the surrounding teeth may brighten while the restoration stays the same shade, creating a patchy look.
Enamel wear from misuse
Whitening products don’t “melt” enamel, but frequent or prolonged use—especially with high-strength gels—can roughen the surface and worsen sensitivity. Aggressive brushing with abrasive whitening toothpaste can add to enamel wear over time.
Dry mouth and irritation
Some people notice a dry mouth or mild throat irritation, particularly with strips or trays worn for long periods. Less saliva can raise the risk of bad breath and cavities if it becomes a habit.
How Whitening Products Can Affect Your Gums

Table of Contents
Gums are more sensitive than tooth enamel, so even small amounts of peroxide gel can sting. When exposure is prolonged, you may see a white patch on the gumline (a chemical irritation) that later turns red as it heals. This is usually temporary, but it’s a sign that the product is contacting soft tissue too often.
Practical ways to reduce gum irritation:
- Use only the recommended amount of gel; more does not mean faster results.
- Keep trays and strips aligned to the tooth surface and away from the gumline.
- Wipe away excess gel with a clean cotton swab before wearing the tray.
- Stop the session if you feel sharp burning, and rinse your mouth with water.
- If you have gum disease, recession, or mouth sores, get dental advice before whitening.
Home Teeth Whitening Vs Professional Whitening

Both at-home and in-office whitening can work. The best choice depends on how quickly you want results, how sensitive your teeth are, and whether you have restorations that may affect the final shade.
Home Teeth Whitening
Over-the-counter strips, gels, and whitening toothpaste are convenient and cost-friendly. Because application is self-directed, side effects often come from longer wear times than recommended, repeated rounds back-to-back, or trays that don’t fit well. If you feel increasing sensitivity, take a break for a few days rather than pushing through.
Professional Teeth Whitening
In-office whitening uses higher-strength products under professional supervision, often with soft-tissue protection and controlled timing. Dentists can also check for cavities, cracks, recession, or gum inflammation that may make whitening uncomfortable. This route tends to be faster and more predictable, especially when you want a specific shade match.
How Teeth Whitening Products Can Affect Long-Term Dental Health
Whitening is cosmetic, but it interacts with real dental issues. If you have untreated decay, leaky fillings, exposed roots, or cracks, whitening agents can penetrate deeper and increase pain. Overusing whitening can also encourage habits that wear enamel—like frequent acidic drinks, hard brushing, or constant “touch-ups.”
A quick dental check is especially helpful if you have crowns or bonding in your smile line, since you may need to plan for replacement after whitening to keep color consistent.
Recovery After Teeth Whitening
Temporary sensitivity and gum irritation often settle within hours to a few days. During that window, keep things gentle and let the tooth surface rehydrate.
- Stick to lukewarm foods and drinks for 24–48 hours; extreme temperatures can trigger sensitivity.
- Limit acidic items like citrus, soda, and vinegar-based foods right after whitening.
- Use a toothpaste for sensitive teeth and a soft toothbrush.
- Skip whitening sessions until symptoms are fully gone.
- Contact a dentist if pain is severe, swelling develops, or sensitivity lasts longer than a week.
When To Speak With A Dentist
If you’re not sure which whitening option fits your teeth—or you’ve had sensitivity in the past—ask a dentist before starting. Professional guidance can prevent unnecessary discomfort and help you choose a plan that won’t clash with fillings or crowns.
Teeth Whitening Products FAQ
Are there any negative side effects to teeth whitening?
Yes: temporary tooth sensitivity and gum irritation are the most common side effects.
How long do teeth whitening side effects last?
Most last 1–4 days; see a dentist if symptoms persist beyond a week.
Do teeth become weak after whitening?
No: used correctly, whitening doesn’t permanently weaken enamel, but may cause temporary sensitivity.
Who shouldn’t do teeth whitening?
Pregnant or breastfeeding people, children, and anyone with untreated cavities, gum disease, or extensive restorations.
What is the healthiest way to whiten your teeth?
Dentist-supervised whitening with ADA-accepted products, used as directed, after a dental exam.
Do dentists recommend teeth whitening?
Yes: dentists recommend it for suitable patients after evaluating causes of discoloration and oral health.
How to Remove Coffee Stains on Teeth | LYGOS DENTAL
How to Remove Coffee Stains on Teeth?
Coffee stains usually come from tannins and dark pigments that cling to enamel. Start with prevention—rinse with water after coffee, brush twice daily with fluoride toothpaste, and floss. For existing stains, try gentle whitening products and a professional cleaning. Avoid harsh DIY abrasives that can wear enamel and make staining worse.
Why Coffee Stains Teeth
Coffee contains tannins, a group of plant compounds that stick to the microscopic texture of enamel. Over time, those pigments become easier to see, especially if you sip coffee throughout the day.
Coffee is also acidic. Acid can soften enamel temporarily, which makes it easier for color to settle in—especially when coffee is paired with sugar, flavored syrups, or smoking.
Do Coffee Stains Damage Teeth?
Stains themselves are mostly cosmetic, but they can be a clue that enamel is being exposed to frequent acid. If enamel thins, teeth may feel more sensitive and become more prone to cavities. Keeping stains under control often goes hand in hand with better daily oral care and fewer acidic exposures.
