Infection Risks After Dental Implants | LYGOS DENTAL
Infection Risks After Dental Implants
Infection after a dental implant usually starts with inflammation of the gum around the implant and can progress to bone loss (peri-implantitis) if ignored. Early signs include increasing pain, swelling, bleeding, bad taste or odor, or pus. Prompt dental care and good home hygiene often stop the problem before the implant is affected.
Dental implants are a reliable way to replace missing teeth, but they still require surgical healing. Like any oral surgery, an implant site can become infected if bacteria build up or the tissues struggle to heal. Knowing what to watch for helps you act early and protect your results.
Table of Contents
What Is A Dental Implant Infection?
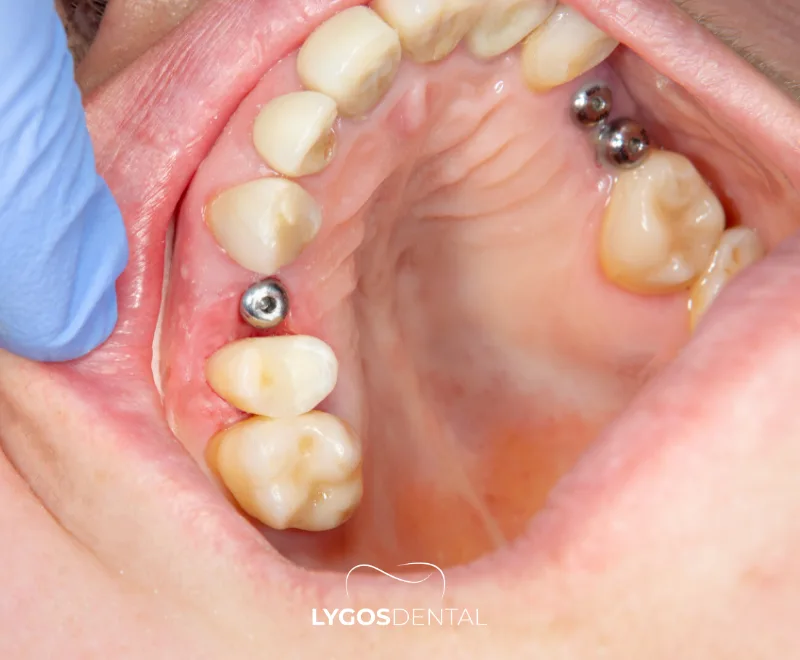
A dental implant infection is inflammation caused by bacteria around an implant. It may involve only the gum tissue (peri-implant mucositis) or, in more advanced cases, the deeper tissues and supporting bone (peri-implantitis). When bone is affected, the implant can loosen over time.
Early Signs And Symptoms
Some soreness is expected after surgery, especially in the first few days. Concern rises when symptoms worsen instead of improving, or when new symptoms appear after the initial healing period.
- Increasing or persistent pain and tenderness around the implant
- Redness, swelling, or bleeding of the gum near the implant
- Bad taste, bad breath, or a feeling of pressure in the area
- Pus (discharge) around the implant or under the gum
- Fever, fatigue, or swollen glands (less common, but urgent when present)
If you notice pus, fever, or rapidly increasing swelling, contact your dentist as soon as possible. These can signal an infection that needs prompt treatment.
Common Causes

Implant infections are usually linked to bacterial biofilm (plaque) accumulating at the gumline or under the gum. Several factors can make this more likely.
- Oral hygiene gaps that allow plaque to collect around the implant or restoration
- Smoking or vaping, which reduces blood flow and slows healing
- Uncontrolled diabetes or other conditions that affect immune response
- Poor fit of a crown or bridge that traps food and makes cleaning difficult
- Early disruption of the healing site (for example, chewing hard foods too soon)
- Incomplete or inappropriate use of prescribed antibiotics (when they are indicated)
Risk Factors That Raise The Chance Of Infection
Some patients are more prone to peri-implant disease. Your dentist may adjust your aftercare plan if any of the following apply.
- Smoking or heavy alcohol use
- A history of gum disease (periodontitis)
- Diabetes that is not well controlled
- Medications or medical conditions that suppress immunity
- High stress, poor sleep, or nutrition that can slow recovery
- Irregular dental maintenance visits after the implant is placed
How Dentists Diagnose An Implant Infection

Diagnosis usually starts with a clinical exam of the gum around the implant. Your dentist may check for bleeding, swelling, pus, and pocket depth around the implant. X-rays can help assess bone levels and rule out other causes of pain.
Treatment Options
Treatment depends on how early the problem is caught. The main goals are to remove bacteria, reduce inflammation, and protect the surrounding bone.
- Professional cleaning and debridement around the implant to remove plaque and hardened deposits
- Antiseptic mouth rinses, such as chlorhexidine, when recommended by your dentist
- Antibiotics when a bacterial infection is confirmed or strongly suspected (your dentist will choose the right option)
- Adjusting the crown or bite if the restoration is trapping plaque or causing excess pressure
- Surgical cleaning and regeneration procedures for advanced peri-implantitis, when needed
Self-treating with leftover antibiotics is risky and can delay proper care. Always follow your dentist’s instructions.
Home Care While You Arrange A Dental Visit
If you suspect an infection, home care can reduce irritation, but it cannot replace professional treatment. Use gentle brushing, keep the area clean, and avoid smoking.
- Rinse gently with warm salt water (avoid aggressive swishing right after surgery)
- Brush carefully with a soft toothbrush and clean between teeth as advised
- Stick to softer foods and avoid chewing directly on the implant area
- Take pain relief only as recommended by your dentist or pharmacist
- Call the clinic urgently if you develop fever, spreading swelling, or trouble swallowing
What Happens If An Implant Infection Is Left Untreated?
When inflammation persists, it can lead to progressive bone loss around the implant (peri-implantitis). Over time, this may reduce support and increase the risk of implant failure. In rare cases, oral infections can spread beyond the mouth and become a wider health issue.
- Ongoing discomfort and swelling
- Bone loss around the implant and gum recession
- Loosening or loss of the implant
- More complex treatment and longer healing time if re-implantation is needed
How To Reduce Infection Risk After Implant Surgery
Most problems are preventable with consistent aftercare and maintenance. Your dentist may tailor advice based on your health history and the type of restoration placed.
- Follow post-op instructions closely, especially in the first 1–2 weeks
- Brush twice daily and clean between teeth with the tools recommended for implants
- Attend follow-up visits so early inflammation is spotted before bone is affected
- Stop smoking before surgery and avoid nicotine during healing
- Manage chronic conditions such as diabetes with your medical team
- Schedule professional implant maintenance cleanings as advised
Book An Appointment
If you think you may have an implant infection—or you want a preventive check—contact our clinic to arrange an appointment. We provide cosmetic dentistry, crowns, dental implants, and general dentistry services.
FAQ
How common is infection after dental implants?
Early infection is uncommon (around 1–5%); peri-implantitis affects about 10% of implants.
What is the 3/2 rule for dental implants?
Place the implant 3 mm apical and 2 mm palatal to the planned crown.
What are the early signs of implant infection?
Pain, swelling, redness, pus/bad taste, bleeding, and increasing tenderness around the implant.
What is the most common complication of dental implants?
Peri-implant mucositis is the most common complication, causing reversible gum inflammation.
What are the disadvantages of dental implants?
Surgery, higher cost, healing time, possible failure, and peri-implantitis are major disadvantages.
