Does Tooth Decay Damage the Heart? | LYGOS DENTAL
Does Tooth Decay Damage the Heart?
Untreated tooth decay can contribute to health problems beyond the mouth. When a cavity progresses to infection, mouth bacteria and inflammation may enter the bloodstream. This is linked to higher cardiovascular risk, and in rare cases can trigger a serious heart infection (endocarditis) in vulnerable patients. Prompt dental treatment and good daily hygiene help lower these risks.
How Tooth Decay Can Affect the Rest of Your Body
A cavity starts when bacteria in dental plaque break down enamel. If decay continues, it can reach the dentin and pulp, where nerves and blood vessels sit. At that stage, the tooth may become infected or develop an abscess.
Infection and gum inflammation make it easier for bacteria to enter the bloodstream. This can happen during everyday activities such as chewing or brushing, especially if the gums bleed easily.
What the Research Suggests About the Heart Connection

Table of Contents
Studies consistently show a link between poor oral health—especially gum disease—and cardiovascular disease. Researchers believe inflammation and short bursts of bacteria in the blood (bacteremia) may play a role. That said, a link does not prove that cavities directly cause heart disease.
Tooth decay matters because it can increase inflammation and, when it turns into a deep infection, it may raise the chance of bacteria reaching the bloodstream. For most healthy people, this is unlikely to cause a heart problem, but it becomes more important if you already have certain heart conditions.
Potential Heart-Related Risks Associated With Dental Infections
Systemic Inflammation
Ongoing gum inflammation or untreated dental infection can contribute to higher inflammatory markers in the body. Inflammation is a known factor in cardiovascular disease, so keeping oral inflammation under control is a sensible prevention step.
Infective Endocarditis in High-Risk Patients
Infective endocarditis is a rare but serious infection of the heart’s inner lining or valves. It can occur when bacteria from the mouth enter the bloodstream and attach to damaged heart tissue or artificial valves. People with specific cardiac conditions may need special precautions before certain dental procedures.
Worsening of Existing Cardiovascular Risk Factors
Oral health problems often cluster with other risk factors such as smoking, diabetes, and limited access to preventive care. Treating decay and gum disease won’t replace medical care for heart disease, but it supports overall health and can reduce one avoidable source of inflammation.
Signs a Cavity or Tooth Infection Needs Urgent Care
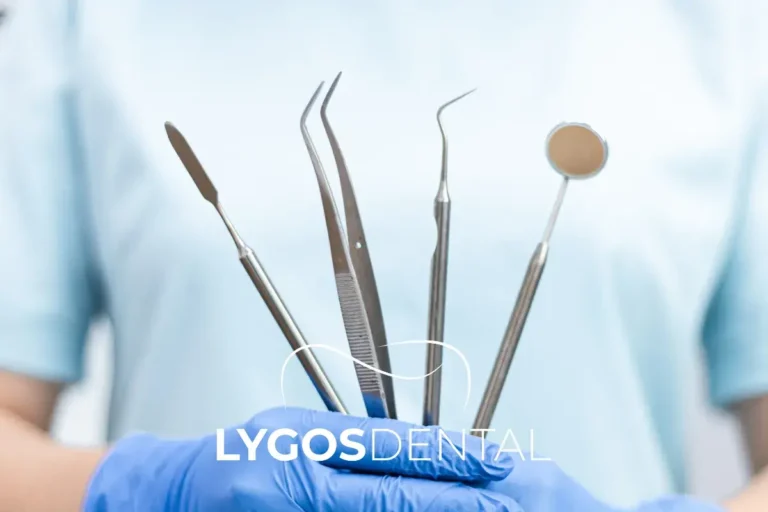
Contact a dentist promptly if you notice any of the following:
- Toothache that lasts more than a day or worsens
- Swelling of the gums, face, or jaw
- Pus, a bad taste, or persistent bad breath
- Fever, fatigue, or feeling unwell alongside dental pain
- Pain when biting or difficulty chewing
Who Is at Higher Risk of Heart Complications?
Extra caution is recommended if you have:
- A prosthetic heart valve or a history of infective endocarditis
- Certain congenital heart conditions (your cardiologist can confirm)
- A weakened immune system (for example, from medication or illness)
- Diabetes that is difficult to control
- Moderate to severe gum disease
How to Protect Your Teeth and Support Heart Health
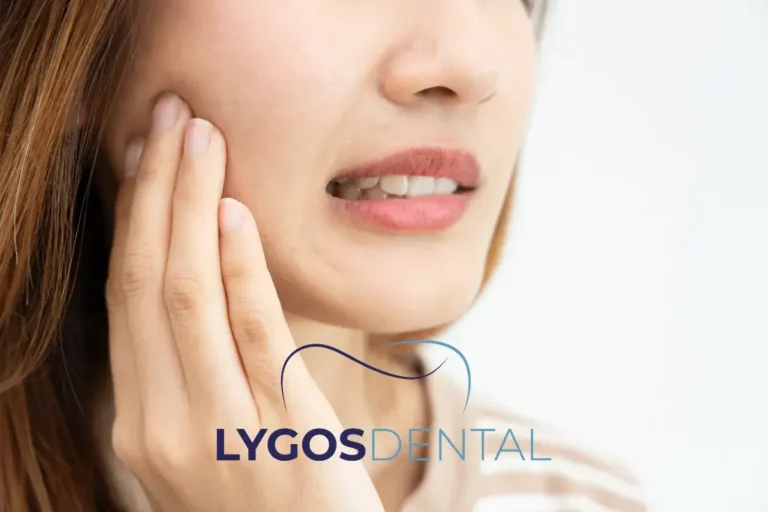
Treat Cavities Early
A filling or crown can stop decay from progressing and reduce the chance of infection. If you have swelling or severe pain, you may need urgent treatment for an abscess.
