The Impact of Rheumatic Diseases on Oral Health | LYGOS DENTAL
The Impact of Rheumatic Diseases on Oral Health
Rheumatic diseases can increase gum inflammation, dry mouth, jaw pain, and the risk of tooth loss. The same oral infections—especially periodontitis—may also raise systemic inflammation and aggravate autoimmune disease activity. With daily plaque control, dry-mouth prevention, and coordinated dental–rheumatology care, most patients can protect their teeth and comfort.
What Rheumatic Diseases Are
Rheumatic diseases are often driven by an overactive immune response that causes ongoing inflammation. Depending on the diagnosis, inflammation may involve joints, connective tissue, blood vessels, and internal organs. Common examples include:
- Rheumatoid arthritis (RA)
- Ankylosing spondylitis
- Systemic lupus erythematosus (SLE)
- Sjögren’s syndrome
- Psoriatic arthritis
- Scleroderma
Oral symptoms vary by condition and by treatment plan. Even when the mouth feels “fine,” low-grade gum inflammation or dry mouth can quietly raise the risk of decay and tooth loss over time.
Common Oral And Dental Problems In Rheumatic Diseases
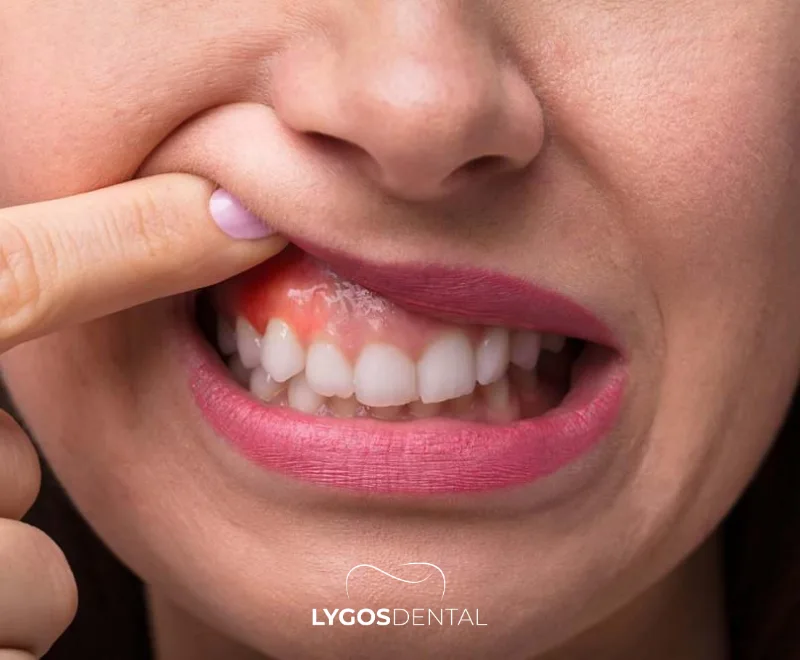
People living with rheumatic disease may find oral hygiene harder during flares, especially if hand or wrist pain limits brushing and flossing. Some medications can also change the mouth’s natural balance of saliva and microbes. Common issues include:
- Gingivitis and periodontitis (gum disease)
- Dry mouth (xerostomia), especially with Sjögren’s syndrome
- Mouth ulcers and sore spots
- Tooth sensitivity, higher cavity risk, and tooth loss
- Jaw discomfort or limited opening (TMJ symptoms)
These problems can affect nutrition, sleep, and confidence. They also deserve attention because untreated gum disease can contribute to systemic inflammation.
How Rheumatoid Arthritis Can Affect Oral Health
Jaw Joint Symptoms
RA can involve the temporomandibular joint (TMJ), which helps the mouth open and close. Inflammation in this joint may cause aching, stiffness, clicking, or difficulty opening wide. During flares, chewing tougher foods can become uncomfortable.
Gum Inflammation And Tooth Loss Risk
Research shows higher rates of periodontitis in people with RA compared with the general population. Gum disease can progress faster when inflammation is uncontrolled or when daily plaque removal is difficult. Over time, advanced periodontitis can lead to loosening teeth and tooth loss.
Can Gum Disease Worsen Rheumatism?
The relationship can work both ways. Periodontitis is a chronic infection and inflammation of the tissues that support the teeth, and it can raise inflammatory markers throughout the body. In RA, periodontal bacteria and the immune response they trigger are being studied for their potential role in increasing disease activity.
For some patients, treating gum disease may help reduce the overall inflammatory burden. It is not a replacement for rheumatology care, but it can support better disease control and may improve comfort in the mouth.
Oral Care Tips For People With Rheumatic Diseases
Small changes to daily routines can make oral care more comfortable and more effective. Aim for consistency rather than perfection, especially during flares.
Daily Habits
- Brush twice daily with a soft-bristled or electric toothbrush. If grip is painful, try a larger handle or a foam grip.