Daily Habits That Prevent Coffee Stains
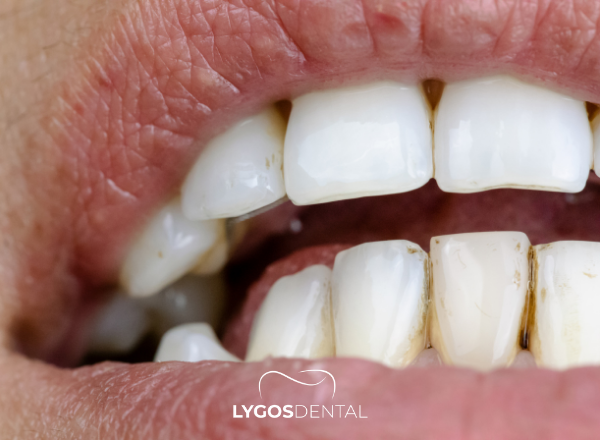
Table of Contents
Rinse, Then Wait Before Brushing
Swish water after your coffee to wash away pigments. If you want to brush, wait about 30 minutes after finishing the drink—brushing right away can scrub softened enamel.
Use The Right Toothpaste
A fluoride toothpaste is the baseline for protecting enamel. If you choose a whitening toothpaste, pick one labeled as enamel-safe and use it as directed. If you notice sensitivity, scale back and talk to your dentist about alternatives.
Floss Daily And Clean Between Teeth
Coffee stains often collect where plaque builds up—along the gumline and between teeth. Flossing and interdental brushes help remove plaque so pigments have fewer places to cling.
Change How You Drink Coffee
Drink coffee in fewer, shorter sessions instead of sipping all morning. A straw can reduce contact with front teeth for iced coffee. If you add milk, it may slightly reduce staining by diluting pigments, though it won’t prevent stains completely.
At-Home Ways To Lighten Coffee Stains
At-home options work best on surface stains. If your teeth look yellow-brown or the discoloration has been there for years, professional care usually delivers the biggest change.
Whitening Strips Or Gels (Over-The-Counter)
Whitening strips and gels typically use hydrogen peroxide or carbamide peroxide to break down stain molecules. Follow the instructions carefully and stop if you develop significant sensitivity or gum irritation.
Electric Toothbrush And Better Technique
Many people see improvement simply by brushing more effectively. Use a soft-bristled brush (manual or electric), angle it toward the gumline, and spend a full two minutes. Hard scrubbing won’t remove deep stains and can irritate gums.
What To Avoid With DIY Whitening
Be cautious with abrasive or acidic DIY methods. Baking soda can be harsh if used too often, and activated charcoal products may be abrasive. Apple cider vinegar and lemon-based mixes are acidic and can erode enamel, which often leads to more staining over time.
Professional Options That Remove Stubborn Stains
Dental Cleaning (Scaling And Polishing)
A professional cleaning removes plaque and tartar that trap stains, then polishes away many surface marks. If you haven’t had a cleaning in a while, this is usually the best first step.
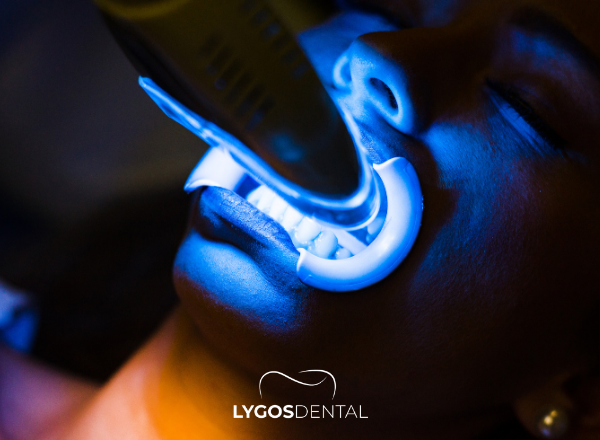
In-Office Whitening
Dentist-supervised whitening uses stronger whitening agents and protects your gums during treatment. It can lift deeper discoloration more predictably than most at-home products.
Veneers Or Bonding
If stains are severe, uneven, or paired with enamel defects, cosmetic options like veneers or composite bonding may be recommended. These cover the tooth surface rather than whitening it, so they’re used when whitening alone won’t meet your goals.
When To See A Dentist
Book a dental visit if stains appear suddenly, if you have tooth pain or sensitivity, or if whitening products cause burning or sores. Your dentist can confirm whether discoloration is from coffee, tartar buildup, medication, or enamel changes—and recommend the safest fix.
FAQ
Do coffee stains on teeth go away?
Often yes—professional cleaning and good brushing can fade coffee stains.
How do I get brown stains off my teeth?
Get a dental cleaning; whitening toothpaste or dentist-approved strips can help at home.
Can old coffee stains be removed?
Yes, old coffee stains are removable with scaling, polishing, or whitening treatments.
How to clean coffee stains off teeth at home?
Brush twice daily with fluoride toothpaste, floss, and consider dentist-approved whitening strips.
Are coffee stains permanent?
Usually no—coffee stains are typically extrinsic and can be removed or lightened.
How to Deal with Dentist Phobia | LYGOS DENTAL
How to Deal with Dentist Phobia?
Dentist phobia (dental anxiety) is an intense fear of dental visits that can cause symptoms like a racing heart, nausea, or panic. The most effective approach is a mix of preparation, clear communication with a supportive dentist, calming techniques, and—when needed—professional help such as CBT or sedation dentistry.
Table of Contents
What dentist phobia is
Dentist phobia goes beyond ordinary nerves. It’s a strong, persistent fear that can make you delay or avoid treatment, even when you know your teeth need care.
People often notice physical symptoms—sweating, a fast heartbeat, shaky hands, dizziness, or stomach upset—either in the waiting room or even while thinking about an appointment.