Keep Daily Oral Care Simple and Consistent
Brush twice a day with fluoride toothpaste, clean between your teeth daily (floss or interdental brushes), and consider an antiseptic mouthwash if your dentist recommends it.
Get Regular Dental Check-Ups
Routine visits help catch early decay, gum inflammation, and bite issues before they turn into infections. If you have a heart condition, tell your dentist and bring your current medication list.
Support a Low-Inflammation Lifestyle
A balanced diet, less added sugar, not smoking, and managing conditions like diabetes protect both oral health and the cardiovascular system.
When to See a Dentist
Book an appointment if you suspect a cavity, have sensitivity that persists, or notice gum bleeding. If you have a high-risk heart condition and need dental work, ask your cardiologist and dentist whether antibiotic precautions are appropriate for you.
At Lygos Dental, we provide modern diagnostic tests, comfortable treatment options, and personalized care plans to help protect your oral health.
Key Takeaway
Tooth decay doesn’t automatically lead to heart disease, but untreated cavities can progress to infection and add to inflammation in the body. Good oral hygiene, timely dental treatment, and coordination with your cardiologist (when needed) are practical steps to reduce avoidable risks.
Get Information Now
You can contact us to learn more about Cosmetic Dentistry, Dental Crown, Dental Implant, and General Dentistry, to make an appointment, or to ask questions about our services.
Frequently Asked Questions
Can a tooth decay be fixed?
Yes, early decay can remineralize; cavities require fillings or crowns.
What is the main cause of tooth decay?
Bacterial acids from sugar breakdown erode enamel and dentin.
What are the 5 stages of tooth decay?
Demineralization, enamel decay, dentin decay, pulp infection, and abscess formation.
When is it too late to stop tooth decay?
It’s too late once decay reaches pulp causing irreversible infection or collapse.
Is tooth decay your fault?
No, decay isn’t solely your fault; biology, diet, habits, and access contribute.
How painful is tooth decay?
Pain ranges from none early to severe, throbbing pain in advanced decay
Cracked Tooth Syndrome | LYGOS DENTAL
Cracked Tooth Syndrome
Cracked tooth syndrome is a small fracture in a tooth that can trigger sharp pain when you bite, especially on release, along with hot/cold sensitivity. Cracks are often hard to spot on X-rays, so diagnosis relies on a careful dental exam. Treatment ranges from bonding or crowns to root canal therapy, depending on depth.
Table of Contents
What Cracked Tooth Syndrome Is
Cracked tooth syndrome refers to a crack in the enamel and/or dentin that causes pain or sensitivity but may not be visible to the naked eye. Because the crack can open slightly under pressure, you may feel a sharp, fleeting pain while chewing and then feel fine once the pressure is released.
People often struggle to identify which tooth is responsible, and the symptoms can come and go. Early assessment matters because a small crack can deepen over time and reach the tooth’s nerve (pulp), making treatment more complex.
Common Causes Of A Cracked Tooth

Cracks can develop from repeated stress on the tooth or from a single traumatic event. Common triggers include:
- Teeth grinding or clenching (bruxism): Night-time clenching can create microcracks that slowly widen.
- Biting hard foods or objects: Ice, hard candy, unpopped popcorn kernels, and nut shells can overload enamel.
- Large fillings or restorations: Teeth with extensive restorations may be weaker and more prone to cracking.
- Trauma or impact: A blow to the face or a sports injury can cause a crack that becomes symptomatic later.
- Sudden temperature changes: Very hot then very cold foods/drinks may stress enamel, especially when a tooth is already weakened.
- Age and normal wear: Cracks are reported more often in adults, as enamel naturally wears and teeth accumulate stress over time.
Symptoms Of Cracked Tooth Syndrome
Symptoms can be intermittent, which is why this condition is sometimes missed at first. The most common signs include:
- Sharp pain when chewing — Often felt when you bite down or as you release pressure.
- Sensitivity to hot or cold — The tooth may twinge with temperature changes.
- Sweet sensitivity — Sugary foods can trigger a quick sting.
- Pain that’s hard to localize — Discomfort may feel like it’s coming from a general area rather than one specific tooth.
- Pressure discomfort — As the crack progresses, the tooth may feel “off” when biting.
