How Do Gum Diseases Affect Heart Health?
How Do Gum Diseases Affect Heart Health?
Gum disease (especially periodontitis) is associated with a higher risk of cardiovascular problems. The likely link is shared inflammation: infected gums can raise inflammatory markers and allow oral bacteria into the bloodstream, which may affect blood vessels. Research shows an association, but it has not proven that gum disease directly causes heart disease.
The Short Answer: What The Research Shows
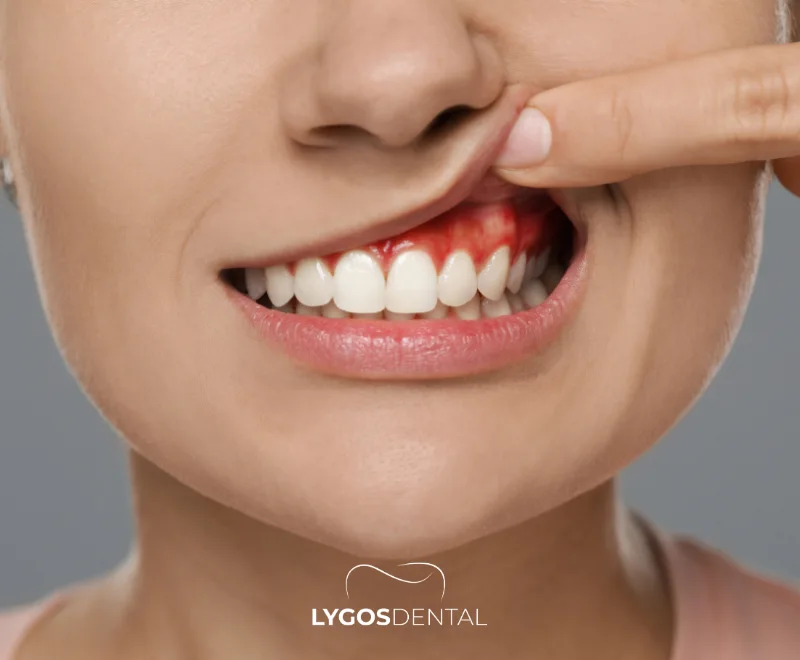
Large studies and expert reviews consistently find an association between periodontitis and atherosclerotic cardiovascular disease (ASCVD), such as coronary artery disease and stroke. That said, association is not the same as causation. Gum disease and heart disease share major risk factors—smoking, diabetes, aging, and socioeconomic factors—so researchers cannot yet say gum disease alone causes heart events.
What Counts As Gum Disease?
Gum disease is an infection and inflammation of the tissues that hold your teeth in place. It typically progresses in stages:
- Gingivitis: Mild inflammation with redness, swelling, and bleeding. It’s often reversible with consistent plaque control and professional cleaning.
- Periodontitis: Deeper infection that damages the gum attachment and supporting bone. Untreated, it can lead to loose teeth and tooth loss.
How Gum Disease May Affect The Heart
Researchers focus on a few biologically plausible pathways. These pathways help explain the association, even though they don’t prove direct cause-and-effect.
1) Systemic inflammation
Periodontitis is a chronic inflammatory condition. Chronic inflammation is also central to atherosclerosis, the process that drives plaque build-up in arteries. When gum inflammation persists, inflammatory signals can spill over into the bloodstream and add to the body’s overall inflammatory burden.
2) Bacteria entering the bloodstream
Everyday actions like brushing or chewing can allow bacteria from infected gums to enter the bloodstream, especially when gums bleed. Oral bacteria and their by-products can then interact with blood vessel walls, potentially contributing to endothelial dysfunction (a key early step in vascular disease).
3) Immune and clotting effects
Chronic infection can keep the immune system activated. Some studies suggest links between periodontitis and changes in platelet function and clotting tendencies, which matters because clots are involved in heart attacks and many strokes.
Does Gum Disease Cause Heart Attacks?
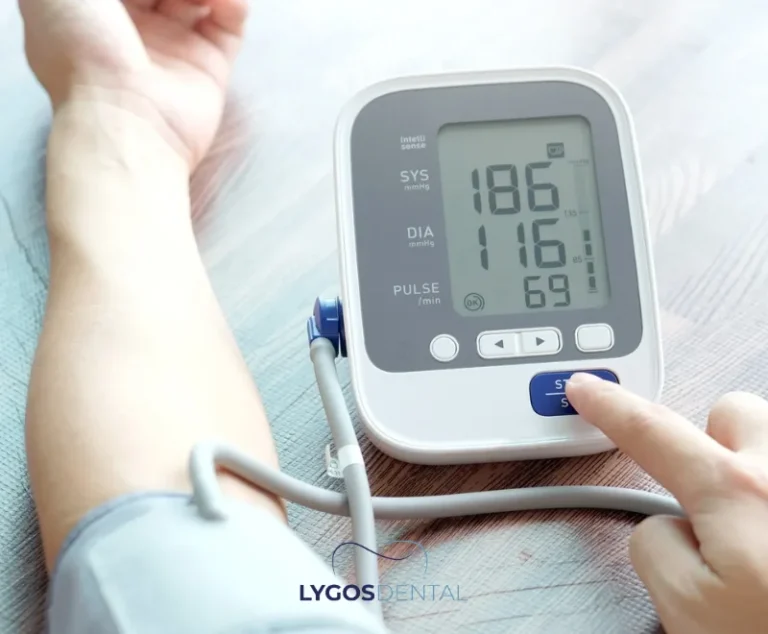
Current evidence supports a relationship, not a guarantee. People with periodontitis tend to have higher rates of heart attack and stroke in observational research, but this does not prove gum disease is the direct trigger. Treating gum disease improves oral health and may lower inflammation, yet clinical trials have not consistently shown a reduction in heart attacks or strokes from dental treatment alone.
