Benito Antonio Dental Aesthetics | LYGOS DENTAL
In the world of entertainment, Benito Antonio has become more than just a music icon, he…
Apical resection (apicoectomy) is a minor dental surgery that removes infected tissue and a small portion of the root tip when a tooth still has inflammation after root canal treatment. By sealing the end of the root and clearing the infection, the procedure can preserve the natural tooth and protect nearby bone and gums.
Meta Title: Apical Resection (Apicoectomy): What It Is, When It’s Needed, and Recovery
Meta Description: Learn what apical resection (apicoectomy) is, why it’s done after a failed root canal, how the surgery works, key benefits and risks, and what to expect during recovery and follow-up care.
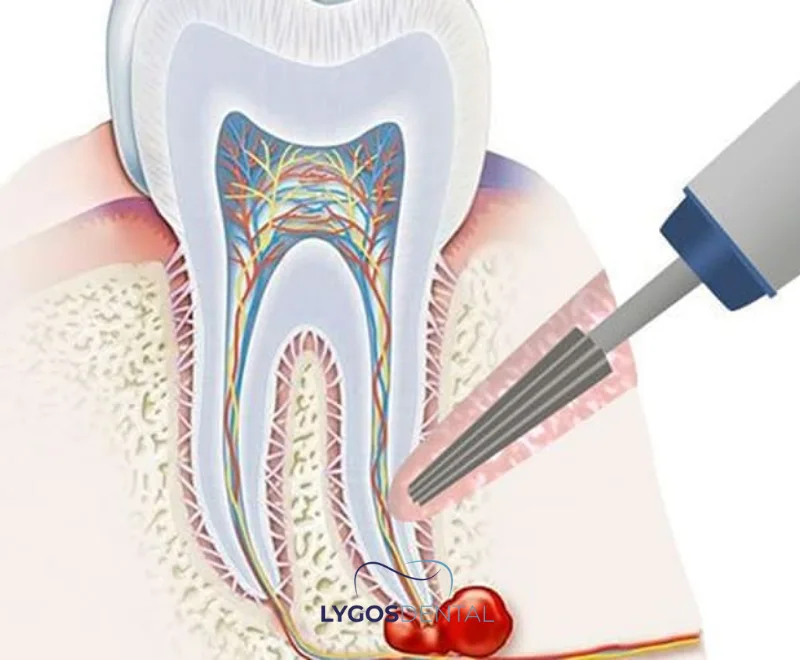
Apical resection is a surgical endodontic procedure used to treat infection at the tip of a tooth root. It’s most often recommended when root canal treatment has already been completed, but the root-end area still shows persistent inflammation, pain, or a recurring abscess. The aim is straightforward: remove the infected tissue and seal the root tip so bacteria can’t keep leaking into the surrounding bone.
Dentists may also call this procedure an apicoectomy. With modern imaging and magnification, it can be carried out with high precision, which improves comfort and predictability for many patients.
Your dentist or oral and maxillofacial surgeon may suggest apical resection when non-surgical options aren’t likely to solve the problem. This usually happens after a root canal that cannot be retreated effectively, or when the root anatomy and existing restorations make retreatment risky.
Apical resection is typically done under local anesthesia. After numbing the area, the clinician makes a small incision in the gum and creates a window in the bone to reach the root tip. Inflamed tissue is removed, and a small portion of the root end is trimmed.
The end of the root is then cleaned and sealed with a biocompatible filling material to reduce the chance of reinfection. Finally, the gum is stitched back in place. Most appointments take about 30–60 minutes, depending on which tooth is treated and how complex the root structure is.
The main advantage is tooth preservation. Keeping your natural tooth can support chewing function, bite stability, and appearance—especially in the front of the mouth. For many patients, apical resection provides a practical “second chance” for a tooth that would otherwise be removed.
Like any surgical procedure, apical resection has potential risks. Most are uncommon and manageable, especially when the case is well planned and postoperative instructions are followed.
Most patients return to normal routines within a day or two, but the surgical site needs time to heal. Discomfort is usually mild to moderate and can be managed with the medications your clinician recommends. Stitches are commonly removed about 7–10 days after the procedure, unless dissolvable sutures are used.
Contact your dental office if you have heavy bleeding, worsening swelling after the first couple of days, fever, or pain that isn’t improving.

Apical resection is usually considered when the tooth can still be saved and has enough healthy structure to function long term. If the tooth is cracked below the gum line, has severe bone loss, or cannot be restored properly, extraction may be the safer choice. Your clinician will weigh prognosis, costs, timeline, and your overall oral health before recommending the best option.
The surgery itself is performed under local anesthesia, so you shouldn’t feel pain during the procedure. Soreness afterward is common and typically improves over a few days with appropriate pain relief.
Most procedures take 30–60 minutes, though complex roots or difficult access can extend the appointment.
Initial gum healing usually happens within 7–10 days. Bone healing around the root tip takes longer and is monitored at follow-up visits, often with X-rays.
Not always. Accessibility, root shape, proximity to nerves or the sinus, and the tooth’s overall restorability all affect suitability. A clinical exam and imaging are needed to confirm whether it’s a good option.
Many cases do well when the tooth is properly selected and the root end can be sealed effectively. Your dentist can give a realistic prognosis based on the tooth involved, existing restoration, and the size of the lesion.