Teeth Whitening Pen
In this article, we will provide a detailed and multi-faceted answer to the question: How does…
Chronic periodontitis is a long-term gum infection caused mainly by plaque and tartar buildup. It can quietly inflame the gums, deepen pockets around teeth, and gradually weaken the bone that holds teeth in place. With early diagnosis, professional cleaning, and consistent home care, progression can be slowed or stopped and tooth loss can often be prevented.
Gum disease often starts with mild symptoms, so it can be easy to ignore. Chronic periodontitis is one of the most common forms and may progress for months or years before pain appears. Untreated disease can lead to loose teeth, tooth loss, and ongoing inflammation that affects overall health.
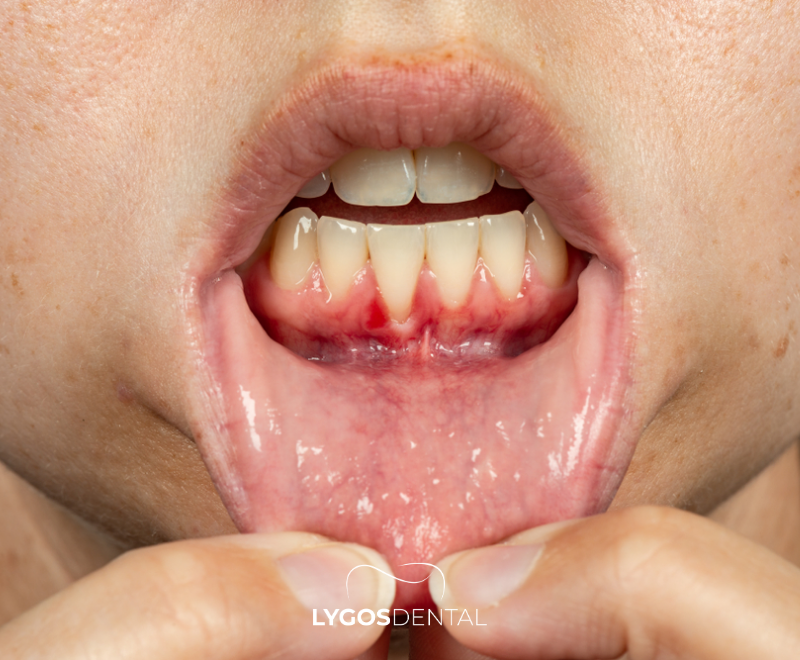
Chronic periodontitis is a slow-progressing inflammation and infection of the tissues that support the teeth. Bacteria in dental plaque trigger irritation of the gums, and over time the infection can reach the periodontal ligament and jawbone. As the supporting structures break down, gums may recede and teeth can become mobile.
Both chronic and acute periodontitis affect the gums and the tissues around teeth, but they behave differently. Chronic disease tends to develop gradually with subtle symptoms, while acute episodes usually appear suddenly and can be painful.
| Feature | Chronic Periodontitis | Acute Periodontitis |
| Onset | Slow, often unnoticed at first | Sudden |
| Symptoms | Often mild at the beginning; may include bleeding, recession, bad breath | More intense pain, swelling; may include fever in severe cases |
| Progression | Develops over months or years | Can worsen quickly |
| Prevalence | More common | Less common |
| Treatment urgency | Planned treatment plus long-term maintenance | Needs prompt care to control symptoms and infection |
Acute flare-ups can sometimes occur on top of chronic disease. If pain or swelling appears suddenly, a dental visit should not be delayed.
The primary trigger is bacterial plaque that stays on the teeth and along the gumline. When plaque hardens into tartar, it becomes harder to remove without professional cleaning and provides a surface where bacteria thrive.

Chronic periodontitis can affect anyone, but certain factors make it more likely or more severe. If you recognise one or more of the risks below, regular dental checks are especially important.
Symptoms can be mild in the early stages. Many people first notice bleeding while brushing or persistent bad breath rather than pain.

Diagnosis is based on a clinical exam and measurements around each tooth. Dentists often use a small probe to measure pocket depths and check for bleeding, along with X‑rays to look for bone loss. The results help determine severity and guide a treatment plan.
Treatment aims to control infection, reduce inflammation, and stabilise the supporting tissues. The right approach depends on how advanced the disease is and how well you can keep the area clean at home.
Most cases begin with professional deep cleaning, often called scaling and root planing. This removes plaque and tartar above and below the gumline and smooths root surfaces to make reattachment easier. Your dentist may recommend antiseptic rinses or local medications depending on pocket depth and inflammation.
Antibiotics may be used in selected cases to reduce bacterial load, either as a local gel placed into pockets or as tablets. They are usually an add-on to thorough cleaning rather than a replacement for it.
When pockets are deep or bone loss is significant, surgery may be recommended. Procedures can include flap surgery to clean deep areas, and regenerative options such as bone grafting or guided tissue regeneration to support healing where appropriate.
Some practices use laser-assisted therapy as part of periodontal treatment. The goal is to reduce bacteria and inflamed tissue with a minimally invasive approach. Suitability depends on the case and the equipment available.
Long-term success depends on maintenance. After active treatment, your dentist or periodontist will usually recommend periodontal maintenance visits at a tailored interval, along with a home-care routine to prevent relapse.
Chronic periodontitis is typically managed rather than “cured” overnight, so consistency matters. These habits help protect the gums and reduce the chance of recurrence.
It is a long-term condition, so the focus is usually on stopping progression and keeping the disease stable. With early care, professional treatment, and ongoing maintenance, many people keep their teeth and gums healthy for years.
Mild cases may improve after a small number of visits, while moderate to advanced disease may need several appointments and ongoing follow-up. If surgery is needed, healing and reassessment can extend the timeline.
Yes. As bone support decreases, teeth can loosen and may eventually need to be removed. Early treatment significantly reduces this risk.
The disease itself is not “caught” like a cold, but the bacteria involved can be shared through saliva. Good oral hygiene for everyone in the household and avoiding sharing toothbrushes are sensible precautions.
If you notice bleeding gums, swelling, or persistent bad breath, book a dental evaluation. Early care is usually simpler and more cost-effective, and it helps protect the teeth and bone support over the long term.