How Dentists Diagnose A Cracked Tooth
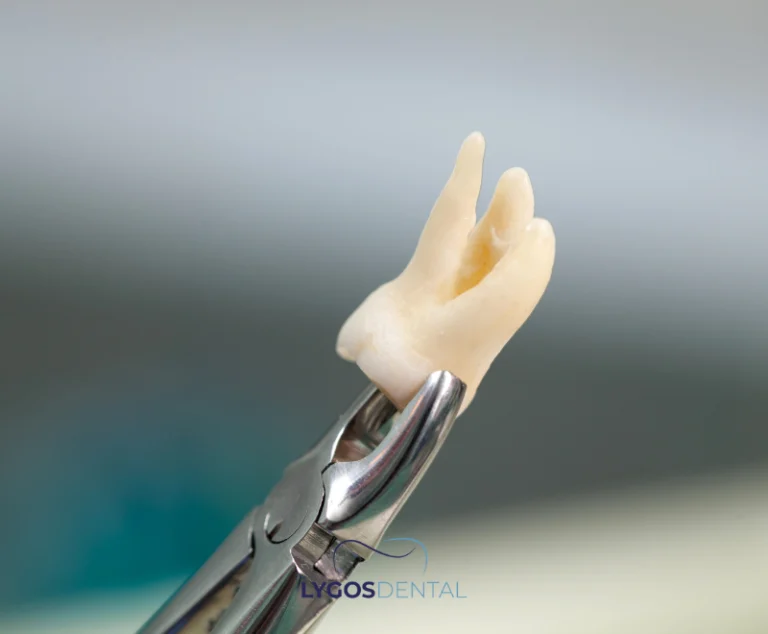
A dental exam is essential because fine cracks may not appear on standard X-rays. Your dentist may use a bite test, special lighting (transillumination), staining, magnification, or periodontal probing to locate the crack and assess its depth.
If symptoms suggest the crack may extend deeper, additional imaging may be recommended to evaluate the tooth and surrounding bone. Diagnosis also includes ruling out other causes of bite pain, such as high fillings, gum inflammation, or tooth decay.
Treatment Options
Treatment depends on where the crack sits, how deep it is, and whether the tooth’s nerve is affected. Your dentist will recommend the least invasive option that protects the tooth and prevents the crack from spreading.
- Bonding or a small filling: For minor surface cracks, bonding can help seal and strengthen the affected area.
- Onlay or crown: When the tooth needs reinforcement, an onlay or crown can hold the tooth together and reduce flexing during chewing.
- Root canal treatment (if the pulp is involved): If the crack reaches the nerve, root canal therapy may be needed, typically followed by a crown to protect the tooth.
- Bite adjustment: In some cases, reshaping a high spot helps reduce pressure on the cracked area.
- Night guard for bruxism: A custom night guard reduces grinding forces and supports long-term protection.
- Extraction (last resort): If the crack extends into the root and the tooth cannot be restored, warning signs may include persistent pain, deep probing, or repeated infection.
Can Cracked Teeth Be Prevented?

You can’t prevent every crack, but these habits can lower your risk:
- Wear a dentist-recommended night guard if you grind or clench your teeth.
- Avoid chewing ice, hard candy, and other hard objects that can overload teeth.
- Don’t use your teeth as tools (opening packages, cracking shells, holding objects).
- Keep up with regular dental checkups so small issues are caught early.
- Support enamel health with a balanced diet that includes calcium and vitamin D.
What Happens If A Cracked Tooth Is Not Treated?
Leaving a crack untreated increases the chance it will spread. Possible outcomes include:
- A larger fracture that shows up suddenly while chewing
- Infection of the pulp and development of an abscess
- A need for more involved treatment, such as root canal therapy and a crown
- Tooth loss if the crack becomes non-restorable
- Jaw discomfort or wear on other teeth if you start chewing on one side
When To See A Dentist
Book an appointment if you notice sharp pain on biting, recurring sensitivity to temperature or sweets, or pain that comes and goes. These symptoms can overlap with other conditions, so an exam is the safest way to identify the cause and protect the tooth.
FAQ
How is cracked tooth syndrome treated?
Crown/onlay to splint; bond minor cracks; root canal if pulp involvement.
How can cracked teeth be repaired naturally?
Cracked teeth can’t be repaired naturally; only temporary protection and prompt dental care help.
Why do cracked teeth hurt so much?
Crack flexing irritates dentin/pulp, causing sharp bite pain and cold sensitivity.
What are the clinical features of cracked tooth syndrome?
Pain on biting/release, cold sensitivity, sometimes sweet sensitivity; vitality tests usually positive.
Is cracked tooth syndrome a dental emergency?
Yes—treat as urgent; early evaluation prevents crack propagation, infection, and tooth loss.
Does cracked tooth syndrome require root canal treatment?
Only if the crack inflames/infects pulp; otherwise crown/onlay or bonding may suffice.
How is cracked tooth syndrome tested?
Bite test, transillumination, probing, and vitality tests; X-rays often miss cracks.
What deficiency causes cracked teeth?
Vitamin D deficiency can weaken mineralization; vitamin A deficiency is also linked to brittleness.