Common reasons people fear the dentist
Dental anxiety usually has a clear trigger. Common causes include:
- A past painful or rushed experience, especially in childhood.
- Fear of pain or needles, even when modern numbing and pain control are available.
- Feeling judged about oral hygiene or the condition of your teeth.
- Loss of control while someone works in your mouth.
- Sensory triggers such as the drill sound, bright lights, smells, or the taste of dental materials.
What to do before your appointment
Choose the right clinic and dentist
Look for a dentist who regularly treats anxious patients and is willing to slow down, explain options, and agree on a comfort plan. If you can, call ahead and briefly say you have dental anxiety so the team can schedule extra time.
Start small and build momentum
If you’ve been avoiding care, begin with a consultation or a simple exam rather than jumping straight into treatment. A few low-pressure visits can rebuild trust and reduce the “unknown” factor.
Plan comfort tools in advance
Bring headphones, a playlist, or a podcast. If mornings increase your stress, book a later slot. Eat a light meal beforehand (unless you’re told to fast for sedation) and arrive early so you’re not rushing.
What to do during the visit
Agree on a stop signal
Ask for a clear signal—often raising a hand—so you can pause the procedure at any time. Knowing you can stop instantly helps many people feel back in control.
Ask for explanations in plain language
Some patients prefer a step-by-step explanation; others feel better with minimal details. Tell your dentist what helps you, and don’t hesitate to ask for short breaks.
Talk about numbing and sedation options
If fear of pain is your main trigger, ask about local anesthetic, topical numbing gel, and techniques that reduce injection discomfort. For more severe anxiety, some clinics offer nitrous oxide (laughing gas), oral sedation, or IV sedation, depending on your needs and medical history.
Calming techniques that often help
These options can make the appointment feel more manageable, especially when you practice them before you’re in the chair:
- Slow breathing: inhale for 4 seconds, exhale for 6–8 seconds, repeating for a few minutes.
- Progressive muscle relaxation: tense and release muscle groups from shoulders to hands.
- Mindful distraction: focus on music, counting, or a calming image rather than dental sensations.
- Grounding: notice five things you can see, four you can feel, three you can hear, two you can smell, and one you can taste.
Natural remedies: what’s realistic and what to watch for
Some people find gentle supports—like chamomile tea or lavender scent—helpful for settling nerves. If you use herbal products or supplements, check with a clinician first, especially if you take medication, are pregnant, or are having sedation. Natural doesn’t always mean risk-free.
Evidence-based treatments for severe dentophobia
If your anxiety is intense or causes you to avoid care for months or years, structured treatment can make a major difference.
Cognitive behavioral therapy (CBT)
CBT helps you identify fear patterns and replace them with practical coping strategies. Many people notice improvement within a focused course of sessions.
Gradual exposure therapy
Exposure therapy reduces fear by building tolerance in small steps—starting with a clinic visit, then a simple cleaning, and progressing only when you feel ready.
Sedation dentistry and medication support
Sedation can be appropriate for certain procedures or severe anxiety. Your dentist (and sometimes your physician) will review your health history and explain benefits, risks, and recovery time.
Virtual reality (VR) distraction
Some clinics use VR as a calming distraction during treatment. Availability varies, but it can be a helpful add-on for patients who respond well to immersive relaxation.
How to keep improving over time
Try to keep appointments regular once you’ve found a supportive dentist. Each successful visit reduces fear and makes the next one easier.
After an appointment, note what worked (music, breaks, numbing, a calmer explanation style) and share it at your next visit so your care plan stays consistent.
Frequently asked questions
How do you treat a dental phobia?
Treat dental phobia with CBT, gradual exposure, and dentist-supported sedation options.
How to deal with anxiety about dentist?
Use relaxation, short appointments, a stop signal, and a supportive companion.
How common is dental phobia?
About 3% have severe dental phobia; dental anxiety affects about 15% of adults.
Why am I still scared of the dentist?
Past painful experiences, loss of control, and generalized anxiety can maintain dental fear.
How do dentists handle anxious patients?
Dentists use clear communication, tell-show-do, breaks, topical anesthesia, and sedation when needed.
Digital Smile Design | LYGOS DENTAL
Digital Smile Design
Digital Smile Design (DSD) is a planning approach in cosmetic dentistry that uses photos, videos, and digital scans to map a smile that fits your face. Before any veneers, crowns, orthodontics, or implants are started, you can preview the proposed result and approve adjustments. The goal is a smile that looks natural and functions well.
A confident smile can change how you speak, eat, and show up socially, but many people feel held back by crooked teeth, stains, gaps, or worn edges. DSD brings structure to a smile makeover by combining clinical measurements with aesthetic design.
Instead of guessing the outcome from a quick chairside mock-up, your dentist can plan the final look digitally and align each treatment step with that plan. That extra clarity helps patients feel more in control and helps clinicians work with fewer surprises.
Table of Contents
What Digital Smile Design is
Digital Smile Design is a digital workflow used to design and communicate a customized smile plan. It connects your teeth to your facial features—such as lip line, midline, smile curve, and proportions—so the result looks balanced rather than “one-size-fits-all.”
DSD is not a single treatment on its own. It’s a way to plan treatments like veneers, crowns, whitening, orthodontics, bonding, gum contouring, and implants with a shared target outcome.
How Digital Smile Design works
1) Records and facial analysis
Your dentist collects detailed records such as high-resolution photos, short videos (to capture natural speech and smile movement), and digital scans or impressions. These are used to analyze how your teeth relate to your lips and facial features.
