How Long Do Veneers Last? | LYGOS DENTAL
With proper care and regular checkups, they can last for many years. However, the main question…
Tooth whitening brightens natural teeth using peroxide-based gels that break down stain molecules inside enamel and dentin. Dentist-led treatments and custom take-home trays usually give the most predictable results. Temporary sensitivity is common, and crowns or fillings won’t change colour, so a dental check helps you choose a safe method and a realistic, natural-looking shade.
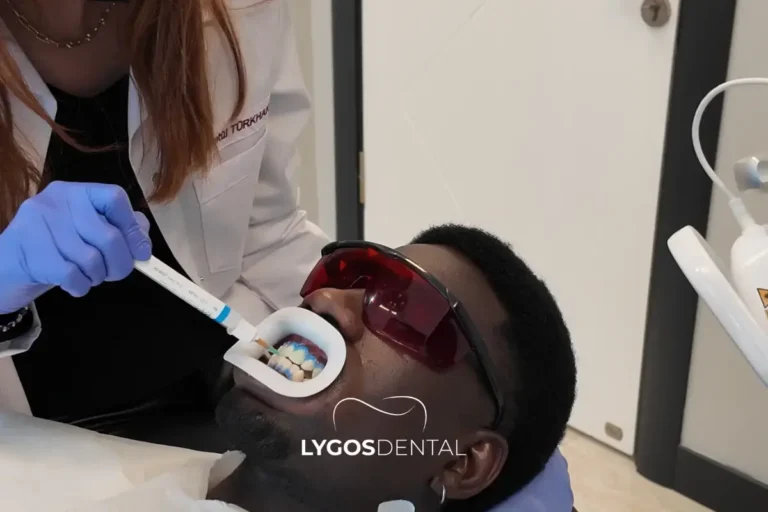
Tooth colour changes for two main reasons: surface stains (for example, coffee, tea, red wine, and smoking) and deeper colour shifts within the tooth. Whitening can improve both, but it only works on natural tooth structure.
Most evidence-based whitening relies on hydrogen peroxide or carbamide peroxide. These agents penetrate enamel and dentin and oxidise stain compounds, which is why they can brighten teeth beyond what most “whitening toothpastes” can achieve.
In-office whitening uses higher-concentration gels with careful gum protection and clinical supervision. The main benefit is speed and close control of soft-tissue safety.
The most common trade-off is sensitivity, often peaking in the first 24–48 hours. If you’re prone to sensitivity, dentists can adjust gel strength, limit exposure time, or use a staged plan rather than pushing for a dramatic change in one visit.
Custom trays with dentist-provided gel are slower than in-office whitening, but results can be very even and easier to fine-tune. Many people prefer this option because they can control day-to-day wear time and stop as soon as the shade looks right.
If your goal is a natural improvement rather than an ultra-bright change, trays are often the most flexible approach.
Whitening strips can work well for mild to moderate staining when used consistently. Results vary more than dentist-supervised options because one-size products don’t account for tooth shape, gum line, existing sensitivity, or restorations.
A practical rule: if a product burns your gums, feels sharp on exposed root areas, or triggers strong sensitivity early, stop using it and get professional advice.
Most “whitening toothpastes” mainly remove surface stains through gentle abrasives and polishing agents. They can make teeth look cleaner and brighter, but they don’t usually change the underlying shade the way peroxide gels can.
They work best as maintenance after whitening, or for people who want small improvements without bleaching.
Light-activated whitening is heavily marketed, but the research is mixed. Some studies show little to no added benefit compared with peroxide alone, while others report faster initial change depending on the gel and protocol.
In practice, diagnosis, gum protection, and a sensible treatment plan usually matter more than whether a lamp is used.
Short-term sensitivity (to cold air or cold drinks) is the most common complaint. It typically settles within a few days.
Desensitising toothpaste, spacing sessions, and choosing a lower-strength plan can help. If you already have sensitivity, whitening may still be possible, but it should be planned around the cause—such as enamel wear, gum recession, cracks, or decay.
Gel that leaks onto the gums can irritate soft tissue. Custom trays and professional barriers reduce this risk.
If your gums turn white briefly during whitening, that’s often a sign of chemical irritation from gel contact and a reminder that fit and application technique matter.
Peroxide whitening, when used as directed, is generally considered safe and effective for healthy adults. Problems usually come from misuse: over-wearing trays, using high-strength gels too often, or stacking multiple products at the same time.
Be cautious with abrasive “hacks.” Charcoal-based products may remove some surface staining, but research has linked many charcoal formulas to increased enamel roughness/abrasion with limited true whitening benefit.
A dental exam is especially important if you have:
Regulations vary by country, but in many places higher-peroxide whitening gels are restricted to dental professionals, and cosmetic whitening for under-18s is generally not permitted.
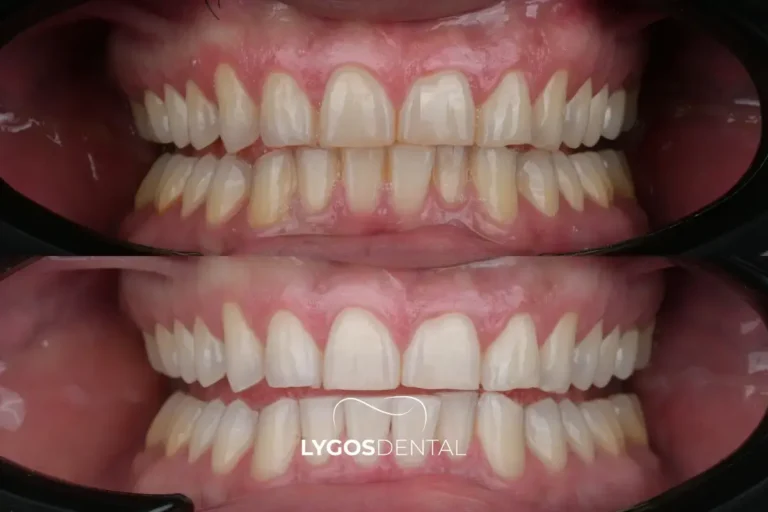
The most believable smiles usually brighten by a few shades rather than a dramatic leap. A dentist can help you choose a target shade that suits your skin tone and avoids the greyish or overly opaque look that can happen when whitening is pushed too far.
Crowns, veneers, bonding, and tooth-coloured fillings do not change colour with whitening. If restorations show when you smile, the usual strategy is to whiten first, then replace or adjust restorations (if needed) to match the new shade.
Longevity depends on habits and maintenance. Coffee, tea, red wine, smoking, and inconsistent brushing shorten results.
Many people maintain their shade with periodic “top-ups” (often using trays) rather than repeating full-strength whitening frequently.
Before you spend money on kits or sessions, make sure you know:
A short dental appointment can prevent weeks of trial-and-error and help you get a result that looks natural.
If you’d like personalised advice, a dentist can check for hidden causes of discolouration, assess sensitivity risk, and recommend a whitening plan that fits your teeth and any visible restorations.
Avoid staining foods and smoking for 24–48 hours; expect temporary sensitivity.
Niacinamide isn’t proven to whiten teeth; use dentist-approved whiteners for predictable results.
Get a dental exam; treat cavities/gum disease; match expectations; plan for sensitivity.
You’ll see teeth lighten a few shades within days; compare photos or shade guide.
Avoid coffee, tea, red wine, tobacco, and dark sauces for 24–48 hours.
Wait about 30 minutes, then brush gently with a soft toothbrush.