Who Should Take This Link Most Seriously?
Everyone benefits from healthy gums, but these groups should be especially proactive:
- People with diabetes, prediabetes, or metabolic syndrome.
- Smokers and former smokers.
- Adults over 40, especially with a history of gum problems.
- Anyone with known heart or vascular disease, high blood pressure, or high cholesterol.
- People with limited access to regular dental care.
Warning Signs You Shouldn’t Ignore
Gum disease can be painless until it becomes advanced. Common signs include:
- Bleeding when brushing or flossing.
- Red, swollen, or tender gums.
- Persistent bad breath or a bad taste.
- Gum recession or teeth that look “longer.”
- Loose teeth or changes in bite.
How To Protect Your Gums And Support Heart Health
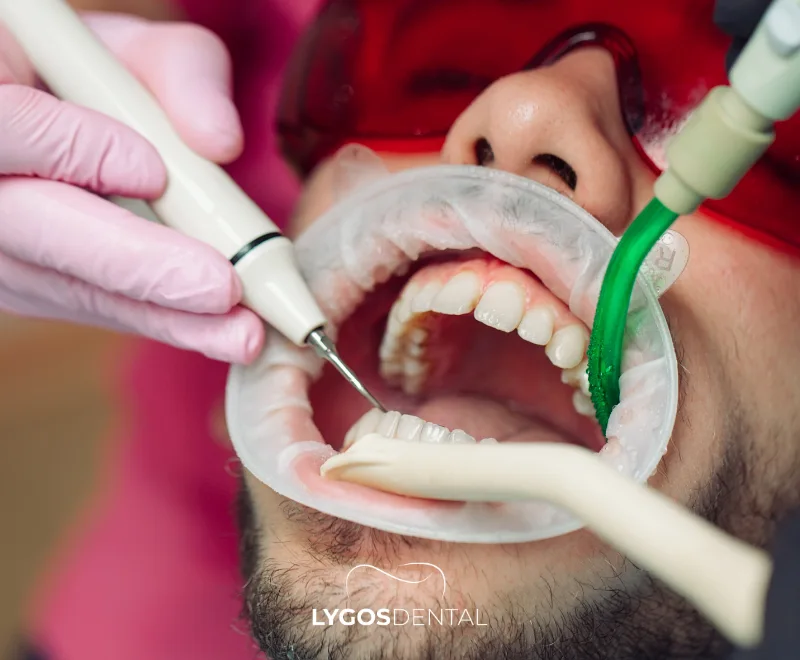
Oral care should be part of your broader cardiovascular risk plan. Practical steps:
Daily habits
- Brush twice daily with fluoride toothpaste and a soft-bristled brush.
- Clean between teeth daily (floss or interdental brushes).
- If you have bridges, implants, or orthodontic appliances, use the tools your dentist recommends.
Professional care
- Schedule routine dental checkups and cleanings based on your dentist’s advice.
- If you have gum pockets or a history of periodontitis, ask about periodontal monitoring and maintenance visits.
Lifestyle and medical factors
- Stop smoking—this is one of the biggest shared risk factors for gum and heart disease.
- Keep diabetes and blood pressure well controlled; poor control worsens gum inflammation.
- Aim for a balanced diet with limited added sugars; frequent sugar exposure feeds plaque bacteria.
A Note About Endocarditis Risk
A small subset of people are at increased risk of infective endocarditis (an infection of the heart lining or valves). For these patients, dentists may recommend specific precautions. If you have a prosthetic heart valve, certain congenital heart conditions, or a history of endocarditis, tell your dentist and cardiologist so they can align on the right plan.
Frequently Asked Questions
Do bleeding gums mean I have heart disease?
No. Bleeding gums most often point to gingivitis or periodontitis. It’s a sign to book a dental visit, and it’s also a reminder to review shared risk factors like smoking and diabetes.
Can better oral hygiene lower heart risk?
Good oral hygiene helps reduce gum inflammation and infection. While it’s not a substitute for managing blood pressure, cholesterol, or diabetes, it’s a sensible part of an overall prevention plan.
If I have heart disease, should I see a dentist more often?
Many people with heart disease benefit from consistent preventive care, especially if they have gum problems. Your dentist can recommend a schedule based on your periodontal status and medications.