2) Digital planning and smile simulation
Design software helps the clinician map tooth shapes, widths, and lengths, then simulate changes based on your goals. You’ll review a proposed smile design and can request tweaks—often before any tooth preparation begins.
3) Trial smile and final treatment
Many clinics create a trial smile (a mock-up) so you can test the look and feel in real life. Once the plan is approved, the dentist carries out the recommended treatment sequence, which may include veneers, crowns, aligners/braces, whitening, or implant work.
Benefits of Digital Smile Design
Patients often choose DSD for predictability and personalization. The key advantages include:
- Clear preview of the proposed result before treatment starts
- Planning tailored to facial proportions, tooth anatomy, and your preferences
- Better communication between patient, dentist, and dental laboratory
- More precise step-by-step treatment sequencing (especially for complex cases)
- Focus on function as well as appearance, supporting long-term comfort
Because you can see the direction early and give input, many people feel more confident moving forward—especially when the plan includes multiple procedures.
Who Digital Smile Design is suitable for
DSD can be helpful for anyone considering cosmetic dentistry, particularly when you want a clear preview and a coordinated plan. It’s commonly used for:
- Crooked or misaligned teeth
- Chipped, cracked, or worn teeth
- Stained or unevenly colored teeth
- Gaps between teeth
- Missing teeth (often planned with implants or bridges)
- Smile makeovers before major events, when timing and sequencing matter
Healthy gums and stable oral health are still essential. If there’s active decay, gum disease, or untreated bite issues, those are typically addressed first to protect the final result.
Dental concerns DSD can help plan
DSD is often used as the “blueprint” for solving several issues at once. Depending on your needs, the plan may include:
Misalignment
Often managed with aligners/braces, and sometimes finished with bonding or veneers for final detailing.
Gaps
Can be closed with orthodontics, bonding, or custom veneers—depending on spacing and bite.
Discoloration
May be treated with professional whitening, or covered with porcelain restorations for uniform shade.
Damage and wear
Edges can be rebuilt with bonding, veneers, or crowns to restore shape and strength.
Missing teeth
Implants or bridges can be placed in a way that matches the designed tooth proportions and gum contours.
Bite problems
Occlusion is assessed so the cosmetic result doesn’t compromise comfort or long-term stability.
Digital Smile Design cost factors
DSD itself is a planning step, so the total price is driven by the treatments included in the plan. A simple case (for example, minor bonding and whitening) is usually less costly than a full makeover that involves veneers, orthodontics, or implants.
Pricing typically depends on:
- Number of teeth being treated
- Type of restorations (bonding, veneers, crowns, implants, etc.)
- Materials selected and laboratory work involved
- Complexity of bite correction and pre-treatment needs
- Clinic location and the technology used for imaging/scanning
If cost is a concern, ask for a staged plan. Many cases can be sequenced so you address the most visible or urgent issues first while keeping the end result consistent with the original design.
What to expect from before-and-after results
Before-and-after results can be striking because DSD targets both tooth details and overall facial harmony. Common improvements include straighter-looking teeth, closed gaps, brighter and more even color, and smoother tooth edges that better match the lip line.
Keep in mind that the best outcomes look natural. A well-planned design aims for symmetry without making the smile look overly uniform or artificial.
Book a consultation
If you’d like a personalized assessment for cosmetic dentistry options such as crowns, implants, or a full smile makeover, contact our clinic to schedule an appointment and discuss whether Digital Smile Design is appropriate for you.
Digital Smile Design FAQ
What is a digital smile design?
A digital smile design is software-based planning to preview and guide cosmetic dental treatment.
Is digital smile design permanent?
Digital smile design isn’t permanent; permanence depends on the dental treatments you choose.
What are the side effects of digital smile design?
Digital smile design itself has no side effects; risks come from the procedures performed.
How does smile design differ from veneers?
Smile design is a planning process; veneers are bonded shells that change tooth surfaces.
What is the difference between smile design and Invisalign?
Smile design plans aesthetics broadly; Invisalign uses aligners to straighten teeth orthodontically.
How To Use An Electric Toothbrush | LYGOS DENTAL
What should you not do with an electric toothbrush?
To use an electric toothbrush, place the bristles gently against your teeth and gumline at about a 45-degree angle, then let the brush do the work. Move slowly tooth by tooth, spending around 30 seconds on each quarter of your mouth for a total of 2 minutes. Avoid scrubbing or pressing hard.
Table of Contents
Why Use An Electric Toothbrush
Electric toothbrushes make the brushing motion for you, so it’s easier to clean consistently.
They can be especially helpful if you have braces, limited hand dexterity, or a tendency to brush too hard.
What Counts As An Electric Toothbrush
Electric toothbrushes are powered brushes that move the bristles automatically.
Depending on the model, the head may oscillate and rotate, pulse, or create high‑frequency vibrations (often called “sonic”).
How To Choose The Right Electric Toothbrush
Brush Head Type
Pick a head that matches your needs. Soft bristles are usually the safest choice for daily use.
If you have sensitive gums, look for a “sensitive” or “gum care” head. For braces, consider an orthodontic head.
Modes And Helpful Features
Common modes include daily clean, sensitive, and deep clean. Start with sensitive if you’re new to powered brushing.
A built‑in 2‑minute timer and 30‑second pacer make it easier to cover every area evenly.
Pressure sensors are useful if you tend to press down while brushing.
Battery And Charging
If you travel, check the expected battery life and whether it uses a charging base or replaceable batteries.
Rinse and dry the handle area before placing it on the charger to avoid buildup.
Budget
Basic models clean well. Higher‑end brushes may add app tracking, extra modes, or more sensors.
