Can an Infected Tooth Be Extracted? | LYGOS DENTAL
Therefore, many people wonder, “Can an infected tooth be extracted?” In this article, you can find…
Tartar (also called dental calculus) forms when plaque is left on teeth long enough to harden. Minerals in saliva “set” the sticky film into a rough deposit—often near the gumline and between teeth. Good brushing, daily flossing, and regular professional cleanings stop plaque before it turns into tartar and irritates gums.
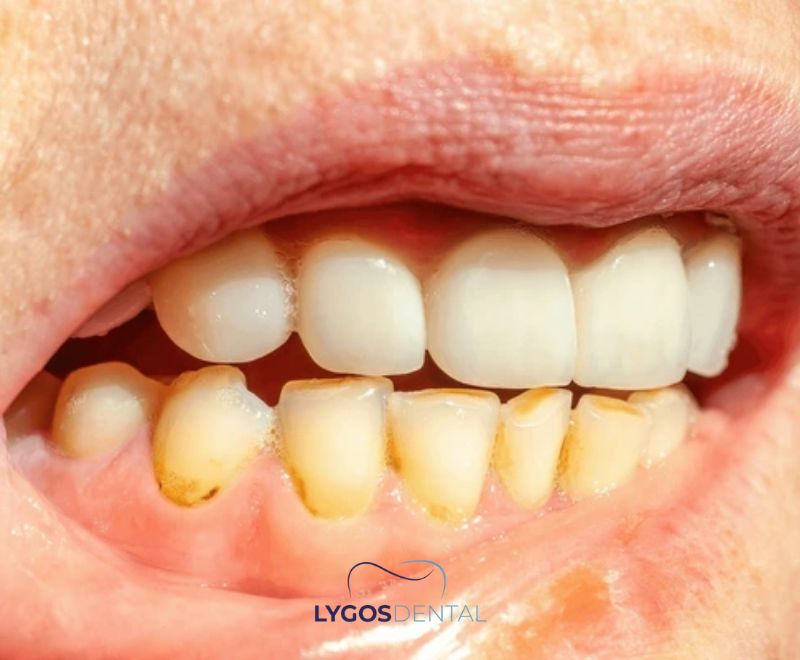
Plaque is a soft, sticky layer of bacteria and food particles that forms on teeth every day. When plaque isn’t removed thoroughly, it can mineralise and become tartar. Unlike plaque, tartar bonds to the tooth surface and creates a rough area where new plaque sticks more easily.
Tartar tends to build up most around the gumline, behind the lower front teeth, and on the outer surfaces of upper back teeth. Over time it can contribute to gum inflammation, persistent bad breath, and a higher risk of cavities.
The most common reason is missed plaque during daily cleaning. If brushing is rushed or irregular, plaque remains along the gumline and between teeth. As it hardens, it becomes tartar that can’t be removed with a toothbrush.
Saliva naturally contains minerals such as calcium and phosphate. People with higher mineral content in their saliva may develop tartar more quickly. Dry mouth (from dehydration, some medications, or mouth breathing) reduces saliva’s cleansing effect and can speed up buildup.
Smoking and other tobacco use can increase plaque and stain deposits. It also irritates gum tissue and can mask early gum disease by reducing visible bleeding. That combination often leads to heavier tartar accumulation over time.
Sugary and starchy foods feed plaque-forming bacteria, especially when snacking is frequent. Sticky foods and sweet drinks can linger on tooth surfaces and between teeth. The longer plaque sits, the more likely it is to harden into tartar.
A toothbrush can’t fully reach the tight spaces between teeth. When floss or interdental brushes aren’t used, plaque builds up in these areas and near the gumline. This is why many people notice tartar first between teeth and behind the lower front teeth.
Tartar can look different depending on where it sits and how long it has been there. Common signs include:

Small routine choices can make a big difference. These habits commonly increase plaque retention and tartar formation:
Once plaque becomes tartar, home care can’t lift it off. A dentist or dental hygienist removes it using professional instruments, often with ultrasonic scaling. Teeth are then polished to smooth the surface and make plaque less likely to stick.
If tartar extends below the gumline or there are signs of gum disease, you may need a deeper cleaning (sometimes called periodontal scaling and root planing). Your dentist will recommend the right approach based on your gum health.
Many people do well with a professional cleaning every 6–12 months. If you build tartar quickly or have gum disease risk factors, your dentist may advise more frequent visits.
Prevention comes down to stopping plaque before it hardens. A simple routine works best when it’s consistent:
Book an appointment if you notice bleeding gums, persistent bad breath, gum swelling, tooth looseness, or pain when chewing. These can be signs of gingivitis or more advanced gum disease, which needs professional care. Early treatment is usually simpler and helps protect the bone supporting your teeth.
Brush with fluoride twice daily, clean between teeth daily, and get regular professional cleanings.
Tartar forms when plaque isn’t removed and mineralizes from saliva.
No; DIY scraping can damage enamel and gums and worsen infection risk.
It can cause gum disease, bad breath, recession, bone loss, and tooth loss.
No; cleaning doesn’t loosen healthy teeth, but it can reveal existing periodontal looseness.