Millie Bobby Brown Teeth Veneers | LYGOS DENTAL
Millie Bobby Brown is a world-renowned actress and a social media sensation who gained fame at…
Dentinogenesis imperfecta is an inherited dentin defect that can make teeth look blue‑gray or yellow‑brown and wear down faster than normal. Because the dentin layer is weak, enamel may chip and teeth can fracture. A dentist can confirm the diagnosis with an exam and X‑rays, then plan protective restorations to preserve chewing and appearance.
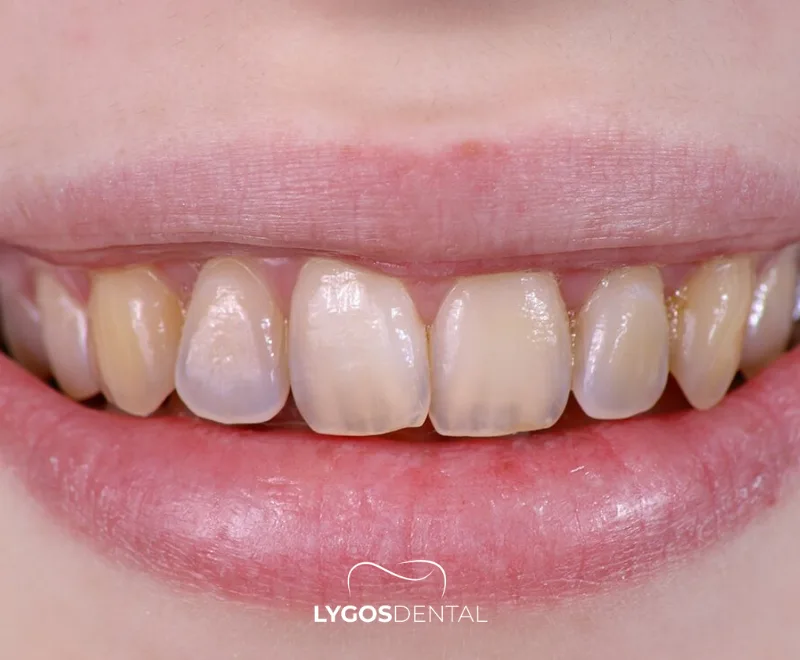
Dentinogenesis imperfecta is a genetic condition where the dentin (the layer under the enamel) forms abnormally. As a result, teeth may look darker, appear more translucent or “opalescent,” and wear down or fracture more easily than expected.
It can affect primary teeth, permanent teeth, or both. Because dentin supports enamel, even a thin chip in the enamel can expose weaker dentin and accelerate breakdown.
Symptoms can vary by age and severity. Many people notice changes in color or rapid wear early on, often in the front teeth.
Children and teens may feel self‑conscious about the appearance of their teeth. Supportive, early care often helps protect both confidence and function.
Dentinogenesis imperfecta is most often inherited in an autosomal dominant pattern, so a parent with the condition may pass it on to a child. In many non‑syndromic cases, the cause is a pathogenic variant in the DSPP gene, which plays a key role in dentin formation.
Some people have dentinogenesis imperfecta as part of osteogenesis imperfecta (a connective‑tissue disorder). In those cases, the dental findings can be linked to collagen gene variants (such as COL1A1 or COL1A2) that also affect bone strength.

Clinicians commonly describe dentinogenesis imperfecta using three types. The types help explain whether the condition is linked to osteogenesis imperfecta and what is seen on dental X‑rays.
Type I occurs alongside osteogenesis imperfecta. Teeth can be discolored and prone to wear, and patients may also have signs such as frequent fractures or blue‑tinted sclerae. Dental management typically requires coordination between dental and medical teams.
Type II is the most common form and affects the teeth without osteogenesis imperfecta. Both primary and permanent teeth may show discoloration, enamel chipping, and accelerated wear. X‑rays often show bulbous crowns, cervical constriction, and reduced or obliterated pulp spaces.
Type III is rare and was first described in the Brandywine population in the United States. Teeth can have severe wear and breakage early in life. Radiographs may show unusually large pulp chambers and thin dentin, sometimes described as a “shell tooth” appearance.
Diagnosis is usually made by a dentist based on a clinical exam and dental imaging. Family history is helpful, since similar tooth changes across generations can point to an inherited dentin disorder.
There is no way to change the genetic cause, but treatment can protect teeth and improve function and appearance. The plan depends on age, severity, and how much tooth structure has already been lost.
Braces or aligners can be used when needed, but planning should account for fragile enamel and dentin. Your orthodontist may coordinate with a restorative dentist to protect teeth throughout treatment.
When tooth loss is extensive, fixed or removable prosthetics can restore chewing and appearance. Dental implants may be an option for adults once jaw growth is complete and overall oral health is stable.
Long‑term maintenance matters because teeth can continue to wear over time. Many patients benefit from scheduled monitoring, preventive cleanings, and timely repair of chips before they become larger fractures.
Type 1 occurs with osteogenesis imperfecta; Type 2 occurs without systemic bone disease.
About 1 in 6,000–8,000 people have dentinogenesis imperfecta.
Amelogenesis imperfecta affects enamel; dentinogenesis imperfecta affects dentin with opalescent, fragile teeth.
Dentinogenesis imperfecta causes tulip-shaped crowns from cervical constriction at the cementoenamel junction.
No culture universally skips oral hygiene; many clean teeth using chewing sticks or rinses.