How To Use An Electric Toothbrush Step By Step
1) Prepare The Brush
Charge the toothbrush if it’s rechargeable.
Attach the brush head firmly, then wet the bristles and add a pea‑sized amount of toothpaste.
2) Position The Brush Correctly
Place the bristles on the tooth surface and along the gumline at about a 45‑degree angle.
Keep a light grip. You should feel the bristles touch the teeth, not mash into the gums.
3) Let The Brush Do The Work
Turn the toothbrush on after the head is in your mouth to reduce splatter.
Guide the brush slowly—one or two teeth at a time—without scrubbing back and forth.
Spend about 30 seconds on each quadrant: upper right, upper left, lower right, and lower left.
4) Don’t Forget The Inner And Chewing Surfaces
Brush the outer surfaces, inner surfaces, and chewing surfaces of your teeth.
Use the tip of the brush head gently behind the front teeth where plaque builds up easily.
5) Finish Up
Spit out toothpaste, then rinse if you prefer. Many dentists recommend only a light rinse so fluoride can keep working.
Rinse the brush head under running water, shake off excess water, and store it upright to air‑dry.
How Often Should You Brush
Brush twice a day for 2 minutes each time.
If your dentist has recommended specific routines for gum disease, orthodontic treatment, or sensitivity, follow their advice.
Common Mistakes To Avoid
- Pressing too hard. More pressure does not mean a better clean and can irritate gums.
- Scrubbing like a manual toothbrush. With a powered brush, slow guidance beats fast strokes.
- Rushing. Use the timer and make sure you cover every surface.
- Skipping the gumline. Plaque often collects where the teeth meet the gums.
Cleaning And Maintenance
How To Clean The Toothbrush
After each use, rinse the brush head well and let it dry in the open air.
Wipe the handle occasionally with a damp cloth. Avoid soaking the handle unless the manufacturer says it’s waterproof.
When To Change The Brush Head
Replace the brush head every 3 to 4 months, or sooner if the bristles fray.
If you’ve been sick, swapping the brush head can be a sensible hygiene step.
FAQ
What is the correct way to use an electric toothbrush?
Hold brush at 45° to gumline, guide slowly tooth-to-tooth; let it vibrate.
What should you not do with an electric toothbrush?
Don’t scrub hard, use excessive pressure, share heads, or submerge non-waterproof handle.
Are you supposed to use toothpaste when using an electric toothbrush?
Use fluoride toothpaste; a pea-sized amount is enough with an electric toothbrush.
Is there a wrong way to use an electric toothbrush?
Yes—pressing too hard or moving too fast reduces cleaning and can damage gums.
How many times should I brush my teeth with an electric toothbrush?
Brush twice daily for two minutes each time, plus after meals when advised.
Do dentists actually recommend electric toothbrushes?
Yes, dentists often recommend electric toothbrushes because they improve plaque removal and brushing consistency.
Smile Design | LYGOS DENTAL
Smile Design: Procedures, Cost, And What To Expect
Smile design is a personalized cosmetic dentistry plan that improves how your teeth and gums look in relation to your face. After an assessment and a digital preview, your dentist combines treatments like whitening, bonding, veneers, or gum contouring to create a natural-looking, balanced smile that still feels like you.
Table of Contents
What Smile Design Is
Smile design is a cosmetic dentistry approach that coordinates tooth shape, color, and alignment with your facial features. Rather than choosing a single treatment, the dentist builds a plan around your proportions—such as lip line, facial symmetry, gum display, and bite—so the final result looks intentional and realistic.
Most clinics use digital photography, scans, and 3D or “digital smile design” software. This lets you see a preview before any irreversible work starts, and it helps the dentist plan details like tooth length, midline, and gum contours.
Benefits Of Smile Design
Smile design focuses on aesthetics, but it often supports function and oral health when planned properly.
Boosts self-confidence in photos and daily interactions.
Creates a more even, youthful appearance by correcting wear, chips, and discoloration.
Can improve bite balance and speech clarity when alignment or spacing is addressed.
Delivers a natural look because tooth shapes and shades are selected for your face and skin tone.
Who Smile Design Is For
Smile design can help if you have:
Discoloration that does not respond well to whitening.
Chipped, worn, short, or uneven teeth.
Gaps, mild crowding, or asymmetry.
An uneven gum line or a “gummy” smile.
There is no strict age limit. The key requirement is healthy gums and stable teeth. If you have cavities, gum disease, or active infection, those issues are typically treated first.
Common Treatments Used In Smile Design
Teeth whitening
Whitening can brighten natural teeth and set the shade for any restorations that may follow. Because restorations do not whiten, dentists often start with whitening when appropriate.
Composite bonding
Bonding uses tooth-colored resin to reshape edges, close small gaps, and repair chips. It is less invasive than veneers, but it may stain or wear faster over time.
Veneers and crowns
Veneers cover the front surface of teeth to adjust shape and color, while crowns wrap the entire tooth when more strength or coverage is needed. Material choice (porcelain, zirconia, etc.) and preparation level affect durability and cost.
Orthodontic aligners or braces
When spacing or alignment is the main issue, orthodontics may be recommended before cosmetic work. Aligners can reduce the amount of tooth reduction needed for veneers or crowns.
Gum contouring and periodontal care
Gum reshaping can level an uneven gum line, reduce a gummy smile, or create more consistent tooth proportions. Any underlying gum inflammation should be treated first for predictable healing.
Implants or bridges
Missing teeth change bite balance and facial support. Implants or bridges may be part of the plan to restore function before final cosmetic refinements.
