How to Care for Dentures?
So, how to care for dentures? In this article, we will detail the steps necessary to…
Infection after a dental implant usually starts with inflammation of the gum around the implant and can progress to bone loss (peri-implantitis) if ignored. Early signs include increasing pain, swelling, bleeding, bad taste or odor, or pus. Prompt dental care and good home hygiene often stop the problem before the implant is affected.
Dental implants are a reliable way to replace missing teeth, but they still require surgical healing. Like any oral surgery, an implant site can become infected if bacteria build up or the tissues struggle to heal. Knowing what to watch for helps you act early and protect your results.
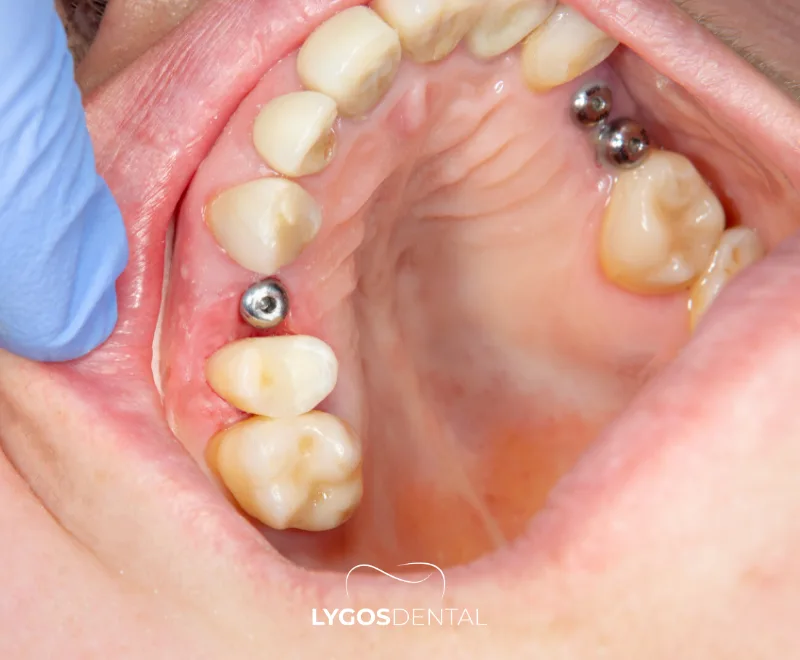
A dental implant infection is inflammation caused by bacteria around an implant. It may involve only the gum tissue (peri-implant mucositis) or, in more advanced cases, the deeper tissues and supporting bone (peri-implantitis). When bone is affected, the implant can loosen over time.
Some soreness is expected after surgery, especially in the first few days. Concern rises when symptoms worsen instead of improving, or when new symptoms appear after the initial healing period.
If you notice pus, fever, or rapidly increasing swelling, contact your dentist as soon as possible. These can signal an infection that needs prompt treatment.

Implant infections are usually linked to bacterial biofilm (plaque) accumulating at the gumline or under the gum. Several factors can make this more likely.
Some patients are more prone to peri-implant disease. Your dentist may adjust your aftercare plan if any of the following apply.

Diagnosis usually starts with a clinical exam of the gum around the implant. Your dentist may check for bleeding, swelling, pus, and pocket depth around the implant. X-rays can help assess bone levels and rule out other causes of pain.
Treatment depends on how early the problem is caught. The main goals are to remove bacteria, reduce inflammation, and protect the surrounding bone.
Self-treating with leftover antibiotics is risky and can delay proper care. Always follow your dentist’s instructions.
If you suspect an infection, home care can reduce irritation, but it cannot replace professional treatment. Use gentle brushing, keep the area clean, and avoid smoking.
When inflammation persists, it can lead to progressive bone loss around the implant (peri-implantitis). Over time, this may reduce support and increase the risk of implant failure. In rare cases, oral infections can spread beyond the mouth and become a wider health issue.
Most problems are preventable with consistent aftercare and maintenance. Your dentist may tailor advice based on your health history and the type of restoration placed.
If you think you may have an implant infection—or you want a preventive check—contact our clinic to arrange an appointment. We provide cosmetic dentistry, crowns, dental implants, and general dentistry services.
Early infection is uncommon (around 1–5%); peri-implantitis affects about 10% of implants.
Place the implant 3 mm apical and 2 mm palatal to the planned crown.
Pain, swelling, redness, pus/bad taste, bleeding, and increasing tenderness around the implant.
Peri-implant mucositis is the most common complication, causing reversible gum inflammation.
Surgery, higher cost, healing time, possible failure, and peri-implantitis are major disadvantages.