Use of Stem Cells in Dental Treatments | LYGOS DENTAL
Use of Stem Cells in Dental Treatments
Stem cells are being studied in dentistry for their potential to support tissue repair—especially in the dental pulp, gums (periodontium), and jawbone. Some approaches have reached early clinical use in carefully selected cases, while others—such as growing a brand‑new tooth—remain experimental and largely limited to animal research.
Table of Contents
What Stem Cells Are and Why They Matter in Dentistry
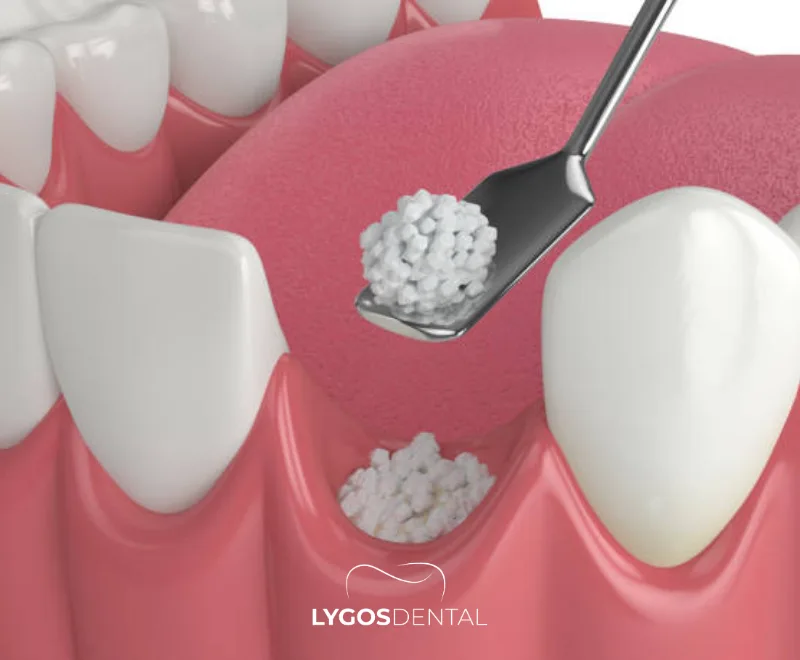
Stem cells are cells that can self‑renew and, under the right conditions, develop into more specialized cell types. In regenerative dentistry, researchers focus mainly on mesenchymal stem cells (MSCs), including dental‑origin stem cells found in tissues such as dental pulp, periodontal ligament, and exfoliated (baby) teeth.
The goal is not to “fill” or “replace” tissue in the classic sense, but to encourage the body to rebuild damaged structures—often with the help of biomaterials (scaffolds) and signaling molecules that guide the healing process.
Where Stem Cell‑Based Approaches Are Being Explored Today
Pulp and Root Canal‑Related Regeneration
When the dental pulp is severely inflamed or infected, conventional root canal treatment removes the diseased tissue and seals the canal. Regenerative endodontics aims to restore living tissue inside the tooth so it can regain some biological function.
Dental pulp stem cells (DPSCs) and stem cells from exfoliated deciduous teeth (often called SHED) have been widely studied for this purpose. The strongest evidence today sits in early clinical research and controlled clinical trials, but protocols are still being refined and are not yet routine in everyday practice.
Gum, Periodontal Ligament, and Bone Regeneration
Periodontitis can destroy the periodontal ligament and the bone supporting the teeth. Conventional periodontal therapy can control infection and slow progression, yet complete regeneration of lost structures is difficult.
Stem cell‑based tissue engineering is being investigated for periodontal bony defects and advanced periodontal disease. Recent reviews and clinical research report promising improvements in certain outcomes, but results vary by defect type, cell source, delivery method, and patient factors.
Scaffolds, Biomaterials, and Growth‑Factor Support
Stem cells rarely work alone. Many regenerative protocols combine cells with biocompatible scaffolds that help the cells attach and organize, plus biological signals that nudge them toward forming the right tissue.
In clinical dentistry, blood‑derived concentrates such as PRP (platelet‑rich plasma) and PRF (platelet‑rich fibrin) are sometimes used as adjuncts because they release growth factors over time. These are not the same as stem cell transplantation, but they can support wound healing and regeneration in selected indications.
Can a New Tooth Be Grown from Stem Cells?
Whole‑tooth regeneration is one of the most exciting ideas in regenerative dentistry—and also one of the least mature clinically. Researchers have created tooth‑germ or tooth‑bud‑like structures in the laboratory and achieved tooth‑like formation in animal models.
At the moment, these advances do not translate to routine “grow me a new tooth” treatment for humans. Challenges include reliably forming enamel, controlling shape and eruption, achieving stable nerve and blood supply, and proving long‑term safety. For patients today, implants, bridges, and prosthetics remain the standard options for missing teeth.
Benefits and Limitations Patients Should Know
Potential benefits
- Biologically driven repair: aims to rebuild tissue rather than simply replace it.
- Better integration: regenerated tissue may behave more like natural gum, bone, or pulp compared with synthetic substitutes.
- Inflammation control: MSCs are being studied for their immunomodulatory effects, which may support healing in some contexts.
Limitations and risks
- Not standardized everywhere: many protocols are still evolving, and availability varies by country and clinic.
- Cost and complexity: cell isolation, expansion, and quality control can be expensive and resource‑intensive.
- Time to see results: true tissue regeneration can take weeks to months, and outcomes are not guaranteed.
- Evidence varies by indication: some applications have stronger human data than others; “tooth regrowth” remains experimental.
Stem Cell–Related Dental Treatments in Turkey

Turkey is a well‑known destination for dental care and health tourism. Regenerative dentistry services may include research‑driven stem cell applications in academic settings, as well as more established adjuncts such as PRP/PRF to support soft‑tissue and bone healing.
As with any cell‑ or tissue‑based intervention, regulatory oversight and clinic credentials matter. Patients should ask whether a procedure is part of an approved clinical protocol, what evidence supports the indication, and how the clinic ensures quality and safety (including laboratory standards when cells are processed).
Get More Information
If you’re considering regenerative options—alongside implants, crowns, or periodontal treatment—book a consultation to review your diagnosis, available therapies, and realistic outcomes based on current evidence.
You can contact us to learn more about Cosmetic Dentistry, Dental Crowns, Dental Implants, and General Dentistry, and to arrange an appointment.
FAQ
Application of stem cells in dentistry
Experimental uses include pulp regeneration, periodontal repair, bone regeneration, and tissue-engineered grafts.
Stem cell dental implants cost
No standard cost; stem-cell dental implants aren’t commercially available outside research trials.
Types of dental stem cells
DPSC, SHED, PDLSC, SCAP, DFSC, gingival MSCs, and alveolar bone MSCs.
Where can i get stem cell dental implants
Only in regulated clinical trials at research dental hospitals; routine clinics don’t offer them.
Stem cell tooth regeneration
Not routine; stem cells may regenerate pulp/periodontium, but whole-tooth regrowth remains experimental.