What To Expect Step By Step
1) Consultation and assessment
Your dentist reviews your goals, examines your teeth and gums, and checks your bite. Photos, X-rays, and digital scans may be taken to plan safely.
2) Digital preview and treatment plan
You may see a mock-up or digital simulation showing proposed tooth shapes and proportions. This is where you confirm the direction—natural, bright, or more dramatic—before proceeding.
3) Preparation and trial smile
If veneers or crowns are planned, the dentist may do a conservative preparation and provide temporary restorations. Some clinics offer a short-term “trial smile” so you can test comfort and appearance.
4) Final placement and bite check
Restorations are fitted, adjusted, and bonded. The bite is checked carefully so chewing feels balanced and edges do not chip easily.
5) Follow-up
A short review visit helps confirm gum health, fit, and comfort. Minor refinements are common and are part of good cosmetic dentistry.
What To Consider Before And After Smile Design
Before treatment
Plan for any necessary dental health work first, such as fillings or gum treatment. If you grind your teeth, discuss a protective night guard early, because it can influence material choice and design.
If you smoke or consume frequent staining drinks (coffee, tea, red wine), reducing them can improve whitening results and keep restorations brighter longer.
After treatment
Brush twice daily with a non-abrasive toothpaste and floss carefully along restoration edges. Regular check-ups and professional cleanings help protect the gums and catch small issues early.
Avoid biting hard objects (ice, pens, very hard nuts) and consider a night guard if you clench or grind. These habits are common causes of chips and premature wear.
Smile Design Cost And Pricing Factors
Smile design pricing varies widely because it depends on the number of teeth involved, the treatments chosen, materials, and the clinic’s location and equipment.
As a broad guide, per-tooth cosmetic restorations (such as veneers or crowns) are often quoted in the four-figure range, and full smile makeovers can reach five figures or more. Some clinics may quote around $1,000–$5,000 per tooth, and comprehensive cases can exceed $20,000 depending on complexity and region.
The most reliable way to budget is to request a written treatment plan with itemized fees, timelines, and any possible alternatives.
Is Smile Design Permanent?
Smile design results are long-lasting, but not “forever.” Longevity depends on the procedure and aftercare.
Veneers and crowns commonly last 10–15 years, sometimes longer with excellent care.
Whitening usually needs touch-ups, often every 6–12 months depending on lifestyle.
Gum contouring is typically stable unless gum disease develops or recession occurs.
Routine dental visits, good home care, and avoiding heavy biting forces are the biggest factors in keeping results looking great.
Smile Design FAQ
How much is smile design in Turkey?
About $2,000–$8,000 total; veneers often $200–$350 per tooth.
What are the procedures for smile design?
Consultation, digital planning, mock-up, whitening, bonding/veneers/crowns, and optional gum contouring.
How long does smile design last?
Usually 3–15+ years, depending on materials, bite habits, and maintenance.
Is smile design worth the investment?
Often yes, if it improves function/appearance and you maintain long-term oral care.
What are the disadvantages of smile design?
Risks include enamel reduction, sensitivity, chipping, gum irritation, and future replacements.
What is the difference between smile design and Invisalign?
Smile design changes shape/color with restorations; Invisalign moves teeth with clear aligners.
Things to Consider After Dental Aesthetic Operations | LYGOS DENTAL
Things to Consider After Dental Aesthetic Operations
After dental aesthetic procedures, your results depend on smart aftercare: protect the treated area, choose soft foods, keep oral hygiene gentle, and manage sensitivity early. Avoid hard or sticky foods, smoking, and skipping follow-ups. Contact your dentist promptly for persistent pain, swelling, bleeding, or loose restorations.
Table of Contents
What Dental Aesthetic Procedures Include
Dental aesthetic procedures improve the look of teeth and gums while often supporting function. Common options include teeth whitening, veneers, crowns, gum contouring, dental implants, and orthodontic treatments such as clear aligners.
Even when the goal is cosmetic, these treatments can help with bite balance, tooth protection, and easier cleaning. Knowing what was done in your case makes aftercare simpler and reduces the risk of accidental damage during healing.
Why Aftercare Matters
Post-treatment care protects both your comfort and the longevity of your dental work. Ignoring instructions can increase the chance of infection, prolonged irritation, or early failure of restorations.
Good aftercare supports proper tissue healing after procedures such as gum contouring or implant placement. It also helps veneers and crowns bond and settle as intended, reducing the likelihood of costly repairs later.
Dietary Recommendations After Treatment
The First 24–48 Hours
Stick to soft, lukewarm foods and drink plenty of water. If you have numbness from anesthesia, chew slowly and avoid biting your cheek or tongue.
Foods And Drinks To Avoid
Avoid hard, crunchy, or sticky foods that can stress new restorations or irritate healing gums. Very hot or very cold drinks can worsen sensitivity, especially after whitening or enamel shaping.
Limit stain-causing items such as coffee, tea, red wine, and deeply colored sauces if you have whitening or new bonding. If you do consume them, rinse with water afterwards.
Helpful Choices
Choose foods that are easy to chew and support healing, such as yogurt, eggs, soups, well-cooked vegetables, and soft fruits. If chewing is uncomfortable, smoothies can be useful, but avoid using a straw after extractions or implant surgery.
Managing Pain, Swelling, And Sensitivity
Mild discomfort is common, and sensitivity can last several days depending on the procedure. Follow the medication plan your dentist recommends and do not exceed the labeled dose for over-the-counter pain relief.