- Clean between teeth daily using floss, floss holders, or interdental brushes—choose what you can use comfortably.
- Use a fluoride toothpaste. If you have frequent cavities, ask your dentist about a higher-fluoride option.
- Rinse after meals with water. If recommended by your dentist, use an antibacterial mouth rinse.
Managing Dry Mouth
- Sip water regularly and limit sugary drinks.
- Use sugar-free gum or lozenges (often xylitol-based) to stimulate saliva.
- Consider saliva substitutes or moisturizing gels before bed.
- Avoid tobacco and alcohol-based mouthwashes, which can worsen dryness.
Dental Visits
Plan routine dental checkups at least every six months, or more often if you have active gum disease or severe dry mouth. Let your dental team know your diagnosis, current medications, and any recent changes in treatment.
Oral And Dental Health During Rheumatic Treatment
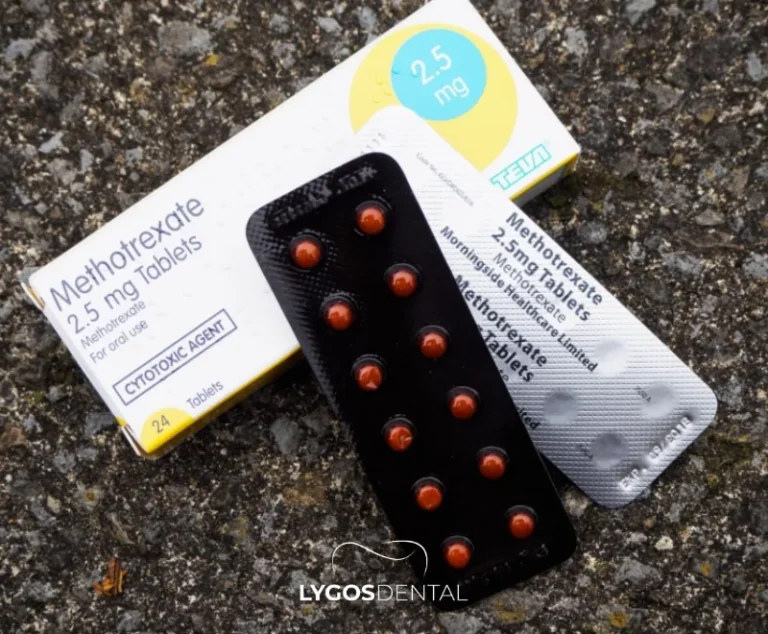
Many rheumatic medications reduce inflammation by calming the immune system. That benefit can come with oral side effects, so it helps to spot problems early and address them promptly.
- Immunosuppressive and biologic therapies can increase the likelihood of oral infections, including fungal infections (thrush).
- Corticosteroids may increase sensitivity and can contribute to oral infections, especially with long-term use.
- Methotrexate can sometimes cause mouth soreness or ulcers, particularly if dosing mistakes occur or folate support is inadequate.
Before any invasive dental procedure, tell your dentist about your medications and your rheumatologist’s contact details. Dental and rheumatology teams can coordinate the safest timing for procedures and decide whether any medication adjustments are needed.
When To Seek Advice
Contact a dentist or clinician if you notice any of the following:
- Bleeding gums that persist despite gentle daily cleaning
- Painful swelling, pus, or a bad taste that does not go away
- Mouth ulcers that last longer than two weeks
- Severe dry mouth with new cavities, burning, or difficulty swallowing
- Jaw pain or limited opening that affects eating
Book An Appointment
If you are managing a rheumatic condition and have concerns about gum health, dry mouth, or jaw discomfort, a dental assessment can help clarify the cause and prevent avoidable complications. Contact us to book an appointment for cosmetic dentistry, crowns, implants, or general dentistry services.
Frequently Asked Questions
Do rheumatic diseases cause gum disease?
They can increase the risk. Chronic inflammation, dry mouth, and difficulty with brushing or flossing during flares can make gingivitis and periodontitis more likely. Early dental care and consistent plaque control reduce the chances of progression.
How can I minimize oral problems if I have a rheumatic disease?
Focus on daily plaque removal, fluoride protection, and dry-mouth prevention. Keep regular dental visits and tell your dentist about medication changes, flares, and any new mouth symptoms so issues are treated early.
Can gum disease worsen rheumatism?
Gum disease can raise systemic inflammation, which may aggravate inflammatory conditions in some people. Treating periodontitis helps reduce the inflammatory burden and supports overall health, alongside medical treatment.
What toothpaste is best for people with dry mouth or sensitive gums?
A fluoride toothpaste is a solid baseline. If you have sensitivity, choose a sensitivity-focused fluoride toothpaste. For significant dry mouth, ask your dentist about remineralizing products, higher-fluoride toothpaste, and moisturizing formulations designed for xerostomia.
