How Long Should a Retainer Be Worn?
In this article, we will provide a detailed and multi-faceted answer to the question: How does…
To reduce sensitivity after teeth whitening, start with a desensitizing toothpaste, avoid very hot, cold, and acidic foods for 24–48 hours, brush gently, and use fluoride to support enamel. If discomfort gets stronger, wakes you at night, or lasts longer than a week, pause whitening and speak with a dentist.
Whitening can brighten your smile quickly, but it can also leave teeth feeling “zingy” for a short time. That sensitivity is usually temporary, and most people can keep it mild with a few simple aftercare steps.
The key is to protect enamel while your teeth settle, and to avoid triggers that make nerves react. The tips below work for both in-office whitening and at-home kits, with one rule: follow your dentist’s or product’s instructions first.
Most whitening products use peroxide-based ingredients that move through enamel and into the underlying tooth structure. During and shortly after whitening, the tooth can be more reactive to temperature and certain foods, which is why cold water or hot coffee may suddenly feel sharp.
Sensitivity tends to be more noticeable if you already have thin enamel, gum recession, worn fillings, or a history of sensitive teeth. Stronger gels and longer wear times can also increase the chance of discomfort.

Choose a toothpaste made for sensitive teeth and use it for several days before whitening, then keep using it afterward. Many formulas rely on ingredients such as potassium nitrate, which helps calm the nerve response over time.
For an extra boost, you can smear a thin layer on the sensitive areas for a minute before rinsing (unless the label says otherwise). If you’re whitening with trays, ask your dentist whether a desensitizing gel is a good fit for you.
Right after whitening, stick to lukewarm foods and drinks and keep acidic items to a minimum. Citrus, soda, vinegar-based dressings, and very spicy foods can irritate teeth that are already on edge.
This is also the window when teeth can re-stain more easily. If you can, choose lighter-colored options (water, milk, plain yogurt, rice, eggs, chicken, bananas) until the next day or two.
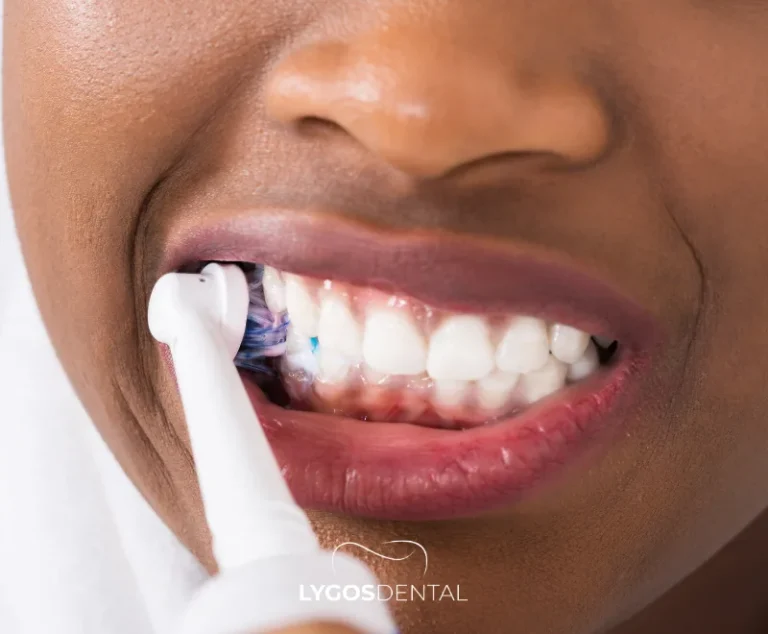
A firm brush and heavy pressure can make sensitivity worse, especially if the gumline is exposed. Use a soft-bristled toothbrush and small circular motions, letting the bristles do the work.
If you floss, do it gently and avoid snapping the floss into the gums. A fluoride toothpaste is a good everyday choice because it supports enamel strength.
Fluoride helps strengthen enamel and can reduce sensitivity for some people. An alcohol-free fluoride mouthwash is often easier to tolerate right after whitening than a strong, minty rinse.
If you’re prone to sensitivity, your dentist may suggest a fluoride or desensitizing gel to use in trays for a short period. This is a common option when you want whitening results without the sting.

Mild sensitivity that fades within a couple of days is common. Pain that keeps getting worse, feels one-sided, or lingers long after a cold drink can signal a problem such as decay, a crack, or gum recession.
Stop whitening and book a dental check if you have strong pain, swelling, or symptoms that last longer than a week. A dentist can apply professional-strength fluoride, protective coatings, or adjust your whitening plan to something gentler.
Most people notice sensitivity for a few hours to a few days. If it isn’t improving after several days, or it’s severe from the start, stop whitening and contact a dentist for advice.
You can eat once you feel comfortable, but avoid very hot, cold, and acidic foods right away. For the first 24–48 hours, many dentists also recommend skipping strongly pigmented foods and drinks (coffee, red wine, berries) to protect the new shade.
Some people feel improvement within a few days, but best results usually come from consistent use for at least two weeks. If you’re whitening again later, start the toothpaste a few days before you begin.
No. Sensitivity varies from person to person and depends on enamel thickness, gum recession, existing restorations, and the strength and wear time of the whitening product. If you’ve had sensitivity in the past, a dentist-supervised approach can help you choose a gentler method.