- Cold compress: Apply to the outside of the face in short intervals during the first day if swelling is expected.
- Gentle brushing: Use a soft toothbrush and avoid aggressive scrubbing around the treated area.
- Saltwater rinse: If advised, rinse gently with warm saltwater to soothe tissues and keep the area clean.
- Night protection: If you clench or grind, ask about a night guard to protect veneers, crowns, and bonding.
Common Mistakes To Avoid
- Eating hard or sticky foods too soon, which can crack or dislodge restorations.
- Using treated teeth as tools (opening packages, biting nails, chewing ice).
- Smoking during healing, which slows recovery and can stain new work.
- Skipping hygiene because the area feels tender; instead, clean gently and consistently.
- Delaying follow-up visits, which are important for checking fit, bite, and healing.
If something feels off—sharp edges, a high bite, or increasing sensitivity—report it early. Small adjustments are often quick when addressed promptly.
What To Do If Complications Arise
Call your dentist if pain worsens instead of improving, or if swelling and bleeding persist beyond what you were told to expect. Fever, a bad taste, or discharge may point to infection and should be evaluated quickly.
If a veneer, crown, or temporary restoration feels loose, avoid chewing on that side and keep the area clean. Arrange an urgent appointment rather than trying to reseat anything at home.
FAQ
What are the must haves after dental surgery?
Keep gauze pressure, take prescribed meds, use ice, rinse gently, eat soft foods.
What not to do after dental surgery?
Avoid smoking, straws, spitting, vigorous rinsing 24h, hard foods, and touching the site.
How to sleep after dental surgery?
Sleep with head elevated on pillows, lying on your back, avoiding pressure on the area.
Can I eat yogurt after dental surgery?
Yes—eat cool, smooth yogurt without seeds once numbness fades, chewing away from site.
Can I kiss after dental surgery?
Avoid kissing for 24–72 hours; it can disturb the clot and introduce bacteria.
What Happens if a Tooth Is Swallowed | LYGOS DENTAL
What Happens If You Swallow A Tooth?
In most cases, a swallowed tooth moves through the digestive system and passes naturally in your stool within a few days. Problems are uncommon, but a sharp or large piece can irritate the gut or, rarely, get stuck. Seek urgent help right away for choking, breathing trouble, severe pain, vomiting, or blood.
Table of Contents
Why People Accidentally Swallow Teeth
Swallowing a tooth is more common than it sounds. It can happen when a loose baby tooth comes out while eating or sleeping, after a sports injury, or when a chipped tooth breaks further during a meal.
Dental work can be another trigger. Crowns, temporary restorations, and small tooth fragments may slip backward if you cough, swallow suddenly, or your mouth is numb after treatment.
Is Swallowing A Tooth Dangerous?
Most of the time, no. A whole tooth is usually small enough to travel through the stomach and intestines without causing harm.
Risk goes up when the tooth (or fragment) is large, jagged, or attached to something sharp, or when the person has a narrowing in the digestive tract from a prior condition or surgery.
What Usually Happens In Your Body
1) Down The Esophagus
After you swallow, the tooth typically slides down the esophagus with food and saliva. If it scratches the throat, you may feel a brief “stuck” sensation, even when it has already moved on.
2) In The Stomach
Stomach acid does not dissolve teeth. The tooth remains intact and usually moves forward with normal digestion.
3) Through The Intestines And Out
Most swallowed objects pass on their own. A tooth may pass within 24–48 hours for some people, but it can also take a few days. Many children’s health services cite a window of about 3–5 days for objects to pass.
You do not need to force it with laxatives. Normal eating, good hydration, and a steady routine are usually enough.
Symptoms To Watch For
Most people feel fine after swallowing a tooth. Still, it’s smart to watch for warning signs that suggest irritation, blockage, or (rarely) that the tooth entered the airway instead of the stomach.
Get urgent help right away if you notice:
- Choking, coughing that won’t settle, wheezing, or trouble breathing
- Severe or worsening chest, throat, or abdominal pain
- Repeated vomiting or inability to keep fluids down
- Blood in vomit or black/tarry stools
- Fever, chills, or a generally unwell feeling after the event
What To Do Right After You Swallow A Tooth
Stay calm and check breathing first. If the person is coughing forcefully, encourage coughing. If there is any breathing trouble, call emergency services.
If breathing is normal, sip water and avoid trying to make yourself vomit. For children, do not give laxatives unless a clinician specifically advises it.
Over the next few days, stick to regular meals. Fiber-rich foods (vegetables, fruits, oats, whole grains) and adequate fluids can support comfortable bowel movements.
When To Contact A Doctor Or Dentist
Contact a clinician the same day if you swallowed a sharp fragment, a long piece, multiple fragments, or if you have known digestive narrowing, prior bowel surgery, or inflammatory bowel disease.
Also contact a clinician if you swallowed a dental restoration (like a crown) and you’re not sure whether it went down the food pipe or into the airway. A dentist can help identify what was swallowed and whether a medical check is needed.
How Doctors Check And Treat It
If symptoms suggest the tooth is stuck in the esophagus or airway, clinicians may use imaging (such as X‑ray) and decide whether removal is needed.
Objects that have reached the stomach usually pass without intervention. If there are signs of blockage or perforation, urgent assessment is required and removal may be done with an endoscope.
Can A Swallowed Tooth Cause Infection?
A decayed tooth contains bacteria, but the digestive system is designed to handle bacteria from food and saliva. Infection from swallowing a tooth is uncommon.
That said, if a sharp edge causes a cut inside the digestive tract, any fever or increasing pain should be taken seriously and checked promptly.
