What is Tooth Extraction? | LYGOS DENTAL
Tooth Extraction: A Comprehensive Guide to Understanding the Procedure, Benefits, and Costs A tooth extraction is…
Pericoronitis is a painful infection of the gum around a partially erupted wisdom tooth. When a small gum flap traps food and bacteria, the area can swell and become tender, causing bad taste, trouble chewing, and limited mouth opening. Dentists treat it with cleaning, medication, and—when it keeps returning—gum flap removal or wisdom tooth extraction.
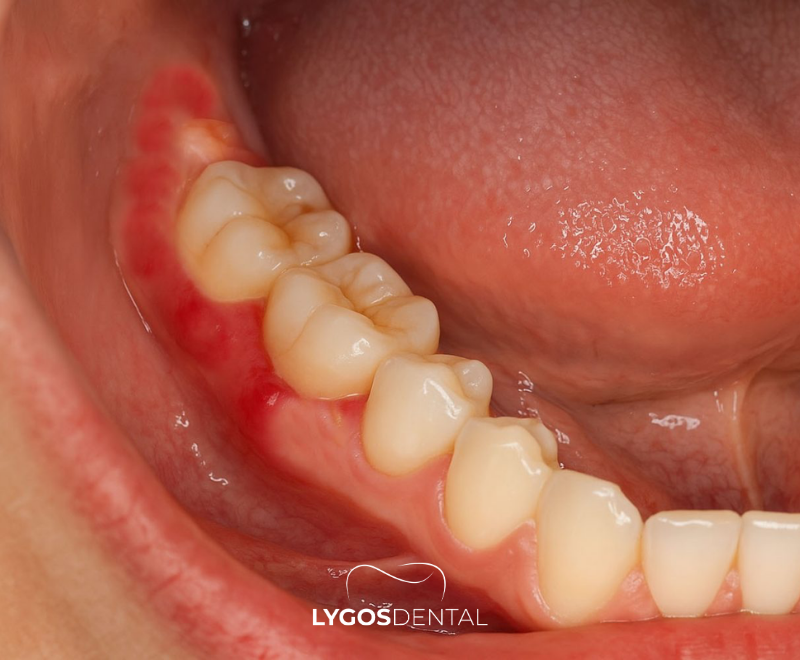
Pericoronitis is inflammation and infection of the gum tissue surrounding a wisdom tooth that has only partially erupted. The partially covered area (often called an operculum) can form a pocket where plaque, food debris, and bacteria collect. That trapped buildup irritates the gum and can trigger an infection that spreads into nearby soft tissue if not treated.
Most cases occur around lower wisdom teeth because they frequently erupt at an angle or remain partly impacted. The risk is higher when the area is hard to clean, when opposing teeth bite into the gum flap, or when general oral hygiene is disrupted. Stress, illness, and smoking can also make it easier for an infection to take hold.
Symptoms can range from mild soreness to significant pain and facial swelling. They often worsen when chewing and may flare up repeatedly over weeks or months.
Pericoronitis can become serious if the infection spreads. Seek urgent dental or emergency care if you notice any of the following warning signs.
A dentist usually diagnoses pericoronitis with an oral exam and a discussion of your symptoms. They check for swelling, trapped debris, and tenderness around the tooth. Dental X-rays are often used to see the tooth’s position and whether there is an impaction or surrounding bone involvement.
For many people, the first step is gently cleaning the pocket around the tooth and flushing it with an antiseptic solution. If there is pus, the dentist may help it drain, which can quickly reduce pressure and pain.
Pain relief is typically managed with anti-inflammatory medication when appropriate. Antibiotics may be prescribed when there are signs of spreading infection, fever, or significant swelling. Medication works best alongside professional cleaning because bacteria can remain trapped under the gum flap.
If the tooth is expected to erupt into a healthy position, removing the gum flap can eliminate the pocket where bacteria collect. This can reduce the chance of recurrence, though it may not be suitable if the tooth is poorly positioned.
If pericoronitis keeps returning, or if the wisdom tooth is impacted or difficult to clean long term, extraction is often the most definitive solution. Your dentist or oral surgeon will confirm the best option based on your X-rays, symptoms, and overall oral health.
Home measures can reduce discomfort while you arrange dental care, but they do not remove the underlying cause. Avoid applying aspirin directly to the gum, and do not rely on home remedies if symptoms are worsening.
With appropriate treatment, pain and swelling often start to improve within a few days. Mild cases may settle in 3–5 days once the area is cleaned and irritation is reduced. More significant infections may take 7–10 days, and recovery after a minor procedure or extraction can take up to around two weeks.
Pericoronitis is more likely to come back when the wisdom tooth remains partly covered by gum tissue. Good daily cleaning helps, but it may not be enough if the tooth is impacted or the gum flap is repeatedly irritated.
Symptoms can temporarily ease if trapped debris is removed and irritation decreases. Even when pain settles, the pocket under the gum flap can remain, so flare-ups are common without dental assessment and long-term management.
Sometimes, yes. Cleaning, medication, and gum flap removal may be enough when the tooth is erupting into a good position. If the tooth is impacted or infections keep returning, extraction is often the most reliable way to prevent repeat episodes.
The infection itself is not considered contagious in the way a cold or flu is. However, the bacteria that cause gum infections are common in the mouth, so prevention focuses on reducing bacterial buildup and improving access for cleaning.