What Is the 7–4 Rule and Why Is It Important in Pediatric Dentistry?
So, how does tooth loss affect speech? In this article, we will examine in detail the…
A tooth cyst is a fluid-filled sac that forms near a tooth root or within the jawbone, often after long‑standing infection or around an unerupted tooth. Many cysts cause no symptoms and are found on dental X‑rays. Treatment depends on the type and size and may include root canal therapy, surgical removal, or tooth extraction, followed by monitoring.
Tooth cysts are usually benign, but they can expand over time and damage nearby teeth, bone, or nerves. Because early cysts are often painless, regular dental check-ups and X-rays play a big role in finding them before they cause complications.
A tooth cyst is a closed sac lined by tissue and filled with fluid or semi‑fluid material. It may develop at the tip of a tooth root, around an unerupted tooth, or elsewhere in the jawbone. Some cysts stay small, while others slowly enlarge and weaken the surrounding bone.
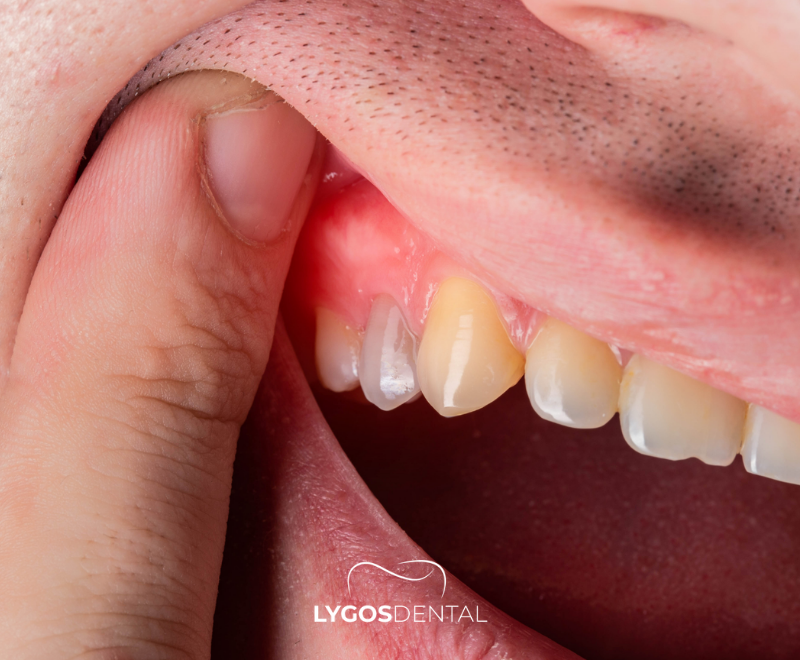
Dentists may use the term “tooth cyst” broadly, but there are different odontogenic (tooth‑related) cysts. The exact diagnosis matters because it affects treatment and follow-up.
Many tooth cysts cause no obvious symptoms until they grow or become infected. When symptoms do appear, they can look similar to other dental problems, so an exam and imaging are important.
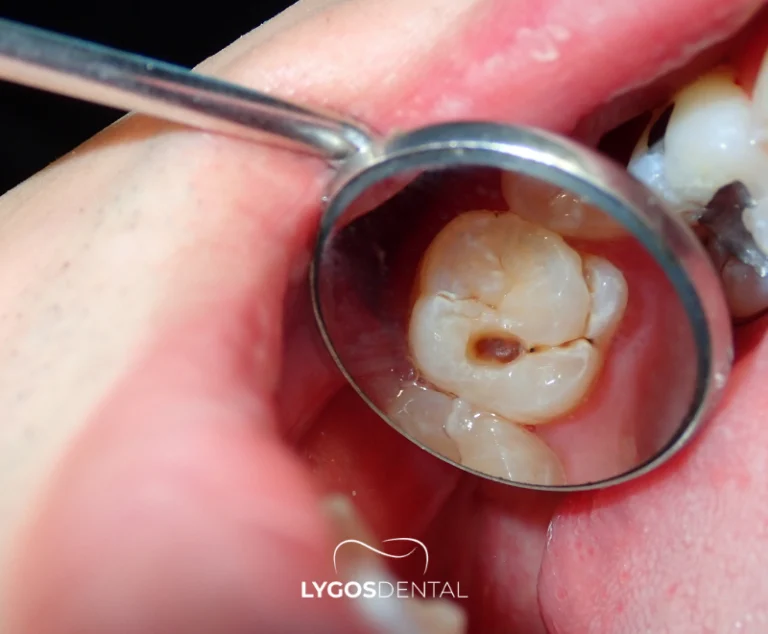
Causes depend on the cyst type, but most are related to infection, inflammation, or tooth development. A dentist may also consider past dental trauma, previous treatment, and how the tooth developed in the jaw.
Treatment is tailored to the cyst’s size, location, and the health of the tooth involved. Your dentist may refer you to an endodontist (root canal specialist) or an oral and maxillofacial surgeon for complex cases.
Most cysts are found on dental X‑rays. Depending on the case, your dentist may use 3D imaging (CBCT) to understand the cyst’s boundaries and its relationship to nearby structures.
If the cyst is associated with an infected tooth, root canal therapy can remove the source of infection. In many cases, addressing the infection allows the surrounding tissue to heal and the lesion to shrink over time.
For larger cysts, true cysts that don’t resolve, or cysts linked to impacted teeth, surgical treatment may be recommended. Options include removing the cyst lining (enucleation) or reducing its size first (decompression or marsupialization) to lower surgical risk.
If the tooth is severely damaged or cannot be predictably restored, extraction may be the safest option. Your dentist can discuss replacement options such as an implant, bridge, or denture once healing is complete.
Antibiotics may be prescribed if there are signs of spreading infection, but they don’t remove the cyst itself. Pain relief medications and mouth rinses may also be used as part of your short‑term care plan.

Recovery varies based on the size of the cyst and the procedure performed. Most people can return to normal routines quickly, but full bone healing may take longer.
Not every tooth cyst can be prevented, especially developmental cysts. Still, you can lower your risk by reducing infections and catching problems early.
Pulp infection or impacted teeth trigger cysts from inflammation around tooth roots.
Treatment includes root canal or extraction plus surgical removal; antibiotics if infected.
Most dental cysts don’t disappear alone; they usually need dental treatment.
Often painless; may cause swelling, pressure, tenderness, or a draining salty taste.
Yes; untreated cysts can destroy jawbone, loosen teeth, and cause recurrent infections.
Removal is usually painless under anesthesia, with mild-to-moderate soreness afterward.