FAQ
What should you do if you swallow a tooth?
Contact a clinician if sharp or symptomatic; otherwise monitor stools and seek care if pain.
Will stomach acid dissolve a swallowed tooth?
No; enamel and dentin resist stomach acid, though fillings may corrode slightly.
How rare is it to swallow a tooth?
It’s uncommon; exact frequency isn’t well documented.
Will I be okay if I swallowed a piece of my tooth?
Likely yes if small and smooth; seek urgent care for pain, vomiting, bleeding.
How long does it take to poop out a swallowed tooth?
Usually 1–3 days; see a clinician if not passed within a week.
Will I choke if I swallow a tooth?
Unlikely; choking risk is during swallowing, not after it reaches the esophagus.
How is Bonding Procedure Performed | LYGOS DENTAL
How Is Dental Bonding Performed?
Dental bonding is done by gently preparing the tooth surface, applying a bonding agent, and shaping a tooth‑colored composite resin to match your smile. A blue curing light hardens the material in seconds, then the dentist trims and polishes it for a natural finish. Most cases take 30–60 minutes per tooth.
Table of Contents
What Is Dental Bonding?
Dental bonding is a cosmetic and restorative technique where a dentist applies composite resin to the tooth to improve its appearance or function. The resin is color-matched to blend with nearby teeth, then hardened with a curing light. Because it usually requires minimal enamel removal, bonding is considered a conservative option compared with veneers or crowns.
When Is Dental Bonding Recommended?
Bonding works best for small-to-moderate changes where the tooth is otherwise healthy. Dentists often use it to correct minor shape issues or repair limited damage. If the tooth is heavily broken down or the bite forces are high, more durable options may be advised.
- Small chips or edge fractures
- Hairline cracks or worn edges
- Small gaps between front teeth
- Discoloration that doesn’t respond well to whitening
- Slightly uneven or misshapen teeth
- Exposed root surfaces from gum recession (to reduce sensitivity and protect the root)
Step-By-Step: How The Bonding Procedure Is Performed
1) Consultation And Shade Selection
Your dentist examines the tooth, checks your bite, and discusses what you want to change. A shade guide is used to choose a resin color that matches your natural enamel (or a slightly brighter shade if you’re bonding after whitening). Photos may be taken to document the starting point and plan the shape.
2) Tooth Preparation
The tooth is cleaned and isolated so the area stays dry. The surface is lightly roughened and treated with an etching gel or conditioning solution to help the resin grip the enamel. A bonding agent is then brushed on and set with a light, creating a strong foundation.
3) Applying And Sculpting The Composite Resin
The dentist places composite resin in thin layers and sculpts it to the desired shape. This step is where the final look is created—contours, edges, and symmetry are adjusted to blend with nearby teeth. For gaps or larger repairs, multiple layers may be used to build strength and a lifelike appearance.
4) Curing, Finishing, And Polishing
A blue LED curing light hardens each layer in seconds. Once the resin is fully set, the dentist refines the shape, checks the bite, and polishes the surface so it reflects light like natural enamel. When done properly, bonding should feel smooth, look seamless, and not interfere with how your teeth come together.
Benefits Of Dental Bonding
Bonding is popular because it delivers noticeable cosmetic improvement with minimal chair time. It can often be completed in a single visit and usually without anesthesia unless the dentist is also treating decay or working near the nerve.
- Cost-effective compared with veneers or crowns
- Fast results (often 30–60 minutes per tooth)
- Conservative approach with little to no enamel removal
- Natural-looking finish when shade and polish are done well
- Easily repairable if a small area chips
Limitations And Risks
Composite resin is strong, but it is not as stain-resistant or wear-resistant as porcelain. Knowing the limits helps you choose the right treatment and set realistic expectations.
- Chipping or cracking, especially if you bite hard objects or grind your teeth
- Staining over time from coffee, tea, red wine, and tobacco
- A shorter lifespan than porcelain restorations (often about 3–10 years, depending on bite and habits)
- Color mismatch if surrounding teeth change shade later (for example after whitening)
Who Is A Good Candidate For Bonding?
Bonding is a good fit for patients with healthy enamel and minor cosmetic concerns. It’s commonly chosen for front teeth where appearance matters most and bite forces may be lighter. If you have active gum disease, untreated decay, heavy clenching, or very large restorations, your dentist may recommend another approach.
Aftercare: How To Make Bonding Last
You can eat and drink soon after bonding, but gentle habits make a big difference in longevity. The resin can pick up stains and wear faster than natural enamel, so prevention matters.
- Brush twice daily with a non-abrasive toothpaste and floss every day
- Avoid biting ice, pens, fingernails, and hard candies
- Limit strong staining foods and drinks; rinse with water after coffee or tea
- Schedule regular cleanings and ask your dentist to check the bonded edges
- If you grind at night, wear a custom night guard to reduce chipping risk
Frequently Asked Questions
Is a dental bonding procedure painful?
Dental bonding is usually painless; numbing is rarely needed unless decay is treated.
How long does a tooth bonding last?
Tooth bonding typically lasts 3–10 years, depending on care and location.
How is dental bonding done?
Dental bonding involves etching, applying resin, shaping, hardening with light, then polishing.
Do teeth rot under bonding?
Teeth can decay around bonding margins if plaque accumulates; resin itself doesn’t rot.
Is bonding better than veneers?
Bonding is cheaper and reversible; veneers last longer and resist stains better.
How long can you eat after dental bonding?
You can eat immediately after bonding, but avoid hard or staining foods for 24 hours.
